
Research Article
J Pediatr & Child Health Care. 2019; 4(1): 1025.
The Therapeutic Management of Autism Spectrum Disorders: Cross-Sectional Retrospective Study of Prescriptors in Morocco
Sefrioui MR¹*, Bensaid M², Elidrissi I³, Kadiri M4, Mehssani J4, Bichra MZ4, AlBouzidi A2, Cherrah Y5, Benmoussa A¹ and Derraji S5
¹Laboratory of Drug Science, Biomedical and Biotechnological Research, Hassan II University, Morocco
²Mohamed V Military Teaching Hospital, Mohamed V University, Rabat Morocco
³Faculty of Medicine and Pharmacy, Mohamed V University, Rabat Morocco
4Psychiatry Service, Mohamed V Military Teaching Hospital, Rabat Morocco
5Laboratory of Pharmacology-Toxicology, Mohamed V University, Rabat Morocco
*Corresponding author: Sefrioui MR, Laboratory of Drug Science, Biomedical and Biotechnological Research, Faculty of Medicine and Pharmacy of Casablanca, Hassan II University, Tarik Ibnou Ziyad Street, Casablanca, Morocco
Received: February 01, 2019; Accepted: March 05, 2019; Published: March 12, 2019
Abstract
Background: Autism Spectrum Disorders (ASD) represents a developmental disorder that affect verbal and nonverbal communication, social interaction and daily activities. Aims: The purpose of this study is to identify different treatment prescribed for individuals with ASD and to evaluate the efficiency of pharmacotherapy and behavioral management in autistic patients from Morocco.
Methods and Procedures: Our survey included 72 health professionals, 50 of whom were drug prescribers and 22 non- prescribers.
Outcomes and Results: 68% of the prescriber professionals prescribe drugs for autism and 65% of these are off label. The most prescribed therapeutic classes are antipsychotics (76%). 56% of prescriber professionals noticed an improvement in the quality of life of children following prescription medication. Moreover, 92% of the professionals prescribe drugs for autism-associated conditions; antiepileptic drugs are the most prescribed (65%). In addition, 26% of prescribing physicians and 28% of non-prescribers associate a diet with the management of ASD. According to them, the improvement in the quality of life of children with autism following the combination of a diet is 20% and 76% respectively. On the other hand, 58% of prescribers and all non-prescriber professionals have shown that the behavioral management method is the most satisfactory method.
Conclusion: These data highlight the high rate of drug prescription for autism disorder in Morocco and despite non FDA-approved uses, the improvement in the quality of life is considerable. Also, Applied Behavior Analysis (ABA) provide successful treatment and optimize outcome.
Keywords: Autism spectrum disorders; Quality of life; Therapeutic management; Prescriptors; Morocco
Background
Autism Spectrum Disorders (ASD) are a developmental condition characterized by disruption of social interaction, communication disorder, repetitive and stereotyped behaviors. The prevalence studies suggest that autism affects as many as 1 in 100 children [1] with a marked excess of boys compared with girls of 4:1 [2,3]. Many observations indicate that genetic and environmental factors play an important role in ASD [4]. Epidemiological evidence such as high disease concordance in monozygotic twins and also family segregation studies indicate that autistic disorder is subject to genetic predisposition [5] and exhibit wide clinical and heterogeneous genetic architecture. Potential environmental factors like prenatal exposure to drugs, congenital viral infections and prolonged or intensive exposure to air pollutants negatively influences neurodevelopment and greatly increase the risk of developing ASD [5-8].
The clinical management of autism focuses primarily on improving the quality of life and trying to establish functional independence of the affected person [9,10] by decreasing core symptoms and lowing aggressive behaviors [11]. Drugs such as antipsychotics are currently used to treat certain associated symptoms such as aggression [12,13]. Only risperidone and aripiprazole psychotropic medication are US FDA approved for the treatment of conditions co-occurred with ASD [14]. Although there is currently no specific pharmacological treatment of autism that directly targets the cause [15]. Using medication treatment may be needful in combination with psychological methods such as Applied Behavior Analysis (ABA) that has been the best treatment for improving behaviors [8], such as adaptive skills [16]. On the other hand, recent studies have shown a link between autism and the modification of microbiota composition [17]. Thereby, several nutritional strategies are suggested as glutenand casein-free diet, cancellation of complex carbohydrate and their substitution with monosaccharides. This nutritional therapy allow to adjust brain connectivity. In addition, Probiotic treatment has proven effective for the treatment of immune and gastrointestinal problems, associated with ASD [18].
