
Research Article
Austin J Emergency & Crit Care Med. 2015; 2(7): 1041.
Factors Affecting the Decision to Prescribe Antibiotics in the Emergency Department
Karacaer Z¹*, Salman N¹, Tezel O², Avci O³, Altun D4 and Eryilmaz M5
¹Department of Infectious Diseases and Clinical Microbiology, Etimesgut Military Hospital, Turkey
²Department of Emergency Medicine, Etimesgut Military Hospital, Turkey
³Department of Biochemistry, Etimesgut Military Hospital, Turkey
4Department of Pediatrics, Etimesgut Military Hospital, Turkey
5Gulhane Military Medical Academy, Department of Emergency Medicine, Turkey
*Corresponding author: Karacaer Zehra, Department of Infectious Diseases and Clinical Microbiology, Etimesgut Military Hospital, Asagi Dikmen mah, Ankara, Turkey
Received: November 26, 2015; Accepted: December 28, 2015; Published: December 30, 2015
Abstract
Background: The aim of this study was to detect the factors affecting physician’s decisions to prescribe antibiotics for patients presenting to our hospital’s emergency department (ED) with symptoms of infectious disease.
Methods: This retrospective observational survey included the data of patients who presented to the ED with symptoms of infectious disease between January 1, 2014, and June 30, 2014. Statistical analysis was performed with SPSS version 22.0. P <0.05 was accepted as statistically significant.
Results: A total of 3,098 patients had symptoms relevant to infectious disease; 2,171 (70.1%) of them were male, and the mean age was 21 years (range 0–88). The most frequent symptom was sore throat (38.8%), and the most frequent initial diagnosis was acute pharyngitis (45.9%). The complete blood count (29.8%) was the most commonly used laboratory test. Of the treatments, 2,103 (86.2%) were empirical and 337 (13.8%) were laboratory-assisted. No culture-supported treatments were encountered. Antibiotics were included in 1,351 (64.2%) of the empirical treatments and in 252 (74.8%) of the laboratoryassisted treatments. It was identified that high fever, chest x-ray requests, signs of infection in stool, signs of infection on urinalysis, and leukocytosis affected the physicians’ decisions to prescribe antibiotics (p <0.001, p <0.001, p <0.001, p <0.001, p= 0.019, respectively).
Conclusion: High fever, chest x-ray requests, signs of infection in stool or on urinalysis, and leukocytosis significantly affected physicians’ decisions to prescribe antibiotics in the ED.
Keywords: Emergency department; Infectious diseases; Laboratory tests; Fever
Abbreviations
SIRS: Systemic Inflammatory Response Syndrome; CBC: Complete Blood Count; ED: Emergency Department; ENT: Ear- Nose-Throat; CRP: C-reactive Protein; LAT: Laboratory-Assisted Treatment; UTI: Urinary Tract Infection; AGE: Acute Gastro Enteriti; ET: Empirical Treatment; STI: Soft Tissue Infection; URTI: Upper Respiratory Tract Infection
Introduction
Infectious emergencies can create permanent tissue and organ damage if they are not treated appropriately, as these infections can transform into Systemic Immune Response Syndrome (SIRS) in a short time. Severe infections, such as meningitis, encephalitis, sepsis, septic shock, necrotizing soft tissue infections, pneumonia, complicated urinary tract infections, and severe forms of all other infections, may require urgent intervention [1]. In addition, certain diseases can be transmitted to health workers and can threaten the health of other sections of society [2].
Infectious diseases constitute an important part of emergency department (ED) admissions. Literature observing the ED admission rate of patients with infectious disease presents that this rate is about 11.3% to 14.2% in Turkey [3-5]. Donnelly et al. [6] reported that there were more than 12 million annual ED visits for acute respiratory tract infection in United States from 2001 to 2010, and antibiotics were used in the majority of these admissions. Complete Blood Count (CBC), peripheral blood smear, acute-phase reactants, urinalysis, and chest x-ray are essential studies done in the Emergency Department (ED) for the diagnosis of infectious diseases [2]. Appropriate treatment should be initiated as soon as possible after determination of a preliminary diagnosis through a detailed history, physical examination, and laboratory test results. Giving appropriate premature antibiotic treatment for infectious diseases that require emergency management prevents chronicity and complications, and increases the survival rate [7]. For successful and accurate treatment in the ED, the primary determination should be whether antibiotic therapy is necessary. Microorganisms should then be identified or cultures should be performed with infection-specific clinical material in order to choose the appropriate antibiotic. However, if there are no suitable laboratory facilities, the potential pathogens and antibiotic resistance should be considered. The final step of successful treatment involves the selection of appropriate antibiotics, as well as the appropriate dose and type of administration, and then monitoring the effectiveness of the treatment [7]. When we examined the current literature, we could find no another studies on the factors influencing physician’s decisions to prescribe antibiotics for infectious diseases in the ED.
