Case Report
Austin J Clin Case Rep. 2014;1(7): 1035.
Localized Treatment of Chronic Buruli Ulcer with Hyperoil™: An Unexpected Outcome
Iabichella ML1,4*, Topolinska M2, Amaku Anzako C2, Pediliggieri C1,4, Izzo A3, Bertolotti A3 and Lugli M4
1Helios Med Onlus, Italy
2Ariwara Hospital, Central Africa
3Inter Med Onlus, Italy
4Department of Cardiovascular, Deep Venous Surgery and Tissue Repair International Centre, Italy
*Corresponding author: Iabichella ML, Helios Med Onlus, International Health Organization, 97016 Pozzallo (RG), Italy
Received: July 10, 2014; Accepted: Aug 05, 2014; Published: Aug 08, 2014
Abstract
The successful sustained outcome of this patient with chronic Buruli Ulcer treated with Hyperoil™, suggests its use for local treatment of infected ulcers with bone exposition. Hyperoil™ use could be particularly effective in endemic areas, far from specialized centers, where African populations living in poor rural areas are more difficult to be treated.
Keywords: Chronic Buruli ulcer; Buruli ulcer local treatment; Osteomyelitis; Infected utaneous ulcer
Background
Buruli Ulcer (BU) is an extensive tissue necrosis resulting from an initial skin infection caused by a diffusible lipid toxin (mycolactone) produced by Mycobacterium ulcerans, a bacterium prevalent in humid, rural tropical areas. Several thousand people are infected each year, especially in tropical Africa, where BUs are often a source of major disability, especially linked with super-infections [1]. As little is known about disease transmission, prevention is difficult. Furthermore, even if several studies are in progress, to date, there is no vaccine[1]. A combination of oral rifampicin and injectable streptomycin is the treatment recommended by World Health Organization [2,3], in early, limited disease [4], but in a few cases in the deep and remote lands, because of the lack medicines, it is not possible use antibiotics [5]. As not all patients with M. ulcerans infection have BU, the synergistic anti-mycobacterial action of antibiotics and immune defense mechanisms may be required to treat the infection efficiently [6]. The differential diagnosis of BU due to M. ulcerans, based on clinical and epidemiologic basis only, is difficult [3],, so the BU diagnosis needs to be confirmed by IS2404 polymerase chain reaction (PCR) [7].
Surgical treatment and functional rehabilitation are often necessary but their use and the best time for surgery for large BUs needs clarification3. High relapse rates [8], prohibitive cost and limited access to surgery in endemic areas in Africa (far from National reference centers for BU treatment) led to search new therapeutic options being easily used by local health care providers in these poorly assisted areas. Some BUs can become chronic as not fully recovered because of inappropriate treatment, or even using reference treatments, that led to infection [9].
Members of the no-profit organization Helios Med periodically go to Ariwara (Congo Democratic Republic, Africa), for training missions to local health care providers working in the surgical clinic. Chronic BU is an endemic pathology in Congo DR, especially in younger population of the most isolated zones. The presence of M. ulcerans was confirmed with Zihel Nielsen method performed in the laboratory equipped by Inter Med Onlus.
Trainings include the antiseptic treatment of the wounds with ozone therapy, being the standard protocol applied for the treatment of BU [9]. During our last mission, on July 2013, the ozone production unit stopped working and, thus, we were obliged to find an alternative wounds local treatment.
The only available antiseptic we had was Hyperoil™, a mixture of hypericum flowers extract (Hypericum perforatum) and nimh oil (Azadirachta indica) produced by RIMOS S.r.L. Mirandola (MO) - Italy (Medical Device Class IIB CE0476), available as oil, gel, cream and gauze gel, that was recently tested to be used in complicated diabetic foot ulcers [10].
Case Presentation
We used Hyperoil™ on 13 years old boy with a chronic BU on the bottom right leg and osteomyelitis. Chronic BU was located on the lateral bottom middle third of the right leg and on the upper pole (at about 4 cm from the perilesional cephalic margin), and appeared about 15 months before. The patient refers the lesion started as a painful nodule on the leg that becomes edematous. Then, the skin above the nodule ulcerated with white-yellow material in the middle of the lesion, having cotton appearance. The lesion becomes largerand deeper in the next days. This patient was previously treated with an unknown antibiotic therapy and his ulcer had a surgical toilette, with temporary improvement of symptoms. Then, because of the lack of money to continue treatments, UB worsened in the following year.
