
Research Article
Austin J Clin Cardiolog. 2015; 2(2): 1038.
Clinical Implications of Recommendations in Current Guidelines on Anticoagulation in Patients with Atrial Fibrillation
Ozdemir E¹, Gursul E²*, Bayata S¹ and Safak O³
¹Katip Celebi University Ataturk Training and Research Hospital, Izmir, Turkey
²Biga State Hospital, Canakkale, Turkey
³Burdur State Hospital, Burdur, Turkey
*Corresponding author: Erdal Gursul, Biga State Hospital , Kibris Sehitleri Street, Canakkale, Turkey
Received: March 30, 2015; Accepted: September 13, 2015; Published: October 01, 2015
Abstract
Atrial Fibrillation (AF) is the most common arrhythmia in the clinics. We aimed to evaluate the clinical implications of anticoagulation in terms of warfarin that is recommended by current guidelines. Among patients having an indication for Oral Anti Coagulation (OAC), those under treatment with warfarin and those that are not taking were compared (n: 205). 117 of the 190 patients with an indication for OAC (57.0% of the patient population; 61.6% of those with an indication for OAC) were found to be taking OAC. 73 patients had an indication, but were not taking warfarin for a variety of reasons. 83 patients were detected, who had an indication for warfarin and did take warfarin, and found to have INR controls in the retrospective screening, 58 of which (69.9%) had an effective INR. No statistically significant differences were found between the groups who were taking and who were not taking warfarin, in terms of HAS-BLED and CHA2DS2-VASc scores (p = 0.656, p = 0.696, respectively). Treatment may not be initiated in patients with an indication for OAC treatment, due to patientrelated reasons, physician-related reasons, medication-related reasons, or therapeutic levels may not be achieved, or drug treatment is interrupted due to various reasons, as a result of patient non-compliance.
Keywords: Atrial fibrillation; Warfarin; INR
Abbreviations
OAC - Oral Anticoagulant Therapy; AF - Atrial Fibrillation; INR - International Normalized Ratio; CAD - Coronary Arterial Disease; DM - Diabetes Mellitus; ECHO – Echocardiography; CRF - Chronic Renal Failure; CHF - Chronic Heart Failure
Introduction
Atrial Fibrillation (AF) is a supraventricular tachyarrhythmia, which is the most common arrhythmia and its prevalence increases with ageing. Although AF is often associated with structural heart diseases, there is no structural heart disease in a considerable portion of patients with AF. Hemodynamic defects and thrombo-embolic events associated with AF cause significant morbidity and mortality [1]. Ischemic stroke is uppermost among thrombo-embolic events due to AF, and AF is a strong independent risk factor for ischemic stroke. Ischemic stroke risk in AF patients varies between 3% and 8% depending on other associated stroke risk factors [2]. Presence of associated structural heart diseases in AF further increases the stroke risk. Ischemic stroke which is a dramatic complication of AF is still an important issue because of its mortality, morbidity, adult disability and incurred costs as it was before.
Currently, in the light of previous studies the most effective treatment for preventing such an important and dramatic complication secondary to AF is Oral Anticoagulant Therapy (OAC) [3]. Randomized controlled studies have shown that OAC therapy achieving effective levels decreases ischemic stroke risk by 68% in unselected AF patients [4]. Also, even though new OAC drugs such as dabigatran, etexilate, rivaroxaban, apixaban are available, currently the most widespread treatment in our country and the world is still warfarin. In short, OAC therapy in AF is an accepted treatment method in preventing thrombo-embolic complications.
In this study, hospitalized patients having AF diagnosis according to criteria in European Society of Cardiology (ESC) 2010 AF treatment guideline and updated guideline published in 2012 were evaluated [5,6]. The patients’ use of warfarin and International Normalized Ratio (INR) effectiveness were evaluated and compared with demographic and clinical data. CHADS2 and CHA2DS2-VASc scores were simultaneously applied to patients and the patients with varying warfarin indication were determined [5,7]. The aim of our study is to evaluate clinical implications of guidelines on warfarin use in AF.
Material and Method
Patients
The medical records of patients hospitalized for any reason in our clinic which is a tertiary health institution between January 1, 2010 and March 31, 2012 were screened and 205 AF patients with adequate information were included into the study. Evaluated demographic and clinical data of the patients were as follows: age, sex, arterial hypertension, Diabetes Mellitus (DM), presence of vessel disease such as Coronary Arterial Disease (CAD) and peripheral arterial disease, smoking, thyrotoxicosis, presence of heart failure, diagnosis of rheumatic mitral valve, presence of cardiac valve prosthesis, previous ischemic stroke or transient ischemic attack or history of systemic embolism, presence of cardiomyopathy, hemogram, creatinine values, presence of chronic renal failure (CRF), dimension of left atrium, presence of spontaneous echo contrast or thrombus at left atrial appendix, number of hospitalizations, etiology of AF (valvular/ non-valvular AF). EF=40 was considered as Echocardiographically (ECHO) confirmed Cardiac Failure (CF). CHA2DS2-VASc and HASBLED scores were calculated in non-valvular AF [6,8].
