
Case Series
Austin J Dermatolog. 2015;2(1): 1032.
An Experience of Photodynamic Therapy with ALA in Moderate to Severe Acne Vulgaris
Resende C1*, Marques H2, Pereira T1, Pardal F3, Torres F4 and Paiva A5
1Consultant Dermatologist, CMH Rawalpindi, Pakistan
2Consultant Dermatologist, CMH Rawalpindi, Pakistan
3Consultant Dermatologist, United Nations Hospital, Darfur, Sudan
4Consultant Dermatolo gist, CMH Gujranwala, Pakistan
5Consultant Dermatologist, CMH Lahore, Pakistan
*Corresponding author: Muhammad Irfan Anwar, Consultant Dermatologist, United Nations Hospital, Nyala, Sudan
Received: January 27, 2015; Accepted: February 16, 2015; Published: February 17, 2015
Abstract
Acne vulgaris is most common dermatological condition which is treated by a wide spectrum of therapeutic armamentarium. Moderate to severe forms are usually managed by topical and/or oral medications, but at times; either they are contraindicated or patients don’t show the optimal response. Topical Photodynamic Therapy (PDT) isan emerging modality for the treatment of acne vulgaris. PDT employs photo sensitizer, oxygen and activating light. There is no consensus so far regarding its light dosimetry and incubation period with photosensitizer however a number of clinical trials are helpful guidance. PDT with Aminolevulininc Acid (ALA) is indeed very promising, from the point of view that this is the only modality other than oral retinoid that have been proved to inhibit sebaceous gland function and to maintain prolonged remission of acne vulgaris. We present accessories of twelve patients who were successfully treated for acne with PDT after photosensitization with topical 5ALA. At the end of follow-up (after 10 weeks) ten patients were not having any new lesion and two were having only few inflammatory lesions. We therefore recommend topical PDT as an important treatment modality for intractable and resistant cases of moderate to severe acne vulgaris.
Keywords: Acne; Photodoynamic Therapy; Aminolevulininc Acid
Introduction
Many patients report an improvement in their acne following sun exposure. Indeed, visible light has been proved in studies to be a moderately effective treatment in acne. It is known that “Propionibacterium acnes” produces porphyrins, particularly coproporphyrin III. Visible light is capable to activate these porphyrins to produce a photodynamic reaction which can destroy bacteria. However, individual responses are variable and are related to differences in concentrations and types of porphyrins in an individual’s follicles and in the capability of the light to penetrate the skin and activate the photodynamic reaction. ALA is shown to be preferentially taken up by the pilosebaceous units. This is metabolized via the haem synthesis pathway to produce a build-up of protoporphyrin IX, a photosensitizer. Once photo activated by light, protoporphyrin IX is changed and excited into a triplet state with the subsequent production of singlet oxygen and many free radicals. This causes damage particularly to mitochondria, nuclei and cell membranes at their cellular level. Therefore, ALA-Photodynamic Therapy (PDT) has the potential to offer a unique way of improving acne by selectively damaging the pilosebaceous unit and killing “Propionibacterium acnes” with little damage to the surrounding skin. We have performed a therapeutic case series using topical ALAPDT to treat 12 patients with acne. The aim was to confirm its efficacy as claimed in literature.
Case Series
This clinical study was performed at CMH Lahore and Rawalpindi, Pakistan .It was approved from the ethical committees of the respective hospitals and was conducted in compliance with the standard protocol and according to the norms of good medical practices. All patients gave their informed consent before enrollment. Twelve patients (one male and eleven females, age range from 20-35 yrs.), with moderate to severe acne according to Pillsbury et al [1] were enrolled over a period of 02 years. Most of the acne lesions were localized on the maxillary eminences and chin of the patients . All patients gave positive history of previous treatment with almost all available medicine for acne in their past including oral retinoid, but all had stopped their treatment two months before the procedure. At baseline, we counted the number of lesions in a template of circular area (of 12 cm diameter) and took photographs. A baseline grading of acne severity was done according to Pillsbury et al [1].
