Abstract
Objective: This study was implemented to assess neuropsychological development status in children after surgical treatment of Congenital Heart Diseases (CHDs).
Methods: 89 children (median age 24 months, range 7-78 months) who received follow-up visit in Fuwai Hospital from September 2015 to March 2016 after surgical treatment of CHDs were recruited and 90 normal children (median age 41 months, range 16 - 68 months) without any CHDs were recruited as the control group. The patients were classified into simple CHDs group (RACHS-1 score ≤2) and complex CHDs group (RACHS-1 score ≥3). Neuropsychological development status was measured according to Pediatric-psychological mental test scale developed by Capital institute of pediatrics, Beijing and statistical analysis was compared.
Results: The results of neuropsychological development showed the normal children behaved better than the children with CHDs (p ≺0.05). The simple CHDs group had better distribution of development quotient than the complex CHDs group (p=0.032) and there was no difference between the normal control group and the simple CHDs group (p=0.420). Multivariate regression analysis indicated that younger age at cardiac surgery, lower preoperative Blood Urea Nitrogen (BUN), higher preoperative Creatinine (Cr) and prolonged duration of Cardiopulmonary Bypass (CPB) accounted for lower scores in the subscales of neuropsychological development (p ≺0.05).
Conclusions: Distinct neuropsychological deficits could be present especially in the children with complex CHDs following surgical treatment. Younger age at cardiac surgery, preoperative BUN, Cr and CPB duration could be used as good predictors for midterm neuropsychological development.
Keywords: Congenital Heart Diseases; Child; Neuropsychological Development; Pediatric Cardiac Surgery
Introduction
It is reported that Congenital Heart Disease (CHD) influences 7-9 per 1000 births in Europe, Asia, and North America, and approximately 25% require surgery in the first year of life. New surgical techniques and optimization in Cardiopulmonary Bypass (CPB), intensive care, and interventional cardiac catheterization have significantly lowered mortality rates for children and adolescents with various CHDs [1-3]. Improved survival of children with congenital heart disease has led to increasing focus on neurodevelopmental outcome, as close to half of the infants undergoing cardiac surgery are affected by neurodevelopmental disability [4].
It is also obvious that at the age of school entry, deficits in cognition, memory, language, reading, mathematics, visual-motor integration and executive function, which are more frequent in the neonates undergoing complex open heart surgery than in the general population [5]. However, just some scattered reports on neuropsychological development in children with CHDs after surgery treatment occurred and there is no recommendations evolved in the guidelines for pediatric cardiac surgery. More importantly, neuropsychological development in children with CHDs after surgery treatment has not been elaborated in China. This study was implemented in Fuwai Hospital to assess neuropsychological development status in these particular children after surgical treatment of CHDs and the results may provide evidence for further intervention. Perioperative factors which may affect neuropsychological development were investigated.
Materials and Methods
Subjects
From September 2015 to March 2016, 100 children (56 males, 44 females; range 7 to 78 months) who received follow-up visit in Fuwai Hospital after surgical treatment of CHDs were eligible to participate in neuropsychological examination. Exclusion criteria for enrollment were as follows: genetic abnormalities; extremely low gestational age newborns and premature infant; history of perinatal asphyxia and hyperbilirubinemia; history of central nervous system diseases, such as ischemic encephalopathy, encephalitis, meningitis and epilepsy, cerebral dysplasia; surgery not requiring CPB; preoperative cardiac arrest. 90 normal children (55 males, 35 females; range 16 to 68 months) were chosen from nursery schools or kindergartens at the same time period and the neuropsychological examination results of them were regarded as control. The normal children were free from congenital heart diseases and the exclusion criteria were the same as above. Informed consent was obtained from all parents and the examination was performed under parental supervision.
