Abstract
Patients with type 2 diabetes who have hypercholesterolemia frequently need to take HMG-CoA reductase inhibitors. A key factor in the pathophysiology of type 2 diabetes is altered pancreatic beta-cell activity, which results in a reduced ability of the pancreas to secrete insulin in response to glucose. The impact of HMG-CoA reductase inhibitors on -cell function must therefore be investigated. The regulation of -cell function is greatly influenced by the cytosolic Ca2+ concentration ([Ca2+]i). The current work looked at how HMG-CoA reductase inhibitors affected the [Ca2+]i signaling and insulin release that glucose-induced in rat islet -cells. Simvastatin, a lipophilic HMG-CoA reductase inhibitor, suppressed the initial phase increase and oscillation of [Ca2+]i caused by 8.3 mM glucose in single -cells at concentrations ranging from 0.1 to 3 g ml—1. The fewer Simvastatin-acid, a lipophilic inhibitor, decreased the first [Ca2+]i rise but was two orders of magnitude less effective. Pravastatin (100g ml—1), a hydrophilic inhibitor, has little impact on [Ca2+]. Simvastatin (0.3g ml–1) reduced glucose-induced insulin production from islets more effectively than simvastatin-acid (30g ml–1), whereas pravastatin (100g ml–1) had no effect. Simvastatin, but not pravastatin, showed a reversible blockage of the L-type Ca2+ channels in -cells in whole-cell patch clamp recordings. Simvastatin also prevented the opening of L-type Ca2+ channels, which is how L-arginine and HCl enhance [Ca2+] Conclusion: By blocking L-type Ca2+ channels in -cells, lipophilic HMG-CoA reductase inhibitors can prevent glucose-induced [Ca2+]i signaling and insulin secretion, and their inhibitory potencies are inversely correlated with their lipophilicities. Precaution must be takenWhen HMG-CoA reductase inhibitors are utilized in clinical settings, attention should be given to these findings, especially in type 2 diabetic patients.
Keywords: HMG-CoA reductase inhibitor; Simvastatin; Pravastatin; Lipophilicity; Islet; β-cell; Cytosolic Ca2+; L-type Ca2+ channel; Insulin secretion; Diabetes
Introduction
The rate-limiting enzyme in cholesterol production is inhibited specifically and competitively by 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase inhibitors [1]. HMG-CoA reductase inhibitors have been shown to be effective in lowering plasma cholesterol levels and lowering the incidence of cardiovascular disease in long-term clinical studies (2–5.3 years) [7,18,19,21]. As a result, HMG-CoA reductase inhibitors are frequently utilized to treat hypercholesterolemic individuals [15]. Patients with diabetes and atherosclerotic plaque frequently experience hypercholesterolemia. One of the main causes of death among diabetic people is cardiovascular disease. HMG-CoA reductase inhibitors are so frequently given to diabetic individuals. According to numerous studies (Hosaka et al., 1977) [16,17,51], type 2 diabetes (non-insulin-dependent diabetes mellitus) is thought to develop and progress as a result of altered pancreatic beta-cell function that results in an impaired insulin secretory response to glucose. Therefore, it is crucial to look into any potential inhibition of -cell functions by HMG-CoA reductase inhibitors. It is well known that the control of -cell processes, including insulin secretion, depends heavily on the cytosolic Ca2+ concentration ([Ca2+]i) [10,26]. Ammala and others 1996). Recent studies have shown that [Ca2+]i oscillations can control gene expression [8,38]. Therefore, the current investigation looked at how HMG-CoA reductase inhibitors affected the [Ca2+]i oscillations and insulin secretion in islet -cells caused by glucose. HMG-CoA reductase inhibitors come in two different varieties: pravastatin, a hydrophilic inhibitor, and simvastatin and lovastatin, lipophilic inhibitors. Simvastatin's lactone ring makes it lipophilic. Simvastatin-acid, an in vivo active metabolite, is partly hydrophilic in its open acid form [20]. The acid form of pravastatin is hydrophilic [20]. Both versions of simvastatin and pravastatin have equivalent HMG-CoA reductase inhibitory activity in decreasing serum cholesterol levels. Inhibitors of HMG-CoA reductase have Although the frequency is very low, it has been clinically and experimentally reported to produce myotonia and severe rhabdomyolysis [24,25,33]. It has been demonstrated that the lipophilicity of HMG-CoA reductase inhibitors plays a key role in their ability to cause fast cell damage in L-myocytes [42]. Therefore, the effects of simvastatin, simvastatin-acid, and pravastatin on glucose-stimulated -cells were compared in the present investigation.
Methods
Selection of-Cells and the Populations of Islets and Individual-Cells
As described before [30], islets and single -cells were produced. In a nutshell, islets of Langerhans were extracted by collagenase digestion from Wistar rats aged 8–12 weeks. Pentobarbital was administered intraperitoneally to the animals to make them unconscious.80 mg/kg-1. After ligating the common bile duct proximal to the pancreas, the abdomen was opened, and collagenase (3 mg ml—1) was injected into the distal end of the duct. This was done in a solution containing 5 mM Ca2+. Cervical dislocation caused the rats to die. After being removed, the pancreas was incubated for 17 minutes at 37°C. Hand-collected islets were either divided into single cells in Ca2+-free HRB for insulin release tests or used in insulin release experiments. Eagle's minimal essential medium, which contains 5. mM glucose, 10% Foetal Bovine Serum (FBS), 100 g ml—1 streptomycin, and 100 U ml—1 penicillin, was used to maintain the single cells in short-term culture for up to 3 days after plating them on coverslips. 5% CO2 and 95% air make up the atmosphere. Throughout this period of culture, the cells reacted to the test chemicals in a predictable way. Physiological and morphological parameters were used to select -cells, as previously described [29].
Solutions
NaCl 121.7, HCl 4.4, HH2PO4, CaCl 2, MgSO4, NaHCO3, and 4-(2-hydro- xyethyl) were the main components of HRB (in mM).HEPES, a -1-piperazineethanesulphonic acid with a pH of 7.4, with 0.1% bovine serum albumin. The following ingredients made up the standard pipette solution for whole-cell patch clamp recording of Ca2+ channel current (in mM): aspartate 75, tetraethylammonium (TEA) 30, HEPES 11, EGTA 11, MgCl2 3, CaCl2, ATP-Na2 3, and GTP 0.1 (at pH 7.2) (Boehringer Mannheim, Indianapolis, IN). To create a whole-cell clamp, an external solution containing Tris-HCl 100, TEA-Cl 30, HEPES 10, and CaCl2 (at pH 7.3) was utilized. 2.
