
Research Article
J Schizophr Res. 2014;1(1): 9.
Attachment Styles, Quality of Life and Service Satisfaction Outcomes in People with Schizophrenia in Israel
Ponizovsky AM1*, Arbitman M2, Baumgarten-Katz I2 and Grinshpoon A2
1Mental Health Services, Ministry of Health, Israel
2Sha'ar Menashe Mental Health Center, Hadera, Israel
*Corresponding author: Ponizovsky AM, Mental Health Services, Ministry of Health, 39 Yirmiyahu St, P.O. Box 1176, Jerusalem, 9446724, Israel
Received: July 09, 2014; Accepted: July 29, 2014; Published: July 31, 2014
Abstract
Aim: To test the hypothesized associations among satisfaction with psychiatric rehabilitation services, health-related quality of life (HRQoL), psychopathology and attachment styles in inpatients with schizophrenia.
Methods: One hundred-one patients with International Classification on Diseases, Tenth Edition (ICD-10) diagnosis of schizophrenia and duration of rehabilitation program no less than six months were recruited from the rehabilitation wards of the Sha'ar Menashe Mental Health Center, Hadera, Israel. The outcome variablesandattachment styleswere assessed with the standardized questionnaires, and psychopathology severity with the Positive and Negative Syndrome Scale (PANSS). Univariate and multivariate analyses were performed to examine the study hypotheses.
Results: Attachment anxiety, dissatisfaction with rehabilitation services and the severity of general psychopathology predicted poorer HRQoL, accounting for 8.7%, 13.9%, and 5.4%, respectively, of the total variance(R2=.30; Adjusted R2=0.26; F4,100=7.98, p<0.001). In turn, the HRQoL was the only predictor of service satisfaction, accounting for 17% of the variance (R2=.17; Adjusted R2=0.13; F4,101=3.95, p=<0.01).
Conclusion: The results confirmed the hypothesized association between HRQoL and satisfaction with rehabilitation services. Despite this relation, attachment anxiety predicted only poorer HRQoL and more severe general psychopathology, but not service dissatisfaction. The results could contribute to the development of innovative rehabilitation strategies to improve both HRQoL and service satisfaction among inpatients with schizophrenia.
Keywords: Attachment Patterns; Satisfaction with Services; Quality of Life; Psychopathology Severity; Schizophrenia
Abbreviations
SMI: Severe Mental Illness; HRQoL: Health-Related Quality of Life; MHC: Mental Health Center; ICD-10: International Classification of Mental and Behavioral Disorders, Tenth Edition; MHCSS-H: Mental Health Client Satisfaction Scale; Q-LES-Q: Quality of Life Enjoyment and Satisfaction Questionnaire-Short Form; RQ: Relational Questionnaire; PANSS: Positive and Negative Syndrome Scale; ANOVA: Analysis Of Variance.
Introduction
In recent decades, there is increasing interest in the systematic consideration of outcomes other than control of symptoms in the evaluation of long-term treatment effectiveness and rehabilitation for people with severe mental illness (SMI).Among others, satisfaction with health-related quality of life (HRQoL) and satisfaction with services are considered to be valuable outcome measures that contribute to the improvement of both quality of life and quality assurance procedures among clients of mental health centers (MHCs) [1,2]. Because many people with SMI have insecure attachment styles that are considered to be risk factors for development and persistence of psychopathology [3-9], we explored to what extent attachment styles are associated with satisfaction with rehabilitation services, HRQoL and severity of psychopathology among inpatients with schizophrenia.
The two recently published systematic reviews of the literature on attachment and psychosis [10,11] demonstrated clinical relevance of attachment style construct to development, course and treatment of psychosis: insecurely attached people have more severe positive, negative and affective symptoms [4], maladaptive coping strategies [12], showed poorer quality of therapeutic alliance [13] and engagement with services [14-15], and recovery style [16-18]. Clients attending MHCs are in contact with multiple professionals and may therefore develop attachments to psychiatric teams or services in general [19-20]. This tendency may be increased by recent mental health policies which allocate people to teams of staff rather than key workers [15]. Attachment to MHC in turn may influence the appraisal of satisfaction with the received service and be closely associated with users' HRQoL in general. A recent study [21] examined the extent to which individuals' appraisal of satisfaction with the received service was influenced by their own attachment style and found that clients with a more insecure attachment style indicated lower levels of attachment to services, independent of psychotic symptom severity. No analogical study has been conducted in Israel.
In this study we will focus on inpatient rehabilitation services for several reasons. First, these services provide a number of interventions to teach users social skills necessary for further daily living in the community and improving quality of their lives. The sense of attachment security facilitates engagement in exploration [22], whereas attachment insecurity impairs acquiring of the skills. Second, users of these services are separated from primary attachment figures for extended time periods and that alone may cause feeling of insecurity and activating their attachment needs. Under such conditions, only mental health personnel may play a role of attachment figures for rehabilitation service users [15,20,23]. Third, MHC users' attachment styles would affect their satisfaction with services and quality of their lives, if the severity of psychopathological symptoms could be controlled for [24].
Satisfaction with services is a subjective condition that results from the comparison between clients' expectations about health care provision and their actual experiences [25,26]. From the service perspective, satisfaction with service can be seen as a result of the ability of the service to provide a standard of care above a certain quality threshold, and the perception of each patient that the care received has been tailored to the patient's own problems [27]. By assessing client satisfaction, clinicians and health managers can learn the client's opinion regarding the services received, and also obtain a quality indicator of the centers' functioning [28]. Assessment of patients' satisfaction with MHCs has been recommended for improving the quality of services [29].
