Department of Cardiology, Indo US Super Speciality Hospitals, India
*Corresponding author: Pankaj Jariwala, Department of Cardiology, Indo US Super Speciality Hospitals, Shyam Karan road, Anand Bagh, Ameerpet, Hyderabad, 500016, India
Received: October 24, 2014; Accepted: November 21, 2014; Published: November 24, 2014
Citation: Pankaj J, Satya Sridhar K, Umadevi N, Sarat Chandra K and Prasada Rao D. Unusual Cause of Pleural Effusion after Surgery for Left Atrial Myxoma. Austin J Clin Cardiolog. 2014;1(5): 1032. ISSN 2381-9111
Chylothorax presenting as a pleural effusion after excision of Left atrial myxoma is not reported so far. In our case, there was delayed clinical manifestation after 3 months of the index surgery. The case was initially managed conservatively, but as drainage of chyle was more than 300- 400 ml per day hence surgical management was sought and successfully treated. We have reviewed in brief the etiology and management of postoperative chylothorax.
Keywords: Pleural Effusion; Chylothorax; Left atrial myxoma; Thoracotomy
Chylothorax is a rare complication after cardiac surgery and rare etiology of pleural effusion. Chyle is enriched lymphatic fluid with fat and its digestive products absorbed through the intestine. Traumatic injury to the thoracic duct leads to leakage of chyle into the pleural space. We report a case of chylothorax and its successful management of a patient who underwent left atrial myxoma excision. To our knowledge this is the first case report of chylothorax after left atrial myxoma surgical excision in literature.
A 50 year old lady presented with complaints of breathlessness at rest since last 1 week. She underwent left atrial myxoma surgery 3months before at another cardiac Institute. As per the discharge records, she had an uneventful postoperative course during previous hospitalization and was discharged in stable condition.
On examination, she was tachypneic with a respiratory rate of 22/min. Her blood pressure in the right upper limb was 130/80 mm Hg and pulse rate of 104 / min. Room air saturation of 94%, which improved to 100 % with oxygen inhalation of 4 liters/ min. There was a stony dull note on percussion and on auscultation, an absent air entry on the left side of the chest. There were no other adventitious sounds. Heart sounds were normal and there was no murmur.
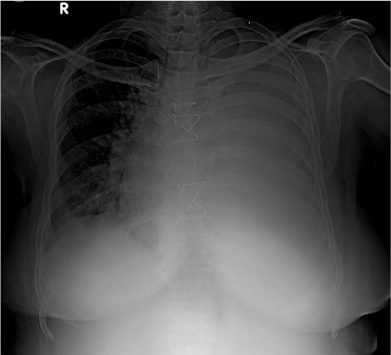
Laboratory investigations were normal and chest x-ray revealed homogenous opacity involving the entire left thorax. Cardiac silhouette was normal in size and contour with minimal shift of the mediastinum to the right (Figure 1).
Pleurocentesis revealed 500 ml of creamy white pleural fluid (Figure 2).The appearance of pleural fluid was diagnostic of chylothorax which was sent for the laboratory evaluation. It revealed normal proteins and sugars, but low levels of cholesterol, high triglycerides and cytology showed predominance of lymphocytes as shown in Table 1. Intercostal drainage was instituted as there was reaccumulation of pleural fluid next day on repeat chest X-ray. The patient was started on low fat diet in consultation with a dietitian.
Daily Intercostal drainage of chyle was more than 300- 400 ml at the end of 1 week of admission (Figure 3). The case was discussed with Cardiothoracic surgeon, as there was no response to the conservative line of management. The possibility of iatrogenic injury to the thoracic duct was suspected during surgical excision of left atrial myxoma.
After 10 days of admission, patient was subjected to left postero-lateral thoracotomy on single lung ventilation. Before thoracotomy patient was given 100 ml of ‘ghee’ which contains high level of triglycerides through the Ryle’s tube. After thoracotomy done and left lung was deflated, we could see clear fluid coming at the recess of descending thoracic aorta with the left pulmonary artery once the visceral pleura was incised (Figure 4). Multiple 4-0 Prolene Teflon pledged suture were taken and recess was closed en mass to ligate the thoracic duct (Figure 5). Vascular adventitial aortic flap was reflected on in this area to ensure the complete sealing off the leakage. Adjacent left parietal pleurectomy done (Figure 6). Thorocotomy was closed in a routine manner.
The patient improved postoperatively to decrease in the drainage of chyle through chest drainage with complete resolution in 1 week. A patient with chest tube was removed and was discharged on 10th post operative day in stable condition. She has completed her 6 month follow up visit with no repeat symptoms with normal chest x-ray.
Chylothorax, lymphatic pleural effusion, is a rarity. It is characterized by its appearance of milky cloudy fluid and biochemistry - elevated levels of triacylglycerols (twice to eight times as much as in serum), low level of cholesterol, elevated lymphocyte count and presence of chylomicrons [1].
Chylothorax results in the loss of large amounts of fat and protein and produce a serious state of inanition [2]. The etiology of chylothorax is as shown in Table 2. Postoperative chylothorax occurs in only 0.2 to 1.5 % of patients undergoing thoracic aortic aneurysm repair, but can complicate any cardiovascular operation [3].
Significant variations in the normal course of thoracic duct drainage pattern can occur. The normal pattern is seen in about 65% of the population. Infrequently, the upper portion of the thoracic duct divides into two branches that drain separately, one in the usual manner and the other reaching the right subclavian vein [4]. This variation from the normal anatomical pattern explains the incidence of chyle leak despite care. In our case possibility of damage to thoracic duct while subclavian vein cannulation might have caused a chyle leak which manifested after a few weeks after resuming normal home diet pattern.