In Morocco autism is a common disorder and no study has been done to describe the prescription practices in the ASD Moroccan population. So, the aim of this study is to identify different treatment prescribed for individuals with ASD and to evaluate the efficiency of pharmacotherapy and behavioral management in autistic patients.
Methods
ASD Cases
A child was included in our study if he or she displayed the criteria for diagnosis and assessment of autism according with the Diagnostic and Statistical Manual of Mental Disorder, Fifth Edition (DSM-V). Our survey involved 90 autistic children, aged 15 years old and under in 2017, hospitalized or in consultation at the Hospital of the Day of Child Psychiatry Service at Errazi Hospital in Salé city and children enjoying Oxygen therapy sessions at the Mohammed V Military Teaching Hospital in Rabat. These children are coming from all the regions of Morocco and from the different social and intellectual classes. Are excluded from our study children over 15 years of age in 2017, children suffering from a disorder other than autism spectrum disorders such as schizophrenic psychoses of children and adolescents, dysthymic psychoses, psychosis acute and others.
Study strategy
This is a Cross-sectional retrospective study, spread over a period of 10 months, between January and October 2017. The survey of professionals took place in Child Psychiatry Service at Errazi Hospital, Salé city and in Mohammed V Military Teaching Hospital in Rabat. Our survey included 72 health professionals, 50 of whom were drug prescribers and 22 non-drug prescribers. Of the 50 prescribers, 72% are psychiatrists, 20% are pediatricians and 8% are child psychiatrist. Of the 22 non-drug prescribing professionals, 59% are psychologists, 23% are psychiatric nurses, 13% are psychomotor doctors and 5% are speech therapists. The study was performed on the patients present at the time of the survey (at least one patient for each professionel was present at the time of survey). The questionnaire addressed to the professionals consists of 17 different questions concerning the Presentation of the professionals, the diagnosis and the symptomatology of the autism, the medical treatment of the autism and associated pathologies, the combination of a diet dietery, the recommended and practiced management method, and a concluding question about the most satisfactory method of care. All of these responses allowed us to study the drug or behavioral management of children with autism.
Data analysis
The results were recorded on an Excel® database and we used percentage for description of qualitative variables.
Results
Our working hypothesis was to establish a survey of health professionals in order to identify current prescription attitudes for individuals with ASD. The exercise duration of prescribing physicians and non-drug prescribing professionals varies between 3 and more than 10 years (60% of prescribers had greater than 10 years of experience and 50% of non-prescribers had a duration of exercice between 5 and 10 yeras).
All prescribers diagnose autism based on behavioral observation and parenting. Among them, 96% are also based on clinical examinations, 36% require radiological examinations, 30% add biological assessments and 44% complete their diagnosis by other tests namely ADOS/ADI (Autism Diagnostic Observation Schedule/Autism Diagnosis Interview). For non-drug prescribing professionals, 92% are based on observation of behavior, 84% are also based on clinical examinations and parents statements, 16% on radiological examinations, 20% on biological examinations and 40% on clinical examinations. Autism is a vast clinical picture whose symptomatology differs from one subject to another. All prescribers confirm that communication and socialization disorders are the main symptoms of autism. Of these professionals, 80% reported behavioral problems, 44% reported stereotyping, 8% noticed sensory disturbances and 10% found other disorders. The majority of these professionals (68%) prescribe drugs for autism. Of the prescriptions, 65% are off-label. Antipsychotics and antidepressants drugs are the most prescribed therapeutic class and were prescribed respectively to 76% and 41% of the ASD children (Figure 1). More than half of these professionals (56%) noticed an improvement in the quality of life of children with autism following prescription medication, the improvement was noted via clinical observations of the professional and also according to the parent report (for exemple reduction of aggression, self-injurious and irritability symptoms).
