
Research Article
Austin J Public Health Epidemiol. 2021; 8(3): 1104.
Household Air Pollution Risk on Respiratory Health among Women: A Case Study of Indian District after Clean Fuel Programme
Bhole V*
Department of Public Health and Epidemiology, National Institute of Health and Family Welfare, India
*Corresponding author: Vaishali Bhole, Department of Public Health and Epidemiology, National Institute of Health and Family Welfare, New Delhi, India
Received: May 28, 2021; Accepted: June 23, 2021; Published: June 30, 2021
Abstract
Objectives: Some of the highest exposures to air pollutants in developing countries occur inside homes where biomass fuels are used for daily cooking. Inhalation of these pollutants may cause deleterious effects on health. Study Design: A total of 450 non-smoking, non-pregnant women aged 15 years and above exposed to domestic smoke from cooking fuels from an early age, working in poorly ventilated kitchen were selected and on investigation presented various health problems.
Method: Symptoms were enquired by means of using standard questionnaire adopted from that of the American Thoracic Society (ATS, 1995). Lung function was assessed by the measurement of Forced Vital Capacity (FVC), (FEV1), i.e. volume of air (in liter) that is forcefully exhaled in one second. Using ratio of FEV1 to FVC (FEVI/FVC), expressed as percentage.
Results: FVC less than 80% of the predicted was considered as abnormal pulmonary function. Symptoms like chest pain, breathlessness, eye irritation, and blackout were found to be significantly higher in biomass users (P <0.05). Moreover, an increasing trend in the prevalence of symptoms/morbid conditions was observed with increase in exposure. Conclusion Thus women exposed to biomass fuels smoke suffer more from health problems and are at greater risk of respiratory illnesses when compared with other fuel users.
Keywords: Biomass fuel; Household air pollution; Health effects; Chronic bronchitis; Lung function; Environmental risk
Introduction
HAP is recognized as a significant source of potential health risk to exposed populations throughout the world. The major sources of HAP worldwide include combustion of fuels, tobacco smoke, ventilation systems, furnishings and construction materials. These sources vary considerably among developing, and developed nations. Environmental Tobacco Smoke, volatile organic compounds from furnishings and radon from soil are major sources of importance in developed countries [1]. Household Air Pollution (HAP) is caused mainly by the residential burning of solid fuels for cooking and to some extent heating, the major types of which are wood, dung, agricultural residues, coal, and charcoal [2-4]. According to the Global Burden of Disease Report, IAP is the leading cause of Disability Adjusted Life Years (DALYs) in Southeast Asia and the third leading cause of DALYs worldwide [5]. It is considered a silent killer that has resulted in 4.3 million deaths worldwide accounting for 7.7% of the global mortality. The adoption of clean stoves by the 3 billion people using traditional fuels is necessary to achieve health, climate, and gender equality goals [6]. The South-East Asian region contributes to the maximum mortality due to household air pollution followed by the Western Pacific region [7]. A developing country like India faces the dual challenge of exposures from both ambient and household air pollution [5]. The most important issue that concerns indoor air quality in household environments of developing countries like India is the exposure to pollutants released during the combustion of solid fuels. Existing evidence suggests that India, with a population of 1.38 billion people living across states at different levels of economic, social, and health development, has one of the highest air pollution levels in the world [8].
In India, approximately 86.7% of rural households and 26.3% of urban households rely on solid biomass fuels for their cooking needs [9]. These practices can adversely affect the respiratory health of individuals and local forests and other environmental resources, as well as contribute to climate change. When used in simple cooking stoves (mostly traditional Indian Chulah), these fuels emit substantial amount of toxic pollutants that include respirable particles, carbon monoxide, oxides of nitrogen , sulfur, benzene, formaldehyde, 1,3-butadiene, and polyaromatic compounds, such as benzo (a) pyrene [10-16]. In households with limited ventilation as is common in rural household of developing countries, exposures experienced by household members, particularly women and young children who spend a large proportion of their time indoors, have been measured to be many times higher than World Health Organization (WHO) guidelines [17]. Millions of people die every year from exposure to fine particles in polluted air that penetrate deep into the lungs and cardiovascular system, causing diseases including stroke, heart disease, lung cancer, Chronic Obstructive Pulmonary Diseases (COPD) and respiratory infections, including pneumonia. Fine particles less than 2.5 micrometers in diameter (PM2.5) pose the greatest health risks because of their small size, as they can lodge deeply into the lungs. Also, the evidence is now emerging of links with a number of other conditions, including low birth weight, asthma, tuberculosis, cataracts and cancer of the upper airways 18. Household Air Pollution (HAP) arising from the combustion of solid fuels for cooking is a major contributor to four of the top five causes of mortality and morbidity in India, and HAP is a significant contributor to outdoor air pollution [19-21]. Clean cooking fuels are a highly cost-effective health intervention and household’s energybehavior indicates the economic development of a country [21].