Conventional treatment of chylothorax includes pleural drainage, total parenteral nutrition, and early duct ligation via a transthoracic surgical approach. Timing of surgery is controversial, but usually a surgical option is considered if 1] Drainage lasts 1 to 3 weeks 2] Daily output > 200mL to 500 ml per day [2]. In postoperative chylothorax, revision should be performed early on, since conservative management is likely to be unsuccessful [5]. The quantity of chyle drained per 24 hours appeared to be the best indicator to guide management decisions.
The surgical options are transthoracic and trans-abdominal duct ligation, which can be attempted via minimally invasive VATS or conventional method. Pleura-peritoneal shunt should be reserved for excessive chylous leaks (of 1 to 2 weeks’ duration, with output greater than 1,000 ml/day) [6] (Table 3).
We opted for the surgical management of in our case because etiology was unexplained as left atrial myxoma excision does not involve manipulation near thoracic duct and there was a continuous drainage of significant amounts of chyle.
Sziklavari et al used radiotherapy in 7 patients with postoperative chylothorax if the daily chyle flow exceeded 450 ml after complete cessation of oral intake. The patients’ mediastinum was radiated an average of six times. Radiotherapy, in combination with dietary restrictions, was successful in all patients [7]. Radiotherapy option was not considered in our patient as patient refused for it and opted for surgical management as she wanted no further recurrence of symptoms.
Post operative chylothorax is a very rare complication and there is no case report of its development after excision of left atrial myxoma surgery. Apart from conservative management, which we tried, but as there was accumulation of chylothorax hence surgical exploration and closure of leak is the best option. Radiotherapy also treatment option but needs larger studies to document its efficacy. There are no guidelines available for the management of chylothorax and individual decision per patient is necessary as per the experience of the Cardiothoracic team as a collective decision.
Laboratory investigations of plural fluid.
Sugar : 96 mg/dL |
Protein : 5.5 mg/dL |
WBC : 2400 cells; Lymphocytes: 100%, RBC: Few |
Cholesterol : 70 mg/dL/Serum Total Cholesterol: 182 mg/dL |
Triglycerides : 800 mg/dL/Serum Triglycerides: 176 mg/dL,Cholesterol/triglyceride ratio <1 |
Gram Stain : Negative. |
Etiology of Chylothorax [2,3,8].
Spontaneous - inborn developmental anomalies of lymphatic vessels (congenital chylothorax) |
Tumors (lymphomas) or Lymphangiomyomatosis |
Infections (lymphadenitis, filariasis) & Specific inflammations (tuberculosis, sarcoidosis) |
Liver Cirrhosis |
Thrombosis of the subclavian vein or superior vena cava |
Complication of surgery of the esophagus, larynx, lungs, mediastinum, heart or great vessels |
Complication of great vessel cannulation or translumbar angiography |
As a sequel of radiotherapy |
Summary of treatment modalities in chylothorax [6].
Conservative strategy Nil by mouth Medium-chain triglycerides by mouth Total parenteral nutrition |
Drainage of chylothorax Thoracentesis Intercostal tube drainage |
Operative strategy Direct ligation of thoracic duct Mass ligation of supra-diaphragmatic thoracic duct Pleuro-peritoneal shunting Pleurectomy Pleurodesis |
Radiotherapy |
Chest X-ray PA view showing homogenous opacity of entire left lung with the shift of the mediastinum to right in the post sternotomy patient suggestive of massive pleural effusion.
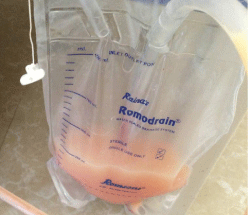
Aspirated creamy white frothy pleural fluid.

Intercostal chest drain bag showing drainage of chyle. There was a daily collection of 300-400 ml despite low fat diet.
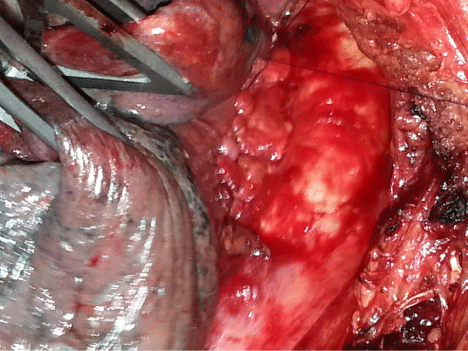
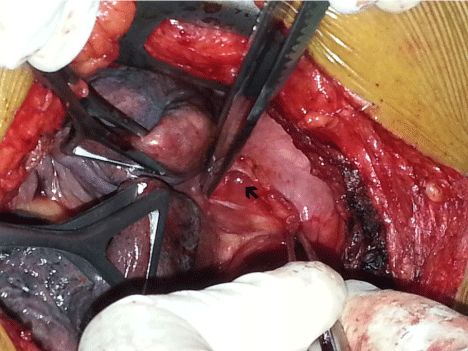
Intra operative photograph showing retracted left lung to expose recess between left pulmonary artery and descending thoracic aorta. There was a continuous drainage of clear fluid [Thick Arrow].
En mass closure of aorto-pulmonary recess using pledeted sutures.
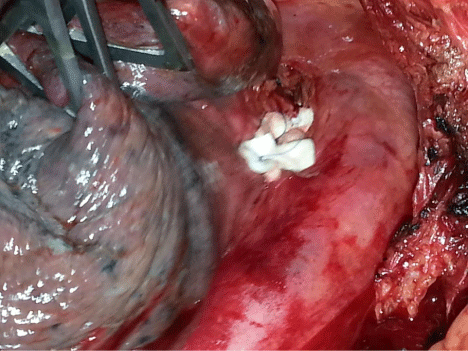
Vascular adventitial aortic flap was covered over to close the recess to assure sealing off the area to prevent any recurrence.