Research Article
Austin Surg Case Rep. 2017; 2(1): 1015.
Research on Application of Nickel-Titanium Shape Memory Alloy Compression Anastomosis Clip (CAC) in Advanced Cancer Intestinal Obstruction Shunt (Anastomosis)
Zhi-feng Xu¹, Liyun Xu¹ and Chengfei Zhao²*
¹Department of Surgery, First Affiliated Hospital, Nanjing Military Region Fuzhou General Hospital, China
²Pharmaceutical and Medical Technology College, Putian University, China
*Corresponding author: Chengfei Zhao, Pharmaceutical and Medical Technology College, Putian University, China
Received: April 28, 2017; Accepted: May 22, 2017; Published: May 29, 2017
Abstract
Purpose: To appraise the security and effectiveness of a new type nickeltitanium shape memory alloy CAC for the advanced cancer intestinal obstruction shunt (anastomosis).
Method: From April, 2006 to March, 2008, 41 patents suffering advanced cancer intestinal obstruction who need the small intestine or ileocolon bypass surgery are divided into two groups randomly. The CAC group performs the small intestine bypass or ileocolon bypass surgery with the CAC; and the manual suture group performs that with the Manual Suture Method. Observe any complication related to the intestinal anastomosis during and after the surgery, as well as the time for passage of gas by anus and efflux time.
Result: The difference of intestinal anastomosis time between the two groups has the statistics significance (P<0.05). Each group has a case of death, which is irrelevant to the surgery. No anastomotic fistula case occurs in the CAC group after surgery, but 2 cases in the manual suture group. The difference between the two groups has the statistics significance (P<0.05)A case of incisional infection occurs in the CAC group after surgery, and 5 such cases in the manual suture group. The difference between the two groups has the statistics significance (P<0.05); No anastomotic stoma obstruction occurs in both the two groups after the surgery. The difference of time for passage of gas by anus between the two groups has no statistics significance (P>0.05). All CACs used by the CAC group are discharged from the body in 10-18d after the surgery.
Conclusion: The application of CAC in advanced cancer intestinal obstruction anastomosis is safe and reliable, as well as easy to operate, which can release the obstruction to improve living quality.
Keyword: Malignancy; Intestinal obstruction; Bypass anastomosis; Compression anatomosis clip; Manual suture
Introduction
The advanced cancer intestinal obstruction is one of the common syndrome for tumor of abdomen and pelvis. For the extensive lesion of tumor as well as surgery anamnesis and intraperitoneal chemotherapy etc., the intestinal obstruction often occurs in many parts of body requiring the surgery treatment. The nickel-titanium shape memory alloy CAC (compression anastomosis clip) is a newtype intestinal anastomosis device in recent years, which has been successfully applied to the alimentary canal anastomosis for clinic laparotomy or video-assisted surgery both home and abroad, and has forming standard operation method [1-5]. Based on the successful clinic application of CAC in gastro jejunostomy, our section further applies the CAC to perform the small intestinal bypass or ileocolon bypass surgery for 20 cases of advanced cancer intestinal obstruction. The report is as following.
Information and Method
Information
From April 2006 to March 2008, our section treated 41 cases of advanced cancer intestinal obstruction. During the surgery, we found that their advanced tumor had been infiltrated and cannot be cut off, which needs bypass anastomosis at the near end of obstruction and far end of ansa intestinalis. They are divided into compression anastomosis clip (CAC) group of 20 cases and manual suture group of 21 cases randomly with the envelope method. The CAC group performs the small intestine bypass or ileocolon bypass surgery with the CAC; and the manual suture group performs that with the Manual Suture Method. The differences of age, sex, weight, illness composition and function status (KPS) between the two groups all have no statistic significance (Table 1). All sufferers agree to sign the Informed Consent Form (ICF).
