
Research Article
Austin J Urol.2016; 3(1): 1039.
Transitional Cell Carcinoma of the Bladder in Children Long Term Follow-Up
Marte A*
Department of Urology and Pediatric Surgery, University of Naples, Italy
*Corresponding author: Antonio Marte, Department of Urology and Pediatric Surgery, University of Naples, Largo Madonna Delle Grazie, Italy
Received: November 12, 2015; Accepted: January 04, 2015; Published: January 05, 2016
Abstract
Summary: The aim of our study is to report on long term follow-up on TCCB in children.
Materials and Methods: From 1990 to 2014, 5 patients, female, age range 12-15 years (mean 13.2 years), were referred to our center with TCCB. In 4 patients the clinical symptoms debut was a 'gross hematuria. Of these, 1 patient had been operated on two years before, for UPJ obstruction with double-J stent apposition. The endoscopy performed during this operation as a diagnostic routine did not show any abnormality of the bladder wall. In 1 patient the tumor was an incidental finding during cystoscopy for endoscopic correction of vesicoureteral reflux. All patients underwent successful transurethral resection by pediatric resectoscope.
Results: At a mean follow-up of 15 years no recurrence was registered. All patients underwent to the following follow-up: endoscopy, renal and bladder ultrasound and urinary cytology every 6 months the first year. US and urinary cytology every 6 months the first two year then yearly and out of protocol after 5 years free of disease. The oldest patients of this series were recently contacted by telephone interview to prepare the present review by asking them to perform a reno-vesical ultrasound which was negative in all patients.
Conclusion: The low incidence of TCC shows the rarity of this finding in the pediatric population and an unexpected exclusive prerogative of the female sex, in our experience. The main clinical manifestation of such injuries is haematuria; commonly these are solitary lesions, low-grade histology and low risk of progression. Our case studies, probably one of the longest follow-up in the literature, confirm that in this age group the prognosis also in the long term is particularly favorable.
Keywords: Bladder; Children; Transitional cell carcinoma
Introduction
Transitional Cell Carcinoma of the Bladder (TCCB) is a rare disease in the first two decades of life. It occurs with a frequency that is 9 times higher in males than females and its origin is commonly type mesothelial. On the basis of the 1973 World Health Organization classification, tumors were classified as Transitional Cell Carcinoma of the Urinary Bladder (TCCB). Owing to more detailed histological criteria, this term has been replaced by papillary urothelial neoplasm of low malignant potential and low-grade carcinoma of the urinary bladder in the World Health Organization-International Society of Urologic Pathology consensus classification system of urothelial neoplasms 2004. Cases of TCCB, and reported in the literature regarding the pediatric population, are less than 150.
In 1969, Javadpour e Mostofi conducted a study of 10,000 patients with TCCB and found that only 40 of these were less than 20 years [1]. Many studies have subsequently described the characteristics of these tumors in children that, in many ways, manifest differently from adult forms as often these are solitary lesions, low-grade and rarely tend to relapse [2,3]. The aim of our study is to report our experience of TCCB in children.
Materials and Methods
From 1990 to 2014, 5 patients, female, age range 12-15 years (mean 13.2 years), were referred to our center with TCCB. All patients had a family and medical history negative for risk factors such as family history of cancer of the urinary tract, chronic exposure to carcinogens such as benzidine, diaminofenile, 4-nitrodiphenyl and use of anticancer drugs such as cyclophosphamide. In 4 patients the clinical symptoms debut was a 'gross hematuria. Of these, 1 patient had been operated on two years before, for UPJ obstruction with double-J stent apposition. The endoscopy performed during this operation as a diagnostic routine did not show any abnormality of the bladder wall. In 1 patient the tumor was an incidental finding during cystoscopy for endoscopic correction of vesicoureteral reflux.