AF classification
Valvular and non-valvular AF patients were determined. Patients with valve prosthesis, moderate-severe mitral stenosis or moderate-severe mitral insufficiency were considered as valvular AF patients. The patients without above mentioned valvular diseases were considered as non-valvular AF patients. The number of both groups of patients was determined and the groups were compared in terms of INR effectiveness. The patients were evaluated in 3 groups according to AF period. Paroxysmal AF episodes lasting less than 2 days with spontaneous resolution, persistant AF episodes lasting more than 7 days and requiring intervention with drugs or electrophysiological tools and permanent AF patients whose disease was accepted as being permanent [6]. The number of paroxysmal, persistent and permanent AF patients was determined and the groups were compared in terms of INR effectiveness.
Embolism and bleeding risk score systems in Nonvalvular AF
CHA2DS2-VASc, CHADS2 scores for anticoagulant indication and HAS-BLED to determine bleeding risk were calculated in non valvular AF. In 2001, CHADS2 scoring system was developed in order to determine embolism risk in non-valvular AF [7]. In calculating the score Chronic Heart Failure (CHF), age, Diabetes Mellitus (DM) are considered as 1 point and stroke as 2 points. The highest score is 6 and in patients with a score of =2 to start anticoagulant therapy is recommended. CHADS2 scores are calculated and mean of the score and number of patients with and without anticoagulant indication were determined. By CHADS2 scoring system low risk patients were thought to be overlooked; thus, in 2012 CHA2DS2- VASc score was developed [6]. In CHA2DS2-VASc scoring system CHF, hypertension, DM, vessel disease, age between 64-75 years and female sex are considered as 1 point and age over 75 years, ischemic cerebrovascular disease and systemic emboli as 2 points. The highest score is 9point and in patients with a score of 2 to start anticoagulant therapy is recommended. The CHA2DS2-VASc score of the patients was calculated and the number of patients with and without anticoagulant indication according to CHA2DS2-VASc scoring system was determined. The patients were separated into 3 groups according to CHA2DS2-VASc score: patients with a score of 0, 1 and 2. The number of the patients in each group was determined and INR effectiveness was compared between groups. The patients requiring different recommendations for anticoagulant therapy based on CHADS2 and CHA2DS2-VASc scores were determined and characteristics of the patients were reported. To determine bleeding risk in non valvular AF HAS-BLED scoring system was developed. [7] In HAS-BLED scoring system hypertension (systolic blood pressure over 160 mmHg), abnormal kidney (chronic dialysis or presence of renal transplant or serum creating in =200 mmol/L)/abnormal liver function (chronic liver disease or aspartat aminotransferase/ alanin aminotransferase/ alkalin phospatase >3x ULN together with bilirubin >2 x ULN), stroke, history of or tendency for bleeding, labile INR (time within therapeutic range is <60% or non-stable, high INR values, advanced age (>65 years), concomittant drug use (such as antiplatelet agents, nonsteroidal anti-inflammatory drugs)/alcohol intake are considered as 1 point. Patients with a score of = 3 were considered as having high risk for bleeding. HAS-BLED risk score of the patients was calculated and the number of patients in the low/ high risk groups was determined.
Anticoagulant therapy
Presence of valvular AF (valve prosthesis with AF and echocardiographically confirmed moderate-severe mitral stenosis or moderate-severe mitral insufficiency with AF) is considered as indication for warfarin use. In presence of non-valvular AF CHA2DS2- VASc score was evaluated. Presence of one of the other parameters along with CHA2DS2-VASc score = 2 and female sex is considered as indication for anticoagulant therapy in non-valvular AF. The indications for antiplatelet therapy (aspirin/aspirin+clopidogrel) and/or anticoagulant therapy were evaluated. Patients taking indicated anticoagulant therapy, patients taking anticoagulant therapy without indication and patients not taking anticoagulant therapy while there’s no indication for it were determined. The reason for not taking anticoagulant therapy in patients having an indication for this therapy was looked for. By screening medical records number of patients not taking anticoagulant therapy because of undetermined reason, patient’s rejection of the therapy, history of major bleeding and high HAS BLED score was determined as the reasons for not taking the drug. INR effectiveness was evaluated in control patients taking warfarin with indication for this therapy. The patients having INR measurement at least once a month were considered as patients checked for INR effectiveness and patients with no INR measurement after baseline and/or patients having INR measurement with an interval of more than a month were considered as patients not checked for INR effectiveness. If in more than 60% of the follow up period INR was 2.0 - 2.5 in non-valvular AF and 2.5-3.0 in valvular AF, then INR was considered as effective; otherwise ineffective. The number of patients not checked for INR effectiveness was determined.
