Abstract
Background: Pain, functional limitations of upper extremities and sleep disorders are important problems that affect the quality of life and daily activities. Pain is one of the most common symptoms observed in patients with Carpal Tunnel Syndrome (CTS). Because pain limits the upper extremities’ functions and adversely affects sleep quality, the daily activities of the individuals are limited, and their quality of life is impaired.
Aim: To assess pain, upper extremity functions and sleeps quality in participant with CTS.
Objectives: The purpose of this study is to determine if sensory therapy is a beneficial modality to relieves pain, improve participants’ sleep quality and upper extremity functions in patients with CTS.
Methods: Thirty volunteers (27 females and 3 males) diagnosed with CTS, ages from 33 to 68 years, and were included in the study. Demographic characteristics were noted, pain intensity, upper extremity functions and sleep quality of the subjects were assessed. Pain intensity using the Visual Analog Scale (VAS), upper extremity functions using Shoulder and Hand Disabilities of the Arm (DASH), and sleep quality were measured Pittsburgh Sleep Quality Index (PSQI).
Study type: Randomized, double-blind study.
Results: When the values before and after the sensory therapy were compared, a significant decrease (p˂0.05) was found in the pain intensity at rest, with activity, and during day and night. Additionally, differences in DASH and PSQI values showed statistically significant improvement in both upper extremity functions and sleep quality (both p˂0.05).
Conclusion: In the light of the study results, we concluded that sensory therapy improves sleep quality and upper extremity functions, and that it relieves pain symptoms in patients with CTS.
Keywords: Carpal tunnel syndrome; Sensory therapy; Sleep quality
Abbreviations
CTS: Carpal Tunnel Syndrome; VAS: Visual Analog Scale; DASH: Disabilities of the Arm, Shoulder and Hand; PSQI: Pittsburg Sleep Quality Index; BMI: Body Mass Index; TENS: Transcutaneous Electrical Nerve Stimulation
Introduction
Carpal Tunnel Syndrome (CTS) is the clinical term for the pain that occurs in association with the compression of median nerve during gliding of the nerve between carpal bones and transverse ligaments; it is the most common focal compression neuropathy of upper extremities. Clinical symptoms are nocturnal paresthesia, pain, decrease in grip strength and loss of function in the hand [1,2]. An increase in pain intensity during night and dysesthesia are observed in 80% of patients. The etiology is multifactorial; most cases are classified as idiopathic [3]. It is frequent in females aged 30–50, and occurs five times more frequently in females than in males [4].
The patients with CTS awake from sleep frequently during the night with pain and paresthesia symptoms. This is thought to be associated with increased pressure on the carpal tunnel resulting from wrong positioning of the hand [5]. Increased pain and paresthesia during the night leads to frequent sleep interruptions, an increase in duration of sleep interruptions and napping, and consequently to a decrease in sleep quality [6,7]. Impaired sleep quality is an important problem because it may adversely affect daily activities and life quality as fatigue and pain increase. One study has shown that many diseases associated with pain affect sleep quality [8].
Treatment of CTS is generally classified as conservative or surgical. Surgical treatment is preferred for severe cases (e.g., denervation of the median nerve), whereas conservative treatment is preferred for cases with mild to moderate CTS [9]. Methods such as oral steroids, local steroid injections, physiotherapy, electrotherapy, splinting and modifications in the working environment and sensory treatment are also used during conservative treatment [10,11]. The efficacy of different conservative approaches has been examined by several studies [2,9]. Sensory therapy based on the teaching of new senses and establishing the relationship with the old sense of the sensory memory. There are three phases of sensory therapy: Early Phase is focus on moving touch, continuous touch, pressure and the localization of tactile senses; Late Phase is passed when moving and continuous touch sense is return, purpose of that is to facilities tactile sense; Compensation Training. The efficacy of sensory therapy has also been shown through assessments of clinical and electro diagnostic evidence [11]. However, to our knowledge, no study investigating the effect of sensory treatment on patients’ sleep quality has been performed to date.
The purpose of this study is to subject the patients with CTS to sensory therapy and to investigate its effects on upper extremity functions and sleep quality.