Assessing the prudent use of antibiotics in the ED may provide opportunities to correct application mistakes and prevent antibiotic resistance. It is a significant problem to identify the most common types of infection in the ED, and to determine the laboratory tests and treatments required for these infections. At our centre, there have been no previous studies dealing with this subject. The aim of the present study was to investigate the factors that influence physicians’ decisions to prescribe antibiotics to patients presenting to our ED with infectious disease symptoms.
Materials and Methods
We performed a retrospective observational study, analyzing the written and digital records of patients admitted to our ED with complaints of infectious diseases between January 1, 2014, and June 30, 2014. Patients with incomplete data were excluded from the study. In our hospital, emergency medicine specialists serve in the ED during working hours (8:00 a.m. to 5:00 p.m.). Outside of working hours (5:00 p.m. to 8:00 a.m. and on weekends), two specialists from other fields serve in the ED. In this study, we did not perform any individual assessments or personal comparisons of the physicians. During a six-month period, 32 different specialists worked ED shifts. These included three emergency medicine specialists, two Ear/ Nose/Throat (ENT) specialists, three infectious disease specialists, one Cardiologist, two Paediatricians, three general surgeons, three neurologists, two urologists, one neurosurgeon, one dermatologist, one pulmonologist, one psychiatrist, two physical medicine and rehabilitation specialists, one gastroenterology specialist, one family medicine specialist, one gynaecologist, one plastic surgeon, one medical microbiology specialist, one ophthalmologist, and one internal medicine specialist. The physicians belonged to three groups: the emergency medicine group, the internist group, and the surgeon group. One specialist from medical microbiology was included in the internist group.
Each patient’s age, gender, symptoms, body temperature, x-ray results, CBC, sedimentation rate, C-Reactive Protein (CRP), urinalysis, stool analysis, physician’s specialty, initial diagnosis, treatment approach (empirical, laboratory-assisted, or culturesupported), antibiotics group, and conclusion (discharge, dispatch, or hospitalization) were recorded.
Our ED facilities include X-ray, CBC, sedimentation, CRP, urinalysis, stool analysis, blood and urine cultures. According to the reference values of our laboratory, the following were considered normal: CBC with leukocytes of 3.5–10.5 x 103/μl, sedimentation rate of =20 mm/h, CRP of =5 mg/dl, and urinalysis showing < 3 erythrocytes and < 4 leukocytes in all microscopic fields. Stool samples with a macroscopic appearance of soft-liquid consistency with blood and/or mucus, or microscopically involving leukocytes, erythrocytes, or any kind of parasite, were considered pathological [8]. X-rays performed in the ED were not reported by a radiologist, so we could not include the X-ray results in this study. However, the effects on decision-making for antibiotic prescriptions with regard to chest X-ray requests (in patients with fever, cough, sputum production, dyspnea, or chest pain) were investigated. The patient’s body temperatures were evaluated with a tympanic thermometer (Covidien 303000 Genius 2 Tympanic Thermometer, ear mode); < 37°C was considered normal, 37°C – 37.9°C was subfebrile, and =38°C was febrile.
Treatment decisions that used CBC, X-ray, sedimentation rate, or CRP results were designated Laboratory-Assisted Treatment (LAT). These included Urinary Tract Infection (UTI) treatments based on urinalysis and CBC, and Acute Gastro Enteritis (AGE) treatments based on stool analysis. Treatments performed according to culture results were considered the culture-supported approach, and all others were defined as Empirical Treatment (ET).
