
Case Report
A Case Report. Austin J Surg. 2015; 2(7): 1078.
Intramucosallipoma Causing Iliocecal Intussusception in a Patient with Cutaneous Lipomas: A Case Report
Brook M¹, Licata L² and Lindsey DE²*
¹Deparment of Medicine, University of Ohio State, USA
²Department of Surgery, University of Ohio State, USA
*Corresponding author: David E Lindsey, Department of Surgery, University of Ohio State, Room 634, 395 W. 12th Avenue, Columbus, Ohio, 43210, USA
Received: September 15, 2015; Accepted: December 11, 2015; Published: December 14, 2015
Abstract
Introduction: Intussusceptions in adults is rare occurrence and benign lesions such as lipomas are an especially rare cause.
Presentation of Case: This is a case of a 32-year-old man with a history of cutaneous lipomas presenting with small bowel obstruction due to intussusception with a lipoma lead point.
Discussion: Close to 50% of bowel lesions causing intussusception in adults are due to malignant disease. The standard treatment for intussusception in adults is resection. Attempted reduction prior to resection can limit the amount of bowel needing to be removed; however seeding of malignancy is a feared complication. A family or personal history of cutaneous and systemic conditions causing benign tumors can help determine whether a benign etiology is likely and reduction can be safely performed.
Conclusion: Clinical clues from history and physical exam can help determine whether a benign etiology is likely and whether resection prior to reduction should be attempted.
Keywords: Llipoma; Intussusception; Bowel obstruction
Introduction
Intussusception is defined as the telescoping of one segment of the gastrointestinal tract into another. Intussusception in adults is a rare cause of bowel obstruction accounting for approximately 1% of cases [1]. While the majority of causes of intussusception in children are deemed to be idiopathic, in adults 90% of the cases are the result of a pathogenic process [2,3].
The most likely lead points in adults include benign and malignant tumors, inflammatory lesions, post-operative adhesions, and Meckel’s diverticula [3-5].
Lipomas are third most common primary benign tumor of the gastrointestinal tract [6]. A lipoma is a benign soft tissue tumor made of fat. The majority of gastrointestinal lipomas are found within in the colon, and 90% of them are sub mucosal [7]. A lipoma is an uncommon cause of intussusception but because of their intramural location can serve as a lead point.
As intussusception in adults is a fairly rare phenomenon and often has a nonspecific presentation, clinical suspicion must be high for the diagnosis to be made. We report a case of iliocecal intussusception in a patient with a history of cutaneous lipomas.
Presentation of Case
A 32-year-old male with a history of multiple cutaneous lipomas presented to the emergency department with 4 days of worsening abdominal pain, nausea, and vomiting. He had a history of multiple excised lipomas and one biopsied with pathology revealing “fatty tissue.” Family history revealed multiple relatives with lipomas. The patient’s vital signs were within normal limits on admission and initial labs demonstrated a normal WBC and lactate. His exam was significant for a soft, mildly tender abdomen, with pain worst over the epigastrium, with no peritoneal signs. Multiple lipomas were palpable over the abdominal wall and a fecal occult blood test was positive. A CT scan done in the emergency department demonstrated ileocolonic intussusception without focal fluid collections or free air (Figure 1). The patient was initially treated non-operatively with nasogastric tube decompression, bowel rest, and IV fluids. His symptoms progressed to obstipation with bilious effluent from his NG tube. A follow up acute abdominal series was done which demonstrated findings suggestive of small bowel obstruction and he was taken to the operating room. A diagnostic laparoscopy was performed and an attempted laparoscopic reduction of intussusception was unsuccessful. The surgery was then converted to open. The colon was visualized with a non-reducible dark mass apparent inside. An iliocectomy with ileocolonic anastomosis was performed and intraoperative findings demonstrated an ileocecocolic mass lead point with necrotic small bowel trapped in the cecum (Figures 2-4). Pathology revealed benign submucosal lipoma.
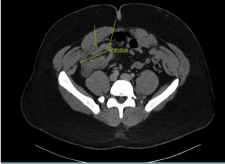
Figure 1: Computed tomography of abdomen showing a segment of
intussusception of ilium into cecum measuring approximately 7.7 cm in length.
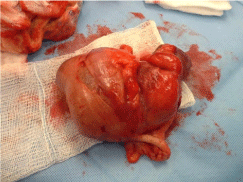
Figure 2: Intraoperative view showing the iliocecal intussusception.
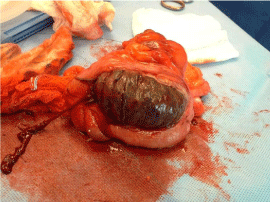
Figure 3: Necrotic small bowel trapped in the cecum.
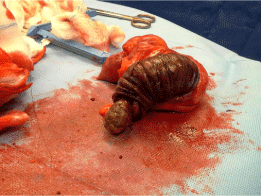
Figure 4: Lipoma lead point pictured.