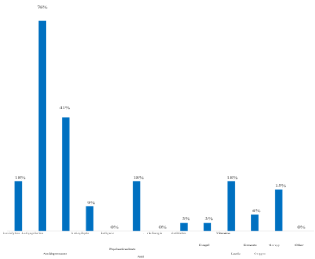
Figure 1: Distribution of therapeutic classes prescribed for autism.
All prescribers (100%) diagnose conditions associated with autism. Psychomotor disorders, sensory deficits and intellectual disability are always associated with ASD. Other pathologies may be associated such as epilepsy (72%), digestive disorders (60%), psychiatric disorders (48%) and eating disorders (Pica, bulimia, food selectivity...) (24%). The majority of these professionals (92%) prescribe drugs for these associated conditions, antiepileptic drugs are the most prescribed drugs (65%) (Figure 2). For non-prescribers, 92% diagnose diseases associated with ASD. Epilepsy is the most common pathology (80%), followed by psychomotor problems (68%), intellectual disability (60%), digestive disorders (44%), sensory deficits (36%), psychiatric disorders (32%), and other disorders (24%). Among prescribing physicians, 26% associate a diet with the management of ASD. According to them, the improvement in the quality of life of children with autism following the combination of a diet is very low (20%). The gluten-free and casein-free diet represents 100% of the combined diets, followed by the preservative-free diet (46%) and the hypotoxic diet without dyes (8% each). For non prescribers, 28% associate a diet with the care of children with autism. Still, 76% confirm that according to parents statements, the diet reduce the digestive disorder of autistic children. The gluten-free and casein-free diet represents 100% of the diets associated with these non-prescribers, followed by the no preservatives diet (29%). The hypotoxic diet and without dyes are not associated. According to our survey, medication prescriptions represent the most recommended (68%) and most practiced (60%) therapeutic management method by prescribing professionals. Other management methods are also practiced and recommended by prescribers (Figure 3). According to 58% of these professionals, the behavioral management method is the most satisfactory in communication and socialization improvements. ABA is the most common method (72%) and the most recommended (88%). These professionals practice and recommend other management methods (Figure 4). For non-drug prescribing professionals, the behavioral management method is the most satisfactory in terms of results like eye contact, cooperative with people reduction of agitation and repetitive movements, decreases behaviors problems. ABA is the most popular method (64%) and the most recommended method (76%). Other methods of behavioral management are practiced and recommended by non-drug prescribing professionals (Figure 5). The combination of a diet is the most recommended method (36%) according to these professionals (Figure 6).
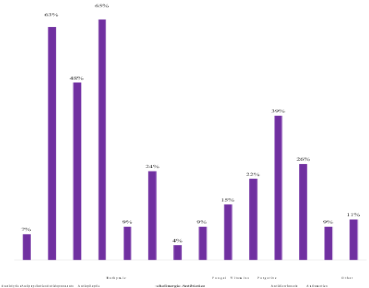
Figure 2: The distribution of prescriptions according to the therapeutic
classes prescribed for the pathologies associated with autism.
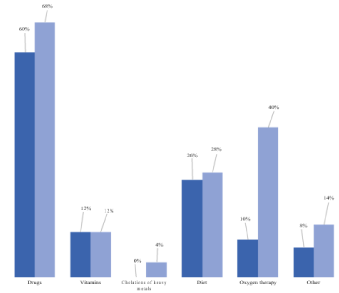
Figure 3: Drug Management Methods.
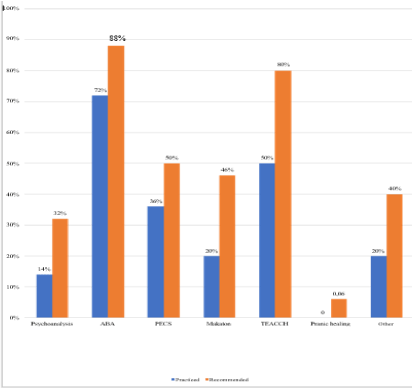
Figure 4: Behavioral and developmental management methods.
