
Research Article
Austin J Clin Cardiolog. 2015; 2(2): 1040.
Non Invasive Mechanical Ventilation in Elders with Acute Heart Failure
Calvo SG1* and Padilla LD2
¹Respiratory Unit, Hospital King Juan Carlos, Mostoles, Spain
²Respiratory Unit, Hospital Universitario 12 de Octubre, Madrid, Spain
*Corresponding author: Gonzalo Segrelles Calvo, c/Gladiolo s/n; Hospital King Juan Carlos, Mostoles, Madrid, Spain
Received: November 18, 2014; Accepted: September 13, 2015; Published: October 08, 2015
Abstract
The aim of the study was to confirm the usefulness of Non-Invasive Ventilation (NIV) in elders with multiple comorbidities,admittedfor Respiratory Acidosis (RA) due to Heart Failure (HF), and to determine their survival one year after discharge.
Design: Observational prospective trial made at the Hospital Universitario La Princesa (Madrid) between October of 2009 and December of 2012. We included 42 elderly patients with HF and AR treated with NIV.
Results: 62% were females, with a mean age of 78.2 years. Charlson Index was 3.41 and the mean of prescriptions per day was 5.8. The main complication during admission was cardiovascular disease, and 25% of patients passed away during admission. The most frequentre-admissiondiagnosiswas HF. Global survival was 60%.
Discussion: NIV is a useful treatment for elderly patients with HF and nonintubation orders. The principal factors associated to mortality were: low pH and high PaCO2 at ER, high respiratory rate and previous comorbidities.
Keywords: Heart failure; Noninvasive ventilation; Respiratory acidosis; Elderly; Non-intubation orders
Introduction
Heart Failure (HF) has an incidence of 10% in patients older than 65 years, reaching a 40% in those older than 80 [1], which translates to be the cause of 75% of hospitalizations in this group [2,3]. HF is more frequent in women, producing a 50-60% of total, according to previous studies [2]. The physiopathology of HF in elders is complex and various factors are involved, related not only to age but also to associated comorbidities [4].
Non-Invasive Ventilation (NIV) is advised in acute HF secondary to Acute Pulmonary Edema (APE), reducing the risk of intubation, as well as improving symptoms and gas exchange parameters [5,6]. NIV is more efficient than oxygen therapy [7] and similar to Continuous Positive Air way Pressure (CPAP) regarding clinical outcomes [8,9]. Further more, latest guidelines recommend the use of either NIV or CPAP for acute HF [10,11].
Now a days, there is not sufficient data concerning the indication of NIV in elderly patients admitted for Acute HF (AHF), considering their multiple comorbidities and performance status limitations. The hypothesis of our study was that NIV is useful in this clinical scenario. The main objective was to determine the benefit (efficiency, utility, suitability) of NIV in elder patients admitted for acute HF causing respiratory acidosis, defined as time to gas exchange normalization, days of hospitalization, complications during treatment, mortality rate, and evolution 1 year after hospital discharge.
Methods
Study design
Prospective observational study carried out in the Respiratory Care Unit (RCU) of Hospital UniversitarioLa Princesa (HULP), from October of 2009 to December of 2012. The HULP is a tertiary hospital located in Madrid, Spain, which provides health care to an estimated population of 350.000 habitants. Our RCU has 4 beds integrated to the Respiratory Ward, allowing non-invasive monitoring of hemodynamic parameters (blood pressure, heart rate, Respiratory Rate (RR), peripheral pulseoximetry (SpO2) and continuous electrocardiography) and respiratory support by NIV along with mechanical invasive ventilation in selected patients on which a tracheostomy was performed. Specialized nursing care providers and a Respiratory Care physician are in charge of the RCU during morning shifts, whereas a physician assumes its supervision during night shifts and weekends. The entire population of this study were treated with Bi-Level Positive Airway Pressure (BiPAP) in Pressure Support (PS) mode.
