
Case Report
Austin J Surg. 2018; 5(2): 1128.
Focal Nodular Hepatic Steatosis: CT and US Guided Biopsy Findings Correlating with Surgical Histopathology
Assaf Y* and Augustin SM
Department of Surgery, University of Missouri-Kansas City (UMKC) School of Medicine, USA
*Corresponding author: Yazen Assaf, Department of Surgery, University of Missouri-Kansas City (UMKC) School of Medicine, USA
Received: December 13, 2017; Accepted: January 15, 2018; Published: February 12, 2018
Abstract
Focal hepatic steatosis is uncommon. We report a case in a 55-year-old African American female found to have a multiple liver lesions on CT scan confirmed on histopathology from ultrasound-guided biopsy and surgical specimens.
Case Report
A 55 year old African American female with history of myasthenia gravis, hypertension, pernicious anemia and endometrial atypia presented to our institution with complaints of severe non-radiating, left lower quadrant abdominal pain associated with unintentional weight loss. She denied any episodes of hematochezia or hematemesis and endorsed normal bowel function. She did report a family history of breast cancer, though a recent mammogram only revealed a benign nodule. Physical exam demonstrated a well-developed female with a BMI of 21 and the finding of tenderness to palpation in the left lower quadrant (Figure 1).
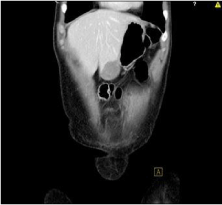
Figure 1: It shows tenderness to palpation in the left lower quadrant.
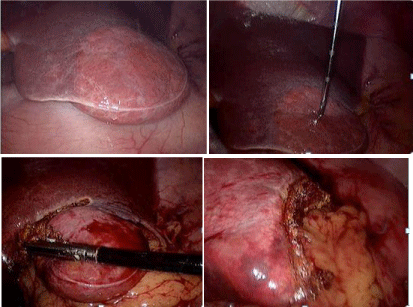
Figure 2: It shows diagnostic laparoscopy and possible liver resection.
Initial laboratory work showed normal lipid panel, normal transaminases, and normal alkaline phosphatase. CT abdomen and pelvis with contrast showed normal liver size and contour with multiple small ill-defined hypo-attenuating liver lesions. The largest lesion in the inferior right lobe measured 1.2 x 1 x .8 cm. Other smaller lesions were scattered throughout the periphery of both liver lobes. A 2.4 x 4 x 3.8 cm mass was also seen invading the left anterior abdominal wall with extension into the inferior left liver lobe concerning for metastatic disease. Additionally, mixed sclerotic and lytic changes of the right iliac bone were noted in addition to incidental findings of irregular thyroid and breast nodularity on CT chest, further raising concern for metastatic disease.
During the initial diagnostic work up, ultrasound-guided liver biopsy showed liver parenchyma with marked micro- and macrovesicular steatosis along with focal lobular inflammation but absence of portal spaces. Additional laboratory work showed normal CEA, AFP, CA19-9, CA 125 levels and a nonreactive hepatitis screen. In the following weeks, she underwent an extensive metastatic workup in search of a primary source for her presumed metastatic liver lesions. Outpatient mammography showed BIRADS 3 benign breast nodules likely due to fibrocystic disease. EGD showed atrophic gastritis with biopsies negative for H. Pylori and atypia. Ultrasound of the thyroid showed multiple thyroid lesions with a large complex cystic lesion in the mid to inferior left thyroid, measuring 4.3 x 2.1 x 2 cm. Subsequent FNA of these nodules were negative for malignancy. In the interval months following discovery of the liver masses, the cancer workup failed to reveal a primary source.
A 6 month follow-up CT showed a stable 3.9 cm transverse heterogeneously enhancing mass within the anterior inferior aspect of the left hepatic lobe, similar to the previous measurement of 4.0cm. The mass abuts the left rectus abdominus musculature anteriorly and the gastric antrum posteriorly with stable loss of tissue planes between these structures. Other scattered predominantly sub-centimeter hypodense liver lesions throughout both lobes were stable to slightly decreased in size. No new lesions were detected and were referred to general surgery for further evaluation of her liver masses (Figure 2).
After careful examination of the patient and evaluation of imaging, surgery was discussed with the patient and she agreed to proceed with diagnostic laparoscopy and possible liver resection. Intra-operatively, frozen sections of the smaller right liver masses and larger left liver mass on the anterior surface of the liver failed to reveal anything other than steatosis. This was followed up by resection of the left liver mass, with grossly normal appearing margins. Further inspection of the gall bladder, visible portion of the pancreas, stomach, spleen, transverse colon and small intestines was unremarkable. Final surgical pathology report was consistent with focal steatosis of right and left liver masses with no signs of malignancy. The patient has been recovering well at this time.
Discussion
Hepatic steatosis is mainly a diffuse process but can present in many localized forms such as: multinodular, hypersteatosis, focal geographic, focal nodular, intralesional, perilesional, and subcapsular [1]. Although diffuse hepatic steatosis is the most commonly encountered subtype, focal subtypes, when encountered, can mimic metastatic disease processes and can result in unnecessary invasive interventions. We report a unique case of hepatic steatosis with focal nodular distribution as evidenced by CT scan and surgical histopathology.
Hepatic steatosis can be diagnosed by three main imaging modalities: Ultrasound, CT scan, and MRI [2]. Ultrasound is relatively insensitive as it requires at least 30% fat to detect an increased echogenicity that is characteristic of steatosis. CT imaging shows steatosis as having lower density than normal liver tissue but also is unable to detect lower fat quantities. MRI and H-MRS are currently the most accurate modalities as they can quantify the hepatic lipid content [2]. Measuring Proton Density Fat Fraction (PDFF) of the liver has been found as accurate as liver biopsy in diagnosing hepatic steatosis [3]. Quantification of hepatic lipid content, however, is not routinely done. In this case, focal hepatic steatosis was diagnosed after an extensive workup for metastatic disease involving multiple invasive procedures. Focal steatosis presents a diagnostic dilemma as the need to rule out malignant etiology often outweighs the risks of invasive procedures. However utilization of MR imaging in evaluating liver masses can potentially decrease the cost and morbidity associated with liver biopsy.
References
- Karcaaltincaba, Musturay. Imaging of hepatic steatosis and fatty sparing. European Journal of Radiology. 2007; 61: 33-43.
- Alastair D B, Bellamy C. “Fatty Liver Disease.” MacSween’s Pathology of the Liver, Elsevier. 2018; 966-1088.
- Idilman IS, Aniktar H, Idilman R, Kabacam G, Savas B, Elhan A, et al. Hepatic steatosis: quantification by proton density fat fraction with MR imaging versus liver biopsy. Radiology. 2013; 267; 767-75.