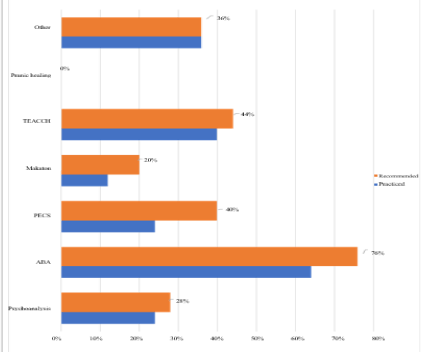
Figure 5: Distribution of non-prescribers according to the methods of care
taken and recommended.
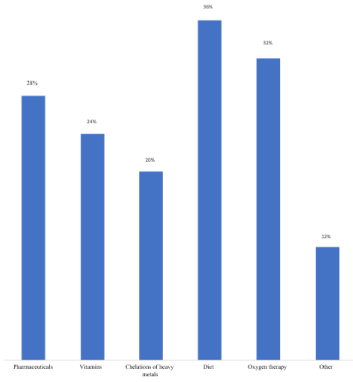
Figure 6: Distribution of non-prescribers according to recommended drug
management methods.
Only 28% of prescribing professionals have confirmed that there is a chance to cure autism. Nearly half say that autism Cannot be cured under any circumstances. However, 24% did not answer this question clearly. They have chosen the term improvement of quality of life by early and adequate care. They insisted that this question depends on several factors and especially the severity of the disorder. Among non-prescribers, 20% confirmed that there is a chance to cure autism. On the other hand, more than half say that autism cannot be cured under any circumstances. Only 24% did not answer this question.
Discussion
Autism is defined in international classifications as an Invasive Developmental Disorder characterized by a qualitative alteration of social interactions and communication, as well as by the restricted, repetitive and stereotyped nature of behaviors, interests and activities [19]. According to our survey, professionals rely on different criteria to diagnose autism with variant symptomatology. This difference is explained by the difficulty of diagnoses that require specialized clinics, including multidisciplinary teams of scientific training, knowing the literature on the subject, and having a sufficient number of references for the constitution of a clinical expertise.
Medicated management of autism and these associated pathologies:
The purpose of this study was to characterize use of different treatment for Moroccan individuals with ASD and to evaluate the efficiency of pharmacotherapy and behavioral management in autistic patients.
We found that 68% of professionals prescribe drugs for the therapeutic management of ASD. This value is consistent with the US prevalence rate where 50-75% of children with ASD are on psychotropic medication [20,21]. The drug prescription rate in Morocco is higher than those found in England (24% on psychotropic drugs) [22] and in Germany (33%) [20]. According to our study, antipsychotics are the most prescribed drugs (76%), which is consistent with the international situation. Antipsychotics have made a dramatic breakthrough among patients with autism [22- 27]. According to a US study, drug prescriptions for autism were as follows: Antipsychotics (66%), Antidepressants (21%), Antiepileptics (59%), Anxiolytics (21%), Psychostimulants (18%), Vitamins (25%) Antibiotics (47%), Antifungals (48%) [22-27]. According to our study, antiepileptics are much less prescribed (9%) for the therapeutic management of ASDs, but they are the leading prescription for the associated pathologies (65%). On the other hand, psychostimulants are little prescribed which contrasts with international and European studies [22,23,25-27]. Methylphenidate, psychostimulant indicated in the global management of ADHD (Attention Deficit Disorder with or without Hyperactivity), is little prescribed in Morocco whereas it would be the most used molecule for children with ASD in Europe [28]. These results probably illustrate a form of Moroccan exception. Surprisingly, no specialist reports the use of melatonin in the management of sleep disorders, although it has proved its effectiveness and interest in improving the symptoms of the autistic core [29]. According to our survey, off-label prescriptions are in the majority with a rate of 65%. This value is higher than that mentioned in a French study (7%). In autism even more than in the pediatric population, most prescriptions are off-label [30,31], and this trend is steadily increasing [33,34]. More than half of the prescribers (56%) have noticed an improvement in the quality of life of children with autism following prescription medication. According to a French study, only 32% of parents noted an overall positive effect of treatment. The main improvements observed were the overall behavior of the child (28%) and the decrease in the intensity and frequency of behavioral disorders (22%), particularly anger (4%) and motor hetero-aggressiveness (4%). Sleep (10%), attention and concentration (8%), as well as mood and anxiety (5%) were also improved. For the treatment of associated pathologies, antiepileptic drugs top the list (65%) followed by antipsychotics (63%) and antidepressants (48%). Among the prescribing professionals, 72% associated epilepsy with autism, compared to 80% for non-prescribers. Our results are consistent with those of an American study in which 72% of children had epileptic seizures [32]. Antiepileptic drugs have a historically larger role because of the high rate of epileptic comorbidity in this population [32]. Besides the essential features of autism, there are other less typical manifestations. Sensory disturbances are common in our population. These disturbances can thus be manifested by an exaggerated search for sensory stimulation or by an avoidance of these sensations. Behavioral problems such as aggressive behavior towards others or towards oneself (self-injury) are common in 100% of children. These crises are due to incomprehensible situations, changes in routines, communication problems and sensory problems. Sleep disorders often pose huge problems for parents and caregivers.
