Abstract
Objective: The aim of this study was to evaluate the efficacy of Integrated Approach of Yoga Therapy (IAYT) as an add-on treatment for pain, tenderness, back disability, and spinal flexibility in patients undergoing conventional treatment for chronic low back ache.
Design: 120 patients suffering from Chronic Low Back Pain (CLBP), aged 18–75 years (yoga group = 41.29±15.87, control group = 41.63±13.48) from Ebnezar orthopedic center, Bengaluru were randomly assigned into2 groups-a yoga group and a control group-to receive IAYT or therapeutic exercises after intermittent lumbar traction and ultrasound (20 minutes per day). Both groups practiced supervised interventions for three weeks at the center and later, for 12 weeks, at their residences after the completion of treatment.
Outcome Measures: Both groups were assessed for pain, tenderness, back disability, and spinal flexibility on the 1st day in the pre-test and on the 21st day in the post-test. Data were analyzed using repeated measures analysis of variance (RMANOVA).
Results: There were significant differences within (RMANOVA, p<0.001) and between the groups (RMANOVA, p<0.001) in pain, tenderness, back disability, and spinal flexibility with greater improvement in the yoga group than in the control group. Pain in the yoga (39.9%, 66%, 85%, 98.9 %) and control (25.5%, 45%, 63%, 74%), tenderness in the yoga (60%, 81%, 95%, 99 %) and control (37%, 51%, 60%, 80.7%), back disability in the yoga (55%, 81%, 96%, 99.7 %) and control (35%, 53%, 63.8%, 80.7%), movements- flexion in yoga (77%, 126%, 183%, 232%) and control (33%, 64%, 99%, 132%), extension in yoga (75%, 113%, 130%, 132%) and control (34%, 68%, 102%, 121%), right lateral flexion in yoga (78%, 113%, 126%, 129%) and control (32%, 66%, 99%, 117%), left lateral rotation in yoga (76%, 109%, 119%, 120%) and control (33%, 67%, 100%, 113%), right lateral rotation in yoga (70%, 107%, 136%, 143%) and control (29%, 58%, 89%, 114%), left lateral rotation in yoga (66%, 103%, 129%, 130%) and control (28%, 55%, 84%, 107%). All these improved in the yoga group better than the control group on the 21st day, the 3rd month, the 6th month, and at one year, respectively.
Conclusion: IAYT an add-on to conventional physiotherapy provides significantly better improvement than therapeutic exercises alone in patients suffering from CLBP.
Keywords: Chronic low back pain; Integrated approach of yoga therapy; Therapeutic exercises; Physiotherapy
Introduction
Low back pain is a common condition comprising a major health problem worldwide [1]. Low back pain was identified by the Pan American Health Organization as one of the top three occupational health problems to be targeted by surveillance within the WHO Region of the Americas. Thirty-seven percent of Chronic Low Back Pain (CLBP) worldwide and 39% of CLBP in South East Asia, including India and China, is attributable to occupational ergonomic stressors, both physical and psychosocial [2]. Campbell, et al. report that in the United States the estimated annual cost to society of back pain is between £13 billion and £33 billion ($20–50 billion) [3]. Low back pain is the most prevalent musculoskeletal condition and the most common cause of disability in developed nations [4]. As part of the Global Burden of Disease 2010 Study (GBD 2010), the global burden of musculoskeletal conditions was estimated using updated methods that address the methodological limitations of previous GBD studies. Burden was expressed in Disability-Adjusted Life Years (DALYs) [5]. The lifetime prevalence of low back pain is estimated at 60–85%, while the annual prevalence in the general population ranges from 15–45% [6]. In about 85% of these cases, low back pain is secondary to nonspecific or functional causes, meaning that no specific underlying anatomic etiologic condition can be identified [7]. Back pain patients incur up to 75% more medical expenditures than patients without back pain [8]. The most commonly prescribed medications for low back pain are Nonsteroidal Anti-Inflammatory Drugs (NSAIDs), skeletal muscle relaxants, and opioid analgesics [9]. Benzodiazepines, systemic corticosteroids, antidepressant medications, and antileptic drugs are also prescribed [10]. According to Chou, et al. NSAIDs and skeletal muscle relaxants are moderately effective for short-term pain relief, while tricyclic antidepressants showed small to moderate effects; there was also fair evidence that acetaminophen, tramadol, benzodiazepines, and gabapentin provide pain relief [9]. The utilization rates for injection therapies have risen about 250% between 1994 and 2001; however, the evidence for these therapies is controversial [11]. Lastly, surgical treatment of non-specific low back pain has not been shown to be reliably successful [12]. Depending on the outcome measure or surgery utilized, “success” rates for surgery for low back pain only range from 40% to 65% [11]. Patients who do not improve after treatment with self-care activities and/or medications are good candidates for non-pharmacological treatments. Non-pharmacological treatments include physical treatments (i.e., heat, ice, ultrasound, and massage therapy), spinal manipulation and forms of injection therapy [9]. A biopsychosocial approach is now considered to be the gold standard for treating chronic pain [13].
Although the causal relationship between psychological symptoms and CLBP is complex, research evidence indicates that psychological symptoms often improve in low back pain patients after exercise interventions, even if the interventions were not specifically designed to affect the psychological symptoms. Conversely, placebo or sham treatments for low back pain have not resulted in significant changes in psychological symptoms. Data from the National Center for Complementary and Alternative Medicine (NCCAM) show that the usage of Complementary and Alternative Medicine (CAM) treatments for all conditions is on the rise in the US [11]. Reviews, meta-analyses, [14–16] and practice guidelines from the American Pain Society and the American College of Physicians [9] support yoga as an evidence-based treatment for CLBP with at least moderate benefit. Five large (n = 90–313) and five smaller Randomized Controlled Trials (RCTs) (n = 20–60) support yoga’s effectiveness for reducing pain and improving function in adults with CLBP [17]. The present research was planned to study the effects of yoga as an adjunct to physiotherapy-the standard conventional treatment in the management of chronic low back ache-as there were no studies on chronic low back ache comparing yoga to physiotherapy [18].
Methodology
One hundred twenty patients with CLBP from the outpatient department of Ebnezar Orthopedic Center, Parimala Health Care Services, and Bengaluru were recruited for the study. A sample size of 120 was obtained by calculating the effect sizes based on the mean and standard deviation of an earlier published interventional study [19] (Table 1) includes the baseline characteristics. One hundred twenty patients of both genders with CLBP, aged 18–75 years, were included in the yoga group (41.29±15.87) and in the control group (41.63±13.48).
CHARACTERISTICS
YOGA
(N=57)
CONTROL (N=55)
Age (M±SD)
41.29±15.87
41.63±13.48
Sex
Males
35
27
Females
25
33
Occupation
Skilled workers
28
22
Semi-skilled workers
11
9
Unskilled workers
4
3
Others
17
26
Duration of the disease
<1yr
26
23
1-3yrs
18
19
3-5yrs
11
10
>5yrs
5
8
Co-Morbidities
Diabetes
4
6
Hypertension
10
9
Overweight/Obesity
2
3
Others
10
12
Table 1: Demographic data.
The inclusion criteria were: a) patients with CLBP with persistent pain > three months prior to recruitment due to common causes like muscle sprain, spinal stenosis, facet joint arthritis, occupational causes, unaccustomed activities, or improper posture; b) degenerative diseases (lumbar spondylitis); c) IVDP with or without neurological involvement, recurrent back aches, including both males and females aged 18-75 years who were advised physiotherapy by the consulting orthopedician were included in the study. It was ensured that these patients had no previous exposure to yoga. Exclusion criteria included the following: a) patients with CLBP with persistent pain < three months; b) CLBP due to uncommon causes such as congenital, traumatic, infective, inflammatory, neoplasm, metabolic, and degenerative conditions; c) patients who underwent surgeries; d) referred CLBP due to gynecological diseases, genitourinary problems, or gastrointestinal conditions; e) post-traumatic conditions and patients who were not willing to be part of the study. The study was approved by the institutional ethical committee, and signed informed consent was obtained from all the participants.
