Clinical Image
Austin J Pathol Lab Med. 2014;1(3): 1.
An Unexpected Hemorrhoidectomy Lesion
Ryan Yu1*, Samih Salama1,2 and Salem Alowami1,2
1Department of Pathology and Molecular Medicine, McMaster University, Canada
2St. Joseph`s Hospital, Canada
*Corresponding author: Ryan Yu, Department of Pathology and Molecular Medicine, McMaster University, HSC-2N22B, 1280 Main Street West, Hamilton, ON, Canada
Received: October 28, 2014; Accepted: October 31, 2014; Published: November 03, 2014
Clinical Image
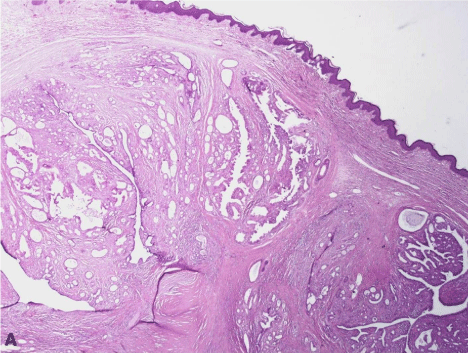
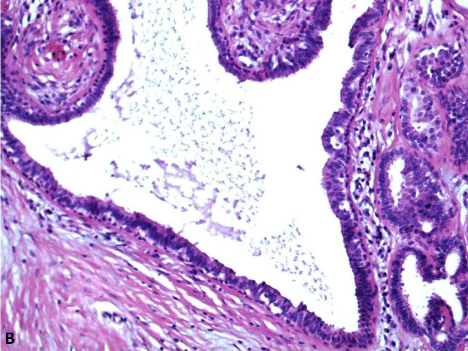
A 54-year-old woman presented with rectal bleeding. Anorectal examination showed a 2.5 cm polypoid lesion covered by skin at 9 o'clock, thought to be an external hemorrhoid, in continuity with internal hemorrhoids. Microscopic examination of the hemorrhoidectomy specimen showed a well-circumscribed dermal tumor comprised of tubules, cysts, and papillary folds projecting into cystic spaces (Figure A, H&E, 12.5x). The lumina were surrounded by a double cell layer consisting of an inner secretory cell layer and an outer myoepithelial cell layer (Figure B, H&E, 100x). The findings were consistent with hidradenoma papilliferum, an uncommon, benign skin adnexal tumor of apocrine differentiation. It presents in women, usually in the 3rd to 5th decades of life, as a small, fleshcolored nodule. Hidradenoma papilliferum occurs almost exclusively on the vulva and only occasionally in the perianal region, so it is usually not considered in the differential diagnosis of a perianal mass. Hidradenoma papilliferum has a malignant counterpart that must be excluded.
Figure A: A well-circumscribed dermal nodule, without connection to the epidermis, consisting of tubular, cystic, and papillary structures (H&E, 12.5x).