Association of a food exclusion scheme
Only 26% of prescribing professionals associate a diet with the therapeutic management of children with ASD. According to these prescribers, the improvement in quality of life following the combination of a diet is very low (20%), which justifies this minimal rate of prescribing. For non-prescribers, 28% associate a diet. According to them, the percentage of improvement in the quality of life of children with autism is very high (76%), which is at odds with the minimal rate of its prescription by these professionals. All diets are gluten-free and casein-free diets, according to all professionals. These prescription rates of diet by these professionals are consistent with the data described in the literature where 20 to 70% of professionals prescribe a diet according to a review [35]. It has long been known that the exclusion of wheat and animal milks reduces autism symptoms suggesting that autistic children have a defect in gluten and casein metabolism [18]. By incomplete degradation, gluten can provide many peptides that pass into the bloodstream because of the excessive permeability of the intestine. Subsequently, gluten produces gliadin morphine, a very toxic substance that interacts in communication between neurotransmitters and neuroreceptors. Subsequently, these peptides reach the brain’s receptors as opioids. These “peptides” will behave in the body like certain opioids and promote the development of a whole range of behavioral disorders, ranging from hyperactivity to autism, through personality disorders; indifference, withdrawal and lack of language are the major consequences [36]. More recently, Elder et al. in 2006 conducted a randomized controlled trial of two groups of children aged 2 to 16 years with ASD. The latter benefited from a gluten-free diet without casein or from a placebo dietary treatment, in cross-over. This trial was inconclusive in favor of glutenfree casein-free diet [35]. In total and in spite of the number of articles published on this topic, the authors advise against this regime because of the absence of rigorous clinical facts validating its application. In addition, it is contraindicated to put children of growth age on a diet without medical supervision. From this, we can explain the contradiction and the difference in improvement rates of the autistic child following the association of a diet between prescribers and nonprescribers.
Cure autism
The question of curing autism represented for some professionals a puzzled question, others found themselves in a situation of hesitation before answering. According to current research, autism is not a disease and, researchers agree that autism is a neuro-developmental disorder whose causes are not yet defined, and which may or may not be associated with other issues (intellectual disability, epilepsy, intestinal disorders, allergies, etc.). It is important to understand how the genetic and environmental risk factors can interact and have an effect on the normal development of the brain and contribute to a phenotype of autism that present an heterogeneity between patients. Thereby, targeted therapy might be needed for the treatment of each patient group with ASD [4]. For the Federation, autism can also be defined as a permanent state or way of being. Numerous studies have shown that the development of the full potential of people with autism can be more effectively promoted through the use of recognized educational methods and intervention models, rather than medical approaches. So, Muhle et al. [4] declared that While waiting for personalized medicine, clinicians should apply behavioral strategies and prescribe drugs only for associated symptoms. Autism is not and will never be a disease, but a neuro-developmental condition, and its characteristics may change during development and some people will see a significant improvement. Moreover, an improvement does not mean a cure. In our opinion, we should deploy our energy and resources to empower them to take a meaningful place in the community, to the extent of their abilities.
