
Case Report
Austin J Dermatolog. 2017; 4(2): 1073.
Development of Genital Ulcer due to Hydroxyurea Treatment in a Patient with Polycythemia Vera - A Case Report
Duarte L¹, González LF²*, Motta A², Rolón M³ and Rojas P²
¹Dermatology Service, Simón Bolivar Hospital, Colombia
²Department of Dermatology, El Bosque University, Colombia
³Pathology Service, Simón Bolivar Hospital, Colombia
*Corresponding author: Luis Fernando González, Department of Dermatology, El Bosque University, Bogotá, Colombia
Received: March 07, 2017; Accepted: May 29, 2017; Published: June 12, 2017
Abstract
Genital ulcers due to Hydroxyurea treatment, is a very rare entity that requires the skills of dermatology specialists to suspect and diagnose it in early stages. We present a case of 48 years old female with history of polycythemia vera under treatment of Hydroxyurea during 10 years. She developed a painful genital ulcer in 15 days without any other manifestations. Herpetic etiology, HIV and primary syphilis were rejected. The skin biopsy specimen revealed neoangiogenesis associated with lymphoplasmocytic perivascular inflammatory infiltrate without evidence of vasculitis. There was a completely resolution of the lesions, 8 weeks after Hydroxyurea cessation. The patient was referred to the oncology service to continue her hematologic treatment.
Keywords: Hydroxyurea; Genital ulcer; Polycythemia vera
Introduction
Hydroxyurea is a chemotherapeutic agent used since 1960 to handle different myeloproliferative disorders. It is generally well tolerated, but in approximately 9% of patients, it will be present some side effects like nausea, headache, diarrhea and fever [1]. With its prolonged use, it can cause some skin manifestations, such as xerosis, nail disorders, diffuse hyperpigmentation, dermatomyositis-like lesions and less frequently, ulcers. Ulceration due to hydroxyurea is located in areas of major trauma, predominantly in the lower limbs, mouth and, less frequently, genital area [1-3]. We present this case because of its low prevalence, thinking about the importance of early suspicion and recognition like one of the non infectious skin lesions etiologies. It is mandatory to provide early treatment and improve the patient quality of life.
Case Presentation
We report a 48 year-old female patient, who has a medical history of polycythemia vera since 2006, receiving only oral hydroxyurea 1g per day, without any other coadjuvants treatments. After 10 years of treatment, in 2016, she was admitted to the emergency room with 15 days of a painful ulcer located in the genital area. On physical examination, well defined edge ulcer with fibrous base in the labia majora genitals was found (Figure 1). A clinical diagnosis of the ulcer was suspected, Bechet disease was dismissed since it was confirmed the absence of oral ulcer, eye or skin injuries. Clinical features of herpes simplex and syphilis ulceration, doesn’t belong to the patient type of lesion. The first one usually presents erosive and erythematous halos that follow a neural distribution, the second one, presents as a painless continuity solution, clean background, with microbiological spiroketa in culture specimen. VDRL titers, HIV, IgG and IgM for herpes type I and II was negative. A skin biopsy was performed, including culture and immunochemistry protocols. Histopathology describes an important dermal sclerosis and neoangiogenesis associated with lymphoplasmacytic perivascular inflammatory infiltrate without evidence of vasculitis on genital area (Figure 2,3). Periodic-Acid- Schiff (PAS) and Ziehl-Neelsen (ZN) stains were negative for fungi or bacterial structures. Given the clinical presentation, the background of hydroxyurea exposure and histopathological findings a diagnosis of ulcer due to hydroxyurea was made. The patient was referred to the oncology service and the withdrawal of hydroxyurea resulted in complete resolution of clinical picture in eight weeks (Figure 4).
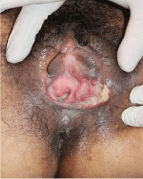
Figure 1: Ulcer 4 x 5 cm, irregular and erythematous borders.
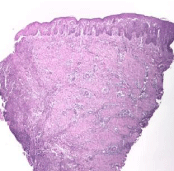
Figure 2: H-E 5X. Ulcer biopsy showing intersticial fibroses and slight
neoangiogenesis.
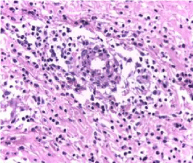
Figure 3: H-E 40X. Lymphoplasmocytic perivascular inflammatory infiltrate
without evidence of vasculitis.
Discussion
Polycythemia Vera is one of the chronic myeloproliferative neoplasms, which are characterized by clonal proliferation of myeloid cells and the presence of an elevated red blood cell mass. One of the main entities of its treatment is the Hydroxyurea (HU), a chemotherapeutic agent used to maintain a platelet count below 600,000/microL and the hematocrit below 50% [1,4,5].
The reported adverse events during HU treatment are numerous and concerning different body systems, including bone marrow, gastrointestinal system and multiple cutaneous alterations such as xerosis, scaling, atrophy of the skin and subcutaneous tissues, skin hyperpigmentation, facial and acral erythema, palmoplantar keratoderma, partial non-cicatricial alopecia, nail alterations, solar hypersensitivity with eruptive appearance of squamous cell and basal cell carcinomas [4,5].
Cutaneous ulcers during HU therapy, are still today a poorly recognized side effect of this drug. The first reports of ulcers use of hydroxyurea are since 1985, appearing in approximately 9% of patients with myeloproliferative diseases receiving high doses for prolonged periods, most often between 2 and 7 years of drug use [1,5]. Most are described in the lower limbs, in areas of major trauma. Two case reports of genital ulcers, one in glans and another was found only in vaginal mucous and the case presented (Table 1). The similarities that these cases have, comparing with ours is that when the dose is reduced or the UH treatment is discontinued; the genital ulcers progressively decrease in size until they disappear completely in 6 to 8 weeks.