Calculations of [Ca2+Ji As previously described [28,30], [Ca2+]i was quantified using dual-wavelength fura-2 microfluorometry in conjunction with imaging. In a nutshell, 1 M fura-2 acetoxymethylester was incubated with cells on coverslips for 30 min at 37°C in HRB containing 2.8 mM glucose. Then, with the cells mounted in a chamber, HRB was superfused at a rate of 1 ml min—1 at 37°C. An Intensified Charge-Coupled Device (ICDD) camera was used to detect emission signals at 510 nm, and an Argus-50 system created ratio images while the cells were activated at 340 and 380 nm in alternate intervals every 2.5 s. Japan's Hamamatsu is home to Hamamatsu Photonics. Calibration curves were used to convert ratio results to [Ca2+]i [30].
Electrical Physiological Signals
Using the conventional whole-cell patch-clamp arrangement, voltage-dependent Ca2+ channel currents in single -cells were captured under superfusion conditions at 1 ml min—1 at 30°C [11]. Pipettes were made of borosilicate glass (Sutter Instruments Co., Novata, CA, USA), fire polished, and at their tips were coated with Sylgard 184 (Dow Corning, Midland, MI, USA). When the usual pipette solution was used to fill them, their resistance was 2 7 MM. An Axopatch-200B amplifier and the program pCLAMP (Axon Instruments, Inc., Foster City, CA, U.S.A.) were used to monitor membrane currents. The potential was maintained at —70 mV and pulsed with depolarizing voltage to 0 mV. Applied at a frequency of 0.2 Hz for a period of 100 ms. The data were digitalized at 10 kHz, filtered at 5 kHz, and saved in a computer (IBM; Tokyo, Japan). The Clampfit tool was used to analyze the data. The reference potential was the pipette's zero-current potential, which was acquired right after the junction potential had been corrected but before the seal had been established.
Measuring Insulin Ejection
The procedures for measuring insulin release were followed exactly [9,28]. In a nutshell, groups of five islets that were extracted from Wistar rats between 8 and 12 weeks of age were first stabilized for 30 min in HRB containing 2.8 mM glucose. Islets were then treated in 1 ml of HRB for 30 minutes at 37°C. Amount of insulin was discovered by the use of an enzyme immunoassay kit from Morinaga in Yokohama, Japan.
Material
Sankyo Co. (Tokyo, Japan) synthesized simvastatin, simvastatin-Na (simvastatin-acid), and pravastatin and graciously contributed them for our study. Pravastatin and simvastatin-acid were dissolved in distilled water, whereas simvastatin was dissolved in 100% ethanol. For the experiments, HRB was treated with tiny aliquots of the stock solutions of HMG-CoA reductase inhibitors. At a final ethanol concentration of less than 0.1%, [Ca2+]i in -cells remained unaffected. Dojin Chemical (Humamoto, Japan) provided the fura-2 and fura-2 acetoxymethylester. Life Technologies Inc. (New York, NY, USA) provided the FBS. We bought mevalonic acid lactone from Nacalai-Tesque Chemical Co. in Tokyo, Japan. Other compounds came from either Nacalai-Tesque or Sigma Chemical Co. (St. Louis, Missouri, United States).
Statistic Evaluation
The mean and s.e. mean were used to express the calculated values (n = number of observations). The Student's t-test was used for the statistical analysis. When P 0.05, differences were deemed statistically significant. Inhibition was therefore visible at the single cell level if the experiments revealed that the response to the initial glucose stimulation obtained in the presence of HMG-CoA reductase inhibitors was consistently lower than the response to the subsequent glucose stimulation obtained after washing out the inhibitors. It was established at the conclusion of the studies that the cells responded to 300 M tolbutamide with significant increases in [Ca2+]i, a feature of healthy -cells [9]. Simvastatin, simvastatin-acid, and pavastatin effects on the glucose-induced first phase [Ca2+Ji induction in single -cells] The peak of the first phase [Ca2+]i increase in response to 8.3 mM glucose was diminished in the presence of 0.3 g ml—1 simvastatin (Figure 1b). Simvastatin at a greater dosage of The first phase [Ca2+]i rise was severely reduced or even completely stopped by 3 g ml—1 (Figure 1c). Simvastatin is removed after washing, and the first phase [Ca2+]i rises in reaction to the second 8.3 mM glucose causes an increase in [Ca2+]i during the first phase. However, simvastatin-acid marginally decreased the first phase [Ca2+]i rise at 30 g ml—1 (Figure 3a) and severely inhibited it at 100 g ml—1 (Figure 3b) in a reversible way. a mean Simvastatin inhibits glucose-induced first phase [Ca2+]i rises in individual -cells. (a) In superfusion conditions, a rise in glucose concentration from 2.8 to 8.3 M induced the first phase [Ca2+]i increase in individual rat pancreatic - cells. Most -cells reacted to two consecutive challenges.
2+ Using 8.3 mM glucose (G8.3)gains in [Ca] with a comparable The restoration of stimulation with 8.3 mM glucose showed that the inhibition was reversible (Figure 1b and c). Simvastatin at concentrations of 0.1–3 g ml–1 also decreased the mean amplitude of the first phase [Ca2+]i increase for the single -cells under study (P 0.05, P 0.02, P 0.001, and P 0.0001 for the three g ml–1 simvastatin concentrations, respectively) (Figure 2). Simvastatin inhibits the first phase [Ca2+]i response to glucose as a result, and this inhibition is concentration-dependent. Simvastatin-acid, which has inhibitory effects at doses of 1 and 10 g ml—1, had no effect on it.