In “Pradhan Mantri Ujjwala Yojana” (PMUY), the government provided gas connections to a total of 50 million poor households (from 2016 to 2018) [22]. Piped Natural Gas (PNG) connections have reached more than 11% of households annually with a goal of 20 million by early next decade helping to move LPG to rural areas.
Despite being an industrialized state, over 78% of rural households in Maharashtra state in India use firewood as principle cooking fuel [23]. Yet there is limited data available on health effects involved in the biomass and clean fuels in view of availability of clean fuel the rural areas.
Methods
The study was carried out in the rural area of Nagpur district in the state of Maharashtra, India during the span of the year 2017-18. The study was cross sectional and used multistage random sampling technique. The randomization was done at three levels that are district, tehsil (block) and village to identify the study area (Figure 1). District Nagpur has fourteen blocks, out of which Katol was selected randomly for the study, which has 82.38% biomass fuel use according to Census 2011. Katol block has over 165 villages out of which twenty villages were then selected from the block based on their distance from the block headquarter and their proximity from national highway to reduce the confounding factor of vehicular pollution. Seven villages were with-in 10km, 8 were in 10-20 km radius and 5 were more than 20km. All procedures were in accordance with the ethical standards of the Institutional Review Board and with the Helsinki declaration of 1975 that was revised in 2000. Ethical clearance was taken from the Institutional Ethics Committee of Rashtrasant Tukdoji Maharaj Nagpur University India. Informed consent was obtained from all subjects of the study. Respiratory symptoms in detail were enquired by means of a standard questionnaire adopted from the American thoracic society [24], and chronic bronchitis was diagnosed from the presence of cough with expectoration for 3 months in a year for at least two consecutive years on the recommended criteria of ATS. The survey was conducted at two levels, viz., individual and household. The study population was rural women who cook using the different types of fuel. Women aged 15 years and above involved in cooking who were non-smokers, non-pregnant were included in the study. For sample calculation, prevalence of three major diseases like Chronic Obstructive Pulmonary Disease (COPD), lower respiratory infection and low back pain was taken into consideration. Four hundred and fifty (450) households having at least one women cook were selected for collecting primary data on several household parameters like socioeconomic, demographic, and housing characteristics. Information about the prevalence of respiratory symptoms experienced in the past 1 year lasting for 3 months or more, frequency of the signs and symptoms, were collected. Respiratory symptoms broadly included dry cough, cough with phlegm, wheezing and chest discomfort, chest pain and nasal obstruction [25]. In addition, prevalence of headache, eye irritation, nausea, dizziness, shortness of breath etc. were also evaluated. Lung function was measured on completion of interviews. Lung function tests by spirometry were performed with informed consent of the participant. The tests were performed according to the methods suggested by the American Thoracic Society using a portable, electronic spirometer (Schillar Ltd, UK). Calibration checks were undertaken weekly. Before performing the pulmonary function test, each woman was subjected to a detailed history including the history of smoking, location of the kitchen, adequacy of ventilation, type of cooking fuel used, and clinical examination. Exposure was calculated in each woman by the number of hours spent in a day for cooking. Height was measured in standing position and without shoes, and weight was recorded with minimal clothing. Body Mass Index (BMI) was calculated. For spirometry, participants were seated without nose clips and measurements were classified as acceptable if the woman had at least three good blows, and if best and second best values of Forced Expiratory Vital Capacity (FVC) and Forced Expiratory Volume in 1 second (FEV 1), respectively, did not differ by more than 0.20 liters. The data were compared with predictive values based on age, sex and height. The parameters like Forced Vital Capacity (FVC), Forced Expiratory Volume in 1 second (FEV1), FEV1% and Forced Expiratory Flow 25-75 (FEF25-75). Peak Expiratory Flow Rate (PEFR) was measured using Wright’s Peak Flow Meter (Clement and Clarke, UK). FVC and FEV1 were expressed in litres, PEFR in litres/min, FEF25-75 in litres/sec, FEV1% was presented as the ratio of FEV1, and FVC expressed in percentage.
