Case Report
Austin J Dermatolog. 2014;1(3): 1012
Mast cell Infiltration in a Patient with Cutaneous Plasmacytosis
Wei Jin and Zhang Jianzhong*
Department of Dermatology, Peking University People's Hospital, China
*Corresponding author: Zhang Jianzhong, Department of Dermatology, Peking University People's Hospital, Beijing, China
Received: June 09, 2014; Accepted: July 02, 2014; Published: July 07, 2014
Keywords
Plasmacytosis; Mast cell infiltration; Cutaneous
Mast cells are important effector cells of the immune system and are found in all vascularized tissue, especially in the skin and mucosa of the respiratory and gastrointestinal tracts. Mast cells release a variety of inflammatory mediators that may induce heterogeneous symptoms [1-3]. Here we report a case of cutaneous plasmacytosis with mast cell infiltration and discuss the clinicopathological features and differential diagnostic considerations.
A 41-year-old Chinese female presented with reddish brown macules and plaques on the trunk over 9 years. The lesions were slightly itchy. The patient had been diagnosed as dermatitis and urticaria pigmentosa in local hospitals. She failed to respond to antihistamines and topical corticosteroids. The patient had a 3-year history of chronic non-atrophic gastritis. She had no other remarkable past medical history.
On physical examination, multiple oval brownish macules, papules, and plaques about 1.0~2.0mm in diameter were found on the waist and other parts of the trunk. Friction on the lesion could induce wheal and flush response (positive Darier sign, figure 1A).
The complete blood count, urine analysis, total serum IgE level, serum biochemical analysis were all normal. Rheumatoid factor and antinuclear antibody were negative. Abdominal ultrasound and chest X-ray examination were normal. Immunoglobulin G (IgG) was 35.2g/L (reference: 6.94-16.68g/L), IgA 6.75g/L (0.68-3.78g/ L), β2-microglobulin (-), KAPPA light chain 3160mg/dL (629- 1350mg/dL), LAMBDA light chain 1260mg/dL (313-723mg/ dL), C-reactive protein (CRP) 43.8mg/L(<7.9mg/L), erythrocyte sedimentation rate (ESR) 93mm, Bence Jones protein (-), peripheral blood IgH gene rearrangement (-), chromosome check: 46XX [20]. Bone marrow puncture and biopsy findings revealed inactive bone marrow hyperplasia, higher ratio of plasma cells.
The histopathology of the skin biopsy showed many plasmocytes and a few mastocytes infiltrated in the superficial and middle dermis. Immunohistochemical staining showed that the infiltrates were positive for CD117, CD38, CD138, KAPPA, and LAMBDA partially(+), Ki67 (5% +), PAS staining, acid-fast staining (-). Toluidine blue staining showed small purple heterophilic granules in the cytoplasm of a few cells in the dermis (figure 1B-F). Giemsa staining of gastric biopsy (-).
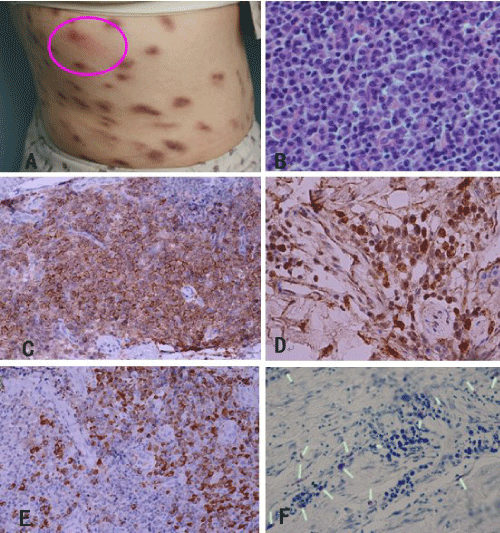
Figure 1: Clinical and histopathological findings. A. Skin lesions with positive Darier sign; B. Dense infiltration of plasma in middle and deep dermis. HE, �400; C. Positive stain for CD138; D. focal positive stain for CD117; E. Partial positive stain for KAPPA; F. Toluidine blue staining showed small purple heterophilic granules in the cytoplasm of a few infiltrates of the dermis.
Based on these clinical and laboratory findings, the patients was diagnosed as cutaneous plasmacytosis associated with mast cell infiltration. She was given thalidomide 150mg/day, for six months with minimal effects. Antihistamines were given to control her itching. She was followed-up for 12 months and the lesions remained stable.