Statistical Analysis
Quantitative data were shown as mean ± std. (Standart Deviation) in tables. Categorical data were shown as n (number) and percentage (%). In analysis of quantitative data conformity with normal distribution Kolmogorov-Smirnov test was used, and in variables with normal distribution parametric methods and in variables with abnormal distribution nonparametric methods were used. In comparisons between groups Pearson Chi-Square and Fisher’s exact test statistical analysis were used. p<0, 05 was considered as statistically significant and p=0, 05 as statistically insignificant. In assessing the findings of the study, statistical analysis of data was done by using SPSS (Statistical Package for Social Sciences) 15.0 for Windows software package by 95% confidence.
Results
109 of the 205 patients (53.2%) included into the study were female and mean age was 68, 57±13, 68 years. Distribution of 190 patients with anticoagulant indication according to CHA2DS2- VASc score was as follows: paroxysmal AF in 33 patients (17, 4%), persistent AF in 50 patients (26, 3%), permanent AF in 107 patients (56, 3%). 162 (79%) patients had non-valvular AF and 32 (15, 6%) of the valvular AF patients had mitral valve disease and 11 (5.4%) had valve prosthesis. In 7 of patients (4.4%) with non-valvular AF there was no risk factor for embolism (CHA2DS2-VASc=0). There was 119 patients (58.1%) taking warfarin and 86 patients (41.9%) not taking warfarin. HAS-BLED scores of non-valvular AF were as follows: 81 patients (50.0%) had a score of < 3 and 81 patients (50.0%) = 3 (Table 1).
Patients
(n:205)
Female n (%)
109 (53.2)
Age year± SD
68.57± 13.68
=65 n ( %)
76 (37.1)
66-74 n (%)
55 (26.8)
=75 n (%)
74 (36.1)
Diabetes Mellitus n (%)
37 (18)
Chronic Heart Failure n (%)
54 (26.3)
Chronic Renal Failure n (%)
30 (14.6)
Cerebrovascular Diseases n (%)
27 (13.2)
Hypertension n (%)
162 (79)
Vascular Disease* n (%)
86 (42)
Smoking n (%)
119 (58)
Ischemic Cardiomyopathy n (%)
47 (22.9)
Hypertrophic Cardiomyopathy n (%)
5 (2.4)
Dilated Cardiomyopathy n (%)
13 (6.3)
Hyperthyroidism n (%)
7 (3.4)
Echocardiographic Findings n (%)
Ejection Fraction % ± SD
% 51.41± 13.17
Left Atrial Size
46.09± 7.48
Left Atrial SEC or thrombus n (%)
6 (2,9)
Warfarin Situation
Taking Warfarin n (%)
119 (58,1)
Not Taking Warfarin n (%)
86 (41,9)
Type of AF
Paroxysmal AF n (%)
40 (19,5)
Persistant AF n (%)
58 (28,3)
Permanent AF n (%)
107 (52,2)
Etiology of AF
Valvular AF - mitral valve disease n (%)
32 (15,6)
Valvular AF- prosthetic valve n (%)
11 (5,4)
Non- valvular AF n (%)
162 (79)
CHA2DS2-VASc Score#
3,51±1,79 (0-8)
CHA2DS2-VASc=0 n (%)
7 (4,4)b
CHA2DS2-VASc=1 n (%)
16 (9,8)b
CHA2DS2-VASc=2 n (%)
139 (85,8)b
HAS-BLED Score#
2,54±1,21
HAS-BLED < 3 n (%)
81 (50,0)b
HAS-BLED = 3 n (%)
81 (50,0)b
SD: Standart Deviation; SEC: Spontan Echo Contrast; AF: Atrial Fibrillation
*Peripheral artery disease, cerebrovascular disease, Coronary Artery Disease
#Scores was calculated at non-valvular atrial fibrillation group (n: 162).
Table 1: Distribution of patients based on their demographic and clinical characteristics.
When anticoagulant/antiplatelet drug profile of the patients were evaluated, there was 73 patients with warfarin indication according to CHA2DS2-VASc score but not taking warfarin; 12.3% of patients were taking clopidogrel + acetylsalicylic acid and 23.1% only acetylsalicylic acid. The distribution of subgroup of patients with warfarin indication according to CHA2DS2-VASc score and using the drug was as follows: 58 patients with warfarin indication who were taking the drug were checked for INR effectiveness and INR value was found to be effective; 25 patients with warfarin indication who were taking the drug were checked for INR effectiveness and INR value was found to be ineffective; 34 patients with warfarin indication who were taking the drug weren’t checked for INR effectiveness; 2 patients without warfarin indication but taking warfarin with unknown reason (without indication). This is a total of 119 patients taking warfarin. Warfarin indication of patients according to CHA2DS2-VASc score, status of drug use and INR effectiveness were presented in (Table 2 and Figure 1).
