Research Article
Austin J Cerebrovasc Dis & Stroke. 2014;1(3): 1013.
Distribution, Severity and Radiologic Features of Intracranial Stenosis in Asymptomatic Pakistanis
Ayeesha K Kamal1*, Farzin Majeed2, Muhammad S Ilyas3, Munawar Hussain4, Kamran Masood4, Bilal Ahmed5, Hasan Rehman6, Zafar Sajjad7 and Scott E Kasner8
1Department of Neurology and Stroke Service, Aga Khan University, Pakistan
2Fogarty Cerebrovascular Research Fellow, Aga Khan University, Pakistan
3Department of Neurology, Dow University of Health Sciences, Pakistan
4Department of Radiology, Dow University of Health Sciences, Pakistan
5Department of Epidemiology and Biostatistics, Aga KhanUniversity, Pakistan
6Department of Medicine, Aga Khan University, Pakistan
7Department of Radiology, Aga Khan University, Pakistan
8Department of Neurology, University of Pennsylvania, USA
*Corresponding author: Ayeesha Kamran Kamal, Department of Neurology, Aga Khan University, Stadium Road –74800, Karachi, Pakistan
Received: July 15, 2014; Accepted: August 15, 2014; Published: August 19, 2014
Abstract
Background: Intracranial atherosclerotic disease (ICAD) is the most common ischemic stroke subtype globally. It accounts for 30-50% of all ischemic strokes in Asians.
Aims: The aim of the study is to report the frequency of asymptomatic ICAD and its associated Magnetic Resonance Imaging (MRI) findings.
Methods: 200 adult participants were recruited from the Radiology Departments of two major diagnostic centers in Karachi. Eligible participants were confirmed for the absence of stroke symptoms via the Questionnaire for Verifying Stroke Free Status (QVSFS). QVSFS negative subjects underwent MRI on a 1.5 Tesla scanner. Images were centrally reviewed on Di com Viewer 3.0 with electronic calipers to calculate the degree of ICAD.
Results: Mean age of subjects was 37.1 years (S.D 15.1) with50.5% men (n=101) and 49.5% women (n=99).Asymptomatic ICAD was found in34.5% (n=69) subjects. Of the 3800 intracranial arteries studied, 2.2% (n=88) had biological disease. 20.5% (n=18) of these vessels had atherosclerotic irregularities, 43.2% (n=38) had mild stenos is, 11.4% (n=10) had moderate stenos is, 5.7% (n=5) had severe stenos is while 19.3% (n=17) were completely occluded. The posterior cerebral artery (42% of stenosed arteries, n=37) was most affected. 23.5% (n=47) of subjects had peri-ventricular lucencies, 10.5% (n=21) had brain atrophy while 3.5% (n=7) had silent brain infarcts. There was a significant association between asymptomatic ICAD and peri ventricular lucencies (PR 1.59; 95% CI 1.35-1.99).
Conclusion: Asymptomatic ICAD is common in young Pakistanis, with no gender predilection; it preferentially affects the posterior circulation. Silent infarcts are rare compared to peri ventricular lucencies and atrophy.
Keywords: Stroke; Intracranial Stenosis; Developing Countries; Asymptomatic; Radiology; Prevention; Epidemiology
Background
Two-thirds of stroke-related mortality worldwide is attributable to stroke in low and middle income countries [1]. Pakistan, currently the world’s sixth most populous nation [2,3], reports a1 in 4 lifetime prevalence of stroke symptoms over the age of 35 years [4]. Intracranial atherosclerotic disease (ICAD) is a major subtype of ischemic stroke [5] with an estimated prevalence of 20-54% amongst South Asians [6]. In fact, about 30-50% of all ischemic strokes in Asians occur due to ICAD [7].
The Karachi Intracranial Stenosis Study (KISS) [8], that looked at symptomatic ICAD stroke in hospitalized patients reported that 80% patients had significant concomitant asymptomatic stenosis (> 70% stenosis).
Aims
There is a relative paucity of data on asymptomatic ICAD especially from regions where it is most prevalent and wherein the window for intervention for primary prevention lies. The aim of the asymptomatic ICAD study is to determine the frequency of ICAD in those without clinically evident stroke and its associated Magnetic Resonance Angiography (MRA) findings. Findings from this study will help us determine the magnitude of asymptomatic ICAD in the Pakistani population and with it identifies the need to act early and focus on primary prevention.