Statistical analysis was performed with SPSS software version 22.0. Data distribution was assessed with the Kolmogorov-Smirnov test. Definitive statistics were calculated, and since they were not suited to normal distribution, the scale data expressed the median (minimum-maximum) and categorical data were expressed as numbers and percentages. For comparisons among groups, the Pearson’s chi-square test was used, and a p-value of <0.05 was considered significant. Approval for the study was obtained from our hospital’s local ethics committee.
Results
During the study period, 9,042 patients were admitted to the ED, and 3,098 (34.26%) of them had symptoms associated with infectious disease. Of these patients, 2,171 (70.1%) were male and 927 (29.9%) were female, with a mean age of 21 years (range 0–88 years). Seven hundred thirty-five (23.7%) of the patients were under 18 (411 males, 324 females), 6.1% were younger than 5 years, and 1.3% were over 65.
Within the study period, the most common symptom was sore throat (38.8%) (Table 1), and acute pharyngitis was the most common preliminary diagnosis for the infectious diseases (45.9%) (Table 2).
Symptoms
Number
Percentage
sore throat
1201
38,8
fever
765
24,7
weakness
671
21,7
cough
313
10,1
headache
258
8,3
joint pain
244
7,9
diarrhea
189
6,1
nausea
164
5,3
ear ache
143
4,6
vomiting
119
3,8
stomachache
88
2,8
runny nose
73
2,4
chill
63
2
chills
51
1,6
dysuria
45
1,5
stuffiness
42
1,4
chest pain
35
1,1
dyspnea
30
1
a red area of skin
18
0,6
flank pain
16
0,5
dysphonia
11
0,4
other symptoms
26
0,8
total
4565
147,4
Other symptoms: wounds with purulent, backache, dizziness, exanthem, sputum production
Table 1: Distribution of the symptoms of patients with infectious diseases.
Diseases
Number
Percentage
Acute pharyngitis
1422
45,9
Acute tonsillitis
704
22,7
AGE
301
9,7
Acute sinusitis
154
5
AOM
121
3,9
Acute bronchitis
107
3,5
UTI
105
3,4
Pneumonia
49
1,6
Coryza
49
1,6
Seasonal influenza
33
1,1
STI
25
0,8
Other infections
28
0,9
Total
3098
100
AGE: Acute Gastro Enteritis, AOM: Acute Otitis Media, UTI: Urinary Tract Infections, STI: Soft Tissue Infections, Other infections: fever of unknown origin, acute laryngitis, suspicion of rabies exposure, chickenpox, zona, scarlet fever
Table 2: Distribution of infectious diseases.
The physician’s ET and LAT approaches were evaluated according to their specialties. It was noted that the emergency physicians mostly preferred the LAT approach, while the surgeon group mostly preferred the ET approach. There was a statistically significant difference between the emergency, internist, and surgeon groups for the ET and LAT approaches (<0.001 and <0.001, respectively). The treatment approaches according to the departments are summarized in Table 3.
Departments
Patients
Prescription
Laboratory-assisted therapy*
Empirical therapy*
n
%
n
n
%
P value+
n
%
P value+
Emergency medicine
529
17,1
426
127
29,8
<0,001
299
70,2
<0,001
Internal Departments
1553
50,1
1254
141
11,2
1113
88,8
Infectious Disease
240
7,7
156
24
15,4
132
84,6
Cardiology
218
7
191
19
9,9
172
90,1
Pulmonology
113
3,6
99
20
20,2
79
79,8
PMR
103
3,3
89
14
15,7
75
84,3
Pediatric
204
6,6
159
14
8,8
145
91,2
Neurology
162
5,2
127
13
10,2
114
89,8
Family practice
92
3
81
10
12,3
71
87,7
Dermatology
126
4,1
105
8
7,6
97
92,4
Gastroenterology
92
3
77
7
9,1
70
90,9
Psychiatry
109
3,5
91
7
7,7
84
92,3
Internal Medicine
38
1,2
34
3
8,8
31
91,2
Microbiology
56
1,8
45
2
4,4
43
95,6
Surgery Departments
1016
32,8
760
69
9,1
691
90,9
ENT
358
11,6
281
21
7,5
260
92,5
Surgery
183
5,9
122
17
13,9
105
86,1
Neurosurgery
130
4,2
92
9
9,8
83
90,2
Urology
160
5,2
134
9
6,7
125
93,3
Obstetrics and Gynecology
76
2,5
56
6
10,7
50
89,3
Plastic Surgery
70
2,3
41
5
12,2
36
87,8
Ophthalmology
39
1,3
34
2
5,9
32
94,1
Total
3098
100
2440
337
13,8
2103
86,2
ENT: Ear Nose and Throat, PMR: physical medicine and rehabilitation, *a comparison of the treatment according to the number of prescription, + a comparison of the LAT according to the departments, + a comparison of the empirical therapy according to the departments
Table 3: Distribution of the number of patients who were examined and treatment according to the departments.
