
Case Report
J Pediatr & Child Health Care. 2017; 2(1): 1011.
A Rare Case Report of Esophageal Lung Associated with VACTERL Anomaly
Loganathan PK¹*, Nair V³, Albrashdi Y³ and Boulton J4
¹Department of Neonatology, Queen Elizabeth University Hospital, Scotland
²Department of Neonatology, University Hospital of Crosshouse, Scotland
³Department of Radio-Diagnosis, Alberta Children’s Hospital, Calgary, Canada
4Department of Pediatrics, Section of Neonatology, Alberta Children’s Hospital, Canada
*Corresponding author: Prakash Kannan Loganathan, Department of Neonatology, Queen Elizabeth University Hospital, Maternity Building, Glasgow, Scotland
Received: December 20, 2016; Accepted: January 19, 2017; Published: January 23, 2017
Abstract
Background: Communicating Broncho-pulmonary-foregut malformation is one of the rare anomalies and esophageal lung is one among them.
Case Report: We report on a preterm infant with right esophageal lung associated with VACTERL anomaly.
Conclusion: This case is to report this rare association, and its unique clinical presentation and diagnosis.
Keywords: Esophageal lung; Broncho-pulmonary foregut malformation; VACTERL
Abbreviations
CBPFM: Communicating Broncho-Pulmonary Foregut Malformation; CT: Computed Tomography; ECHO: Echocardiogram; TEF: Tracheo-Esophageal Fistula; VACTERL: Vertebral defects, Anal atresia, Cardiac, Tracheo-Esophageal Fistula (TEF) with Esophageal atresia, Renal dysplasia and Limb deformities; VATER: Vertebral defects, Anal atresia, Tracheo-Esophageal Fistula (TEF) with Esophageal atresia and Renal dysplasia
Introduction
Anomalous origin of bronchus from the esophagus is rare and also known as the esophageal lung. It is one of the rare anomalies in the group of “Communicating broncho-pulmonary-foregut malformation”. The esophageal lung is associated with higher incidence of esophageal atresia, Tracheo-Esophageal Fistula (TEF) and VACTERL (Vertebral defects, Anal atresia, Cardiac defects, Tracheo-esophageal fistula, Renal anomalies, and Limb abnormalities) [1]. We report an extremely rare case of a preterm infant with right esophageal lung associated with VACTERL anomaly. This rare association, difficulty in diagnosis and unique clinical presentation is the focus of this case report.
Case Report
A 30week preterm female infant was born to a 23-year-old mother after the uneventful pregnancy. Her antenatal scan showed mild dilation of cerebral lateral ventricles, with bilateral foot abnormality, and probably sacral dysplasia. She was delivered in the special care baby unit by cesarean section, indicated for fetal distress. She was intubated at birth and post-intubation chest X-ray showed the complete collapse of the Right lung with mediastinal shift (Figure 1). After receiving one dose of surfactant and baby was transferred to tertiary neonatal intensive care unit for ongoing management. At admission she was noted to have dysmorphic features like low set ears, arthrogryposis, right lower limb dysplasia (fibula agenesis) with poly-syndactyly, and bifid great toe on the left leg. As a part of congenital anomaly work up we carried out various investigations. Chest X-ray showed adequately expanded right lung, multiple fused and segmented thoracic spine vertebrae (Figure 2). Echocardiogram (ECHO) showed type 1 truncus arteriosus with large VSD, and dysplastic truncal valve. She had a normal cranial ultrasound and renal ultrasound showed right kidney hydronephrosis. The gastric tube could not be passed beyond 8cm and the presence of dilated stomach on abdominal radiography confirmed the diagnosis of esophageal atresia with tracheaesophageal fistula (Figure 2). On day 3 of life fistula was ligated along with gastrostomy tube insertion and during bronchoscopy baby was noted to have small stenotic right main bronchus. Post surgery she noted to have a complete collapse of the right lungs. There was no improvement with antibiotics, lung recruitment strategies and alpha dornase nebulisation. Chest Ultrasound showed minimal pleural effusion, not accounting for the complete collapse. With computed tomography scan, right main bronchus and upper lobe bronchi were identified but could not identify bronchus intermedius and its branches. Right middle lobe and lower lobes are completely opacified. Right lung had normal pulmonary artery supply and pulmonary vein drainage. While planning for repeat bronchoscopy, babe also had issues with the progression of gastrostomy tube feeding. Contrast study through gastrostomy tube showed the abnormal orientation of right bronchus intermedius, which formed a communication with the distal part of the esophagus (Figure 3). With the preferential passage of contrast into the bronchus rather than duodenum and gastric outlet obstruction was suspected. With the presence of vertebral, cardiac, Tracheo-esophageal fistula, right kidney hydronephrosis and limb anomalies- VACTERL association was diagnosed. In view of truncus arteriosus and the need for right pneumonectomy, Baby was transferred to cardio-thoracic surgery center. CT angiogram showed markedly hypoplastic left pulmonary artery. With the constellation of multiple anomalies, multi-disciplinary consultations were made with cardiac surgery, cardiology, General surgery, neonatology and family. The decision was taken for palliative care and the baby passed away comfortably on day seventy-one of life. The parents deferred autopsy.
