
Case Report
Austin J Clin Cardiolog. 2015; 2(2): 1039.
Brugada Type I ECG Pattern after Flecainide Intoxication
Schultinge L1,2*, Kuijper AFM1, Voogel AJ¹ and Oosterwerff E1,3
¹Department of Cardiology, Spaarne Hospital Hoofddorp, Netherland
²Department of Internal Medicine, Maastricht University, Netherland
³Department of Cardiology, Onze Lieve Vrouwe Gasthuis, Netherland
*Corresponding author: Schultinge L, Department of Internal Medicine, Maastricht University, Prof. Oudlaan 13, 5707 KW Helmond
Received: May 14, 2015; Accepted: September 14, 2015; Published: October 01, 2015
Abstract
Flecainide (a class 1c antiarrhythmic) is known for different electrocardiographic effects like prolongation of PR and QT intervals and the QRS complex duration. We report a case of Brugada syndrome, after flecainide intoxication in an elderly female who presented with a non-fatal suicide.
Methods: On admission the serum concentration of flecainide was tested. Several Electrocardiograms (ECG) were made. Six weeks after discharge and Ajmaline provocation test was performed.
Results: The serum concentration of flecainide measured was 2.90 mg/l (therapeutic range 0.45 – 0.90 mg/L, toxic effects are observed from 1 mg/L [1]. On the ECG, Brugada pattern type I was observed. In-hospital monitoring showed no abnormalities. Ajmaline provocation test was negative for Brugada.
Conclusion: We present a case of Brugada pattern, with the suggestion of a congenital Brugada syndrome, after flecainide overdose in a patient, with false-negative Ajmaline provocation test.
Keywords: Flecainide; Brugada; Intoxication
Abbreviations
ECG: Electro Cardio Gram
Introduction
Flecainide is a commonly used class IC antiarrhythmic agent that blocks sodium channels. It is mostly used for the treatment of supraventricular arrhythmias. Flecainide produces a dose-dependent decrease in intracardiac conduction [2]. It is known from several case reports that an overdose of flecainide causes changes in the ECG [3- 8]. we present a case with a Brugada type I pattern following flecainide overdose.
Case Report
A previously healthy 64-year old woman was presented in our hospital with a non-fatal suicide. After ingestion of 4000 mg of her husbands’ flecainide (slow release) she presented at the emergency department. The patient took four doses of 1000 mg slow release flecainide; the first dose 26 hours before admission and the last dose 12 hours before admission. She complained about dizziness, muscle weakness and nausea. She had vomited at home; no signs of the ingested medication were present in the vomit. Family history for sudden cardiac death was negative. Physical examination revealed no abnormalities with normal oxygen saturation and an arterial blood pressure of 130/80 mmHg. The ECG showed a Brugada type I pattern in V2. (Figure 1) The patient was admitted to the coronary care unit. Blood analysis revealed a mild kidney dysfunction (creatinine 116 umol/l; ref range 50 - 100 umol/l) with normal potassium concentration (4, 6 mmol/l; ref range 3.5 - 5.0 mmol/l) and normal calcium concentrations (2.42 mmol/l; ref range 2.10 - 2.60 mmol/l). Results of serum flecainide level were 2.90 ml/l (therapeutic range 0.45 – 0.90 mg/L) on admission. No further flecainide levels were measured. Because the patient was dehydrated due to vomiting, she was treated with intravenous sodium chloride 0.9%. No other medication was given. Subsequent ECGs (Figure 2) during admission showed a complete resolution in a couple of days. In-hospital monitoring showed no rhythm disturbances. After psychiatric assessment the patient was discharged from the hospital on the fourth day.
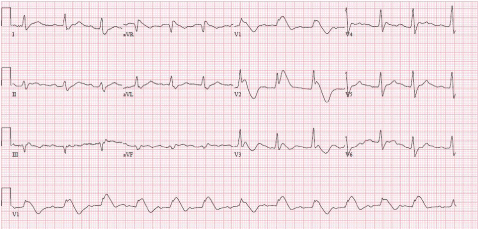
Figure 1: ECG on admission.
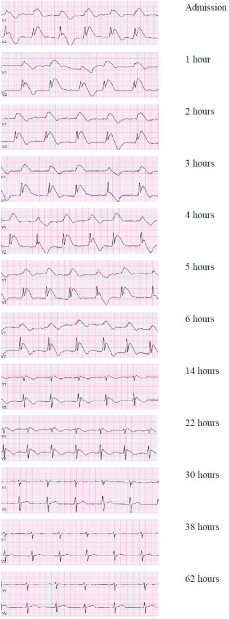
Figure 2: Subsequent ECG’s after flecainide overdose.
Methods
On admission the serum concentration flecainide was measured. During the first six hours after admission, an ECG was performed hourly. After six hours an ECG was performed every eight hours until discharge. The patient was discharged after 70 hours of observation. Seven weeks later an Ajmaline provocation test was performed. This test was performed with the electrodes placed in the third inter costal space.
Results
ECG’s showed complete resolution after 30 hours of observation (Figure 2). No rhythm disturbances were observed. The flecainide concentration was 2.90 mg/l, which is extremely high (therapeutic range 0.45-0.90 mg/l, toxic effects are observed from 1 mg/L [1]. To examine the possibility of an underlying congenital form of Brugada an Ajmaline provocation test was performed. The Ajmaline provocation test was negative (Figure 3).