A total of 958 laboratory tests were performed during the study period, and among these, the most used was the CBC (29.8%) (Figure 1). A total of 2,440 (78.8%) of the patients were given prescriptions. In addition, 72 (2.3%) of the patients were using previously prescribed medications at the time of admission, and after examination, all of them were recommended to continue those treatments. Twenty-one (0.7%) patients were referred to another health care institution for various reasons. Nine patients (seven diagnosed with pneumonia and two with acute bronchitis) were hospitalized in the pulmonology clinic, and two patients (one diagnosed with acute tonsillitis and one with acute pharyngitis) were hospitalized in the ENT clinic; the hospitalization rate in this study was 0.4%. Within this period, two patients with Soft-Tissue Infection (STI) underwent surgical drainage and dressings.
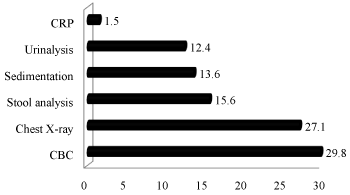
Figure 1: Distribution of the ratio of the laboratory tests used.CRP: Creactive
protein, CBC: Complete blood count.
different types of antibiotics. These were amoxicillin-clavulanic acid (67.4%), cefazolin (6.2%), ciprofloxacin (6.1%), clarithromycin (5.7%), metronidazole (3.2%), penicillin (2.1%), moxifloxacin (1.8%), ampicillin-sulbactam (1.2%), cefixime (1.2%), clindamycin (1%), metronidazole-ciprofloxacin combination (0.9%), azithromycin (0.7%), fosfomycin (0.6%), and other antibiotics (1.8%). It was found that 1,351 (64.2%) of the ETs and 252 (74.8%) of the LATs involved antibiotics.
We detected 2,103 (86.2%) ETs and 337 (13.8%) LATs. No culture-supported or algorithm-driven treatments were encountered. The diagnoses for the ET group were acute pharyngitis (49.4%), acute tonsillitis (28.5%), and acute sinusitis (6.2%). For the LAT group, the diagnoses were acute gastroenteritis (37.1%), acute pharyngitis (19%), and UTI (18.1%). We detected statistically significant difference between treatment approaches of physicians according to diagnosis group (p<0.001) (Table 4). Body temperature was normal in 71.2% of the LAT patients. It was determined that for LAT decisions about antibiotics, chest X-rays were used in 32.9%, stool analysis was used in 32.9%, urinalysis was used in 23.7%, CRP was used in 3.3%.
Diseases
Empirical therapy
Laboratory-assisted therapy
n
%
p value
n
%
p value
Acute pharyngitis
1038
49,4
<0,001
65
19,3
<0,001
Acute tonsillitis
600
28,5
26
7,7
AGE
56
2,7
125
37,1
Acute sinusitis
130
6,2
7
2,1
AOM
93
4,4
1
0,3
Acute bronchitis
60
2,9
27
8
UTI
29
1,4
61
18,1
Pneumonia
16
0,8
22
6,5
Coryza
37
1,8
-
-
Seasonal influenza
20
1
-
-
STI
21
1
1
0,3
Other infections
3
0,1
2
0,6
Total
2103
100
337
100
AGE: acute gastroenteritis, AOM: acute otitis media, UTI: urinary tract infections, STI: soft tissue infections, Other infections: fever of unknown origin, acute laryngitis, suspicion of rabies exposure, chickenpox, zona, scarlet fever.
Table 4: Distribution of the infectious diseases according to the therapy.