Clinical trials across many areas of medicine characteristically include HRQoL as an important outcome variable [30-33]. Several researchers have recommended that HRQoL be part of any outcome evaluation of treatment of patients with SMI [24,34,35]. A considerable body of studies [24,36,37] had shown that HRQoL in schizophrenia is substantially impaired, independent of stage of the illness, with positive, negative and depressive symptoms and side-effects of medication as well as dissatisfaction with social relationships as the major determinants of this impairment. Although several studies regarding HRQoL as the outcome variable in assessing effectiveness of treatment among people with SMI have been performed during the last decade in Israel [30-40], a survey addressing satisfaction with services along with HRQoL is lacking. Such information is needed to improve both quality assurance procedures and HRQoL of the MHCs' users.
The attachment theory proposes that attachment is the base upon which emotional health, social relationships, and one's worldview are built [22,41]. The ability to trust and form reciprocal relationships with the primary caregiver during the first two years of a child's life will affect the emotional health, security, and safety of the child, as well as the child's development and future interpersonal relationships [42]. Although there are different ways of conceptualizing adult attachment [43], based on the notion that attachment style can be determined by a person's model of self (positive or negative) and of others (positive or negative), Bartholomew and Horowitz [44] proposed a four-category attachment style model and this is the model used in this study. Specifically, individuals with a "secure" attachment style (self and other are both positive) are characterized by a sense of self-worth and a trust that others will be available and supportive in times of stress and adversity; they are comfortable seeking and expecting support from others. Individuals with a "preoccupied" attachment style (negative self, positive other) are preoccupied by attachment needs and depend on others for personal validation, acceptance, and approval. Those with "fearful" attachment (self and other both negative) regard others as uncaring and unavailable and themselves as unlovable. "Dismissing" individuals (positive self, negative other) remove themselves from others, regarding themselves as self-sufficient and invulnerable to abandonment by others.
Most investigators who use self-report measures of adult attachment style [43-45] agree that two primary dimensions are involved-attachment anxiety and attachment avoidance-and that “these two dimensions represent different ways of regulating the distress and insecurities resulting from a failure to find external or internal sources of comfort and support” [46]. The anxiety dimensionassesses the degree to which individuals worry about being rejected, abandoned, or unloved by significant others and reflects underlying negative self-model and positive other-model [44]. The avoidance dimensionevaluates the degree to which individuals limit intimacy and interdependence with others and reflects underlying positive self-model and negative other-model [44]. In adult attachment research, there is growing consensus that individual differences are best measured in terms of the attachment anxiety and avoidance dimensions that underlie the four attachment prototypes [46,47].
The present study aimed: 1) to evaluate satisfaction with inpatient psychiatric rehabilitation services and HRQoL outcomes among people with schizophrenia at a conventional state-funded MHC in Israel, and 2) to examine the relations between attachment styles and both outcomes, controlling for potentially confounding effects of psychopathology severity. We hypothesized that 1) satisfaction with services is positively related to life satisfaction; and 2) insecure attachment stylesare negatively related to satisfaction with services and quality of life, whereas positively to the current psychopathology.
Materials and Methods
Setting
The setting for this study was the state-funded Sha'ar Menashe Mental Health Center that is the greatest psychiatric institution in both Israel and Middle East. The center has 420 beds distributed as follows: 130 acute, 90 chronic, 35 geriatric, 40 rehabilitation and 125 maximum high security beds. The hospital serves a catchment area with a mixed Arab-Jewish, lower and middle-income population of 830,000.
Participants
One hundred-one patients from rehabilitation and partly chronic wards were recruited for this study during 2012 according to the followinginclusion criteria: 1) ICD-10 diagnosis of schizophrenia [48]; 2) duration of treatment no less than six months, and 3) sufficient comprehension skills to provide written informed consent for participation in the study. Patients with comorbid serious medical illnesses and organic brain syndromes were not enrolled.The rationale of the selection criteria was to create a homogeneous cohort of typical users of inpatient rehabilitation services. After explanation of the study aims and procedure all participants provided written informed consent for participating in the study as approved by the Institutional Review Boards for HumanStudies.
Measures
The main outcome variables were measured with the Mental ealth Client Satisfaction Scale [49,50], adapted for use with inpatient rehabilitation services, and Quality of Life Enjoyment and Satisfaction Questionnaire-Short Form [51]. The predictor variables were measured with the Relational Questionnaire [44] and the Positive and Negative Syndrome Scale [52].
Mental health client satisfaction scale
The MHCSS-H is a validated Hebrew version of the Charleston Psychiatric Satisfaction Scale [50]. This is self-report multidimensional questionnaire is designed to measure satisfaction with mental health services. Sixteen items describe five service domains (Availability/ Accessibility, Quality of care, Explanation/Participation, Staff's attitude, and Facilities conditions) of satisfaction, including two anchor items (“Overall quality of the care provided” and “Would you recommend this clinic to a friend or relative?”). Responses are rated on a 5-point Likert scale ranging from 1 (“very dissatisfied”) to 5 (“very satisfied”). For this sample, internal consistency of the MHCSS-H was excellent (Cronbach's alpha = 0.94) [50].
Quality of life enjoyment and satisfaction questionnaire
The Q-LES-Q is a self-report form composed of 16 items, each rated on a 5-point scale that indicates the degree of enjoyment or satisfaction experienced over the past week. A total score of 1 to 15 items is computed. The items evaluated each subject's satisfaction with: their physical health; social relations; ability to function in daily life; ability to get around physically; mood; family relations; sexual drive and interest; ability to work on hobbies, work, leisure time activities; economic status; household activities; living/housing situation; medication and overall sense of well-being. To avoid augmenting scores, global item 16, �life satisfaction and contentment over the last week', was not included in the total score. The Q-LES-Q was validated in Hebrew elsewhere [24]; for the present sample, Cronbach's alpha was 0.91.