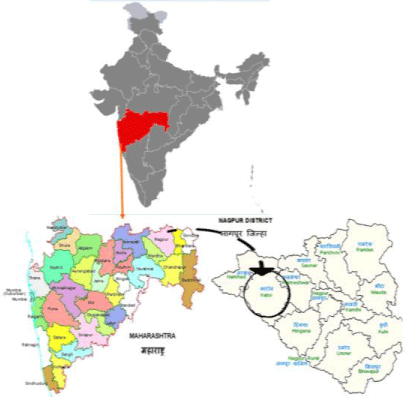
Figure 1:
Statistical analysis was done using IBM 21 version of SPSS. Percentage, mean and standard deviation was calculated. The Chisquare test trend and analysis of variance was used for statistical analysis a confidence level of 95%.
Results
Physical access to LPG was reported by (44.9%) of respondents, although 50.9 % of them used mixed fuels as main source of fuel (that is gas and wood, crop residue, dung cakes). Only 10 % of the respondents were using LPG alone for their energy requirement. Out of the 202 households, which had a gas connection, only 40 households (8.89%) obtained their gas connection under Pradhan Mantri Ujjwala Yojna (PMUY) a Government of India scheme to provide clean fuel to low income population. Most frequently used fuel for cooking was LPG (52.4%) in combination with wood (47.6%). The overall mean household consumption of wood fuel was 5kg per day. Dung (21.6%) and Kerosene (12.0%) were used less frequently.
Table 1 shows the distribution of age, height, weight, BMI, and exposure index of cooking according to different types of symptoms (eye irritation, dizziness, dry cough, phlegm, wheezing, headache, nasal irritation, and body ache) encountered by study subjects. The symptomatic women had higher age (P <0.05) and low BMI. Similarly, the symptomatic women had a higher duration of exposure (P <0.05). The height was similar in all the groups irrespective of presence or absence of symptoms/morbid conditions. Women with morbid conditions (abnormal pulmonary function, chronic bronchitis, bronchial asthma, cataract, and anemia) had significantly higher age and greater duration of exposure (P <0.05) except for bronchial asthma where it did not reach statistical significance though the mean age and EI was higher
Symptoms
Age
Weight
Height
BMI
Duration
Exposure Index
Cough
Presence
41.89 ± 13.75
51.24 ± 7.95
153 ± 14.81
22.21 ± 4.13
1.763 ± 0.63
313 ± 3.444
Absence
40.30 ± 13.62
52.04 ± 9.50
155.99 ± 12.91
21.43 ± 3.19
1.73 ± 0.66
137 ± 3.39
P value
P >0.05
P >0.05
P <0.05
P >0.05
P >0.5
0.386
Phelgm
Presence
42.9 ± 13.45
51.34 ± 7.80
152.22 ± 15.05
22.51 ± 4.12
1.77 ± 0.63
279 ± 3.48
Absence
39.35 ± 14.12
52.37 ± 9.27
156.88 ± 12.84
21.35 ± 3.20
1.71 ± 0.66
162 ± 3.36
P value
P >0.05
P >0.05
P <0.001
P <0.01
P >0.5
0.104
Cough Phelgm
Presence
42.96
50.82 ± 7.77
151.38 ± 15.51
22.5814
1.77 ± 0.63
247 ± 3.488
Absence
39.53
52.28 ± 9.172
157.09 ± 11.98
21.245
1.72 ± 0.66
203 ± 3.33
P value
P >0.05
P >0.05
P <0.001
P <0.001
0.06
Wheezing
Presence
43.68 ± 13.71
51.00 ± 8.071
151.02 ± 15.42
22.77 ± 4.42
1.78 ± 0.63
2143 ± 233.56
Absence
39.35 ± 13.43
51.91 ± 8.78
156.61 ± 12.62
21.25 ± 3.17
1.72 ± 0.66
2363 ± 233.23
P value
P <0.05
P >0.05
P <0.001
P <0.001
P <0.5
0.002
Headache
Presence
41.73 ± 13.74
51.49
153.97 ± 14.46
22.00 ± 3.97
1.76 ± 0.63
424 ± 3.42
Absence
36.27 ± 12.50
51.27 ± 9.22
153.69 ± 11.47
21.60 ± 1.95
1.57 ± 0.75
26 ± 3.23
P value
P <0.001
P <0.001
P <0.001
P >0.05
P <0.5
0.052
Chest pain
Presence
51.48 ± 8.45
51.86 ± 8.80
153.53 ± 13.43
22.18 ± 3.76
1.78 ± 0.63
275 ± 3.674
Absence
41.99 ± 13.76
5090 ± 7.85
154.61 ± 13.43
21.64 ± 4.06
1.70 ± 0.66
175 ± 2.99
