
Special Article – Surgery Case Reports
Austin J Surg. 2019; 6(16): 1203.
Rectal Cancer Masquerading as Retro Rectal Tumour - A Rare Case Report
Ashok K1*, Bhatt N1, Alka Y1 and Nandita C2
1Departments of Surgical Gastroenterology, Sanjay Gandhi Post Graduate institute of Medical Sciences, India
2Departments of Pathology, Sanjay Gandhi Post Graduate institute of Medical Sciences, India
*Corresponding author: Ashok Kumar, Department of Surgical Gastroenterology, Sanjay Gandhi Post Graduate Institute of Medical Sciences, Raebareli Road, Lucknow-226014, India
Received: July 02, 2019; Accepted: July 29, 2019; Published: August 05, 2019
Abstract
The retrorectal or presacral space is an area that can keep a group of heterogeneous and rare tumours. These lesions range from benign cysts to complex malignant masses that can invade the surrounding pelvic structures. Osseous tumours also represent 10% of retro rectal tumours. Rectal cancer presenting as rectorectal tumor is a rare entity and difficult to diagnosis preoperatively and may affect the treatment strategy. We herein present a rare case of rectal cancer presenting as retrorectal tumor which could be diagnosed only after surgery on histology and Immunohistochemistry.
Keywords: Rectal cancer; Retrorectal tumor; Clinical presentation; Histopathology; Immunohistochemistry
Case Details
A 42 year old female patient without any co-morbidity, presented to us with a history of discomfort in perineal region associated with altered bowel habits in form of constipation and sense of incomplete evacuation for five months. There was a past history of lower segment caesarean section with tubectomy. Per rectal examination revealed an extra rectal hard palpable lump 3 cm above the anal verge, mucosa was free, lumen was compromised, and upper margin could not be reached. Colonoscopy showed normal mucosa in the rectum with external compression. MRI of the abdomen and pelvis revealed 10×9×10 cms pre sacral lobulated heterogeneous mass. Mass was sitting more on the left side of the rectal wall. The lesion was heterogeneously hyperintense on T1 & T2 W images with areas of calcification within the lesion (Figures 1A & 1B). Preoperative CEA and CA 19.9 were normal. She was taken up for surgery with the diagnosis of retro rectal dermoid.
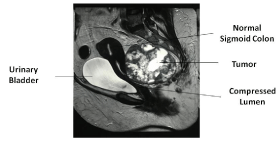
Figure 1A: Retrorectal tumor with calcification compressing anteriorly
(Sagittal View).
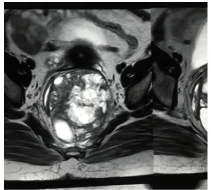
Figure 1B: Retrorectal tumor with calcification compressing rectum anteriorly
(Coronal View).
Patient underwent excision of tumor with enbloc excision of sigmoid and rectum with Total Hysterectomy (TAH) and Bilateral Salphingo Oophorectomy (BSO) (Figures 2A and 2B). Stapled coloanal anastomosis and diverting loop ileostomy.
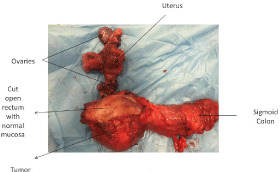
Figure 2A: Excised Specimen.
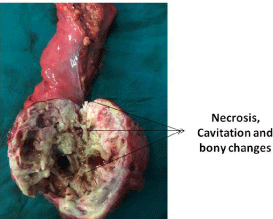
Figure 2B: Cut open tumour.
Histopathology of specimen showed poorly differentiated carcinoma; tumour involving submucosa and muscularis propria. Tumor was seen in subserosal connective tissue, but not breaching serosal surface, and all margin were free of tumor. Osseous metaplasia (Figures 3A and 3B) was seen in the tissue. Mucosa of rectum was free of tumor in its whole extent (Figure 4). On IHC tumour was positive for CK and negative for Vimentin, CD99, EMA, HMB-45 and BCL-2 (Figure 5A and 5B). Uterine biopsy revealed leiomyoma, proliferative endometrium and ovaries had follicular cyst.
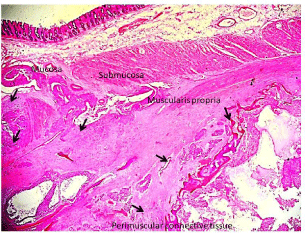
Figure 3: Tumour (black arrows) in submucosa, muscularis propria and
perimuscular connective tissue. Mucosa is unremarkable H&E, 100X.
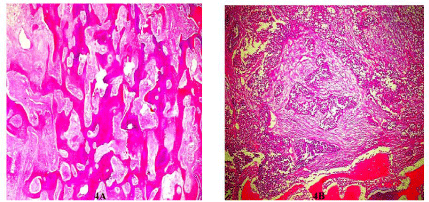
Figure 4: A-Tumour islands separated by metaplastic bone formation; BTumour
islands separated by desmoplastic stroma and metaplastic bone.