Study population
Patients admitted to our RCU for HF and respiratory acidosis (pH < 7.35 and PaCO2 >45mmHg), treated with NIV and at least 70 years old were included. HF diagnosis was based on the European Society of Cardiology recommendations [10], while the Chronic Respiratory Obstructive Disease (COPD) diagnosis followed the Spanish Guideline of COPD (GesEPOC) [12]. A “do-not-intubate” indication was considered in the entire population since the following criteria: 1.The patient decided not to be treated by invasive respiratory support through an orotracheal intubation, or had previously stated this wish signing a legal document regarding this matter. 2. The corresponding physician who treated the patient during an acute scenario (Emergency Room (ER), Intensive Care Unit (ICU), Respiratory or Internal Medicine Ward) had not considered the patient as an optimal candidate for invasive respiratory support since a poor prognosis or lacking life performance status were concluded. 3. A legal representative orcare giver manifested their wish to avoid any intensive care measure. The following patients were excluded: 1. Patients admitted to the RCU, however without NIV required. 2. Patients where NIV was initiated in the other units other than the RCU, and after wards were not admitted to the latter. 3. Patients who rejected NIV. The ethics committee of the HULP approved the study, and informed consent was given by all the participants. All data was retrieved from the HULP databases, allowing access to clinical variables in order to complete the 1-year follow up.
Variables And Statistical Analysis
The SPSS 15.0 package for Windows (SPSS Inc., Chicago IL) was used for the statistical analysis. Table 1 shows the variables included in the study. Descriptive analysis is presented using parameters such as means, range and Standard Deviation (SD), and qualitative data is shown as absolute numbers and percentages. Normality in the distribution was assessed by the Kolmogorov-Smirnov test. The difference between quantitative variables was analyzed by the t-student test, and qualitative data by the chi-square and Fisher exact. A p-value < 0.05 was considered statistically significant.
Baseline
Emergency Room (ER)
Admission
Demographic
Age, sex, LADL*, PC^, smoking habit.
Clinical
COPD features: LTOT/NIV♩, BODE/BODExref, GesEPOC8 phenotype, PFTγ, thoracic CTθ and treatment.
Referred symptoms by patients.
Complications.
Charlson Indexref, previous HF episodes.
Vasoactive drugs instauration.
Length of stay.
ICU evaluation.
ICU evaluation and admission (invasive mechanical support treatment)
Physical examination features.
Deceases (during admission and 90 days after)
Complementary tests
ECG♮, X-Ray characteristics
Blood tests: complete blood count, biochemical analysis (kidney function and solutes), NT-proBNP y C-reactive protein, and arterial blood gases.
LADL*: Limited Activities Of Daily Living. PC^: Primary Caretaker, LTOT/VMD♩: Long-Term Oxygen Therapy/Non Invasive Ventilation, PFTγ: Pulmonary Function Tests, Thorax TCθ: Thorax Computerized Tomography, ECG♮: Electrocardiogram.
Table 1: Recorded data: Baseline characteristics, ER features, and during admission to the RCU.
N (%)
Mean (SD)
Sex (females)
26 (62%)
Age (years)
78.2 (8.3)
Charlson Index
3.41 (1.75)
Respiratory comorbidities:
30 (71.5%)
� COPD
16 (38.1%)
� OSA
11 (26.2%)
� TB
3 (7.2%)
Prescriptions per day
5.8 (2.1)
Functional status:
� Independent
20 (47.6%)
� Partially dependent
14 (33.3%)
� Dependent
8 (19%)
Mobility:
� Walks around
12 (54.5%)
� Bed-chair
6 (27.2%)
� Immobilized
4 (18.1%)
Institutionalized
3 (7,1%)
Caretaker
12 (28.5%)
Dyspnea (MRC):
� Grade III
18 (42.8%)
� Grade IV
5 (12%)
Home respiratory therapies:
� LTOT
16 (38%)
� NIV
2 (5%)
Table 2: Baseline characteristics.