Design
This was a prospective randomized, parallel, active controlled study on patients with CLBP in the age range of 18-75 years. Patients attending the outpatient department of Ebnezar Orthopedic Center who satisfied the inclusion criteria were recruited for the study. After the initial screening for selection criteria, patients were assigned to either the yoga group or the control group. A computer-generated random number table (www.randomization.org) was used for randomization. Numbered envelopes concealed the sequence until the intervention was assigned. One hundred twenty patients suffering from CLBP were randomized into two groups: the yoga group and the control group.
Both groups were given conventional physiotherapy for 20 minutes using intermittent lumbar traction and ultrasound for three weeks. The control group received therapeutic exercises and Supine guided Rest (SR) for 40 minutes. The study group additionally received 40 minutes of IAYT, which consists of shithilikaranavyayamas (loosening practices), shaktivikasakavyayamas (strengthening practices), yogasanas, pranayama, meditation, and relaxation techniques.
The study group was taught integrated yoga, while the control group was taught non-yogic, back-specific physiotherapy exercises by certified therapists. Both groups were assessed for pain, tenderness, back disability, and flexibility on the first day in a pre-test and on the 21st day in a post-test. After this, participants were asked to practice at home daily for the next three months. Patients were asked to keep track of their practice daily in a diary provided for the maintenance of practice at home. Compliance was supervised by telephone calls once every three days, and a weekly review was conducted once a week for 12 weeks. The daily review cards were checked for regularity; any questions on the part of the participants were answered. The evaluation was conducted by the senior research fellow. All patients were asked to mark their home practice daily in the diary provided for this purpose; at every visit, their clinical progress and therapy received that day were documented. Assessments were carried out on the first day, the 21st day, the 3rd month, the 6th month, and at one year.
Intervention for the yoga group
The schedule at the center for the yoga group included 40 minutes of IAYT practice after 20 minutes of physiotherapy with intermittent lumbar traction and ultrasound for three weeks. The IAYT practice included shithilikaranavyayamas (loosening practices) and saktivikasaka (strengthening practices) followed by yogasanas and relaxation techniques. Patients were later advised to continue the IAYT practice for 40 minutes at home for the next 12 weeks. The concept used to develop a specific module of IAYT for CLBP was taken from the traditional yoga scriptures (Patanjali yoga sutras, yoga vasishtha, and upanishads), which highlight a holistic lifestyle for positive health at physical, mental, emotional, and intellectual levels [20] (Table 2).
Conventional physiotherapy: Was carried out at the center for 21 days which included
20.0 min
a) Intermittent lumbar traction -10 min
b) Ultrasound – 10 min
Integrated yoga therapy practice: The patient was made to practice at the center for 40 min for 21 days after the conventional physiotherapy and later was advised to continue at home for the next 3 months. This included the following practices:
40.0 min
Shithilikarana vyayama (loosening practices):
10.0 min
1. Foot and ankle loosening practices
Passive rotation of each toe (clockwise and counterclockwise)
5 rounds
0.5 min
Toe bending
10 rounds
0.5 min
Passive rotation of ankle (clockwise and counterclockwise)
10 rounds
0.5 min
Ankle bending
10 rounds
0.5 min
Ankle rotation (clockwise and counterclockwise)
10 rounds
0.5 min
2. Knee loosening practices
Bending the knee in prone position
5 rounds
0.5 min
Knee bending – both sides
10 rounds
0.5 min
Knee rotation – both sides
10 rounds
0.5 min
Passive patella rotation
5 rounds
0.5 min
3. Hip and waist loosening practices
Half butterfly
10 rounds
0.5 min
Full butterfly
10 rounds
0.5 min
Waist rotations (both internal and external)
10 rounds
0.5 min
4. Upper limbs loosening practices
Finger loosening
5 rounds
0.5 min
Wrist loosening
5 rounds
0.5 min
Wrist rotation (clockwise and counterclockwise)
10 rounds
0.5 min
Elbow loosening
10 rounds
0.5 min
Shoulder loosening
10 rounds
0.5 min
5. Neck loosening practices
Forward and backward bending
5 rounds
0.5 min
Sideward tilting
5 rounds
0.5 min
Neck rotation (both clockwise and counterclockwise )
5 rounds
0.5 min
6. Relaxation: Instant
2.0 min
7. Strengthening exercises (sakti vikaasaka suksma vyayama)
5.0 min
Lumbar stretch
5 rounds
1.0 min
Crossed lumbar stretch
5 rounds
1.0 min
Straight leg-raise breathing: single and both legs
5 rounds
1.0 min
Setubandhasana lumbar stretch
5 rounds
1.0 min
Pavanamuktasana lumbar stretch
5 rounds
1. min
8. Quick relaxation technique: Consists of three phases involving observing the abdominal movements, synchronizing them with breathing, and chanting of ‘‘A’’ kara, wherein ‘‘A’’ is the mantra.
3.0 min
9. Yogasanas
10.0 min
Table 2: Yoga module for chronic low back ache.
Yogic sukshma vyayamas (loosening and strengthening practices): These are safe, rhythmic, repetitive stretching movements synchronized with breathing. These practices mobilize and strengthen the joints and muscles. Relaxation techniques: Three types of guided relaxation techniques were interspersed between the physical practices of sukshmavyayamas and asanas. Asanas (physical postures): Asanas are characterized by the effortless maintenance of the final posture by internal awareness. Asanas were selected in standing, supine, and prone positions that would relax and strengthen the back. Pranayama: The practice of voluntary regulated breathing while the mind is directed to the flow of breath is called pranayama. These practices promote autonomic balance through mastery of the mind. Meditation: Patanjali defines meditation (dhyana) as the effortless flow of a single thought in the mind without distractions (pratyaya ekataanata dhyanam). This has been shown to offer physiologic benefits through alert rest to the mind-body complex. Counseling: Yogic concepts of health and disease, yama, niyama, bhakti yoga, Jnana yoga, and karma yoga were addressed in the counseling classes. These sessions were aimed at understanding the need for lifestyle change, weight management, and preventing early aging by yogic self-management of psychosocial stresses.
Intervention for the control group
The routine schedule of the control group included 40 minutes of therapeutic exercises with supine guided rest after 20 minutes of physiotherapy with intermittent lumbar traction and interferential therapy for two weeks (Table 3). Therapeutic exercises included loosening and strengthening practices for all the joints of the upper and lower limbs, specific back practices, and supine rest. Later patient was advised to continue the therapeutic exercise practice of 40 minutes at home for the next 12 weeks.