Results
Temporal profile of the [Ca2+Ji-induced incuease in single uat pancueatic -cells due to glucose At a basal glucose content of 2.8 mM, [Ca2+]i in individual -cells varied between 30 and 150 nM (7.8–3.7 nM for 58 cells). As previously reported, an increase in glucose concentration from 2.8 mM to 8.3 or 1.07 mM resulted in a biphasic increase in [Ca2+]i in -cells: a first peak at about 400–500 nM (Figure 1), followed by a moderate elevation at about 100–200 nM that was occasionally superimposed with an oscillation of [Ca2+]i (second phase). Unless otherwise stated, the effects of HMG-CoA reductase inhibitors on the initial [Ca2+]i increase were investigated in the current investigation. Glucose stimulation was performed twice: once with inhibitors present and once without to assess the impact of the inhibitors at the single cell level. In control studies, 8.3 mM glucose was used to stimulate -cells twice. Twenty of the 29 cells responded to the first stimulation by increasing [Ca2+]i, while 24 of the 29 cells responded to the second stimulation. When it came to the amplitude of the first phase [Ca2+]i increase, the response to the first stimulation was either greater than or equivalent to the response to the second stimulation in 22 of these 24 responding cells (92%; Figure 1a).
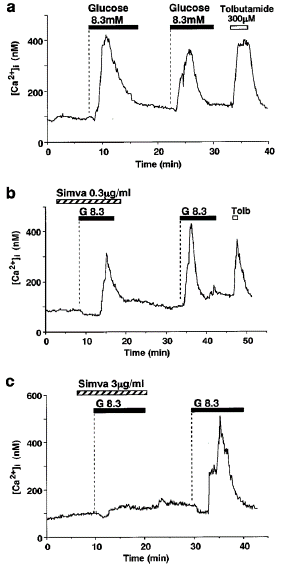
Figure 1: Glucose-induced first phase [Ca2+]i increases and their inhibition by simvastatin in single β-cells. (a) A rise in glucose concentration from 2.8 to 8.3 M, under superfusion conditions, evoked the first phase [Ca2+]i increase in single rat pancreatic β- cells. The majority of β-cells responded to two sequential challenges 2+challenge was either larger than or comparable to that in response to the second challenge. In the presence of simvastatin (Simva) at 0.3 μg ml—1 (b) and 3 μg ml—1 (c), the first phase [Ca2+]i increase was reduced and abolished, respectively. After washing out simvastatin, the first phase [Ca2+]i increase was restored in response to the second challenge with 8.3 mM glucose. Tolbutamide at 300 μM (Tolb) induced rapid increases in [Ca2+]i as seen in (a) and (b). The bars above the tracing indicate the periods of exposure to the agents specified. Dotted lines indicate beginning of exposure. The basal glucose concentration was 2.8 mM throughout measurements when not indicated otherwise. The results shown are representative of 14 cells in (a), six in (b) and ten in (c).
Concentration-response relationship for the inhibition of glucose-induced first phase [Ca2+]i increases by HMG-CoA reductase inhibitors in single β-cells. The mean amplitude of the first phase [Ca2+]i increase in response to 8.3 mM glucose was averaged and expressed as the mean±s.e.mean. The number of single β-cells examined was 127 for the control and 18 - 50 for each experimental condition. The mean amplitude of the first phase [Ca2+]i increase was reduced by simvastatin at 0.1 - 3 μg ml—1 and simvastatin-acid at 30 - 100 μg ml—1. ¶P<0.05 for 0.1 μg ml—1 simvastatin, ¢P<0.02 for 0.3 μg ml—1 simvastatin and 30 μg ml—1 simvastatin-acid,
¢¢P<0.002 for 100 μg ml—1 simvastatin-acid, *P<0.001 for 1 μg ml—1 simvastatin, and **P<0.0001 for 3 μg ml—1 simvastatin vs the control.
Simvastatin-acid doses of 30 and 100 g ml—1 considerably decreased the first phase [Ca2+]i increase's amplitude (P0.01 for 30 g ml—1 and P0.002 for 100 g ml—1) (Figure 2). Simvastatin-acid suppresses the first phase [Ca2+]i response to glucose as a result, but its inhibitory activity is about two orders of magnitude less strong than that of simvastatin (Figure 2).
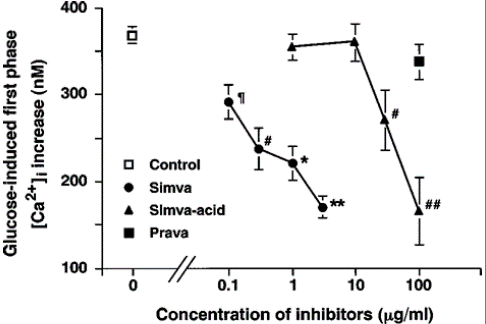
Figure 2:
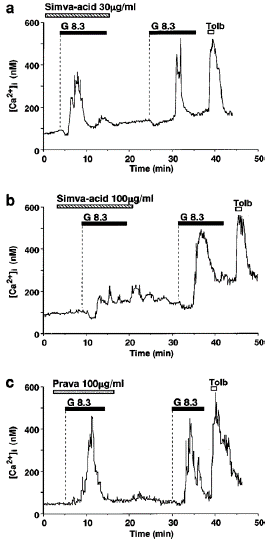
Figure 3: Simvastatin-acid, but not pravastatin, inhibits glucose- induced first phase [Ca2+]i increases in single β-cells. Simvastatin-acid (Simva-acid) at 30 μg ml—1 reduced (a) and at 100 μg ml—1 abolished phase [Ca2+]i increase in response to 8.3 mM glucose (G8.3). After washing out simvastatin-acid, the first phase [Ca2+]i increase was restored in response to the second challenge with 8.3 mM glucose. (c) Pravastatin (Prava) at 100 μg ml—1 had no effects on the first phase [Ca2+]i increase in response to 8.3 mM glucose. The results shown are representative of eight cells in (a), six in (b) and 17 in (c).
The [Ca2+]i response to 8.3 mM glucose was unaffected by the addition of pravastatin to the superfusion solution at concentrations up to 100g ml—1 (Figures 2 and 3c). According to the findings, the hydrophilic HMG-CoA reductase inhibitor had no immediate impact on how the -cells responded to glucose. Simvastatin and puavastatin effects on glucose-induced [Ca2+Ji oscillation in individual -cells
It There is evidence to support the theory that [Ca2+]i oscillations in islet -cells are causally linked to the pulsatile secretion of insulin, which is crucial for the physiological regulation of glucose metabolism [49,50]. So, it was investigated how HMG-CoA reductase inhibitors affected [Ca2+]i oscillations. Simvastatin partially and almost completely suppressed the [Ca2+]i oscillations brought on by 8.3 M glucose at concentrations of 0.3 and 3 mg/ml, respectively (Figure 4a). The oscillations were either totally or partially reversible after washing away the inhibitor. Simvastatin partially suppressed the [Ca2+]i oscillations at doses of 0.1 and 1 mg ml—1 as well (results not shown). Pravastatin, however, comes in a range of concentrations. Up to 100 g ml—1 had no discernible impact (Figure 4b). Only two of the 14 cells that displayed [Ca2+]i oscillations (14% continued to oscillate clearly throughout treatment with 1 g ml—1 simvastatin for approximately 15 min), while 13 cells (93%) remained to oscillate after the medication was removed, demonstrating a potent and reversible inhibition (Figure).