In all twelve patients, pre procedure skin preparation was done with plain water scrub, followed by topical 5ALA application on face, applied two hours before the irradiation and the treatment side was occluded with the help of a cling film to augment absorption of 5ALA. A Waldmann PDT lamp (Waldmann Medical, Schwenningen, Germany) with a wavelength ranging from 600 to 1200 nm was used as light source. Patient and staff wore protective goggles. Skin was then irradiated using waldmann PDT lamp. The light dose was 52J/cm2and irradiance 75mw/cm2 and total duration for the exposure time was 8-10min. During the procedure skin was cooled with inbuilt fan of the lamp. The lamp switches off automatically when the timer has counted down. Those who experienced more discomfort or pain were provided with cold pack application for affected areas. Patients were advised to avoid sun for 48 hours. They were given advice regarding wound care, and informed that the acne lesions may become weepy or pustular followed by crusting which is the desired effect. The patient is advised to use topical polymyxin ointment on the lesions and methyl prednisolone on the red areas for three to four days, they were asked to contact in case of any problem. The appointment for subsequent second and third session was given 10-14 days later .12 Patients had three sessions of PDT where as two had four sessions.
Patients were called back for follow-up visit at 3, 8and 10 weeks. At every follow-up visit acne severity was graded, number of lesions counted and photograph of the irradiated areas were re-taken. But, the final inference was drawn on the results of 10th week follow-up (Table 1). On follow-up visit at three weeks, 04 patients out of 12 were having inflammatory lesions while 08 patients were cleared off any lesion. On follow-up visit of 8 weeks, 02 patients were having active inflammatory lesions. On last visit at 10thweek, still 02 patients were having inflammatory lesions and rest of the patients didn’t have any new lesion (Figure 1).
Patinet no
Age
(yrs)
Sex
Location of AcneType of Acne
Acnea score before PDT
Acne score at 10th Week after PDT
1
21
F
Cheeks and chin
Papulo-Pustular
3
1
2
24
F
Cheeks
Papulo-Pustular
2
1
3
32
F
Cheeks and forehead
Papulo-Pustular,comedonal
3
1
4
36
F
Cheeks
Papulo-Pustular
3
1
5
27
F
Cheeks
Papulo-Pustular
2
1
6
30
F
Cheeks and forehead
Papulo-Pustular,comedonal
3
1
7
31
M
Cheeks and chin
Papulo-Pustular
3
1
8
22
F
Cheeks
Papulo-Pustular
3
2
9
27
F
Cheeks,chin and forehead
Papulo-Pustular
2
1
10
31
F
Cheeks
Papulo-Pustular,comedonal
3
1
11
29
F
Cheeks
Papulo-Pustular
3
1
12
22
F
Cheeks
Papulo-Pustular,cystic
3
1
a Clinical Acne score was graded according to Pillsbury et al [1]
Table 1: Laboratory values at hospital admission.
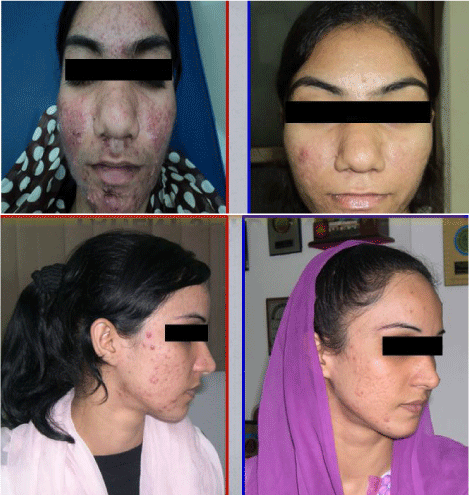
Figure 1: Acne Patients before and after treatment with PDT.
Discussion
Topical, systemic antibiotics and isotretinoin are often very good treatment options for patients with moderate to severe acne vulgaris. There are, however, few problems coming up with these conventional modalities like the emerging resistance of macrolides and oxytetracycline [2]. Many patients observe that they feel an improvement of their acne after sun exposure [3]. In fact visible light has been shown in various studies to improve acne [4]. However, many patients experience need for different treatment modality because of either of the severe adverse effects or contraindications to the available treatment modalities.
Photodynamic therapy was being used successfully for decades in many precancerous skin lesions like actinic keratosis, superficial basal cell carcinomas and there are many studies available in literature where ALA PDT had been effectively used to treat moderate to severe acne vulgaris [5,6,7,8].
