
Research Article
Austin J Reprod Med Infertil. 2016; 3(1): 1035.
Perspectives on the Management of Infertility in Primary Care: A Survey of Healthcare Providers in a Regional Health Care System in Southwest Virginia
Gentry AL¹*, Pagidas K¹ and Johnson I²
¹Department of Obstetrics and Gynecology, University of Louisville School of Medicine, USA
²Department of Obstetrics and Gynecology, Virginia Tech Carilion School of Medicine, USA
*Corresponding author: Adrienne L. Gentry, Department of Obstetrics and Gynecology, University of Louisville School of Medicine, 550 Chestnut St. Louisville, KY 40202, USA
Received: May 25, 2016; Accepted: July 05, 2016; Published: July 07, 2016
Abstract
Purpose: The objective of this study is to identify current practice patterns of the primary care providers in the Carilion Clinic system for the evaluation, management, and referral of patients with infertility.
Methods: A 15 question survey was emailed to primary care physicians, physician assistants, and nurse practitioners in the Carilion Clinic system. The survey included a demographic analysis of the practice, and provided questions in regards to practice patterns in the evaluation, treatment, and referral of an infertile couple. The inclusion criteria were all PCPs (family medicine, internal medicine). Exclusion criteria included any other field of medicine
Results: Twenty-five percent of PCPs in the Carilion network answered the survey. Majority of responders were family medicine (80%), and physicians (80%). Fifty-five percent were female and thirty percent have been practicing medicine for more than 20 years. Half of PCPs were comfortable initiating the diagnostic evaluation of the infertile couple and of these, seventy three percent order diagnostic testing. Less than half (42%) of providers refer patients greater than age 35 that present with infertility for more than 6 months.
Conclusion: This survey provides insight into the variation of practice patterns of infertility by primary care providers (PCPs). Although half of PCPs that answered our survey are comfortable initiating the evaluation of the infertile couple, they are not following the current referral guidelines. This can lead to delayed diagnosis, and decreased time to achieve pregnancy. Based on these results, an educational model may be beneficial for PCPs that are interested in the evaluation of the infertile couple.
Keywords: Infertility; Primary care providers; Clomiphene
Introduction
Approximately 10-15 percent of couples will experience infertility during their reproductive years. While the majority of women see an OBGYN for annual gynecological exams, some women that live in rural areas, and/or with limited access to care, seek gynecological care from a primary care provider. However, there may be an increase in the utilization of primary care providers within inner cities secondary to health care reform and the fact that women’s preventive health care must be covered. Surprisingly, there is limited data in regards to the percent of women that receive their well women care also known as an annual gynecological exam from a family medicine and/or internal medicine provider versus an OBGYN.
These primary care providers are often the first resource for women and couples for fertility counseling and, thus serve a critical role in the identification of women and couples experiencing difficulty conceiving. They also play an important role in the initial evaluation of the infertile couple.
Interestingly, after review of multiple academic primary care residency programs that have posted their residency curriculum on their website within the United States, they report that infertility education is part of their curriculum; albeit brief and superficial in scope. Furthermore, multiple primary care textbooks review the evaluation and initial work up of the infertility couple, including that of the American Academy of Family Physicians (AAFP).
Depending on the country, some primary care providers believe that infertility should be a part of their practice and desire it to be a part of their residency education [1,3]; however, others do not believe it should be a scope of their practice [2]. Interestingly, a study that was published in 1992 in Israel stated that primary care providers and general gynecologists should not be evaluating and treating the infertile couple [4]. This is likely due to the limited resources that were available and the novel concept of infertility at that time. Later in 2003, Smith et al. stated that general practitioners have the ability to treat couples with infertility with the idea of preventing some referrals to subspecialists; however, more guidelines would need to be developed [5].
Of the studies that had a positive outlook on primary care providers evaluating and treating infertile couples, the majority of them agreed that further education and algorithms would provide more competent providers, earlier evaluation and diagnosis, and more satisfied patients.
Despite the numerous surveys and work done in other countries in regards to primary care providers attitudes towards evaluation and treatment of the infertile couple, there is a paucity of information in the literature regarding the practice patterns of primary care providers in the United States. The objective of this study is to identify current practice patterns of the primary care providers in the Carilion Clinic system for the evaluation, management, and referral of patients with infertility.