There were no intraoperative or immediate post-operative complications and the patient was discharged home five days postoperatively.
The patient returned 7 days later with post-operative wound infection requiring incision and drainage. On subsequent follow-up patient remained in good condition.
Discussion
Adult intussusception symptoms are often vague and include abdominal pain, vomiting, diarrhea, melena, obstruction, and, more rarely, weight loss and general malaise [3,8]. Intussusception is most accurately identified by CT scan although other diagnostic imaging such as abdominal radiograph and ultrasound are often employed to make the diagnosis [3,4]. The treatment of adult intussusception is always surgical, but there is debate whether reduction should be attempted first in order to limit the amount of bowel that needs to be resected. A high WBC count, presence of obstruction, and longer intussusception lengths are some of the factors that can be used to help determine when surgical intervention is necessary [9]. Some of the feared complications with attempted reduction prior to surgery are intraluminal seeding if malignancy is present, anastomotic complications if there is bowel gangrene, and bowel perforation [3,10,11].
Cases in which intussusception lead points are believed to be either benign lesions or post-surgical adhesions, attempted reduction before resection is the preferred treatment modality. The therapeutic dilemma arises when the etiology cannot be accurately determined. Close to 50% of bowel lesions are thought to be malignant, with the majority of malignant lesions due to metastatic disease. This includes metastatic melanoma, the most common metastatic lesion of the small intestine, metastatic lymphomas, sarcomas and carcinomas [3,8]. Benign lesions that are commonly encountered as lead points include lipomas, polyps, and neurofibromas8.
Lipomas can arise spontaneously or as part of syndromes including Lipomatosis, Dercum’s disease, Madelung’s disease and as well as various hamartomatous polyposis syndromes [12]. Lipomosarcomas, malignant fatty soft tissue tumors, are very rare entities, with only a few reported instances in the literature [13]. Clinical indicators, such as the cutaneous lipomas observed on physical exam in our patient, can give us clues to the etiology of the lead point and whether or not reduction should be attempted. A history of Peutz-Jegher Syndrome, Scleroderma, Neurofibromatosis and other cutaneous and systemic conditions can also provide hints as to whether polyps, neurofibromas, or other benign etiologies could be potential lead points.
Conclusion
Intussusception in adults is a rare occurrence that presents with nonspecific signs and symptoms. Because malignancy is the cause of almost 50% of the pathologic lesions, surgery is the treatment of choice. The decision whether to attempt reduction prior to resection is case specific, and it should be tailored according to the clinical picture. A thorough history and physical is essential, taking care to inquire about a personal or family history of cancer, cutaneous disorders, and other genetic and systemic diseases. These clinical clues can help determine whether a benign etiology is likely and reduction is a safe technique.
References
- Laws HL, Aldrete JS. Small-bowel obstruction: a review of 465 cases. South Med J. 1976; 69: 733-734.
- Agha FP. Intussusception in adults. AJR Am J Roentgenol. 1986; 146: 527-531.
- Azar T, Berger DL. Adult intussusception. Ann Surg. 1997; 226: 134-138.
- Ioannidis O, Cheva A, Kakoutis E, Athina K, Nikolaos P, Stergios R, et al. Acute adult intussusception caused by primary cecal non Hodgkin lymphoma. Acta Gastroenterol Belg. 2011; 74: 451-453.
- Weilbaecher D, Bolin JA, Hearn D, Ogden W 2nd. Intussusception in adults. Review of 160 cases. Am J Surg. 1971; 121: 531-535.
- Ashley SW, Wells SA Jr. Tumors of the small intestine. Semin Oncol. 1988; 15: 116-128.
- Vecchio R, Ferrara M, Mosca F, Ignoto A, Latteri F. Lipomas of the large bowel. Eur J Surg. 1996; 162: 915-919.
- Honjo H, Mike M, Kusanagi H, Kano N. Adult intussusception: a retrospective review. World J Surg. 2015; 39: 134-138.
- Kim J, Lim J, Jeong J, Kim W. Conservative management of adult small bowel intussusception detected at abdominal computed tomography.Korean J Gastroenterol. 2015; 65: 291-296.
- Felix EL, Cohen MH, Bernstein AD, Schwartz JH. Adult intussusception; case report of recurrent intussusception and review of the literature. Am J Surg. 1976; 131: 758-761.
- Garg PK, Jain BK. Reduction of Adult Intussusception: More Harm than Benefit. World J Surg. 2015; 39: 2606.
- Salam GA. Lipoma excision. Am Fam Physician. 2002; 65: 901-904.
- D’Annibale M, Cosimelli M, Covello R, Stasi E. Liposarcoma of the colon presenting as an endoluminal mass. World Journal of Surgical Oncology. 2009; 7.