Case Report
Austin J Dermatolog. 2014;1(2): 1007.
Spontaneous Regression of Atypical Primary Cutaneous Diffuse Large B-Cell Lymphoma on Cheek upon Methotrexate Withdrawal
Seow Hoong Foo*, Evmorfia Ladoyanni and Indre Verpetinske
Department of Dermatology, Corbett Hospital, Dudley Group Hospitals NHS Foundation Trust, UK
*Corresponding author: Seow Hoong Foo, Dermatology Department, Corbett Hospital, Dudley Group Hospitals NHS Foundation Trust, Vicarage Road, Stourbridge, West Midlands, DY8 4JB, United Kingdom
Received: March 22, 2014; Accepted: May 05, 2014; Published: May 07, 2014
Abstract
Primary cutaneous diffuse large B–cell lymphoma (PCDLBCL) accounts for approximately 6% of all cutaneous lymphomas. PCDLBCL are usually seen in leg, however they can be seen in other location in 15% of cases.It usually affects elderly women and is associated with poor prognosis.Solitary lesions are relatively rare. The recommended treatment is as for systemic diffuse large B–cell lymphoma (DLBCL). We present an atypical case of PCDLBCL occurring on the cheek of an elderly woman and its spontaneous resolution upon withdrawal of methotrexate therapy for rheumatoid arthritis. It is paramount to recognise these cases and correlation being undertaken in order to avoid inappropriate chemotherapy.
Keywords: Primary cutaneous diffuse large B–cell lymphoma; Cheek; Methotrexate; Spontaneous resolution
Abbreviations
PCDLBCL: Primary Cutaneous Diffuse Large B–cell Lymphoma; PCBCL: Primary Cutaneous B– Cell Lymphoma
Background
Primary cutaneous diffuse large B–cell lymphoma (PCDLBCL) accounts for approximately 6% of all cutaneous lymphomas. PCDLBCL is usually seen in leg, however it can be seen in other location in 15% of cases [1]. It usually affects elderly women and its presentation is more commonly with multiple red or bluish–red nodules rather than solitary lesions.
When compared with other types of primary cutaneous B– Cell lymphoma (PCBCL), the prognosis of PCDLBCL is less favourable with a 5–year survival rate of approximately 20–50% [1]. Diagnosis is made by clinicopathological correlation, immunohistochemical findings, and molecular pathology.
When compared to the general population there is an excess risk of lymphoma in patients with chronic inflammatory polyarthritis on DMARDSs (disease modifying anti–rheumatic drugs) such as methotrexate [2]. We present the case of PCDLBCL occurring on the cheek of an elderly woman and its spontaneous resolution upon withdrawal of methotrexate therapy for rheumatoid arthritis. It is important that correlation is being undertaken in any case of atypical presentation of PCDLBCL in order to avoid inappropriate chemotherapy.
Case Presentation
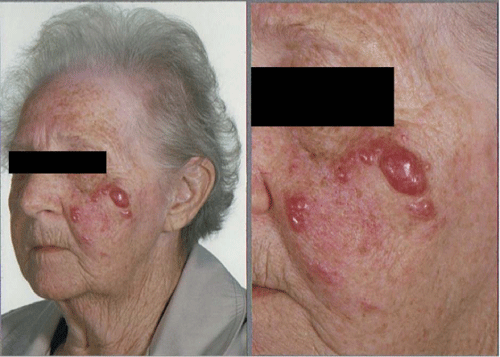
A 78–year old woman presented to the dermatology department with a 5–week history of multiple erythematous nodules on left cheek (Figure 1). These nodules did not bleed and only caused mild itching occasionally. She was otherwise well in herself. She had suffered from moderate to severe rheumatoid arthritis for 25 years, which was controlled on combination therapy of methotrexate and sulfasalazine for the last 8 years. Clinical examination revealed multiple firm painless smooth erythematous nodules on left cheek, with the largest nodule being 1.5cm in diameter (Figure 1). There was no palpable lymphadenopathy or hepatosplenomegaly. An urgent skin biopsy was performed.
Figure 1: Multiple firm painless smooth erythematous nodules on left cheek.
Histological examination revealed at low power a diffuse infiltrate involving the entire dermis with sparing of a thin subepidermal grenz zone. At higher power, there was a dense atypical lymphocytic proliferation with destruction of adnexal structures and extension into the subcutaneous tissue. Immunohistochemical testing showed a CD20 positive B cell population with diffuse BCL staining. CD10 was negative. These findings were suggestive of diffuse large B–cell lymphoma (DLBCL).
Further computer tomography (CT) staging scans revealed no internal involvement. The haematology team worked her up to commence R–CHOP (Rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisolone) chemotherapy for DLBCL. Due to the potential interaction of methotrexate with her chemotherapy regime, she was advised to stop it. She continued on sulfasalazine for the management of her rheumatoid arthritis.