Methods
A 15 question survey was developed. Two hundred and forty three primary care providers were identified within the Carilion Clinic system by searching public emails within the Carilion server. The primary care providers were comprised of physicians, resident physicians, physician assistants, and nurse practitioners. The survey was reviewed and approved by the Virginia Tech -Carilion School of Medicine IRB. Carilion Clinic is a hospital system in Western Virginia serving a population of approximately one million people. Surveys were sent via email on three different occasions between December 2013 through March 2014. Data were collected and analyzed using Survey Monkey.
The survey included a demographic analysis of the practice, and provided questions in regards to practice patterns in:
1) The evaluation of an infertile couple; 2) Treatment of an infertile couple; 3) Diagnosis and Referral of an infertile couple. (Insert Survey)
The questions asked for the three categories were:
1) The evaluation of an infertile couple
a) I am comfortable initiating the diagnostic evaluation of patient that present with infertility
b) Do you order diagnostic testing for patients that present with infertility
c) If you answered yes to the above question, what tests do you order?
2) Treatment of an infertile couple
a) I perform ovulation induction with clomiphene citrate in my practice.
b) Dose of clomiphene citrate that I feel comfortable prescribing is
3) Diagnosis and Referral of an infertile couple.
a) I routinely refer patients less than 35 years old that present with infertility for more than one year.
b) I routinely refer patients less than 35 years old that present with infertility for more than two years.
c) I routinely refer patients 35 and older that present with infertility for more than 6 months.
d) I routinely refer patients 35 and older that present with infertility for more than 1 year.
e) I refer my patients with infertility to (OBGYN, REI, other)
Answers to the questions were either yes/no, multiple choice or 5-point Likert scale depending on the question being asked. The inclusion criteria were all primary care providers (family medicine, internal medicine, general practitioners), regardless of age, sex, gender, and ethnic characteristic. Exclusion criteria included any other field of medicine.
Results
The e-mailed survey was completed by 60 out of 243 primary care providers (25%). Three of the email addresses were undeliverable. Table 1 provides a demographic summary of the respondents. Less than half (44%) of providers were between the ages of 31-45, and 34% were between the ages of 46-60. Only, five percent of providers were older than 60 years of age. Just over half (55%) of the providers were female. Rural health care providers made up 33% of the respondents, suburban practitioners made up 47%, and 18% of the providers practice in inner cities. Recently trained providers (less than 5 years) were 37% of the responders, whereas 30 percent had practiced medicine for more than 20 years.
Number
Percent
Total Surveys Sent
243
Responses
60
24.7
Specialty
Family Medicine
50
83.3
Internal Medicine
8
13.3
Other
2
3.3
Experience, y
<5
22
36.7
9-May
6
10
14-Oct
9
15
15-19
5
8.3
20 or more
18
30
Age,y
<30
10
16.95
31-45
26
44.1
46-60
20
33.9
>60
3
5.1
gender
Male
27
45
Female
33
55
Degree
MD/DO
46
76.7
Nurse Practioner
12
20
Physician Assistant
2
3.3
Pracice Size
Individual Practice
1
1.67
5 or Fewer providers
17
28.3
6 or greater providers
39
65
other
3
5
Practice location
Rural
20
33.3
Suburban
28
46.7
Urban
11
18.4
Other
1
1.7
Table 1: Demographic Table.
Overall, half of primary care providers (53%) report that they feel comfortable initiating the diagnostic evaluation of patients that present with infertility (17% somewhat agree and 37% strongly agree), while approximately seven percent do not feel comfortable (strongly disagree); (Figure 1). Seventy percent of responders reported that they refer patients less than 35 years of age when they have a history of one year of infertility, and seventy-eight percent state they refer patients less than 35 years of age with more than two years of infertility (Figure 2). Less than half (42%) of providers refer patients greater than age 35 that present with infertility for more than six months, and 74 percent said they would refer patients greater than age 35 that present with infertility for more than a year (Figure 3).

Figure 1: Percent of providers that are comfortable initiating the diagnostic
evaluation of patients that present with infertility.

Figure 2: Providers that refer patients less than 35 that present with infertility
for more than one or two years.