Conventional physiotherapy: was carried out only at the center for 21 days and included
20.0 min
a) Intermittent lumbar traction -10 min
b) Ultrasound – 10 min
Therapeutic practices: The patient was made to practice at the center for 40 min for 21 days after the conventional physiotherapy and later was advised to continue at home for the next 3 months. This included the following practices:
40.0 min
Loosening exercises
10 min
1. Foot and Ankle
• Passive rotation of the toes (each toe clockwise and counterclockwise) 10 rounds 0.5 min
10 rounds
0.5 min
• Passive rotation of the ankle (both clockwise and counterclockwise)
10 rounds
0.5 min
• Toe bending
10 rounds
0.5 min
• Ankle bending
10 rounds
0.5 min
• Ankle rotation
10 rounds
0.5 min
2. Knee
• Knee bending- both sides
10 rounds
0.5 min
• Knee rotation- both sides
10 rounds
0.5 min
3. Hip and waist loosening practices
• Half butterfly
10 rounds
0.6 min
• Full butterfly
10 rounds
0.6 min
• Waist rotations (both internal and external)
10 rounds
0.5 min
4. Upper limb loosening practices
• Finger loosening
10 rounds
0.6 min
• Wrist loosening
10 rounds
0.6 min
• Wrist rotation (both clockwise and counterclockwise)
10 rounds
0.5 min
• Elbow loosening
5 rounds
0.5 min
• Arm loosening (both forward and backward movements)
10 rounds
0.5 min
5. Neck loosening practices
• Forward and backward bending
10 rounds
0.5 min
• Sideward tilting
5 rounds
0.5 min
• Neck rotation (both clockwise and counterclockwise)
5 rounds
0.5 min
6. Quick pause
2.0 min
7. Strengthening exercises
5.0 min
• Palm exercises
5 rounds
0.5 min
• Elbow exercises
10 rounds
0.5 min
• Arm exercises
5 rounds
0.5 min
• Back exercises
5 rounds
0.5 min
• Thigh exercises
5 rounds
0.5 min
• Calf exercises
5 rounds
0.5 min
8. Rest
3.0 min
9. Back specific practices
15.0 min
• Lumbar stretch
5 rounds
3 min
• Crossed lumbar stretch
5 rounds
3 min
• Straight leg raising (single/both)-30/60/90 degrees
5 rounds
5 min
• Pelvic tilt
5 rounds
4.0 min
10.Supine rest
5.0 min
Table 3: Control module for chronic low back ache.
Blinding and masking
Double blinding was not possible as this was an interventional study. The questionnaires were coded and analyzed only after the study was completed. The statistician who did the randomization and analyzed the data and the researcher who carried out the assessments were blinded to the treatment status of the subjects.
Outcome variables
The measures assessed were pain (using a numerical rating scale), back muscle tenderness, and back disability score and spinal flexibility.
Pain
A simple and reliable tool for measuring subjective pain consists of a horizontal straight line of 10 cm marked on a clean white sheet. One end of the line is marked 0 and represents “No pain”; the other end is marked 10, and it represents “Worst possible pain”. Patients were asked to mark the severity of their pain experienced over the 10cm scale. Separate sheets were used during every assessment [20].
Tenderness
xBack muscle tenderness was graded by the clinician using the following key: Grade 1 = tenderness on deep palpation; Grade 2 = patient winces on pressure; Grade 3 = patient winces and withdraws; and Grade 4 = patient does not allow one to touch [21].
Back disability score
This was assessed by the Oswestry Low back pain Disability Index (ODI), a self-administered questionnaire developed by Jones and Hunt, England (Fairbank, 2000) and used to measure disability. It consists of 50 questions broken into 10 sections: pain intensity, personal care, standing, sleeping, lifting, walking, sex life, social life, sitting, and travelling. Each item was scored by the patient on a 5-point scale (0-4). The scores for each of the 10 sections of the ODI are added, and the final score is expressed as “percent disability; the higher the score, more severe the disability [22].
Flexibility
Lumbar spinal flexibility was measured using a Lenthon Goniometer (dial-type goniometer of Anand Agencies, Pune) for the Flexion (F), Extension (E), Right Lateral Flexion (RLF), Left Lateral Flexion (LLF), Right Lateral Rotation (RLR), and Left Lateral Rotation (LLR) movements of the back.
Data sheets marked by all patients for pain (NRS) and (BDS) were coded and kept for future assessment. All measurements were taken before the intervention on the first day and after treatment on the 21st day.
Statistical methods
The data were analyzed using SPSS Version 10. The baseline values of the two groups were checked for normal distribution by Shapiro- Wilk’s test. Repeated measures analysis of variance (RMANOVA) with Bonferroni was used for assessing “within” and “between” group differences, respectively. (Tables 1 & 2) show the interventions of both study and control groups.
Results
The study profile is shown in (Figure 1). There were three dropouts in the study group and five in the control group. The two groups (60 subjects each) were similar with respect to socio-demographic and medical characteristics (Table 1). The baseline data for all the variables were normally distributed and did not differ significantly between the groups. (Table 4) shows the results between and within groups on the 21st day, the 3rd month, the 6th month and at one year. Results in the yoga group showed significance compared to the control groups for all the parameters.
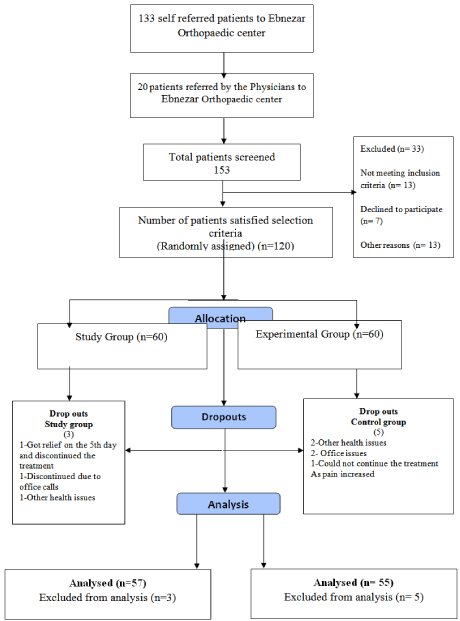
Figure 1: Trial profile.
1st Day
15th Day
1st Month
6th Month
1 Year
NRS
Control
9.22±1.05
6.84±0.96***
5.00±1.04***
3.40±0.87***
2.35±1.09***
Exp
8.68±1.05
5.21±1.61***
2.91±1.64***
1.26±1.22***
0.09±0.29***
Between groups
P values
0.008
<0.001
<0.001
<0.001
<0.001
TN
Control
3.58±0.50
2.24±0.51***
1.75±0.48***
1.42±0.57***
0.69±0.60***
Exp
3.35±0.77
1.33±0.69***
0.61±0.67***
0.16±0.37***
0.02±0.13***
Between groups
P values
0.062
<0.001
<0.001
<0.001
<0.001
BDS
Control
42.58±14.02
27.64±12.66***
19.82±10.21***
15.38±8.46***
8.18±6.93***
Exp
42.39±15.98
18.89±7.83***
7.79±5.22***
1.49±2.31***
0.11±0.45***
Between groups
P values
0.945
<0.001
<0.001
<0.001
<0.001
F
Control
16.22±4.39
21.62±4.54***
26.73±4.83***
32.29±5.06***
37.73±5.06***
Exp
17.16±4.86
30.42±6.19***
38.91±5.03***
48.67±6.04***
57.04±3.03***
Between groups
P values
0.286
<0.001
<0.001
<0.001
<0.001
E
Control
12.80±2.98
17.27±3.38***
21.55±3.49***
25.93±3.05***
28.33±1.97***
Exp
12.86±3.10
22.53±3.84***
27.40±2.69***
29.67±0.74***
29.93±0.37***
Between groups
P values
0.918
<0.001
<0.001
<0.001
<0.001
RLF
Control
12.85±3.14
17.04±3.53***
21.45±3.38***
25.64±2.93***
27.98±1.99***
Exp
13.04±3.36
23.23±3.57***
27.82±2.32***
29.58±0.84***
29.96±0.26***
Between groups
P values
0.77
<0.001
<0.001
<0.001
<0.001
LLF
Control
13.25±3.19
17.71±3.38***
22.15±3.37***
26.60±3.28***
28.31±2.16***
Exp
13.58±3.73
24.00±3.65***
28.40±2.53***
29.77±0.63***
30.00±0.00***
Between groups
P values
0.622
<0.001
<0.001
<0.001
<0.001
RLR
Control
16.24±4.29
20.95±4.13***
25.69±4.21***
30.76±4.27***
34.78±3.32***
Exp
16.33±4.36
27.81±4.47***
33.84±3.88***
38.65±1.83***
39.74±0.77***
Between groups
P values
0.909
<0.001
<0.001
<0.001
<0.001
LLR
Control
16.91±4.41
21.78±4.36***
26.27±4.92***
31.25±4.45***
35.11±3.64***
Exp
16.89±5.19
28.19±4.89***
34.35±4.09***
38.82±1.92***
38.91±5.32***
NRS: Numerical Rating Scale; TN: Tenderness; F: Flexion; E: Extension; RLF: Right Lateral Flexion; LLF: Left Lateral Flexion; RLR: Right Lateral Rotation; LLR: Left Lateral Rotation
Table 4: Results within and between groups.