Relational questionnaire
The RQ is used to assess adult attachment styles: they are described by 4 brief statements and participants are asked to endorse the statement that is most self-descriptive (they are described in the Introduction section). In addition to the categorical forcedchoice approach we also applied the dimensional approach, asking participants to indicate how much each description corresponded to their general relationship style. Responses were rated on a 7-point Likert-type scale ranging from 1 (“Not at all like me”) to 7 (“Very much like me”). Completing the forced-choice section first serves to counterbalance and minimize order effects when participants rank the degree to which each prototype characterizes them.The attachment anxiety dimension was calculated as (fearful plus preoccupied scores) minus (secure plus dismissing scores) and the attachment avoidance dimension was computed as (fearful plus dismissing scores) minus (secure plus preoccupied scores) [53]. The validity of this attachment classification has been demonstrated by its empirical relationships to self-concept and interpersonal functioning [44] and to psychological wellbeing and social functioning [54].
To ensure completion of the self-reported questionnaires, the researcher (MA) did read the items to the participants. In the end of the session, the researcher used the PANSS for assessing the severity of positive, negative and general psychopathological symptoms. Its 30 symptom items are scored from absent (1) to extreme problem (7).The Cronbach's a for the present sample was 0.70 for the positive scale, 0.92 for the negative scale, and 0.87 for both general psychopathology scale and PANSS as a total.
Statistical analyses
Pearson product moment correlations were calculated to test the relationships among all measures. To test our hypotheses, firstly, univariate analyses comparing intergroup measurements were performed using ANOVA with Tukey HSD post-hoc single comparisons. Then multiple regression analyses on linear models were performed to predict service satisfaction and quality of life outcomes from insecure attachment dimensions (anxiety and avoidance), controlling for the severity of positive, negative and general symptomatology. For all analyses, the level of statistical significance was established at p < .05. Statistical analyses were performed with SPSS version 17 for Windows (SPSS Inc., Chicago, IL) (Table 1).
Characteristic
n
%
Gender
Male
91
90.1
Female
10
9.9
RQ attachment styles
Secure
30
30.6
Fearful-avoidant
20
20.4
Preoccupied
11
11.2
Dismissing-avoidant
37
37.8
Mean
SD
Age at examination (yr.)
37.5
11.1
Age at first psychiatric contact (yr.)
23.3
7.2
Duration of disorder (yr.)
13.8
10.1
Number of hospitalizations
10.3
11.0
Duration of last hospitalization (mo.)
26.7
37.4
PANSS total score
63.8
12.6
Positivesyndrome
13.2
4.2
Negative syndrome
20.0
4.9
General psychopathology
30.5
5.8
Quality of life (Q–LES–Q)
3.73
.75
Satisfaction with services (MHCSS)
3.67
.75
RQ= the Relationship Questionnaire [44]
PANSS = the Positive and Negative Syndrome Scale [52]
Q–LES-Q = the Quality of Life Enjoyment Satisfaction Questionnaire[51]
MHCSS = Mental Health Client Satisfaction Scale [49]
Table 1: Basic characteristics of the sample (n=101).
Results
Sample characteristics
Basic sociodemographic and clinical characteristics of the participants show in Table 1. The vast majority of patients was men with the diagnosis of paranoid schizophrenia (ICD-10: F20.0) and typical age of onset in young adulthood. The severity of psychopathology, as measured by PANSS total and subscale scores, was moderate. Forced-choice one of the four RQ attachment styles resulted in 30 patients with secure, 20 patients with fearful-avoidant, 11 patients with preoccupied and 37 patients with dismissingavoidant patterns (Table 2).
Variable
A. Secure
(n=30)B. Fearful-avoidant(n=20)
C. Preoccupied
(n=11)D. Dismissing-avoidant(n=37)
ANOVA
(df=3,101)
F-valueTukey HSD post-hoc
comparisonsMean
SD
Mean
SD
Mean
SD
Mean
SD
Age (yr.)
35
7.8
35.5
11.2
39.6
13.1
39.1
12.1
1.12
A=B=C=D
Education (yr.)
11.5
1.8
9.7
3.8
10.9
2.7
10.8
2.8
1.64
A=B=C=D
Age at first psychiatric contact (yr.)
25.1
7.3
21.6
6
18.7
4.7
24.3
8
2.80*
A=B=D>C
Duration of disorder (yr.)
10.4
7
13.3
11.05
20.5
12.5
14.2
9.3
3.13*
A<C
Number of hospitalizations
7.1
9.5
9.8
8.3
20.3
19.7
10.2
8.9
4.12**
A=B=D<C
Duration of last hospitalization (mo.)
21.3
18.1
20
25.7
10.8
12.9
35.3
49.7
1.97
A=B=C=D
Q-LES-Q
3.9
0.7
3.5
0.9
3.6
0.5
3.69
0.6
1.11
A=B=C=D
MHCSS
3.8
0.8
3.8
0.8
3.6
0.4
3.6
0.6
0.5
A=B=C=D
PANSS, total score
59.3
8.7
68.2
11.1
62.6
10.2
63.5
13.4
2.5
A=B=C=D
POSITIVE syndrome
11.6
2.5
14.7
4.7
13.2
2.8
13.4
4.8
2.51
A=B=C=D
NEGATIVE syndrome
19.1
4.1
21
4.9
19.3
5.6
19.8
5
0.7
A=B=C=D
GENERAL psychopathology
28.6
4.06
32.5
4.9
30.2
4.6
30.1
6
2.32
A=B=C=D
a Q-LES-Q = the Quality of Life Enjoyment Satisfaction� uestionnaire (Endicott et al, 1993)
b MHCSS = Mental Health Client Satisfaction Scale� Pellegrin et al, 2001)
cPANSS = the Positive and Negative Syndrome Scale (Kay et al, 1987)
d RQ = the Relationship Questionnaire (Bartholomew & Horowitz, 1991)
*p <.05,� **� p<.01,� ***� p<.001
Table 2: Demographic and clinical characteristics, quality of life and satisfaction with services across the RQ attachment patterns.
