
Case Presentation
Austin J Dent. 2019; 6(1): 1125.
A Rare Case of Odontogenic Keratocyst Crossing Lower Midline
Krishna R¹*, Johny J², Punathil S³ and Khan NM²
¹Dental House Surgeon, Department of Oral Medicine and Radiology, Sree Anjaneya Institute of Dental Sciences, Kerala, India
²Department of Oral Medicine and Radiology, Sree Anjaneya Institute of Dental Sciences, Kerala, India
³Department of Paediatric and Preventive Dentistry, Sree Anjaneya Institute of Dental Science, Kerala, India
*Corresponding author: Rani Krishna, Dental House Surgeon, Department of Oral Medicine and Radiology, Sree Anjaneya Institute of Dental Sciences, Kerala, India
Received: December 12, 2018; Accepted: January 10, 2019; Published: January 17, 2019
Abstract
Odontogenic Keratocyst (OKC) is a common developmental odontogenic cyst affecting the maxillofacial region that arises from the dental lamina. The OKC is distinctive among jaw cyst given its tendency toward recurrence and aggressive clinical behaviour. The diagnostic approach is based on a combined analysis of the medical history, the clinical and radiographic appearance. The diagnosis may be confirmed by the anatomical pathology report. Finally treatment consist of surgical excision and follow up is characterised by high recurrence rate. This article presents a case of OKC in the anterior mandible and a review of diagnostic aids and different treatment modalities.
Keywords: Anterior Mandible; Enucleation; Odontogenic Keratocyst
Introduction
The odontogenic keratocyst (OKC) was first used by philipsen in 1956 [1]. It is one of the most aggressive odontogenic cysts of the oral cavity. OKC is known for its rapid growth and its tendency to invade the adjacent tissues including bone [2,3]. Odontogenic Keratocyst arise in the jaws arise from cell rest of dental lamina and are usually seen during the second to fourth decade of life with a slight male predilection. The majority of the patients are in the age ranges of 20- 29 and 40-59 years [4], but cases ranging from 5-80 years have been reported [5]. A total of 70% to 80% keratocysts are most commonly found in the lower jaw in the angle between jaw and mandibular branch and in the maxilla in the area of third molar [1-3]. Growth is chiefly in anteroposterior dimension, and the lesions may attain remarkable size without significantly deforming the jaw skeleton. The particular tendency to rapid growth is due to the higher activity of the epithelial cells of the cyst lining, stimulating osteolytic activity of the prostaglandin substances in the cell population of the cyst lining and the higher accumulation of the hyperkeratotic scales in the lumen of the cyst, resulting in greater difference in hydrostatic pressure
Case Presentation
A 12 year old female patient reported to the department of oral medicine and radiology with a chief complaint of swelling on the left chin noticed since last two months which was initially small in size and gradually increased to the present size, there was no period of remission or exacerbation. And not associated with pain or any other symptoms. The medical and dental history were non-contributory. On extra oral examination Figure 1, a diffuse swelling seen on the left side of the chin with no apparent colour change on the skin surrounding and the swelling was bony hard and non-tender on palpation.

Figure 1: Extraoral View: Showing a diffuse swelling seen on the left side
of chin.
On intraoral examination Figure 2a, 2b on inspection, a solitary oval shaped swelling was noticed on the labial vestibule which is extending from the distal aspect of 33 to the distal aspect of 41. The swelling was found to be approximately 7cm X 1cm in size with well-defined margins and no change in the surrounding mucosa. Obliteration of labial vestibule was seen. Also 34, 35, 36 and 37 were found to be lingually inclined and 34 and 35 have grade 1 mobility. On palpation, all the inspectory findings were confirmed and the swelling was found to be non-tender and bony hard in consistency with area of soft fluctuancy. On electric pulp testing 33, 32,31,41,42 shows early response. Based on the history and clinical examination, a provisional diagnosis of Central Giant Cell Granuloma was considered as it is more commonly seen in younger age group, and affects mandibular anterior region, crossing midline and Odontogenic Keratocyst was given as first differential Diagnosis.
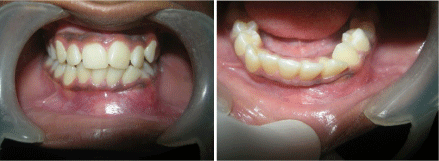
Figure 2: Intraoral View: Showing a solitary oval shaped swelling
was noticed on the labial vestibule which is extending from the distal aspect
of 33 to the distal aspect of 41.
Intra Oral Peri Apical Radiograph Figure 3 revealed a welldefined radiolucency extending from 34 to 42 with sclerotic border. Panoramic radiograph Figure 4 revealed a solitary well defined oval shaped radiolucency with sclerotic border extending from 34 to 42 measuring 8cm X 3cm in size also shows displacement of root apex of 32 and 33. Lateral Mandibular occlusal radiograph Figure 5 revealed bicortical plate expansion from 33 to 42 and also shows scalloping between 32 and 33. Root Canal treatment was done on the affected region’s teeth i.e. 35, 34, 33,32,31,41 and 42 followed by cyst enucleation, and chemical cauterization using Carnoy’s solution was done, the biopsy specimen was sent for histopathologic examination, which revealed corrugated surface with parakeratinization and palisaded basal layer suggestive of Odontogenic Keratocyst (Figure 6). Patient was kept on follow up and recalled after 1 month and panoramic radiograph Figure 7 revealed bone formation in the previously affected region.
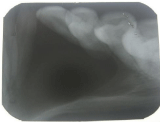
Figure 3: Intra Oral Periapical Radiograph: Revealed a well-defined
radiolucency extending from 34 to 42 with sclerotic border.