Conclusion
Finally, our data highlight the high rate of drug prescription for autism disorder in Morocco and despite non FDA-approved uses, the improvement in the quality of life is considerable. Also, educational behavioral intervention provide successful treatment. It is possible that parents of children are worried about the behavioral problems of their children and are willing to try the drugs, lack of FDA approval not withstanding. It is important to monitor the improvement of the condition of the autistic child. This approach helps clinicians to establish the benefits of treatment received for the well-being of these patients.
References
- Kogan MD, Blumberg SJ, Schieve LA, Boyle CA, Perrin JM, Ghandour RM, Singh GK, et al. Prevalence of parent-reported diagnosis of autism spectrum disorder among children in the US, 2007. Pediatrics. 2009; 124: 1395-1403.
- Fombonne E. Epidemiology of autistic disorder and other pervasive developmental disorders. J Clin Psychiatry. 2005; 66: 3-8.
- Santangelo SL, Tsatsanis K. What is known about autism: genes, brain, and behavior? Am J Pharmacogenomics. 2005; 5: 71-92.
- Muhle RA, Reed HE, Stratigos KA, Veenstra-VanderWeele J, et al. The Emerging Clinical Neuroscience of Autism Spectrum Disorder. JAMA Psychiatry. 2018; 75: 514-523.
- Bailey A, Le Couteur A, Gottesman I, Bolton P, Simonoff E, Yuzda E, et al. Autism as a strongly genetic disorder: evidence from a British twin study. Psychol Med. 1995; 25: 63-77.
- Hultman CM, Sandin S, Levine SZ, Lichtenstein P, Reichenberg A, et al. Advancing paternal age and risk of autism: new evidence from a population-based study and a meta-analysis of epidemiological studies. Mol Psychiatry. 2011; 16: 1203-1212.
- Modabbernia A, Velthorst E, Reichenberg A. Environmental risk factors for autism: an evidence-based review of systematic reviews and meta-analyses. Mol Autism. 2017; 8: 13.
- Matson JL, Sipes M, Fodstad JC, Mary E. Fitzgerald. Issues in the Management of Challenging Behaviours of Adults with Autism Spectrum Disorder. CNS Drugs. 2011; 25: 597-606.
- Carbone PS, Farley M, Do TD. Primary care for children with autism. American Family Physician. 2010; 81: 453-460.
- Myers SM, Johnson CP. American Academy of Pediatrics Council on Children with Disabilities. Management of children with autism spectrum disorders. Pediatrics. 2007; 120: 1162-1182.
- Cadman T, Eklund H, Howley D, Hayward H, Clarke H, et al. Caregiver burden as people with autism spectrum disorder and attention-deficit/hyperactivity disorder transition into adolescence and adulthood in the United Kingdom. Journal of the American Academy of Child and Adolescent Psychiatry. 2012; 51: 879-888.
- McDougle CJ, Kem DL, Posey DJ. Case series: use of ziprasidone for maladaptive symptoms in youths with autism. J Am Acad Child Adolesc Psychiatry. 2002; 41: 921-927.
- West L, Waldrop J, Brunssen S. Pharmacologic treatment for the core deficits and associated symptoms of autism in children. J Pediatr Health Care. 2009; 23: 75-89.
- Canitano R, Scandurra V. Psychopharmacology in autism: an update. Prog Neuropsychopharmacol Biol Psychiatry. 2011; 35: 18-28.
- Posey DJ, Erickson CA, McDougle CJ. Developing drugs for core social and communication impairment in autism. Child Adolesc Psychiatr Clin N Am. 2008; 17: 787-801.
- Virues-Ortega J. Applied behavior analytic intervention for autism in early childhood: meta-analysis, meta-regression and dose-response meta-analysis of multiple outcomes. Clin Psychol Rev. 2010; 30: 387-399.
- Van De Sande MM, VJ van Buul, Brouns FJ. Autism and nutrition: the role of the gut-brain axis. Nutr Res Rev. 2014; 27: 199-214.
- Claudia Cristiano, Adriano Lama, Francesca Lembo, Maria P Mollica, Antonio Calignano, Giuseppina Mattace Raso. Interplay Between Peripheral and Central Inflammation in Autism Spectrum Disorders: Possible Nutritional and Therapeutic Strategies. Frontiers in physiology. 2018; 9: 184.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV-TR). Washington DC.
