Abstract
Anti-N-Methyl-D-Aspartate Receptor (anti-NMDA-R) encephalitis is an immune-mediated syndrome that was first described in 2007. We describe two patients with anti-NMDAR encephalitis who developed Pneumatosis Intestinalis (PI) during the course of their disease. Pneumatosis intestinalis in the setting of anti-NMDA-R encephalitis has not previously been reported in the literature. That led to speculation whether the association between anti-N-methyl-Daspartate receptor encephalitis and pneumatosis intestinalis is secondary to immunosuppression, medication effect, or a direct manifestation of auto antibodies will require further study. Our patients highlight the occurrence of this rare complication in critically ill patients with NMDA-R encephalitis who usually admit to pediatric intensive care unit. Early recognition and appropriate therapy are essential to recovery in patients who develop this complication.
Keywords: Anti-n-methyl-d-aspartate receptor; Pneumatosis intestinalis; Encephalitis
Abbreviations
Anti-NMDA-R: Anti-N-Methyl-D-Aspartate Receptor; PI: Pneumatosis Intestinalis; CSF: Cerebrospinal Fluid; EEG: Electroencephalogram; NG: Nasogastric; NJ: Nasojejunal; TPN: Total Parenteral Nutrition
Introduction
Dalmau et al first described anti-NMDA-R encephalitis in 2007 [1]. The classic presentation of anti-NMDA-R encephalitis includes psychiatric, neurologic, and autonomic symptoms [2]. Patient evaluation includes examination of Cerebrospinal Fluid (CSF), brain MRI, Electroencephalogram (EEG), and Anti-N-methyl-D-aspartate receptor antibodies in blood and CSF fluid [3].
In the other hand, Pneumatosis Intestinalis (PI) is a wellrecognized manifestation of Necrotizing Enterocolitis (NEC) in the newborn. However, limited information is available concerning PI in older children. West et al reported sixteen older infants and children with PI [4]. Associated conditions include short bowel syndrome, congenital heart disease, iron ingestion, nesidioblastosis, hemolytic anemia, rheumatoid arthritis, bronchopulmonary dysplasia, and malrotation [4]. In adults, PI has been reported after treatment with cetuximab, docetaxel, sunitinib, a-glucosidase inhibitor, and after neoadjuvant chemotherapy for esophageal cancer [5-9].
In this report, we describe two patients with anti-NMDA-R encephalitis whose clinical course was complicated by PI.
Case Presentation
Case A
A 13-year old African American female with a past medical history of attention deficit hyperactivity disorder was admitted to the psychiatric unit due to sub-acute altered mental status, auditory and visual hallucinations, and violent behavior. Her condition progressed to fluctuating levels of alertness and she developed catatonia, difficulty breathing and a fever. Her EEG was consistent with encephalopathy without seizure. Lumbar puncture showed a normal opening pressure and mild pleocytosis with 35 white blood cell, and positive EBV by PCR. A head CT and brain MRI were normal. During the next few days of hospitalization, she developed tachycardia, clonus, garbled speech, agitation, aggressive behavior and hyperreflexia. Due to altered mental status and concerns for aspiration, she was started on Nasogastric (NG) feeding that was subsequently changed to Nasojejunal (NJ) due to feeding intolerance. A presumptive diagnosis of autoimmune encephalitis was made, after infectious diseases were ruled out. She was empirically treated with IV methylprednisolone and Rituximab. After this, she developed seizures and was started on levetiracetam. Risperidone, lorazepam, trihexyphenidyl hydrochloride, clonidine, gabapentin, and chloral hydrate were added for a symptomatic management of her agitation and pain. On day 10, the result of anti-NMDA-R antibody from cerebral spinal fluid was reported as positive, with a titer of 1:40. Due to the progressive course of her illness, she was started on plasmapheresis for five cycles followed by intravenous immunoglobulin for 2 doses. She received also piperacillin/tazobactam and vancomycin for possible pneumonia and ganciclovir for EBV. On day 12, she developed abnormal movements with limb stiffening, head deviation, and orolingual dyskinesia. On day 13, she developed sudden onset eye blinking, oral-facial dyskinesia, and tonic synchronized flexion of neck, upper and lower extremities associated with a brief desaturation. An EEG demonstrated seizure activity and she developed status epilepticus. She was transferred to the pediatric intensive care unit, treated with fosphenytoin, and required mechanical ventilation for 3 days. She had tachycardia and tachypnea with intermittent hypertension presumed to be due to an autonomic dysfunction. A week later, she developed fever, seizure, and diarrhea. Stool Clostridium difficile, rotavirus, and adeno virus studies were negative. Her examination showed abdominal distension. She continued to have diarrhea and on day 28 developed bilious emesis. Her abdominal radiograph revealed pneumatosis in her cecum and ascending colon (Figure 1A). An abdominal CT scan demonstrated extensive pneumatosis (Figure 1B-1D). All enteral feeding was discontinued and she was started on piperacillin/ tazobactam and Total Parenteral Nutrition (TPN). The pneumatosis resolved after 3 days based on imaging by serial abdominal radiographs. NJ Feeds were restarted gradually and finally a gastric-tube was placed. By day 46 her neurologic status improved, as did her sleep and communication. However, she continued to be emotionally labile. She was started on monthly IVIg and mycophenolate mofetil for long-term management. She received inpatient rehabilitation services and was then discharged home. During her outpatient follow up, she continued to show improvement and remained seizure free.
