
Special Article - Clinical Cases and Images
Austin J Dermatolog. 2016; 3(1): 1042.
Annular Lichen Scrofulosorum – An Unusual Presentation of Micropapular Tuberculid
Muhammad Irfan Anwar1*, Rabia Ghafoor2, Nazia Shazhad3 and Tahira Muqaddas3
1Department of Dermatology, Pakistan Navy Ship Shifa, Pakistan
2Department of Dermatology, Jinnah Post Graduate Medical Centre, Pakistan
3Lahore General Hospital, Pakistan
*Corresponding author: Muhammad Irfan Anwar, Department of Dermatology, Pakistan Navy Ship Shifa, Karachi, Pakistan
Received: November 26, 2015; Accepted: January 04, 2016; Published: January 06, 2016
Abstract
Cutaneous tuberculids are rare manifestations of systemic tuberculosis mainly seen in children and young adults, having high degree of cellular immunity to mycobacterium tuberculosis. It is usually seen with underlying occult tuberculosis of lungs, lymph nodes, bones or after tuberculosis vaccination. It is clinically characterized by perifollicular multiple grouped or annular Micropapular eruption, predominantly over the trunk and limbs. A high index of suspicion is needed in endemic areas, as the condition imitates with many common cutaneous diseases. We herein, report a rare case of large annular lichen scrofulosorum, which is a rare morphological pattern of lichen scrofulosorum. Complete clearance of lesions was witnessed after a short course of anti tuberculous therapy.
Keywords: Annular Lichen Scrofulosorum (LS); Tuberculid; Tuberculosis
Introduction
Tuberculids are cutaneous hypersentivity reactions in patients suffering from occult or apparent systemic tuberculosis. They are usually divided into Micropapular, papular and nodular types depending predominantly on the size of individual lesions. Lichen Scrofulosorum is a prototype example of Micropapular tuberculids, comprising mainly of perifollicular grouped or annular papules. The lesions are usually asymptomatic; skins colored to reddish brown papules and are mainly found on the chest, abdomen, back and proximal parts of the upper limbs. Large annular lesions extending up to 7-9 cm are extremely rare and to our knowledge have never been reported from this region, despite of endemicity of systemic tuberculosis.
Case Presentation
A 16 years old girl presented with more than 2 years history of non-pruritic skin colored, perifollicular spiny Micropapular eruption, arranged in 5 large annular plaques (Figure 1). Three of these annular lesions were present over trunk, one over left side of neck and one over right popliteal fossa. All of them were of more than 7cm of diameter and the largest one measured over popliteal fossa was of 9 cm. She denied history of fever and cough but reported significant weight loss for last few months. Peripheral lymph nodes were not enlarged. BCG scar was seen on right deltoid area. She mentioned that her mother was successfully treated for pulmonary tuberculosis with standard antituberculous drugs for 6 months. Being the only daughter in family, patient was in habit of sleeping with her mother. Clinical differentials were Lichen Scrofulosorum, Lichen nitidus, Keratosis pilaris, Phrynoderma and Micropapular sarcoidosis. Skin biopsy for histopathology was performed which showed well formed epithelioid cell granuloma with langhans type giant cells, infiltrating upper dermis and around hair follicles (Figure 2 and 3). Montoux test was positive with in duration of 11×14mm, with raised ESR of 50 mm and chest roentgenogram showed bilateral hilar lymphadenopathy with nodular and calcific foci in upper right zone. Mycobacterial Polymerase Chain Reaction (PCR) could not be done due to non-availability of test. A final diagnosis of “Annular Lichen Scrofulosorum” was made and the patient was put on 4 drugs standard Antituberculous Therapy (ATT). Her cutaneous eruptions responded very well with complete clearance after 4 weeks of therapy (Figure 4). She was advised to complete standard 6 months ATT, with monthly follow-up visits in dermatology outpatient department to monitor therapy and outcome.

Figure 1: Large annular plaques over trunks.
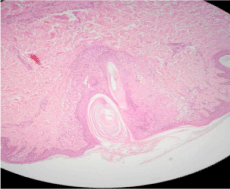
Figure 2: Photomicrograph of histopathology showing granulomatous
inflammation with giant cell in upper dermis and around hair follicle.
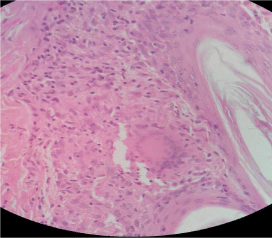
Figure 3: Photomicrograph of histopathology showing granulomatous
inflammation with giant cell in upper dermis and around hair follicle.
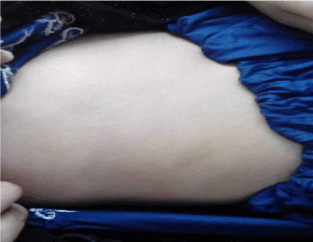
Figure 4: Complete resolution of lesions after 4 weeks.
Discussion
LS were first described by Hebra in 1868 as lichenoid eruptions in children and young adults with underlying mycobacterial tuberculosis [1]. In a large series of 39 patients, LS represented 7.6% of all patients with cutaneous tuberculosis reported over a 7-years period. In this series 84% of patients were less than 15 years of age; 72% had a focus of mycobacterium tuberculosis in the body, either in the lymph nodes, bone, lung or intracranially [2-4]. Up to 30% of patients may have no obvious underlying focus of tuberculosis. Lichen Scrofulosorum has also been reported with mycobacterium avium infection, more recently with mycobacterium Szulgai and also after BCG (Bacillus Calmette-Guerin) vaccination [5-7].