Methods
We have summarized this study in this paper and provided relevant details. The entire study protocol is accessible at www. clinicaltrials.gov at Study ID: NCT0207287.
Study Design and Setting
A prospective cross-sectional study was carried out from March to June 2013 at the Radiology Departments of Aga Khan University [9] and Dow University of Health Sciences (DUHS) in Karachi.
Participating centers
Aga Khan University is a private not for profit academic center with a fee for service system. The Dow University Radiology Center is public sector, government funded and subsidized entity. Radiology departments in both centers are equipped with 1.5 Tesla MRI scanners.
City /Country setting
These centers are located in Karachi, Pakistan’s largest city with inhabitants of all ethnicities; Karachi has a population of 13 million inhabitants [10] and these centers cover the bulk of MRI scanning for the city and the country with combined volumes of greater than 2000 scans per month. These are general volumes of patient turnover.
Study population
We recruited adult Pakistani patients >18 years who presented to the participating centers for MRI Brain for indications other than transient ischemic attack (TIA) or stroke(headache, epilepsy, rhino sinusitis etc.). Subjects were required to have no clinical history of stroke or TIA, confirmed by a negative result on the Questionnaire to Verify Stroke-free Status (QVSFS).
Data collection procedures/ study flow
Non-probability purposive sampling was used to recruit consecutive patients prospectively from the two study sites. All eligible participants were screened for presence of stroke symptoms via QVSFS by trained data collectors after which an informed consent was taken for enrollment into the study. A previously tested Urdu version of QVSFS was used [4,11,12]. QVSFS consists of eight questions, six of which are related to stroke symptoms namely hemiplegia, hemi-anesthesia, hemianopia, loss of vision in one eye, inability to speak and inability to understand [13]. Those who consented to the study and were QVSFS negative were subject to detailed interview and an additional 5 minute Time of flight MRA without contrast was performed. Images were then collected on Compact Disks (CD) for centralized image viewing and quantification. The reviewers were experienced investigators who had previously systematically reviewed vasculature and were unaware of the medical history of the participant.
Data collection tools/ variables
A standardized Data collection form (DCF) was used to collect baseline demographic information.
A magnetic resonance imaging (MRI) reading form adapted from the work of Ward law [14,15] was used to review imaging findings. Modifications made to the form included using angiographic data to record information on cerebral vasculature. In each subject, 19 arteries (bilateral anterior cerebral arteries (A1&A2), bilateral middle cerebral arteries (M1&M2), bilateral posterior cerebral arteries, bilateral vertebral arteries, bilateral internal carotid artery- petrous bilateral internal carotid artery- cavernous, bilateral internal carotid artery- supraclinoid and basilar artery) were examined for the number, degree, and distribution of stenosis. Biologically relevant disease ranging from atherosclerotic irregularity to measurable stenosis was noted and measured. The following radiologic variables were noted : stroke [16], acute stroke lesions [17], silent brain infarcts [18], cortical infarcts [19], lacunar infarcts [19], atrophy [20], leukoaraiosis [21], arterial review [22,23]. All radiologic data were directly archived into a centralized computer using Dicom 3.0 software. The method used to calculate stenosis was adapted from the one used in the Warfarin versus Aspirin in Symptomatic Intracranial Disease [24] study which is as follows:
Percentage stenosis= [1- (Dstenosis/D normal)*100[14, 25]
Where D stenosis is the diameter of the artery at the site of the most severe stenosis, and D normal is the diameter of the proximal normal artery.
The software allowed zooming, panning, measurements, annotations and segmentation of the images. It has the ability to rotate (90, 180 degrees) and flip (horizontal, vertical) images. It also provides angle values which helps in measuring stenosis around corners. Intracranial occlusive lesions were rated by giving them 1 of 5 grades depending on the narrowness of the arteries as follows: <25% as atherosclerotic disease, 25% to 49% reduction as mild stenosis,50% to 74% reduction as moderate stenosis, 75% to 99% reduction as severe stenosis, and no opening graded as complete occlusion [17]. Any vessel that was congenitally absent or atretic was not counted as stenosed.
