
Case Report
Austin Crit Care J. 2021; 8(1): 1033.
The Use Extracorporeal Membrane Oxygenation Therapy in a Severe Blunt Chest Trauma with a Main Tracheal Injury
Zhang J¹, Han H¹, Liu H¹, Li Y¹, Wu M² and Chen X¹*
1Department of Critical Care Medicine, Qilu Hospital of Shandong University, China
2Department of Thoracic Surgery, Qilu Hospital of Shandong University, China
*Corresponding author: Xiaomei Chen, Department of Critical Care Medicine, Qilu Hospital of Shandong University, Wenhuaxi Road 107, Jinan 250012, China
Received: February 16, 2021; Accepted: February 24, 2021; Published: March 03, 2021
Abstract
Major tracheobronchial trauma by blunt chest trauma is high mortality rates worldwide. The use conventional mechanical ventilation in a tension pneumothorax patient by major tracheobronchial trauma has been ineffective with barotrauma. However, the application of Veno-Venous Extracorporeal Membrane Oxygenation (VV-ECMO) in trauma patients has been controversial, but VV-ECMO plays a crucial role when conventional management has failed. VV-ECMO provides adequate tissue oxygenation and an opportunity for recovery. Neither ECMO-associated bleeding nor clotting of the extracorporeal circuit is an upmost for trauma patients. We report a case of previously healthy 16-year-old man with left main bronchial rupture after vehicular accident, who had progressive dyspnea and left tension pneumothorax. After the chest tube drainage, double-lumen endotracheal intubation and mechanical ventilation initiation, severe respiratory distress kept on deterioration. On VV-ECMO transfer to our hospital, we performed emergency thoracotomy and identified the rupture of the left main bronchus. After operation, the patient’s condition improved. VV-ECMO and mechanical ventilation were stopped on days 8 and 9, respectively. He was discharged without complications from the ICU on day 20.
Keywords: Veno-venous extracorporeal membrane oxygenation; Blunt trauma; Major tracheobronchial rupture
Introduction
Major Tracheobronchial Trauma (MTT) by blunt chest trauma is extremely rare (1-3 %) and high mortality rates worldwide, especially in young adults. A rapid increase in tracheobronchial pressure can lead to blowout perforation of the trachea, which can lead asphyxia. Most of the MTT patients die before arriving at the hospital. It remains a challenge for trauma critical care. The early diagnosis of the highly lethal injury is crucial for survival [1]. Generally, initial management includes airway established, decompression of pneumothorax, and hemorrhage control. Additionally, support with Extracorporeal Membrane Oxygenation (ECMO) as a temporary rescue modality offers potential benefit survive in trauma patients [2-4]. ECMO is able to provide respiratory and cardiovascular support for patients. However, systemic heparinization is a key issue for ECMO as it can induce intracranial and surgical site bleeding with heparinization. We present a successful case of a teenager with left bronchi rupture due to severe crush injury, who received ECMO as supportive therapy on perioperative period, and discuss the heparin-free ECMO application.
Case Presentation
A 16-year-old male suffered a blunt thoracic trauma after being crashed into a tree while riding his electric bicycle. He was rushed to local emergency department. Physical examination revealed a blood pressure of 110/60 mmHg with a heart rate of 128 beats/min, a spontaneous respiration rate of 30 breaths/min and a pulse oxygen saturation (SpO2) of 80%. Breathing was inaudible by auscultation in the left lung. Whole body Computed Tomography (CT) was performed without showing any intracranial hemorrhages or definitive abdominal organ injuries. The chest CT scan showed leftside tension pneumothorax. Prompt left closed thoracic drainage was performed with a rush of air. Simultaneously, fluid was infused and immobilization of the chest wall was done. Despite above done, his SpO2 level decreased to 73%. Therefore, single-lumen endotracheal intubation followed by double-lumen endotracheal intubation was inserted and Mechanical Ventilation (MV) was started. However, persistent large-volume air leaks and poor tidal volumes still existed. Due to the technical restriction for further surgery treatment in the local hospital, our hospital ECMO team were sent to perform Veno- Venous (VV) ECMO. Catheters were inserted into the left jugular vein (17-Fr cannula for inflow, the tip nearly reached right atrium) and right femoral vein (21-Fr cannula for outflow, the tip located at inferior vena cava). After we established VV-ECMO with heparin (Maquet, ROTAFLOW Console, Germany) at 4000 rpm on pump flow, 5L/min on gas flow and FdO2 on 0.8, the patient’s SpO2 quickly rising at 100% and his respiratory distress was alleviated significantly, allowing about 146 km transport to our hospital. The injury severity score was 17 and the probability of survival was 0.63.