Data collection
The perioperative data of children with CHDs following surgical treatment were obtained from hospital records. Preoperative parameters included month age at surgery, body weight, gender, hemoglobin, platelet count, blood glucose, Blood Urea Nitrogen (BUN), serum albumin, serum Creatinine (Cr) and Left Ventricular Ejection Fraction (LVEF). Intraoperative perfusion data included CPB time, aortic cross-clamping time, nadir nasopharyngeal temperature and the lowest Central Venous Pressure (CVP) before CPB. Postoperative parameters were collected including mechanical ventilation time, postoperative nadir pulse Oxygen Saturation (SpO2), Postoperative Pediatric Intensive Care Unit (PICU) stay time and postoperative hospital stay time. All of the operations were performed with full-flow non-pulsatile extracorporeal circulation under mild (32 to 34°C) or moderate hypothermia (26 to 28°C) according to the surgeon’s preference and cardiac diagnosis.
Neurodevelopmental examination
The same trained and licensed examiner assessed all these children following cardiac surgical treatment and normal control children with Infants Neuropsychological Examination Table for children aged between 0 and 6 (hereunder referred to INET) developed by the Capital Pediatrics Research Institute, Beijing. It comprises five subscales: gross motor, fine motor, adaptability, language and social behavior. Mental age is calculated as one fifth of overall five subscales scores. Development Quotient (DQ) is originally defined as the ratio of mental age to chronological age multiplied by 100. Neuropsychological development was classified according to the score of DQ: supernormal, =130; excellent, 120-129; smart, 110-119; medium, 90-109; slow, 80-89; borderline mental retardation, 70-79; hypophrenia, ≺70.
Classification of CHDs surgeries
The Risk Adjustment for Congenital Heart Surgery (RACHS-1) method is commonly used among pediatric population clinically and the congenital heart surgeries are classified into 1 to 6 according to this method [6]. In this study, there was no surgery ranked equal or greater than 5, so the children received CHD surgeries were divided into simple CHDs group (RACHS-1 score less than or equal to 2) and complex CHDs group (RACHS-1 score equal or greater than 3).
Statistical analysis
Data analysis was performed using IBM SPSS Statistics version 22 (IBM SPSS Statistics, IBM Corporation, Chicago, IL). Continuous variables were presented as mean with Standard Deviation (SD) and categorical variables were presented as counts and percentages. Normally distributed data were compared with the Student t test. When a normal distribution for continuous data was not assumed, Kruskal-Wallis correlation was selected to analyze the correlation between different variables. ANOVA analysis was performed to analyze the differences of neuropsychological development among simple CHDs group, complex CHDs group and normal group. Relationships between INET subscales and perioperative parameters were evaluated by forward stepwise multivariable regression analysis. Probability values are two-sided with a p value less than 0.05 considered statistically significant.
Results
Characteristics of Children with CHDs
Of 100 children with CHDs after surgical treatment recruited in this study, 11 refused to cooperate with the examiner and did not fulfill the neuropsychological test. Finally 89 children with CHDs after surgical procedure in FuWai Hospital received examination between September 2015 and March 2016. According to classification of RACHS-1 method, 53 subjects were classified in the simple CHDs group and 36 were in the complex CHDs group. Demographic and clinical data of the simple CHDs group and the complex CHDs group are presented in Table 1.