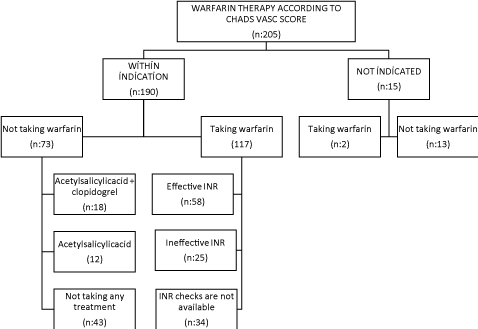
Figure 1: Distribution of patients using and patients not using warfarin in
terms of CHA2DS2-VASc.
Patients
(n:205 )
Within indication but do not receive warfarin
The reason of not taking warfarin
Unknown n (%)
53 (25.8)
The patient did not want the drug n (%)
14 ( 6.9)
Major bleeding history n (%)
4 (1.9)
High HAS-BLED score n (%)
2 (0.9)
Agents that used instead of warfarin
Aspirin+ clopidogrel n (%)
12 (5.8)
Aspirin n (%)
18 (8.7)
Within indications, taking warfarin and INR checks available
Effective INR n (%)
58 (28.6)
Ineffective INR n (%)
25 (12,3)
Within indications, taking warfarin but INR checks are not available n (%)
34 (16.3)
Not indicated but takig warfarin n (%)
2 (0.9)
Not indicated and do not receive warfarin n (%)
13 (6,4)
INR: International Normalized Ratio
Table 2: Distribution of patients’ warfarin use status based on the reasons.
Non valvular patients were assessed in terms of CHADS score; in case CHADS score is 0 CHA2DS2-VASc score was calculated. In 8 patients with a CHADS score of 0 CHA2DS2-VASc score was 1 and in 7 patients with a CHADS score of 0 CHA2DS2-VASc score was 2 or more. So to say, in 7 patients without OAC indication according to 2006 recommendations new recommendation was absolute indication for OAC use and also in 8 patients without OAC indication new recommendation was indication for OAC use. When the patients were assessed, the risk factor causing the difference in recommendations was mostly found as addition of a vascular cause.
There was no difference in terms of sex and age of the patient groups who have indication for warfarin according to CHA2DS2- VASc score and using and not using the drug (p=0.190, p=0.231; respectively). Between patients with non-valvular AF etiology and AF patients with mitral valve disease and AF patients with prosthesis valve replacement there was statistically significant differences and all of the patients with a prosthetic valve were using warfarin (p=0.004). Comparison of patients according to warfarin use is presented in table 3. There was no statistically significant difference between patients using warfarin and not using warfarin in terms of HAS-BLED and CHA2DS2-VASc scores (p=0.656, p=0.696; respectively). 77 patients with CHA2DS2-VASc =2 were using warfarin and 58 patients with CHA2DS2-VASc =2 weren’t using warfarin. 44 patients with HASBLED = 3 were using warfarin and 36 patients with HAS-BLED = 3 weren’t using it (Table 3).
Taking Warfarin
n (%)
Not Taking Warfarin
n (%)
p
Gender
Male
60 (51,3)
30 (41,1)
Female
57 (48,7)
43 (58,9)
0,190
Age
=65
45 (38,5)
19 (26)
66-74
31 (26,5)
22 (30,1)
0,231
=75
41 (35,0)
32 (43,8)
Type of AF
Paroxysmal AF
18 (15,4)
15 (20,6)
Persistant AF
35 (29,9)
15 (20,6)
0,321
Permanent AF
64 (54,7)
43 (58,8)
Etiology of AF
Valvular AF - mitral valve disease
23 (19,6)
9 (12,3)
Valvular AF- prosthetic valve
11 (9,4)
0 (0)
0,004
Non- valvular AF
83 (71,0)
64 (87,7)
CHA2DS2 –VASc Score*
CHA2DS2-VASc=0
0 (0)
0 (0)
CHA2DS2-VASc=1
6 (7,2)
6 (9,4)
0,656
CHA2DS2-VASc=2
77 (92,8)
58 (90,6)
HAS-BLED Score*
HAS-BLED < 3
39 (46,9)
28 (43,7)
HAS-BLED = 3
44 (53,1)
36 (56,3)
0,696
AF: Atrial Fibrillation
*Scores was calculated at non-valvular atrial fibrillation group (n: 162).