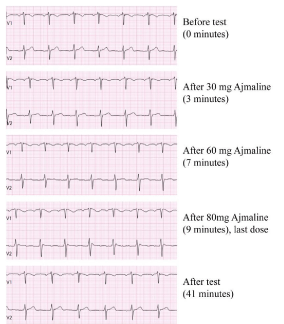
Figure 3: Ajmaline test.
Discussion
Brugada syndrome was first described in 1992 and is characterized by episodes of syncope or unexpected sudden death in patients with structurally normal hearts. In the classic Brugada type 1 ECG shows elevated ST segment (=2 mm) descends with an upward convexity to an inverted T wave. This is referred to as the “coved type” Brugada pattern. In the type 2 pattern (combined from the original designation of types 2 and 3 patterns), the ST segment has a “saddle back” ST-T wave configuration, in which the elevated ST segment descends toward the baseline, then rises again to an upright or biphasic T wave. The syndrome is associated with a high risk of sudden cardiac death [9]. Brugada-type ST-segment elevation is the result of a loss of action potential dome in the right ventricular epicardium but not endocardium, associated with a defect in a cardiac sodium channel [10]. Previous studies have suggested that flecainide can induce a new Brugada ECG pattern or can unmask a Brugada syndrome by inducing a type 1 Brugada pattern in patients with pre-existing type 2 or type 3 Brugada patterns [11]. Drug induced Brugada pattern can be generally seen at standard therapeutic dose of flecainide and such patients may have a possible underlying genetic predisposition (like SCN5A mutations) causing abnormality of native sodium channel activity.
Flecainide causes a rate dependent slowing of a rapid sodium channels slowing phase of depolarisation. Few articles report Brugada type I pattern following flecainide overdose [3-8]. all of these reports state that the Brugada type I pattern is only due to the flecainide overdose, but none of them performed further diagnostic tests to assure this conclusion. To our knowledge none of these case reports performed a diagnostic Ajmaline provocation test to assure that the Brugada type I pattern found in this patient is not related to the congenital form of the Brugada syndrome.
In our case the Ajmaline provocation test was negative. It is known from previous publication that an Ajmaline provocation test has a sensitivity of only 80% [13]. Therefore it is plausible that this test was false-negative. Family history in this patient is negative for sudden cardiac death or known Brugada. However, the ECG on admission in this case report is very suspicious for an underlying Brugada, therefore we are unable to rule out an underlying congenital Brugada syndrome. We recommended the patient to perform genetic testing on her and her first degree relatives. Unfortunately the patient refused further testing.
Conclusion
We report a Brugada type I pattern after a severe flecainide overdose, with a possible false negative Ajmaline provocation test. We believe that even after a severe flecainide overdose a Brugada type I pattern on the ECG is very suspicious for the congenital form of the Brugada syndrome.
References
- Ellenhorn M, Schonwald S, Ordog G, Wasserberger J. Medical Toxicology. Diagnosis and Treatment of Human Poisoning. 2nd edition ed. Baltimore, Md., USA: Williams & Wilkins; 1997.
- Aliot E, Capucci A, Crijns HJ, Goette A, Tamargo J. Twenty-five years in the making: flecainide is safe and effective for the management of atrial fibrillation. Europace. 2011; 13: 161-173.
- Chhabra L and Spodick DH. Brugada pattern masquerading as ST-segment elevation myocardial infarction in flecainide toxicity. Indian Heart J. 2012; 64: 404-407.
- Rognoni A, Bertolazzi M, Peron M, Maccio S, Cameroni GT, Gratarola A, et al. Electrocardiographic changes in a rare case of flecainide poisoning: a case report. Cases J. 2009; 1626-2-9137.
- Chubb H, Cooklin M and Rosenthal E. Brugada phenocopy with a flecainide overdose: a pharmacological dose effect? J Cardiovasc Electrophysiol. 2014; 25: 547-548.
- Soni S and Gandhi S. Flecainide overdose causing a Brugada-type pattern on electrocardiogram in a previously well patient. Am J Emerg Med. 2009; 27: 375.e1-375.e3.
- Hudson CJ, Whitner TE, Rinaldi MJ, Littmann L. Brugada electrocardiographic pattern elicited by inadvertent flecainide overdose. Pacing Clin Electrophysiol. 2004; 27: 1311-1313.
- Reiffel JA. Does a Brugada pattern ECG precipitated by excessive-dose flecainide provide a diagnosis of a Brugada syndrome patient and/or contraindicate its use? A case study. Circ Arrhythm Electrophysiol. 2011; 4: e47-51.
- Brugada P and Brugada J. Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome. A multicenter report. J Am Coll Cardiol. 1992; 20: 1391-1396.
- Antzelevitch C. The Brugada syndrome: ionic basis and arrhythmia mechanisms. J Cardiovasc Electrophysiol. 2001; 12: 268-272.
- Brugada R, Brugada J, Antzelevitch C, Kirsch GE, Potenza D, Towbin JA, et al. Sodium channel blockers identify risk for sudden death in patients with ST-segment elevation and right bundle branch block but structurally normal hearts. Circulation. 2000; 101: 510-515.
- Wang Z, Fermini B and Nattel S. Mechanism of flecainide's rate-dependent actions on action potential duration in canine atrial tissue. J Pharmacol Exp Ther. 1993; 267: 575-581.
- Hong K, Brugada J, Oliva A, Berruezo-Sanchez A, Potenza D, Pollevick GD, et al. Value of electrocardiographic parameters and ajmaline test in the diagnosis of Brugada syndrome caused by SCN5A mutations. Circulation. 2004; 110: 3023-3027.