Case Report
Austin Surg Case Rep. 2016; 1(1): 1002.
Metastatic Melanoma Presenting as Intussusception in an 80-Year-Old Man: A Case Report
Raymond B* and English G
Department of Surgery, University of Pittsburgh Medical Center, USA
*Corresponding author: Raymond Benjamin, Department of Surgery, University of Pittsburgh Medical Center-Hamot, Erie PA, USA
Received: September 23, 2015; Accepted: November 25, 2015; Published: January 20, 2016
Abstract
Metastatic melanoma is one of the most common metastatic malignancies to the gastrointestinal tract; however, its diagnosis is rarely encountered in the premortem setting. Intussusception or the invagination of one continuous segment of bowel within one another is a rare entity in adults as compared to children. In adult patients presenting with small bowel obstructions, intussusception represents only approximately 1% of these cases. Despite excellence in imaging modalities in detection of intussusception, only 90% of the causative etiologies are found, of which, 65% are caused by a neoplastic process. This is an uncommon clinical presentation of metastatic melanoma as the causative etiology of intussusception in an 80-year-old male who was evaluated in the emergency department with signs and symptoms of bowel obstruction.
Keywords: Intussusception; Melanoma; Metastatic melanoma
Case Presentation
An 83-year-old male with a past medical history significant for hypertension, coronary artery disease status post myocardial infarction and percutaneous stent placement, arthritis, cataracts, gastroesophageal reflux disease, chronic anemia, and melanoma presented to the emergency department at a tertiary care facility with chief complaint of worsening left lower quadrant abdominal pain, increased abdominal distention, nausea, and multiple episodes of non-bloody, non bilious emesis. The patient had been following with the gastrointestinal service at the same institution regarding chronic anemia requiring multiple outpatient blood transfusions as well as intravenous iron therapy. Within six months of presenting to the emergency department, the patient had been evaluated with esophagogastroduodenoscopy, push enteroscopy, and colonoscopy which were negative for identification of significant pathology resources of bleeding. As part of the emergency department workup, the patient underwent a non-contrast CT scan of the abdomen and pelvis which indicated a small bowel intussusception with a transition point in the left lower quadrant (Figure 1). Surgical consultation was requested and the patient was taken emergently to the operating room.
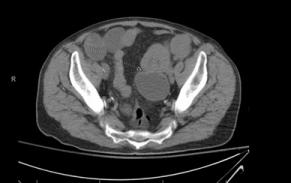
Figure 1: Non contrast CT scan Abdomen/Pelvis with small bowel
intussusception with transition point in the LLQ (indicated by arrow).
In regards to the patient’s melanoma, he was originally diagnosed in July of 2006 at which time the patient underwent a wide local left forehead skin excision by a local dermatologist which revealed a focus of melanoma, unfortunately further pathology regarding this lesion is unavailable. The patient later developed two addition areas of suspected melanoma approximately six months later on the left forehead; one of such lesions was suspected to be local recurrence of the previously resected lesion. Patient was taken to the operating room where two wide local excisions were performed, sentinel node mapping and biopsy, scalp flap and advancement flap. The two skin lesions were positive for metastatic melanoma with Breslow thickness of 1.8mm and 2mm, Clark classification 3. Three lymph nodes were identified during the mapping processes all of which were negative for malignancy.
Operative findings
Patient was taken emergently to the operating room where an exploratory laparotomy was performed. After entering the peritoneal cavity, a small amount of adhesions was encountered which were then freed using bovie electrocautery. There was an obvious transition point of the small bowel at the level of the jejunum. There was evidence of dilated proximal small bowel and decompressed bowel distal to this transition point. At the transition point, there was a palpable mass present as well as lymphadenopathy in the adjacent mesentery which was also resected with the surgical specimen. No additional lesions were identified in either the large or small bowel which was examined its entirety. The intussusception was resected with gross margins and primary anastomosis was performed.
Pathology
An 8.5cm segment of small intestine was resected which showed an area of intussusception. The specimen was opened to revealed a partially exophytic polypoid yellow-orange mass in the mid aspect region of the bowel in the area of intussusception measuring 5.5cm in greatest dimension causing the telescoping of the bowel segment. Sectioning reveals apparent extension into the muscular wall and close to the serosal surface. Seven peri-intestinal lymph nodes were negative for metastatic tumor. Microscopically, predominant spindle cell morphology with high cellularity, mitotic activity, and moderate pleomorphic was identified. Tumor shows immunohistochemical expression of S100. Additional melanoma markers including Melan A and HMB-45 were negative. Despite the negative additional tumor markers, the overall impression, given clinical history of melanoma, the morphology and the immunoreactivity for S100, the diagnosis is compatible with metastatic melanoma.