Table 3: Comparison of demographic and clinical characteristics of patients with warfarin indication based on their warfarin use status.
When the patient groups who achieved and who hasn’t achieved effective INR value were compared there was no statistically significant difference between groups regarding sex, age, clinical risk factors, AF type, AF etiology, echocardiographical data, HAS-BLED and CHA2DS2-VASc scores. In 33 patients with CHA2DS2-VASc =2 INR was effective and in 17 patients with CHA2DS2-VASc =2 INR was ineffective. In 2 of the whole patient group with prosthetic valve who were using warfarin INR was found to be ineffective (Table 4).
Effective
Ineffective
p
n (%)
n (%)
Gender
Male
29 (50)
12 (48)
0.867
Female
29 (50)
13 (52)
Age
=65
23 (39.7)
8 (32)
66-74
18 (31)
8 (32)
0.768
=75
17 (29.3)
9 (36)
Type of AF
Paroxysmal AF
8 (13.8)
4 (16)
Persistant AF
16 (27.6)
6 (24)
0.928
Permanent AF
34 (58.6)
15 (60)
Etiology of AF
Valvular AF - mitral valve disease
13 (22.4)
5 (20)
Valvular AF- prosthetic valve
9 (15.5)
2 (8)
0.645
Non- valvular AF
36 (62.1)
18 (72)
CHA2DS2-VASc Score*
CHADS-VASc=1
3 (8.3)
1 (5.6)
CHADS-VASc=2
33 (91.7)
17 (94.4)
0.784
HAS-BLED Score*
HAS-BLED < 3
20 (55.6)
13 (77.2)
0.375
HAS-BLED = 3
16 (44.4)
5 (27.8)
Table 4: Comparison of demographic and clinical characteristics of patients with warfarin indication and using warfarin based on their INR status.
Analysis of the reasons not using oral anticoagulant therapy have revealed non-prescription of the drug because it was rejected by the patient as number one among the known reasons (6.9%). Non-prescription because of bleeding history of the patient (2%) and non-prescription because of high HAS-BLED score (1%) followed this, respectively. Thus, non-prescription by the clinician as a result of benefit-risk ratio assessment was 11.4%. In the retrospective evaluation of patients comprising 17.1% of the total population in whom warfarin was indicated but no warfarin use was observed, no reason could be detected for not using the drug. Thus, the largest group of patients comprised from patients not using warfarin for an unknown reason. When this group is evaluated it was observed that 43% of them were = 75 years old, 83% had hypertension, 15% CVO and 11% CRF (Table 5).
Table 5: Distribution of reasons for not using warfarin in patients with warfarin indication but not using warfarin.
Discussion
Atrial Fibrillation (AF) is the most common arrhythmia in general population. Its prevalence increases markedly by ageing and reaches to 8%-10% at the age of >80 years [6]. Currently, several risk calculation methods are used to determine stroke risk in AF patients. After initiation of OAC therapy in patients with high risk for stroke, risk of stroke decreases markedly [9]. When transient ischemic attacks and clinically silent ischemia that can be detected by cerebral imaging methods are also taken into account, cerebral ischemia associated with non-valvular AF is over 7% annually [10].
In the first large study presenting the national data regarding OAC therapy in AF patients, the rate of OAC use in AF patients was 7% in 1980-1981 but increased to 32% in 1992-1993. The rate of never treated patients was reported as down to 48% from 90% [10]. In other OAC studies, OAC use was found as between 32-57% and rate of never treated patients was reported as between 22-59% [11,12]. AFFIRM trial was conducted in 4.060 AF patients with a mean age >70 years and in 70.8% of the patients’ hypertension, 38.2% CAD, 13% stroke, 32.1% CF was reported. In the end of the trial, in terms of stroke rate no difference was found between patients with sustained AF and patients returning to normal sinusal rhythm. Trial has revealed that most of the patients who have experienced stroke were either not using warfarin treatment or their INR values were below therapeutic levels [13]. In our study presence of CVD (n=27, 13, 2%), CF (n=54, 26, 3%), hypertension (n=162, 79%) is similar to AFFIRM trial.
In our study, retrospective evaluation of patients with OAC indication who were using warfarin has revealed that number of patients with INR control was 83 and in 58 of these patients (69.9%) INR was effective. These figures that are obtained from patients followed up in a tertiary center are consistent with the INR effectiveness rate target outlined in the guidelines. Conduction of this study in a large tertiary center of our country may have contributed to the fact that the findings are within the range of worldwide standards. In our study, it was observed that 12.3% of patients with an indication for warfarin use but haven’t used the drug (n=73, 35, 4%) have used clopidogrel + acetyl salicylic acid and 23.1% have used only acetyl salicylic acid. The fact that the study was conducted in a tertiary center which is serving to a very large geographic area and a heterogeneous patient population makes the findings more significant. 69.9% of the patients with warfarin indication who have showed up in follow up have achieved effective INR values and this rate is within the targeted range; however, the fact that 35.4% (n=73) of patients with warfarin indication haven’t used warfarin for various reasons is an indicator for us that we’re still in 1990’s in terms of indicated warfarin use [12].