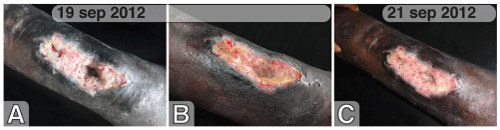
On September 19th 2012, when the boy was visited by us for the first time, a chronic UB (13.5x5 cm, Figure 1A) appeared localized, exuding and smelly, with focal exposed bone necrosis on two sites (depth, respectively, 0.3 mm and 1 cm) in a limited area healed, with slight scar retraction, in the third distal area of the right leg (approximately 4 cm from the cephalic peri-lesional margin). The ulcer was delimited by partially regular and undermined edges, skin being scarcely elastic and edematous in the area around the lesion.
Figure 1 : Chronic Buruli Ulcer before starting treatment with Hyperoil™ (A). The first application Hyperoil™ oil (B) on September 19th 2012 and after 2 days (C) on September 21st 2012.
Two areas in the lesion (1 cmq and 3 cmq, respectively) showed exposed periosteal with bony fragment necrosis of the tissue. The bottom of the ulcer was strength fibrous. The peripheral cutaneous tissue of the ulcer was hyper-keratotic, dystrophic, hyper-chromic and with some necrosis.
The patient needed to use a walking stick and feel pain (VAS score = 5).
The clinical anamnesis and objective evaluation confirm the diagnosis of chronic BU.
Management
This wound was treated with Hyperoil™ oil applications (Figure 1B) on any other day. The skin around the wound was carefully cleaned with normal Ringer solution and gauze having a few drops of Hyperoil™ oil. The ulcer’s bed and undermined edges were, than, cleaned, as, exudates and fibrin residuals or necrotic materials were removed, with a gauze with Hyperoil™. Then, a little Hyperoil™ oil was dropped in the ulcer including exposed bone. In addition, ulcer was covered with gauze and bended to maintain dressing in the appropriate zone and let the ulcer cleaned from dust. Surprisingly, 2 days after the first application of Hyperoil™ skin hyperchromia was reduced, lesion edges and ulcer fundus showed an improvement of cutaneous tropism (Figure 1C).
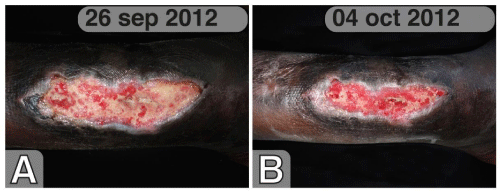
Necrosis was completely cleaned after the first week of therapy (on September 26th 2012) and chronic UB showed a partial reduction of fibrin with the appearance of granulation tissue (Figure 2A).
Figure 2 : Chronic Buruli Ulcer after 1 week (A) and 2 weeks (B) of treatment with Hyperoil™.
After 2 weeks, the bone turned to be covered (Figure 2B); the granulation tissue was well represented on the whole area of the ulcer. Peri-lesional edges were no more undermined. The ulcered area was reduced and the wound become superficial. The patient was able to walk without any aim and pain disappeared (VAS = 0).
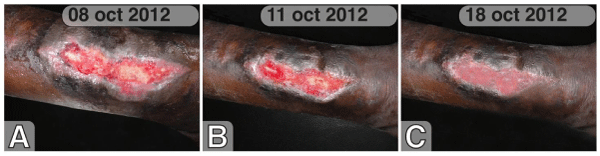
Eighteen days after starting Hyperoil™ treatment, new epithelium appeared on the lower pole of the lesion, and new skin appeared when medication was substituted (Figure 3A).
Figure 3 : Chronic Buruli Ulcer after 18 days (A), 3 (B) and 4 (C) weeks of treatment with Hyperoil™.
After 3 weeks, the ulcer continued to reduce its hyperchromy and it’s without discoloration size, without any cicatrized area (Figure 3B). This was a surprising outcome.
One month later, on October 18th 2012, the ulcer was completely healed (Figure 3C) without scar retraction.
The absence of relapse was confirmed by a phone follow-up call, with a local physician, on May 2014.
The patient gave his consent to publish the results of this case.
Discussion
Chronic BU remains a serious health issue especially where WHO recommendations are difficult or cannot be applied due to severe poverty and geographical isolation[9].
The differential diagnosis of BU needs to be confirmed by Ziehl- Neelsen (ZN) staining [11] and PCR7. Diagnostic tests are suitable for use in primary care settings but these are difficult to be performed in the most isolated zones. Often, but not in our case, diagnosis has to be performed on a clinical basis, only.