Between group results
Pain: (Numerical rating scale): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 21st day (p<0.001), the 3rd month (p<0.001), the 6th month (p<0.001) and at one year (p<0.001) compared to the control group, indicating a reduction in pain scores.
Tenderness (TN): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating a reduction in tenderness.
Back disability score (Oswestry disability index): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating a reduction in back disability scores.
Spinal flexibility
A) Flexion: RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001) and at one year (p<0.001) as compared to the control group, indicating an improvement in the flexion movement of the spine.
B) Extension: RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating an improvement in the extension movement of spine.
C) Right Lateral Flexion (RLF): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p&0.001), and at one year (p<0.001) as compared to the control group, indicating an improvement in both right and left lateral flexion movements of the spine.
D) Left Lateral Flexion (LLF): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating an improvement in both the right and left lateral flexion movements of the spine.
E) Right Lateral Rotation (RLR): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating an improvement in both the right and left lateral rotation movements of the spine.
F) Left Lateral Rotation (LLR): RMANOVA with Bonferroni showed a significant difference in the yoga group on the 15th day (p<0.001), the first month (p<0.001), the 6th month (p<0.001), and at one year (p<0.001) as compared to the control group, indicating an improvement in both the right and left lateral rotation movements of the spine.
Within group results
Pain (Numerical rating scale): A significant reduction of pain scores was observed in the yoga group post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day). In the control group, a reduction of pain scores was observed in the post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day).
Tenderness (TN): A significant reduction of tenderness was observed in the yoga group post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day). In the control group, a significant reduction of tenderness was observed in the post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day).
Back disability score (Oswestry disability index): A significant reduction in back disability scores was observed in the yoga group post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day). In the control group, a significant reduction in back disability scores was observed in the post- assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day).
Spinal flexibility
A) Flexion: A significant improvement of flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
B) Extension: A significant improvement in extension was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
C) Right Lateral Flexion (RLF): A significant improvement in both right and left lateral flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
D) Left Lateral Flexion (LLF): Significant improvement in both right and left lateral flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
E) Right Lateral Rotation (RLR): Significant improvement in both right and left lateral rotation was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
F) Left Lateral Rotation (LLR): Significant improvement in both right and left lateral rotation was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
Within group results
Tenderness (TN): A significant reduction of tenderness was observed in the yoga group post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day). In the control group, a significant reduction of tenderness was observed in the post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day).
Back disability score (Oswestry disability index): A significant reduction in back disability scores was observed in the yoga group post-assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day). In the control group, a significant reduction in back disability scores was observed in the post- assessments (21st day, 3rd month, 6th month, and one year) as compared to the pre-assessments (first day).
Spinal flexibility
A) Flexion: A significant improvement of flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
B) Extension: A significant improvement in extension was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
C) Right Lateral Flexion (RLF): A significant improvement in both right and left lateral flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
D) Left Lateral Flexion (LLF): Significant improvement in both right and left lateral flexion was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
E) Right Lateral Rotation (RLR): Significant improvement in both right and left lateral rotation was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
F) Left Lateral Rotation (LLR): Significant improvement in both right and left lateral rotation was observed in the yoga group post-assessments (15th day, 1st month, 6th month, and one year) as compared to the pre-assessments (first day).
Discussion
This randomized active controlled trial on 120 participants included patients of both genders (M-62, F-58), aged 18-75 years with (CLBP). Results showed significantly greater improvement in the yoga group than the control group in reduction of pain, tenderness, and back disability (p<0.001, RMANOVA).
Despite the wide range of pharmacological, non-pharmacological and surgical treatment options currently available for patients with low back pain, a substantial proportion of patients fail to achieve adequate pain relief and continue to experience significant pain, pain-related distress, and disability [23]. Recent practice guidelines from the American College of Physicians and the American Pain Society suggest that if low back pain does not improve with standard pharmacological therapy and self-care, non-pharmacological treatments should be considered [9]. Approximately 40% of patients with chronic back pain report using complementary and alternative therapies such as massage, reflexology and acupuncture [24]. Yoga has also generated a great deal of interest and attention among the general public and the Western scientific community as an alternative treatment for a variety of chronic health conditions, including chronic pain. Yoga is an ancient practice that originated in India over 4,000 years ago and consists of several key components, including physical postures (asanas), breathing techniques (pranayama), relaxation, and meditation (dhyana) [25]. An estimated 14.9 million Americans practice yoga, 21% of whom use it for treating neck and back pain [26].
Yoga interventions impact multiple outcomes that are important to the health and well-being of people afflicted with chronic low back pain. Recent, high quality evidence suggests that yoga provides comparable effects to-and is more appealing than-formal stretching and strengthening programs led by physical therapists. Reviews, meta-analyses, and practice guidelines from the American Pain Society and the American College of Physicians support yoga as an evidence-based treatment for CLBP with at least moderate benefit [23]. Among the three peer-reviewed studies of yoga and CLBP that have been published, two of the studies evaluated an unspecified method of hatha yoga. One study lacked a control group, [27] while the other was not powered to reach statistical significance [28]. The third was a feasibility analysis of Iyengar yoga presenting only baseline data and therapy adherence rates [29]. However, no studies to date have compared yoga’s effectiveness to physiotherapy, the most common non-pharmacologic reimbursable treatment physicians recommend [30].
As per the above studies and their assessments discussed in a metaanalytic study, there are no studies to this date that has compared the effectiveness of yoga to physiotherapy. None of the studies of yoga and CLBP published so far have both a control and a yoga group, which is important to rule out the possibility of the benefits of yoga [23]. Hence, the present study was planned to evaluate the efficacy of yoga as an add-on to the conventional non-pharmacological treatment of CLBP, and it found a significantly greater reduction in pain, tenderness, and back disability in the yoga group than the control group.
Pain reduction
In a recent narrative systematic review of the literature, seven RCTs were identified that had been conducted on yoga for CLBP, and noted that yoga led to a significant reduction in pain intensity in five of the trials [14]. A study conducted by Wren, et al. reviewed six RCTs of yoga for CLBP and suggested that yoga shows promise in reducing pain, pain-related disability, negative mood, and pain medication among patients with CLBP [31]. Five large (n=90- 313) and five smaller randomized controlled trials (RCTs) (n=20- 60) support yoga’s effectiveness for reducing pain and improving function in adults with CLBP [17]. Studies have established the role of yoga in decreasing the pain and disability associated with CLBP, along with improved flexibility within one week to four months of yogic intervention with no adverse effects [32].