Sample characteristics by attachment style
Table 2 presents and compares the sociodemographic and clinical characteristics, as well as MHCSS and Q-LES-Q mean scores across the four RQ attachmentstyles. ANOVA with post-hoc tests showed no significant differences in all variables studied, except for earlier onset (F=2.80, df=3, p<.05) and longer duration (F=3.13, df=3, p<.05) of the disorder in patients with the preoccupied attachment style versus securely attached patients, and a greater number of psychiatric admissions in those with preoccupied attachment compared to patients with other attachment styles (F=4.12, df=3, p<.01) (Table 3).
Variable
1
2
3
4
5
6
7
8
1. Attachment anxiety a
-
2. Attachment avoidance a
-.183
-
3. PANSS b total
.239*
-.263**
-
4. Positive syndrome b
.227*
-.215*
.753**
-
5. Negative syndrome b
.070
-.200*
.817**
.359**
-
6. General psychopathology b
.305**
-.231*
.919**
.589**
.650**
-
7. Q-LES-Q c
-.333**
.078
-.217*
-.066
-.140
-.314**
-
8. MHCSS d
-.069
.086
-.178
-.072
-.187
-.178
.389**
-
aRQ= the Relationship Questionnaire [44]
bPANSS = the Positive and Negative Syndrome Scale [52]
cQ-LES-Q = the Quality of Life Enjoyment Satisfaction Questionnaire [51]
dMHCSS = the Mental Health Client Satisfaction Scale [49]
Table 3: Correlation matrix for continuous variables (n=101).
Correlation analysis
Table 3 presents correlations among the parameters of interest. We found that satisfaction with services was positively and moderately correlated to HRQoL (r=·39, p< ·01), but not with other variables. Attachment anxiety was negatively correlated to HRQoL (r=–·33, p<·01) and positively to PANSS total score (r=·24, p<·05), positive syndrome (r=·23, p<·05) and general psychopathology (r=·31, p<·01) scores. Conversely, Attachment avoidance demonstrated significant negative associations with all PANSS subscale and total scores. In addition, a significant negative correlation between HRQoL and PANSS general psychopathology scores was noted (r=–·31, p<·01) (Table 4 and Figure 1).
Quality of life outcome
�
t-value (�=0)
p
Total % variance
accounting for
Predictors
Attachment anxiety
-.23
2.48
.015
8.7%
Satisfaction with services
.34
3.88
<.0001
13.9%
PANSS general psychopathology
-.38
2.75
.007
5.4%
Excluded variables
PANSS positive syndrome
.19
1.75
.083
--
Model properties: R2= 0.30; Adjusted R2=0.26; F(4,101)=7.98;� p < .0001
Satisfaction with services outcime
�
t-value (�=0)
p
Total % variance
accounting for
Predictors
Quality of life
.403
3.88
<.0001
17%
Excluded variables
-.065
-.034
.623
.286
.535
.755
--
--
PANSS general psychopathology
.054
.342
.733
--
Model properties: R2= 0.17; Adjusted R2=0.13; F(4,101)=3.95;� p = .003
aQ-LES-Q = the Quality of Life Enjoyment Satisfaction Questionnaire [51]
bRQ [44]
cMHCSS = Mental Health Client Satisfaction Scale [49]
dPANSS = the Positive and Negative Syndrome Scale [52]
Attachment anxiety
PANSS positive syndrome
Table 4: Regression models for predicting quality of lifea and satisfaction with servicesc from insecure attachment styles band psychopathology dimensionsd
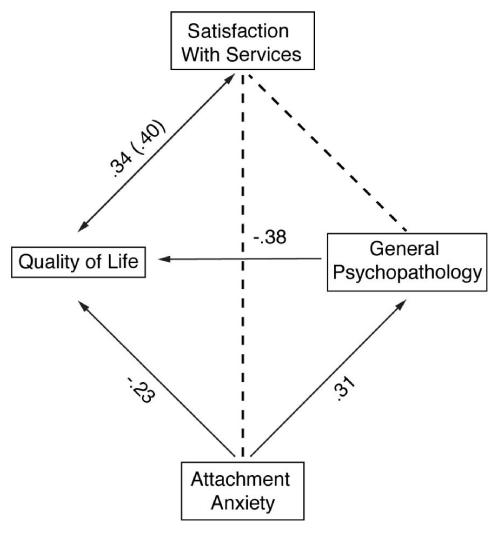
Figure 1: The relationships between attachment anxiety, general psychopathology, and service satisfaction and health-related quality of life. Standardized estimation β are shown.
Predicting HRQoL and service satisfaction
Table 4 summarizes the results of regression analyses testing our hypotheses about associations between attachment dimensions and satisfaction with HRQoL (model 1) and between attachment dimensions and service satisfaction (model 2), and controlling for the severity of psychopathological symptoms. In the first model, the HRQoL outcome was predicted by attachment anxiety, satisfaction with services and PANSS general psychopathology, which accounted for 8·7%, 13·9%, and 5·4% of the total variance, respectively(R2=·30; Adjusted R2=0·26; F4,101=7·98, p<0.001). In the second model, the service satisfaction was predicted by only HRQoL, accounting for 17% of the total variance (R2=.17; Adjusted R2=0.13; F4,101=3.95, p=<0.01). Figure 1 illustrates the obtained results.