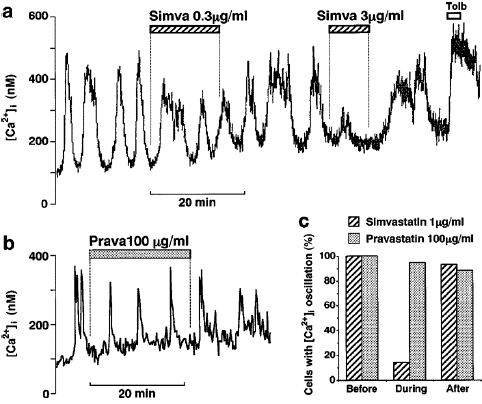
Figure 4: Simvastatin, but not pravastatin, inhibits glucose-induced [Ca2+]i oscillations in single β-cells. (a) Simvastatin (Simva) at 0.3 μg ml—1 partially and at 3 μg ml—1 almost completely inhibited [Ca2+]i oscillations induced by 8.3 mM glucose in a reversible manner. (b) Pravastatin (Prava) at 100 μg ml—1 had no effects on [Ca2+]i oscillations. The results shown are representative of five cells in (a) and 15 in (b). (c) Effects of simvastatin and pravastatin on the incidence of [Ca2+]i oscillations.
Among the 14 cells exhibiting [Ca2+]i oscillations in response to 8.3 mM glucose, two cells oscillated during treatment with 1 μg ml—1 simvastatin for about 15 min, and 13 cells oscillated after washing out this drug. In contrast, among the 18 oscillating cells, 17 and 15 cells oscillated during treatment with and after washing out 100 μg ml—1 pravastatin, respectively. 4c). In contrast, among 18 cells that exhibited [Ca2+]i oscillations, 17 (94%) and 15 cells (88%) exhibited oscillations during treatment with and after washing out 100 μg ml—1 pravastatin, respectively, in a manner similar to that before the drug treatment.
Effects of simvastatin and pavastatin on glucose-induced insulin secretion from islets Insulin release from rat islets, under static incubation conditions, was stimulated with 8.3 mM glucose. The Simvastatin, 0.3 g ml—1, significantly inhibited stimulated insulin release (P 0.05) (Figure 5). Simvastatin-acid minimally inhibited the release of insulin at 30 g ml—1, the concentration at which it only slightly affected the statistically insignificant first phase [Ca2+]i response to glucose. Pravastatin, however, did not have any effect on the release of insulin at 100 mg/ml. Simvastatin and pavastatin's effects on L-type Ca2+ channels in individual -cells It has been demonstrated that the Ca2+ influx through the L-type Ca2+ channels in the -cell plasma membrane is primarily, if not entirely, responsible for the glucose-induced increase in [Ca2+]i in -cells [4,13]. Consequently, we looked at how HMG-CoA reductase inhibitors affected the Ca2+ currents of individual pancreatic -cells using a whole-cell voltage-clamp setup. A depolarizing pulse from a holding potential of —70 to 0 mV in the control external solution containing 2.8 mM glucose evoked a long-lasting inward current with an amplitude of about —70 pA (Figure Aa, B, and C), whose characteristics are similar to those of the current flowing through L-type Ca2+ channels in -cells [4]. The current fell quickly and noticeably when exposed to 3 g ml-1 simvastatin (Figures Ab and B), and it returned to normal after rinsing the simvastatin out.
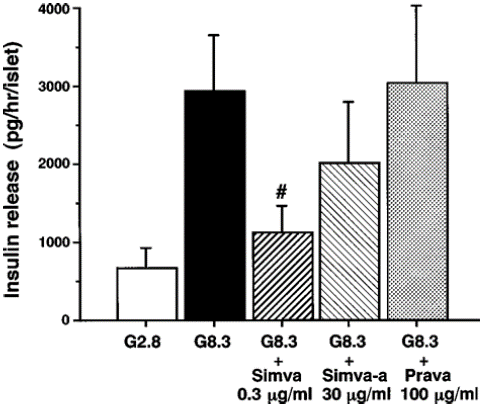
Figure 5: Simvastatin and simvastatin-acid, but not pravastatin, inhibit glucose-induced insulin secretion in islets. Insulin release from islets stimulated with 8.3 mM glucose, under static incubation conditions, was inhibited in the presence of 0.3 μg ml—1 simvastatin (Simva). Glucose-stimulated insulin release was mildly reduced by 30 μg ml—1 simvastatin-acid (Simva-a), but not significantly. Pravas- tatin (Prava) at 100 μg ml—1 was without effect on glucose-stimulated insulin release. The results are expressed as the mean±s.e.mean of six experiments. ¢, Significant difference (P<0.05) vs the 8.3 mM glucose (G8.3) group and the pravastatin group.
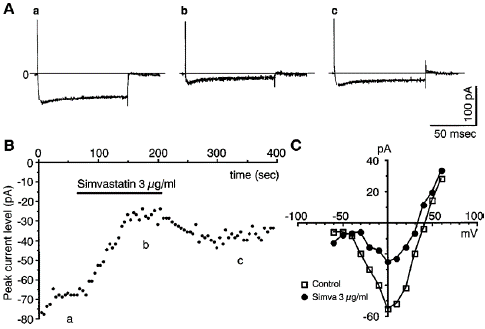
Figure 6: Simvastatin inhibits Ca2+ currents in single β-cells. (A) Whole-cell Ca2+ currents in a single β-cell depolarized to 0 mV from the holding potential of —70 mV before (a), during (b) and after exposure to 3 μg ml—1 simvastatin (c) under superfusion conditions. (B) Recording of the temporal change of the whole-cell Ca2+ currents. a, b and c, specify the time points at which the current traces in Aa, Ab and Ac were taken. (C) The current-voltage relationship of the peak Ca2+ current amplitude in the control and in the presence of 3 μg ml—1 simvastatin. The results shown are representative of five cells in (A) and (B) and three in (C).