Peri ventricular lucency was classified according to the 3 point system proposed by van Swieten et al. [21].
Silent brain infarcts were defined as vascular disease manifesting as infarcts as detected on MRI in the absence of transient ischemic attack or stroke [18].
Ethical approval and human subjects’ protections
All participants provided written informed consent. This was taken after explaining the risks and benefits associated with taking part in the study. Ethical approval was taken from AKU Ethical Review Committee and the Institutional review board of DUHS. (ERC number 2327 CHS ERC 12 and IRB 360/DUHS 2012). All scans were reviewed within 24 hours by the radiology faculty and there was provision in the study to report any critical incidental findings like aneurysms first to the referring physician and in his absence or inability to contact , the report was communicated to the patient with an urgent specialist referral. All gathered data was numerically coded so as not to reveal the identity of the participants. All electronic transfer within centers was done through decoded CDs that were centralized to a single password protected workstation for analysis.
Sample size estimation
A minimum sample size of 200 participants was required in order to achieve 80 % power for detecting a minimum difference of 20% in the prevalence of radiological findings between asymptomatic ICAD positive and ICAD negative persons assuming a 1:3 ratio in patients with ICAD versus no ICAD and at a level of significance of 5%.
Statistical analysis
For categorical variables (brain atrophy, silent brain infarcts and peri-ventricular lucencies proportions were calculated. The independent contribution of any ICAD-associated finding was examined in the Univariate Cox proportional hazards model, which was used to calculate prevalence ratios. In order to compute the statistically adjusted Prevalence Ratios (PR), multivariable Cox regression analysis was done. The level of significance of ≤ 0.05 was set for the analysis. Statistical analyses were conducted using Statistical Package for Social Sciences (SPSS); Version 19.
Results
Mean age of the participants was 37.1 years (S.D 15.1 years) with nearly 62% (n=124) of the participants being younger than 40 years. There was a roughly equal proportion of males (50.5%, n=101) and females (49.5%, n=99) in the study (Table I – Demographic Data).
Frequency in patients
with ICAD
69 (34.5%)n (%)
Frequency in patients with no ICAD
131 (65.5%)
n (%)
Age (Years)
Mean (SD)
38.6 (15.1)
36.31 (15)
Gender
Males
Females
36(52.2%)
33 (47.8%)
65(49.6%)
66 (50.4%)
Clinical Risk factors
Diabetes
Hypertension
Dyslipidemia
CVD
A.Fib
4 (5.8%)
17 (24.6%)
7 (10.3%)
2 (2.9%)
1 (1.4%)
14 (10.7%)
36 (27.5%)
3 (2.2%)
1 (.8%)
2 (1.5%)
Table 1: Baseline Demographics of Participants.
MRI-MRA Findings
A total of 3800 intracranial arteries in 200 patients were studied. ICAD was found in 34.5% (n=69) of the subjects.
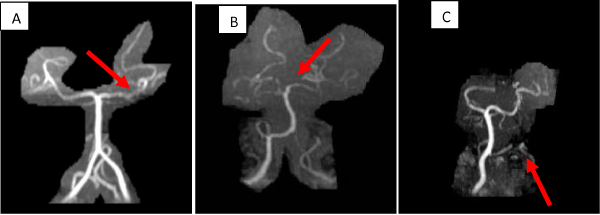
A total of 88 vessels were found to have any degree of stenosis. Of these, majority of the vessels were either mildly stenosed (43.2%, n=38) or had atherosclerotic irregularities (20.5%, n=18). The commonest artery affected was the posterior cerebral artery (PCA) (42% of stenosed arteries, n=37) followed by vertebral artery (34% of stenosed arteries, n=30). Detailed findings are presented in Table 2 (Figure 1).
MRI images showing Asymptomatic ICAD in the posterior circulation.
The arrows point at the point of stenosis in each vessel (A)Left Posterior Cerebral Artery (B) Right Posterior Communicating Artery (C) Left Vertebral Artery.
Figure 1 :MRI images showing Asymptomatic ICAD in the posterior circulation.
The arrows point at the point of stenosis in each vessel (A)Left Posterior Cerebral Artery (B) Right Posterior Communicating Artery (C) Left Vertebral Artery.