The results of warfarin use were analyzed along with analysis of various trials studying a very large number of stroke incidents. Prognosis of stroke patients with AF were found to be worse than stroke patients with sinusal rhythms and mortality rate was 2 times more [14,15]. At the follow up after 6 months and 12 months recurrent stroke was found to be 2 times higher than patients without AF [16-18]. The fact that 5-year mortality rate is higher in patients with AF (52% vs 78%) have shown us that we’re far from the desired values [19].
In our study, when non-valvular AF patients were evaluated by CHA2DS2-VASc score the number of patients with their respective scores were as follows: 0=7 patients (4.4%); 1=16 patients (9.8%); = 2=139 (85, 8%). Distribution of patients with indication for warfarin according to CHA2DS2-VASc score and have used the drug was as follows: 0=0 patient (0%), 1=6 patients (7.2%), = 2=77 (92, 8%); distribution of patients with indication for warfarin according to CHA2DS2-VASc score but haven’t used the drug was as follows: 0=0 patient (0%), 1=6 patients (9, 4%), = 2=58 patients (90, 6%). Analysis of the findings have revealed that warfarin use increases as the risk score increases; but in higher scores the number of patients with indication for warfarin but haven’t used the drug has also increased. The notion that adverse event risk such as risk of embolism and risk of bleeding increases in these patients may have led to non-prescription of warfarin even by clinicians in tertiary health institutions in indicated cases.
In daily practice, it’s known that OAC is not prescribed to AF patients with high risk of stroke and in most of the patients using warfarin INR control is ineffective and a portion of patients stop taking warfarin after starting therapy. There are various factors effecting patients’ compliance. These are mainly patient-related, clinician-related, drug-related and environmental factors and interaction between them. OAC treatment is not prescribed to patients in daily practice because of following reasons: the patients can’t properly conduct INR control, don’t want to use the drug, there is uncertainty in risk-benefit status of patients with poor condition and clinicians beware of prescribing the drug since they are wary of the major bleeding complications. In a trial 313 AF patients were followed up for 6 months. In that study, it was reported that 75 (50%) of 168 patients with OAC indication have used OAC therapy, 54 (30%) have used antiplatelet therapy and 39 (20%) haven’t used any prophylactic treatment. 80% of patients included into study were over 70 years old and/or have high risk for stroke [20]. In our patient population, the patients who have indication for warfarin but haven’t used the drug because of unknown reasons were the largest group by 17.1%. These were followed by 17 patients (8.4%) in whom reason of the non-prescription of the drug is not known, 4 patients with history of major bleeding (2%), 2 patients with high HAS-BLED score (1%). The number of patients rejecting warfarin prescription was 14 (6.9%) and regarding warfarin use this leads to the notion that since clinicians and patients are wary of the adverse effects, the treatment of the patients is often interrupted.
In SPORTIVE II study a total of 254 AF patients were distributed into two treatment arms: “ximelagatran” and “warfarin”, and dose safety and tolerability of ximelagatran were researched. This study has showed that 12 months after the start of the therapy, rate of patients with INR values of 2-3 was 57% and 43% in warfarin treatment arm could not reach targeted INR values [21]. In our study, the number of patients using warfarin during the follow-up with an indication for it, and having INR control with effective INR value was 58; constituting 28.6% of all patients and % 69.9 of followed-up patients with warfarin indication have used warfarin.
At the same time, in our study anticoagulant therapy wasn’t started in 73 (35, 4%) patients with anticoagulant indication. When these 73 (35, 4%) patients were evaluated, it was observed that 12, 3% used clopidogrel + acetylsalicylic acid, and 23, 1% used only acetyl salicylic acid. In our study it was found out that the rate of patients having oral anticoagulant therapy indication, however using antiplatelet therapy (n=73, 35, 4%) was similar to literature data [22].