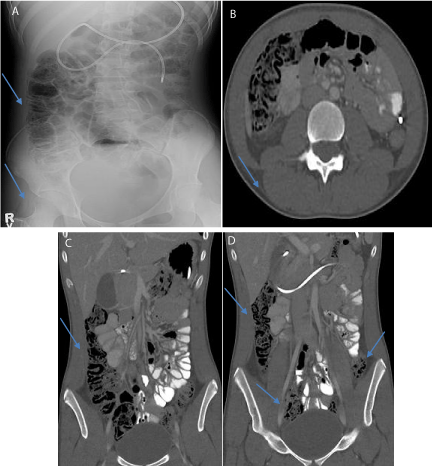
Figure 1: A 13 year old was diagnosed with anti NMDA-R encephalitis. On
day 28 of her hospitalization, her abdominal radiograph (A) shows ascending
colon pneumatosis. On her abdominal CT scan the axial section (B) shows
pneumatosis of hepatic flexure of the colon and the coronal section (C and
D) shows extensive pneumatosis extending from the cecum through the
descending and sigmoid colon. NJ tube also seen on these images.
Case B
A 7 year old female presented with fever for 10 days and abnormal behavior for 2 days. She had difficulty ambulating, nasal speech, and mood lability. She had trouble using her dominant hand and could not dress herself. On admission, a lumbar puncture opening pressure was 29mm H2O, CSF analysis showed mildly elevated protein 48mg/dl, and normal cell count. She was started on vancomycin, ceftriaxone, and acyclovirs empirically pending further testing for infections but antibiotics were discontinued once laboratory testing for common infectious etiologies of encephalitis were negative. A brain MRI showed no acute abnormalities. She then developed choreathetoid movements involving the left upper extremity and neck and intermittent twitching of left face. The long-term video EEG showed no seizures. Her mental status declined drastically over 6 days of hospitalization and repeat MRI demonstrated an abnormal area of increased T2-weighted signal within the inferior aspect of the left cerebellar hemisphere. A repeat lumbar puncture was done and Anti-NMDA- R antibodies, paraneoplastic autoimmune antibodies, and oligoclonal bands were sent. She was empirically treated with IVIg and IV methylprednisolone followed by oral prednisolone. Due to her encephalopathy and aspiration risk, a nasogastric feeding tube was placed in the first few day of the admission and later replaced with NJ tube for feedings. It was noted that she had abdominal distention by examination. Anti-NMDA-R antibodies were reported as positive in the CSF but negative in the serum. Due to minimal improvement another five-day course of methylprednisolone was started. Rituximab was given on the 25th day of hospitalization but she developed a rash and cyclophosphamide was started for immunosuppression. Clonidine, lorazepam, chloral hydrate, trihexyphenidyl hydrochloride, and trazodone were added for symptomatic management of her agitation. Due to anticipation of prolonged tube feeds, a gastrojejunostomy tube was placed.