Results
During the inclusion period, a total of 320 patients were admitted to the RCU and 42 patients were included for analysis (Figure 1). Out of these 42, 26 were females (62%), with a mean age of 78.2 ± 8.2 years and a Charlson index of 3.4 ± 1.75. The mean of prescriptions per day was 5.8. (Table 2) shows baseline variables. Previous HF was documented in 34 patients (81.5%), all of them being followed on an outpatient clinic (51% in Cardiology ambulatory care clinic). Thirty patients (72%) had been admitted for AHF in the previous year, and 10 of these patients presented RA. Supplementary oxygen therapy was prescribed in 38% of population. NIV was initiated in the ER in 75% of cases (gasometrical evolution is presented in Table 3).
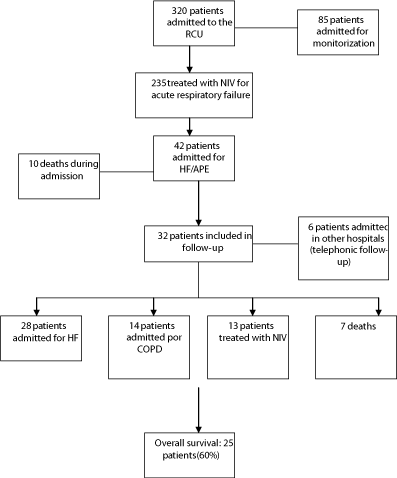
Figure 1: Flowchart of patients included in the study.
ER
1 hour after NIV
24 hours after NIV
At discharge
pH
7.24 ± 0.08
7.29 ± 0.09
7.35 ± 0.08
7.41 ± 0.034
PaCO2 (mmHg)
83.1 ± 19.1
76.7 ± 17.4
66 ± 14.2
55.2 ± 11.5
PaO2 (mmHg)
59 ± 21.3
78.7 ± 18.4
69.20 ± 20
63.5 ± 10.8
Bicarbonate (mEq/L)
34.8 ± 5.3
36.7 ± 5.4
38.2 ± 5.7
34.3 ± 5.8
Data is presented as mean ± SD unless otherwise specified SD: Standard Deviation.
Table 3: Arterial Blood Gases (ABG) evolution.
The most frequent complication during admission was acute renal failure (18%), followed after cardiovascular disease: atrial fibrillation (14.8%) and acute myocardial infarction (3.6%). The mortality was of 25% (10 patients). Main differences between deceased patients and those who survived after admissionare summarized in (Table 4). After a 1-year follow-up, main re-admittance diagnosis was AHF (28 patients), followed after COPD exacerbation (12 patients). The 66% of these re-admitted patients presented AR before 3 months after discharge (Table 5). The entire population survival after 1 year was of 60%.
Deaths
Survivors
p-value
n = 10
n = 32
Age
82.1
79.7
0.123
Sex (female)
6
20
0.382
Charlson Index
3.8 (1.92)
3.9 (1.84)
0.971
COPD
5
11
0.239
FEV1
24.80%
37.30%
0.024
% LVEF
64.1
50.3
0.691
LTOT
1 patient (14.3%)
6 patients (28.6%)
0.721
Previous NIV
0
1
0.627
RA previous admissions
7
3
0.003
Limitations:
-Independent
2 (20%)
18 (90%)
0.007
-Partially dependent
5 (50%)
9 (64.28%)
0.255
-Dependent
3 (30%)
5 (62.5%)
0.031
Dyspnea III-IV (MRC)
15
8
0.004
Initial pH
7.19
7.25
0.004
Initial PaCO2
88.7
69.1
0.007
Creatinine (mg/dl)
1.05
1.29
0.527
Leucocytes (/mm3)
8,975
9,675
0.288
%Neutrophils
70
79
0.05
C-reactive Protein
1.58
6.03
0.005
MBP*(mmHg)
75.2
76
0.327
RR** (bpm)
32
27
0.071
Temperature (�C)
36.2
36.4
0.875
COPD: Chronic Obstructive Respiratory Disease; FEV1: Forced Expiratory Volume in 1 second; LVEF: Left Ventricular Ejection Fraction; LTOT: Long-term oxygen therapy; RA: Respiratory Acidosis; MRC: Medical Research Council; MBP*: mean blood pressure; RR**: respiratory rate.