Flexible bronchoscopy and second CT (Figure 1) were performed immediately in our hospital, but did not enable us to accurately visualize the tracheobronchial lesions. After multidisciplinary discussion and agreement, patient was taken to the operating room for thoracotomy as well under general anesthesia and ECMO. Rupture length of 3.5 cm and two third of the circumference in left side of main bronchus were detected. Additionally, multiple longitudinal diffuse fissures with inflammatory edema on the 6cm length between left main bronchus to segment of bronchi were also identified (Figure 2). Considering several failure attempts to repair the rupture and probably inevitable bronchopleural fistula, the decision was to perform the whole left pneumonectomy. The operating time was lasting for 3 hours with a blood loss volume of 100 ml. After change to a single lumen tube, the patient was readmitted to the ICU. When the initiation of ECMO with standard heparin, heparin was micro-pump injected (125-750 u/hour), and Activated Clotting Time (ACT) was monitored in every 2 hours. ACT was remained between 160s to 180s. Meanwhile, arterial and venous blood gas were tested every 6 hours. Starting at 6 hours before the surgery, heparin was stopped on ECMO to ensure less bleeding until the end of the surgery. Heparin-free ECMO was remained 7.5 hours without increasing the pump flow.
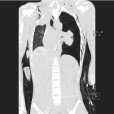
Figure 1: Chest CT showed left tension pneumothorax, a suggestion of a
rupture of the left main bronchus can be seen.
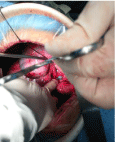
Figure 2: Show the rupture length of 3.5 cm and 2/3 of the circumference in
left side of main bronchus during surgery.
Subsequently, ECMO weaning was initiated because all of his underlying diseases were removed and improvement of lung function on his spontaneous breathing. VV-ECMO was stopped on day 8 without any ECMO-related complications. MV was liberated on day 9 with extubation. The patient was discharged in favorable condition on day 20.
Discussion
Despite of kinds of MV technique and the improvement knowledge of the mode of ventilation parameters, patients with tracheal ruptures are still unable to benefit from the equipment. ECMO has been proved to be a rescue, aggressive and successful therapy when conventional methods are ineffective [5]. We described the case experienced a left main tracheal rupture induced by severe blunt trauma patient using ECMO.
Diagnosis of tracheal ruptures is based on a high clinical suspicious. Ventilating the patient with persistently low tidal volumes and large-volume air leaks despite adequate chest drainage are highly suggestive of a large tracheobronchial tear. Diagnostic confirmation is usually made by bronchoscopy or with CT scans, which will reveal the size and site of the tracheal disruption. Unfortunately, both techniques did not work in our patient. In cases of clinical instability, thoracotomy is necessary as both a lifesaving procedure and diagnostic method under direct vision even if the other diagnosis has not previously been confirmed.