P value
P >0.05
P >0.05
P >0.05
P >0.05
<0.5
0.32
Breathlessness
Presence
42.36 ± 13.77
52.37 ± 8.61
153.63 ± 13.47
22.38 ± 3.68
1.78 ± 0.63
270 ± 3.68
Absence
39.99 ± 13.56
50.15 ± 8.042
154.45 ± 15.48
21.37 ± 4.11
1.71 ± 0.66
180 ± 2.98
P value
P >0.05
P <0.01
P >0.05
P <0.01
P <0.5
0.098
Eye Irritation
Presence
41.57 ± 14.03
52.38 ± 8.61
154.33 ± 13.05
22.18 ± 3.74
1.78 ± 0.64
269 ± 3.59
Absence
41.41 ± 13.16
50.24 ± 8.20
153.53 ± 16.30
21.68 ± 4.15
1.71 ± 0.65
174 ± 3.125
P value
P >0.05
P <0.05
P >0.05
P >0.05
P <0.5
0.564
Blackout
Presence
41.30 ± 13.94
52.61 ± 8.65
154.51 ± 13.54
22.23 ± 3.74
1.77 ± 0.64
256 ± 3.58
Absence
41.56 ± 13.45
50.01 ± 7.96
153.23 ± 15.36
21.64 ± 4.04
1.73 ± 0.64
194 ± 3.21
P value
P >0.05
P <0.001
P >0.05
P >0.05
P <0.5
0.72
Sneezing
Presence
40.88 ± 15.15
53.38 ± 8.18
153.93 ± 15.46
22.88 ± 4.21
1.8163
98 ± 3.66
Absence
41.56 ± 13.31
50.96 ± 8.46
153.97 ± 13.98
21.72 ± 3.76
1.7386
352 ± 3.36
P value
P >0.05
P <0.01
P >0.05
P <0.01
P <0.5
0.83
Chest tightness
Presence
40.44 ± 15.05
52.92 ± 8.14
153.71 ± 15.53
22.741 ± 4.10
1.75 ± 0.69
105 ± 3.61
Absence
41.71 ± 13.30
51.05 ± 8.50
154.03 ± 13.92
21.74 ± 3.79
1.75 ± 0.63
241 ± 3.37
P value
P >0.05
P <0.05
P >0.05
P <0.05
0.9
Joint pain
Presence
40.63 ± 14.96
51.48 ± 8.06
156.42 ± 13.97
21.13 ± 2.59
1.75 ± 0.69
90 ± 3.67
Absence
41.61 ± 13.41
51.49 ± 8.55
153.34 ± 14.33
22.18 ± 4.12
1.75 ± 0.63
360 ± 3.36
P value
P >0.05
P >0.05
P >0.05
P <0.05
>0.5
0.784
Dizziness
Presence
42.15±14.49
51.98±8.91
155.46±13.08
21.62±3.37
1.79±.64
209 ±3.69
Absence
40.77±13.01
51.06±8.02
152.65±15.18
22.28±4.26
1.72±.64
345± 3.37
P value
P>0.05
P>0.05
P<0.05
P>0.05
P<0.05
0.05
Nausea
Presence
43.09 ± 14.90
50.06 ± 8.10
156.24 ± 13.59
20.61 ± 2.996
1.74 ± 0.70
54 ± 4.22
Absence
41.18 ± 13.55
51.68 ± 8.49
153.65 ± 14.30
22.16 ± 3.88
1.75 ± 0.63
396 ± 3.3
P value
P >0.05
P >0.05
P >0.05
P <0.01
P >0.05
0.36
Nasal Discharge
Presence
40.86 ± 13.66
52.60 ± 7.31
155.11 ± 13.20
24.99 ± 3.67
1.678 ± 0.66
56 ± 3.21
Absence
41.49 ± 13.47
51.32 ± 8.59
153.95 ± 14.09
21.55 ± 3.72
1.76 ± 0.64
39 ± 43.45
P value
P >0.05
P >0.05
P <0.001
P <0.001
P <0.5
0.34
Table 1: Distribution of age, height, body mass index and Exposure Index of cooking among biomass fuel users and non-users according to presence or absence of symptoms (mean ± SD).
Table 2 shows the comparisons of symptoms/morbidities in different fuel users for all the 450 study participants who were able to perform spirometry. All the participants were divided into two fuel categories that is LPG/biogas users, and biomass fuel users based on the primary fuel type used by the households. The comparison was made for lung function parameters among women cooking with fuel in these two categories. Significance test at 5% level of significance was used to estimate the difference between the means of the three groups. The results showed that the mean values of FEV1 and the ratio of FEV1/FVC of LPG users were more than the corresponding values for biomass fuel users. The analysis of variance shows that the difference was found statistically significant for and FVC/FEV% ratio for biomass fuel users while for gas users it was not significant.