Simple CHDs Group (n=53)
Complex CHDs Group (n=36)
P-value
Sex, male/female, n
34/19
17/19
0.116
Age at surgery, m, mean ± SD
24.03 ± 19.85
22.55 ± 21.05
0.738
Weight at surgery, kg, mean ± SD
11.24 ± 4.64
10.14 ± 4.51
0.272
Preoperative Hb, g/L, mean ± SD
123.23 ± 19.81
121.81 ± 15.59
0.719
Preoperative PLT, x10^9/L, mean ± SD
314.26 ± 96.84
286.33 ± 113.64
0.217
Preoperative BG, mmol/L, mean ± SD
4.38 ± 0.87
4.42 ± 0.78
0.812
Preoperative BUN, mmol/L, mean ± SD
4.01 ± 1.13
4.31 ± 1.62
0.354
Preoperative Cr, mmol/L, mean ± SD
30.10 ± 6.55
31.13 ± 9.96
0.556
Preoperative Alb, g/L, mean ± SD
44.39 ± 2.88
42.85 ± 3.64
0.035
Preoperative LVEF, %, mean ± SD
66.95 ± 5.30
63.99 ± 9.77
0.068
Intraoperative CPB, min, mean ± SD
72.81 ± 40.41
99.47 ± 62.46
0.016
Intraoperative aortic clamp, min, mean ± SD
43.24 ± 31.50
61.72 ± 41.63
0.021
Intraoperative nadir nasopharyngeal temperature, °C, mean ± SD
30.67 ± 2.29
30.33 ± 1.74
0.462
Intraoperative lowest CVP before CPB, mmHg, mean ± SD
3.06 ± 1.23
2.75 ± 1.25
0.255
Postoperative ventilation, h, mean ± SD
15.19 ± 12.87
19.34 ± 17.02
0.194
Postoperative lowest oxygen saturation,%, mean ± SD
97.57 ± 2.34
97.50 ± 3.24
0.911
Postoperative ICU stay, d, mean ± SD
40.81 ± 51.06
64.06 ± 74.48
0.084
Postoperative hospital stay, d, mean ± SD
12.29 ± 7.80
15.50 ± 7.32
0.103
Table 1: Demographic and clinical data of the simple CHDs group and the complex CHDs group.
Comparison on perioperative parameters
The complex CHDs group did not differ significantly in terms of month age at surgery from the simple CHDs group (22.55 ± 21.05 vs. 24.03 ± 19.85, p=0.738), suggesting that there was no direct relationship between the surgery timing and the severity of congenital heart diseases. Possibly, the surgery timing was more relevant with the progress of the diseases, the parental understanding of the diseases and first doctor’s medical advice. As expected, mean aortic cross clamp time and CPB time was longer in the complex CHDs group than those in the simple CHDs group (p ≺0.05), which means longer surgery time and more accurate hemodynamic management were necessary in the complex CHDs group. The complex CHDs group had lower preoperative serum albumin compared with the simple CHDs group (42.85 ± 3.64 vs. 44.39 ± 2.88, p=0.035), which indicated the children with complex CHDs might suffer from poorer nutrient reserves and more interstitial edema or water retention problems in vivo.
Comparison on INET subscales between CHDs and normal children
Compared with the normal control children, the subscale scores of children with CHDs decreased obviously. When it referred to the gross and fine motor domains, the children with CHDs scored lower than the normal children (p ≺ 0.05). Poorer coordination between hands and feet suggested cerebellar hypoplasia might exist in some children with CHDs. When it referred to the language domain, the children with CHDs lagged behind the normal children (p ≺0.001), mostly in imitation of pronunciation, coherence and comprehension, suggesting retardation in the development of auditory speech area and motor language area might exist in the children with CHDs. The children with CHDs got less scores than the normal children in the items of adaptation ability and social behavior (p ≺0.05), indicating that the children with CHDs could be with poor self-care ability. The children with CHDs differed significantly in terms of Development Quotient (DQ) from the normal children (90.67 ± 11.41 vs. 96.48 ± 7.54, p ≺ 0.001), suggesting that strengthen training and appropriate psychological intervention should be imposed on the children with CHDs. Outcomes for all the items’ scores in the test scale between the children with CHDs and the normal children were summarized in Table 2.
Subscales scores
Normal group (n=90)
CHD group (n=89)
P-value
Gross motor
40.30 ± 16.40
30.60 ± 20.22
0.001
Fine motor
39.44 ± 16.16
29.66 ± 20.44
< 0.001
Adaptability
40.08 ± 15.98
30.61 ± 19.90
0.001
Language
40.24 ± 16.35
30.32 ± 20.24
< 0.001
Social behavior
39.52 ± 15.35
30.96 ± 21.06
0.002
DQ
96.48 ± 7.54
90.67 ± 11.41
< 0.001
Table 2: Outcomes for all the subscales scores in the test scale between the children with CHDs and the normal children (mean ± SD).