A study comparing 2004 guidelines with anticoagulation guidelines of 2000 has showed that indications for starting the therapy is slightly expanded and became clearer. During the transition from 2000 to 2004 guidelines, oral anticoagulant therapy rate has increased, and has approximately been doubled. Increase was observed in patients with high and very high risk (17%). In the study by Simona Bo et al. a total of 313 AF patients were included, and 106 patients with oral anticoagulant therapy indication were followed-up between April 2000 and April 2004. Since the therapy was highly recommended and the necessary explanations were made clearly, rate of oral anticoagulant therapy use have increased to 81, 9% (n=87) from 56, 6% (n=60) (23-199) [21]. In our study, due to being inadequately informed of oral anticoagulant therapy, 19.2% (n=14) of 73 patients not using warfarin themselves have rejected the therapy, and therefore their therapies could not be started. It is obvious that oral anticoagulant therapy use will increase if the importance of oral anticoagulant therapy in AF patients is clearly communicated to the patient. In a study by Mc Alister FA et al., out of 307 AF patients, 185 patients having indication for oral anticoagulant therapy were followed-up for 6 months. As a result of an increase in patients’ training program, the number of patients using oral anticoagulant therapy increased to 135 (73%) from 89 (48%) at the end of 6 months. This increase in the number has reached to a statistically significant level (p< 0.0001) [23].
In the cohort study of 601 patients with AF using warfarin, records of approximately 6-year were screened. During 5-year follow up, 263 patients (44%) used oral anticoagulant, 309 (51%) patients used oral anticoagulant therapy in a certain interval during the study, INR was between 2-3 at 68% of the time during the study, and annual bleeding risk was found to be higher in patients using warfarin (9%) relative to the patients using aspirin (4, 7%) and patients not having any treatment (4, 6%). Bleeding was the most common complication of the therapy. While bleeding risk increases along with INR increase, 50% of the bleeding episodes occurred while INR was below 4. Bleeding risk was highest within 3 months after the start of the therapy. In earlier months of the therapy, bleeding is usually gastrointestinal, and originates from urinary system, and underlying lesion usually needs to be investigated [24]. In our study, reason for non-prescription of warfarin in terms of bleeding was history of major bleeding by 5.4% (n=4) and the most common major bleeding was upper gastrointestinal system bleeding (2.3%). As it can be concluded from the above mentioned study; even though oral anticoagulant therapy markedly decreases mortality, morbidity and stroke risk in AF patients, use of anticoagulant therapy is still inadequate due to certain reasons. The therapeutic level can’t be achieved in most of the patients in whom oral anticoagulant therapy was started or most of the patients can’t take the drugs regularly once the therapy is started.
None of the studies about the oral anticoagulant therapy use predictors of (until the study by Albert et al.) hasn’t looked for the possibility that AF classification could be a predictor for anticoagulant therapy use. For the first time, Albert et al. suggested that persistent/ permanent AF was an independent predictor for anticoagulant therapy use [25]. In our research, when classified as paroxysmalpersistent- permanent, AF classification/typology, with p=0.32, did not reach a statistically significant level. However, when AF ethiology was classified as valvular-mitral disease/valvular-prostethic valve/ non-valvular, it was determined that warfarin use, with p=0.004, was significantly higher at valvular AF with prosthetic valve.
A study conducted by McCormick et al. on long-term care patients indicated that as the number of risk factors for stroke increased, so did the use of anticoagulant therapy [26]. However, these values could not reach statistical significance. Similarly, on the basis of the idea that having high risk score for stroke could be an independent predictor for indicated oral anticoagulant therapy, a tendency for increase was observed in our study but it wasn’t statistically significant, either. These findings suggest that what constitutes a high stroke risk is not clear on clinicians’ minds.
Atrial Fibrillation (AF) is the most common arrhythmia in the clinics. The prevalence has been gradually increasing in last several decades due to the aging population and prolongation of survival. Stroke and systemic embolism risk are significantly higher for AF patients compared to patients without AF. Oral Anticoagulant Therapy (OAC) therapy is recommended for patients with high stroke risk. OAC therapy significantly decreases the risk of mortality, morbidity and stroke, and that is why this therapy is especially important for OAC patients. However, OAC therapy of patients with OAC indication is usually not initiated, initiated warfarin therapy does not reach at the targeted INR level, or drug cannot be used regularly and is stopped for various reasons. Consequently, inadequate and incomplete use of anticoagulation therapy significantly increases the stroke, stroke-based mortality, hospitalization rate and the economic costs. Recent studies and recently available agents, as well as up to date guidelines encourage clinicians for the initiation of OAC therapy.
References
- Kannel WB, Abbott RD, Savage DD, Mc Namara PM. Epidemiological features of chronic atrial fibrillation: The Framingham Study. N Eng J Med. 1982; 306: 1018-1022.
- Albers GW, Dalen JE, Laupacis A, et al. Antithrombotic therapy in atrial fibrillation. Chest. 2001; 119: 194- 206.
- Warfarin versus aspirin for prevention of thromboembolism in atrial fibrillation Stroke Prevention in Atrial Fibrillation II study. Lancet. 1994; 343: 687-691.