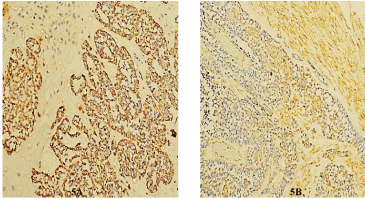
Figure 5: A- Cytokeratin Positive; B- Vimentin Negative.
In view of the poorly differentiated adenocarcinoma of epithelial origin & high suspicion of primary rectal cancer, patient was further evaluated with repeat CEA which was normal. PET scan (Figure 6) revealed multiple liver metastasis without any other site of tumor uptake. No other site of primary could be identified. Patient was subjected for 6 cycles of palliative chemotherapy which included ifosphamide plus epirubicin based chemotherapy. She survived about 12 months after surgery.
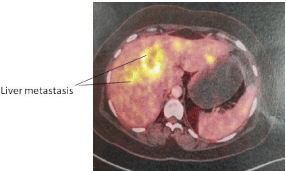
Figure 6: PET Scan showing multiple liver metastasis.
Discussion
The retrorectal or presacral space is an area that can keep a group of heterogeneous and rare tumours. These lesions range from benign cysts to complex malignant masses that can invade the surrounding pelvic structures. Osseous tumours also represent 10% of retrorectal tumours.It may present with constipation, bleeding, obstruction and perineal discomfort. Sometimes patients are asymptomatic and detected during routine surveillance. These tumors can invade the rectal mucosa and present as a rectal cancer. Rectal cancer typically arises from the epithelial lining and invades the various layers of the rectum; however epithelial malignancy without involvement of mucosa and normal looking mucosa on endoscopy are very rare possibility. Our patient was a case of rectal cancer with normal looking mucosa, where biopsy was unnecessary. Yoshito et al. has also reported a case of 46 Y/M with the history suggestive of rectal cancer with bony metastasis on MR where colonoscopy revealed stenosed lumen and normal looking adenomatous mucosa [1] the mucosal biopsy was negative. Similar case has been reported by Cherenfant et al; who have reported a case of rectal cancer with extraluminal primarily and reported histologically different from sacral tumour, This was reported in a male patient who had already gone a pull-through procedure for Hirschsprung’s disease in past; He hypothesised that tumour immerged from and extruded from entrapped segment of rectal mucosa at the time of patient childhood procedure [2]. A case by Beppu et al [3]; presented a case of 58 years old man with anal bleeding and abdominal pain; Abdominal CT showed thickening of rectal wall and sigmoid colon and left hydronephrosis. Barium enema revealed marked narrowing with mucosal irregularities from rectum to sigmoid colon; Biopsy specimens showed inflammatory cells; as demonstrated by this case, when diffuse infiltrative carcinoma is strongly suspected, it is an imperative to perform multiple deep biopsies from the affected region.
The lack of pre-operative diagnosis may lead to a different therapeutic strategy as compare to post-operative diagnosis in rectal cancer.
In a case of imaging diagnosis of retrorectal tumor and no symptoms of rectal cancer, it is rather impossible to diagnose rectal cancer if the rectal mucosa is normal on colonoscopy. Yoshito et al in their case performed endoscopic mucosal resection followed by boring biopsies which finally revealed signet ring cell carcinoma. The normal looking mucosa and negative biopsy likely suggest that cancerous lesion was covered with normal epithelium they suggested the bore biopsy at times is helpful to establish the diagnosis if the suspicion of malignancy is very high [1]. Cytokeratin 20 & Cytokeratin 7 are also helpful in such situation specially if there is poorly differentiated adenocarcinoma [4] But it will require tumour tissue which is not possible before surgery. Our case was very rare presentation of epithelial malignancy without involvement of mucosa; however the rest of the other layer of rectum was infilterated by tumour and the osseous metaplasia
Conclusion
In a case of imaging diagnosis of retrorectal tumor and without classical presentation of rectal cancer, it is difficult to diagnose rectal cancer if the rectal mucosa is normal on colonoscopy The lack of pre-operative diagnosis may lead to a different therapeutic strategy as compare to post-operative diagnosis in rectal cancer. Epithelial malignancy without involvement of mucosa on histology is a rare possibility. Immunohistochemical Expression of CK 20 and CK 7 may be helpful in difficult situation.
References
- Hirata Y, Kanno K, Kishikawa N, Tomoda S, Kimura K, Kobayashi T, et al. Primary Signet Ring Cell Carcinoma of Rectum Diagnosed by Boring Biopsy in Combination with Endoscopic Mucosal Resection. Case Rep Med. 2018; 2018: 5860815.
- Cherenfant J, Ruggiero FM, Gage M, Poritz L. Primary Rectal Cancer from Outside the Rectum. J Gastrointest Dig Syst. 2014; 4: 6.
- Beppu K, Osada T, Tomoda N, Mizui T, Ikari T, Inou T, et al. A case of diffuse infiltrative carcinoma of large intestine and the challenges of diagnosis; Progress of Digestive Endoscopy. 2012; 81: 138-139.
- Selves J, Long-Mira E, Mathieu MC, Rochaix P, Ilié M. Immunohistochemistry for Diagnosis of Metastatic Carcinomas of Unknown Primary Site. Cancers (Basel). 2018; 10: 108.