Item
the group of CAC (20 case)
the group of (21case)
P value
Age(year)
55.8?13.6
57.5?11.2
>0.05
sex [(men/female) [case]
14/6
13/8
>0.05
Weight (kg)
56.3?7.9
55.8?12.6
>0.05
KPS evaluate
50?10
50?10
>0.05
Disease
>0.05
Gastric cancer
8
10
Carcinoma of colon
5
4
Ovarian carcinoma
4
3
Pancreatic cancer
2
1
Cervical carcinoma
1
2
Table 1: The clinical data of 41 patients (x ± s).
The CAC used by this institute is a double-ring device containing oval Nickel-Titanium memory-Shape alloy in diameter of 30×8mm (Figure 1), provided by the Niti Alloys Technologies, Ltd, Israel. The nickel-titanium alloy ring is molded in high temperature, and cooled in 00C icy brine for 20~30s. At that time, it becomes soft to open in an angle of 30°~40°. It gets back to the clipping status after heating under body heat to form the compression anastomosis with the pressure of 400g/cm².

Figure 1: Nitinol pressure consistent folder.
Method
Both the two groups were treated with bypass anastomosis surgery. The manual suture group performed the small intestine sideto- side anastomosis or ileocolon side-to-side anastomosis with the manual suture method. The surgery makes the proximal intestine of tumor and the intended anastomotic intestine overlapped for 10cm. The seromuscular layer of the two intestinal loops was oversewed for 4-5cm on the mesentery surface at 1.0cm place away from the middle line of vertical axle. The two sections of intestinal wall were cut open completely along the middle line of neutral axis up to the intestinal cavity. The contents in the cavity of proximal intestine were sucked up by vacuum extractor, and then the back wall of cut intestinal wall was interlockingly oversewed with absorbable thread continuously and completely. The front wall was oversewed by inverting suture continuously and completely. The seromuscular layer of front wall was oversewed with 1# silk suture, with the two external angles embedded in half pouch. The CAC group performed the small intestine sideto- side anastomosis or ileocolon side-to-side anastomosis with CAC. Firstly, the cancerous proximal intestine section was clipped with intestinal clamp, and arranged relatively paralleling to the distal small intestine (or ileum, colon), with about 5cm overlapped each other. The two intestine sections were oversewed by a stitch with 1# silk suture; the two ansa intestinalis were cut open respectively in a 5mm notch with electrotome. The small notch was intended to be used for anastomosis (Figure 2). The CAC device was cooled in icy water for 20s, and then pushed to the blade of clamp holder. The first time of cocking made the anastomosis clip reaches the open position. The anastomosis clip was placed into the intestinal cavity through the small notch on ansa intestinalis; the second time of cocking made the anastomosis clips closed and retract, and then third time of cocking was performed. The two layers of intestinal wall clamped between the two clips were cut-out by the cutting blade inner the clamp holder to form temporary channel for the contents of intestine passing anastomotic stoma. After that, the last cocking was performed to separate the clamp holder and ring clip. The clamp holder was removed, with the ring clip held in the anastomotic intestine section (Figure 3). Then, the opening was confirmed by the tip of a bend clip forceps, and enlarged properly. The 5mm cutting notch on ansa intestinalis was oversewed by inverting suture completely with 3-0 absorbable thread, and then embedded by adding seromuscular layer. The intestinal clamp was released, and the retention suture was cutoff. As the final step for the both groups, the mesentery hiatus between the ansa intestinalis was oversewed, the abdominal drain was placed by the side of anastomotic stoma, and the abdomen was closed.
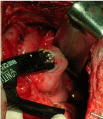
Figure 2: Application nitinol compression anastomosis clip to the small
intestine anastomosis.
Statistics
The SPSS 11.5 software was used for the statistic analysis, with the data expressed by x ± s, and the compare means proved by t.
