Case Report
Austin Surg Case Rep. 2016; 1(1): 1003.
Wandering Gallstones (Gallbladder Fistulae)
Pillay Y*
Department of General Surgery, Prince Albert Parkland Health Region, Canada
*Corresponding author: Yagan Pillay, Department of General Surgery, Prince Albert Parkland Health Region, Saskatchewan, Canada
Received: December 12, 2015; Accepted: January 18, 2016; Published: January 20, 2016
Abstract
Wandering gallstones Gallbladder fistulae are a rare surgical entity and usually present with complications of the fistulae such as gallstone ileus or bowel perforation. They usually present in an elderly patient cohort with extensive medical morbidities. This case report looked at two types of gallbladder fistulae and their outcomes. In both cases, the complications of the fistula was managed and not the fistula itself. The intestinal obstruction for the gallstone ileus as well as the gallstone coleus was surgically treated in both cases which necessitated a laparotomy on both occasions. The gallstone ileus had an enterotomy and gallstone removal. This was closed primarily. The gallstone coleus could not be primarily repaired after stone extraction and a Hartman`s resection was performed. In both cases the patient had a stormy post-operative course but did eventually make a complete recovery. One patient developed septic shock while the other developed a pulmonary embolus. This required an intensive care admission for both patients. Gallbladder fistulae are often managed conservatively and the gallbladder is usually treated surgically at a later date. In many case reports the gallbladder itself is never dealt with and this may be detrimental to patient care as an occult malignancy will need to be actively excluded. This can occur in 2-6 percent of cases. Cholecystitis or cholangitis can also occur in 5-10 percent of cases.
Keywords: Gallbladder fistulae; Cholecystoduodenal; Cholecystocolonic gallstone ileus; Gallstone coleus
Introduction
Gallbladder fistulae are quite rare with a reported incidence of 0.9% [1]. This case report discusses two types of fistulae, cholecystoduodenal and cholecystocolonic as well as their subsequent management. Both patients presented with intestinal obstruction and no signs or symptoms of biliary tract disease. In both cases surgery was performed for the complications of the fistulae while the fistulae themselves were conservatively managed.
Case 1: Cholecystoduodenal fistula
An 85 year old Caucasian female was referred with intestinal obstruction of five days duration. She had nausea and bile stained vomiting. Clinically she was stable and not jaundiced. She had abdominal pain and distention but no signs of rebound or guarding. Her rectal exam was normal with no obvious masses. She had a fracture of the right hip that was treated with Open Reduction and Internal Fixation (ORIF) and developed the intestinal obstruction while convalescing in hospital. She had no medical history and her surgical history was significant only for the ORIF. Her blood results were normal and her Computerized Tomography (CT) scan showed a large gallstone in the distal ileum causing intestinal obstruction (Figure 2). Her gallbladder also showed multiple large gallstones and a cholecystoduodenal fistula (Figure 1). She signed an informed consent for an exploratory laparotomy. At surgery a large gallstone was removed from the distal ileum through an enterotomy and primary closure (Figure 3). Her gallbladder had ruptured with an empyema in the right upper quadrant which was drained and all her gallstones removed (Figure 4). A Blake drain was placed in the right subhepatic space to drain the gallbladder. The gallbladder was not removed and the cholecystoduodenal fistula could not be clearly identified due to excessive inflammation and fibrosis. Her recovery was quite eventful and required an Intensive Care Unit (ICU) admission with Total Parenteral Nutrition (TPN). She was also put on antibiotics and inotropic support. She eventually made a complete recovery and was sent home after one month. The ruptured gallbladder was never treated surgically and four years later she has completely recovered with no further episodes of abdominal pain or jaundice.
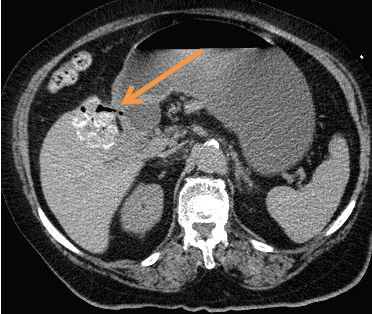
Figure 1: CT scan axial view showing the cholecystoduodenal fistula (orange
arrow).
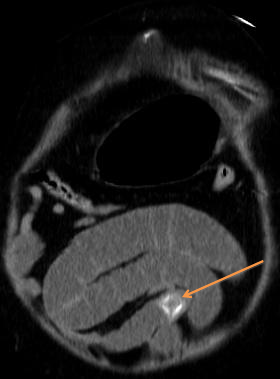
Figure 2: CT scan coronal view of the gallstone ileus causing intestinal
obstruction (orange arrow).