Materials and Methods
This experimental research study was conducted on participants with CTS applied to Physiotherapy and Rehabilitation Department of Beydagi State Hospital (Malatya, Turkey). It is a randomised, doubleblind study. The randomised, double-blind study is an experimental procedure in which neither the subjects of the experiment nor the persons administering the experiment know the critical aspects of the experiment nor the people participating in the trial are randomly allocated. The sample of the study consisted of patients with CTS who applied to the Physiotherapy and Rehabilitation Department of Beydağı State Hospital (Malatya, Turkey). The participants who were included in the study were selected out of the sample that who volunteered and fulfilled the inclusion criteria of the study was included in accordance with the random improbable sampling method. The power analysis that was conducted using the software NCSS PASS suggested that a sample number of 30 achieves a statistical power of 80% at 5% level of significance with a 95% confidence interval. Thirty-five persons diagnosed with CTS, ages 33 to 68 years, were enrolled in the study. Two participants was quitted the treatment for decrease in pain and paresthesia, and did not attend the control in the third week, two participants was withdrew and did not attend in the third week without any explanation, one participant was do local steroid injection while the treatment continued after five of the original participants withdrew from the study, the total sample number was 30 (27 females and 3 males).
Selection criteria
The criteria for inclusion in the study were: not having any cognitive, mental, psychological or neurological problems; no medical record of diabetes mellitus; having a positive score on at least one of the CTS-specific tests (Phalen, Reverse Phalen, Tinel’s and Carpal Compression Tests); and not having been subjected to any medical treatment, steroid injection or surgical treatment in relation to CTS.
Procedure
Prior to the study, all participants in the study were informed verbally and in writing about the purpose and duration of the study; the forms used for assessment and the assessment process itself; then, the patient’s approval was obtained. Demographical details of the participants such as age, height, weight, body mass index (BMI) and dominant hand were recorded. The side of the CTS and CTSrelated symptoms were recorded, and the pain intensity, anomalies and functionality of upper extremities and sleep quality were assessed before and after the therapy. The Visual Analog Scale (VAS), used for assessment of the pain intensity, is a scaled measurement of 10 cm in length where there are two extremes, with zero corresponding to no pain and ten corresponding to an unbearable amount of pain [12]. The participants are asked to mark the pain intensity on the scale, and the length of the interval between the mark and zero point corresponds to the pain intensity of the patient.
The Disabilities of the Arm, Shoulder and Hand (DASH) was used to assess anomalies and upper extremity functions. DASH assesses changes in functionality due to wounding of upper extremities, anomalies, limitations in activities, workforce effects and extracurricular activities [13,14]. DASH has been shown to be a valid and reliable method to assess upper extremity entrapment neuropathies, and the reliability and validity of the questionnaire for a Turkish population has been tested previously [15,16]. The questionnaire, which consists of three sections and 38 questions in total, was filled out by each participating patient: they were asked to mark the most appropriate answer (1: no difficulty, 2: mild difficulty, 3: moderate difficulty, 4: severe difficulty and 5: unable). The survey yields a score of 0 to 100, and the higher the score, the more severe the disability.
The Pittsburgh Sleep Quality Index (PSQI) was used to assess sleep quality. Using 19 questions, PSQI measures seven components, including subjective sleep quality over the last month, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleeping medications, and daytime dysfunction. Each component has a range of 0 to 3 points, and the global score is calculated by summing the scores of each component. A global score ≤5 is indicative of good sleep quality, whereas a score >5 is indicative of poor sleep quality [17]. The validity and reliability of this test was tested for a Turkish population, and its coefficient of internal consistency was reported to be 0.80 [18].
The sensory therapy was applied to the participants for 30 minutes five days per week and continued for three weeks and after three weeks pain intensity, upper extremity functions, sleep quality of the subjects were assessed again (Figure 1). The therapy was performed using different objects sequentially. Spiky balls were used for massaging in all directions during 2 min to apply pressure on paresthesia areas on the hand and to stimulate the sense of touch. Various parts of the hand were tapped. Rougher and softer sides of a sponge, as well as a material made up of a soft metal, were sequentially slid over various parts of the hand. A brush was used for massaging that followed sliding a piece of cotton over various parts of hands. The hands were dipped into a bowl filled with sand and macaroni. The participants touched surfaces covered with different types of fabrics. The length of the duration of the treatments with each object was two minutes. Lastly, conventional Transcutaneous Electrical Nerve Stimulation (TENS) was performed with Chattanooga (ELSA Corp.), each with four rounds, carbon-impregnated rubber electrodes 4 cm in diameter. The participants were received conventional TENS (pulse frequency 100 Hz, pulse amplitude 100 mA, pulse duration 100 μs and pulse pattern continuous) once a day for 4 minute periods for three weeks.