- Mandell DS, Morales KH, Marcus SC, Stahmer AC, Doshi J, Polsky DE. Psychotropic medication use among Medicaid-enrolled children with autism spectrum disorders. Pediatrics. 2008; 121: 441-448.
- Schubart JR, Camacho F, Leslie D. Psychotropic medication trends amongchildren and adolescents with autism spectrum disorder in the Medicaid program. Autism. 2014; 18: 631-637.
- Murray ML, Hsia Y, Glaser K, Simonoff E, Murphy DG, Asherson PJ, et al. Pharmacological treatments prescribed to people with Autism Spec-Trum Disorder (ASD) in primary health care. Psychopharmacology (Berl). 2014; 231: 1011-1121.
- Bachmann CJ, Manthey T, Kamp-Becker I, Glaeske G, Hoffmann F. Psychopharmacological treatment in children and adolescents with autismspectrum disorders in Germany. Res Dev Disabil. 2013; 34: 2551-2563.
- Cohen D, Raffin M, Bodeau N, Canitano R, Bonnot O, Périsse D, et al. Risperidone and aripiprazole in children and adolescents with autism and/or intellectual disability: a Bayesian meta-analysis. Res Autism Spectr Disord. 2013; 7: 167-175.
- Esbensen AJ, Greenberg JS, Seltzer MM, Aman MG. A longitudinal investigation of psychotropic and non-psychotropic medication use among adolescents and adults with autism spectrum disorders. J Autism Dev Disord. 2009; 39: 1339-1149.
- Rosenberg RE, Mandell DS, Farmer JE, Law JK, Marvin AR, Law PA. Psychotropic medication use among children with autism spectrum disorders enrolled in a national registry, 2007-2008. J Autism Dev Disord. 2010; 40: 342-351.
- Wong AY, Hsia Y, Chan EW, Murphy DG, Simon off E, Buitelaar JK, et al. The variation of psychopharmacological prescription rates for people with Autism Spectrum Disorder (ASD) in 30 countries. Autism Res. 2014; 7: 543-554.
- Directorate-General, ECHCP. Some elements about the prevalence of Autism Spectrum Disorders (ASD) in the European Union. Luxembourg: European Commission, Public Health; 2006; 16.
- Tordjman S, Najjar I, Bellissant E, Anderson GM, Barburoth M, CohenD, et al. Advances in the research of melatonin in autism spec-trum disorders: literature review and new perspectives. Int J Mol Sci. 2013; 14: 20508-20542.
- Penfold RB, Stewart C, Hunkeler EM, Madden JM, Cummings JR, Owen-Smith AA, et al. Use of antipsychotic medications in pediatric populations: what do the data say? Curr Psychiatry Rep. 2013; 15: 426.
- Myers SM, Johnson CP. Management of children with autism spectrum disorders. Pediatrics. 2007; 120: 1162-1182.
- Coury DL, Anagnostou E, Manning-Courtney P, Reynolds A, Cole L, McCoy R, et al. Use of psychotropic medication in children and adolescents with autism spectrum disorders. Pediatrics. 2012; 130: S69-S76.
- Persico AM, Arango C, Buitelaar JK, Correll CU, Glennon JC, Hoekstra PJ, et al. Unmet needs in paediatric psychopharmacology: present scenario and future perspectives. Eur Neuropsychopharmacol. 2015; 25: 1513-1531.
- Williams PG, Woods C, Stevenson M, Davis DW, Radmacher P, SmithM. Psychotropic medication use in children with autism in the Kentucky Medicaid population. Clin Pediatr (Phila). 2012; 51: 923-927.
- Elder JH, Shanker M, Shuster J, Theriaque D, Burns S, Sherrill L. The gluten-free, casein free diet in autism: results of a preliminary ouble blind clinical trial. J Autism Dev Disord. 1996; 36: 413-420.
- Knivsberg AM, Wiig K, Lind G, Magne N. Dietary intervention in autistic syndromes. Brain defunct. 1990; 3: 315-327.