Table 4: Differences between survivors and deceased patients during admission.
LTOT at discharge
ER
NIV
ICU
Deaths
HF admissions
22
15
8
0
5
28
COPD admissions
10
12
4
0
2
12
Other causes admissions
4
0
1
0
0
4
36
27
13
0
7
Table 5: 1 year follow-up after discharge.
Discussion
According to our data, NIV is a useful therapy in elderly patients with multiple comorbidities and limited performance status (52.3% were considered at least partially dependent), admitted for AHF and AR. The main factors associated to mortality were lower pH at admission (7.19 vs 7.25, p = 0,004), higher levels of PaCO2 (88.7 vs 69.1 mmHg, p=0.007), previos admission due to AR (p = 0.003), and higher grades of dyspnoea according to the Medical Research Council (MRC) scale (p = 0.004), and among COPD patients lower Forced Expiratory Volumes in 1 second (FEV1) (24.8% vs 37.3%, p=0.024). Ruiz-Laiglesia et al. determined a COPD prevalence of 27.4% in patients with HF, which was also an independent factor associated to mortality and earlier read mission [13].
The rest of parameters did not show significant differences between deceased patients and survivors. However, deceased patients were older (82.1 vs 79.7 years of age), presented a higher respiratory rate at admission (32 vs 37 bpm, p = 0.071), and decline in functional status. Where as some groups have previously identified age as an independent factor associated to poor prognosis concerning NIV (ref), other studies have confirmed that NIV is effective regardless of age [14,15] in ARF. Not with standing, a higher mortality was observed in patients with poor functional status (p = 0.031) and survival in those with greater status (p = 0.007). Thus, in our opinion, the main factor associated to NIV effectiveness in elders is their basal situation; hence, comorbidities and decline in functional status. As previous data reported, early readmission for AHF was higher in older patients, especially in those with more comorbidities [16] and decline of their functional status [17]. In accordance to this, other studies have stated that earlier admissions in elder patients diagnosed of HF were related to a greater number of comorbidities, incrementing their risk of mortality after 1 year [18]. Additionally, Sacanella et al. presented a lower 1-year cumulative survival in patients with diminished activities of daily living (Barthel index) and lower quality of life at discharge when compared to their previous situation [19].
The main limitations of our study were basically two: 1) We have carried out an observational study without a group control, thus, we can only hypothesize about the utility of NIV in elders, and 2) A reduced sample size. The latter is probably a consequence of not considering this sort of patients optimal for NIV in an ER environment; hence, a Respiratory Care physician is not aware of the admission, at least in our hospital daily basis scenario.
The results obtained in our study suggest that elder patients with HF and RA treated with NIV, have a fair survival during admission and 1 year after discharge. Basal functional status seems to be a paramount feature concerning admission out comes.
References
- Lloyd-Jones D, Adams R, Carnethon M, De Simone G, Fergu- son TB, Flegal K, et al. Heart disease and stroke statistics-2009 update: a report from the American Heart Association Statis- tics Committee and Stroke Statistics Subcommittee. American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2009; 119: 480-486.
- San Román Terán CM, Guijarro Merino R, Guil García M, Villar Jiménez J, Martín Pérez M, Gómez Huelgas R. Analysis of 27,248 hospital discharges for heart failure: a study of an administra- tive database 1998-2002. RevClinEsp. 2008; 208: 281-287.
- Nieminen MS, Brutsaert D, Dickstein K, Drexler H, Follath F, Harjola VP, et al., EuroHeart Survey Investigators; Heart Fai- lure Association, European Society of Cardiology. EuroHeart Failure Survey II (EHFS II): a survey on hospitalized acute heart failure patients: description of population. Eur Heart J. 2006; 27: 2725-2736.
