Case Report
Austin Surg Case Rep. 2018; 3(1): 1022.
Inflammatory Stenosis of Ascending Colon: Differential Diagnosis between Granulomatous Disorders
Altomare M1*, Armiraglio L2, Casieri R2, Gjoni E2, Carsenzuola V2 and Scandroglio I2
1Resident in General Surgery, University of Milan, Milan, Italy
2Department of General Surgery Hospital of Busto Arsizio, Busto Arsizio, Italy
*Corresponding author: Altomare M, Resident in General Surgery, University of Milan, Milan, Italy
Received: January 10, 2018; Accepted: January 24, 2018; Published: January 31, 2018
Abstract
Background and Goal: Crohn’s disease (CD) and Tuberculosis (TB) are granulomatous disorders that could affect the intestinal tract with similar clinical, radiological and endoscopic findings [1-2]. TNF-α antagonists are monoclonal antibodies directed against Tumor Necrosis Factor alpha (TNF- α) cytokine with important role in inflammatory activity of disease [3]. This immunosuppressive therapy is one of the major therapeutic alternatives for CD but it may be complicated by several possible infections, as reactivation of a latent TB. An increasing incidence of CD in countries where TB continues to be highly prevalent [4-5] has increased the necessity for a clearer understanding of their comparative pathology and differentiating features. Because clinical-endoscopic signs cannot certainly establish the diagnosis, the use of Polymerase Chain Reaction (PCR) to reveal the DNA of Mycobacterium from biopsy tissue seems to represent the gold standard method [6-7] even if present a small percentage of false negative. The presence of Koch bacilli (BK) at microscopic exam is rare (35-60%) [8].
The histopathological examination of segmental biopsies in affected and non-affected colonic mucosa or definitive pathological examination after surgery may be faithful. Whereas older studies indicated that most patients had coexisting pulmonary TB, recent studies indicate pulmonary involvement in fewer than 50% of patients.
Recent article from Seo et al show that the misdiagnosis rate between CD and Intestinal TB (ITB) is still high, especially in case of ITB initially misdiagnosed as CD [9].
Keywords: Tuberculosis; Crohn’s disease; liver tests; Granulomatous disorders
Case Presentation
We present a case of 36 years old woman investigated in the emergency department because of intermittent abdominal pain in Right Iliac Fossa (RIF) associated with distension of the abdomen and nausea. The clinical report reveals a history of diarrhea, weight loss in the last six months and appendectomy performed 3 months before. Histological exam of appendix resulted suspicious for Crohn’s disease (Figure 1-2). In addition the patient reported close contact with TB affected patient (her mother) in the last year. The blood tests reveal poorly inflammatory index (CRP 2.11mg/dl) and a mild impairment of liver tests (AST 53 UI/L, ALT 60UI/L, ALP 279 U/L, ϒ-GT 129 UI/L). Furthermore serology reveals a positive QuantiFERON-Tb Gold test that confirmed the positivity of Mantoux reaction. Coproculture and urinoculture were negative for BK.
Colonoscopy characterized stenosis of right colon with severe inflammatory response suggestive for Crohn’s Disease (Figure 3-4). A total-body CT scan performed has shown thickness and oedema of the last tract of ascending colon that involved part of ileum. In addiction paracolic and lateral neckcaseous lymphadenitis is described (Figure 5-6). We perform Fine Needle Aspiration Cytology (FNAC) on lateral neck nodes (Figure 7) but Ziehl-Neelsen staining methods and RT-PCR resulted negative.
Right hemicolectomy has been performed in order to resolve the acute obstruction. The postoperative course was regular. The definitive histopathological examination revealed the presence of granulomatous inflammation with typical granulomas with localized caseous necrosis properties of TB (Figure 8-9). The Lowenstein-Jensen culture was positive for KB after 8th week.
The patient underwent anti-TB therapy with resolution of symptoms. The endoscopic control after 4 months describes normal results of right hemicolectomy without any sign of inflammation.