Vessel
<25%
25-49%
50-74%
75-99%
Complete occlusion
Total
MCA
5 (5.7%)
10 (11.4%)
5 (5.7%)
-
-
20 (22.7%)
ACA
-
1 (1.1%)
-
-
1 (1.1%)
Vertebral
3 (3.4%)
14 (16%)
1 (1.14%)
2 (2.27%)
10 (11.4%)
30 (34.1%)
PCA
10 (11.4%)
13 (14.7%)
4 (4.5%)
3 (3.4%)
7 (8%)
37 (42.0%)
Total
18 (20.5%)
38 (43.2%)
10 (11.4%)
5 (5.7%)
17 (19.7%)
88
Table 2: Stenosed Vessels by degree of stenosis and vessel type.
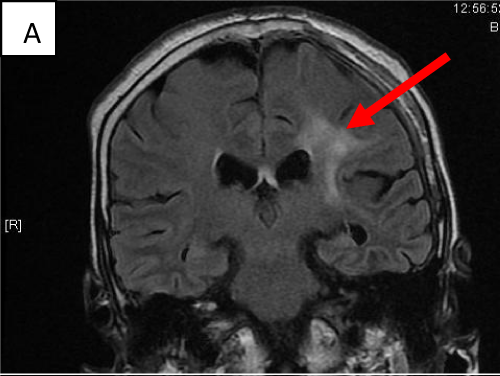
A mean of 1.3 vessels were diseased per patient (88 vessels in 69 subjects) among those who had ICAD with the highest number of affected vessels in a single patient being 3.3.5% (n=7) of all subjects had silent brain infarcts (Figure 2), 23.5% (n=47) subjects had peri-ventricular lucencies (Figure 3) while 10.5% (n=21) showed cortical brain atrophy (Figure 4). Peri-ventricular lucencies were found to be statistically associated with asymptomatic ICAD (PR 1.59; 95% CI 1.35-1.99) when Cox Regression analysis was applied. Asymptomatic ICAD was not significantly associated with brain atrophy or silent brain infarcts.
Silent brain infarct.
The Arrow points at the region of infarction.
Figure 2 :Silent brain infarct.
The Arrow points at the region of infarction.
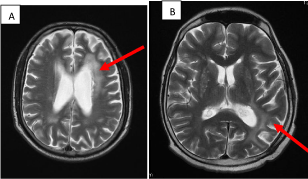
Periventricular Hyperintensities.
Increased signals as pointed by the arrows is evident on T2 images in the periventricular areas.
Figure 3 :Periventricular Hyperintensities.
Increased signals as pointed by the arrows is evident on T2 images in the periventricular areas.
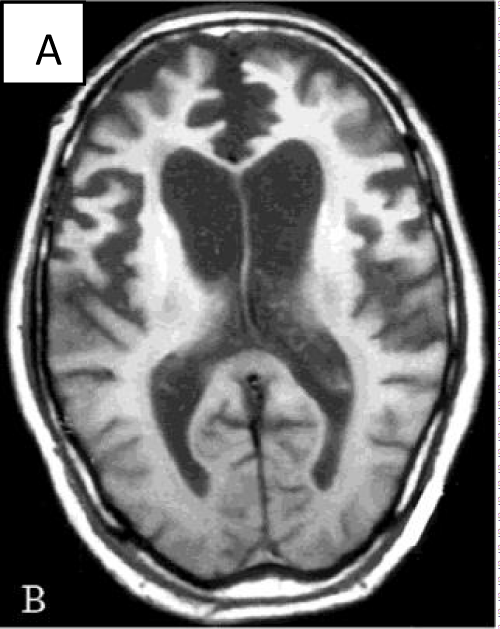
Brain volume reduction.
Diffuse reduction in brain volume is evident by the narrowing of gyri and widening of sulci.
Figure 4 :Brain volume reduction.
Diffuse reduction in brain volume is evident by the narrowing of gyri and widening of sulci.
Discussion
This study shows us that asymptomatic ICAD is present in approximately one third (34.5%, n=69) of Pakistani South Asians presenting for MRI without a history or symptoms of prior stroke. The most commonly affected arteries were the Posterior Cerebral arteries followed by Vertebral and Middle Cerebral arteries. Of all affected arteries, about 20% (n=17) showed complete occlusion in clinically silent areas.
