
Case Report
Austin J Urol. 2016; 3(2): 1044.
A Case of Distal Vaginal Scarring following Cloacal Repair
Jacobson NS¹*, Stock JA² and Fantl JA¹
¹Urogynecology, Mount Sinai School of Medicine, New York
²Pediatric Urology, Mount Sinai School of Medicine, New York
*Corresponding author: Nina S. Jacobson, Mount Sinai School of Medicine, 1176 5th Ave, NY 10029, New York
Received: June 21, 2016; Accepted: July 14, 2016; Published: July 18, 2016
Abstract
Background: Newborns with severe cloacal malformations must undergo surgical reconstruction in infancy. Further surgical management during adulthood is often needed to restore specific functions.
Case: A 17 year old female presented with inability to engage in vaginal intercourse. She had undergone cloacal reconstruction in infancy. Pelvic exam revealed normal labia, a vaginal-urethral common opening <5mm and a fibrous scar at the distal vagina. Diagnostic evaluation included pelvic hydrosonovaginogram, Voiding Cystourethrogram (VCUG), MRI and Examination Under Anesthesia (EUA) with cystoscopy and vaginoscopy. Surgical repair consisted of a perineal flap vaginoplasty.
Summary and Conclusion: This report describes the importance of a thorough preoperative evaluation when managing gynecologic complications of a rare cloacal malformation. Vaginoplasty was performed without compromising bowel or bladder function.
Introduction
Cloacal malformations are rare and complex birth anomalies. They represent the most severe form of anorectal malformations. Failure of the urogenital septum to separate the cloacal membrane results in the urethra, vagina and rectum opening into a single common channel. The world wide incidence is estimated at approximately one in 50,000 live births [1]. Majority of data available on patients with these anomalies focus on urinary and fecal continence as primary outcome measures. Very few publications specifically address gynecologic and obstetric outcomes [2].
Case Presentation
A 17 year-old female presented with a history of a cloacal malformation repaired as an infant. The specifics of her anatomy at birth as well as those of her reconstructive surgery were unknown. The operative report was not available. The patient provided letters of correspondence between her surgeon and consulting physicians. Through these letters it became known that she underwent urethroplasty, vaginoplasty, anoplasty and temporary colostomy with reversal. Reconstruction involved laparotomy and the use of small bowel for vaginal replacement.
Additionally, the patient had a diagnosis of vesicoureteral reflux and reduced function of her right kidney. Menarche occurred at age 15 and was followed by regular menstrual cycles with significant dysmenorrhea. She reported continence of bladder and bowel. The primary reason for consultation was the inability to engage in vaginal intercourse and an unsuccessful self-motivated trial of vaginal dilators.
Pelvic examination revealed normal labia and a vaginal-urethral common opening <5mm at the external urethral meatus site. However, the actual urethral meatus was not visible. A fibrous scar was seen between the anus and the common opening which allowed indentation upon digital pressure (Figure 1). Diagnostic imaging included apelvic hydrosonovaginogram, Voiding Cystourethrogram (VCUG) and MRI.
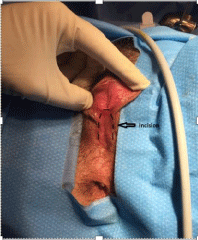
Figure 1: Pre-operative exam demonstrating location of incision.
Hydrosonovaginogram revealed a potential vaginal space behind the introital fibrous scar. This vaginal space measured 6.7 cm length x 2.6 cm antero-posterior x 4.1 cm width with narrowing of the distal 2cm. The thickness of the fibrous scar was asymmetric, measuring4.4mm anteriorly and 2.5mm posteriorly. The distance from the urethra to rectum was 2.6cm. VCU Gallowed verification of the common channel between the vaginal space and the urethra. It also revealed that the contrast filled the vaginal space after voiding (Figure 2).
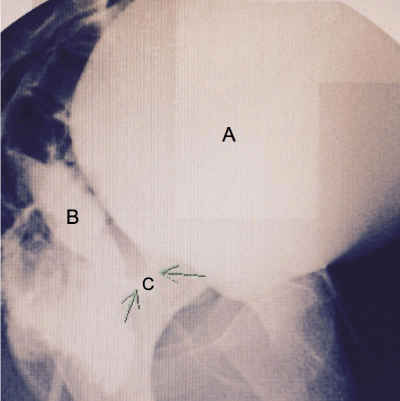
Figure 2: Voiding Cystourethrogram (VCUG). A. Bladder. B. Vaginal Space
C. Common Channel.
MRI was requested for additional information on the remaining pelvic structures. A unicornuate uterus with a noncommunicating left rudimentary horn, bilateral hydrosalpinx, and an urachal remnant were observed. The perineal fibrous scar replacing the distal vagina at the region of the introitus was again measured with similar results to those seen on VCUG.
Examination under anesthesia, cystoscopy and vaginoscopy under general anesthesia were subsequently performed. The cystoscopy confirmed a common channel ending with the cervixposteriorly and the bladder anteriorly. Evaluation of the bladder was normal and the distance from the cervix to the common opening was >10cm.
The corrective procedure included an inverted U-shaped incision which was made over the fibrous perineal scar and development of a flap with a posterior base (Figure 1). The incision was extended proximally towards the common channel. The vaginal opening was then dilated using Hagar dilators up to 10mm in diameter. The flap was then anchored along the posterior vaginal wall and the incision closed. Lubricated gauze was initially used for packing.