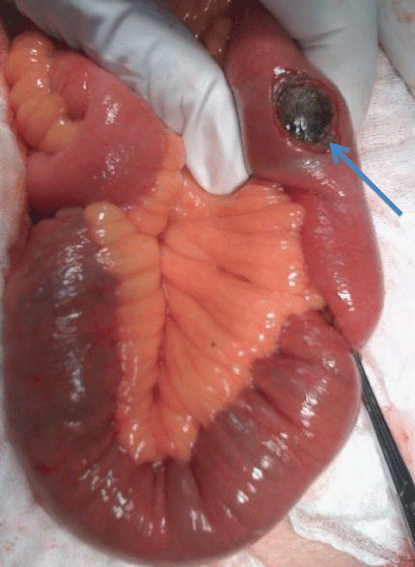
Figure 3: Enterotomy showing the gallstone in the distal ileum (blue arrow).

Figure 4: Gallstones removed from ruptured empyema gallbladder.

Figure 5: Ileal gallstone removed. The gallstone was 3 X 2 cm and faceted.
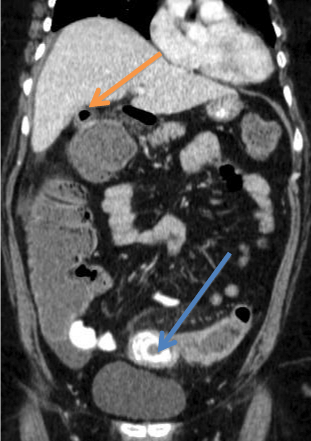
Figure 6: CT scan coronal view showing pneumobilia (orange arrow)and
large gallstone coleus, 4 x 3 cm in the sigmoid colon(blue arrow). Case 2:
Cholecystocolonic fistula.
Case 2: Cholecystocolonic fistula
A 57 year old Caucasian female was referred from a rural hospital with intestinal obstruction of three days duration. This was initially managed conservatively due to her previous abdominal surgery. Her blood results showed an elevated leukocyte count and she was treated empirically with antibiotics. She had no medical history and her surgical history indicated 2 previous caesarean sections. Clinically she remained stable with no signs of jaundice. The abdominal examination showed tympanic bowel with no obvious masses. She had no signs of rebound tenderness or guarding. The rectal exam was normal with no obvious masses. Failure of conservative management necessitated a CT scan which showed a large gallstone in the sigmoid colon causing an obstruction as well as a cholecystocolonic fistula between the gallbladder and the hepatic flexure of the colon (Figure 7). An initial attempt was made in the operating room to remove the gallstone with a sigmoidoscope but this was unsuccessful. An informed consent was taken for an exploratory laparotomy. Intraoperatively she had an intestinal obstruction at the
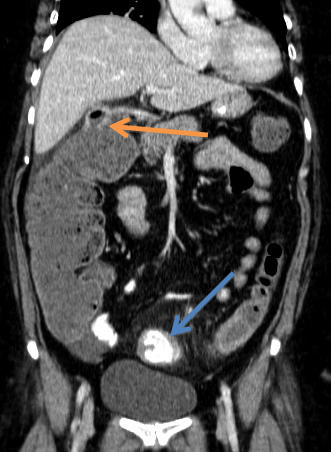
Figure 7: CT scan coronal view showing cholecystocolonic fistula between
the gallbladder and hepatic flexure of the colon (orange arrow). The large
gallstone coleus can also be seen (blue arrow) in the sigmoid colon.
rectosigmoid junction (Figure 8). The gallstone was removed through a colotomy. A primary repair was not feasible as the colon appeared ischaemic and friable. A Hartman`s resection was performed instead. The cholecystocolonic fistula was managed conservatively. Her postoperative recovery was slow and complicated by a pulmonary embolus that was medically managed. She was eventually discharged home two weeks later, once she had been taught stoma management. A year later she developed a parastomal hernia which is currently being managed conservatively. To date she has developed no abdominal pain or jaundice.
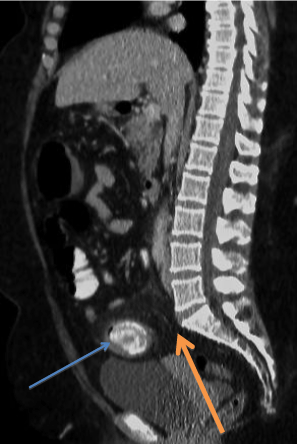
Figure 8: CT scan sagittal view showing the impacted gallstone (blue arrow)
in the rectosigmoid junction at the level of the sacral promontory (orange
arrow).