Influence of surgery types on INET subscale scores
To make further analysis about the influence of CHD surgery types on the results of the INET, analysis of variance was used to compare the two CHDs groups and the normal group. Both of the two CHDs groups got less scores in the INET than the normal group (p ≺0.05). The complex CHDs group lagged behind the normal group (86.74 ± 11.93 vs. 96.48 ± 7.54, p ≺0.001) and the simple CHDs group (86.74 ± 11.93 vs. 93.34 ± 10.32, p=0.001) in DQ scores, suggesting that the more complex the CHD surgery types, the lower neuropsychological development, which need evaluating more rigorously. It could provide reasonable intervention and avoid further damage on the neuropsychological development by effective evaluation. There was no significant difference in the DQ scores between the simple CHDs group and the normal group (p=0.056), suggesting that the simple type CHD surgery could not influence the neuropsychological development dramatically. Outcomes for all the subscale scores in the test scale between the two CHD group and the normal group were summarized in Table 3.
Subscales scores
Simple CHDs group n=53
Complex CHDs group n=36
Normal group n=90
Gross motor
32.31 ± 20.31
28.08 ± 20.10
40.30 ± 16.40
Fine motor
31.17 ± 20.52
27.43 ± 20.40
39.44 ± 16.16
Adaptability
32.21 ± 19.85
28.26 ± 20.01
40.08 ± 15.98
Language
32.32 ± 20.59
27.38 ± 19.64
40.24 ± 16.35
Social behavior
32.68 ± 21.43
28.42 ± 20.53
39.52 ± 15.35
DQ
93.34 ± 10.32
86.74 ± 11.93
96.48 ± 7.54
Table 3: Outcomes for all the subscales scores between the two CHDs group and the normal group (mean ± SD).
Difference on DQ distribution between CHDs and normal children
The Kruskal-Wallis correlation was performed to assess the difference in DQ distribution among the two CHDs groups and the normal group. The proportion of children whose DQ were below the medium level in the complex CHDs group was higher than that in the normal group (50% vs. 18.9%, p ≺0.001) and the simple CHDs group (50% vs. 28.3%, p=0.032). The simple CHDs group did not differ in the DQ distribution from the normal group (p=0.420). The results of DQ distribution suggested that neuropsychological development in the children after simple type CHDs surgery treatment were close to that in the normal children. However, with the surgical complex increasing, the possibility of DQ retardation significantly increased. The distribution of DQ in different groups was shown in Figure 1.
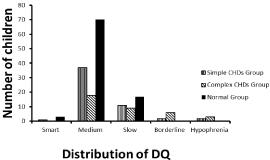
Figure 1: The distribution of DQ in different groups.
Risk factors on neuropsychological development impairment
Association between INET subscale scores and perioperative parameters were evaluated by forward stepwise multivariable regression (Table 4). Full-scale scores were correlated with the month age at surgery (p ≺0.05), suggesting that small month age at surgery could influence the midterm neuropsychological development. Relationship was found between preoperative BUN and the fullscale scores (p ≺0.05). However, the reason why increased BUN was correlated with high scores was indefinite. It might be related to preoperative nutritional reserve. Relationship was found between preoperative Cr and the full-scale scores (p ≺0.05), suggesting that preoperative renal function could increase water retention, which would further influence the central nervous system. Lower social behavior item score was associated with longer CPB time (p=0.041), suggesting that longer duration of non-pulsatile blood flow would not favor brain development.