Post-operatively the patient used tampons covered with lubricated condoms as dilators until medical grade vaginal dilators were tolerated. She was able to advance to a 2cm dilator at 6 weeks with modest discomfort. Her vagina had healed well and there were no complications. At 4 months she could advance a 1” diameter dilator 5-6cm deep, and accommodate the entire length of the examiner‘s index finger. At 7 months she advanced to a 1.5” diameter dilator with similar depth (Figure 3). Shereported improvement in dysmenorrhea but has not yet engaged in sexual intercourse.
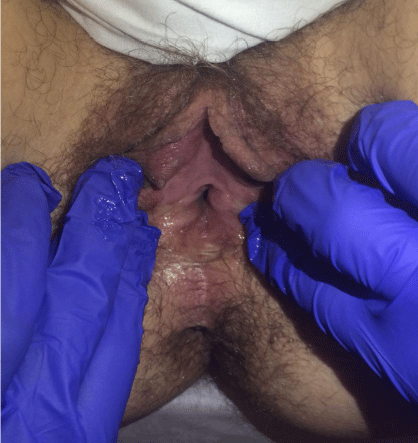
Figure 2: Post-operative exam at 4 months.
Summary and Conclusion
At seven weeks gestation the cloaca in normal human embryogenesis is a common chamber into which the primitive urinary tract, genital tract and bowel converge. A urorectal septum then descends and separates the rectum from the urogenital sinus. Lastly, the urogenital sinus differentiates into the urinary and genital tracts. When there is a cloacal malformation, the vagina, urethra and rectum are fused creating a channel that opens into a common opening. The length of the channel varies from 1 to 10cm, with an average length of 3cm. Associated defects are common. Infants with a cloaca need a colostomy at birth with efforts made to leave a long enough distal colon for subsequent reconstruction [3].
Corrective surgery is typically performed in the neonatal period and depends on the extent of the defect. In general, cloacal defects are classified according to the length of the common channel: =3cm 3 to 5cm, or >5cm [4].
Surgical approaches have evolved since the 1980’s. At that time the posterior sagittal anorectovaginoplasty was the most commonly performed operation. This involved separating the rectum from the urogenital tract, followed by separation of the vagina from the urethra and bladder. The common channel was then reconstructed as a neo-urethra, the vagina placed posterior to the urethra, and finally rectum placed within limits of the external anal sphincter [3]. In 1996 the Total Urogenital Mobilization (TUM) was introduced. The operative time was dramatically reduced and led to better functional results. TUM involves en-bloc mobilization of the urethra and vagina towards the perineum and creating separate openings. When the common opening is 3 to 5cm, a transabdominal approach may be required. Separation of the lower urinary from the genital tract as well as vaginal replacement with intestinal tract may be needed [4]. For cases with cloacas >5cm, the common channel is left intact. Laparotomy is usually required to separate the vagina and rectum from the trigone or bladder neck [3].
Treatment goals after reconstruction for these anomalies include urinary control, bowel control, and potential for sexual and obstetrical function later in life. Studies on long-term outcomes often focus on bowel and bladder control. There is less data on the gynecologic and sexual function considerations.
Menstrual abnormalities, sexual dysfunction and infertility are common. Menstruation is complicated by obstruction. The etiology is usually vaginal and/or cervical stenosis. Up to 40% of those with obstruction may experience hematometra or hematocolpos, often with associated dysmenorrhea [2].
Inability to engage in sexual intercourse after initial reconstruction in infancy has been reported. One review of 19 patients revealed that 56% of those who had a vaginoplasty required further vaginal reconstruction to facilitate menstruation or sexual activity. Less than half of these patients were sexually active [5]. Pregnancy is rare and cesarean section is recommended as mode of delivery.
Other than gynecologic abnormalities, cloacal malformations are also associated with structural renal anomalies in up to 83% of cases, and vesicoureteral reflux in over half. Less common are spinal, gastrointestinal and cardiac abnormalities [2].
This is a case of cloacal malformation reconstructed in infancy. The patient was likely born with a common channel measuring >3cm. The vagina was either partially or totally replaced with small bowel and she was urine and bowel-continent at presentation. The distal vaginal scar prevented her from engaging in vaginal intercourse. The main concern prior to surgery was the risk of disturbing her urine and bowel function while achieving ability to engage in vaginal intercourse. A thorough evaluation aimed to reach such objectives. Imaging and additional examination under anesthesia and cystoscopy confirmed a safe distance between the urethra and rectum to perform a U-shaped vaginoplasty without compromising the previously reconstructed urethra and anus.
References
- Hendren WH. Cloaca, the most severe degree of imperforate anus: experience with 195 cases. Ann Surg. 1998; 228: 331.
- Cardamone S, Creighton S. A gynecologic perspective on cloacal malformations. Curr Opin Obstet Gynecol. 2015; 27: 345.
- Levitt MA, Pena A. Cloacal malformations: lessons learned from 490 cases. Semin Pediatr Surg, 2010; 19: 128.
- Pena A. Surgical management of cloacal malformations: a review of 339 patients. J Pediatr Surg, 2004. 39: 470.
- Couchman A, Creighton SM, Wood D. Adolescent and adult outcomes in women following childhood vaginal reconstruction for cloacal anomaly. J Urol. 2015; 193: 1819.