On day 53 of her admission, she developed abdominal distension. One day later the abdominal radiograph and CT scan showed PI with minimal free intraperitoneal air but her clinical exam was not concerning for surgical intervention (Figure 2). The G-tube feeds were held for strict bowel rest. She then developed diarrhea and the stool was found to be positive for Norwalk virus and cytomegalovirus. The PI resolved on day 66. Jejunostomy-feeds were re-started and increased slowly, but increased abdominal distention was noted. On day 75 a repeat abdominal radiograph demonstrated PI again. The enteral feeds were held again and TPN was started. Enteral feeding was restarted and slowly increased without any complications. Mental status eventually improved and she slowly began to tolerate oral feeding. The choreoathetoid movements steadily decreased and she started to regain verbal function. She began ambulating with assistance via gait belt and was transferred to rehabilitation after 4 months of hospitalization. On outpatient follow up, she completed six monthly cyclophosphamide infusions and oral prednisolone was tapered gradually. She was started on mycophenolate mofetil as a maintenance disease-modifying agent. During the outpatient follow up over 18 months, she has been walking without any support, and her speech has continued to improve. She has resumed school and functions independently with no more abnormal movements.
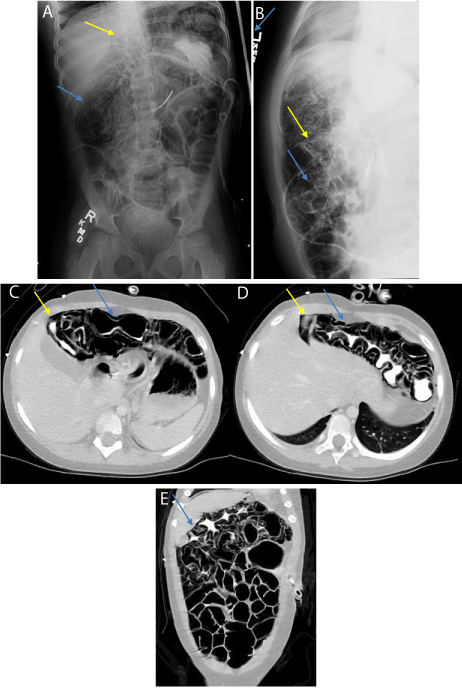
Figure 2: Seven-year-old girl was diagnosed with anti NMDA-R encephalitis.
On day 54 of hospitalization her supine abdominal radiograph (A) shows
pneumatosis coli in the region of the transverse colon (blue arrows) and a
minimal triangle of intraperitoneal free air (yellow arrow) in the right upper
quadrant. The cross fire lateral abdominal radiograph (B) shows minimal
intraperitoneal free air under abdominal wall (yellow arrow), pneumatosis
coli (blue arrow) and gaseous distention of bowel loops. Gastrojejunostomy
tube also shown. The abdominal CT scan (axial section C and D and coronal
section E) shows a small amount of pneumoperitoneum (yellow arrow) and
extensive pneumatosis (blue arrow) of the colon with gaseous distention
involving large and small bowel.
Discussion
Pneumatosis Intestinalis (PI) is defined as air in the bowel wall and is a radiographic finding and not a clinical diagnosis [5]. The etiology varies from benign conditions to fulminant gastrointestinal disease. The pathogenesis of PI is not very clear, but the process may involve loss of mucosal integrity, increased intraluminal pressure, and increased intraluminal gas production because of bacterial overgrowth [5]. The predisposing factors that have been associated with PI include trauma, inflammatory diseases, autoimmune diseases, pulmonary causes, celiac disease, leukemia, amyloidosis, organ and bone marrow transplant, congenital heart disease, motility disorders, short bowel syndrome, and drugs [10]. PI has been reported in patients with autoimmune disease such as systemic sclerosis, systemic lupus erythematosus, dermatomyositis, and Sjögren’s syndrome [11]. One case reported PI in a corticosteroid-dependent child [12].
To our knowledge, this is the first report of PI occurring in two patients with anti NMDA-R encephalitis.
Given the complex course of our two patients, it is difficult to know if the PI is due to a medication side-effect. Both patients received high dose steroids and rituximab, though both patients had abdominal distension early on in the course of the illness before being placed on those medications. Both cases also had infections which may have had a role in the development of PI ; case A had EBV infection before developing PI and case B had diarrhea 5 days after developing the PI with positive Norwalk virus and cytomegalovirus in the stool. Moreover, we speculate the role of the presence of NMDA receptors in the enteric nervous system which has been reported in the mouse model of colitis [13-15]. The role of peripheral NMDA glutamate receptors in the mechanism of GI motility is of special interest, but the exact mediatory pathways and concomitant neurotransmitter releases have not yet been elucidated clearly [16].
