
Case Report
J Dis Markers. 2021; 6(1): 1042.
Ovarian Vein Syndrome in a Woman with Abdominal Pain
Rodriguez-Morata A¹*, Reyes-Ortega JP¹, Robles- Martin ML¹, Gallardo-Pedrajas F¹, Gómez-Pascual JA²
¹Department of Angiology and Vascular Surgery, Quirónsalud Málaga Hospital, Málaga, Spain
²Department of Urology, Hospital Quirónsalud, Málaga, Spain
*Corresponding author: Rodriguez Morata Alejandro, Department of Angiology and Vascular Surgery, Quirónsalud Málaga Hospital, Málaga, Spain
Received: May 20, 2021; Accepted: June 12, 2021; Published: June 19, 2021
Abstract
Ovarian Vein Syndrome (OVS) is a rare and a controversial disease caused by varicose veins, a crossing and dilated ovarian veins inducing chronic ureteral obstruction [1]. We report a case of a woman with a large history of chronic abdominal pain and urinary symptoms with left chronical ureteral obstruction successfully treated by transvenous embolization with coils and foam.
Keywords: Abdominal pain; Ovarian veins; Varicose veins; Coil embolization
Introduction
Chronic abdominal pain is a frequent cause of consultation in women between 30-45 years, especially multiparous. This pain produces great discomfort that can affect your quality of life. In a high percentage of cases, the clinical symptoms presented by these women will be secondary to a conventional pelvic congestion syndrome, but exceptionally it may be caused by an ovarian vein syndrome.
Pelvic venous congestion syndrome and ovarian vein syndrome are two very similar entities that share symptoms (chronic hypogastralgia) and pathophysiology (dilated ovarian vein), but in the case of ovarian vein syndrome, it also produces urinary symptoms such as frequent urinary tract infections and hydronephrosis especially in the right kidney [2-6].
The anatomical relationships of the ovarian veins in the pelvis make them a possible cause of ureteral obstruction, being more frequent the involvement of the right ureter except in the case of pathologies that determine stasis in the left renal vein.
We present a peculiar case of ovarian vein syndrome in a 65-yearold woman with symptoms of left renal colic of several months of evolution that resolved with embolization of the gonadal vein.
Case Presentation
65-year-old woman with a history of hypercholesterolemia under treatment with simvastatin 20 mg and psoriatic arthritis under treatment with methotrexate.
She was referred to our service from Urology for a chronic clinical status of left flank pain compatible with recurrent renoureteral crisis. In CT-Angio made in venous phase, it could be seen how the left gonadal vein in its course towards the renal vein intimately contacted with the left ureter, producing compression and dilation of it retrogradely until causing ipsilateral hydronephrosis of the kidney (Figure 1).
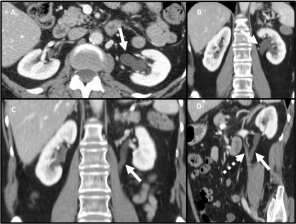
Figure 1: AngioCT scan in venous phase. A) Axial section where pyelocaliceal
dilation is seen (arrow). B) Same finding in coronal section. C) In a coronal
section, the arrow points to the dilated ureter. D) Coronal section that
indicates (solid arrow) the dilated ureter at the point of intersection with the
left ovarian vein (dashed arrow).
According to the Service of Urology, we performed a phlebography to complete the study of the left gonadal vein and proceed to its treatment by embolization in case it was necessary to treat it to reduce the pressure on the ureter.
The phlebography was performed from a superficial vein of the right arm, with a 5F introducer, a 0.035” hydrophilic guidewire and a multipurpose catheter to access the left renal vein. In the left renal phlebography the gonadal vein was not seen. This indicated that there was apparently no insufficiency and that his valve system was respected. We access with the Rebar TM reinforced microcatheter (Medtronic) in the left ovarian vein, and repeated the phlebography observing the presence of an imprint in the ovarian vein by the ureter with some pelvic varicose veins in the distal area (Figure 2).
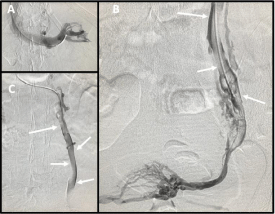
Figure 2: A) Normal phlebography of the left renal vein. B and C) Left ovarian
vein with a dilated appearance and with a marked imprint (arrows) of the left
ureter in all its extension.