Risk factors
Gross motor p-value
Fine motor p-value
Adaptability p-value
Language p-value
Social behavior p-value
RACHS-1 score
0.416
0.427
0.5
0.346
0.188
Age at surgery
< 0.001
< 0.001
< 0.001
< 0.001
< 0.001
Body weight
0.536
0.757
0.825
0.758
0.894
Hemoglobin
0.422
0.984
0.36
0.715
0.699
Platelet count
0.493
0.614
0.72
0.879
0.729
Blood glucose
0.394
0.24
0.694
0.556
0.856
BUN
0.006
0.001
0.001
0.001
0.004
Alb
0.337
0.43
0.347
0.216
0.804
Cr
0.04
0.015
0.005
0.004
0.016
LVEF
0.271
0.11
0.136
0.071
0.161
CPB time
0.087
0.087
0.072
0.061
0.041
Aortic cross-clamping time
0.127
0.186
0.15
0.11
0.645
Nadir nasopharyngeal temperature
0.089
0.323
0.335
0.332
0.768
CVP
0.849
0.732
0.693
0.722
0.558
Mechanical ventilation time
0.338
0.331
0.204
0.466
0.984
SpO2
0.231
0.287
0.199
0.372
0.117
PICU stay
0.568
0.752
0.818
0.435
0.075
Postoperative hospital stay
0.469
0.957
0.505
0.702
0.732
Table 4: Results of forward stepwise multivariable regression.
Discussion
Over the past two decades, with advances in surgical techniques and improvement in perioperative management, the survival of children with complex CHDs after surgery treatment has increased. Currently, perioperative survival in neonates undergoing cardiac surgery is ≻90% in most parts of the world. Meanwhile, more and more concern has been focused on the neuropsychological retardation of these children [4]. Some studies [7-10] have reported early neurodevelopmental outcomes following congenital heart surgery in neonates and infants prospectively. It could provide valuable anticipatory guidance for patients, families, teachers, and therapists by neurodevelopmental assessments and quality of life assessments [11]. With early identification of risk factors influencing neuropsychological development and treatment of developmental disorder and delays, children with CHDs may have opportunity to achieve their full potential, which will further help the children with CHDs develop better to adapt to the society [12]. It will also reduce the economic burden of these children’s family, which is of vital importance in China.
In 1998, Jenkins and 11-member national panel of pediatric cardiologists and cardiac surgeons created the Risk Adjustment for Congenital Heart Surgery (RACHS-1) method, to place surgical procedures into six risk categories. Cardiac surgeries during which more than one procedure are performed simultaneously are placed in the risk category of the highest risk procedure [13]. In this study, RACHS-1 method was used to classify different congenital heart surgery into different groups.
New burger [14] reported a high prevalence of neurodevelopmental impairment in patients with HLHS syndrome and other single right ventricle anomalies at age 14 months. Consistent with their reports, it was found with the RACHS-1 scores increasing, the DQ scores decreased significantly in this observation. Guerra et al. [15] used Bayley Scale to test 93 children born within 6 weeks who received complex CHD surgeries and reported that these children scored lower in the scale than the normal population. Consistent with Guerra, it was found that the younger the children received CHD surgery, the lower scores in the INET in this study. Although the scores in the INET elevated with the increase of age, which was in accordance with the rule of intelligence development of the children, the influence of the complexity of CHD surgery on the neuropsychological development should not be neglected which was demonstrated in this study. Normal children without CHDs were recruited in this study to avoid the error of measurements of Neuropsychological Examination. The distribution of DQ in normal children verified the validity of this INET scores.
Previous studies [16-18] reported that postoperative mixed venous oxygen saturation, days in the intensive care unit, length of stay in hospital and complications such as epilepsy, hypotension, arrhythmia or sepsis were risk factors associated with neurologic, motor and developmental deficits in children after CHD surgeries. In this study, multiple stepwise regression analysis identified preoperative BUN, Cr and CPB time associated with INET scores. With the increase of preoperative Cr and CPB time, the scores decreased dramatically. Conversely, with the decrease of preoperative BUN, the scores increased significantly. However, the mechanism how preoperative BUN affects the scores was uncertain. After evaluation on 340 pediatric patients with chronic kidney diseases, Mendley et al. [19] found that 35% had poor performance on at least one test of executive function. Keunen et al. [20] reported that adequate protein intake and energy supply could protect brain neurons with immunemodulatory and/or anti-inflammatory effects and improve brain development in preterm infants with white matter injury. It will be the next step to explore whether protein adjustment has influence on neuropsychological development.