Discussion
To our knowledge, this is the first study that examined associations among attachment styles, psychopathology, and satisfaction with inpatient rehabilitation services and quality of life among individuals with schizophrenia. The results confirmed our hypotheses only in part. As expected (hypothesis 1), there was a significant positive association between HRQoL and satisfaction with services. However, contrary to our assumption (hypothesis 2), only attachment anxiety was associated with HRQoL but not with service satisfaction, whereas attachment avoidance was not linked to either. The findings suggest that interventions reducing both attachment anxiety and general psychopathology could improve the users' HRQoL and thus satisfaction with rehabilitation services.
In the present study we used both dimensional and categorical approaches, each of which had an advantage resulting in specific findings. While the head-to-head comparisons of the attachment styles failed to find an association with both satisfaction with HRQoL and services, the dimensional approach revealed a significant negative association between attachment anxiety and HRQoL. The categorical approach, in turn, enabled revealing a positive association between the preoccupied attachment style and the indicators of the severe course of disorder (early onset, longer duration and numerous psychiatric admissions), whereas the current levels of positive, negative and general symptoms were comparable across the individual attachment styles. In contrast, the dimensional approach demonstrated the associations of attachment anxiety with the current levels of positive and general symptoms, whereas attachment avoidance correlated with all types of symptom severity.
Although we found a significant positive association between HRQoL and satisfaction with services and a negative associationbetween HRQoL and anxiety attachment as well, both anxiety and avoidance insecure dimensions were not directly linked to service satisfaction. The latter finding contrasts with Blackburn et al.'s study [21] which found an association between insecure attachment styles and poor attachment to mental health services. Our findings could be explained from the perspective of attachment-related affect regulation strategies [43,55]. According to this theory, people with anxiety attachment (preoccupied by attachment needs and dependent on others for personal validation, acceptance, and approval) use a hyperactivating strategy of affect regulation to reduce their distress in threatening situations by proximity seeking to an attachment figure. In the context of service satisfaction, it means that being more dependent on therapeutic relationships and more sensitive to any clues of neglect and abandonment, they are often dissatisfied with the relationships created in response to their engagement. Conversely, people with avoidant types of attachment over-regulate their affect and avoid relational situations that are likely to be distressing; attachment avoidance is associated with fear of intimacy and low levels of emotional involvement in close relationships [56-58]. Using affect regulation deactivating strategies, patients with avoidant attachment are more likely to have difficulties in engagement and developing a therapeutic alliance, in help seeking, and in adhering to treatment and services.
Although both dimensions of attachment insecurity (anxiety and avoidance) were significantly related to the current levels of psychopathology, the prototypical approach revealed that only the preoccupied attachment style was associated with the indicators of the severe course of the illness. The results lend support to previous findings which demonstrated that individuals with schizophrenia who have the preoccupied and fearful-avoidant attachment styles were most symptomatic and distressed [59], and had earlier onset of the illness and longer durations of psychiatric hospitalizations [5]. These findings are also consistent with studies that demonstrated the positive association of insecure attachment styles with emotional dysregulation and with symptoms of both depression and generalized anxiety in a non-clinical sample [60] and in "situational depression" [61] and schizophrenia, as well [61,62], suggesting that insecure attachment styles promote ineffective emotion regulation and increases the risk for these disorders. Interestingly, out of all the PANSS dimensions, only the current level of general psychopathology (i.e. mainly, depressive and anxiety symptoms) was a significant predictor of HRQoL (5.4% of the total variance) but not satisfaction with services. The findings suggest that although non-specific psychopathology and attachment anxiety play defined roles in HRQoL appraisal, their role in the user's subjective evaluation of satisfaction with inpatient services seems negligible.Interestingly, however, our predictors of HRQoL are consonant with the factors that Blackburn et al [21] found to be correlated with client attachment to mental health services. That study found that patients from psychiatric rehabilitation units with more insecure attachment styles and greater severity of depression demonstrated lower levels of attachment to services. Taken together, these findings lend support to the meaningful inter-correlation between HRQoL and satisfaction with services, which was found in our study.
Strengthens and limitations
The relatively large sample size enhances robustness of the study findings. The use of the complementary approaches to attachmentconceptualization (categorical vs. dimensional) appeared to be productive and enabled the important accessory findings. Although the overall sample size is reasonable, there are relatively small numbers of patients in each insecure group, which precluded controlling for other variables, and might impact on the validity of the findings of our inter-category comparisons. However, these findings were validated by regression analysis using the dimensional approach as a better way of investigating the associations among attachment, quality of life, service satisfaction and the severity of general psychopathology. Another limitation is that the study's participants were self-selected people with schizophrenia in inpatient rehabilitation setting and, hence, generalization of the study findings to people from other psychiatric settings and diverse populations should be considered with great caution.
