
Case Report
Austin J Surg. 2016; 3(1): 1081.
Problems in Tropical Proctology
Weledji EP¹* and Enoworock G²
¹Department of Surgery, University of Buea, Cameroon
²Department of Pathology, University of Buea, Cameroon
*Corresponding author: Weledji EP, Department of Surgery, Faculty of Health Sciences, University of Buea, Regional Hospital Buea, PO Box 126, Limbe, S.W. Region, Cameroon
Received: February 01, 2016; Accepted: March 22, 2016; Published: March 29, 2016
Abstract
Anorectal pathology is a growing problem in the developing (tropical) world. Five proctology cases and other anorectal pathologies that highlight the problems of diagnosis and management in a developing tropical country (Cameroon) in West Africa are discussed. Proctological procedures can be safe and effective therapeutic modalities. However, the problems of proctology practice in the developing world include: patients’ ignorance and fear of anorectal procedures rendering fecal incontinence; insufficient health education accentuating late diagnosis and management of anorectal disease; a poor referral system; the lack of trained colorectal surgeons and pathologists; limited resources; and the greater need for understanding sexually transmitted diseases such as HIV/AIDS in the practice of proctology.
Keywords: Haemorrhoids; Cloacal injury; Rectal prolapse; Anal tuberculoma; HIV ulcer; HIV-associated malignancies
Abbreviations
HIV: Human Immunodeficiency Virus; AIDS: Acquired Immune Deficiency Syndrome
Background
Anorectal pathology is a growing problem in the developing world. The adoption of the western low fibre diet aggravates the symptoms of haemorrhoids and anal fissures. In addition, sub- Saharan Africa has the highest prevalence of HIV/AIDS and HIV is one of the sexually transmitted organisms that affects the anorectum with a predilection for the external anal sphincter [1,2]. Included in this group are the other sexually transmitted organisms associated with high risk behaviors including anorectal intercourse that cause proctitis and anogenital ulcerations. Other viral organisms include cytomegalovirus, Herpes Simplex Virus (HSV), human papilloma virus (condylo-mataacuminatum), and molluscumcontagiosum. Bacterial organisms include Campylobacter jejuni, Chlamydia trachomatis, Lymphogranuloma venereum, Haemophilusducreyi (chancroid), Neisseria gonorrhoeae (gonorrhoea), Donovaniagranulomatis (granuloma inguinale) and Treponemapallidum (syphilis). The presence of more than one offending organism is common and the presenting symptoms may range from gastrointestinal (diarrhoea, rectal bleeding) to visible lesions in the anus and perineum [2]. The diarrhoea associated with the opportunistic colonic infections (CMV and bacterial colitis/proctitis), is severe and encourages anal ulceration, fissures and pruritis. The tenesmus from diarrhea causes straining that aggravates haemorrhoids. Thus stool cultures for salmonella, shigella, campylobacter and cryptosporidium with microscopy for giardia, ova, cysts and amoebae are mandatory [1,2]. An understanding of HIV/AIDS is therefore important to the practice of proctology as these patients frequently present with proctological diseases. The distribution of the most common anorectal pathologies reported in HIV patients include anal ulcer (29–32%), anal condyloma (32–43%), anal fissure (6–33%), anal fistula (6–33%), perirectal abscess (3–25%) and haemorrhoids (4– 14%..3With increasing survival of HIV/AIDS patients on Highly Active Anti-Retroviral Therapy (HAART) the other non-AIDS related anorectal disorders requiring treatment predominate. The two factors most associated with poor wound healing are AIDS and a poor performance status (ASA or Korsakoff’sscore) [3-5]. Two-thirds of AIDS patients needing surgical treatment for anorectal disease were rendered symptom- free. So treatment is well-worth doing as the survival is close to patients with AIDS who did not have anorectal disease [5,6]. This paper ascertained the short-comings and problems of proctology practice in a typical sub-saharan country (Cameroon) located at the West African coast (the Gulf of Guinea) through 5 case presentations.
Case Presentation
Problem 1
The lack of trained colorectal surgeons, pathologists and resources
Case: Chronic massive prolapsed haemorrhoids managed by ablation and correction in a poor resourced area.
We report a case of a 75-year-old man with symptomatic chronic circumferentially prolapsed haemorrhoids and associated obstructive defaecation (Figure 1a). He had several failed attempts at surgical repair by general medical practitioners. The specialist’s knowledge that failed haemorrhoidectomy may be due to an associated rectal mucosal prolapse led to the successful approach of ablation and correction of the associated rectal mucosal prolapse with a modified Delorme’s procedure akin to a stapled anopexy (Figure 1b).