Schaefer et al. [21] examined neurodevelopment, psychological adjustment, and health-related quality of life in fifty-nine adolescents after bypass surgery for Congenital Heart Disease (CHD) during early childhood. The results indicated that these adolescents manifested persistent cognitive and motor impairments. Similarly, Razzaghi et al. [22] analyzed 420 children with CHDs and 180048 children without CHDs, found that children with CHDs were more likely accompanied with autism spectrum disorder (crude OR, 4.6; 95% CI, 1.9-11.0) or intellectual disability (crude OR, 9.1; 95% CI, 5.4-15.4). In this study, children with CHDs received surgery at a relatively younger month-age (23.40 ± 20.24), despite the children in the complex CHDs group showed a certain degree of anxiety in the process of evaluating adaptability and social behavior, but whether the children with CHDs would present with autism spectrum disorder or depression still need long-term follow-up and supervision.
Limitation of this Study
There were several limitations in this study. The study was a single-center small-sample study in China. Another limitation is the lack of information about the preoperative INET scores of the CHDs children, socioeconomic status and parental education. Brain MRIs were not performed in most subjects because of demand for narcotic. In addition, the long-term implications of these neurodevelopmental concerns at the age of school entry remain to determine. However, this study highlighted the influence of congenital heart surgeries on the midterm neuropsychological development.
Conclusion
Distinct neuropsychological deficits could be present especially in the children with complex CHDs following surgical treatment. Younger age at cardiac surgery, preoperative BUN, Cr and CPB duration could be used as good predictors for midterm neuropsychological development. The finding stressed the importance of routine follow-up assessment in specialized centers for children with complex CHDs who underwent cardiac surgery to provide early appropriate therapeutic intervention and parental guidance.
Acknowledgements: This work is supported by National Natural Science Foundation of China (81170233) and Scientific Research Foundation for the Returned Overseas Chinese Scholars, Ministry of Education of China (2013-LH01).
Contributors’ Statement
Dr Guan, Dr Hei and Prof Long conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript.
Dr Lin, Liang, Wang, Wei and Dr Yao designed the data collection instruments, collected data, carried out the initial analyses, and reviewed and revised the manuscript.
Dr Jiang reviewed and revised the manuscript.
Dr Li and Dr Zhang conceptualized and designed the study, coordinated and supervised data collection, and critically reviewed the manuscript for important intellectual content.
References
- Andropoulos DB, Ahmad HB, Haq T, Brady K, Stayer SA, Meador MR, et al. The association between brain injury, perioperative anesthetic exposure, and 12-month neurodevelopmental outcomes after neonatal cardiac surgery: a retrospective cohort study. Paediatr Anaesth. 2014; 24: 266-274.
- Asakai H, Stojanovski B, Galati JC, Zannino D, Cardamone M, Hutchinson D, et al. Risk Factors for Peri-Procedural Arterial Ischaemic Stroke in Children with Cardiac Disease. Pediatr Cardiol. 2017.
- Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Borden WB, et al. Heart disease and stroke statistics-2013 update: a report from the American Heart Association. Circulation. 2013; 127: 143-152.
- Snookes SH, Gunn JK, Eldridge BJ, Donath SM, Hunt RW, Galea MP, et al. A systematic review of motor and cognitive outcomes after early surgery for congenital heart disease. Pediatrics. 2010; 125: e818-e827.
- Gaynor JW, Gerdes M, Nord AS, Bernbaum J, Zackai E, Wernovsky G, et al. Is cardiac diagnosis a predictor of neurodevelopmental outcome after cardiac surgery in infancy?. J Thorac Cardiovasc Surg. 2010; 140: 1230-1237.