With this pathological image we proceeded to catheterization of the entire left gonadal vein to practically its confluence in the renal vein and its embolization with six Concerto (Medtronic) microcoils (three coils of 1.6 x 40 cm and three coil of 2 x 50 cm). The embolization was complemented with the introduction of 10 c.c of 2% polidocanol foam in the embolized vein and a fine accessory vein that ran parallel to it and connected with the pelvic varicocele (Figure 3).
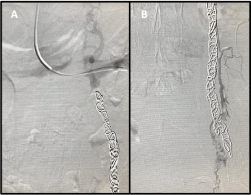
Figure 3: The embolization of the ovarian vein in this syndrome should be
done almost to its full extent, starting distally (B) and extending to a plane
more proximal to the point of initial contact with the ureter (A).
The technique was performed successfully, without incident and the patient was discharged 24 hours after the procedure.
In the weekly review with ultrasound monitoring in Urology, they observed the progressive decrease of the abdominal pain and complete remission in one month, like hydronephrosis.
Discussion
Ureteral obstruction secondary to its relationship with the ovarian vein, the so-called ovarian vein syndrome, has been discussed by many authors since Clark’s initial description in 1964 [1].
Ovarian vein syndrome occurs more frequently on the right side and can have different forms of clinical presentation.
It can present in many cases as an acute episode in pregnant women that consists of an acute pyelonephritis or a renoureteral crisis. During pregnancy, there is an increase in the diameter of the ureter that reaches its maximum at week 22 and usually returns to normal three weeks after birth. It has been shown that this dilation is not due to the pressure exerted by the uterus, having a greater relationship with the hormonal changes that occur in this state. Although throughout this stage there is an increase in flow in the ovarian vein, this is accompanied by an increase in the diameter of the vein so that the pressure does not increase. After gestation, the involution of the vein is slow and sometimes not complete [7].
More exceptionally, a chronic ovarian vein syndrome can occur as in the case of our patient. It usually manifests as a repeated urinary infection or as a continuous dull pain in the renal fossa which is frequently exacerbated between ovulation and menstruation [8].
Numerous causes have been involved in its etiopathogenesis:
• Increased pressure from a dilated ovarian vein [9,10].
• Existence of an aberrant ovarian vein [8].
• Existence of a fibrous tract [1].
• Thrombophlebitis of the ovarian vein [11,13].
• Tumours that invade the cava [10,14].
The diagnosis of this entity, when it occurs chronically, is difficult because we do not usually relate the coincidence in time of the clinical episode of nephritic colic with the premenstrual and menstrual periods. Generally, the diagnosis is usually made after evaluating the ultrasound and urography that would demonstrate ureteropyelic dilation together with signs of stenosis or “stop” at the ureteral level in the place affected by its relationship with the ovarian vein. The level of involvement is usually the lumbar ureter (L3-L4) or at the level of the pelvic rim. Retrograde ureteropyelography should only be used when intravenous urography does not demonstrate the distal ureter [14,15]. Currently, phlebography is not usually used routinely in diagnosis [14], but in our opinion given its close relationship with the dilated gonadal vein, it should be performed in a standard way and for therapeutic purposes.
In the case presented, CT-Angio revealed the diagnosis by observing how the ovarian vein at the lumbar level presents a dilation and crossing that encompasses the ureter causing pyeloureteral dilation and signs of stenosis at that level.
Differential diagnosis must be made with other extrinsic processes that can cause ureteral obstruction [16]. The most advisable diagnostic test would be a CT-Angio scan. Especially when the symptoms of renal pain are altered with changes in position two pathologies should be considered: renal ptosis (if the pain appears or increases when standing) and the ovarian vein syndrome (if the pain appears with the decubitus position) [17].
Regarding treatment, there are different options, and its indication will depend on the form of presentation of the syndrome. In pregnant women it usually remits after pregnancy.
The classic treatment has been surgical through ureterolysis [8]. Within the surgical option, it can be approached openly or by laparoscopy.
In recent years, several articles have been published that compare the results between open surgery and laparoscopic surgery in the treatment of ovarian vein syndrome, concluding the lower morbidity, shorter hospital stay, less convalescence of the laparoscopic approach compared to the open [18,19].
In our opinion, before considering surgical treatment, we should offer the patient a phlebography. It is tested to confirm the diagnosis and carry out its treatment, using coil embolization if necessary. This treatment is minimally invasive and can be enough to solve the problem, with a very fast recovery of the patient [20].