Our reported prevalence (34%) is relatively higher than previously reported figures of 4-29 % in international data. This is particularly concerning since prior studies have targeted higher risk populations [26-28] as compared to the general population that was selected for our study. Regionally comparable data is sparse; however another study from Karachi on hospitalized stroke patients reported the prevalence of stenosis to be 80% on the asymptomatic side [29]. Other prevalence studies [28,30-37] in asymptomatic patients have mostly used transcranial Doppler ultrasound (TCD) for detecting ICAD which is less sensitive than an MRA for detecting stenosis and is limited to fewer and larger arteries (usually MCA) (Table 3).
Study
Population
Prevalence
Comments
Uehara et al
(2005) [40]
425 Japanese asymptomatic
patients requesting evaluation
for cerebrovascular disease via MRA
(mean age 64 � 20 years; 57% men)
3.5% for >=50%, 9.6% for >= 25%
Patients requesting cerebrovascular evaluation likely to have higher prevalence of risk factors and intracranial disease.
Huang et al
(2007) [35]
1,068 subjects aged = 50 years
from random population-based sample with no previous history of stroke or TIA, and adequate acoustic windows evaluated by TCD
5.9%
(MCA stenosis)
Only MCA studied
Wong et al
(2007)[33]
590 (92%) of geographically
defined Chinese population
aged=40 years. Accesses using Transcranial Doppler (TCD)
6.9%
Unclear if 52 of total 642� contacted are missing due to technically inadequate study or subject accessibility iss
es; 19 with previous history of stroke.
Tang et al
(2007) [37]
3057 Chinese patients aged > 50 yrs. with at least one vascular risk factor (hypertension, diabetes, and hyperlipidemia) and no prior stroke or TIA� were accessed using TCD
12.6%
(MCA stenosis)
The prevalence escalated quadratically with increasing number of associated factors: from 7.2% for one, to 29.6% for four associated factors.
Uehara et al
(2000) [27]
156 Japanese subjects with no evidence of stroke who presented at a neurologic clinic with concerns about a possible stroke(mean age 63 years) underwent MRA
14.7%
11.5% extra-cranial carotid stenosis.� Age and hypertension are significant predictors for intracranial artery stenosis. MRA is sufficiently efficient in patients in whom cerebral artery occlusive lesions is suspected.
Uehara&Tabuchi et al
(2001) [36]
151 Japanese asymptomatic patients scheduled to undergo CABG evaluated via MRA
21% with > 50% intracranial stenosis
16.6% subjects had extra cranial stenosis.
Park et al
(2006) [28]
835 asymptomatic Korean adults who voluntarily underwent a health screening examination and MRA. The subjects had no history of stroke or cardiovascular disease.
3%
ICAS was distributed as follows:
ACA�� 16%,�� MCA 52%,
PCA��� 26%, and distal internal carotid arteries 6.5%.
The ratio of ICAS to extra cranial atherosclerosis was 6:1.
Elmore et al
(2003) [34]
510 asymptomatic persons referred for carotid Doppler ultrasound (mean age 71 � 11 years, 50% men)
12.9%
Laboratory accuracy 93%, extra cranial carotid stenosis in 39.2%.
Thomas et al
(2004) [26]
2165 Chinese type II diabetic patients with no prior history of stroke (mean age 54� 11yrs.) evaluated using TCD.
29.6%
(MCA stenosis)
Age, hypertension and dyslipidemia were independent predictors of MCA stenosis.
Table 3: Prevalence Estimates of Asymptomatic Intracranial Stenosis in Asia.
The majority of our subjects were patients younger than 50 years. This finding is very much in line with the findings of another burden study from Karachi where the average age for stroke was 50 years [4]. Hence, our results reiterate the exceptionally high burden of atherosclerotic diseases at a relatively younger age in Pakistan.
Associated MRI findings showed that only 3.5% (n=7) of study subjects had silent cortical brain infarcts while 23.5% (n=47) had peri ventricular lucencies. Per ventricular lucencies are usually found as lacunars infarctions caused by occlusion of small penetrating cerebral arteries resulting from arteriosclerotic changes of parent cerebral arteries [38]. They are considered an important risk factor for clinical cerebrovascular disease in the general population and are strongly associated with small-vessel vasculopathy. We theorize that the small sub cortical strokes found in this population may be due to undetected hypertension causing direct small vessel disease and asymptomatic ICAD causing penetrator artery disease resulting in small sub cortical disease more frequently than silent cortical brain infarcts.