Our speculation may suggest a mechanism where anti-NMDA-R antibodies could lead to intestinal injury.
Children with NMDA receptor encephalitis are often very immunosuppressed. They are usually unable to verbally report abdominal discomfort or pain. Whether PI in this population is secondary to immunosuppression, drug effect, or a direct manifestation of impact auto antibodies will require further study. Until the role of these factors is better understood it is important that physicians caring for these patients especially pediatric intensive care team should have a heightened awareness of the risk of PI. In addition, it will worthwhile to develop a future studies to study the possible role of NDMA receptors in gastrointestinal system and PI.
References
- Dalmau J, Gleichman A, Hughes E, Rossi J, Peng X, Lai M, et al. Anti-NMDAreceptor encephalitis: case series and analysis of the effects of antibodies. The Lancet Neurology. 2008; 7: 1091-1098.
- Day G, High S, Cot B, Tang-Wai D. Anti-NMDA-Receptor Encephalitis: Case Report and Literature Review of an Under-Recognized Condition. J GEN INTERN MED. 2011; 26: 811-816.
- Titulaer M, McCracken L, Gabilondo I, Armangué T, Glaser C, Iizuka T et al. Treatment and prognostic factors for long-term outcome in patients with anti-NMDA receptor encephalitis: an observational cohort study. The Lancet Neurology. 2013; 12: 157-165.
- West K, Rescorla F, Grosfeld J, Vane D. Pneumatosis intestinalis in children beyond the neonatal period. Journal of Pediatric Surgery. 1989; 24: 818-822.
- Petrides C, Kyriakos N, Andreas I, Konstantinos P, Chrysanthos G, Athanasios P, et al. Pneumatosis Cystoides Intestinalis after Cetuximab Chemotherapy for Squamous Cell Carcinoma of Parotid Gland. Case Reports in Surgery. 2015; 1-3.
- Iwasaki M, Okajima K, Takano T, Misaki H. Case of portal venous gas and pneumatosis cystoides intestinalis occurring during chemotherapy for a castration-resistant prostate cancer. Hinyokika Kiyo. 2014; 60: 575-578.
- Ohtake S, Namura K, Fujikawa A, Sawada T, Ohta J, Moriyama M, et al. A case of pneumatosis cystoides intestinalis secondary to sunitinib treatment for renal cell carcinoma. Hinyokika Kiyo. 2014; 60: 75-78.
- Tanabe S, Shirakawa Y, Takehara Y, Maeda N, Katsube R, Ohara T, Sakurama K, et al. Successfully treated pneumatosis cystoides intestinalis with pneumoperitoneum onset in a patient administered alpha-glucosidase inhibitor. Acta Med Okayama. 2013; 67: 123-128.
- Akasaka H, Wajima N, Kimura A, Sakuraba S, Kubo N, Yamana D, et al. A case of pneumatosis cystoides intestinalis after neoadjuvant chemotherapy for esophageal cancer. 2014; 41: 2375-2377.
- Kurbegov A, Sondheimer J. Pneumatosis Intestinalis in Non-neonatal Pediatric Patients. PEDIATRICS. 2001; 108: 402-406.
- Sagara A, Kitagawa K, Furuichi K, Kitajima S, Toyama T, Okumura T, et al. Three cases of pneumatosis intestinalis presenting in autoimmune diseases. Mod Rheumatol. 2012; 22: 610-615.
- Cruz A, Naik-Mathuria B, Bisset G. Pneumatosis Intestinalis in a Corticosteroid-Dependent Child. The Journal of Emergency Medicine. 2015; 48: 607-608.
- Zhou Q, Nicholas Verne G. NMDA Receptors and Colitis: Basic Science and Clinical Implications. Rev Analg. 2008; 10: 33-43.
- Kirchgessner A. Glutamate in the enteric nervous system. Current Opinion in Pharmacology. 2001; 1: 591-596.
- McRoberts J, Coutinho S, Marvizón J, Grady E, Tognetto M, Sengupta J, et al. Role of peripheral N-Methyl-D-Aspartate (NMDA) receptors in visceral nociception in rats. Gastroenterology. 2001; 120: 1737-1748.
- Kaszaki J, Erces D, Varga G, Szabo A, Vecsei L, Boros M. Kynurenines and intestinal neurotransmission: the role of N-methyl-d-aspartate receptors. Journal of Neural Transmission. 2011; 119: 211-223.