Treatment of tracheal ruptures ranges from nonoperative management to full reconstruction. General management recommendations for all patients with a tracheal rupture include airway humidification, broad spectrum antibiotics to prevent mediastinitis, and cough suppression to minimize injury. Traditionally, the treatment of choice was urgent surgical repair depends on the location and length of the tear. When laceration of the bronchus involving more than one third of the circumference needs surgical repair, it tends to cause severe stenosis with repeated lung infections and collapse. Severe cases may require pneumonectomy. Nevertheless, management must be individualized to the particular patient and the consultant surgeon’s preference. Moreover, it may be considered transferring these rare cases of bronchial rupture to an experienced thoracic and trauma surgery center. Our severe case was undergone the pneumonectomy based on the estimation and capability of the surgeon. Even though no strong recommendations regarding type and timing of surgery can be made based on the available literature, many successful cases showed that patients were benefit from surgery [6].
Conventional mechanical ventilation is the mainstay of treatment for severe respiratory failure associated with trauma. However, when extensive lung injury is present, this technique may not be sufficient to prevent hypoxia, and furthermore, may exacerbate pulmonary damage by barotrauma. ECMO provides oxygenation of blood and removal of carbon dioxide via an extracorporeal circuit. It is a technique that provide “lung rest” by permitting reduced ventilator settings and limiting further lung damage (barotrauma) while maintaining tissue perfusion and oxygenation [7,8]. If optimal chest drainage and ventilation fail to restore a stable condition for MTT, ECMO can be indicated urgently before surgery. It can also permit surgeon to facilitate surgical repair and postoperative management (particularly ventilation). Our case suggested that ECMO was both feasible and safe in a carefully selected trauma patient. Although our patient has not brain injury evidence, more findings do not support neurological injury as an absolute contraindication to ECMO [9].
The choice for the type of ECMO approach (ie, Veno-Arterial (VA) mode, or VV mode) depends on the involvement of the cardiac system as well as profound shock or unstable haemodynamics. For haemodynamically instability patients, the use of VA ECMO was recommended [10]. This reduces venous bleeding by lowering central blood pressure, but risks major is air embolism in cases involving large venous tears. With VVECMO, the blood flow is easily maintained. This technique offers theoretical benefits by allowing native pulmonary flow (increasing the pulmonary alveolar oxygen content) and easier weaning. Either VV ECMO or VA ECMO type was selected, no differences was in several complication factors. However, there was a trend toward more blood transfusion in the VA ECMO type [3].
Trauma-induced coagulopathy is often present in these patients with significant morbidity and mortality rates [11,12]. In the past, hemorrhage is a seriously issue in trauma patients, and bleeding complications are often seen in trauma patients treated with ECMO [13,14]. Regarding to the anti-coagulation measures balance between the preventing thrombosis from occurring in the device and causing severe organ bleeding complications, appropriate anti-coagulation measures should be applied. Specialized patient management strategies, including initiating heparin-free ECMO and titrating the ACT and APTT goals based on bleeding risk, have been applied in an effort to decrease bleeding risk in post-trauma ECMO patients. Nevertheless, with the further development of technique including centrifugal pumps and heparin-coated circuits, ECMO can reduced the amount of additional heparin needed. Neither ECMO-associated bleeding nor clotting of the extracorporeal circuit occurred in three survived patients [15]. More successful heparin-free cases reported among polytrauma patients with coexisting organ hemorrhage [14,15]. Our patient was received non-heparin ECMO as bridge during the operation for 6 hours. This case demonstrates the successful use of ECMO in the management of acute tracheal injury due to trauma.
ECMO support requires a highly trained and dedicated team with a well-equipped intensive care unit. An important consideration prior to referral is, therefore, that critically ill patients have to be transported long distances for tertiary transfer. In our center, ECMO is available at any time within 30 min, and the ECMO team (mainly intensivist) is called as soon as the medical rescue team is sent to the scene of the emergency.
Capsule Summary
What is already known
A main tracheal ruptured is a highly lethal injury.
What is new in the current study
ECMO as a temporary rescue modality offers potential benefit survive in a main tracheal ruptured trauma patient. The utilization of the ECMO devices was safe and effective for facilitated surgery process. Heparin-free ECMO can be a safe and feasible rescue method under more careful observation during surgery.