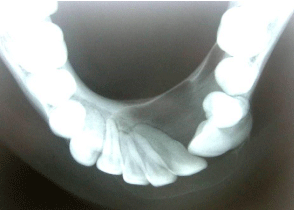
Figure 4: Lateral Mandibular Occlusal Radiograph: Revealed bicortical
plate expansion from 33 to 42 and also shows scalloping between 32 and 33.
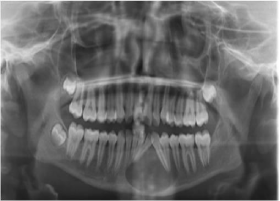
Figure 5: OPG: Revealed a solitary well defined oval shaped radiolucency
with sclerotic border extending from 34 to 42 measuring 8cm X 3cm in size
also shows displacement of root apex of 32 and 33.
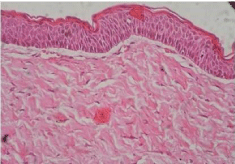
Figure 6: Histopathology (40X): Which revealed corrugated surface with
parakeratinization and palisaded basal layer.
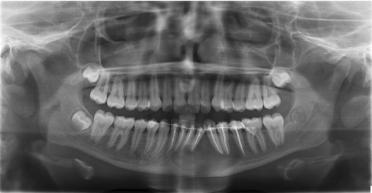
Figure 7: Postoperative View: Revealed bone formation in the previously
affected region.
Discussion
OKC is a common developmental odontogenic keratocyst, and its biological behaviour is similar to a benign neoplasm [6]. Therefore, in the latest WHO classification of odontogenic tumors in 2005, it has been given the term keratocystic odontogenic tumor [7]. OKC are generally thought to be derived from either the epithelial remnants of the tooth germ or the basal cell layer of the surface epithelium [8,9].
OKC may be found in any age, with peak the prevalence between the age 10 and 40 years [9]. The mandible is involved in 60% to 80% of cases with a marked tendancy to occur in the posterior body and ascending ramus [10]. However in this case, the lesion was present in anterior mandible.
Radiological examination of most of the cases reveals a welldefined radiolucency with thin corticated margins with the majority of these being unilocular, but larger lesions present as multilocular lesions [7,4].
The OKC shows highly distinct histopathological features with uniform cyst lining, wavy parakeratin formation, hyperchromatic, and palisaded basal cells and a flat interface between the epithelium and underlying connective tissue wall. When the cyst is inflamed, these classic microscopic features are often completely lost, which can lead to an inappropriate diagnosis. NBCCS (also known as Gorlin-Goltz syndrome or jaw cyst-basal cell nevus-bifid rib syndrome) should be considered when a patient presents with multiple OKCs. NBCCS is an inherited genetic condition which occurs due to mutation of the PTCH1 gene. Palmar and plantar pits, bifid ribs, multiple basal cell cancers of the skin and calcified falx cerebri are the other findings of this syndrome. The lesions found with NBCCS are comparitively less aggressive than traditional basal cell epithelioma, because of this the designation “nevoid,” or having biologic behaviour more similar to a nevus was mentioned.
Conclusion
This case has defined that, the clinical impression and radiographic picture are not distinctive enough to be used as the only standard for rendering a diagnosis of any cyst occurring on the jaws. We can’t confine to ourselves associated symptoms such as age, sex, location and shape of the lesion. Due to high recurrence rate and aggressive behaviour of OKCs all the tissues removed, should be submitted for histopathologic evaluation and a definitive diagnosis.
References
- Philipsen HP. Om keratocysyts (kolesteatomer) Kaeberne Tandlaegebladet.1956; 60: 963-980.
- Toller P. Origin and growth of cysts of the jaws. Ann R coll Surg Engl. 1967; 40: 306-336.
- Ba K , Li X, Wang H, Liu Y, Zheng G, Yang Z , et al. Correlation between imaging features and epithelial cell proliferation in keratocystic odontogenic tumor. dentomaxillofac Radio. 2010; 39: 368-374.
- Philipsen HP. Keratocystic odontogenic Tumor. In: BarnesL, Eveson JW, Reichart P, Sidransky D, editors. World Health Organization Classification of Tumors: Pathology and Genetics of Head and Neck Tumors. Lyon: IARC Press. 2005: 306-307.
- Gonzalez-Alva P, Tanaka A, Oku Y, Yoshizawa D, Itoh S, Sakashita H, et al. Keratocystic Odontogenic Tumor: A retrospective study of 183 cases. J Oral Sci. 2008; 50: 205-212.
- Bhargava D, Deshpande A, Pogrel MA. Keratocystic Odontogenic Tumor (KCOT) A Cyst to a tumor. Oral maxillofac surg. 2012; 16: 163-170.
- Kramer IR, Pindborg JJN, Shear M. Keratocystic Odontogenic Tumors. Berlin, Heidelberg: Springer-Verlag. 1992: 37.
- Sansare K , Raghav M , Mupparapu M, Mundada N, Karjodkar FR, Bansal S, et al. Keratocystic Odontogenic Tumor: Systematic review with analysis of 72 additional cases from mumbai, India. Oral surg oral med Oral pathol oral Radiol. 2013; 115: 128-139.
- Yildirim GG, Ataoglu H, Kalayci A, Ozkan BT, Kucuk K, Esen A. Conservative treatment protocol for keratocystic odontogenic tumor. A follow up study of 3 cases. J Oral Maxillofac Res. 2010; 1: 7.
- Madras J, Lapointe H. Keratocystic odontogenic Tumor: Reclassification of the odontogenic keratocyst from cyst to tumor. Tex Dent J. 2008; 125: 446- 454.
- Shear M. The aggressive nature of the odontogenic keratocyst: Is it a benign cystic Neoplasm? Part I. Clinical and early experimental evidence of aggressive behavior. Oral Oncol. 2002; 38: 219-226.