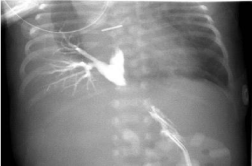
Figure 1: Chest X-ray showing the complete collapse of right lung at birth.
Note the mediastinal shift and the presence of endotracheal tube.
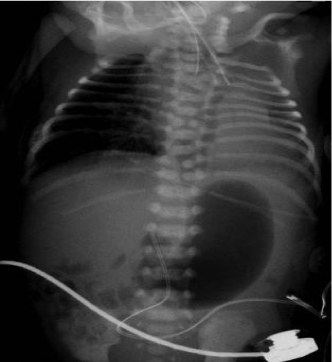
Figure 2: Chest X-ray showing coiling of the gastric tube in the upper part
of the esophagus and dilated stomach. Note there are multiple vertebral
anomalies and inflated right lung.
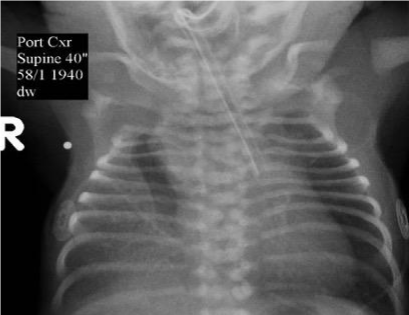
Figure 3: Contrast study through gastrostomy tube showing the retrograde
flow of contrast into right lower bronchus clearly showing bronchial markings.
Discussion
Broncho-pulmonary foregut malformation is a term is described initially by Gerle [2]. He used this term to describe pulmonary sequestration communicating with the Gastro-intestinal tract. Since there are much more variations in these category, Srikanth et al coined the term Communicating Broncho-Pulmonary Foregut Malformation (CBPFM) to indicate communication between esophagus or stomach with the respiratory tract or a part of the lungs [3]. When there an anomalous origin of bronchus from esophagus it is termed as the esophageal lung. CBPFM is commonly associated with esophageal atresia, Tracheo-Esophageal Fistula (TEF) to the distal esophagus, duodenal stenosis with the annular pancreas, imperforate anus, vertebral anomalies, and ambiguous genitalia [1,4].
CBPFM arises when cells of respiratory potential arise from esophagus distal to normal lung bud or a part of lung bud originating from esophagus instead of the ventral laryngotracheal tube. This group of cells is invaginated into adjacent normal pulmonary tissue, often maintaining a communication with esophagus or stomach by a pedicle. As pedicle outgrows its vascular supply, it disconnects with the respiratory tissue and forming a sequestration, but instead if the pedicle fails to disconnect it will form CBPFM [5]. Srikanth et al, with their own experience and literature review of 57 patients proposed an anatomical classification system [3]. Group I: anomaly is associated with esophageal atresia and tracheo-esophageal fistula; Group Ia: if entire lung arises from esophagus; Group Ib: if part of lung arises from esophagus; Group II: one lung originates from the lower esophagus; Group III: an isolated anatomic lung lobe or segment communicates with the esophagus or stomach. Group IV: A portion of the normal bronchial system communicates with the esophagus. Based on their classification our case report falls under type 1B wherein portion of lung arises from the esophagus. In their review of 57 patients, only 2 of them had type 1B and our case report is further unique with its association of VACTERAL anomalies.