Results
The difference of intestinal anastomosis time between the two groups has the statistics significance (P<0.05). No anastomotic fistula case occurs in the CAC group after surgery, but two cases in the manual suture group. The difference between the two groups has the statistics significance (P<0.05); A case of incisional infection occurs in the CAC group after surgery, and 5 such cases in the manual suture group. The difference between the two groups has the statistics significance (P<0.05); No anastomotic stoma obstruction occurs in both the two groups after the surgery. The difference of time for passage of gas by anus between the two groups has no statistics significance (Table 1). During the perioperative period 2 cases of death occurred. A case of CAC group died of pulmonary embolism in the second day after surgery and a case of manual suture group died of pulmonary infection in the fifth day after surgery. Both the two cases of death have nothing with the surgery operation. In the CAC group, the 3d abdomen X-ray detection shows that all CAC devices are holding the place after surgery (Figure 3). The CAC devices were discharged together with dejection in 10~18 days after the surgery [5], sufferers discharged the CAC before leaving the hospital, and remaining 14 sufferers discharged at home; we visited them randomly in 2 months after surgery. All of them had no syndrome such as infection, intestinal obstruction, stenosis etc. The gastrointestinal contrast in 2 months after surgery confirmed that no stenosis on the anastomotic stoma, with smooth and complete mucous membrane.
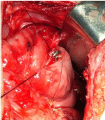
Figure 3: Nitinol compression anastomosis clip retained in the intestine.
Discussion
The incidence of the advanced cancerous intestinal obstruction is about 3% among all tumors, which is highest in digestive tract cancer and gynecological neoplasm±s. According to the literature report, the incidence of vicious intestinal obstruction is 5%~42% in the progressive-phase ovarian cancer, and is 4%~24% in the progressivephase colorectal cancer [6,7]. If the obstruction cannot be mitigated in 24~48 hr after the non-surgery treatment, or, the symptom increases or even the peritonitis occurs during the directly observed therapy, it should be treated with surgery in time. When the obstructed part is difficult to remove, such as the tumor spreads towards the peripheral tissues widely or the conqlutination is too wide to strip however, no necrosis occurs in the intestinal canal, the bypass anastomosis can be done by separating the distal and proximal intestine to eliminate the obstruction [8].
The compression anastomosis is a new type of technology. The clinical application of CAC on colon anastomosis was firstly completed in Israel [9], and became mature in recent years. The CAC device is made of memory metal nickel-titanium alloy, with the special features of changing conformation together with the temperature. The mechanism is similar to the Murphy button and biofragmentable ring of previous intestinal compression anastomosis. It causes the local necrosis of intestinal wall for the event and cosistent intensive pressure directly on tissue of intestinal wall. Once the intestinal wall tissues die completely, the CAC will run into the intestinal cavity and discharge together with the dejection. The concrescence of intestinal wall occurs at the same time with tissue necrosis. Finally, an even and unified compression anastomotic stoma is formed. However, the Murphy button and biofragmentable ring have the disadvantages such as inconsistent pressure, small inner diameter, high price etc [10,11].
The differences between the CAC and manual suture in the advanced cancerous intestinal obstruction bypass anastomosis are: (1) During the CAC operation, the two anastomotic ansa intestinalis were cut open respectively only in 5mm notch to place the CAC device. The device stays in the intestinal canal temporarily and will be discharged together with the dejection. In addition, the CAC adopts almost “no touch” operation. In the process of compression anastomosis, the two layers of intestinal wall clamped between the two clips were cut-out by the cutting blade inner the clamp holder to form temporary channel for the contents of intestine passing anastomotic stoma. It needs no decompression in intestinal canal, which prevents the pollution of contents in canal and reduce the infection. While in the manual suture, the intestinal canal is open completely, and it requires the decompression. Therefore, the possibility of pollution and incidence of incisional infection are increased. (2) After the CAC compression anastomosis, the mucosa covers the edge to from a complete, smooth, even and consistent anastomotic stoma. The manual suture forms a new rough cut on the anastomotic stoma, where the restenosis is possible. (3) Performing bypass anastomosis with CAC is easily handled, without high requirement to the technique of manual suture. In addition, the anastomosis period is reduced obviously. The two groups have no difference in the respects of enterocinesia recovery and food in taking time after surgery; while, the manual suture is complicated to operate, with obvious dropsy due to intestine dilatation inflammation. In addition, the anastomotic leak is very possible if the skill of manual suture is not so exquisite.