Clinical implications
Our findings that insecure attachment dimensions are differentially linked to HRQoL and service satisfaction provides useful information for clinical interventions. For example, they suggest that if the desired outcome is to improve an individual's mental healthrelated quality of life, interventions fostering increased security could be useful for only anxiously attached patients. The simplest way to achieve this goal is reduction of general psychopathological symptoms (depression and anxiety) with antidepressant drug treatment. There are many other treatment options relevant to attachment styles and affect regulation (e.g.,cognitive-behavioral, interpersonal and individual therapies, stress management, enhancement of coping skills, etc.), a more nuanced discussion of which remain beyond the scope of the current study. If the patient scores high on attachment anxiety, lowering the general symptoms and raising HRQoL could indirectly result in more satisfaction with services received. Another possibility is therapeutic interventions focusing on improving the quality of interpersonal relationships that may have an indirect effect of increasing attachment security. A study that demonstrated a significant change from insecure to secure attachment style over the course of time-limited individual therapy [63] supports this therapeutic option. Proposed effects of oxytocin (a neurohypophysial hormone) on social emotions and relationships (increasing trust and reducing fear) in healthy samples [64] and individuals with schizophrenia [65,66] present a new treatment option, which warrants further investigation. In the framework of a cognitive interpersonal approach [67], identification of certain attachment styles could help in the choice of primary and secondary forms of therapy in early phases of the development of morbid processes. For example, a prospective study showed that attachment styles predicted improvement in pre-psychotic symptoms and functioning during six-month psychosocial need-adapted treatment among persons with at-risk mental states for psychosis [68]. Finally, knowledge of the patient's attachment style can predict recovery style and, hence, therapeutic outcome. For instance, it may help to understand why insecurely attached patients use sealing-over instead of integrating recovery strategies. As a previous study showed, �sealers' had a history of insecure attachment and vulnerable self-esteem and were unable to face up to the personal impact of a psychosis [16]. Understanding of the relationship between recovery style and engagement will be a step forward in designing interventions to enhance engagement with services [14].
In conclusion, the results confirmed the hypothesized association between HRQoL and satisfaction with rehabilitation services. However, attachment anxiety predicted dissatisfaction only with HRQoL This information could contribute to the development of innovative rehabilitation strategies to improve both HRQoL and service satisfaction among inpatients with schizophrenia.
References
- Rohland BM, Langbehn DR, Rohrer JE. Relationship between service effectiveness and satisfaction among persons receiving Medicaid mental health services.Psychiatr Serv. 2000; 51:248-250.
- Marwaha S, Johnson S, Bebbington P, Angermeyer MC, Brugha T, Azorin JM, et al. Correlates of subjective quality of life in people with schizophrenia: findings from the EuroSC study. See comment in PubMed Commons below J Nerv Ment Dis. 2008; 196: 87-94.
- Dozier M. Attachment organization and treatment use for adults with serious psychopathological disorders. Dev Psychopathol. 1990; 2: 47-60.
- Berry K, Barrowclough C, Wearden A. A review of the role of adult attachment style in psychosis: unexplored issues and questions for further research. See comment in PubMed Commons below Clin Psychol Rev. 2007; 27: 458-475.
- Ponizovsky AM, Nechamkin Y, Rosca P. Attachment patterns are associated with symptomatology and course of schizophrenia in male inpatients. See comment in PubMed Commons below Am J Orthopsychiatry. 2007; 77: 324-331.
- Bifulco A, Moran PM, Ball C, Lillie A. Adult attachment style. II: Its relationship to psychosocial depressive-vulnerability. See comment in PubMed Commons below Soc Psychiatry Psychiatr Epidemiol. 2002; 37: 60-67.
- Van Buren A, Cooley EL. Attachment styles, view of self, and negative affect. North Am J Psychol. 2002; 4:417-430.
- Picken AL, Berry K, Tarrier N, Barrowclough C. Traumatic events, posttraumatic stress disorder, attachment style, and working alliance in a sample of people with psychosis. See comment in PubMed Commons below J Nerv Ment Dis. 2010; 198: 775-778.
- Ponizovsky AM, Levov K, Schultz Y, Radomislensky I. Attachment insecurity and psychological resources associated with adjustment disorders. See comment in PubMed Commons below Am J Orthopsychiatry. 2011; 81: 265-276.
- Gumley AI, Taylor HE, Schwannauer M, MacBeth A. A systematic review of attachment and psychosis: measurement, construct validity and outcomes. See comment in PubMed Commons below Acta Psychiatr Scand. 2014; 129: 257-274.
- Korver-Nieberg N, Berry K, Meijer CJ, de Haan L. Adult attachment and psychotic phenomenology in clinical and non-clinical samples: a systematic review. See comment in PubMed Commons below Psychol Psychother. 2014; 87: 127-154.
- MacBeth A, Schwannauer M, Gumley A. The association between attachment style, social mentalities, and paranoid ideation: an analogue study. See comment in PubMed Commons below Psychol Psychother. 2008; 81: 79-93.
- Owens KA, Haddock G, Berry K. The role of the therapeutic alliance in the regulation of emotion in psychosis: an attachment perspective. See comment in PubMed Commons below Clin Psychol Psychother. 2013; 20: 523-530.
- Tait L, Birchwood M, Trower P. Predicting engagement with services for psychosis: insight, symptoms and recovery style. See comment in PubMed Commons below Br J Psychiatry. 2003; 182: 123-128.
- Arbuckle R, Berry K, Taylor JL, Kennedy S. Service user attachments to psychiatric key workers and teams. See comment in PubMed Commons below Soc Psychiatry Psychiatr Epidemiol. 2012; 47: 817-825.
- Drayton M, Birchwood M, Trower P. Early attachment experience and recovery from psychosis. See comment in PubMed Commons below Br J Clin Psychol. 1998; 37 : 269-284.
- Tait L, Birchwood M, Trower P. Adapting to the challenge of psychosis: personal resilience and the use of sealing-over (avoidant) coping strategies. See comment in PubMed Commons below Br J Psychiatry. 2004; 185: 410-415.