Recent research has also indicated that yoga can reduce pain catastrophizing, increase pain acceptance, and improve overall emotional functioning among individuals with chronic pain [33–36]. A number of studies have demonstrated the effectiveness of yoga in reducing pain in individuals with CLBP. For example, in addition to studying yoga’s effect on functional disability, [37] studies have also assessed clinical levels of pain, pain-related fears of movement, and pain attitudes. Their results suggested that, in addition to the yoga group having less functional disability post treatment, the yoga group demonstrated two times greater reduction in pain than the control group. In 2009, Saper, et al. [38]. found greater decreases in the pain scores of the yoga group as compared to the control group from baseline to 12 weeks. In a study conducted by Williams, et al. in 2009, individuals randomized to the yoga group showed greater improvements in pain intensity than those to the control group [39].
In Cox, et al.’s study of 2010, pain-related outcomes were measured using the Aberdeen back pain scale and pain efficacy; the study found a greater decrease of pain at the 4th week of follow-up in the yoga group than in the control group [40]. Tekur, et al. studied the efficacy of IAYT in patients with CLBP and documented a 49% reduction in numerical rating scale scores in the yoga group [32]. One of the studies on common neck pain and yoga, which assessed pain using a numerical rating scale, also showed a 95.5% reduction of pain in the yoga group compared to a 61.2% reduction in the control group [41]. One more study, conducted by Ebnezar, et al. on OA knees and yoga, found 37.31% and 64.88% pain reduction in the yoga group that was assessed using NRS on the 15th day and the 90th day, respectively [42]. A residential two-week yoga program that assessed pain using VAS reported a 55% pain reduction in the study group [43]. A 2003 study by Williams, et al. [44] an three-month out-patient program, found a 70% pain reduction in the yoga group. Another study, conducted by Groessel, et al. in 2008, [45] found a 14% pain reduction after 10 weeks of yoga in Veterans Administration (VA) patients with chronic back pain; in the current study, yoga was added after the conventional physiotherapy, which has shown a significant difference between and within groups (RMANOVA, p<0.001) with a greater reduction in the yoga group (by 39.9% on the 21st day, 66% by the 3rd month, 85% by the 6th month and 98.9% by one year) than the control group (25.5% by the 21st day, 45% by the 3rd month, 63% by the 6th month and 74% by one year.
Tenderness
The present study has shown a significant difference both between and within groups (RMANOVA, p<0.001) with a reduction of tenderness in the yoga group of 60% by the 21st day, 81% by the 3rd month, 95% by the 6th month, and 99% by one year as compared to the control group, which saw a reduction of 37% by the 21st day, 51% by the 3rd month, 60% by the 6th month, and 80.7% by one year.
Back disability
Most of the studies measuring functioning/disability have demonstrated the beneficial effects of yoga among adults with CLBP. Studies have established the role of yoga in decreasing the pain and disability associated with CLBP within one week to four months of yogic intervention with no adverse effects [32]. Williams, et al. conducted a randomized controlled trial to assess the impact of Iyengar yoga therapy in participants with non-specific chronic low back pain, and the results revealed less functional disability in the yoga group than in the control group at the post-treatment assessment with a 77% reduction in functional disability after 12 weeks [37]. In another study with an intensive residential yoga program, back disability was assessed using the ODI and results showed a significant difference between groups, with the yoga group experiencing a greater decrease in disability (69.2%) than the control group [32]. In the Williams, et al. study, individuals randomized to the yoga group showed greater improvements in functional disability than those randomized to the control group [39].
In a study by Sherman, et al. Vini yoga was used to treat CLBP on an out-patient basis, which showed approximately a 37% reduction at 6< week, 60% at 12 weeks, and 62% at the end of 26 weeks as assessed by the Roland Morris Disability Scale [46]. The present study has shown a significant difference both between and within groups (RMANOVA, p<0.001), with a reduction in back disability assessed by the ODI with three weeks of IAYT in the yoga group (55% by the 21st day, 81% by the 3rd month, 96% by the 6th month, and (99.7% by one year as compared to the control group (35% by the 21st day, 53% by the 3rd month, 63.8% by the 6th month, and 80.7% by one year).
Spine flexibility
Almost all studies of yoga intervention for treating CLBP measure physical functioning/disability as a primary outcome. It is viewed as a more reliable and objective measure of CLBP because it is often measured either by actual physiological performance or by questionnaires with items that are tied to specific behaviors [11]. Studies have established the role of yoga with improved flexibility within one week to four months of yogic intervention with no adverse effects [41]. In a study conducted Telles, et al. in 2008, [32] the yoga group demonstrated significant increases in handgrip strength for both hands and significant improvements in low back and hamstring flexibility. The efficacy of a week-long intensive residential yoga program on disability caused by pain and spinal flexibility in patients with CLBP was studied by Tekur, et al. In this study, Spinal Flexion (SF), Spinal Extension (SE), Right Lateral Flexion (RLF), and Left Lateral Flexion (LLF) were assessed; they found a significant improvement in SF by 28.3%, SE by 51.52%, RLF by 26.36%, and LLF by 39.15% in the first week, which did not change significantly after shifting to the control intervention in the second week. This points to the spill-over effect of yoga. In the control group, there was a nonsignificant improvement in the first week, followed by significant improvement in all the variables in the second week. The overall change at the end of two weeks in both groups was significant within groups but did not differ significantly between groups.
The present study has shown a significant difference both between and within groups (RMANOVA, p<0.001) with improvement of spinal flexibility of flexion in yoga (77%, 126%, 183%, 232%) and control (33%, 64%, 99%, 132%); extension in yoga (75%, 113%, 130%, 132%) and control (34%, 68%, 102%, 121%); right lateral flexion in yoga (78%, 113%, 126%, 129%) and control (32%, 66%, 99%, 117%); left lateral rotation in yoga (76%, 109%, 119%, 120%) and control (33%, 67%, 100%, 113%); right lateral rotation in yoga (70%, 107%, 136%, 143%) and control (29%, 58%, 89%, 114%); and left lateral rotation in yoga (66%, 103%, 129%, 130%) and control (28%, 55%, 84%, 107%). All these variables improved in the yoga group more than in the control group on the 21st day, the 3rd month, the 6th month, and at one year, respectively.
Mechanisms
Yoga and exercise bring about a decrease in cortical concentration, an increase in neurotransmitters, immune mediator, thereby improves cognition, sleep, negative symptoms, uplifts mood, lowers anxiety, and improves concentration [47]. Exercise is considered an acceptable method for improving and maintaining physical and emotional health. A growing body of evidence supports the belief that yoga benefits physical and mental health via. down-regulation of the Hypothalamic-Pituitary-Adrenal (HPA) axis and the Sympathetic Nervous System (SNS) [48].
Several factors would have contributed to the beneficial effects observed in both groups in this study. As noted in several earlier studies, physiotherapy intervention might increase blood flow. Better results in the yoga group may be due to its stress-reducing effect as yoga is meant to bring about better emotional stability and is achieved by a multifactorial approach that includes safe physical practices (asanas), breathing techniques (pranayama), meditation (dharana and dhyana), and introspective corrections in one’s cognitive errors by inputs at an intellectual (jnana yoga) and emotional level (bhakti yoga).
Yogasanas: It is known that physical exercise therapy plays an important role in the treatment of CLBP. Studies have shown that exercises help adult patients with CLBP return to normal daily activities and work, [50] decreases pain, and improves functional capacity in health care professionals [51]. Although yoga postures appear to be similar to many physical exercises, there are several basic differences. Yogic physical practices are mainly spinal stretches that are maintained with ease and effortlessness (Sthiramsukhamaasanam- Patanjali). Yoga postures offer voluntary introspective relaxation of the parts that are stretched; they are not just isometric exercises. The deep relaxation of the spinal muscles achieved during safe body movements with mindful awareness is another major factor that improves flexibility and reduces pain [32]. This is supported by earlier observations of increased paraspinal Electromyographic (EMG) activity during pain in subjects with CLBP [52]. Yoga has been shown to reduce EMG activity in conditions like chronic pain, especially headache [53].