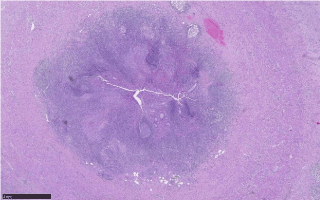
Figure 1:
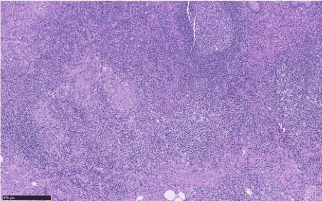
Figure 2:
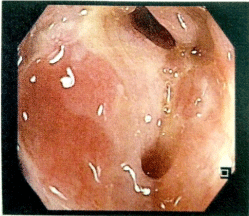
Figure 3:
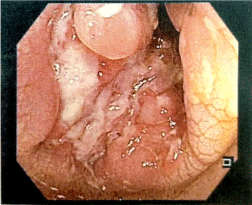
Figure 4:
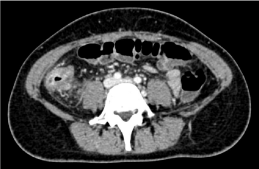
Figure 5:
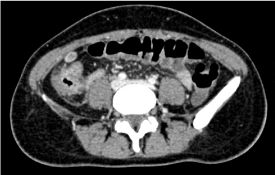
Figure 6:
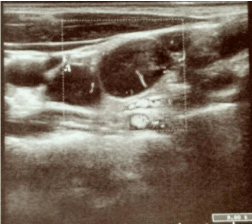
Figure 7:
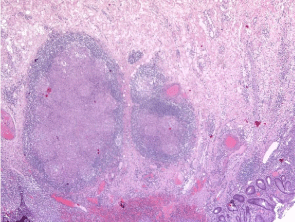
Figure 8:
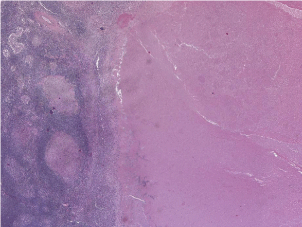
Figure 9:
Conclusion
Intestinal TB and CD could show similar clinical, radiological and histopathological findings6; differential diagnosis could be difficult especially in areas with high prevalence of TB such as Asia and Africa. Histopathological examination and/or segmental colonic biopsies are fundamental to define correct diagnosis. Reduce the misdiagnosis rates is one of the most important goal in order to start correct therapy and management as soon as possible. A multidisciplinary approach is fundamental.
References
- Pulimood B, Peter S, Ramakrishna B, Chacko A, Jeyamani R, Jeyaseelan L, et al. Segmental colonscopic biopsies in the differentiation of ileocolic tuberculosis from Crohn’s disease. J of Gastr and Hepatol. 2005; 20: 688-696.
- Das K, Puri S, Puri AS. Gastrointestinal: Multiple colonic strictures caused by tuberculosis. J of Gastr and Hepatol. 2006; 21: 476.
- Hommes DW, Oldenburg B, van Bodegraven AA, van Hogezand RA, de Jong DJ, Romberg-Camps MJ, van der Woude J, et al. Guidelines for treatment with infliximab for Crohn’s disease. Neth J Med. 2006; 64: 219-229.
- Pai CG, Khandige GK. Is Crohn’s disease rare in India? Indian J Gastroenterology. 2000; 19: 17-20.
- Ouyang Q. Inflammatory bowel disease in China. J of Gastr and Hepatol. 2000; 15: S25.
- Gan HT, Chen YQ, Ouyang Q, Bu H, Yang XY. Differentation between intestinal tuberculosis and Crohn’s disease in endoscopic biopsy specimens by polymerase chain reaction. Am J Gastroenterol. 2002; 97: 1446-1451.
- Amarapurkar DN, Patel ND, Amarapurkar AD, Agal S, Baigal R, Gupte P. Tissue polymerase chain reaction in diagnosis of intestinal tuberculosis and Crohn’s disease. J Assoc. Physician India. 2004; 52: 863-867.
- Chatzicostas C. Koutroubakis IE, Maria Tzardi, Maria Roussomoustakaki, Panagiotis Prassopoulos, Elias A Kouroumalis. Colonic tuberculosis mimicking Crohn’s disease: Case report. BMC Gastroenterol. 2002; 2: 10.
- Seo H, Seohyun Lee, Hoonsub So, Donghoi Kim, Seon-Ok Kim, Jae Seung Soh, et al. Temporal trend in the misdiagnosis rates between Crohn’s disease and intestinal Tubercolosis. World J Gastroenterol. 2017; 23: 6306-6314.