N
Mean
Std. Deviation
Sig.
FVC Predicted
wood
249
2.84
0.927
0.656
LPG/Bioga
201
2.88
1.136
FVC Measured
wood
249
1.2935
1.37433
0.274
LPG/Bioga
201
1.4411
1.48157
FVC Percentage
wood
249
44.26
44.745
0.201
LPG/Bioga
201
49.91
48.624
FEV1 Predicted
wood
249
2.362
0.79359
0.77
LPG/Bioga
201
2.3863
0.97336
FVC1 Measured
wood
249
1.1255
1.24093
0.715
LPG/Bioga
201
1.1698
1.32366
FEV1%
wood
249
47.4297
48.7313
0.228
LPG/Bioga
201
53.2786
53.832
FVC/FEV1%
wood
249
89.0861
18.6204
0.031
LPG/Bioga
201
84.75
23.9426
Table 2: Comparison of symptoms/morbidities in different fuel users.
Table 3 describes the comparison of symptoms/morbidities in different fuel users. Participants experienced various symptoms like eye irritation, headache, giddiness, dry cough, and nasal irritation during cooking. The prevalence of symptoms like eye irritation, headache, and dry cough was higher among biomass users as compared with, LPG. Chi-square test across all cooking fuel categories revealed statistically significant difference for eye irritation, chest pain, blackout (P<0.01) and breathlessness (P <0.05). Furthermore, the prevalence of morbid conditions was found to be significantly higher among biomass users for Dysnosea (64.5%), chestpain (66.8%), eye irritation (65.4%) and blackout (62.1%) compared with other fuels.
Respiratory Index
wood
LPG
Total
P value
Cough
151(70.6)
162(68.6)
313(69.6)
>0.05
Phelgm
135(65.2)
144(61.5)
279(63.3)
>0.05
Nasal discharge
31(14.5)
25(10.6)
56(12.4)
>0.05
Nasal Obstruction
Sneezing
49(22.9)
49(20.8)
98(21.8)
>0.05
Chest pain
143(66.8)
132(55.9)
275(61.1)
<0.05
Shortness of breath
138(64.5)
132(53.8)
270(60.0)
<0.05
Non Respirotory Index
Eye irritation
136(65.4)
133(56.6)
269(60.7)
<0.05
Wheezy chest
105(49.1)
109(46.2)
214(47.6)
>0.05
CO symptoms
Dizziness
103(48.1)
106(44.6)
209(46.4)
>0.05
Headache
205(95.8)
219(92.8)
424(94.2)
>0.05
Nausea
25(11.7)
29(12.3)
54(12.0)
>0.05
Other
11.70%
12.30%
12.00%
Joint pain
36(16.8)
54(22.9)
90(20)
>0.05
Blackout
133(62.1)
127(53.8)
260(57.8)
<0.001
Table 3: Comparison of symptoms/morbidities in different fuel users.
Table 4 shows the lung function parameter FVC (observed and percent predicted) among participants with respiratory symptoms/ morbidities. The presence of symptoms/morbid conditions (dry cough, phelgm, abnormal pulmonary function, chronic bronchitis, bronchial asthma) was associated with lower values of FVC, FEV and FVC/FEV ratio (P <0.05 to 0.001). The asymptomatic women had significantly higher values as compared to symptomatic women (P <0.05 to 0.001).