Atherosclerosis of the intracranial arteries has also been found to be associated with cerebral atrophy leading to cognitive impairment and dementia [35]. Whereas the majority of studies evaluating the relation of ICAD and brain volume reduction have been performed in symptomatic patients with severe stenosis, recent population based studies [33,37] have also suggested that asymptomatic intracranial atherosclerosis is also related to poorer neuropsychological [39] performance, even with mild degrees of stenosis.
We think that our observed higher proportion of ICAD is because we used a sensitive modality like MRI for detecting intracranial stenosis; our methods were standardized with the help of special software designed for measuring stenosis. International studies have mostly used Transcranial Doppler ultrasound for detecting ICAD which is less sensitive than an MRA for detecting stenosis; they have different cutoffs and also restrict their observations to single arteries compared to our observation of disease on the entire circle of Willis. We performed our literature search on PubMed using keywords asymptomatic ICAD, Intracranial Stenosis and limited our search to English articles only. We also searched accompanying references.
This study also has diagnostic limitations since we have not used a 4 vessel angiogram for diagnosing ICAD. This is because 4 Vessel angiography is an invasive procedure and it would be dangerous and unethical if used on otherwise healthy stroke free patients since it increases the risk of disabling stroke by 1.5 to 3 % [40], which is unacceptable ethically and doesn’t justify the risk of investigation. However we have used an excellent noninvasive tool with the same technical capacity at both centers. Thus the diagnostic limitations are homogenous in our study population. This study is also limited in that it is a study based on convenience sampling of participants presenting for MRI at diagnostic centers, thus it isn’t exactly a community based observation which would be a better representation of ICAD prevalence.
Our study has several strengths. We did not bias participation to those who were medically high risk (known HTN, DM, and PAD etc). We verified asymptomatic status using a validated questionnaire (QVSFS) and validated regionally applicable tools for risk assessment. We used the same diagnostic at both the centers and evaluated them with a centralized offline assessment performed by experienced investigators using a standardized definition and approach. We also had several limitations. We did not use a gold standard e.g. angiography, however a procedure with an inherent risk of stroke would not be ethically justified in stroke free participants. A 3.0 Tesla study with plaque characterization would have yielded more insight into pre stroke mechanisms. Although we were able to study a wide range of younger participants with no stroke risk factors, we were unable to randomly draw subjects from a community -based population due to resource limitations and logistics. Our study has applicability to mostly urban transitional Pakistan, as we do not have significant rural representation.
In conclusion, our observation of prevalent asymptomatic atherosclerosis in young participants supports the need for future global studies focused on community-based longitudinal imaging with increased precision to further define natural history and perhaps consider early prevention from strokes from symptomatic ICAD.
Acknowledgement
The authors would like to acknowledge the patience, kindness, time and cooperation of all patients and their families who contributed to this study. We would also like to take this opportunity to acknowledge and thank Aslam Hussain and Barkat Ali for study site recruitment work; Muhammad Jan and Anita Andani who performed data double entry; MRI technical Staff Mr and Ms. Hina Tejani for her excellent secretarial support, Mr. Sarwar at Dow Radiology, Ms. Dennis Fernandes, Mr. Salman Karim , Ms. Laila Ladak at the Clinical Trials Unit for administrative and logistic support. Dr. Azizunissa Irumnaz at the Clinical Trials Unit for her excellent support for staff training for ethics and Good Clinical Practice for all field and key staff. Abdul Muqeet at the AKDN e Health Resource center for support and standardization of Di COM on centralized review. Mr. Musa Khan and Mr. Khawaja Mustafa, the librarians for library assistance. Dr Romaina Iqbal for her intellectual input for Principal Component Analysis, In addition the stroke team would like to acknowledge the support of the Section of Neurology at AKUH who always facilitate logistically and provide protected time for all research endeavors.