Figure 3: Providers that refer patients 35 yo and older that present with
infertility for more than six months and one year.
Over half of providers (60%) refer their patients to a Reproductive Endocrinology and Infertility specialist, the remainder refers to an Obstetrician and Gynecologist (Figure 4). The majority of providers (73%) order diagnostic testing for patients that present with infertility (Figure 5). Of the providers that would order diagnostic testing, forty percent would order a luteal phase progesterone, nine percent would order a hysterosalpingogram (HSG), forty-nine percent would order a trans vaginal ultrasound, seventy- eight percent would order a semen analysis, ninety-one percent would order a thyroid stimulating hormone (TSH), eighty percent would order a prolactin, thirteen percent would order a day 3 follicle stimulating hormone(FSH), fiftythree percent would recommend ovulation predictor kits, and fortyfour percent would recommend luteal phase basal body temperature charting. However, none of the providers would order an antimullerian hormone (AMH) (Figure 6). Only eight percent (five providers) feel comfortable prescribing an ovulation induction agent, clomiphene citrate at different doses (50mg, 100mg, 150mg), (Figure 7). None of the providers would order 50mg x 5 days, 250mg x 5 days, or 250mg x seven days. However, one of the five (20%) providers would order 100mg x 5 days, two of the five (40%) providers would order 150mg x 5 days, and the other two (40%) would order 200mg x 5 days.

Figure 4: Providers referred to by PCP for further infertility workup.

Figure 5: Percent of providers that order diagnostic tests of patients that
present with infertility.

Figure 6: Diagnostic tests that providers would order or recommend.
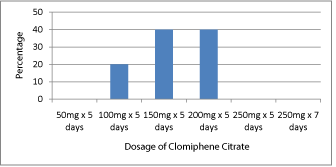
Figure 7: Dosage of clomiphene citrate prescribed by providers that feel
comfortable prescribing clomiphene citrage.
Discussion
This survey provides important insight into the infertility practice patterns by the primary care provider. There is certainly a significant variation in practice patterns among primary care providers in their evaluation and management. The diagnosis and treatment of the infertile couple can be straight forward or quite challenging depending on the etiology. The American Society of Reproductive Medicine (ASRM) and the AAFP both specifically state a diagnostic evaluation for infertility should be initiated when a woman fails to conceive after twelve months of regular unprotected intercourse [6- 8]. This exact evaluation is warranted in a woman that is 35 years and older when she has not conceived after only six months of regular unprotected intercourse.
ASRM states the basic infertility work up should include a thorough history and physical, uterine cavity evaluation, tubal evaluation, basic lab work including thyroid stimulating hormone (TSH) and prolactin, and a semen analysis of the male partner [6,7]. The AAFP basically provides the same basic infertility work up as described by ASRM [7]. The sequence of evaluation and testing is based on the patient and or couple’s history and presentation.
It is important that primary care providers that do feel comfortable initiating the basic evaluation know when the appropriate time is to refer, because depending on a patient’s age it can be a time sensitive manner. This is mainly due to the decrease in fertility and poorer pregnancy outcomes as a woman get older.
A breadth of literature states that there is an age related decline in fertility starting at age 32 with a dramatic decline by the age of 37 [9]. Not only is there a decline in fertility as a woman ages after 35, but there is also an increase in adverse pregnancy outcomes [9, 10]. These adverse outcomes include an increase in miscarriage rate, chromosomal abnormalities, gestational diabetes, preeclampsia, small for gestational age, and cesarean section [9,10].