Antibiotic therapy, recommended by WHO, is really effective even at long term [12,13], but is relatively expensive and, in some cases, difficult to be reached especially in the most poor and remote endemic areas of BU, where traditional poorly-effective remedies remain a frequent choice [14]. In these areas the recommended surgical approach is difficult to be applied, too, due to the lack of or the difficulty to access to hospitals [14].
Having a cheap and simple-to-be-transported therapeutic option, as Hyperoil™ to treat patients with chronic BU, could give to local well trained health care providers a new topical local treatment. This approach to the patient with chronic BU, including health education [15], could permit BU treatment and control.
Conclusion
Despite not having PCR confirmation of the diagnosis of UB, the unexpected recovery of this patient treated with Hyperoil™ opens a new perspective for the future of local chronic UB treatment. Properly designed, controlled trials are needed to confirm this first observation.
Acknowledgment
The authors thank the Canossian Sisters of the mission in Ariwara Hospital, RD Congo, the Congo Ministry of Health and Andrea Rossi, professional medical writer, for his assistance in medical writing.
References
- Einarsdottir T, Huygen K. Buruli ulcer. Hum Vaccin. 2011; 7: 1198-1203.
- Etuaful S, Carbonnelle B, Grosset J, Lucas S, Horsfield C, Phillips R, et al. Efficacy of the combination rifampin-streptomycin in preventing growth of Mycobacterium ulcerans in early lesions of Buruli ulcer in humans. Antimicrob Agents Chemother. 2005; 49: 3182-3186.
- Kibadi K, Boelaert M, Fraga AG, Kayinua M, Longatto-Filho A, Minuku JB, et al. Response to treatment in a prospective cohort of patients with large ulcerated lesions suspected to be Buruli Ulcer (Mycobacterium ulcerans disease). PLoS Negl Trop Dis. 2010; 4: e736.
- Nienhuis WA, Stienstra Y, Thompson WA, Awuah PC, Abass KM, Tuah W, et al. Antimicrobial treatment for early, limited Mycobacterium ulcerans infection: a randomised controlled trial. Lancet. 2010; 375: 664-672.
- [No authors listed]. Buruli ulcer. A disabling infection. Prescrire Int. 2010; 19: 261-262.
- Schutte D, Um-Boock A, Mensah-Quainoo E, Itin P, Schmid P, Pluschke G. Development of Highly Organized Lymphoid Structures in Buruli Ulcer Lesions after Treatment with Rifampicin and Streptomycin. PLoSNegl Trop Dis. 2007; 1: e02.
- Buruli ulcer. Mycobacterium ulcerans infection. 2014.
- Kibadi AK. [Relapses after surgical treatment of Buruli ulcer in Africa]. Bull Soc Pathol Exot. 2006; 99: 230-235.
- Bertolotti A, Izzo A, Grigolato PG, Iabichella ML. The use of ozone therapy in Buruli ulcer had an excellent outcome. BMJ Case Rep. 2013; 2013.
- Iabichella ML. The use of an extract of Hypericum perforatum and Azadirachta indica in advanced diabetic foot: an unexpected outcome. BMJ Case Rep. 2013; 2013.
- [No authors listed]. Buruli ulcer: progress report, 2004-2008. Wkly Epidemiol Rec. 2008; 83: 145-154.
- Vouking MZ, Tamo VC, Tadenfok CN. Clinical efficacy of Rifampicin and Streptomycin in combination against Mycobacterium ulcerans infection: a systematic review. Pan Afr Med J. 2013; 15: 155.
- Klis S, Ranchor A, Phillips RO, Abass KM, Tuah W, Loth S, et al. Good Quality of Life in Former Buruli Ulcer Patients with Small Lesions: Long-Term Follow-up of the BURULICO Trial. PLoS Negl Trop Dis. 2014; 8: e2964.
- Mulder AA, Boerma RP, Barogui Y, Zinsou C, Johnson RC, Gbovi J, et al. Healthcare seeking behaviour for Buruli ulcer in Benin: a model to capture therapy choice of patients and healthy community members. Trans R Soc Trop Med Hyg. 2008; 102: 912-920.
- Agbenorku P, Agbenorku M, Amankwa A, Tuuli L, Saunderson P. Factors enhancing the control of Buruli ulcer in the Bomfa communities, Ghana. Trans R Soc Trop Med Hyg. 2011; 105: 459-465.