We investigated the effects of laboratory tests and fever on the antibiotic prescription rate. In terms of fever, the antibiotic prescription rate for patients with normal body temperature was lower than for patients who were subfebrile or febrile (p <0.001). In terms of the CBC, it was determined that the antibiotic prescription rate was remarkably higher in patients with high leukocyte counts compared to patients with normal leukocytes (p= 0.019). We detected that more than half of the patients with chest X-ray requests were prescribed antibiotics (p <0.001). The majority of patients with pathological urinalysis results, and all of the patients with pathological stool analyses, were given antibiotic prescriptions (p <0.001 and p <0.001, respectively). In patients with high CRP levels, antibiotic prescriptions were given more often; however, this difference was not statistically significant (p= 0.425). It was observed that the sedimentation rate did not affect the decision to use antibiotics (p= 0.876) (Table 5).
Without the use of antibiotic (n/%)
The use of antibiotic (n/%)
P values
Fever
normal
1152/50,5
1128/49,5
<0,001
subfebrile
207/45
253/55
febrile
136/38
222/62
Chest X-ray
absent
1398/49,3
1440/50,7
<0,001
present
97/37,3
163/62,7
Stool analysis (n:149)
normal
69/80,2
17/19,8
<0,001
pathological
0
63/100
Urinalysis (n:119)
normal
19/86,3
3/13,7
<0,001
pathological
10/10,3
87/89,7
CRP
normal
0
2
0,425
high
3
9
WBC
normal
85/44,3
107/55,7
0,019
high
28/29,8
66/70,2
Sedimentation
normal
25/35,2
46/64,8
0,876
high
20/35,9
39/66,1
CRP: C-reactive Protein, WBC: White Blood Cells, reference range: WBC 3,5-10,5 x103/μl, Sedimentation =20 mm/h, CRP =5 mg/dl, Urinalysis: microscopically contain <3/ml erythrocyte, <4/ml leukocyte, Stool analysis: macroscopically; normal rigidity, does not contain mucus, microscopically; does not contain erythrocyte, leukocyte or parasite
Table 5: Distribution of the antibiotic usage rates according to fever and laboratory tests.
Discussion
During the six-month study period, the ED admission rate of patients with infectious disease was 34.26%. In an eight-month study executed by Tasdelen-Fisgin et al., this rate was 11.3% [3], and in a study by Demircan et al. [4], the rate was 11.6%. Another study reported that in a university hospital ED, the admission rate of infectious disease patients in a one-month period was 14.2% [5]. We suggest that the higher rate of admissions in our ED represents its important role in our hospital with regard to the diagnosis and treatment of infectious diseases.
Our study period covered the months that respiratory and droplet-emitted infections are more commonly seen, and this was reflected in the high admission rates of patients with complaints such as sore throat, fever, and cough associated with Upper Respiratory Tract Infection (URTI). This is also confirmed by the fact that more than half of our patients were diagnosed with acute pharyngitis and tonsillitis. In a study executed in a university hospital ED, the most common cause of admissions for high fever was found to be sore throat and cough [9]. Another study observed that the most common initial diagnoses for infectious diseases were URTI (29.4%) and UTI (22.5%) [3]. Although our study’s URTI rates were higher compared to those in other studies, URTI was in the foreground among infectious diseases the ED in all similar studies. This result raises questions about the necessity of ED admissions for infectious diseases. Admissions to infection-specific polyclinics instead of EDs may allow for a more detailed and controlled approach to treatment. In addition, decreased ED admissions for infectious diseases may permit more appropriate use of ED facilities.
During the evaluation of infectious diseases in our ED, we determined that laboratory tests were not used at the necessary rates. CBC and chest X-ray were the most commonly performed tests, but no cultures or antibiograms were performed during the study period, and we acknowledge that this was a serious drawback. To solve this problem, an algorithm should be utilized that includes taking culture samples at the first ED admission. According to those results, appropriate antibiotic treatment could be decided after the polyclinic admission. A study in India that followed a protocol for the management of febrile patient admissions in the ED used an example of this algorithm, and it was reported that unnecessary tests and the inappropriate use of antibiotics were thereby reduced [10]. Biochemical tests help the physician to decide on an antibiotic prescription, but for evidence-based antibiotic usage, cultures have significant importance [11]. Currently, rapid diagnostic tests, such as rapid strep A and tests for rotavirus and adenovirus, have been developed as diagnostic tools [12,13]. In addition to algorithms, we recommend the use of rapid tests in ED settings.