References
- Mussi A, Ambrogi MC, Ribechini A, Lucchi M, Menoni F, Angeletti CA. Acute major airway injuries: clinical features and management. Eur J Cardiothorac Surg. 2001; 20: 46-51.
- Ried M, Bein T, Philipp A, Muller T, Graf B, Schmid C, et al. Extracorporeal lung support in trauma patients with severe chest injury and acute lung failure: a 10-year institutional experience. Crit Care. 2013; 17: R110.
- Wu SC, Chen WT, Lin HH, Fu CY, Wang YC, Lo HC, et al. Use of extracorporeal membrane oxygenation in severe traumatic lung injury with respiratory failure. Am J Emerg Med. 2015; 33: 658-662.
- Cordell-Smith JA, Roberts N, Peek GJ, Firmin RK. Traumatic lung injury treated by Extracorporeal Membrane Oxygenation (ECMO). Injury. 2006; 37: 29-32.
- Yen TS, Liau CC, Chen YS, Chao A. Extracorporeal membrane oxygenation resuscitation for traumatic brain injury after decompressive craniotomy. Clin Neurol Neurosurg. 2008; 110: 295-297.
- Ballouhey Q, Fesseau R, Benouaich V, Leobon B. Benefits of extracorporeal membrane oxygenation for major blunt tracheobronchial trauma in the paediatric age group. Eur J Cardiothorac Surg. 2013; 43: 864-865.
- Wang FY, Fang B, Yu ZH, Shao JS, Wen WB, Zhou LX. Severe thoracic trauma caused left pneumonectomy complicated by right traumatic wet lung, reversed by extracorporeal membrane oxygenation support-a case report. BMC Pulm Med. 2019; 19: 30.
- Bosarge PL, Raff LA, McGwin G, Carroll SL, Bellot S, Diaz-Guzman E, et al. Early initiation of extracorporeal membrane oxygenation improves survival in adult trauma patients with severe adult respiratory distress syndrome. J Trauma Acute Care Surg. 2016; 81: 236-243.
- Kruit N, Prusak M, Miller M, Barrett N, Richardson C, Vuylsteke A. Assessment of safety and bleeding risk in the use of extracorporeal membrane oxygenation for multitrauma patients: A multicenter review. J Trauma Acute Care Surg. 2019; 86: 967-973.
- Huang YK, Liu KS, Lu MS, Wu MY, Tsai FC, Lin PJ. Extracorporeal life support in post-traumatic respiratory distress patients. Resuscitation. 2009; 80: 535-539.
- Chang R, Cardenas JC, Wade CE, Holcomb JB. Advances in the understanding of trauma-induced coagulopathy. Blood. 2016; 128: 1043- 1049.
- Dobson GP, Letson HL, Sharma R, Sheppard FR, Cap AP. Mechanisms of early trauma-induced coagulopathy: The clot thickens or not? J Trauma Acute Care Surg. 2015; 79: 301-309.
- Wu MY, Lin PJ, Tseng YH, Kao KC, Hsiao HL, Huang CC. Venovenous extracorporeal life support for posttraumatic respiratory distress syndrome in adults: the risk of major hemorrhages. Scand J Trauma Resusc Emerg Med. 2014; 22: 56.
- Wen PH, Chan WH, Chen YC, Chen YL, Chan CP, Lin PY. Non-heparinized ECMO serves a rescue method in a multitrauma patient combining pulmonary contusion and nonoperative internal bleeding: a case report and literature review. World J Emerg Surg. 2015; 10: 15.
- Muellenbach RM, Kredel M, Kunze E, Kranke P, Kuestermann J, Brack A, et al. Prolonged heparin-free extracorporeal membrane oxygenation in multiple injured acute respiratory distress syndrome patients with traumatic brain injury. J Trauma Acute Care Surg. 2012; 72: 1444-1447.