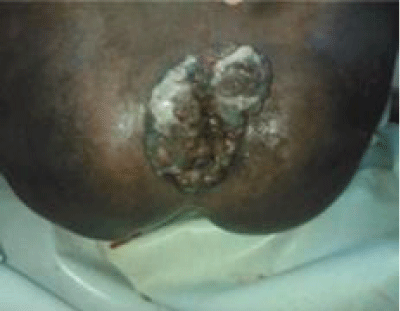
Figure 1a: Chronic prolapsed haemorrhoids.

Figure 1b: Post Milligan-Morgan and modified Delorme’s procedure.
Problem 2
Myths and late presentations
Case: Neglected incarcerated large rectal prolapse managed by Delorme’s procedure
We report a case of a 64-year-old man with an incarcerated (irreducible) large rectal prolapse for which the treatment of choice might traditionally have been an Altimeter’s procedure (perineal excision of the prolapsed, coloanal anastomosis and repair of the pelvic floor) is reported (Figure 2a). A technically- difficult Delorme’s procedure (rectal mucosal excision and placation of the prolapsed muscle wall) was performed in this situation, with an excellent immediate outcome. Delorme’s procedure is safe and effective even in large incarcerated rectal prolapse. At 6 months, there was no recurrence of the rectal prolapse and continence much improved (Figure 2b).
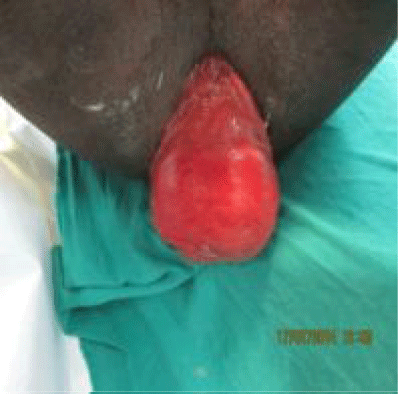
Figure 2a: Large, incarcerated rectal prolapse.
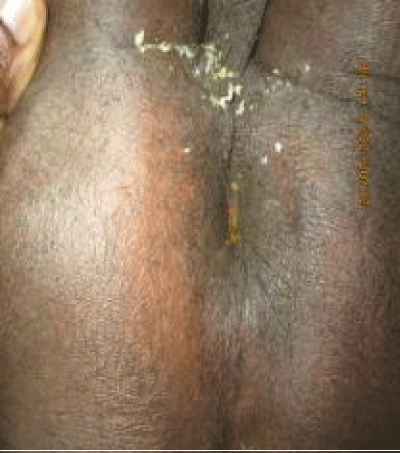
Figure 2b: Post Delorme’s repair.
Problem 3
Obstetric anal sphincter (cloacal) injury
Case: Secondary repair of severe chronic fourth-degree perineal tear due to obstetric trauma.
We report a case of a 32-year- old woman with anal incontinence as a result of severe chronic fourth-degree perineal tear secondary to birthing with complete disruption of the perineum. Secondary repair consisted of an anterior sphincter repair and levatorplasty rendered excellent immediate clinical result. The great majority of cloacal defects due to obstetric injury do not require tissue replacement, as there has been no tissue loss- it is merely in the wrong place (Figure 3a). These defects involve the introitus, anal canal, rectovaginal septum and anal sphincters. Repair is achieved simply by returning all displaced tissues to their normal anatomical position; this is facilitated by careful and accurate apposition of the main landmarks: the posterior fouchette, dentate line and anal verge. Repair of the sphincters would restore anatomical and cosmetic normality with usually very satisfactory cosmetic and functional outcome (Figure 3b).
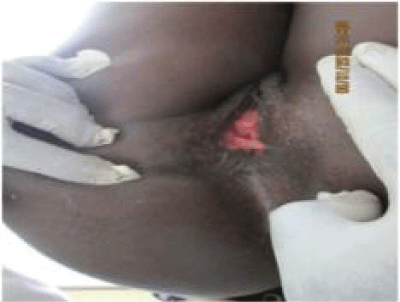
Figure 3a: Cloacal injury prior to repair.