- Ringer JM, Buchanan EE, Olesek K, Lysaker PH. Anxious and avoidant attachment styles and indicators of recovery in schizophrenia: associations with self-esteem and hope. See comment in PubMed Commons below Psychol Psychother. 2014; 87: 209-221.
- Goodwin I. The relevance of attachment theory to the philosophy, organization, and practice of adult mental health care. See comment in PubMed Commons below Clin Psychol Rev. 2003; 23: 35-56.
- Catty J, Cowan N, Poole Z, Ellis G, Geyer C, Lissouba P, et al. Attachment to the clinical team and its association with therapeutic relationships, social networks, and clinical well-being. See comment in PubMed Commons below Psychol Psychother. 2012; 85: 17-35.
- Blackburn C, Berry K, Cohen K. Factors correlated with client attachment to mental health services. See comment in PubMed Commons below J Nerv Ment Dis. 2010; 198: 572-575.
- Bowlby J. A secure base: Clinical applications of attachment theory. New York, NY: Basic Books, 1988.
- Berry K, Drake R. Attachment theory in psychiatric rehabilitation: in orming clinical practice. AdvPsychiatr Treat. 2010; 16: 308-315.
- Ritsner MS, Arbitman M, Lisker A, Ponizovsky AM. Ten-year quality of life outcomes among patients with schizophrenia and schizoaffective disorder II.Predictive value of psychosocial factors.Qual Life Res. 2012; 21: 1075-1084.
- Sitzia J, Wood N. Patient satisfaction: a review of issues and concepts. See comment in PubMed Commons below Soc Sci Med. 1997; : 1829-1843.
- Crow R, Gage H, Hampson S, Hart J, Kimber A, Storey L, et al. The measurement of satisfaction with healthcare: implications for practice from a systematic review of the literature. See comment in PubMed Commons below Health Technol Assess. 2002; 6: 1-244.
- Ruggeri M, Lasalvia A, Bisoffi G, Thornicroft G, Vàzquez-Barquero JL, Becker T, et al. Satisfaction with mental health services among people with schizophrenia in five European sites: results from the EPSILON Study. See comment in PubMed Commons below Schizophr Bull. 2003; 29: 229-245.
- Trujols J, Garijo I, Siñol N, del Pozo J, Portella MJ, Pérez de los Cobos J. Patient satisfaction with methadone maintenance treatment: the relevance of participation in treatment and social functioning. See comment in PubMed Commons below Drug Alcohol Depend. 2012; 123: 41-47.
- Mental Health Commission. Your Views of Mental Health Inpatient Services: Inpatient Survey 201, University of Ulster. 2012.
- Wenger NK, Mattson ME, Furberg CD, Elinson J. Assessment of quality of life in clinical trials of cardiovascular therapies. See comment in PubMed Commons below Am J Cardiol. 1984; 54: 908-913.
- Spilker B, Molinek FR Jr, Johnston KA, Simpson RL Jr, Tilson HH. Quality of life bibliography and indexes. See comment in PubMed Commons below Med Care. 1990; 28: DS1-77.
- Katschnig H, Freeman H, Sartorius N, & editors. Quality of Life in Mental Disorders, 2nd edn. New York: Wiley. 2005.
- Bottomley A, Aaronson NK; European Organisation for Research and Treatment of Cancer. International perspective on health-related quality-of-life research in cancer clinical trials: the European Organisation for Research and Treatment of Cancer experience. See comment in PubMed Commons below J Clin Oncol. 2007; 25: 5082-5086.
- Kulkarni J, de Castella AR, Filia KM, Filia SL, Marston N, Montgomery W, et al. Australian Schizophrenia Care and Assessment Programme: real-world schizophrenia: outcomes. Aust NZ J Psychiatry. 2007; 41: 969-979.
- Green CA, Polen MR, Janoff SL, Castleton DK, Wisdom JP, Vuckovic N, et al. Understanding how clinician-patient relationships and relational continuity of care affect recovery from serious mental illness: STARS study results. PsychiatrRehabil J. 2008; 32: 9-22.
- Bow-Thomas CC, Velligan DI, Miller AL, Olsen J. Predicting quality of life from symptomatology in schizophrenia at exacerbation and stabilization. See comment in PubMed Commons below Psychiatry Res. 1999; 86: 131-142.
- Malla A, Payne J. First-episode psychosis: psychopathology, quality of life, and functional outcome. See comment in PubMed Commons below Schizophr Bull. 2005; 31: 650-671.
- Kravetz S, Faust M, Dasberg I. A comparison of care consumer and care provider perspectives on the quality of life of persons with persistent and severe psychiatric disabilities. See comment in PubMed Commons below Psychiatr Rehabil J. 2002; 25: 388-397.
- Grinshpoon A, Naisberg Y, Weizman A. A six-month outcome of long-stay inpatients resettled in a hostel. See comment in PubMed Commons below Psychiatr Rehabil J. 2006; 30: 89-95.
- Roe D, Werbeloff N, Gelkopf M. Do persons with severe mental illness who consume the psychiatric rehabilitation basket of services in Israel have better outcomes than those who do not? See comment in PubMed Commons below Isr J Psychiatry Relat Sci. 2010; 47: 166-170.
- Fonagy P, Steele M, Steele H, Moran GS, Higgitt A. The capacity for understanding mental states: The reflective self in parent and child and its significance for security of attachment. Infant Ment Health J. 1991; 12: 201-218
- O'Connor TG, Rutter M. Attachment disorder behavior following early severe deprivation: extension and longitudinal follow-up. English and Romanian Adoptees Study Team. See comment in PubMed Commons below J Am Acad Child Adolesc Psychiatry. 2000; 39: 703-712.