VACTERL are non-randomly occurring group of malformations like Vertebral defects, Anal atresia, Tracheo-Esophageal Fistula (TEF) with esophageal atresia, cardiac, Renal dysplasia and limb deformities, out of which at least three should be there to make a diagnosis of VACTERL. More importantly, there should not be any clinical or laboratory evidence of the alternative diagnosis. The probable explanation for this association is probably due to developmental field defects that occur in blastogenesis. Of these vertebral anomalies are more common (60-80%) and in our case we had multiple fused and segmented thoracic vertebrae.Clinical presentation of CBPFM depends on the type of malformation and associated anomalies. It could be asymptomatic, recurrent respiratory tract infection and respiratory failure. Diagnosis is usually difficult due to its rarity and uncommon presentation. Investigations would include radiography, upper GI contrast and CT scan of thorax along with angiogram. In our case we considered differential diagnosis of Congenital Pulmonary Airway Malformations (CPAM) especially Congenital Cystic Adenomatoid Malformation (CCAM), pleural effusion, chylothorax, lung atelectasis, accidental ligation of right main bronchus or leakage from the ligated fistula, all of which were ruled out by USS thorax, needle aspiration and CT scan. Contrast study of the esophagus (esophagram) can be useful, but in cases of esophageal atresia, contrast study through gastrostomy tube with suspected lung in dependent lesion will help us in making the diagnosis. A cardiac angiogram may be essential to identify the supplying vessel to the sequestrated lung, which helps in surgery.In our case report, Initial chest radiograph taken at birth showed completely collapsed lung and then subsequent x-rays showed adequately inflated right lung. This is probably due to retrograde flow of air from the stomach, draining into right lungs through broncho-esophageal fistula (during positive pressure ventilation at resuscitation at the time of birth). Immediately after the surgical ligation of trachea-esophageal fistula, there is no air draining from stomach to the right lung, which led to complete collapse of the right lung. Complete anatomy is illustrated in (Figure 4).In our literature search, we found only three case reports of the right esophageal lung associated with VACTERL/VATER anomaly [6-8]. This case report is to emphasize the importance of considering CBPFM as one of the diagnoses in any infant with persistent unilateral lung opacification, especially worsening with feeding should raise the suspicion of this rare anomaly [1].
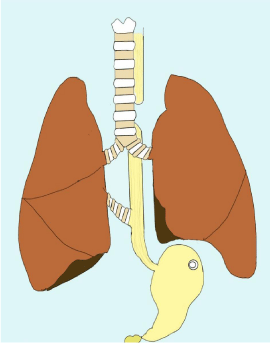
Figure 4: Illustration of complete anatomy showing esophageal atresia,
tracheo- esophageal fistula, gastrostomy tube and right broncho-esophageal
communication.
References
- Colleran GC, Ryan CE, Lee EY, Sweeney B, Rea D, Brenner C. Computed tomography and upper gastrointestinal series findings of esophageal bronchi in infants. Pediatr Radiol. 2016.
- Gerle RD, Jaretzki A, Ashley CA, Berne AS. Congenital bronchopulmonaryforegut malformation. Pulmonary sequestration communicating with the gastrointestinal tract. N Engl J Med. 1968; 278:1413-1419.
- Srikanth MS, Ford EG, Stanley P, Mahour GH. Communicating bronchopulmonary foregut malformations: classification and embryogenesis. J Pediatr Surg. 1992; 27: 732-736.
- Verma A, Mohan S, Kathuria M, Baijal SS. Esophageal bronchus: case report and review of the literature. Acta Radiol. 2008; 49: 138-141.
- Leithiser RE, Capitanio MA, Macpherson RI, Wood BP. “Communicating” bronchopulmonary foregut malformations. AJR Am J Roentgenol. 1986; 146: 227-231.
- Bleicher MA, Melmed AP, Bogaerts XV, Sklar GS. VATER association and unrecognized bronchopulmonary foregut malformation complicating anesthesia. The Mt Sinai J Med. 1983; 50: 435-438.
- Davies RP, Kozlowski K, Wood BP. Radiological case of the month. Rightupper- lobe esophageal bronchus (with VATER anomalies). Am J Dis Child. 1989; 143: 251-252.
- Linke F, Kraemer W, Ansorge M, Brzezinska R, Berger S. Right esophageal lung in a preterm child with VACTERL association and Mayer-Rokitansky- Kuster-Hauser syndrome. Pediatr Surg Int. 2005; 21: 285-288.