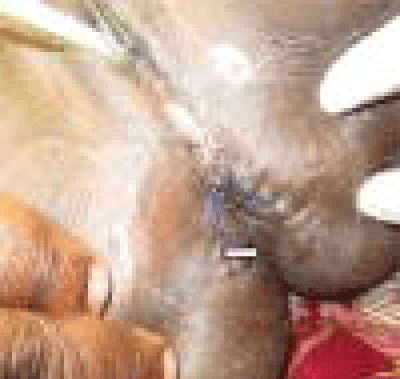
Figure 3b: Post anterior sphincter repair and anterior levatorplasty.
Problem 4
Not all anal lesions are malignant
Case: Ano-rectal tuberculoma simulating cancer in the Acquired Immune Deficiency Syndrome (AIDS).
We report a case of ano-rectal tumour clinically diagnosed as cancer in a 36- year-old male AIDS patient. Patholoygical analysis of the biopsy specimen revealed tuberculosis (Figure 4). The tumour regressed enormously and the general condition of the patient improved during the follow up with anti-tuberculous and antiretroviral therapy.
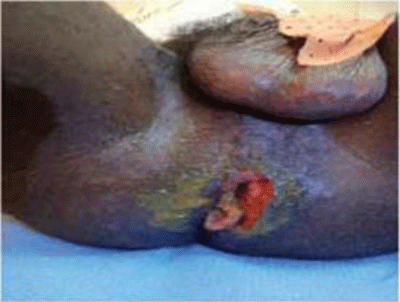
Figure 4: Ulcerating ano-rectal tuberculoma and histology showed caseating
granuloma.
Problem 5
Beware of the AIDS-associated anal ulcer
Case: A case of HIV-associated ulcer
A 48-year-old heterosexual African man presented as an emergency with a progressive disabling anal pain for three days on a background one-year history of a chronic anal ulcer. He had been Highly Active Antiretroviral Therapy (HAART) - naive since being diagnosed Human Immunodeficiency Virus (HIV 2)-positive 11 years previously. With the aid of the Eisenhamer retractor, the ulcer cavity was demonstrated as located proximal to the dentate line with a broad based ulcer secondarily extending in a horse-shoe manner in the intersphincteric and submucosal planes consistent with an HIV ulcer (Figure 5). The treatment entailed unroofing of cavities and debridement to eliminate trapping of stool and pus that cause severe pain. Because of a possible herpetic aetiology of the ulcer, he was commenced on acyclovir 200 mg bd for two weeks.
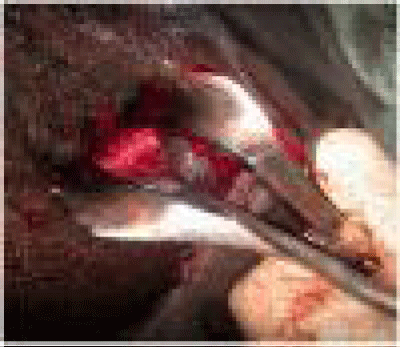
Figure 5: HIV ulcer after deroofing and debridement (broad base and
involving the submucosal and intersphincteric planes).
Discussion
Proctological procedures can be safe and effective therapeutic modalities. The problems of proctology practice in the developing world includes: patients’ ignorance and fear that anorectal procedures may render anal incontinence as illustrated in cases 1 and 3; (2) insufficient health education accentuating late diagnosis and management of anorectal disease as illustrated in case 3; (3) a poor referral system as seen in case 1;(4) the lack of trained colorectal surgeons, pathologists and limited resources as illustrated in cases 1,2,3,4 and 5; (5) the understanding of HIV/AIDS in the practice of proctology as illustrated in cases 4 and 5 [7-10].
Obstetric (cloacal) injury is the commonest cause of anal incontinence in the developing world [11]. As prevention is not always possible, immediate recognition and adequate primary treatment is of importance. The outcome of anterior sphincter repair following obstetric trauma is good but long-term follow-up is required because of the underlying complexity of obstetric injury [12].