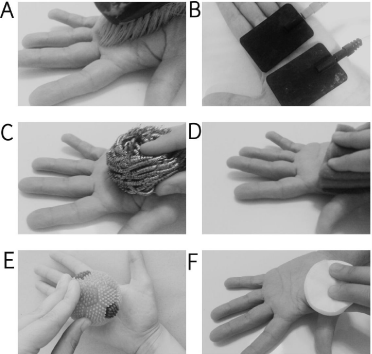
Figure 1: Sensory Training: (A) Brush; (B) TENS; (C) Soft metal material; (D)
Sponge; (E) Spiky balls; (F) Cotton.
Statistical analysis
SPSS for Windows Version 16 was used for the analysis of the data. Standard deviation was calculated for all variables. A paired sample t-test was used for calculations because its parametric conditions were met and the differences between pairs were normally distributed. A significance level (p) 0.05 was chosen.
Results
The study, which aimed to investigate the effect of sensory therapy on sleep quality, was conducted on thirty persons previously diagnosed with CTS. The average age of participants in the study was 49.8 ± 8.03, BMI28.1 ± 2.42, housewife ratio of participants 27 (90%). The demographical characteristics obtained prior to the study are presented (Table 1). Bilateral hand affected the ratio of participants 15 (50%), ratio of the dominant hand affected 26 (86.7%). The data regarding participants’ dominant hand, affected hand and professions were summarized (Table 2). Pain intensities compared before and after the treatment showed statistically significant decreases (p<0.05) in pain intensity at rest, with activity, and during day and night (Table 3). When DASH and PSQI results before and after the treatment were compared, a significant amount of decrease (p<0.05) was found for both scales (Figures 2 & 3).
n=30
Min
Max
X ± SD
Age (year)
33.00
68.00
49.8 ±8.03
Height (cm)
145
193
163±8
Weight (kg)
8.00
94.00
71.7±14.9
BMI (kg/m²)
21.70
32.40
28.1±2.42
X: Mean; SD: Standard Deviation; Min: Minimum; Max: Maximum; BMI: Body Mass Index.
Table 1: Demographic characteristics of individuals.
n
%
Gender
Male
Female
30
3
27
10
90
Dominant hand
Right
Left
26
4
86.7
13.3
Affected hand
Right
Left
11
4
36.7
13.3
Bilateral affected
15
50
Job
Housewife
27
3
90
10
Table 2: Dominant hand, affected hand and professional features.
n=30
Before
sensory training
X ± SD
After
sensory training
X ± SD
p
Rest Pain
5.53±2.78
4.47±2.73
0.000*
Night Pain
6.73±3.00
5.60±3.05
0.000*
Morning Pain
4.81±2.92
3.92±2.72
0.003*
Activity Pain
7.18±2.88
5.65±2.82
0.000*
X: Mean; SD: Standard Deviation; p<0.05’; *: Paired Sample; T: Test.
Table 3: Comparison of pain level of individuals before and after sensory training.
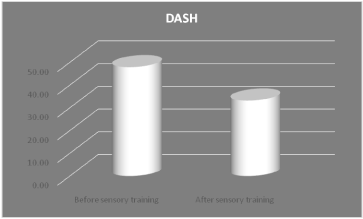
Figure 2: Comparison of DASH scores of individuals before and after
sensory training.

Figure 3: Comparison of PSQI scores of individuals before and after sensory
training.
Discussion
This study showed that sensory therapy positively affects the sleep quality and upper extremity functions of patients with CTS. Previous studies investigating the distribution of CTS according to age, class and gender found that CTS is two to ten times more frequent in females than males [19,20]. In our study, onset of the disease was found to be on average at age 49 years; 90% of the participants were female. Both findings are in agreement with the literature. In our study, the female to male ratio was calculated as nine.
In the literature, CTS is observed bilaterally in 76% to 87% of the cases, and the dominant hand is affected more frequently [21]. In our study, the ratios were similar to ones reported in the literature. Fiftyfive percent of the patients with CTS suffer from bilateral entrapment, and the dominant hand is affected first and more severely in bilateral cases. The dominant hand is also affected more frequently in unilateral cases in the literature [20]. The percentage of bilateral involvement was 95% in our study. Involvement of the dominant hand was also more frequent in our participants with unilateral involvement.
It has been reported that obesity is an independent risk factor for CTS; 70% of CTS cases suffer from obesity in persons with a BMI 29- 31 kg/m² [22]. Another study reported that a high BMI is a risk factor for CTS [23]. In our study, the obesity ratios and BMI values were similar to those reported in the literature.
Although studies on housewives reported an association between housework and CTS [24,25], whether activities such as handicraft are risk factors for CTS have not yet been investigated. In our study, the proportion of housewives was 90%among the female participants; therefore, being a housewife was determined to be a risk factor for CTS.