The main technical difference between venous embolization of ovarian venous insufficiency and that carried out in ovarian vein syndrome is that in the latter, it must be done in the entire vein, that is, proximal and distal to the junction with the ureter, while in the typical insufficiency of the ovarian vein, we embolize the distal and middle part, without getting too close to its junction with the cava (or kidney, in this case). It is the most similar way to total resection that could be done with laparoscopy. The embolized vein becomes fibrous and retracts in about 3 weeks, like any scar tissue, and for ureteral compression, it is as if it had been removed.
In conclusion, in those patients with clinical symptoms of nephritic colic, especially on the right side, in which the usual obstructive causes have been ruled out, this unusual clinical status of ovarian vein syndrome should be borne in mind in the differential diagnosis. Confirmed this status, the treatment that our judgment is most indicated at present would be gonadal phlebography and coil embolization.
References
- Clark J. The right ovarian vein syndrome. Clinical Urography: An Atlas End Texbook of Roentgenologic Diagnosis. 2nd ed. Philadelphia, PA: W.B. Saunders; 1964: 1227-1236.
- Shah MS, Tozzo PJ. Right ovarian vein syndrome. Urology. 1974; 3: 488- 490.
- Meiraz D, Savir A. Ovarian vein syndrome: a case report. J Urol. 1981; 125: 737-738.
- Maubon A, Ferru JM, Thiebaut C, et al. Left ovarian vein syndrome. J Radiol. 1997; 78: 223-225.
- Dykhuizen RF, Roberts JA. The ovarian vein syndrome. Surg Gynecol Obstet. 1970; 130: 443-452.
- Marcondes PR, Ferreira AA, Lane E. Diagnosis of the right ovarian vein syndrome. Am J Obstet Gynecol. 1969; 103: 888-889.
- Moyano Calvo JL, Teba del Pino F, Arellano Gañán R, Romero Tejada JC, Albacete Almodóvar P, Ruiz Zarate C, et al. Síndrome de la vena ovárica: tratamiento por embolización percutánea y revisión del mismo. Arch Esp Urol. 1993; 46: 802-806.
- Dure-Smith P. Ovarian syndrome: is it a myth?. Urology. 1979; 13: 355-364.
- Roberts JA, Dykhuizen RF. The ovarian vein syndrome. Surg Gynecol Obstet. 1970; 130: 443-452.
- Melnick RG, Bramwit DM. Bilateral ovarian vein syndrome. Am J Roentgenol Radium Ther Nucl Med. 1971; 113: 509-512.
- Coolsaet BL. Ureteric pathology in relation to right and left gonadal veins. Urology. 1978; 12: 40-49.
- Hubmer G. The ovarian vein syndrome. Eur Urol. 1978; 4: 263-268.
- Ashleigh RJ, Sambrook P. Case report: unilateral hidronephrosis following obstruction of the inferior vena cava by tumour thrombus. Clin Radiol. 1991; 44: 130-131.
- Sanz Jaka JP, Mendivil Dacal J, Estébanez Zarranz J, Aldabe Villanueva J, Arocena Lanz F. Síndrome de la vena ovárica. Arch Esp Urol. 1988; 41: 827-830.
- Monsalve Rodríguez M, Gómez Cisneros S, García Alonso J. Síndrome de la vena ovárica. Actas Urol Esp. 1984; 8: 79-84.
- Koch MO, Coussens D and Burnett L. The ovarian remnant syndrome and ureteral obstruction: medical management. J Urol. 1994; 152: 158-160.
- Marcovich R, Wolf S. Laparoscopy for the treatment of positional renal pain. Urology. 1998; 52: 38-43.
- Elashry OM, Nakada SY, Wolf JS, Figenshau RS, Mc Dougall EM, Clayman RV. Ureterolysis for extrinsic ureteral obstruction: a comparision of laparoscopic and open surgical techniques. J Urol. 1996; 156: 1403-1411.
- Gettman MT, Yair Loton MD, Cadeddu J. Laparoscopic treatment of ovarian vein syndrome. JSLS. 2003; 7: 257-263.
- Reyes Ortega JP, Robles Martín ML, Rodríguez Morata A. Tratamiento endovascular de la insuficiencia venosa pélvica primaria: varicocele masculino y varices periuterinas. En: Guerra Requena M, Rodríguez Morata A, editores. Tratamiento endovascular de la patología venosa. Capítulo de Cirugía Endovascular. 2018; 175-184.