Anorectal pathology is one of the most common indications for surgery in HIV-positive patients especially as they have not been impacted by highly active anti- retroviral therapy [13]. However, not all tumour-like lesions that occur in immune depressed patients are neoplasia, and not all anal ulcers are anal fissure. This is illustrated in cases 4 and 5 respectively. Case 4 - ano-rectal tuberculoma simulating cancer in the acquired immune deficiency syndrome illustrates a rare localization of a common disease and highlights the importance of pathological analysis of specimens in diagnosis and management of patients even when clinical presentation may appear obvious 9. Case 5 demonstrates an HIV-associated ulcer which must be distinguished from an idiopathic anal fissure in HIV-positive patients and from other sexually transmitted diseases that cause anogenitalulcers as the treatments differ [10]. In resourced areas biopsies would identify treatable aetiologies of these ulcers, including Herpes Simplex Virus (HSV), cytomegalovirus, Treponemiapallidum, mycobacterium, cryptococcus, Haemophilusducreyi, Chlamydia trachomatis and cancer. As condylomaacuminatum and HSV infections are common secondary causes of pruritus ani in HIV/AIDS, biopsy of aperianal skin ulcermay identify the aetiology [14]. Surgical treatment of the HIV ulcer consists of debridement, unroofing cavities to eliminate trapping and intralesional steroid injection (80–160 mg methylprednisolone acetate in 1 ml of 0.25% bupivacaine) for the idiopathic HIV-associated ulcer. Repeat steroid injection is performed on patients with idiopathic HIV-associated ulcer who develop recurrent pain. HIV-associated ulcers are most commonly associated with patients with clinical AIDS and lower CD4 counts and it appears that since the introduction of HAART it is a less common clinical problem [1,3]. Symptomatic relief is the goal of treatment as HIV ulcer healing is not common [13].
Haemorrhoidectomy is indicated for AIDS patients who fail conservative treatmenst such as rubber band ligation, infrared coagulation, or sclerotherapy Symptomatic improvement of the underlying anorectal pathology such as haemorrhoids, perianal sepsis, and ulcers may make delayed wound healing an acceptable complication in AIDS [15,16]. Sphincter preservation is of the utmost importance during all anal operations because male homosexuals have a tendency towards incontinence and the diarrhoea associated with opportunistic colonic infections is often severe. Setons are required for most fistulae and for the disintegrating perineum syndrome [1,4,17]. For idiopathic anal fissures, lateral internal anal sphincterotomy is appropriate for patients who fail conservative measures (warm soaks, stool softeners, topical diltiazem ointments, butulinum toxin injection), but do not have chronic diarrhoea or preexisting incontinence. Alternatively a cutaneous advancement flap is preferred in those with a contraindication to sphincterotomy [1,17].
Other common problems not illustrated include anal warts in AIDS patients which tend to be aggressive, dysplastic and harder to eradicate. As with other viral infections, it is impossible to eradicate the causative human papilloma virus (HPV 6,11,16,18) infection by surgical excision. For this reason surgical excision of condylomas is effectively performed more for relief of symptoms and cosmesis [18,19]. The premalignant anal carcinoma in-situ lesion may be rapidly progressive in immunocompromised patients (transplant recipients and HIV patients). Even so, it is a rare condition perhaps because the rate of progression is slower than the natural history of the HIV disease and there is a need for caution when considering treatment [20,21]. Radiotherapy may be helpful for symptomatic cases otherwise the patient is kept under observation. Chemoirradiation is the treatment of choice for most invasive anal (squamous cell) cancers and a salvage Abdominoperineal Resection (APR) can be useful if the CD4 count is > 200 [22]. Otherwise the perineal wound will not heal [23,24]. It should be noted that the AIDS –associated malignancies such as squamous cell carcinoma may be mistaken for a small benign ulcer, Kaposi’s sarcoma may resemble an ulcerated haemorrhoid and non-Hodgkin’s lymphoma may resemble a perianal abscess [22,25,26]. The diagnosis of the latter can be made by a needle biopsy via the perineum and not inside the anal canal as the patient will develop a fistula in the lymphomatous tissue [26]. The pathophysiological consequences of advanced disease (e.g. immunosuppressant, malnutrition, infections and neoplasms) could dictate the scaling down of the magnitude of surgery to an acceptable and safe level [27].
References
- Beck DE, Wexner SD. AIDS and the colorectal surgeon. Part 11; anorectal diseases. Postgrad Adv Colorectal Surg. 1990: 1-13.
- Jayasuriya A, Robertson C, Allan PS. Twenty-five years of HIV management. J R Soc Med. 2007; 100: 363-366.
- Brar HS, Gottesman L, Surawicz C. Anorectal pathology in AIDS. Gastrointest Endosc Clin N Am. 1998; 8: 913-931.
- Smit S. Guidelines for surgery in the HIV patients. Continuous Medical Education (CME). 2010; 28: 8.
- Morand E, Merlini D, Saraggio A, Foschi D, Trabucchi E. Prospective study of healing time haemorrhoidectomy. Dis Colon Rectum. 1999; 42: 1140-1144.