Authors
Comorbidities
Dose of Hydroxyurea
Presence of vasculitis
Management time with HU
Mucous location
Karincaoglu, et al (2003)
Chronic myeloid leukemia
4 g/day
Yes
2 weeks
Genital (Vulva)
Lei Su , et al (2011)
Polycytemia Vera
1.0±0.5g/day
Yes
12 years
Genital (glans)
Table 1: Ulcer due to hydroxyurea treatment, case reports [2-4].
HU or hydroxycarbamide, is a non-alkylating hydroxylated urea analog with antineoplastic and antiviral properties. It is instead a non-competitive inhibitor of the enzyme ribonucleotide reductase, which results in depletion of desoxyribonucleotides, cessation of DNA synthesis and death of S-phase cells [6].
Hydroxyurea-induced cutaneous ulcers are usually small, welldefined and shallow with an adherent, yellow, fibrinous necrotic base. They are typically found in the perimalleolar region but also on the lower leg. Genital ulcer is extremely rare, but when it’s presented are bigger than cutaneous one and are correlated with a greatest doses and time of treatment with HU [1,7].
The ulcer cause is unknown, however it is believed that long term HU therapy leads to cumulative cytotoxicity for the basal cells of the epidermis, due to inhibition of DNA synthesis and formation of free radicals. The injury progresses until cellular repair mechanisms are no longer able to regenerate keratinocytes and endothelial cells [8,9].
The diagnosis is made by clinical, suspecting in patients using this drug, a skin biopsy is useful to rule out other diagnoses. The histology of the lesion is usually a specific, but may show epidermal atrophy, dermal fibrosis, scar tissue without vasculitis and, occasionally, fibrinoid thrombi.
Differential diagnosis must be done with many entities including infectious etiologies such a herpes simplex virus, syphilis, cytomegalovirus, chancroid, venereal lymphogranuloma and Human Immunodeficiency Virus. Non infectious causes include tumors, pyoderma gangrenosum, trauma and vasculitis. In this patient, Behçet disease was rejected, be considering no major criteria was presented [10].
Treatment involves stopping the medication, there by lesion improvement is achieved after two or three months as was observed in our case, in whom complete resolution of the lesion was observed 2 months after stopping hydroxyurea [11,12] (Figure 4).
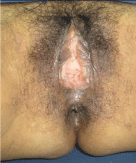
Figure 4: Ulcer resolution after 8 weeks of discontinuation hydroxyurea
treatment.
Conclusion
We report the case of a patient with ulcer secondary to chronic use of hydroxyurea in unusual location (vaginal mucosa), who after the drug suspension presented complete resolution of the lesion within two months, as described in the literature.
We believe it is a demonstrative case and of great academic interest because of the diagnostic challenge presented and its easily management when it is well diagnosed. Despite hydroxyurea is not a drug commonly prescribed in dermatology area and its adverse effects are rare, a large number of skin lesions presentation can simulate this entity, and always it would be suspect if hydroxyurea treatment is in between.
References
- Quattrone F, Dini V, Barbanera S, Zerbinati N, Romanelli M. Cutaneous ulcers associated with hydroxyurea Therapy. Journal of Tissue Viability. 2013; 22: 112-121.
- Badawi M, Almazroa S, Azher F, Alsayes F. Hydroxyurea-induced oral ulceration. Oral Surg Oral Med Oral Pathol Oral Radiol. 2015; 120: 232-234.
- Karincaoglu Y, Kaya E, Esrefoglu M, Aydogdu I. Development of large genital ulcer due to hydroxyurea treatment in a patient with chronic myeloid leukemia and Behcet’s disease. Leuk Lymphoma. 2003; 44: 1063-1065.
- Lei Su, Zheng J, Lingling X. Antineutrophil cytoplasmic antibody-associated vasculitis in a patient with polycythemia vera after long-term hydroxyurea treatment. Leukemia & Lymphoma. 2011; 52: 2193-2194.
- Saravu K, Velappan P, Lakshmi N, Ananthakrishna B, Thomas J. Hydroxyurea Induced Perimalleolar Ulcers. J Korean Med Sci. 2006; 21: 177-180.
- Dissemond J, Körber A. Hydroxyurea-induced ulcers on the leg. Canadian Medical Association Journal. CMAJ. 2009; 180: 1132.
- Kelly RI, Bull RH, Marsden A. Cutaneous manifestations of long-term hydroxyurea therapy. Australas J Dermatol. 1994; 35: 61-64.
- Kovacic P. Hydroxyurea (therapeutics and mechanism): Metabolism, carbamoyl nitroso, nitroxyl, radical, cell signaling and clinical application. Medical Hypothesis. 2011; 76: 24-31.
- Besses C, Alvarez L. How to treat essential thombocythemia and polycythemia vera. Clinical Lymphoma, Myeloma & Leukemia. 2016; 16: S1-S114-123.
- Dorado JS, Montes JO, Espinar PC. Diagnostic and therapeutic protocol for genital ulcers. Medicine. 2014; 11: 3024-3028.
- Lopes FC, Ferreira R, Martins D, Albuquerque DM, Silveira AA, Costa R, et al. In vitro and in vivo anti-angiogenic effects of hydroxyurea. Microvascular Research. 2014; 94: 106-113.
- Ayalew T. Clinical manifestations and diagnosis of polycythemia vera. 2016.