Disclosures
Dr. Ayeesha Kamran Kamal is the co-director and recipient of grant entitled of The International Cerebrovascular Translational Clinical Research Training Program (Fogarty International Center, National Institutes of Health). Dr. Farzin Majeed is a neurovascular research fellow whose mentored research practicum training is currently funded by Award Number D43TW008660 from the Fogarty International Center and the National Institute of Neurologic Disorders and Stroke. Dr Ayeesha Kamran Kamal is also funded by Grand Challenges Canada, URC HEC. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Fogarty International Center, National Institute of Neurologic Disorders and Stroke or the National Institute of Health.
References
- Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012; 380: 2095-2128.
- Internet World Stats, top ten countries with the highest population.
- Population Census Organization. Census 2011. 2011
- Kamal AK, Itrat A, Murtaza M, Khan M, Rasheed A, Ali A, et al. The burden of stroke and transient ischemic attack in Pakistan: a community-based prevalence study. BMC Neurol. 2009; 9: 58.
- Wong LK. Global burden of intracranial atherosclerosis. Int J Stroke. 2006; 1: 158-159.
- Moussouttas M, Aguilar L, Fuentes K, Anyanwu B, Manassarians H, Papamitsakis N, et al. Cerebrovascular disease among patients from the Indian subcontinent. Neurology. 2006; 67: 894-896.
- Komotar RJ, Kellner CP, Raper DM, Strozyk D, Higashida RT, Meyers PM. Update on the natural history of intracranial atherosclerotic disease: A critical review. World J Radiol. 2010; 2: 166-171.
- Khan M, Rasheed A, Hashmi S, Zaidi M, Murtaza M, Akhtar S, et al. Stroke radiology and distinguishing characteristics of intracranial atherosclerotic disease in native South Asian Pakistanis. Int J Stroke. 2013; 8: 14-20.
- Iqbal MP, Yakub M. Smokeless tobacco use: a risk factor for hyperhomocysteinemia in a Pakistani population. PLoS One. 2013; 8: e83826.
- Hergens MP, Lambe M, Pershagen G, Terent A, Ye W. Smokeless tobacco and the risk of stroke. Epidemiology. 2008; 19: 794-799.
- Husain N, Creed F, Tomenson B. Depression and social stress in Pakistan. Psychol Med. 2000; 30: 395-402.
- Samir N, Mahmud S, Khuwaja AK. Prevalence of physical inactivity and barriers to physical activity among obese attendants at a community health-care center in Karachi, Pakistan. BMC Res Notes. 2011; 4: 174.
- Berger K, Hense HW, Rothdach A, Weltermann B, Keil U. A single question about prior stroke versus a stroke questionnaire to assess stroke prevalence in populations. Neuroepidemiology. 2000; 19: 245-257.
- Samuels OB, Joseph GJ, Lynn MJ, Smith HA, Chimowitz MI. A standardized method for measuring intracranial arterial stenosis. AJNR Am J Neuroradiol. 2000; 21: 643-646.
- Wardlaw J. Image Analysis Tools.
- Asplund K, Tuomilehto J, Stegmayr B, Wester PO, Tunstall-Pedoe H. Diagnostic criteria and quality control of the registration of stroke events in the MONICA project. Acta Med Scand Suppl. 1988; 728: 26-39.
- Wardlaw JM, Sellar R. A simple practical classification of cerebral infarcts on CT and its interobserver reliability. AJNR Am J Neuroradiol. 1994; 15: 1933-1939.
- Vermeer SE, Longstreth WT Jr, Koudstaal PJ. Silent brain infarcts: a systematic review. Lancet Neurol. 2007; 6: 611-619.
- Rovira A, Grivé E, Rovira A, Alvarez-Sabin J. Distribution territories and causative mechanisms of ischemic stroke. Eur Radiol. 2005; 15: 416-426.
- Farrell C, Chappell F, Armitage PA, Keston P, Maclullich A, Shenkin S, et al., Development and initial testing of normal reference MR images for the brain at ages 65-70 and 75-80 years. Eur Radiol. 2009; 19: 177-183.
- van Swieten JC, Hijdra A, Koudstaal PJ, van Gijn J. Grading white matter lesions on CT and MRI: a simple scale. J Neurol Neurosurg Psychiatry. 1990; 53: 1080-1083.
- Tatu L, Moulin T, Bogousslavsky J, Duvernoy H. Arterial territories of human brain: brainstem and cerebellum. Neurology. 1996; 47: 1125-1135.