Symptoms
FEV/FVC ratio
FEV 1
FVC
Cough
Presence
86.59 ± 20.76
2.91 ± 1.35
2.96 ± 1.29
Absence
88.40 ± 22.34
2.75 ± 1.42
2.77 ± 1.35
P value
>0.05
>0.05
>0.05
Phelgm
Presence
89.25 ± 13.94
2.94 ± 1.33
3.12 ± 1.28
Absence
84.59 ± 27.48
2.78 ± 1.41
2.60 ± 1.33
P value
<0.001
>0.05
<0.001
Cough Phelgm
Presence
89.25 ± 13.93
2.93 ± 1.35
3.06 ± 1.30
Absence
84.59 ± 27.48
2.78 ± 1.35
2.70 ± 1.31
P value
<0.05
>0.05
<0.05
Wheezing
Presence
88.48 ± 14.67
3.03 ± 1.33
3.17 ± 1.25
Absence
85.94 ± 25.77
2.71 ± 1.35
2.66 ± 1.32
P value
>0.05
<0.05
<0.001
Headache
Presence
86.91 ± 21.79
2.95 ± 1.32
2.99 ± 1.27
Absence
90.93 ± 7.52
1.46 ± 1.10
1.46 ± 1.10
P value
>0.05
<0.001
>0.001
Chest pain
Presence
92.61 ± 14.29
3 ± 1.31
3.00 ± 1.32
Absence
78.55 ± 26.86
2.64 ± 1.38
2.74 ± 1.28
P value
<0.001
<0.05
<0.05
Breathlessness
Presence
91.13 ± 17.57
3.05 ± 1.32
3.05 ± 1.33
Absence
81.16 ± 24.66
2.58 ± 1.36
2.68 ± 1.26
P value
<0.001
<0.001
<0.05
Eye Irritation
Presence
92.02 ± 14.35
3.04 ± 1.31
3.05 ± 1.33
Absence
79.09 ± 27.27
2.55 ± 1.37
2.63 ± 1.26
P value
<0.001
<0.001
<0.001
Blackout
Presence
91.80 ± 14.55
3.07 ± 1.28
3.10 ± 1.30
Absence
80.78 ± 26.68
2.59 ± 1.40
2.63 ± 1.28
P value
<0.001
<0.001
<0.001
Sneezing
Presence
90.02 ± 14.04
3.01 ± 1.19
3.11 ± 1.28
Absence
86.34 ± 22.80
2.82 ± 1.39
2.84 ± 1.32
P value
>0.05
>0.05
>0.05
Dizziness
Presence
90.76 ± 15.93
3.23 ± 1.17
3.28 ± 1.20
Absence
84.01 ± 24.56
2.54 ± 1.41
2.580 ± 1.32
P value
<0.05
<0.001
<0.001
Table 4: FVC, FEV and FVC/FEV ratio among study subjects with respiratory symptom/morbidities.
Discussion
The study determined the role of domestic smoke on the health of 450 non-smoking rural women exposed to different types of cooking fuels. The study also included the clinical diagnosis of the symptoms reported by the women through spirometry during field visits and the duration of health conditions was assessed, information regarding use of fuels in years was enquired with The time spent near the biomass fuel was subjected to recall bias. Women presenting with various symptoms/morbid conditions were older and had a greater duration of cooking. Symptoms like eye irritation, headache, and diminution of vision were found to be significantly higher in biomass users (P <0.05). Pokheral AK et al. observed a significant association between current biomass usage and the development of nuclear cataracts (OR=2.58; 95% CI: 1.22-5.46), which also increased with the duration of exposure in years [26]. Similar findings were also reported by Ravilla TD et al. (AOR = 1.28; 95% CI: 1.10-1.48) [27].
It was observed that women with respiratory symptoms had higher risk of being exposed to biomass fuel as compared to those without symptoms, which is similar to the findings reported in Mexico and in India [28,29]. A systematic review by Sana A. et al. also concluded that COPD was more likely to be diagnosed among women who had a history of exposure to biomass fuel (OR = 1.38; 95% CI: 1.28-1.57) [30]. However, a study in Pakistan found no such associations [31].
The present study showed that women with self-reported cardiovascular symptoms/conditions were at higher risk of being ever exposed to biomass fuel and similar findings were reported by a study in Odisha, India (p <0.05), in Nigeria (OR = 1.67; 95% CI: 1.56-4.99) and in China (OR = 2.58; 95% CI: 1.53-4.32) [32-34].
To summarize, more than two-thirds of the families were using biomass in our study and it was found that being ever exposed to biomass fuel was significantly associated with their socio-demographic characteristics, self-reported ophthalmic, respiratory, dermatological, cardiovascular symptoms/conditions.
Our study findings also suggest that households using both LPG and biomass fuel for cooking may have serious health implications from exposure to mixed fuel use. Although the best health benefits result from exclusive use of LPG, even partial LPG adoption has shown to improve health outcomes [35]. Access to the clean fuels like LPG though increased by a program like PMUY, but the stacking (multiple fuel use) of fuels needs to be addressed. India’s Council for
Energy, Environment, and Water (CEEW) noted in their Access to Clean Cooking Energy and Electricity Survey of States (ACCESS) that households’ use of LPG increases with the age of connection [36]. Therefore, if the PMUY policy provides an impetus for families to even partially adopt LPG when they would otherwise be wholly reliant on unclean fuels, it can be considered an effective policy. The penetration of clean fuel was low in the study area and as such, the number of connections given in the whole Nagpur district until 2018 were only 12,000 [37]. So considering that Nagpur has 14 blocks, these are less as compare to other parts of India. The reason for this could be the district was not a high priority district in the programme [38].