We observed that ET was most commonly used in the diagnosis of acute tonsillitis and acute pharyngitis. In a study observing culture material from an ED, 21% of throat cultures were positive, 18% were beta-hemolytic streptococcus, and the remainder were throat flora [14]. In addition, 70% of cases of acute tonsillopharyngitis are known to be viral-sourced [7]. It is clear that ET directs physicians toward the improper use of antibiotics. The diagnosis of beta-hemolytic streptococcal infections with rapid diagnostic tests may reduce the antibiotic prescription rate for the most common infections in the ED. Another important issue regarding antibiotic prescriptions is antibiotic resistance. In our study, ET was the most preferred treatment method, and 64.2% of the ETs involved antibiotics. We suggest that this preference may give rise to improper antibiotic usage, thereby increasing the development of antibiotic resistance.
We observed that LATs were frequently used in AGE, and stool analysis results affected the physician’s antibiotic-prescription decisions. However, the diagnostic value of single-stool microscopy for AGE is still a controversial issue. Bozdemir et al. [15] examined patients admitted to the ED with complaints of diarrhea, and revealed that 50.5% of the patient’s stool analyses showed leukocytes, 14.2% showed erythrocytes, and only 6.8% had parasites. In another study, Suer et al. [9] reported that 33.07% of AGE cases were diagnosed as invasive gastroenteritis microscopically, but in none of the stool cultures were Salmonella spp. or Shigella spp. observed. Similarly, Yücel et al. [14] reported that nothing was observed in stool cultures from the AGE-diagnosed ED patients. Although stool analysis had a significant effect on physician’s antibiotic-prescription decisions, we cannot comment on the diagnostic accuracy of this analysis based on our study results.
Modified Centor Scoring is a reliable tool indicating the empirical antibiotic use at streptococcal pharyngitis patients [16]. This scoring system considers age, physical examination findings (exudates or swelling on tonsils, tender or swollen anterior cervical lymph nodes), fever (>38°C) and cough of patients. Our study data does not include physical examination findings so we can’t make an algorithm dependent comparison on antibiotic prescription decisions. Besides this we detected that the patient’s body temperatures affected the physician’s antibiotic-prescription decisions. In the LAT patients, four other parameters (high leukocyte count, an X-ray request, urinalysis, and stool analysis) also had significant effects on the prescription of antibiotics. This may be the reason that 74.8% of LAT patients were given antibiotic prescriptions. The small number of patients who underwent CRP testing may have affected the insignificant statistical results. In terms of sedimentation, this is affected by age, and there are reasons for sedimentation heights other than infections. These factors may have influenced the decisions of physicians.
Another important finding of this study was the prescribed antibiotic groups. Ozdemir et al. [17] documented that penicillinbeta- lactamase combinations were the most commonly used antibiotics in the diagnosis of URTI in the ED. Considering that the most frequent diagnostic group was URTI, and group A betahemolytic streptococcus is the most often encountered bacterial pathogen for URTI, we can assess as appropriate the physicians’ preference for amoxicillin-clavulanic acid at a rate of 67.4%. Our study’s quinolone prescription rate was 6.1%. In a multi-centre study investigating quinolone usage in the treatment of UTI in the ED, 87.3% of physicians stated that within the last year, they preferred quinolone most frequently for UTI [18]. A study observing elderly patient admissions to the ED documented that the most frequent reasons for quinolone usage were UTI, lower respiratory tract infections, chronic obstructive lung disease, and AGE [19]. We think that the lower quinolone prescription rate in our study can be explained by lower rates of AGE, UTI, and pneumonia diagnoses during the study period.
Conclusion
We recommend that physicians, particularly in the surgical group, should undergo training on the rational use of antibiotics. We determined that high fever, chest x-ray requests, signs of infection in stool or in urinalysis, and leukocytosis had significant effects on physicians’ decisions with regard to prescribing antibiotics. However symptoms suggestive of infectious diseases as in example of weakness, cough, headache, joint pain, nausea, and vomiting, abdominal pain can also occur in other systemic diseases. In the ED the use of microbiological tests (which can easily and quickly identify the microorganism such as rapid tests), as well as algorithms for accurate diagnosis and appropriate treatment, can reduce the use of unnecessary and improper antibiotic prescriptions.