Restored just partially (Figure Ac and B). Figure C displays the current-voltage correlations of -cells before and after exposure to 3 g ml—1 simvastatin. Simvastatin decreased the Ca2+ current amplitude without changing the voltage-current relationship. Pravastatin, however, had no impact on the Ca2+ current at 100 g ml—1 (results not shown). Simvastatin inhibits auginine- and KCl-induced [Ca2+Ji incueases in single cells. According to Ashcroft and Rorsman (1989), the main mechanism for the glucose-, L-arginine-, and HCl-induced releases of insulin is the Ca2+ influx through the L-type Ca2+ channels. When carried across the -cell plasma membrane, the cationic amino acid arginine immediately depolarizes the membrane at relatively high quantities (1 to 20 mM). It activates L-type Ca2+ channels in a voltage-dependent manner, increasing [Ca2+]i [6,14,23,28]. Through a direct depolarization, HCl also causes L-type Ca2+ channel activation and a long-lasting rise in [Ca2+]i (Yaekura et al., 1999). Simvastatin's ability to block L-type Ca2+ channels led researchers to investigate if it may also block [Ca2+]i increases brought on by arginine and HCl. Simvastatin significantly decreased the [Ca2+]i response to arginine in a reversible manner when given in combination with sequential administration of 10 mM arginine in short pulses (Figure 7a). 25 mM HCl and a sustained rise in [Ca2+]i were generated. Simvastatin significantly decreased it (Figure 7b). About 20 seconds after the medication was administered, the inhibition began.
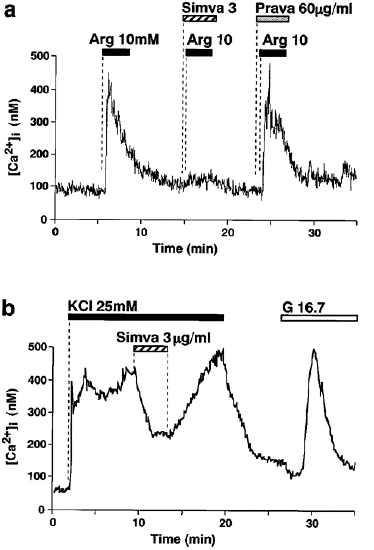
Figure 7: Simvastatin (Simva) inhibits [Ca2+]i increases in response to L-arginine (Arg) and HCl in single β-cells. (a) An increase in [Ca2+]i induced by 10 mM L-arginine was inhibited in the presence of 3 μg ml—1 simvastatin, but not б0 μg ml—1 pravastatin (Prava). (b) A sustained increase in [Ca2+]i induced by 25 mM HCl was almost instantaneously inhibited by the addition of 3 μg ml—1 simvastatin, and it was restored upon washing out the drug. The glucose concentration was 8.3 mM in (a) and 2.8 mM in (b). G1б.7: change to 1б.7 mM glucose. The results shown are representative of five cells in (a) and 14 in (b).
Discussion
The novel results of our study were as follows: (1) Among the HMG-CoA reductase inhibitors, simvastatin was approximately two orders of magnitude more potent than simvastatin-acid in inhibiting glucose-induced [Ca2+]i signalling in rat islet -cells, whereas pravastatin was ineffective; (2) Simvastatin inhibited glucose-induced insulin secretion from islets more potently than Simvastatin and simvastatin-acid were the only HMG-CoA reductase inhibitors that reduced the glucose-induced first phase [Ca2+]i rises and [Ca2+]i oscillations, whereas pravastastin had no effect on any of these variables. The [Ca2+]i's [Ca2+ Inhibition] Potency Rank Order Simvastatin, Simvastatin Acid, and Pravastatin increased in the same order as the suppression of insulin secretion. The [Ca2+]i rise and insulin secretion were both partially inhibited by simvastatin at 0.3 g ml—1, although the magnitude of the inhibition was slightly greater for insulin secretion. This may be explained by the longer simvastatin treatment duration for insulin secretion (30 min) than for [Ca2+]i (10–15 min). The primary signal that initiates insulin secretion is a rise in [Ca2+]i (Wollheim & Sharp, 1981; Gilon et al., 1993; Ammala et al., 1993; Yada et al., 1994; Henquin, 1994). All of these findings point to the inhibition of the [Ca2+]i rise as the cause of the inhibition of insulin production. Simvastatin blocks L-type Ca2+ channels in -cells, as was amply shown by the whole-cell patch-clamp investigation. This idea was expanded upon backed up by the discovery that Simvastati.
arginine and HCl, the insulin secretagogues that activate L-type Ca2+ channels and therefore increase [Ca2+]i, were blocked in their ability to elevate [Ca2+]i [6,14,23,28] (Yaekura et al., 1999). Simvastatin inhibits Ca2+ currents with temporal characteristics that are comparable to those of inhibiting [Ca2+]i rises (Figure B vs. Figure 7b). Simvastatin also causes Ca2+ currents to rebound after drug washout. Simvastatin blocked both [Ca2+]i increases and L-type Ca2+ channels, whereas pravastatin had no impact on either; hence, the two activities changed simultaneously. According to Henquin (1994) and Ashcroft & Rorsman (1989), the main mechanism by which glucose-induced [Ca2+]i increases in -cells occur is Ca2+ inflow through L-type Ca2+ channels. Therefore, our findings show that The blocking of L-type Ca2+ channels is the main, if not the only, component preventing [Ca2+]i increases. It's also possible that the inhibitory activity of HMG-CoA reductase inhibitors results from the decreased amount of mevalonate that results from the inhibition of HMG-CoA reductase, which catalyzes the formation of mevalonate from HMG-CoA [1]. However, 100 M mevalonic acid lactone was present both during the experimental (30 min) and preincubation periods. Simvastatin decreased the first [Ca2+]i response to glucose in a way that was comparable to the studies used as a control that lacked mevalonate (data not shown). The finding that simvastatin administration resulted in the inhibition of Ca2+ currents and [Ca2+]i increases starting as soon as 10 to 20 seconds later suggests that the metabolic change that lowers mevalonate levels is not the mechanism underlying the inhibition of L-type Ca2+ channels and [Ca2+]i increases, but rather a more direct interaction between the drug and the plasma membrane L-type Ca2+ channels.