Over half of the primary care providers in the Carilion network are comfortable initiating the evaluation of the infertile couple. Of those that stated they would do a work up, nine percent would do a hysterosalpingogram for evaluation of tubal patency, 40% would evaluate if the woman was ovulatory, 49% would evaluate the uterus via trans vaginal ultrasound, almost all would order TSH (91%) and prolactin (80%), and 77% would order a semen analysis on male partner. However, few would evaluate ovarian reserve, with only 13% ordering a day 3 FSH, and none of the providers ordering an AMH. This data is important because it allows us to evaluate the cause of the couple’s infertility, and whether or not the primary care provider is capturing the diagnosis. Approximately 30% of a couple’s infertility is secondary to a female cause [6]. Ovulation disorders make up twentyfive percent of female infertility, meaning ovulating infrequently or not at all. Ovulatory disorders can be secondary to polycystic ovarian syndrome (the most common ovulatory disorder), an elevated prolactin, hypothalamic dysfunction, or premature ovarian insufficiency. Thirty percent of a couple’s infertility is related to male factor alone, while a third of couples that present have both male and female factors that contribute to their infertility diagnosis [6]. The majority (77%) of the providers that answered this study would capture a male factor related cause, forty percent would evaluate if the patient was ovulatory, and a number of the providers would evaluate etiology of ovulatory dysfunction. This information should be encouraging to patients and referral specialists that the primary care providers are able to evaluate, diagnose, and rule out the most common causes of infertility.
In review, both colleges specifically state that an infertility work up should include a thorough history and physical exam, evaluation for ovulatory dysfunction, ovarian reserve testing via AMH if available and/or day 3 FSH and antral follicle count, estradiol, TSH, and prolactin levels, uterine abnormalities, tubal patency, and peritoneal factors such as endometriosis [6-8]. The fact that none of the providers would order an AMH level is not surprising since a day 3 FSH is currently the standard of care in evaluating ovarian reserve. AMH is a more novel method in the evaluation of ovarian reserve, and knowledge of interpretation may be limited.
Per our survey results over half (60%) of the providers refer their patients that present with infertility to a Reproductive Endocrinology and Infertility specialist, the remainder send their patients to a general gynecologist. However, the providers are not referring the patients based on ASRM’s current guidelines as stated above.
The majority of the providers (70%) stated they would refer a woman that is less than 35 years of age after one year of unprotected intercourse that did not conceive. Whereas, less than half of the respondents stated they would refer a patient greater than 35 that has been unable to conceive after 6 months of unprotected intercourse, but 65 percent of the providers would refer these patients after one year of infertility.
It is uncertain why these providers would not refer based on the current guidelines given the recommendations by ASRM and the AAFP. One reason could be that these providers are not currently up to date with these current guidelines. Furthermore, only some of the providers appeared to order correct diagnostic tests.
Another reason for these discrepancies could be based on the location the provider received his or her training and comfort in the field. Of note, the majority of the respondents had either practiced for less than five years, or greater than 20 years. Maybe, the providers with a longer tenure feel more comfortable with the evaluation and diagnosis; however, are unaware of the referral recommendations. Whereas, the providers that have practiced only a short time are less comfortable with the evaluation, but more knowledgeable and up to date with when to refer. The survey did not distinguish the age or tenure of which providers ordered which diagnostic test or their referral patterns.
Furthermore, very few providers (8%) that answered the survey admitted to prescribing clomiphene citrate. Currently, the recommendations for the use of clomiphene citrate are to provide ovulation induction in women diagnosed with an ovulatory dysfunction and for use as an oral agent for unexplained infertility [11]. Clomiphene citrate is a selective estrogen receptor modulator that competitively binds to estrogen receptors and inhibits endogenous estrogen from binding to its own receptors. It is most important to have an adequate diagnosis of ovulatory dysfunction prior to prescribing clomiphene citrate, as the primary indication for the medication is for women with infertility secondary to an ovulation and/or oligo ovulation. If the patient has a diagnosis of unexplained infertility, the literature clearly supports the use of Clomiphene citrate in treatment regimens [12]. For the purposes of a primary care practice, however, clomiphene citrate would likely only be prescribed for an ovulatory patient.
The recommended starting dose for all patients novel to the drug is 50mg daily for five days after a natural or induced withdrawal bleed [11]. If the lowest dose does not adequately promote follicular growth and ovulation the dose may be titrated by 50 mg up to a maximum daily dose of 150mg daily for five days. However, studies report there is a minimal increase in clinical pregnancy rate when doses greater than 100 mg daily are used [11].
Though only five providers felt comfortable prescribing clomiphene citrate, two of the five would prescribe as high as 200mg x 5 days, with one only feeling comfortable prescribing up to 150mg x 5 days. Again, our survey was not built to allow us to determine the length of practice time of the respondents that were prescribing this medication.