References
- Willke Topcu A. Clinical approach to infectious disease emergencies. TurkiyeKlinikleri J Inf Dis-Special Topics. 2009; 2: 1-9.
- Ulutan F. Laboratory diagnosis of infectious disease in emergency medicine. TurkiyeKlinikleri J Inf Dis-Special Topics. 2009; 2: 10-20.
- Tasdelen-Fisgin N, Genc S, Tanyel E, Yilmaz H, Baydin A, Tulek N. Examination of incidence of infectious diseases among the patients who applied to the emergency clinic. Klimik J. 2006; 19: 110-113.
- Demircan C, Cekic C, Akgul N, Odabasi A, Calisir N, Kiyici S, et al. Profiles of the patients in the emergency internal medicine unit: one-year experience. UludagUniversitesi Tip FakültesiDergisi. 2005; 31: 39-43.
- Edirne T, Edirne Y, Atmaca B, Keskin S. Yüzüncü Yil Üniversitesi Tip Fakültesi acil servis hastalarinin özellikleri. Van Tip Dergisi. 2008; 15: 107- 111.
- Donnelly JP, Baddley JW, Wang HE. Antibiotic Utilization for Acute Respiratory Tract Infections in U.S. Emergency Departments. Antimicrobial Agents and Chemotherapy. 2014; 58: 1451–1457.
- Ozturk R. Acile nfeksiyon hast a likl arinda antibiy ot ikkullanimive profilaksi. I.U. Cerrahpasla Tip Fakultesi Surekli Tip Egitimi Etkinlikleri, Ic Hastaliklarinda Aciller. Sempozyum Dizisi. 2002; 29: 361-372.
- Demiral T. Akut infek siyözish allereyaklasim. STED. 2002; 11: 206-208.
- Suer K, Guvenir M, Ozgul Y, Kaptanoglu AF. Evaluation of patients with fever presented to the emergency department: a university hospital experience. Cumhuriyet Med J. 2013; 35: 480-487.
- Thangarasu S, Natarajan P, Rajavelu P, Rajagopalan A, Devey JSS. A protocol for the emergency department management of acute undifferentiated febrile illness in India. International Journal of Emergency Medicine. 2011; 4: 1-4.
- Cakmakci M. Evidence based medicine and antibiotic use: how? ANKEM Derg. 2007; 21: 13-17.
- Ciftdogan DY, Vardar F. Rapid diagnostic tests for infectious diseases. Çocuk Sagligive Hastaliklari Dergisi. 2009; 52: 159-166.
- Gozukucuk R, Gocmen I, Nas Y, Yilmazer F, Unuvar E. The effectiveness of rapid strep a test in the diagnosis of streptococcal tonsillopharyngitis. J Child. 2011; 11: 157-159.
- Yucel N, Kuzucu C, Yetkin F, Tunc E. Evaluation of the cultures of patients with symptoms of infection admitted to emergency department. Inönü Universitesi Tip Fakültesi Dergisi. 2010; 17: 359-364.
- Bozdemir MN, Kuk S, Yildiz M, Atescelik M, Basturk M, Kilicaslan I. Evaluation of the patients who presented emergency department complaining of diarrhea. Firat Tip Dergisi. 2007; 12: 118-120.
- Choby BA. Diagnosis and treatment of streptococcal pharyngitis. American Family Physician. 2009; 79: 383-390.
- Ozdemir S, Ozturk TC, Metiner Y, Ak R, Ocal O. Evaluation of the prescriptions written for upper respiratory tract infections. North Clin Istanbul. 2015; 2: 107-114.
- Guneysel O, Alsen S, Eroglu S, Akici A. Evaluation of emergency department physicians’ quinolone using habits in the treatment of urinary tract infections. Turk J Emerg Med. 2006; 6: 101-107.
- Akici A, Guneysel O, Eroglu S, Denizbasi A, Onur O, Sardas S. Quinolon utilization in elderly at emergency service and evaluation of adverse events of quinolons. AkademikAcil Tip Dergisi. 2008; 7: 24-28.