Simvastatin inhibited the glucose-induced first phase [Ca2+]i rise and [Ca2+]i oscillation, in a fully or partially reversible manner, at concentrations ranging from 0.1 to 3 g ml—1. In this concentration range, the less lipophilic simvastatin-acid had no impact, but at the The first phase [Ca2+]i rises were suppressed at higher dosages of 30 and 100 g ml—1. Simvastatin-Ac had a potency that was roughly two orders of magnitude lower than that of simvastatin. At concentrations up to 100 M, the hydrophilic pravastatin had no effect on either the glucose-induced [Ca2+]i oscillation or the first phase [Ca2+]i rise. Simvastatin has been shown to be significantly more potent than pravastatin in other studies, including those that found that it worsened segment shortening in dogs' reperfused myocardium [34] and prevented the proliferation of human smooth muscle cells [44]. The inhibitory potencies of the HMG-CoA reductase inhibitors seemed to correlate with their lipophilicity in both our investigation and these publications. A demonstration of the partition coeAcient between water and n-octanol, a Simvastatin has a lipophilicity of 25118, simvastatin-acid has a lipophilicity of 75.8 and pravastatin has a lipophilicity of 0.34 [20]. These results in a relative lipophilic ratio of roughly 70000: 2000: 1. This proportion is consistent with the HMG-CoA reductase inhibitor's relative potency for inhibiting [Ca2+]i rises and insulin secretion seen in the current investigation. Simvastatin is highly lipophilic, so it is likely that it has a strong affinity for cell membranes and, as a result, may also have an easy time entering the intracellular space. It is also likely that these properties are connected to simvastatin's capacity to effectively inhibit Ca2+ channels in the plasma membrane of beta-cells, thereby preventing [Ca2+]i and insulin responses to glucose. Contrarily, hydrophilic pravastatin only accesses the body at a slow rate. This is probably why the medication has no immediate impact on Ca2+ channels, [Ca2+]i increases, or insulin secretion. plasma membrane and the intracellular space. The amplitude of the first phase [Ca2+]i response to 8.3 mM glucose was mildly attenuated in -cells that had been cultured for 1 day with a high concentration of pravastatin (100 g ml—1) in comparison to that in the paired -cells cultured under control conditions (T. Yada, unpublished data), supporting this theory.
Simvastatin has been shown to have a serum concentration of roughly 0.01 g ml—1 of simvastatin and its active metabolites in healthy volunteers after oral dosing [36]. The concentration at which simvastatin was found in our data was showed a quick and considerable suppression of the [Ca2+]i rise brought on by glucose, which was one order of magnitude larger at 0.1 g ml—1. Simvastatin may induce the inhibitory effect at lower concentrations when used chronically because HMG-CoA reductase inhibitors are frequently used for a lengthy period of several years or more [7,10,18,19]. Diabetic patients frequently develop hypercholesteremia. Type 2 diabetes has been linked to functional changes in -cells [17,49], It is possible that some type 2 diabetes patients have -cells that are more susceptible to lipophilic HMG-CoA reductase inhibitor inhibition. Simvastatin may further attenuate -cell activity in type 2 diabetes patients with impaired insulin secretory capacity [16,51] (Hosaka et al., 1977). This may have a pathophysiologically substantial impact on glucose metabolism. It is also possible that people with lower rates of drug metabolism and/or extrusion due to more or less compromised liver and/or kidney functions, as is the situation in some type 2 diabetes patients, have serum simvastatin levels higher than 0.01 g ml—1. According to a recent study [46], Simvastatin and simvastatin-acid serum concentrations increased one order of magnitude higher and exceeded 0.1 g ml—1, the level at which the suppression of - cells was detected in the present investigation, when simvastatin was coupled with the CYP3A4 inhibitor itraconazole. Additionally, it has been noted that in healthy persons, blood concentrations of fluvastatin, an HMG-CoA reductase inhibitor with a lipophilicity similar to that of simvastatin-acid, can reach levels as high as 0.25 g ml—1 [3].
It is crucial from a clinical standpoint to understand how HMG-CoA reductase inhibitors affect blood glucose levels and glucose metabolism. poor insulin production and/or action (insulin sensitivity) are thought to be the two main causes of type 2 diabetes and poor glucose tolerance. Regarding the effects of HMG-CoA reductase inhibitors on insulin action, it has been shown that lovastatin, a lipophilic HMG-CoA reductase inhibitor, disrupts the early events of insulin signalling, which include tyrosine phosphorylation of the insulin receptor β subunit and MAP kinase, association of the p85 subunit of PI-3 kinase with insulin receptor substrate- 1, and activation of MAP kinase [27,40]. Simvastatin [47,48] and pravastatin [22] have been shown to significantly cut LDL cholesterol, however they do not improve or even slightly aggravate insulin resistance in patients with hypercholesterolaemia.
Regarding the effects on blood glucose, it has been demonstrated that plasma glucose concentrations were moderately but significantly increased after pravastatin therapy from 8:00 a.m. to 1:00 p.m. in response to breakfast and lunch [22]. Simvastatin treatment significantly increased plasma glucose concentrations both at fasting and during an Intravenous Glucose Tolerance Test (IVGTT), according to a study in people with type 2 diabetes and hyperlipidemia. This increase was accompanied by an increase in fasting insulin concentrations but not insulin responses to the IVGTT [48]. This finding would suggest that the plasma insulin concentration rises to make up for the decreased insulin sensitivity, but not enough to keep blood sugar levels low, leading to hyperglycemia [48]. Despite the small number of publications, these in vitro and in vivo investigations show that the use of HMG-CoA reductase inhibitors reduces insulin sensitivity. The current work also demonstrated a unique simvastatin effect that directly inhibits the insulin secretory response to glucose in -cells. Therefore, it would seem that lipophilic HMG-CoA reductase inhibitors have the potential to reduce secretion, may potentially impact insulin sensitivity, and, as a result, may hasten the pathophysiology and development of type 2 diabetes. As a result of blocking L-type Ca2+ channels and [Ca2+]i signaling in pancreatic -cells, simvastatin, a lipophilic HMG-CoA reductase inhibitor, is able to block glucose-induced insulin production. When using HMG-CoA reductase inhibitors, this conclusion should be considered with caution. Specifically in type 2 diabetic patients, in the therapeutic setting. Since insulin production is regulated by L-type Ca2+ channels and [Ca2+]i signaling, it is important to look into any potential effects of HMG-CoA reductase inhibitors on -cell activities other than secretion.