During the application of CAC in advanced cancer intestinal obstruction anastomosis, we summarized the following: (1) before the anastomosis, only a stitch fixing is needed at the cutting place of two ansa intestinalis instead of 2~3 acus at the membrane edge and side wall of involutory system. Make the two ansa intestinalis interlay each other for 5cm by the hand for the location of anastomosis clip. (2) After the anastomosis clip was placed and the clamp holder was removed, the opening was confirmed by the tip of a bend clip forceps, and enlarged properly to prevent the no cutting, incomplete cutting and too narrow cutting notch of the anastomosis clip. (3) The cutting notch was oversewed by inverting suture completely with 3-0 absorbable thread, and then embedded by adding seromuscular layer. Even if the anastomosis clip was oversewed, the absorbable thread can come off after broken up, and make sure the smooth and flat anastomotic stoma without foreign matters remaining after comingoff of anastomosis clip.
Regarding the question whether CAC causes early or delayed casting-off and intestinal obstruction, the domestic research by Jiang Zhiwei [12] and Wang Jianping has shown that: all oval CACs in diameter of 3cm can be discharged safely from the body through ileocecal valve after the surgery, without hazard of intestinal obstruction. In addition, the result of research shows that, the time for discharging CAC is averagely the eleventh to fifteenth days after the surgery. The research proved that, application of CAC in advanced cancer intestinal obstruction anastomosis is worth of publicity for its security and effectiveness. Due to the limited cases of this group, the experience about nickel-titanium shape memory alloy CAC in advanced cancer intestinal obstruction anastomosis needs further accumulation.
References
- Lee HY, Woo JH, Park SY, et al. Intestinal Anastomosis by Use of a Memoryshaped Compression Anastomosis Clip (Hand CAC 30): Early Clinical Experience. J Korean Soc Coloproctol. 2012; 28: 83-88.
- Oida T, Kawasaki A, Mimatsu K, et al. Sutureless compression anastomosis with a biofragmentable anastomosis ring. Hepatogastroenterology. 2011; 58: 1445-1449.
- Giessler GA, Fischborn GT, Schmidt AB. Clampless anastomosis with an intraluminal thermosensitive gel: first application in reconstructive microsurgery and literature review. J Plast Reconstr Aesthet Surg. 2012; 65: 100-105.
- Chun J, Lee D, Stewart D, Talcott M, et al. Comparison of the compression anastomosis ring (EndoCAR) with a circular stapled anastomosis in a porcine model. Surg Innov. 2011 ; 18: 235-240.
- Hua S, Xiong L, Wen Y, et al. Safety and efficacy of gastrointestinal anastomosis with nickel titanium compression anastomosis clip. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2011; 36: 351-354.
- Myers SR, Rothermel WS, Shaffer L. The effect of tissue compression on circular stapler line failure. Surg Endosc. 2011; 25: 3043-3049.
- Hur H, Kim HH, Hyung WJ, et al. Efficacy of NiTi Hand CAC 30 for jejunojejunostomy in gastric cancer surgery: results from a multicenter prospective randomized trial. Gastric Cancer. 2011; 14: 124-129.
- Zhang D, Zheng C, Song C. A modified method of using laparoscopic compression anastomosis clip for gastrointestinal anastomosis. Minim Invasive Ther Allied Technol. 2010; 19: 350-354.
- Vlasov AA, Vazhenin AV, Plotnikov VV, et al. Application of compression equipment using the “form memory” effect and super-elasticity of titanium nickelide in surgery for rectal cancer. Vopr Onkol. 2010; 56: 169-171.
- Park P, Leveque JC, La Marca F, et al. Dural closure using the U-clip in minimally invasive spinal tumor resection. J Spinal Disord Tech. 2010; 23: 486-489.
- Liu PC, Jiang ZW, Zhu XL, et al. Compression anastomosis clip for gastrointestinal anastomosis. World J Gastroenterol. 2008;14: 4938-4942.
- Li XX, Zheng CZ, Yin K, et al. Application of laparoscopic compression anastomosis clip for laparoscopic gastrointestinal anastomosis. Zhonghua Wei Chang Wai Ke Za Zhi. 2008; 11: 228-230.