Interestingly, there is also very limited data in regards to practice patterns of general gynecologists in regards to evaluation, treatment, and referral of patients with infertility. One study that was identified, by Rothenberg and colleagues [13], included a survey sent to general OBGYNs in an academic network. The physicians that engaged in general Obstetrics and Gynecology practice were much more comfortable prescribing clomiphene citrate (92%) than the 8% of primary care providers in our own survey. Per their study, most OBGYNs would order a semen analysis (92%), similarly in our study a majority of primary care providers also ordered a semen analysis (78%). Over half of OBGYNs in the Rothenberg study but only a small number of primary care providers in our study (9%) would evaluate for tubal patency. Rothenberg noted that general OBGYNs were more likely to refer a 38 year with primary infertility to subspecialists compared to a 29 year old. There is an obvious difference between primary care providers and general OBGYNs in regards to their evaluation and referral patterns in regards to infertility patients when comparing our study to Rothenberg’s [13]. This is likely due to the mandated OBGYN residency program curriculum to include adequate exposure to reproductive physiology and infertility to provide a practicing general OBGYN enough competencies in all aspects of the field of OBGYN.
The primary care providers in the entire health care system are extremely important in delivering primary gynecological care to our patients. Often and increasingly so in the current healthcare environment, they are the first line access to women and couples. Given that they are this first line, they have the opportunity to optimize education of patients regarding reproductive health and fertility. If properly equipped, they can also identify and execute early basic intervention and appropriate referral of the infertile patient.
The authors recognize that this survey was only seen by a limited number of primary care providers, and that this is likely a mere snap shot of what is practiced in this country. In a larger population and in different parts of the country, the results could be different or similar. The differences could be based on patient demographic as well as differences in training institutions. It would be interesting to send the survey to different parts of the country as well as the world and to compare the answers to the questions.
Based on the survey results, an education model that could be implemented during medical school or residency training may be beneficial for primary care providers that are interested in the diagnosis and initiation of the basic evaluation of the infertile couple.
References
- Eldein HN. Family physician’s attitude and practice of infertility management at primary care-Suez Canal University, Egypt. Pan Afr Med J. 2013; 15:106.
- Hassa H, Ayranci U, Unluoglu I, Metintas S, Unsal A. Attitudes to and management of fertility among primary health care physicians in Turkey: An epidemiological study. BMC Public Health. 2005; 5: 33.
- Ittner E, Himmel W., Kochen MM. German family physicians’ attitudes toward care of involuntarily childless patients. Fam Med. 2000; 32: 119-125.
- Weingarten MA, Reinitz A, Hart J. Attitudes to Primary-care Gynaecology among Family Physicians and Gynecologists in Israel. Scand J Prim Health Care.1992; 10: 36-41.
- Smith LF. The role of primary care in infertility management. Hum Fertil (Camb) 2003; 6: S9-S12.
- Definitions of infertility and recurrent pregnancy loss: a committee opinion. Fertil Steril. 2013; 99: 63.
- Diagnostic evaluation of the infertile female: a committee opinion. Fertil Steril. 2015; 103: e44-50.
- Lindsay TJ, Vitrikas KR. Evaluation and Treatment of Infertility. Am Fam Physician. 2015; 91: 308-314.
- Laopaiboon M, Lumbiganon P, Intarut N, Mori R, Ganchimeg T, Vogel JP, et al. Advance maternal age and pregnancy outcomes; a multi country assessment. BJOG. 2014; 1: 49-56.
- Female age-related fertility decline. Committee Opinion No. 589. The ACOG Committee on Gynecologic Practice. Fertil Steril. 2014; 101: 633.
- Homburg R. Clomiphene citrate -end of an era? A mini-review. Hum Reprod. 2005; 20: 2043-2051.
- Diamod MP, Legro RS, Coutifaris C, Alvero R, Robinson RD, Casson P, et al. Letrozole, Gonadotropin, or Clomiphene for Unexplained Infertility. N Engl J Med. 2015; 373:1230-1240.
- Rothenberg SS, Bhatte N, Nayak SR, Menke MN. Practice patterns of infertility evaluation and referral among general obstetrician-gynecologists within a large health system: a preliminary report. Fertil Steril. 2014; 102: e240-e241.