References
- Alberts AW. Discovery, biochemistry and biology of lovastatin. Am J Cardiol. 1988; 62: 10J-5J.
- Ammälä C, Eliasson L, Bokvist H, Larsson O, Ashcroft FM, Rorsman P. Exocytosis elicited by action potentials and voltage-clamp calcium currents in indivi- dual mouse pancreatic B-cells. J Physiol. 1993; 472: 665-88.
- Appel S, Rüfenacht T, Kalafsky G, Tetzloff W, Kallay Z, Hitzenberger G, et al. Lack of interaction between fluvastatin and oral hypoglycemic agents in healthy subjects and in patients with non-insulin-dependent diabetes mellitus. Am J Cardiol. 1995; 76: 29A-32A.
- ashcroft FM, Rorsman P. Electrophysiology of the pancreatic β-cell. Puog. Biophys. Prog Biophys Mol Biol. 1989; 54: 87-143.
- bergsten P. Slow and fast oscillations of cytoplasmic Ca2+ in pancreatic islets correspond to pulsatile insulin release. Am J Physiol. 1995; 268: E282-7.
- blachier F, Mourtada A, Sener A, Malaisse WJ. Stimulus-secretion coupling of arginine-induced insulin release. Uptake of metabolized and nonmetabolized cationic amino acids by pancreatic islets. Endocrinology. 1989; 124: 134-41.
- byington RP, Jukema JW, Salonen JT, Pitt B, Bruschke AV, Hoen H, et al. Reduction in cardiovascular events during pravastatin therapy. Pooled analysis of clinical events of the Pravastatin Atherosclerosis Intervention Program. Circulation. 1995; 92: 2419-25.
- Dolmetsch Re, XU H, Lewis RS. Calcium oscillations increase the eAciency and specificity of gene expression. Natuue. 1998; 392: 933-6.
- Fujitani S, Ohazahi H, Yada T. The ability of a new hypoglemic agent, A-416, compared to sulphonylureas, to increase cytosolic Ca2+ in pancreatic β-cells under metabolic inhibition. Bu J Phaumacol. 1997; 120: 1191-8.
- Gilon P, Shepherd RM, Henquin JC. Oscillations of secretion driven by oscillations of cytoplasmic Ca2+ as evidenced in single pancreatic islets. J Biol Chem. 1993; 268: 22265-22268.
- Hamill OP, Martya A, Neher E, Sakmann B, Sigworth FJ. Improved patch-clamp techniques for high-resolution current recording from cells and cell-free membrane patches. Pflugers Arch. 1981; 391: 85-100.
- Hellman B, Gylfe E, Grapengiesser E, Lund PE, Berts A. Cytoplasmic Ca2+oscillations in pancreatic β- cells. Biochim Biophys Acta. 1992; 1113: 295-305.
- Henquin JC. Cell biology of insulin secretion. In: Hahn CR, Weir GC, editors Philadelphia: Lea & Febigar,. Joslin’s diabetes mellitus. 1994; 56-80.
- henquin JC, Meissner HP. Effects of amino acids on membrane potential and 8бRb+ fluxes in pancreatic β-cells. Am J Physiol. 1981; 240: E245-52.
- Hoeg JM. The HMG CoA Reductase Inhibitors. Cuuu Opin Lipidol. 1990; 1: 29-33.
- Pfeifer MA, Halter JB, Porte D. Insulin secretion in diabetes mellitus. Am J Med. 1981; 70: 579-88.
- Porte D, Kahn SE. The key role of islet dysfunction in type II diabetes mellitus. Clin Invest Med. 1995; 18: 247-54.
- Sacks FM, Pfeffer MA, Moye LA, Rouleau JL, Rutherford JD, Cole TG, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators. N Engl J Med. 1996; 335: 1001-9.
- Scandinavian Simvastatin Survival Study Group. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian simvastatin Survival Study (4S). Lancet. 1994; 344: 1383-9.
- Serajuddin ATM, Ranadive SA, Mahoney EM. Relative lipophilicities, solubilities, and structure-pharmacolo- gical considerations of 3-hydroxy-3-methylglutaryl-coenzyme A (HMG-CoA) reductase inhibitors pravastatin, lovastatin, me- vastatin, and simvastatin. J Phaum Sci. 1991; 80: 830-4.
- Shepeherd J, Cobbe SM, Ford I, Isles CG, Lorimer AR, Macfarlanw PW, et al. Prevention of coronary heart disease with pravastatin in men with hypercholesterolemia. West of Scotland Coronary Prevention Study Group. N Engl J Med. 1995; 333: 1301-7.
- Prevention of coronary heart disease with pravastatin in men with hypercholesterolemia. N Engl J Med. 333: 1301-1307.
- Sheu WH, Shieh SM, Shen DD, Fuh MM, Jeng CY, Chen YD, et al. Effect of pravastatin treatment on glucose, insulin, and lipoprotein metabolism in patients with hypercholesterolemia. Am. Heaut J. 1994; 127: 331-336.
- Smith PA, Sahura H, Coles B, Gummerson N, Prohs P, Ashcroft FM. Electrogenic arginine transport med- iates stimulus-secretion coupling in mouse pancreatic β-cells. J Physiol. 1997; 499: 625-635.
- Tobert JA. Efficacy and long-term adverse effect pattern of lovastatin. Am J Cardiol. 1988; 62: 28J-34J.
- Tobert JA. HMG-CoA Reductase Inhibitors, gemfibrozil, and myopathy. Am J Caudiol. 1995; 75: 862.
- Wollheim CB, Sharp GWG. Regulation of insulin release by calcium. Physiol Rev. 1981; 61: 914-73.
- Xu XQ, Mcguire TF, Blashovich MA, Sebti SM, Romero G. B fibroblasts. Auch. Biochem. Biophys. Lovastatin Inhibits Stimul Mitogen-Activated Protein Kinase Insulin HiRC. 1996; 326: 233-7.
- Yada T. Action mechanisms of amino acids in pancreatic B-cells. In: Reseauch, Flatt PR, Lenzen S, editors. Insulin Secuetion and Pancueatic B-cell. London: Smith-Gordon and Company Limited. 1994; 129-35.