Symptoms such as numbness and pain are observed in the distribution of nervus medianus (the first three fingers on the palmar side and radial side of the fourth finger) in CTS, and these two symptoms are those most frequently reported [26]. Assessment of pain during day and night, at rest and with activity in our study enabled a detailed analysis of pain. Pain and paresthesia were observed in all participants (100%). Previous studies showed that sensory therapy decreases pain and numbness in persons with CTS [11]. The sensory therapy that we applied to our participants was found to contribute to a decrease in pain during day and night, and between pain at rest and during activity.
It has been reported that application of sensory treatment to 18 patients with CTS for five times a week for two weeks significantly improved the sense of light touch, pressure and the two-point discrimination. Therefore, it was suggested that inclusion of the sensory therapy in the rehabilitation programme could increase the sense of touch and improve using hands functionally [11,27]. Sensory therapy has been shown to improve hand functions that were restricted; this improvement results from its decompressing the carpal tunnel [28]. The effect of the therapy on hand functions was found to be concordant with the literature in our study as well.
The DASH questionnaire is frequently used to assess the upper extremity anomalies [16]. A study on CTS showed that sensory therapy increases the DASH scores significantly and improved upper extremity functions [29]. In our study, decrease in the score of upper extremity anomalies and progress in the upper extremity functions were found following the treatment.
It has been shown in the literature that sleep quality is significantly impaired in patients with CTS [30]. The researchers concluded that individuals with CTS experience sleep interruptions more often than do persons without CTS, and that the scores related to sleep disturbance indexes are higher for CTS patients. They also found that nocturnal paresthesia is the most important factor that interrupts the sleep in individuals with CTS [30]. This study supports our results, as sleep quality in our participants with CTS was also previously impaired. However, the effect of sensory therapy on sleep quality had not been studied to date. In our study, significant improvements in sleep quality were detected in participants with CTS; therefore, it was concluded that sensory therapy is a promising method than can be used to increase sleep quality of participants with CTS and to relieve the symptoms.
Limitations of the Study
Not having used objective sleep assessment techniques and a relatively low sample size are important limitations of this study. Future studies involving sleep laboratories are required.
Conclusion
To conclude, sleep quality of the patients with CTS is significantly impaired, and their sleep duration during the night decreases. It was concluded that sensory therapy, in addition to conservative treatments, will contribute to improvements in patients’ sleep quality and upper extremity functions, and will relieve the symptoms of CTS.
References
- Vogelin E, Meszaros T, Schoni F, Constantinescu MA. Sonographic wrist measurements and detection of anatomical features in carpal tunnel syndrome. J The scientific World. 2014; 657906: 1-6.
- Alfonso C, Jann S, Massa R, Torreggiani A. Diagnosis, treatment and follow-up of the carpal tunnel syndrome: a review. Neurol Sci. 2010; 3: 243-252.
- Thurston A. Carpal tunnel syndrome. Orthop Trauma. 2013; 27: 332-341.
- Maddali Bongi S, Signorini M, Bassetti M, Del Rosso A, Orlandi M, De Scisciolo G. A manual therapy intervention improves symptoms in patients with carpal tunnel syndrome. Rheumatol Int. 2013; 33: 1233–1241.
- McCabe SJ, Uebele AL, Pihur V, Rosales RS, Atroshi I. Epidemiologic associations of carpal tunnel syndrome and sleep position: is there a case for causation? Hand. 2007; 2: 127-134.
- Zarrabian MM, Johnson M, Kriellaars D. Relationship between sleep, pain, and disability in patients with spinal pathology. Arch Phys Med Rehabil. 2014; 95: 1504-1509.
- Lehtinen I, Kirjavainen T, Hurme M, Lauerma H, Martikainen K, Rauhala E. Sleep-related disorders in carpal tunnel syndrome. Acta Neurologica Scandinavica. 1996; 93: 360-365.
- Bigatti SM, Hernandez AM, Cronan TA, Rand KL. Sleep disturbances in fibromyalgia syndrome: relationship to pain and depression. Arthritis Rheum. 2008; 59: 961-967.
- Page MJ, Massy-Westropp N, O’Connor D, Pitt V. Splinting for carpal tunnel syndrome. Cochrane Database Syst Rev. 2012; 7: 010003.
- Huisstede BM, Hoogvliet P, Randsdorp MS, Glerum S, Van Middelkoop M, Koes BW. Carpal tunnel syndrome. Part I: effectiveness of nonsurgical treatments da systematic review. Arch Phys Med Rehabil. 2010; 91: 981-1004.