All patients underwent to the following diagnostic tests: urinalysis with cytology and reno vesical ultrasound. In all patients, urinary cytology was not indicative for the TCCB. Reno vesical ultrasound demonstrated the presence of a vegetating formation protruding into the bladder cavity (0.9cm-1.2cm), at posterolateral bladder wall (three left / two right) without any involvement of the ipsilateral ureteral ostium. In one case a previous US made diagnosis of left intravesical ureterocele (17 x 9 mm) associated to duplex left system. Transurethral resection was performed in all patients by pediatric resectoscope removing completely the lesion. (Figure 1-3) No complications occurred in any patient after surgery. In one case, given the particular macroscopic aspect and microscopic extemporaneous examination of the lesion, the patient was administered a single dose of 40mg of mitomycin C in 40cc of saline for intravesical instillation soon after the resection of the tumor. The lesions removed were examined Histologically (Figure 4) (Table 1).
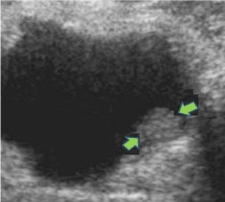
Figure 1: Female, 13 year-old postero lateral left-side TCCB: Preoperative
US.
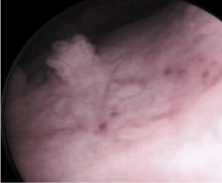
Figure 2: Endoscopic view of TCCB.
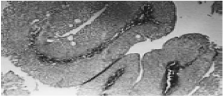
Figure 3: EE 10X subtle papillae, not fused with increased number of layers,
cell nuclei increased and slight not isometric nuclear shape with preservation
of order and cell polarity.

Figure 4: Female 15 years. Endoscopic view of a broad-based formation
friable and bleeding to the touch. Soon after the TURB a single dose of
mitomycin was administered.
Patient
Presenting Symptoms
US
D.B, ? 13 yrs
Gross hematuria
papillary tumor left lateral wall, 0.9 cm
F.G. ? 12 yrs
Gross hematuria
papillary tumor in the right lateral wall, 1 cm
A.N. ? 12 yrs
Gross Hematuria
papillary tumor right lateral wall, 1.5 cm
M.P. ? 14 yrs
Incidental finding, asymptomatic
Left, 0.9 cm
R.T. ? 15 yrs
Gross hematuria, urgency UTI
Left ureterocele, 17 cm
Table 1: Demographic data.
Results
The histological examination revealed for all 5 cases, the presence of a papilloma transitional cell with areas of grade G1 proliferative activity according to the classification WHO 1973 and PUNLMP type (urothelial neoplasms low biological risk of malignant progression) according to the classification WHO 1998-2004 [4,5]. The histological findings showed the presence of subtle papillae, not fused with increased number of layers, increased cell nuclei and slight nuclear anisometria with preservation of order and polarity. All patients underwent to the following follow-up: endoscopy, renal and bladder ultrasound and urinary cytology every 6 months the first year. US and urinary cytology every 6 months the first two year then yearly and out of protocol after 5 years free of disease. At a mean follow-up of 15 years (range 25-1year) no recurrence was registered. The oldest patients of this series were recently contacted by telephone interview to prepare the present review by asking them to perform a renovesical ultrasound which was negative in all patients.
Discussion
Bladder cancer is, in man, is the fifth leading cause of death from malignant carcinoma, with a frequency which amounts to 2.1% of all causes of cancer death. It occurs in both sexes, with a male to female ratio which is 7: 1, with a higher incidence in the sixth decade of life. Among the various histological types, the most frequent (90-95%) is constituted by the papilloma transitional cell that is histologically characterized by the presence of giant cells, with nuclei massed, loss of cell polarity and altered ratio nucleus cytoplasm. Macroscopically, the lesions affecting the adult are mostly multiple, sessile or pedunculated, with a high frequency of relapse. The locations are more frequent between the roof and the bladder trigone and the side walls [4]. In the pediatric population, the incidence of TCCB is less than 1% constituting a rare disease. In addition many studies show that, in children, the characteristics of these injuries take on particular aspects of kindness as occur as isolated lesions, low-grade organic, low risk of malignant progression and relapse over time. Only to a lesser extent than 3% of cases, these lesions invade the lamina propria with features of malignancy [6]. On the treatment of TCCB, given the benignity of lesions in the pediatric population, the majority of Authors consider that it is sufficient just removal of the lesion transurethral. In our experience, only one patient, due to the particular endoscopic characteristics of the lesion, we felt necessary to administer intravesical a single dose of 40 mg of mytomicin –C post-resection . Several studies show, in fact, the positive effect of a single dose of the drug for immediate intravesical in patients with carcinomas of the bladder at low risk. These benefits seem to be limited in preventing an early recurrence of the disease, while little is known about the possibility that the drug may prevent recurrence in the long term. However, this approach is considered an alternative to the only clinical observation or chemotherapy intravesical protracted [7,8].