- Nakayama Y, Shibasaki M, Shime N, Nakajima Y, Mizobe T, Sawa T. The RACHS-1 risk category can be a predictor of perioperative recovery in Asian pediatric cardiac surgery patients. J Anesth. 2013; 27: 850-854.
- Andropoulos DB, Easley RB, Brady K, Mckenzie ED, Heible JS, Dickerson HA, et al. Neurodevelopmental outcomes after regional cerebral perfusion with neuromonitoring for neonatal aortic arch reconstruction. Ann Thorac Surg. 2013; 95: 648-654.
- Tabbutt S, Gaynor JW, Newburger JW. Neurodevelopmental outcomes after congenital heart surgery and strategies for improvement. Curr Opin Cardiol. 2012; 27: 82-91.
- Gaynor JW, Wernovsky G, Jarvik GP, Bernbaum J, Gerdes M, Zackai E, et al. Patient characteristics are important determinants of neurodevelopmental outcome at one year of age after neonatal and infant cardiac surgery. J Thorac Cardiovasc Surg. 2007; 133: 1344-1353.
- Tabbutt S, Nord AS, Jarvik GP, Bernbaum J, Wernovsky G, Gerdes M, et al. Neurodevelopmental outcomes after staged palliation for hypoplastic left heart syndrome. Pediatrics. 2008; 121: 476-483.
- Tabbutt S. How to improve neurodevelopmental and quality of life outcomes following early surgery for congenital heart disease? Dev Med Child Neurol. 2013; 55: 1072-1073.
- Marino BS. New concepts in predicting, evaluating, and managing neurodevelopmental outcomes in children with congenital heart disease. Curr Opin Pediatr. 2013; 25: 574-584.
- Jenkins KJ. Risk adjustment for congenital heart surgery: the RACHS-1 method. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu. 2004; 7: 180-184.
- Newburger JW, Sleeper LA, Bellinger DC, Goldberg CS, Tabbutt S, Lu M, et al. Early developmental outcome in children with hypoplastic left heart syndrome and related anomalies: the single ventricle reconstruction trial. Circulation. 2012; 125: 2081-2091.
- Guerra GG, Robertson CM, Alton GY, Joffe AR, Cave DA, Dinu IA, et al. Neurodevelopmental outcome following exposure to sedative and analgesic drugs for complex cardiac surgery in infancy. Paediatr Anaesth. 2011; 21: 932-941.
- Newburger JW, Wypij D, Bellinger DC, du Plessis AJ, Kuban KC, Rappaport LA, et al. Length of stay after infant heart surgery is related to cognitive outcome at age 8 years. J Pediatr. 2003; 143: 67-73.
- Limperopoulos C, Majnemer A, Shevell MI, Rohlicek C, Rosenblatt B, Tchervenkov C, et al. Predictors of developmental disabilities after open heart surgery in young children with congenital heart defects. J Pediatr. 2002; 141: 51-58.
- Martinez-Biarge M, Jowett VC, Cowan FM, Wusthoff CJ. Neurodevelopmental outcome in children with congenital heart disease. Semin Fetal Neonatal Med. 2013; 18: 279-285.
- Mendley SR, Matheson MB, Shinnar S, Lande M, Gerson AC, Butler R, et al. Duration of chronic kidney disease reduces attention and executive function in pediatric patients. Kidney Int. 2015; 87: 800-806.
- Keunen K, van Elburg RM, van Bel F, Benders MJ. Impact of nutrition on brain development and its neuroprotective implications following preterm birth. Pediatr Res. 2015; 77: 148-155.
- Schaefer C, von Rhein M, Knirsch W, Huber R, Caflisch J, Landolt MA, et al. Neurodevelopmental outcome, psychological adjustment, and quality of life in adolescents with congenital heart disease. Dev Med Child Neurol. 2013; 55: 1143-1149.
- Razzaghi H, Oster M, Reefhuis J. Long-term outcomes in children with congenital heart disease: National Health Interview Survey. J Pediatr. 2015; 166: 119-124.