Discussion
In 1869, Nettleship described urticaria pigmentosa (UP) [4] and in 1887 Unna documented an increase in mast cells in UP [5]. Systemic disease associated with mast cell hyperplasia was reported by Ellis in 1949 [6]. The presence of typical skin lesions of urticaria pigmentosa is the most common clinical sign of mastocytosis (both cutaneous and systemic disease), which appear as fixed, dark red-brown pruritus macules or papules. The affected areas include the trunk and extremities, while the face, scalp, palms, and soles tend to be free of lesions. The lesions had Darier's sign from mild trauma, such as rubbing or scratching, that is considered pathognomonic of mastocytosis and it reflects mast-cell degranulation and release of inflammatory mediators [7-9].
In this patient, the slightly itchy reddish-brown papules and plaques with positive Darier's sign were observed, suggestive of UP. As signs and symptoms of mastocytosis are unspecific and often overlap with some other diseases, the diagnosis may be overlooked and there might be an unusually long latency period between the first symptoms and the final diagnosis. To confirm the diagnosis, the histopathological and histochemical examinations as well as special staining are required.
Cutaneous plasmacytosis is defined as an accumulation of mature plasma cells limited to the skin. Cutaneous plasmacytosis usually has no or only a small number of mast cells within the lesion. Therefore, albeit extremely rare, mast cell infiltration should be included in the differential diagnostic consideration of cutaneous plasmacytosis due to their pathological similarity, and special staining such as Giemsa or Toluidine blue staining is useful for differentiating mast cells from plasma cells.
Gastrointestinal symptoms including abdominal pain, diarrhoea, vomiting, gastritis, and peptic ulcers could be prominent or common in patients with mastocytosis and are thought to be caused by mast cell proinflammatory mediators and/or mast cell organ infiltration [10]. Because this patient has a 3-year history of chronic non-atrophic gastritis, we performed gastric biopsy, abdominal ultrasound and chest X-ray examinations to rule out possible systemic involvements.
Abundant mast cell infiltration in the dermis is observed in a variety of cutaneous conditions, such as mastocytosis, allergic reaction, arthropod reaction, and friction (eg. scratching). The coexistence of plasmacytosis with mast cell infiltration is rare, and such coexistence hasn't been documented in the English published literature. The clear mechanism of which is unknown. The clinical picture, to some extent, may be generated by the acute or chronic release of mast cell-derived mediators, such as histamine, heparin, tryptase, leukotrienes and cytokines [10]. These clinical signs and symptoms are highly variable inter- and intra-individually. The clinical manifestations are often non-specific and can be found in both mastocytosis and cutaneous plasmacytosis. The disease can be stable for quite a long time and long-term follow-up is necessary.
References
- Escribano L, Akin C, Castells M, Orfao A, Metcalfe DD. Mastocytosis: current concepts in diagnosis and treatment. Ann Hematol. 2002; 81: 677-690.
- Valent P, Akin C, Escribano L, Födinger M, Hartmann K, Brockow K, et al. Standards and standardization in mastocytosis: consensus statements on diagnostics, treatment recommendations and response criteria. Eur J Clin Invest. 2007; 37: 435-453.
- Amon U, Hartmann K, Horny HP, Nowak A. Mastocytosis - an update. J Dtsch Dermatol Ges. 2010; 8: 695-711.
- Nettleship E. Rare forms of urticaria. Br Med J. 1869; 18: 323.
- Unna PG. Beitrage zur anatomie und pathogeneses der urticaria simplex und pigmentosa. Mschr Prakt Dermat Studien. 1887, 3H: 1.
- ELLIS JM. Urticaria pigmentosa; a report of a case with autopsy. Arch Pathol (Chic). 1949; 48: 426-435.
- Akoglu G, Erkin G, Cakir B, Boztepe G, Sahin S, Karaduman A, et al. Cutaneous mastocytosis: demographic aspects and clinical features of 55 patients. J Eur Acad Dermatol Venereol. 2006; 20: 969-973.
- Hartmann K, Henz BM. Mastocytosis: recent advances in defining the disease. Br J Dermatol. 2001; 144: 682-695.
- Ishida M, Iwai M, Kagotani A, Iwamoto N, Okabe H. Cutaneous mastocytosis with abundant eosinophilic infiltration: a case report with review of the literature. Int J Clin Exp Pathol. 2014; 7: 2695-2697.
- Magliacane D, Parente R, Triggiani M. Current concepts on diagnosis and treatment of mastocytosis. Transl Med UniSa. 2014; 8: 65-74.