Management of TBBC in children after TURB varies among centers and paediatric guidelines are currently lacking [9].
The paucity of cases of TCC in the pediatric population has not yet allowed the drafting of a treatment protocol and follow-up for this condition. As for the follow-up in the literature sometimes AA suggest applying a more invasive protocol only in cases of invasion of the lamina propria by performing a cystoscopy every 3 months in the first year and then every year for 5 years [6]. In our experience we have considered sufficient subject our patients to ultrasound scans and urine cytology every 6 months for 1 year and then every year; and only 2 endoscopic control postoperatively.
Regarding the diagnosis, the bladder US has shown to be the gold standard of diagnostic tools but in case of differential diagnosis with eventual clots adherent to the bladder wall some authors have shown that MRI can be a useful diagnostic mean [10]. Another particular datum from our case-study is the absolute prevalence of girls while also in recent reports the prevalence is mainly constituted of boys [9,11].
Conclusion
The low incidence of TCC shows the rarity of this finding in the pediatric population and an unexpected exclusive prerogative of the female sex, in our experience. The main clinical manifestation of such injuries is hematuria; commonly these are solitary lesions, low-grade histology and low risk of progression.Our case studies show probably one of the longest follow-up in the literature and confirm that in this age group the prognosis also in the long term is particularly favorable.
References
- Javadpour N, Mostofi FK. Primary epithelial tumors of the bladder in the first two decades of life. J Urol. 1969; 101: 706-710.
- Benson RC Jr, Tomera KM, Kelalis PP. Transitional cell carcinoma of the bladder in children and adolescents. J Urol. 1983; 130: 54-55.
- Mottola A, Daniele G, De Benedetto A, Bianchi S. [Transitional cell carcinoma of the bladder in the first four decades of life]. Minerva Urol Nefrol. 1998; 50: 139-141.
- Samson W, Peter AF, Loui P, Dehner MB, Jonathan IA. Urothelial neoplasms in patients 20 years or young: a clinicopathological analysis using the world health organization 2004 bladder consensus classification. J Urol. 2005; 174: 1976-1980.
- Eble JN, Sauter G, Epstein JI, Sesterhenn IA. Pathology and genetics of tumor of the urinary system and male genital organs. In World Health Organization Classification of Tumors. 2004; 89-123.
- Gülpinar O, Soygür T, Baltaci S, Akand M, Kankaya D. Transitional cell carcinoma of bladder with lamina propria invasion in a 10-year-old boy. Urology. 2006; 68: 204.
- Solsona E, Iborra I, Ricos JV, Monros JL, Casanova J, Dumont R. Effectiveness of a single immediate mitomycin C instillation in patients with low risk superficial bladder cancer: short and long-term followup. J Urol. 1999; 161: 1120-1123.
- Barghi MR, Rahamani MR. Immediate intravesical instillation of mitomycin C after transurethral resection of bladder tumor in patients with low-risk superficial transitional cell carcinoma of bladder. Urol J. 2006; 3: 220-224.
- Berrettini A, Castagnetti M, Salerno A, Nappo SG, Manzoni G, Rigamonti W, et al. Bladder urothelial neoplasms in pediatric age: experience at three tertiary centers. J Pediatr Urol. 2015; 11: 26.
- Rodriguez A, Burday D, Sexton W, Ahmad N, Pow-Sang JM. Urothelial carcinoma in a child. Arch Esp Urol. 2005; 58: 473-475.
- Huang H, Li X, Jin J. Treatment of bladder transitional cell carcinoma in children: a single center experience from China. Arch Iran Med. 2015; 18: 250-252.