Yogasanas reduce stiffness and increase flexibility of the spine. These yogasanas are practiced with deep internal awareness and relaxation. Stimulation comes in the form of a stretch during a movement, and once the stretch is at its peak (being maintained with ease and a calm mind), slowly returning to a resting position and sinking into deep relaxation. This process of a stretch followed by relaxation carried out with deep internal awareness (the process of alternate stimulation and relaxation) helps to erase deep-seated stress. When the final posture of the asana is maintained with relaxation, the deeper corrections take place. The prana blocks are diffused, giving a great sense of freedom from a stiff back [49]. Another explanation of yoga’s efficacy in pain reduction may lie in endorphin production at a cortical level, which is known to result from the alternating stretch and relax procedures of yogasana practice [54].
Om meditation: Studies on different types of meditation have consistently shown increased mental alertness even while being physiologically relaxed. In a previous study, Om chanting has been shown to bring about therapeutic effects in a functional neuroimaging study by decreasing the BOLD signal in limbic structures in healthy volunteers, similar to vagal nerve stimulation [55]. The Om meditation used in this study has also been shown to provide the same psycho-physiological rest seen in the earlier study. These yogic practices-be they physical, breathing, or mental-practiced independently or as a combination, seem to produce better mental alertness even while being physiologically relaxed, in both sick and healthy persons, which may account for the reduction in anxiety and depression [56]. In the present study, this physiological rest may form the basis of stress reduction, which reduces pain and disability in CLBP patients.
Relaxation: Oxygen consumption is used as a measure of the degree of rest or relaxation. When the body-mind complex is relaxed, the amount of oxygen used is much lower, and this can be measured by the oxygen we consume. Studies have shown that oxygen consumption decreased 10% after employing deep relaxation techniques. The yoga-based relaxation technique has also shown to reduce physiological signs of arousal [57]. A significant decrease in oxygen consumption and an increase in breath volume were recorded after guided relaxation. During yoga relaxation, the power of the low frequency component of the heart rate variability spectrum reduced, whereas the power of the high frequency component increased, suggesting reduced sympathetic activity. One study has also shown that a yoga-based isometric relaxation reduced physiological signs of anxiety [58] (Vempati, et al. 1999), indicating reduced sympathetic tone [59].
Pranayama: These practices remove the carbon dioxide from the body and cleanse the system. All the breathing exercises correct the rhythm of breathing by synchronizing body movements with inhalation and exhalation. Yogic breathing-or the pranayama-is a unique method for balancing the autonomic nervous system [60]. Research done on pranayama has shown that specific pranayama practices can have a relaxing effect on the sympathetic nervous system, thereby reducing stress levels [61]. Reduced anxiety scores, autonomic arousal, and Vanillylmandelic Acid (VMA) urinary VMA levels were found after the practice of IAYT in patients with generalized anxiety disorder [62]. Pranayama practices also reduce breath frequency to master emotional surges, and increase deep internal awareness in preparation for meditation [49].
Back-specific practices
The Setubandhasana lumbar stretch builds up the strength of the supporting postural lumbar spinal muscles. The dorsal stretch and straight leg rising (ekapadasana) help to build up the front (abdominal) support for the back. Pavanamuktasana practice provides a traction effect [10]. The current study also addresses some of the shortfalls of earlier studies, which may be helpful for future researchers. Although this study found yoga to be superior to “physical movements” and non-yogic breathing exercises on both pain and disability outcomes, it did not indicate the specific nature of the physical movements. In the present study, physical movements (or the therapeutic exercises and their nature) have been described in detail, the same as the study group intervention [3]. The first RCT of yoga for CLBP found that yoga led to statistically greater post-treatment improvements in functional status compared with a traditional exercise group (involving stretching, aerobic, and strengthening exercises). However, this effect was not clinically significant, and the effect dropped to a trend level of statistical significance by 14 weeks post-intervention [46]. Our study describes both the clinical and statistical significance of the post data and the follow-up data of the 3rd month, 6th month, and one year.
The limitations of most previous yoga studies include being nonrandomized, [63] a lack of validated outcome measures, a lack of data on dose response, and little examination of the underlying mechanisms. In addition, the yoga interventions being studied are often not well described [45]. One of the meta-analytical study raises two important issues: first, there is no study with an active control group on yoga and CLBP; and second, issue quoting that the treatment gains are attributable to the already established general benefits of physical activity for CLBP, and not specifically due to the effects of yoga [9,51]. The present study may fulfill both criteria, having both the study and an active control group and secondly, the study includes yoga as an add-on to the conventional physiotherapy. One more recent RCT that compared yoga with stretching (and a small number of strengthening exercises) failed to detect any significant differences in pain annoyance or disability between yoga and stretching groups at any given time [64]. These mixed findings suggest a need for further research that compares the efficacy of yoga with other forms of physical activity, including traditional exercise programs and alternative therapeutic approaches (e.g., pilates, tai chi) [23]. In the current study, yoga therapy has been added as a complement to the conventional physiotherapy with an active control group, and significant differences have been found for pain and disability.
According to one meta-analytic study, post-treatment adherence data presented in earlier studies suggest that the participants varied in the extent to which they maintained a regular yoga practice beyond the formal intervention period. This is not surprising, given that the study protocols themselves varied in the “prescribed” amount of yoga practice, both during the intervention and post-intervention [23]. By contrast, the present study protocol maintained a uniform schedule for assessing the regularity of practice both during the intervention and post-intervention. A study conducted by Holtzman, et al. [23]. also found that a number of other issues warrant attention in future research; for example, Woodyard, et al. state that the quality of yoga practice among patients with CLBP has received little attention. Although trials typically assess the quantity of yoga practiced (e.g., number of minutes) during the intervention phase, they do not appear to assess whether patients are engaging postures correctly, with proper breath and focused attention to sensation. All of these components are presumed to be necessary to obtain the full benefits of a yoga practice [65].
Follow-up assessments
In a study by Posadzki, et al. the difference between the two groups became statistically significant at the three-month followup, when the yoga group reported a 70% decrease in present pain compared to the 38% reduction reported by the control group [14]. In the present study, the yoga group showed a 66% pain reduction at the three-month follow-up, 85% pain reduction at the 6th month, and 98% pain reduction at one year as compared to the control group, which saw a 45% reduction at the 3rd month, 63% at the 6th month, and 74% at the one year follow-up. Regarding the back disability, a study by Sherman, et al. that used Vini yoga on CLBP on an outpatient basis has shown about a 37% reduction at the 6 weeks, 60% at 12 weeks, and 62% at the end of 26 weeks as assessed by the Roland Morris Disability Scale [46].
Strengths of the study
The strengths of this study include the following points: 1) randomized controlled trial; 2) good sample size; 3) supervised matched intervention for both groups with the same duration;4) longer follow-ups of 3 months, 6 months, and one year with good compliance (3% dropouts); 5) intervention of the study is applicable for patients of all age groups. The results of this study have shown marked differences in all the variables between the groups and thus, can be considered by clinicians as evidence for incorporating the yoga module into the management of CLBP.
Implications of the study
The intervention of the present study is simple, easy to practice, and cost effective compared to the conventional management and helps in reducing the economic burden on patients suffering from CLBP.
Suggestions for future work
Studies using MRI and biochemical markers may shed light on the mechanisms. Longer follow-ups may be carried out to rule out the validity of the intervention.
Conclusion
An adjunctive program of the IAYT for CLBP improves spine flexibility and reduces pain and disability. IAYT offers a valuable addition as a non-pharmacological intervention and a complementary therapy in offering better relief to patients with CLBP.