Discussion
Gallbladder fistulae are a rare complication of cholelithiasis. They occur in 0.9 percent of patients undergoing biliary tract surgery [1]. The three common sites are cholecystoduodenal, cholecystocolonic and cholecystogastric.
70 percent of the fistulae are cholecystoduodenal and 20 percent cholecystocolonic [1]. Costi et al in a review of the English literature reported only 231 cases of cholecystocolonic fistulae between 1950 and 2006 [2]. The pathophysiology arises due to inflammation of the gallbladder and a contiguous organ resulting in fistula formation [3]. A second theory postulates an impacted gallstone at Hartman`s pouch which erodes into an adjacent organ [3].
Management of the fistula depends on the patient presentation and entails one of the following; (1) enterotomy and stone extraction; (2) enterotomy and open cholecystectomy; (3) bowel resection, fistula closure and open cholecystectomy [4,5].
Enterotomy and stone extraction is the commonest described technique as more than half the fistulae close spontaneously once the distal obstruction is removed. The major risk factor is an undiagnosed cholangiocarcinoma with a prevalence of between 2-6 % [4,6]. Recurrent gallstone ileus can also occur with an incidence of 5-8% [6]. The commonest problem is that of recurrent Cholecystitis with an incidence of 10 % and cholangitis with an incidence of 5% [5,7].
The major controversy entails management of the untreated gallbladder. This may not be possible at the index surgery especially in the face of extensive comorbidity in an elderly patient cohort. The gallbladder will need to be dealt with surgically at another time. Five percent of patients who underwent lithotomy alone go on to develop biliary symptoms which includes malignancy [4,7]. Diagnostic imaging plays a key role in preoperative diagnosis. X-rays can show pneumobilia and the Ultrasound (US) often shows gallstones in the intestine. Computerised Tomography (CT) scan remains the gold standard for diagnosing the rigler triad (i.e. pneumobilia, small bowel obstruction and gallstones in the right iliac fossa) [8,9].
In both reported cases the fistula was managed conservatively and to date neither patient has developed any biliary complications.
The first patient is now 90 years old and remains asymptomatic. Given her age it was decided to manage her conservatively after a discussion with her and her family. The second patient has also remained asymptomatic but has developed a parastomal hernia that is currently being managed conservatively. In conversations with the patient we have decided to remove the gallbladder in the event we reverse her colostomy. The parastomal hernia will be repaired at the same time.
Conclusion
The diagnosis of a gallbladder fistula is often a late one with attendant increases in both morbidity and mortality. CT scan remains the gold standard for diagnosis. The degree of surgical intervention is often influenced by the patient`s clinical condition at the time of admission.
The management of the fistula complication remains the mainstay of treatment and the gallbladder fistula itself is often treated on an ad hoc basis.
References
- Glenn F, Mannix H Jr. Biliary enteric fistula. Surg Gynecol Obstet. 1957; 105: 693-705.
- R. Costi, Randone B, Violi V, Scatton O, Sarli L, Soubrane O, et al. “Cholecystocolonic fistula: facts and myths. A review of the 231 published cases,” Journal of Hepato-Biliary-Pancreatic Surgery. 2009; 16: 8-18.
- Yeung YP, Ah Chong K, Chung CK, Chun AYW: Biliary papillomatosis: report of seven cases and review of English literature. J HepatobiliaryPancreat Surg. 2003; 10: 390-395.
- Halabi WJ, Kang CY, Ketana N, Lafaro KJ, Nguyen VQ, Stamos MJ, et al. Surgery for Gallstone Ileus: A Nationwide Comparison of Trends and Outcomes. Ann Surg. 2013; 37: 2782-2790.
- Kasahara Y, Umemura H, Shiraha S, Kuyama T, Sakata K, Kubota H. Gallstone ileus. Review of 112 patients in the Japanese literature. Am J Surg. 1980; 140: 437-440.
- Hayes N, Saha S. Recurrent gallstone ileus. Clin Med Res. 2012; 10: 236-239.
- Clavien PA, Richon J, Burgan S, Rohner A. Gallstone ileus. Br J Surg. 1990; 77: 737-742.
- Katz DS, Yam B, Hines JJ, Mazzie JP, Lane MJ, Abbas MA. Uncommon and unusual gastrointestinal cause of the acute abdomen: computed tomographic diagnosis. Semin Ultrasound CT MR. 2008; 29: 386-398.
- Ripolles T, Miguel-Dasit A, Errando J, Morote V, Gomez-Abril SA, Richart J. Gallstone ileus: Increased diagnostic sensitivity by combining plain film and ultrasound. Abdom Imaging. 2001; 26: 401-405.