The study observes a higher prevalence of respiratory symptoms and lung function capacity impairment in Biomass Fuel users as compared with clean fuel (LPG), users. This urges to have a greater emphasis on clean fuel programmes to improve the health of women cooks [39]. In a study conducted in Turkey a highly significant (p <0.00001) reduction of FEV1, FVC, FEV1/FVC and FEF25-75 was observed in case of biomass fuel users. A study conducted in an urban Indian slum showed significantly lower FVC, FEV1, FEV1% and PEFR values in bio-fuel using women in comparison to modern fuel users (kerosene and LPG) his study eventually concludes showing the adverse effects of biomass fuels (especially wood) use on the deterioration of pulmonary function.
The other objective of the PMUY scheme that of health benefits of clean fuel are not achieved in the study area as seen from the results of spirometry.
Conclusion
The present study investigated the association of symptoms (HAP related) such as difficulty in breathing, and dry cough with the presence of HAP sources and contributory factors. HAP and its detrimental effects are preventable. The rural poor living in illventilated house should be provided with better housing conditions. The policy makers should promote the use of clean fuel (LPG) in cost effective manner. Incomplete switchover to cleaner alternatives has hampered the health benefits of cleaner fuels and behavioral changes may decrease the health effects of HAP. Therefore, these households may require continued public health interventions such as subsidies and regular health education. Grass root workers in the health system need to be involved in PMUY programme to educate women and make them aware of the deleterious effects of HAP on their own health and of their children.
Thus, in conclusion the present study showed that the women using biomass fuel for cooking suffered more from respiratory and other morbidities than the women using other types of cooking fuels. Also, the morbidities found to be increased with increase in duration of cooking.
Ethical Approval
Ethical clearance was taken from the Institutional Ethics Committee of Rashtrasant Tukdoji Maharaj Nagpur University India. Informed consent was obtained from all subjects of the study.
References
- Parikh J, Balakrishnan K, Laxmi V, Biswas H. Exposure from cooking with biofuels: pollution monitoring and analysis for rural Tamil Nadu, India. Energy. 2001; 26: 949-962.
- Balakrishnan K, Sankar S, Parikh J, et al. Daily average exposures to respirable particulate matter from combustion of biomass fuels in rural households of southern India. Environ Health Perspect. 2002; 110: 1069- 1075.
- Balakrishnan K, Sambandam S, Ramaswamy P, Mehta S, Smith KR. Exposure assessment for respirable particulates associated with household fuel use in rural districts of Andhra Pradesh, India. J Expo Anal Environ Epidemiol. 2004: S14-25.
- Arku RE, Birch A, Shupler M, Yusuf S, Hystad P, Brauer M. Characterizing exposure to household air pollution within the Prospective Urban Rural Epidemiology (PURE) study. Environ Int. 2018; 114: 307-317.
- Naghavi M, Wang H, Lozano R, Davis A, Liang X, Zhou M, et al. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: A systematic analysis for the Global Burden of Disease Study 2013. The Lancet. 2015; 385: 117-171.
- IEA, IRENA, UNSD, WB, WHO. Tracking SDG 7: The Energy Progress Report 2019. Washington DC. 2019.
- Global Health Observatory visualizations. Household Air pollution. Geneva: World Health Organization. 2012.
- Balakrishnan Kalpana. The impact of air pollution on deaths, disease burden, and life expectancy across the states of India: the Global Burden of Disease Study 2017. India State-Level Disease Burden Initiative Air Pollution Collaborators 2019. The Lancet Planetary Health.
- Census of India 2011. Houses, Household Amenities and Assets. Government of India. 2013.
- Behrens A, Lahn G, Dreblow E, Nuñez-Ferrer J, Carraro M, Veit S. Escaping the vicious cycle of poverty: Towards universal access to energy in developing countries. Brussels: Centre for European Policy Studies. 2012. CEPS Working Document 363.
- Barnes DF, Floor WM. Rural energy in developing countries: a challenge for economic development. Annu Rev Energ Environ. 1996; 21: 497-530.
- Ezzati M, Kammen DM. Household energy, indoor air pollution and health in developing countries: Knowledge base for effective interventions. Annu Rev Energ Environ. 2002; 27: 233-270.
- Fullerton DG and Bruce N. Indoor air pollution from biomass fuel smoke is a major health concern in the developing world. T Roy Soc Trop Med H. 2008; 102: 843-851.
- Bruce N, Perez-Padilla R, Albalak R. Indoor air pollution in developing countries: A major environmental and public health challenge. Bull. World Health Organ. 2000; 78: 1078-1092.
- Edwards JHY, Langpap C. Fuel choice, indoor air pollution and children’s health. Environ and Dev Econ. 2012; 17: 379-406.