- Piot P, Kazatchkie M, Dybul M, Lob-Leryt J. AIDS: lessons learned and myths dispelled. The Lancet. 2009; 374: 260-263.
- Johnson DB, DiSiena MR, Fanelli RD. Circumferential mucosectomy with stapled proctopexy is a safe, effective outpatient alternative for the treatment of symptomatic prolapsing haemorrhoids in the elderly. Surg Endosc. 2003; 17: 1990–1995.
- Senapati A, Nicholls RJ, Thomson JP, Phillips RK. Results of Delorme's procedure for rectal prolapse. Dis Colon Rectum. 1994; 37: 456-460.
- Neto IJ, Sia ON, Lopes EA, Macacaria RL, Wattéa HH, Souzaa RFL, et al. Perianal tuberculosis: A rare disease of late diagnosis. J of Coloproctology. 2014; 34: 124-127.
- Modesto VL, Gottesman L. Surgical debridement and intralesional steroid injection in the treatment of idiopathic AIDS-related anal ulcerations. Am J Surg. 1997; 174: 439-441.
- Guise JM, Morris C, Osterweil P, Li H, Rosenberg D, Greenlick M. Incidence of fecal incontinence after childbirth. Obstet Gynecol. 2007; 109: 281-288.
- Fernando RJ, Sultan AH, Kettle C, Thakar R. Methods of repair for obstetric anal sphincter injury. Cochrane Database Syst Rev. 2013; 12: CD002866.
- Gonzalez Ruth C, Heartfield W, Briggs B, Vukasin P, Beart RW. Anorectal pathology in HIV/AIDS infected patients has not been impacted by highly active antiretroviral therapy. Dis Colon Rectum. 2004; 47: 1483–1486.
- Weledji EP. Human immunodeficiency virus and the anorectum. Alex J Med. 2013; 49: 163-167.
- Moore BA, Fleshner PR. Rubber band ligation for hemorrhoidal disease can be safely performed in select HIV-positive patients. Dis Colon Rectum. 2001; 44: 1079-1082.
- Hewitt WR, Sokol TP, Fleshner PR. Should HIV status alter indications for hemorrhoidectomy? Dis Colon Rectum. 1996; 39: 615-618.
- Wexner SD, Smithy WB, Milsom JW, Dailey TH. The surgical management of anorectal diseases in AIDS and pre-AIDS patients. Dis Colon Rectum. 1986; 29: 719-723.
- Nielson CM, Harris RB, Dunne EF, Abrahamsen M, Papenfuss MR, Flores R, et al. Risk factors for anogenital human papillomavirus infection in men. J Infect Dis. 2007; 196: 1137-1145.
- Palefsky J. Human papilloma virus infection in HIV-infected persons. Top HIV Med. 2007; 15: 130-133.
- Scholefield JH, Hickson WG, Smith JH, Rogers K, Sharp F. Anal intraepithelial neoplasia: part of a multifocal disease process. Lancet. 1992; 340: 1271-1273.
- Palefsky JM, Holly EA, Efirdc JT, Da Costa M, Jay N, Berry JM, et al. Anal intraepithelial neoplasia in the highly active antiretroviral therapy era among HIV-positive men who have sex with men. AIDS. 2005; 19: 1407-1414.
- Nigro N, Vaitkevicius V, ConsidineJr B. Combined therapy for cancer of the anal canal. A preliminary report. Dis Colon Rectum. 2009; 27: 354-356.
- Albaran RG, Webber J, Steffes CP. CD4 cell counts as a prognostic factor of major abdominal surgery in patients infected with the human immunodeficiency virus. Arch Surg. 1998; 133: 626-631.
- Horberg MA, Hurley LB, Klein DB, Follansbee SE, Quesenberry C, Flamm JA, et al. Surgical outcomes in human immunodeficiency virus-infected patients in the era of highly active antiretroviral therapy. Arch Surg. 2006; 141: 1238-1245.
- Lorenz HP, Wilson W, Leigh B, Schecter WP. Kaposi's sarcoma of the rectum in patients with the acquired immunodeficiency syndrome. Am J Surg. 1990; 160: 681-682.
- Kaplan LD. AIDS-associated lymphomas. Infect Dis Clin North Am. 1988; 2: 525-532.
- Weledji EP, Nsagha D, Chichom A, Enoworock G. Gastrointestinal surgery and the acquired immune deficiency syndrome. Ann Med Surg (Lond). 2015; 4: 36-40.