- Altuntaa O, Kayihan H. Idiopatik karpal tunel sendromunda duyu egitiminin etkisi. Turkish J Physiotherapy and Rehabilitation. 2014; 25: 016.
- Collins SL, Moore RA, McQuay HJ. The visual analogue pain intensity scale: what is moderate pain in millimetres? Pain. 1997; 72: 95–97.
- Jester A, Harth A, Wind G, Germann G, Sauerbier M. Disabilities of the Arm, Shoulder and Hand (DASH) questionnaire: determining functional activity profiles in patients with upper extremity disorders. J of Hand Surgery: British & European Volume. 2005; 30: 23-28.
- SooHoo NF, McDonald AP, Seiler JG, McGillivary GR. Evaluation of the construct validity of the DASH questionnaire by correlation to the SF-36. The Journal of hand surgery. 2002; 27: 537-541.
- Duger T, Yakut E, Oksuz C, Yorukan S, Bilgutay BS, Ayhan C, et al. Reliability and validity of the Turkish version of the disabilities of the Arm, Shoulder and Hand (DASH) questionnaire. Fizyoterapi Rehabilitasyon. 2006; 17: 99–107.
- Ebersole GC, Davidge K, Damiano M, Mackinnon SE. Validity and responsiveness of the DASH questionnaire as an outcome measure following ulnar nerve transposition for cubital tunnel syndrome. Plast Reconstr Surg. 2013; 132: 81-90.
- Buysse DJ, Reynolds CF, Monk TH, Hoch CC, Yeager AL, Kupfer DJ. Quantification of subjective sleep quality in healthy elderly men and women using the Pittsburgh Sleep Quality Index (PSQI). Sleep. 1991; 14: 331-338.
- Agargun YM, Kara H, Anlar O. The validity and reliability of the Pittsburgh sleep quality index. Turkish J Psych. 1996; 7: 107-111.
- Zambelis T, Tsivgoulis G, Karandreas N. Carpal tunnel syndrome: associations between risk factors and laterality. Eur Neurol. 2010; 63: 43-47.
- Mondelli M, Aprile I, Ballerini M, Ginanneschi F, Reale F, Romano C, et al. Sex differences in carpal tunnel syndrome: comparison of surgical and non-surgical populations. Eur J Neurol. 2005; 12: 976-983.
- Mondelli M, Giannini F, Giacchi M. Carpal tunnel syndrome incidence in a general population. Neurology. 2002; 58: 289-294.
- Moghtaderi A, Izadi S, Sharafadinzadeh N. An evaluation of gender, body mass index, wrist circumference and wrist ratio as independent risk factors for carpal tunnel syndrome. Acta Neurol Scand. 2005; 112: 375–379.
- Mondelli M, Curti S, Mattioli S, Aretini A, Ginanneschi F, Greco G, et al. Associations Between Body Anthropometric Measures and Severity of Carpal Tunnel Syndrome. Archives of Physical Medicine and Rehabilitation. 2016; 97: 1456-1464.
- Violante FS, Armstrong TJ, Fiorentini C, Graziosi F, Risi A, Venturi S, et al. Carpal tunnel syndrome and manual work: a longitudinal study. J Occup Environ Med. 2007; 49: 1189-1196.
- Tang X, Zhuang L, Lu Z. Carpal tunnel syndrome: a retrospective analysis of 202 cases and a one to one matched case-control study of 61 women pairs in relationship between manuel housework and carpal tunnel syndrome. J Chin Med. 1999; 112: 44-48.
- Maeda Y, Kettner N, Kim J, Kim H, Cina S, Malatesta C, et al. Primary somatosensory/motor cortical thickness distinguishes paresthesia-dominant from pain-dominant carpal tunnel syndrome. Pain. 2016; 157: 1085-1093.
- Jerosch-Herold C, Shepstone L, Miller L. Sensory re-learning after surgical treatment for carpal tunnel syndrome: a pilot clinical trial. Muscle Nerve. 2012; 46: 885–889.
- Jerosch-Herold C, Houghton J, Miller L, Shepstone L. Does sensory relearning improve tactile function after carpal tunnel decompression? A pragmatic, assessor-blinded, randomized clinical trial. Journal of Hand Surgery (European Volume). 2016; 1753193416657760.
- Chung VC, Ho RS, Liu S, Chong MK, Leung AW, Yip BH, et al. Elektroacupuncture and splinting versus splinting alone treat carpal tunnel syndrome: a randomized controlled trial. CMAJ. 2016; 151003.
- Patel JN, McCabe SJ, Myers J. Characteristics of sleep disturbance in patients with carpal tunnel syndrome. Hand (N Y). 2012; 7: 55-58.