Discussion
Intussusception, or the invagination or telescoping of a segment of continuous bowel, is a common presentation in the pediatric population with an upwards of 80% resolving without surgical management and vast majority are idiopathic. The same cannot be said of that of the adult population. Intussusception in adults typically arises secondary to an endoluminal mass which functions as a lead point for the intussusception, of which 65% are secondary to a neoplastic process [1]. Of the neoplastic processes found as a lead points for intussusception, 15% can be further differentiated as malignant, most of which are metastatic [1]. Malignant melanoma being the most common etiology. Despite this, there are few cases of small bowel intussusceptions due to metastatic melanoma in medical literature. The majority of these are identified intraoperative as opposed to radiographical identified in abdominal pain workup [2,3].
Melanoma has a high metastatic potential, of which metastatic melanoma to the GI tract accounts for one third of all metastatic disease to the GI tract [4]. The small bowel represents the most common site of metastatic disease in the gastrointestinal tract for melanoma [5]. The recorded incidence of gastrointestinal metastases of melanoma in an autopsy series reaches up to 60% [6]. However, only 2% to 4% of patients with malignant melanoma are clinically diagnosed with GI metastases [5,7]. Symptoms typically include gastrointestinal bleeding, obstruction, abdominal pain, nausea and vomiting, and weight loss [8]. The risk factors for malignant melanoma with spread to the GI tract include superficial spreading melanoma, axial primary tumor, a Clark level III or IV, high degree of histologic, regression, ulceration, and high mitotic rate [2,9,10]. The interval between the diagnosis of primary malignant melanoma and clinical manifestation of GI metastases ranges from two to 180 months [11,12]. This should prompt a careful clinical follow-up of patients with a history of highrisk melanoma who present with GI symptoms.
We report an uncommon clinical presentation in adults, intussusception, with an underlying pathology, metastatic melanoma to GI tract, which is a rarely diagnosed premortem. This diagnosis, although a rare condition should be considered in the differential diagnosis in any patient who presents with gastrointestinal symptoms and a history of melanoma.
References
- Agha FP. Intussusception in adults. American Journalism Review. 1986; 146: 527-531.
- Dogan M, Ozdemir S, Gecim, Erden E, Icli F, Turk. Intestinal malignant melanoma presenting with small bowel invagination: a case report. Journal of Gastroenterology. 2010; 21: 439-42.
- Mucci T, Long W, Witkiewicz A, Mastrangelo MJ, Rosato EL, Berger AC. Metastatic melanoma causing jejunal intussusception. Journal of Gastrointestinal Surgery. 2007; 11: 1755-1757.
- Washington K, McDonagh D. Secondary tumors of the gastrointestinal tract: surgical pathologic findings and comparison with autopsy survey. Modern Pathology. 1995; 8: 427-433.
- Blecker D, Abraham S, Furth EE, Kochman ML. Melanoma in the gastrointestinal tract. The American Journal of Gastroenterology. 1999; 94: 3427-3433.
- Wysocki WM, Komorowski AL, Darasz Z. Gastrointestinal metastases from malignant melanoma: report of a case. Surgery Today. 2004; 34: 542-546.
- Manola J, Atkins M, Ibrahim J, Kirkwood J. Prognostic factors in metastatic melanoma: a pooled analysis of eastern cooperative oncology group trials. Journal of Clinical Oncology. 2000; 18: 3782-3793.
- Rampone B, Roviello F, Marrelli D, Giovanni De Marco, Rossi S, Corso G, Cerullo G, Pinto E. Late recurrence of malignant melanoma presenting as small bowel intussusception. Digestive Diseases and Sciences. 2006; 51: 1047-1048.
- Schuchter LM, Green R, Fraker D. Primary and metastatic diseases in malignant melanoma of the gastrointestinal tract. Current Opinion in Oncology. 2000; 12: 181-185.
- Liang KV, Sanderson SO, Nowakowski GS, Arora AS. Metastatic malignant melanoma of the gastrointestinal tract. Mayo Clinic Proceedings. 2006; 81: 511-516.
- Berger AC, Buell JF, Venzon D, Baker AR, Libutti SK. Management of symptomatic malignant melanoma of the gastrointestinal tract. Annals of Surgical Oncology. 1999; 6: 155-160.
- Oddson TA, Rice RP, Seigler HF, Thompson WM, Kelvin FM, Clark WM. The spectrum of small bowel melanoma. Gastrointestinal Radiology. 1978; 3: 419-423.