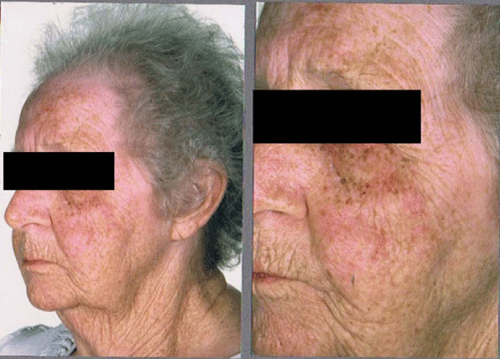
Within 6 weeks of stopping methotrexate the lesions had resolved spontaneously leaving only mild macular erythema (Figure 2). The scheduled chemotherapy was subsequently cancelled. However, her rheumatoid arthritis became poorly controlled causing significant disability. Following further multi–disciplinary team discussions, she was started on Rituximab with the two–pronged aim to control her active rheumatoid arthritis and also prevent further recurrence of DLBCL.
Figure 2: Regression of the lesions on left cheek 6 weeks following withdrawal of methotrexate.
Conclusion
The World Health Organisation (WHO) and the European Organization for Research and Treatment of Cancer (EORTC) classification have divided PCDLBCL into leg type and other [3]. Both subtypes are associated with poor prognosis as they tend to spread to lymph nodes and extracutaneous sites [1].
Clinically PCDLBCL usually affect elderly women and can manifest as a solitary nodule or as multiple tumours restricted to one anatomic site, most commonly the lower leg.On histology a diffuse dermal infiltrate composed of sheets of centroblasts and immunoblasts that effaces adnexal structures can be seen. Grenz zone preservation is usually present. The centroblasts have little cytoplasm and round to oval vesicular nuclei while the immunoblasts have more abundant basophilic cytoplasm and a nucleus containing a single large eosinophilic nucleolus [4]. Immunostaining of the neoplastic cells reveal positive results for CD19, CD20, CD22, CD79a, Mum1, bcl–2 and bcl–6 while staining for CD5, CD10, CD138 and cyclin D1 are usually negative [5]. Molecular analysis can show clonalrearrangement of immunoglobulin genes.
There is evidence in the literature suggesting that patients with chronic inflammatory polyarthritis on DMARDSs such as methotrexate have higher risk of developing lymphoma when compared with the general population [6]. In a prospective cohort study J Franklin et al confirmed the apparent predominance of DLBCL in this patient population [2]. There are also some case reports of PCBCL occurring in patients during methotrexate therapy for rheumatoid arthritis andthe regression of skin lesions after discontinuation of the drug [7,8].
The underlying pathomechanism is not clear and more research is needed [2]. Therefore increased clinical awareness, discontinuation of methotrexate therapy and close observation, together with early involvement of relevant specialities are important in the initial management of this rare cutaneous lympho–proliferative disorder. To the best of our knowledge, we present the first atypical presentation PCDLBCL occurring on the face which regressed spontaneously following withdrawal of methotrexate.
Learning Points
- PCBCL although are usually seen in leg, however they can be seen in other location such as the face.
- PCBCL can be associated with long term methotrexate use which will resolve once methotrexate is withdrawn
- Increased clinical awareness, discontinuation of methotrexate therapy and close observation, together with early involvement of relevant specialities are paramount
- Rituximab can be considered as an effective alternative for these patients
- Paulli M, Lucioni M, Maffi A, Croci GA, Nicola M, Berti E. Primary cutaneous diffuse large B-cell lymphoma (PCDLBCL), leg-type and other: an update on morphology and treatment. G Ital Dermatol Venereol. 2012; 147: 589-602.
- Franklin J, Lunt M, Bunn D, Symmons D, Silman A. Incidence of lymphoma in a large primary care derived cohort of cases of inflammatory polyarthritis. Ann Rheum Dis. 2006; 65: 617-622.
- Burg G, Kempf W, Cozzio A, Feit J, Willemze R, S Jaffe E, et al. WHO/EORTC classification of cutaneous lymphomas 2005: histological and molecular aspects. J Cutan Pathol. 2005; 32: 647-674.
- Kodama K, Massone C, Chott A, Metze D, Kerl H, Cerroni L. Primary cutaneous large B-cell lymphomas: clinicopathologic features, classification, and prognostic factors in a large series of patients. Blood. 2005; 106: 2491-2497.
- Paulli M, Viglio A, Vivenza D, Capello D, Rossi D, Riboni R, et al. Primary cutaneous large B-cell lymphoma of the leg: histogenetic analysis of a controversial clinicopathologic entity. Hum Pathol. 2002; 33: 937-943.
- Wolfe F, Michaud K. Lymphoma in rheumatoid arthritis: the effect of methotrexate and anti-tumor necrosis factor therapy in 18,572 patients. Arthritis Rheum. 2004; 50: 1740-1751.
- Fam AG, Perez-Ordonez B, Imrie K. Primary cutaneous B cell lymphoma during methotrexate therapy for rheumatoid arthritis. J Rheumatol. 2000; 27: 1546-1549.
- Bachman TR, Sawitzke AD, Perkins SL, Ward JH, Cannon GW. Methotrexate-associated lymphoma in patients with rheumatoid arthritis: report of two cases. Arthritis Rheum. 1996; 39: 325-329.
References