LS represent a delayed type IV hypersensitivity reaction to mycobacterial antigens. It is mostly seen in young children and adults due to an effective cellular immune response. Patients usually present with asymptomatic skin coloured to erythematous follicular and perifollicular grouped papules. Most of the lesions are present over trunk and proximal limbs but it can also be seen on other sites like genitalia and legs. Other morphological presentations include, annular, lichenplanus like, psoriasiform and granuloma annular like [8,9]. It may co-exist with other forms of tuberculids like papulonecrotic tuberculid and erythema Induratum of Bazins. Other forms of cutaneous tuberculosis, such as lupus vulgaris, tuberculousgumma and tuberculosis verrucosa cutis, may coexist [10].
Dandle A, described annular LS in a 8 years old girl, who presented with itchy erythematous annular discoid and scaly plaques (3-5cm) over trunk [11]. Total duration of lesions was 3 months. Our case presented with asymptomatic skin coloured large annular plaques (7-9cm) with total central clearance and duration was over two years. The larger size of annular lesions in our case was perhaps due to prolonged duration of disease. Both the patients received BCG vaccination in past; implying that a past vaccination cannot prevent the infection.
Clinical differentials of LS includes all asymptomatic follicular or perifollicular lesions like lichen nitidus, in which the lesions are more shiny and tend to be acral in distribution keratosis spinulosa, here the lesions have spiny projections; Keratosis pilaris, where the individual papules are predominantly scattered over proximal limbs and elbows and are their non-inflammatory nature can witnessed on histopathology; Follicular Mycosis Fungoides (MF), which entails older age bracket and non involuting nature of lesions over time. Other uncommon differentials can be popular sarcoidosis, Micropapularsyphilids and drug eruptions.
Diagnosis is made by histopathology which usually reveals noncaseating granulomatous inflammation in dermis and around hair follicles. As LS is a hypersensitivity reaction against mycobacterium, so there is no use of AFB staining and tissue culture. However, mycobacterial antigens can be detected by Polymerase Chain Reaction (PCR) in lesional specimen [12]. Test of cellular immunity against mycobacterial antigens can be used further to aid the diagnosis of LS; like Montoux test and Quantiferon Gold assay. A thorough clinical and laboratory evaluation should be performed to find out the underlying focus of mycobacterial infections. Most common extra pulmonary focus is lymph nodes followed by bones. Treatment of LS is done with standard 4 drugs anti-tuberculous therapy (Isoniazid, rifampicin, ethambutol and pyrazinamide). Eruption usually clears rapidly within 4-6 weeks of therapy.
To conclude, annular lichen scrofulosorum is a rare morphological pattern of tuberculids. High index of clinical suspicion is needed in endemic areas for the early detection of a potentially treatable infection.
References
- Yates VM, Rook GA. Mycobacterial infections. Burns T, Breatnach S, Cox N, Griffiths C, editors. In: Rook's textbook of dermatology. Massachusetts: Wiley-Blackwell. 2010; 31: 21-22.
- Singal A, Bhattacharya SN. Lichen Scrofulosorum: a prospective study of 39 Patients. Int J Dermatol. 2005; 44: 489-493.
- Hudson PM. Tuberculide (lichen scrofulosorum) secondary to osseous tuberculosis. Clin Exp Dermatol. 1976; 1: 391-394.
- Graham-Brown RA, Sarkany I. Lichen Scrofulosorum with tuberculous dactylitis. Br J Dermatol. 1980; 103: 561-564.
- Komatsu H, Terunuma A, Tabata N, Tagami H. Mycobacterium avium infection of the skin associated with lichen scrofulosorum: report of three cases. Br J Dermatol. 1999; 141: 554-557.
- Ross GL, Chong H, Collyns T. Lichen Scrofulosorum caused by Mycobacte-riumszulgai: a new cause of reaction. Br J Dermatol. 2007; 156: 586-587.
- Evans RG, Warner J. Lichen Scrofulosorum following BCG. Arch Dis Child. 1967; 42: 448.
- Weber FP. Lichen Scrofulosorum imitating Psoriasis. Proc R Soc Med. 1911; 4: 93.
- Kumar U, Sethuraman G, Verma P, Das P, Sharma VK. Psoriasiform type of lichen scrofulosorum: clue to disseminated tuberculosis. Pediatr Dermatol. 2011; 28: 532-534.
- Torrelo A, Valverde E, Mediero IG, Zambrano A. Lichen Scrofulosorum. Pediatr Dermatol. 2000; 17: 373-376.
- Dandale A, Gupta N, Dhurat R, Ghate S. Unusual presentation of lichen scrofulosorum. Indian J Dermatol Venerol Leprol. 2013; 79: 436-438.
- Tan SH, Tan BH, Goh CL, Tan KC, Tan MF, Ng WC, et al. Detection of Mycobacterium tuberculosis DNA using polymerase chain reaction in cutaneous tuberculosis and tuberculids. Int J Dermatol. 1999; 38: 122-127.