Funding: Rajiv Gandhi Fellowship Scheme, University Grants Commission, New Delhi, India.
Acknowledgement
At first, we would like to thank Rajiv Gandhi Fellowship Scheme, University Grants Commission for funding this study. We are thankful to Dr. John Ebnezar for his support and valuable guidance throughout the course and we gratefully acknowledge him for permitting us to conduct the study at his hospital, Ebnezar Orthopedic Centre, Parimala Health Care Services, Bengaluru. We are also thankful to all the staff members of Ebnezar Orthopedic Center for their co-operation and continuous support. We would like to thank Mr. Balaram Pradhan, the statistician who helped us to figure out the results of the study.
References
- Frymoyer JW. Back Pain and Sciatica. N Engl J Med. 1988; 318: 291-300.
- Punnett L, Pruss-Utun A, Nelson DI, Fingerhut MA, Leigh J, Tak S, et al. Estimating the Global Burden of Low Back Pain Attributable to Combined Occupational Exposures. Am J Ind Med. 2005; 48: 459-469.
- Campbell MK, Elbourne DR, Altman DG. CONSORT group. CONSORT statement: Extension to Cluster Randomised Trials. BMJ. 2004; 328: 702- 708.
- Woolf A, Pfleger B. Burden of Major Musculoskeletal Conditions. Bull World Health Organ. 2003; 81; 646-656.
- Damian Hoy, Lyn March, Peter Brooks, Fiona Blyth, Anthony Woolf, Christopher Bain, et al. The Global Burden of Low Back Pain: Estimates from the Global Burden of Disease 2010 Study. Ann Rheum Dis. 2014; 73: 968- 974.
- Burton AK, Clarke RD, McClude TD, Tillotson KM. The Natural History of low back pain in adolescents. Spine. 1996; 21: 2323-28.
- Vuori IM. Dose-Response of Physical Activity and Low Back Pain, Osteoarthritis, and Osteoporosis. Med Sci Sports Exerc. 2001; 33; 551-586.
- Saper RB, Sherman KJ, Delitto A, Herman PM, Stevans J, Paris R, et al. Yoga vs. Physical Therapy vs. Education for Chronic Low Back Pain in Predominantly Minority Populations: Study Protocol for a Randomized Controlled Trial. Trials. 2014; 15: 67.
- Chou R, Qaseem A, Snow V, Casey D, Cross JT, Shekelle P, et al. Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society. Ann Intern Med. 2007; 147: 478-491.
- Di Iorio D, Henley E, Doughty A. A Survey of Primary Care Physician Practice Patterns and Adherence to Acute Low Back Problem Guidelines. Arch Fam Med. 2000; 9: 1015-1021.
- Groessl EJ, Sklar M, Chang D. Yoga as a Treatment for Low Back Pain: A Review of the Literature, Low Back Pain. Dr. Ali Asghar Norasteh (Ed.). 2012.
- Zigler J, Delamarter R, Spivak J, Linovitz RJ, Danielson GO, Haider TT, et al. Results of the Prospective, Randomized, Multicenter Food and Drug Administration Investigational Device Exemption Study of the ProDisc-L Total Disc Replacement Versus Circumferential Fusion for the Treatment of 1-Level Degenerative Disc Disease. Spine. 2007; 32: 1155-1162.
- Gatchel RJ, Peng YB, Peters ML, Fuchs PN, Turk DC. The Biopsychosocial Approach to Chronic Pain: Scientific Advances and Future Directions. Psychol Bull. 2007; 133: 581-624.
- Posadzki P, Ernst E. Yoga for Low Back Pain: A Systematic Review of Randomized Clinical Trials. Clin Rheumatol. 2011; 30: 1257-1262.
- Bussing A, Ostermann T, Ludtke R, Michalsen A. Effects of Yoga Interventions on Pain and Pain-Associated Disability: A Meta-Analysis. J Pain. 2012; 13: 1-9.
- Cramer H, Lauche R, Haller H, Dobos G. A Systematic Review and Meta- Analysis of Yoga for Low Back Pain. Clin J Pain. 2013; 29: 450-460.
- Saper RB, Sherman KJ, Delitto A, Herman PM, Stevans J, Paris R, et al. Yoga vs. Physical Therapy vs. Education for Chronic Low Back Pain in Predominantly Minority Populations: Study Protocol for a Randomized Controlled Trial. Trials. 2014; 15: 67.
- Freburger JK, Holmes GM, Carey TS. Physician Referrals to Physical Therapy for the Treatment of Musculoskeletal Conditions. Arch Phys Med Rehabil. 2003; 84: 1839-1849.
- Tekur P, Chametcha S, Hongasandra RN, Raghuram N. Effect of Yoga on Quality of Life of CLBP Patients: A Randomized Control Study. Int J Yoga. 2010; 3: 10-17.
- Pollard CA. Preliminary Validity Study of the Pain Disability Index. Percept or Index. 1984; 59: 974.
- Swash M, Glynn M. Hutchinson Clinical Manual. 22nd Ed. London: Elsevier Publications. 2005.
- Fairbank JC, Couper J, Davies JB, O’Brien JP. The Oswestry Low Back Pain Disability Questionnaire. Physiotherapy.1980; 66: 271-273.
- S Holtzman, RT Beggs. Yoga for Chronic Low Back Pain: A Meta-analysis of Randomized Controlled Trials. Pain Res Manag. 2013; 18: 267-272.
- Foltz V, St Pierre Y, Rozenberg S, Rossignol M, Bourgeois P, Joseph L, et al. Use of Complementary and Alternative Therapies by Patients with Self- Reported Chronic Pain Back: A Nation-Wide Survey in Canada. Joint Bone Spine. 2005; 72: 571-577.
- Carneiro KA, Rittenberg JD. The Role of Exercise and Alternative Treatments for Low Back Pain. Phys Med Rehabil Clin North Am. 2010; 21: 777-792.
- Saper RB, Phillips RS, Davis RB, Eisenberg DM. Prevalence and Patterns of Hatha Yoga Use in the United States. Poster presented at International Scientific Conference on Complementary, Alternative and Integrative Medicine Research, Boston, MA. Effect of Iyengar Yoga Therapy for Chronic Low Back Pain. 2002.
- Vidyasagar JVS, Prasad BN, Reddy V, Raju PS, Jayshankar M, Sampath K. Effects of Yoga Practices in Nonspecific Low Back Pain. Clin Proc NIMS. 1989; 4: 160-164.
- Galantino ML, Bzdewka TM, Eissler-Russo JL, Holbrook ML, Mogck EP, Geigle P, et al. The Impact of Modified Hatha Yoga on Chronic Low Back Pain: A Pilot Study. Altern Ther Health Med. 2004; 10: 56-59.
- Jacobs BP, Mehling W, Avins AL, Goldberg HA, Acree M, Lasater JH, et al. Feasibility of Conducting a Clinical Trial on Hatha Yoga for Chronic Low Back Pain: Methodological Lessons. Altern Ther Health Med. 2004; 10: 80–83.
- Freburger JK, Holmes GM, Carey TS. Physician Referrals to Physical Therapy for the Treatment of Musculoskeletal Conditions. Arch Phys Med Rehabil. 2003; 84: 1839-1849.
- Wren AA, Wright MA, Carson JW, Keefe FJ. Yoga for Persistent Pain: New Findings and Directions for an Ancient Practice. Pain. 2011; 152: 477-480.
- Tekur P, Singphow C, Nagendra HR, Raghuram N. Effect of Short-term Intensive Yoga Program on Pain, Functional Disability and Spinal Flexibility in Chronic Low Back Pain: A Randomized Control Study. J Altern Complem Med. 2008; 14: 637-644.