- Tatu L, Moulin T, Bogousslavsky J, Duvernoy H. Arterial territories of the human brain: cerebral hemispheres. Neurology. 1998; 50: 1699-1708.
- Cloft HJ, Lynn MJ, Feldmann E, Chimowitz M, et al. Risk of cerebral angiography in patients with symptomatic intracranial atherosclerotic stenosis. Cerebrovascular Diseases. 2011; 31: 588-591.
- Chimowitz MI, Kokkinos J, Strong J, Brown MB, Levine SR, Silliman S, et al. The Warfarin-Aspirin Symptomatic Intracranial Disease Study. Neurology. 1995; 45: 1488-1493.
- Thomas GN, Lin JW, Lam WW, Tomlinson B, Yeung V, Chan JC, et al. Increasing severity of cardiovascular risk factors with increasing middle cerebral artery stenotic involvement in type 2 diabetic Chinese patients with asymptomatic cerebrovascular disease. Diabetes care. 2004; 27: 1121-1126.
- Uehara T, Tabuchi M, Mori E. Frequency and clinical correlates of occlusive lesions of cerebral arteries in Japanese patients without stroke. Cerebrovascular Diseases. 2000; 8: 267-272.
- Park KY, Chung CS, Lee KH, Kim GM, Kim YB, Oh K. Prevalence and risk factors of intracranial atherosclerosis in an asymptomatic korean population. J Clin Neurol. 2006; 2: 29-33.
- Khan M, Rasheed A, Hashmi S, Zaidi M, Murtaza M, Akhtar S, et al. Stroke radiology and distinguishing characteristics of intracranial atherosclerotic disease in native South Asian Pakistanis. International Journal of Stroke. 2012.
- Thomas GN, Lin JW, Lam WW, Tomlinson B, Yeung V, Chan JC, et al. Increasing severity of cardiovascular risk factors with increasing middle cerebral artery stenotic involvement in type 2 diabetic Chinese patients with asymptomatic cerebrovascular disease. Diabetes care. 2004; 27: 1121-1126.
- Uehara T, Tabuchi M, Mori E. Frequency and clinical correlates of occlusive lesions of cerebral arteries in Japanese patients without stroke. Cerebrovascular Diseases. 1998; 8: 267-272.
- Uehara T, Tabuchi M, Mori E. Risk factors for silent cerebral infarcts in subcortical white matter and basal ganglia. Stroke. 1999; 30: 378-382.
- Wong KS, Huang YN, Yang HB, Gao S, Li H, Liu JY, et al. A door-to-door survey of intracranial atherosclerosis in Liangbei County, China. Neurology. 2007; 68: 2031-2034.
- Elmore EM, Mosquera A, Weinberger J. The prevalence of asymptomatic intracranial large-vessel occlusive disease: the role of diabetes. J Neuroimaging. 2003; 13: 224-227.
- Huang HW, Guo MH, Lin RJ, Chen YL, Luo Q, Zhang Y, et al. Prevalence and risk factors of middle cerebral artery stenosis in asymptomatic residents in Rongqi County, Guangdong. Cerebrovascular Diseases. 2007; 24: 111-115.
- Uehara T, Tabuchi M, Kozawa S, Mori E. MR angiographic evaluation of carotid and intracranial arteries in Japanese patients scheduled for coronary artery bypass grafting. Cerebrovascular Diseases. 2000; 11: 341-345.
- Wong KS, Ng PW, Tang A, Liu R, Yeung V, Tomlinson B. Prevalence of asymptomatic intracranial atherosclerosis in high-risk patients. Neurology. 2007; 68: 2035-2038.
- Feldmann E, Daneault N, Kwan E, Ho KJ, Pessin MS, Langenberg P, et al. Chinese-white differences in the distribution of occlusive cerebrovascular disease. Neurology. 1990; 40: 1541-1545.
- Iqbal R, Anand S, Ounpuu S, Islam S, Zhang X, Rangarajan S, et al. Dietary patterns and the risk of acute myocardial infarction in 52 countries: results of the INTERHEART study. Circulation. 2008; 118: 1929-1937.
- Uehara T, Tabuchi M, Mori E. Risk factors for occlusive lesions of intracranial arteries in stroke-free Japanese. Eur J Neurol. 2005; 12: 218-222.