There are possibly three mechanisms by which PDT may improve inflammatory acne. Primarily the photodynamic reaction through active oxygen radicals can kill the culprit bacteria “propionibacterium acnes” involved in the pathogenesis , secondly the toxic reaction also destroys the hyperactive sebaceous glands by apoptosis and necrosis ;reducing seborrhea over a period of time. Thirdly it also reduces the follicular obstruction by improving the keratinocytes shedding and hyperkeratosis. Photodynamic therapy requires photosensitizer,oxygen, and activating light. Porphyry is naturally produced in human sebaceous glands. There is variety of synthetic porphyry in precursors with different pharmacokinetic properties. Among them, ALA and methyl-ester of ALA (MAL) are available for possible offlabel treatment of acne vulgaris.
The application of topical ALA cream on acne affected areas lead to the accumulation of protoporphyrin IX in the pilosebaceous unit. This is the reason why ALA PDT specifically hit the pilosebaceous gland.
Studies in pasthaveused different light sources including 635-nmpulsedlaserlight, a600–700-nm broadband halogen source 550–700-nmbroad- band light. Similarly, different fluencies have been used in the various studies [9,10]. Hongcharuetal, used 550– 700-nm broadband light (17mW cm-2) which would seem a more aggressive regimen than that used in our study, asset brought more severe side-effects experienced by subjects including pain, folliculitis, desquamation, blistering, crusting and pigmentation lasting up to 20weeks [11].
All of our patients experienced rusticated erythematic after PDT but none of them was so severe to merit further treatment except the use of topical methylprednisolone for few days. Almost all of our patients showed mild post inflammatory hyper pigmentation at last follow-up visit.
There are many limitations in our study which; our sample size was small because of the cost of ALA; we lack control group or split face study for comparison. In Pakistan, topical Photodynamic therapy with 5ALA is the first experience in acne, mainly because of the unavailability and cost of ALA cream. The aim was to experience the effectiveness of this emerging modality as claimed by the existing literature. We recommend more control based trials, on larger sample with longer follow ups to determine its effectiveness. We believe that PDT in acne can be optimized provided its parameters regarding light dosimetry, drug delivery and light sources are defined.
References
- Witkowski JA, Parish LC. The assessment of acne: an evaluation of grading and lesion counting in the measurement of acne. Clin Dermatol. 2004; 22: 394-397.
- Eady EA, Jones CE, Tipper JL, Cove JH, Cunliffe WJ, Layton AM. Antibiotic resistant propionibacteria in acne: need for policies to modify antibiotic usage. BMJ. 1993; 306: 555-556.
- Meffert H, Gaunitz K, Gutewort T, Amlong UJ. [Therapy of acne with visible light. Decreased irradiation time by using a blue-light high-energy lamp]. Dermatol Monatsschr. 1990; 176: 597-603.
- Sigurdsson V, Knulst AC, van Weelden H. Phototherapy of acne vulgaris with visible light. Dermatology. 1997; 194: 256-260.
- Kimura M, Itoh Y, Tokuoka Y, Kawashima N. Delta-aminolevulinic acid-based photodynamic therapy for acne on the body. J Dermatol. 2004; 31: 956-960.
- Pollock B, Turner D, Stringer MR, Bojar RA, Goulden V, Stables GI, et al. Topical aminolaevulinic acid-photodynamic therapy for the treatment of acne vulgaris: a study of clinical efficacy and mechanism of action. Br J Dermatol. 2004; 151: 616-622.
- Hong SB, Lee MH. Topical aminolevulinic acid-photodynamic therapy for the treatment of acne vulgaris. Photo dermatol Photoimmunol Photomed. 2005; 21: 322-325.
- Akaraphanth R, Kanjanawanitchkul W, Gritiyarangsan P. Efficacy of ALA-PDT vs blue light in the treatment of acne. Photodermatol Photoimmunol Photomed. 2007; 23: 186-190.
- Itoh Y, Ninomiya Y, Tajima S, Ishibashi A. Photodynamic therapy for acne vulgaris with topical 5-aminolevulinic acid. Arch Dermatol. 2000; 136: 1093-1095.
- Itoh Y, Ninomiya Y, Tajima S, Ishibashi A. Photodynamic therapy of acne vulgaris with topical delta-aminolaevulinic acid and incoherent light in Japanese patients. Br J Dermatol. 2001; 144: 575-579.
- Hongcharu W, Taylor CR, Chang Y, Aghassi D, Suthamjariya K, Anderson RR. Topical ALA-photodynamic therapy for the treatment of acne vulgaris. J Invest Dermatol. 2000; 115: 183-192.