- Carson JW, Carson KM, Jones KD, Bennett RM, Wright CL, Mist SD. A Pilot Randomized Controlled Trial of the Yoga of Awareness Program in the Management of Fibromyalgia. Pain. 2010; 151: 530-539.
- Curtis K, Osadchuk A, Katz J. An Eight-Week Yoga Intervention is Associated with Improvements in Pain, Psychological Functioning, and Mindfulness, and Changes in Cortisol Levels in Women with Fibromyalgia. J Pain Res. 2011; 4: 189-201.
- John PJ, Sharma N, Sharma CM, Kankane A. Effectiveness of Yoga Therapy in the Treatment of Migraine without Aura: A Randomized Controlled Trial. Headache. 2007; 47: 654-661.
- Tilbrook HE, Cox H, Hewitt CE, Kang’ombe AR, Chuang LH, Jayakody S, et al. Yoga for Chronic Low Back Pain: a randomized trial. Ann Intern Med. 2011; 155: 569-578.
- Williams KA, Petronis J, Smith D, Goodrich D, Wu J, Ravi N, et al. Effect of Iyengar Yoga Therapy for Chronic Low Back Pain. Pain. 2005; 115: 107-117.
- Saper RB, Sherman KJ, Cullum-Dugan D, Davis RB, Phillips RS, Culpepper L. Yoga for Chronic Low Back Pain in a Predominantly Minority Population: A Pilot Randomized Controlled Trial. Altern Ther Health Med. 2009; 15: 18-27.
- Williams K, Abildso C, Steinberg L, Doyle E, Epstein B, Smith D, et al. Evaluation of the Effectiveness and Efficacy of Iyengar Yoga Therapy on Chronic Low Back Pain. Spine. 2009; 34: 2066-2076.
- Cox H, Tilbrook H, Aplin J, Semlyen A, Torgerson D, Trewhela A, et al. A Randomised Controlled Trial of Yoga for the Treatment of Chronic Low Back Pain: Results of a Pilot Study. Complement Ther Clin Pract. 2010; 16: 187- 193.
- Bali Y, Nagarathna R, John E, Nagendra HR. Complimentary Effect of Yogic Sound Resonance Relaxation Technique in Patients with Common Neck Pain. Int J Yoga. 2010; 3: 18-25.
- Ebnezar J, Nagarathna R, Yogitha B, Nagendra HR. Effects of an Integrated Approach of Hatha Yoga Therapy on Functional Disability, Pain, and Flexibility in Osteoarthritis of the Knee Joint: A Randomized Controlled Study. J Altern Complement Med. 2012; 18: 463-472.
- Pradhan B. Effect of Integrated Approach of Yoga Therapy for Back Pain. [Doctorate in Hindu Studies, Thesis] Orlando, Florida, USA: Hindu University of America. 2009.
- Williams K, Steinberg L, Petronis J. Therapeutic Application of Iyengar Yoga for Healing Chronic Low Back Pain. International Journal of Yoga Therapy. 2003; 13: 55-67.
- Groessl EJ, Weingar KR, Aschbacher K, Pada L, Baxi S. Yoga for Veterans with Chronic Low-Back Pain. J Altern Complement Med. 2008; 14: 1123- 1129.
- Sherman KJ, Cherkin DC, Erro J, Miglioretti DL, Deyo RA. Comparing Yoga, Exercise, and a Self-Care Book for Chronic Low Back Pain: A Randomized, Controlled Trial. Ann Intern Med. 2005; 143: 849.
- Balasubramaniam M, Telles S, Doraiswamy PM. Yoga on Our Minds: A Systematic Review of Yoga for Neuropsychiatric Disorders. Front Psychiatry. 2012; 3: 117.
- Ross A, Thomas S. The Health Benefits of Yoga and Exercise: A Review of Comparison Studies. J Altern Complement Med. 2010; 16: 3-12.
- Nagendra HR, Nagarathna R. Yoga for Back Pain. Bangalore: Vivekananda Kendra Prakashana. Reprint. 2016.
- Van Tulder M, Malmivaara A, Esmail R, Koes B. Exercise Therapy for Low Back Pain: A Systematic Review within the Framework of the Cochrane Collaboration Back Review Group. Spine. 2000; 25: 2784-2796.
- Hayden JA, Van Tulder MW, Tomlinson, G. Systematic Review: Strategies for Using Exercise Therapy to Improve Outcomes in Chronic Low Back Pain. Ann Intern Med. 2005; 142: 776-785.
- Fryer G, Morris T, Gibbons P. Paraspinal Muscles and Intervertebral Dysfunction: Part One. J Manipulative Physiol Ther. 2004; 27: 267-274.
- Padmashree G. Immediate Effect of Yogic Relaxation on Frontalis Surface EMG. [M.Sc, Thesis]. Bengaluru: Swami Vivekananda Yoga University. 2007.
- Kjaer TW, Bertelsen C, Piccini P, Brooks D, Alving J, Lou HC. Increased Dopamine Tone during Meditation-Induced Change of Consciousness. Brain Research Cognitive Brain Research. 2002; 13: 255-259.
- Kalyani BG, Venkatasubramanian G, Arasappa R, Rao NP, Kalmady SV, Behere RV, et al. Neurohemodynamic Correlates of “OM” Chanting: A Pilot Functional Magnetic Resonance Imaging Study. Int J Yoga. 2011; 4: 3-6.
- Telles S, Nagarathna R, Nagendra HR. Autonomic Changes during OM Meditation. Indian Journal of Physiology and Pharmacology. 1995; 39:418- 420.
- Vempati RP, Telles S. Yoga-Based Relaxation Reduces Sympathetic Activity Judged from Base Line Levels. Psychological Reports. 2002; 90: 487-494.
- Vempati RP, Telles S. Yoga Based Relaxation versus Supine Rest: A Study of Oxygen Consumption, Breath Rate and Volume and Autonomic Measures. Journal of Indian Psychology. 1999; 17: 46-52.
- Telles S, Nagaratna R, Nagendra HR, Desiraju T. Alterations in Auditory Middle Latency Evoked Potentials during Meditation on a Meaningful Syllable-OM. IJN International Journal of Neuroscience. 1994; 76:87–93.
- Brown RP, Gerbarg PL. Sudarshan Kriya Yogic Breathing in the Treatment of Stress, Anxiety, and Depression. Part II-Clinical Applications and Guidelines. J Altern Complement Med. 2005; 11: 711–717.
- Telles S, Nagarathna R, Nagendra HR. Breathing Through a Particular Nostril Can Alter Metabolism and Autonomic Activities. Indian J Physiol Pharmacol. 1994; 38: 133-137.
- Nagaratna R, Nagendra HR, Crisan HG, Seethalakshmi R. Yoga in Anxiety Neurosis – A Scientific Study. In: Proceedings of the International Symposium of the Royal College of Physicians and Surgeons of Glasgow. Update Medicine and Surgery. 1988; 192–196.
- Luskin F, Newell K, Griffith M, Holmes M, Telles S, DiNucci E, et al. A Review of Mind/Body Therapies in the Treatment of Musculoskeletal Disorders with Implications for the Elderly. Alternative Therapies in Health and Medicine. 2000; 6: 46–56.
- Sherman KJ, Cherkin DC, Wellman RD, Cook AJ, Hawkes RJ, Delaney K, et al. A Randomized Trial Comparing Yoga, Stretching, and a Self-Care Book for Chronic Low Back Pain. Arch Intern Med. 2011; 171: 2019–2026.
- Woodyard C. Exploring the Therapeutic Effects of Yoga and its Ability to Increase Quality of Life. Int J Yoga. 2011; 4: 49-54.