- Pachauri S, Jiang L. The household energy transition in India and China. Energy Policy. 2008; 36: 4022-4035.
- Bruce N, Perez-Padilla R, Albalak R. Indoor air pollution in developing countries: A major environmental and public health challenge. Bull. World Health Organ. 2000; 78: 1078-1092.
- World Health Organization. The World Health Report: Reducing Risks, Promoting Healthy Life, Chapter 4, Quantifying Selected Major Risks to Health, No.8, Environmental Risks, WHO, Geneva. 2002.
- WHO. 2018.
- IHME. Global Burden of Disease Results Tool. 2017.
- IIPS and ICF. National Family Health Survey (NFHS-4) 2015-16: India. Mumbai: IIPS: International Institute for Population Sciences and ICF. 2017.
- Government of India, National Sample Survey. “Energy Sources of Indian Households for Cooking and Lighting, Report No. 542 (66/1.0/4)”. Ministry of Statistics and Programme Implementation. 2010.
- Maharashtra Economic Survey Report 2012-13. Government of Maharashtra.
- Pradhan Mantri Ujjwala Yojana: A Giant Step towards Better Life for All. Press Information Bureau. 2016.
- American Thoracic Society (ATS). Standardization of Spirometry. Am J Respir Crit Care Med. 1995; 152: 1107-1136.
- Pokhrel AK, Bates MN, Shrestha SP, Bailey IL, DiMartino RB, Smith KR, et al. Biomass Stoves and Lens Opacity and Cataract in Nepalese Women. Optom Vis Sci. 2015; 90: 257-268.
- Ravilla TD, Gupta S, Ravindran RD, Vashist P, Krishnan T, Maraini G, et al. Use of cooking fuels and cataract in a population-based study: The India eye disease study. Environ Health Perspect. 2016; 124: 1857-1862.
- Venegas AR, Uncal MV, Herna´ndez RP, Bouilloud NEG, Valencia RF, Maya MEM, et al. Prevalence of COPD and respiratory symptoms associated with biomass smoke exposure in a suburban area. Int J Chron Obstruct Pulmon Dis. 2018; 13: 1727-1734.
- Sinha B, Vibha, Singla R, Chowdhury R. Allergic Rhinitis: A neglected disease-A community based assessment among adults in Delhi. J Postgrad Med. 2015; 61: 169-175.
- Sana A, Somda SMA, Meda N, Bouland C. Chronic obstructive pulmonary disease associated with biomass fuel use in women: a systematic review and meta-analysis. BMJ Open Respiratory Research. 2018; 5: e000246.
- Kazi A. Association between Biomass Fuel for Cooking and Serum Nitric Oxide among Women in Karachi, Pakistan. SM Women’s health issues care. 2018; 1: 1001.
- Mohapatra I, Das SC, Samantaray S. Health impact on women using solid cooking fuels in rural area of Cuttack district, Odisha. J Family Med Prim Care. 2018; 7: 11-15.
- Ofori SN, Fobil JN, Odia OJ. Household biomass fuel use, blood pressure and carotid intima media thickness; a cross sectional study of rural dwelling women in Southern Nigeria. Environmental Pollution. 2018; 242: 390-397.
- Lee MS, Hang J, Zhang F, Dai H, Su L, Christiani DC. In-home solid fuel use and cardiovascular disease: a cross-sectional analysis of the Shanghai Putuo study. Environ Health. 2012; 11: 18.
- Gould Carlos and Urpelainen Johannes. LPG as a Clean Cooking Fuel: Adoption, Use, and Impact in Rural India. Energy Policy, Forthcoming. 2018.
- Sumer H, Turaclar UT, Onarlioglu T, Ozdemir L, Zwahlen M. The association of biomass fuel combustion on pulmonary function tests in the adult population of Mid-Anatolia. Soz Praventivmed. 2004; 49: 247-253.
- Dutt D, Srinivasa DK, Rotti SB, Sahai A, Konar D. Effect of indoor air pollution on the respiratory system of women using different fuels for cooking in an urban slum of Pondicherry. Natl Med J India. 1996; 9: 113-117.
- Saha A, Rao NM, Kulkarni PK, Majumdar PK, Saiyed HN. Pulmonary function and fuel use: a population survey. Respir Res. 2005; 6: 127.
- Kaur-Sidhu M, Ravindra K, Mor S, John S, Aggarwal AN. Respiratory Health Status of Rural Women Exposed to Liquefied Petroleum Gas and Solid Biomass Fuel Emissions. Air, Soil and Water Research. 2019.