- Rockson SG and Albers GW. Comparing the guidelines: anticoagulation therapy to optimize stroke prevention in patients with atrial fibrillation. Arch Intern Med. 2004; 43: 929-935.
- Camm AJ, Kirchhof P, Lip GY, et al. Guidelines for the management of atrial fibrillation The Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC). Eur Heart J. 2010; 31: 2369- 2429.
- Camm AJ, Lip GY, De Caterina R, et al. 2012 focused update of the ESC Guidelines for the management of atrial fibrillation an update of the 2010 ESC Guidelines for the management of atrial fibrillation Developed with the special contribution of the European Heart Rhythm Association. Eur Heart J. 2012; 33: 2719-2747.
- Gage BF, Waterman AD, Shannon W, et al. Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA. 2001; 285: 2864-2870.
- Pisters R, Lane DA, Nieuwlaat R, et al. A Novel User-Friendly Score (HAS-BLED) To Assess 1-Year Risk of Major Bleeding in Patients with Atrial Fibrillation the Euro Heart Survey. CHEST Journal. 2010; 138: 1093-1100.
- Wolf PA, Abbott RD and Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke. 1991; 22: 983-988.
- Hart RG and Halperin JL. Atrial fibrillation and thromboembolic: a decade of progress in Stroke prevention. Ann Intern Med. 1999; 131: 688-695.
- Stafford RS and Singer DE. National patterns of warfarin use in atrial fibrillation Arch Intern Med. 1996; 156: 2537-2541
- McCormick D, Gurwitz JH, Goldberg RJ, et al. Prevalence and quality of warfarin use for patients with atrial fibrillation in the long-term care setting. Arch Intern Med. 2001; 161: 2458-2463.
- Sherman DG, Kim SG, Boop BS, et al. Occurrence and Characteristics of Stroke Events in the Atrial Fibrillation Follow-up Investigation of Sinus Rhythm Management (AFFIRM) Study. Arch Intern Med. 2005; 65: 1185- 1191.
- Lamassa M, Di Carlo A, Pracucci G, et al. Characteristics, outcome, and care of stroke associated with atrial fibrillation in Europe: data from a multicenter multinational hospital-based registry (The European Community Stroke Project). Stroke. 2001; 32: 392-398.
- Dulli DA, Stanko H and Levine RL. Atrial fibrillation is associated with severe acute ischemic stroke. Neuroepidemiology. 2003; 22: 118-123.
- Wolf PA, Kannel WB, McGee DL, Meeks SL, Bharucha NE, McNamara PM. Duration of atrial fibrillation and imminence of stroke: the Framingham study. Stroke. 1983; 14: 664-667.
- Lin HJ, Wolf PA, Kelly-Hayes M, et al. Stroke severity in atrial fibrillation. The Framingham Study. Stroke. 1996; 27: 1760-1764.
- Appelros P, Nydevik I and Viitanen M. Poor outcome after first-ever stroke. Predictors for death, dependency, and recurrent stroke within the first year. Stroke. 2003; 34: 122-126.
- Gustafsson C and Britton M. Pathogenetic mechanism of stroke in non-valvularatrial fibrillation: follow-up of stroke patients with and without atrial fibrillation. J lntern Med. 1991; 230: 11-16.
- Ciccone G, Bo S, Scaglione L, et al. Warfarin for non-valvar atrial fibrillation: still underused in the 21st century? Heart. 2003; 89: 553-554.
- Petersen P, Grind M, Adler J, et al. Ximelagatran versus warfarin for stroke prevention in patients with nonvalvular atrial fibriliation. SPORTIF II: a dose-guiding, tolerability, and safety study. J Am Cardiology. 2003; 41: 1445-1451.
- Bo S, Valpreda S, Scaglione L, et al. Implementing hospital guidelines improves warfarin use in non-valvular atrial fibrillation: a before-after study. BMC Public Health. 2007; 7: 203.
- McAlister FA, Man-Son-Hing M, Straus SE, et al. Impact of a patient decision aid oncare among patients with nonvalvular atrial fibrillation: a cluster randomised trial. CMAJ 2005; 173: 496- 501.
- Burton C, Isles C, Norrie J, et al. Thesafety and adequacy of antithrombotic therapy for atrial fibrillation: a regionalcohort study. British Journal of General Practice 2006; 56: 697-702.
- Waldo AL, Becker RC, Tapson VF, Colgan KJ. Hospitalized patients with atrial fibrillation and a high risk of stroke. J Am Coll. Cardiol. 2005; 46: 1729-1736.
- McCormick O, Gurwitz JH, Goldberg RJ, et al. Prevalence and quality of warfarin use for patients with atrial fibrillation in the longterm care setting. Arch Intern Med. 2001; 161: 2458-2463.