- Chivite D, Formiga F and Pujol R. La insuficiencia cardíaca en el paciente anciano. RevClinEsp. 2011; 211: 26-35.
- Metha S and Hill NS. Non invasive ventilation. Am J Respir Crit Care Med. 2001; 163: 540-577.
- Azonlay E, Demonle A, Jabe S, Konatchet A, Meert AP, Papazian L, et al. Palliative noninvasive ventilation in patients with acute respiratory failure. Intensive Care Med. 2011; 37: 1250-1257.
- Masip J, Betbesé AJ, Páez J, Vecilla F, Ca&nTilde;izares R, Padró J, Paz MA et al. Non-invasive pressure support ventilation versus convetional oxygen therapy in acute cardiogenic pulmonary oedema: a randomised trial. Lancet. 2000; 356: 2126-2132.
- Gray AJ, Goodacre S, Newby DE, Masson MA, Sampson F, Dixon S et al. A multicentre randomised controlled trial of the use of continuous positive airway pressure and non-invasive positive pressure ventilation in the early treatment of patients presenting to the emergency department with severe acute cardiogenic pulmonary oedema: the 3CPO trial. Health Technol Assess. 2009; 13: 1-106.
- Vital FM, Saconato H, Ladeira MT, Sen A, Hawkes CA, Soares B et al. Non-invasive pressure ventilation (CPAP or bilevel NPPV) for cardiogenic pulmonary edema. Cochrane Database Syst Rev. 2008 jul 16; (3): CD005351.
- ESC guidelines for the diagnosis and treatment of acute and chronic heart failure 2008. European Heart Journal 2008, 29: 2388-2442.
- Valipour A, Cozzarini W and Burghuber OC. Non-invasive pressure support ventilation in patients with respiratory failure due to severe acute cardiogenic pulmonary edema. Respiration. 2004; 71: 144-151.
- Coordinador: Miratvilles M. Guia espa&nTilde;ola de la EPOC (GesEPOC).Tratamiento farmacológico de la EPOC estable. Arch Bronconeumol. 2012; 48: 247-257.
- Ruiz-Laiglesia FJ, Sánchez-Marteles M, Pérez-Calvo JI, Formiga F, Bartolomé-Satué JA, Armengou-Arxé A et al. Comorbidity in heart failure. Results of the Spanish RICA Registry. QJM. 2014 (en prensa).
- Segrelles G, Zamora E, Girón R, Vázquez E, Gómez-Punter RM, Fernandes G et al. Ventilación mecánica no invasora (VMNI) en una población anciana que ingresa en una Unidad de Monitorización Respiratoria: causas, complicaciones y evolución al a&nTilde;o de seguimiento. Arch Bronconeumol. 2012; 48: 349-354.
- Kida Y, Minakata Y, Yamada Y, Ichinose M. Efficacy of noninvasive positive pressure ventilation in elderly patients with acute hypercapnic respiratory failure. Respiration. 2012; 83: 377-382.
- Forminga F, Chivite D, Conde A, Ruiz-Laiglesia F, Franco AG, Bocanegra CP. Basal functional status predicts three-month mortality after a heart failure hospitalization in elderly patients-the prospective RICA study. Int J Cardiol. 2014; 172: 127-131.
- Eastwood CA, Howlett JG, King-Shier KM, McAlister FA, Ezekowitz JA, Quan H. Determinants of early readmissions after hospitalization for heart failure. Can J Cardiol. 2014; 30: 612-618.
- Roig T, Márquez MA, Hernández E, Pineda I, Sabartés O, Miralles R et al. Geriatric assessment and factors associated with mortality in elderly patients with heart failure admitted to an acute geriatric unit. Rev EspGeriatrGerontol. 2013; 48: 254-258.
- Sarcanella E, Pérez-Castejón JM, Nicolás JM, Masanés F, Navarro M, Castro P et al. Functional status and quality of life 12 months after discharge from a medical ICU in healthy elderly patients: a prospective observational study. Crit Care. 2011; 15: R105.