- Shaver PR, Mikulincer M. Attachment-related psychodynamics. See comment in PubMed Commons below Attach Hum Dev. 2002; 4: 133-161.
- Bartholomew K, Horowitz LM. Attachment styles among young adults: a test of a four-category model. J PersSoc Psychol. 1991; 61: 226-244.
- Fraley RC, Waller NG, Brennan KA. An item response theory analysis of self-report measures of adult attachment. J PersSoc Psychol. 2000; 78: 350-365.
- McWilliams LA, Asmundson GJ. The relationship of adult attachment dimensions to pain-related fear, hypervigilance, and catastrophizing. See comment in PubMed Commons below Pain. 2007; 127: 27-34.
- Fraley RC, Waller NG. Adult attachment patterns: A test of the typological model. In J. A. Simpson & W. S. Rholes (Eds.), Attachment theory and close relationships. New York: Guilford Press. 1998; 77-114.
- World Health Organization: The ICD-10 Classification of Mental and Behavioural Disorders. Diagnostic Criteria for Research.Geneva,WHO. 1993.
- Pellegrin KL, Stuart GW, Maree B, Frueh BC, Ballenger JC. A brief scale for assessing patients' satisfaction with care in outpatient psychiatric services. See comment in PubMed Commons below Psychiatr Serv. 2001; 52: 816-819.
- Elisha D, Khawaled R, Radomislensky I, Ponizovsky AM. Validation of the Charleston Psychiatric Outpatient Satisfaction Scale - Hebrew Version adapted for use in Israel. Open J Psychiatry. 2012; 2: 141-146.
- Endicott J, Nee J, Harrison W, Blumenthal R. Quality of Life Enjoyment and Satisfaction Questionnaire: a new measure. See comment in PubMed Commons below Psychopharmacol Bull. 1993; 29: 321-326.
- Kay SR, Fiszbein A, Opler LA. The positive and negative syndrome scale (PANSS) for schizophrenia. See comment in PubMed Commons below Schizophr Bull. 1987; 13: 261-276.
- Kelley ML, Nair V, Rawlings T, Cash TF, Steer K, Fals-Stewart W. Retrospective reports of parenting received in their families of origin: relationships to adult attachment in adult children of alcoholics. See comment in PubMed Commons below Addict Behav. 2005; 30: 1479-1495.
- Diehl M, Elnick AB, Bourbeau LS, Labouvie-Vief G. Adult attachment styles: their relations to family context and personality. See comment in PubMed Commons below J Pers Soc Psychol. 1998; 74: 1656-1669.
- Cassidy J, Kobak RR.Avoidance and its relationship with other defensive processes.In J. Belsky& T. Nezworski, editors. Clinical implications of attachment. Hillsdale, NJ: Erlbaum. 1988; 300-323.
- Dozier M, Lee S. Discrepancies between self- and other- report of psychiatric symptomatology: Effects of dismissing attachment strategies. Dev Psychopathol. 1995; 7: 217-226.
- Fraley RC, Shaver PR. Adult attachment and the suppression of unwanted thoughts. See comment in PubMed Commons below J Pers Soc Psychol. 1997; 73: 1080-1091.
- Mikulincer M, Horesh N. Adult attachment style and the perception of others: the role of projective mechanisms. See comment in PubMed Commons below J Pers Soc Psychol. 1999; 76: 1022-1034.
- Ponizovsky AM, Vitenberg E, Baumgarten-Katz I, Grinshpoon A. Attachment styles and affect regulation among outpatients with schizophrenia: relationships to symptomatology and emotional distress. See comment in PubMed Commons below Psychol Psychother. 2013; 86: 164-182.
- Marganska A, Gallagher M, Miranda R. Adult attachment, emotion dysregulation, and symptoms of depression and generalized anxiety disorder. See comment in PubMed Commons below Am J Orthopsychiatry. 2013; 83: 131-141.
- Ponizovsky AM, Drannikov A. Contribution of attachment insecurity to health-related quality of life in depressed patients. See comment in PubMed Commons below World J Psychiatry. 2013; 3: 41-49.
- MaBeth A, Gumley A, Schwannauer M, Fisher R. Attachment states of mind, mentalization, and their correlates in a first-episode psychosis sample. See comment in PubMed Commons below Psychol Psychother. 2011; 84: 42-57.
- Travis LA, Bliwise NG, Binder JL, Horne-Moyer HL. Changes in clients' attachment styles over the course of time-limited dynamic psychotherapy.Psychother. 2001; 38: 149-159.
- Churchland PS, Winkielman P. Modulating social behavior with oxytocin: how does it work? What does it mean? See comment in PubMed Commons below Horm Behav. 2012; 61: 392-399.
- Macdonald K, Feifel D. Oxytocin in schizophrenia: a review of evidence for its therapeutic effects. See comment in PubMed Commons below Acta Neuropsychiatr. 2012; 24: 130-146.
- De Berardis D, Marini S, Iasevoli F, Tomasetti C, de Bartolomeis A, Mazza M, et al. The role of intranasal oxytocin in the treatment of patients with schizophrenia: a systematic review. See comment in PubMed Commons below CNS Neurol Disord Drug Targets. 2013; 12: 252-264.
- Gumley A, Schwannauer M. Staying well after psychosis: A cognitive interpersonal approach to recovery and relapse prevention. Chichester: John Wiley & Sons Ltd. 2005.
- Quijada Y, Tizón JL, Artigue J, Kwapil TR, Barrantes-Vidal N. Attachment style predicts 6-month improvement in psychoticism in persons with at-risk mental states for psychosis. See comment in PubMed Commons below Early Interv Psychiatry. 2012; 6: 442-449.