- Yada T, Hamahawa N,Yaehura H. Two distinct modes of Ca2+ signalling by ACh in rat pancreatic β-cells: concentration, glucose dependence and Ca2+ origin. J Physiol. 1995; 488: 13-24.
- Yada T, Kakei M, Tanaka H. Single pancreatic β-cells from normal rats exhibit an initial decrease and subsequent increase in cytosolic free Ca2+ in response to glucose. Cell Calcium. 1992; 13: 69-76.
- Yada T, Sakurada M, Ihida K, Nakata M, Murata F, Arimura, A et al. Pituitary adenylate cyclase activating polypeptide is an extraordinarily potent intra-pancreatic regulator of insulin secretion from islet β-cells. J Biol Chem. 1994; 269: 1290-3.
- Yada T, Sahurada M, Ishihara H, Nahata M, Shioda S, et al. Pituitary adenylate cyclase-activating polypeptide (PACAP) is an islet substance serving as an intra-islet amplifier of glucose-induced insulin secretion in rats. J Physiol. 1997; 505: 319-328.
- Yauhera H, Hahei M, Yada T. cAMP-signaling pathway acts in selective synergism with glucose or tolbutamide to increase cytosolic Ca2+ in rat pancreatic β-cells. Diabetes. 1996; 45: 295-301.
- Hurminghahe DB. HMG CoA reductase inhibitors. Cuuu Opin Lipidol. 1992; 3: 22-8.
- Ichihara H, Satoh H, Abiho Y. Influences of pravastatin and simvastatin, HMG-CoA Reductase Inhibitors, on myocardial stunning in dogs. J Caudiovasc Phaumacol. 1993; 22: 852-6.
- Kennedy ED, Rizzuto R, Theler JM, Pralong WF, Bastianutto C, Pozzan T, et al. Glucose-stimulated insulin secretion correlates with changes in mitochondrial and cytosolic Ca2+ in aequorin-expression INS-1 cells. J Clin Invest. 1996; 98: 2524-38.
- Glucose-stimulated insulin secretion correlates with changes in mitochondrial and cytosolic Ca2+ in aequorin-expressin INS-1 cells. J. Clin. Invest. 98: 2524-2538.
- Hoga T, Hawabata H, Arai H, Matusushima N, Hoihe H, Homai T, et al. Comparative pharmacokinetics and pharmacodynamics of pravastatin and simvastatin. Bull. Mol Biol Med. 1995; 20: 103-5.
- Hosaha H, Hagura R, Huzuya T. Insulin responses in equivocal and definite diabetes, with special reference to subjects who had mild glucose intolerance but later developed definite diabetes. Diabetes. 1997; 26: 944-52.
- Li W, Llopos J, Whitney M, Zloharnih G, Tsie RY. Cell-permeant caged InsP3 ester shows that Ca2+ spike frequency can optimize gene expression. Natuue. 1998; 392: 936-41.
- Matthews DR, Naylor BA, Jones RG, Ward GM, Turner RC. Pulsatile insulin has greater hypoglycemic effect than continuous delivery. Diabetes. 1983; 32: 617-21.
- Mcguire TF, Xu XQ, Corey SJ, Romero GG, Sebti SM. Lovastatin disrupts early events in insulin signaling: a potential mechanism of lovastatin’s anti-mitogenic activity. Biochem Biophys Res Commun. 1994; 204: 399-406.
- Nahahara H, Huriyama M, Yoshidome H, Nagata H, Nagado T, Nahagawa M, et al. Experimental simvastatin-induced myopathy in rabbits. Neuuol J Sci. 1992; 113: 114-7.
- NAHAHARA, YADA H, T, HURIYAMA M, OSAME M. Cytosolic Ca2+ increase and cell damage in Lб rat myoblasts by HMG-CoA Reductase Inhibitors. Biochem Biophys Res Mun. 1994; 202: 1579-85.
- Cytosolic Ca2+ increase and cell damage in Lб rat myoblasts by HMG-CoA reductase inhibitors. Biochem. Biophys. Res. Com- mun. 202: 1579-1585.
- Nahazahi M, Ishihara H, Hahei M, Inuhai H, Asano T, et al. Repetitive mitochondrial Ca2+ signals synchronize with cytosolic Ca2+ oscillations in the pancreatic beta-cell line, MINб. Diabetologia. 1998; 41: 28б:279.
- Negre-Arninou P, Van-Vliet Ah, Van-Eric M, Van- Thiel GC, Van-Leeuwen RE, Cohen LH. 1997.
- Inhibition of proliferation of human smooth muscle cells by various HMG-CoA Reductase Inhibitors; comparison with other human cell types. Biochim Biophys Acta. 1345: 259-2б8.
- Neuvonen PJ, Hantola T, Hivisto HT. Simvastatin but not pravastatin is very susceptible to interaction with the CYP3A4 inhibitor itraconazole. Clin Phaumacol Theu. 1998; 63: 332-41.
- Nielsen S, Schmitz O, Moller N, Porhsen N, Hlausen IC, Alberti HG et al. Renal function and insulin sensitivity during simvastatin treatment in type 2 (non-insulin-dependent) diabetic patients with microalbuminur- ia. Diabetologia. 1993; 1079: 1086.
- Ohrvall ML, Lithell H, Johansson J, Vessby B. 1995.
- Ohrvall Ml, Lithell H, Johansson J, Vessby B. A comparison between the effects of gemfibrozil and simvastatin on insulin sensitivity in patients with non-insulin-dependent diabetes mellitus and hyperlipoproteinemia. Metabolism. 1995; 44: 212-7.
- O’Meara NM, Polonshy HS. Insulin secretion in vivo. In: Hahn CR, Weir GC, editors Philadelphia: Lea & Febigar,. Joslin’s diabetes mellitus. 1994; 96: 81.
- O’Rahilly S, Turner RC, Matthews DR. Impaired pulsatile secretion of insulin in relatives of patients with non-insulin-dependent diabetes. N Engl J Med. 1988; 318: 1225-30.
- Pulsatile secretion of insulin in relatives of patients with non- insulin-dependent diabetes. N Engl J Med. 318: 1225-1230.
- Perley MJ, Kipnis DM. Plasma insulin responses to oral and intravenous glucose: studies in normal and diabetic subjects. J Clin Invest. 1967; 46: 1954-62.
