
Case Report
Austin J Nephrol Hypertens. 2015; 2(5): 1051.
Recurrent Nephrolithiasis in Childhood Progressing to End-Stage Renal Disease: Case Report
Marcos Frata Rihl*, Spada CM, De Souza VC, da Silva Selistre L
Department of Nephrology, University of Caxias do Sul, Brazil
*Corresponding author: Marcos Frata Rihl, Department of Nephrology, University of Caxias do Sul, Francisco Getúlio Vargas Street, 1130, Caxias do Sul, Brazil
Received: August 10, 2015; Accepted: November 15, 2015; Published: November 17, 2015
Abstract
Introduction: The incidence of nephrolithiasis is uncommon in children. However, this disease must not be neglected, because it might lead to progressive loss of renal function and even the need of renal replacement therapy in this age group.
Case Report: Eighteen years-old female patient in renal replacement therapy had been followed since she was four years old because of recurrent urinary tract infections, without any anatomic alterations in the urinary tract. Appeared with a staghorn calculus in her left kidney at nine years old with progressive loss of glomerular filtration rate.
Discussion: Nephrolithiasis is pointed as a risk factor to chronic kidney disease, but rarely is identified as a cause of end stage renal disease. Patients with kidney stone that develop chronic kidney disease correspond from 0.8 to 17.5%, while 0.2 to 3.2% needs renal replacement therapy. The cause of renal insufficiency in patients with nephrolithiasis is multifactorial and includes renal obstruction, recurrent urinary tract infection, frequent surgical interventions and coexistent medical diseases.
Keywords: Nephrolithiasis; Chronic kidney disease; Renal replacement therapy
Abbreviations
US: United States; CKD: Chronic Kidney Disease; ESRD: End- Stage Renal Disease; RRT: Renal Replacement Therapy; eGFR: estimated Glomerular Filtration Rate; DMSA: Dimercaptosuccinic Acid; USRDS: United States Renal Data System
Introduction
The incidence of nephrolithiasis is uncommon in children [1]. In a population-based study from the United States (US) of patients over 10 years of age, adolescents between 10 and 19 years of age accounted for only 4 percent of the total episodes of nephrolithiasis [2]. The hypothesis for the lower pediatric incidence may be due in part to the higher concentrations of crystal formation inhibitors such as citrate and magnesium in the urine of children compared with adults [3,4]. There are a growing number of publications that indicates an increased incidence of this disease in the pediatric population. However, it remains uncertain whether there was a true increase in the risk of pediatric nephrolithiasis or if there was improvement in making the diagnosis of stone disease with the use of computerized tomography or even due to environmental factors [5-7].
In a case series of 221 children with nephrolithiasis from the Mayo Clinic, 148 (67%) had two or more stones during a mean follow-up of 59 months [8]. Schwarz and colleagues reported a recurrence rate of 30%. The incidence of recurrence increases if some metabolic abnormality that contributes to the formation of kidney stones is identified [9,10].
Nephrolithiasis is a condition that rarely leads to Chronic Kidney Disease (CKD) in childhood. Although very infrequent, this disease should not be overlooked because it may lead to progressive loss of renal function and, ultimately, End-Stage Renal Disease (ESRD) requiring Renal Replacement Therapy (RRT) [11-15].
Case Presentation
We describe the case of an 18-year-old white female patient undergoing RRT at our Nephrology Department, because of progressive ESRD due to nephrolithiasis.
She had been followed up at our Division of Pediatric Nephrology since she was 4 years old by recurrent urinary tract infections, where investigations were carried out with urinary tract ultrasound which showed normal anatomical aspect and voiding cystourethrogram that evidenced no vesicoureteral reflux. Her family history of renal disease was negative.
After a period of five years without nephrological follow-up, she returns with a staghorn calculus in the left kidney (Figure 1) and stones in the right kidney and stage II of CKD [16], with 75 ml/min/1.73 m² of estimated Glomerular Filtration Rate (eGFR) by Bedside Schwartz equation, with numerous episodes of nocturia. She underwent metabolic investigation, excluding hypercalciuria, hyperuricosuria, hyperphosphaturia and secondary hyperparathyroidism. She received prophylactic antibiotic therapy because of recurrent urinary tract infections and was followed up with urinary tract ultrasounds and abdominal X-rays. Dimercaptosuccinic Acid (DMSA) renal scintigraphy was performed which showed a moderate deficit of the left kidney function (Figure 2). The absolute renal function index was 15.8% for the left kidney and 34.2% for the right kidney (30%±3% normal range reference); relative renal function index was 31.5% for the left kidney and 64.5% for the right kidney.
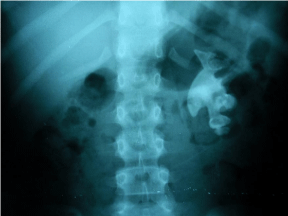
Figure 1: X-ray showing a staghorn calculus in the left kidney.
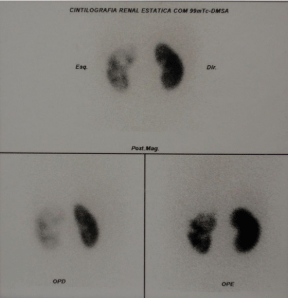
Figure 2: DMSA renal scintigraphy showing a moderate deficit of the left
kidney function (left side of the image).
When she was 10 years old a percutaneous nephrolithotomy with double-J stent was performed (Figure 3) because of hydronephrosis.
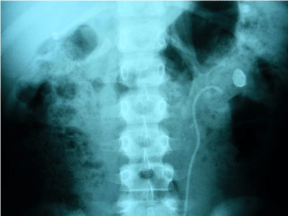
Figure 3: X-ray showing the double-J stent after the percutaneous
nephrolithotomy to reduce hydronephrosis.
In the following year she underwent two unsuccessful procedures of lithotripsy. A new DMSA scintigraphy was performed showing a marked deficit function and cortical involvement signals in both kidneys, with absolute renal function index of 4.7% for the left kidney and 23.9% for the right kidney and relative renal function index of 16.4% for the left kidney and 83.6% for the right kidney.
Less than a year after the procedures, a radical left nephrectomy was performed with pathology reporting chronic pyelonephritis associated with urolithiasis.
At age 15 had eGFR of 58 mL/min/1.73 m². At 17, laboratory tests showed hypocitraturia with 38 ml/min/1.73 m² of eGFR.
At age 18 the patient became pregnant and had a significant worsening of renal function, with a high-risk pregnancy. Fortyfive days after labor, she presented uremic encephalopathy due to progressive loss of glomerular filtration rate, being indicated hemodialysis. Three months later, she changed the modality of the renal replacement therapy to peritoneal dialysis.
Discussion
Although nephrolithiasis is a risk factor for CKD, it is rarely identified as a cause of ESRD [11-15,17].
Patients with kidney stone disease that develop CKD correspond from 0.8 to 17.5% [15]. However, it is important to distinguish stone formers in whom stones are the primary cause of ESRD from those in whom they are a contributing risk factor but not the primary cause [18]. Jungers et al. specifically investigated ESRD cases that had been attributed to kidney stones by reviewing the case histories of 1391 consecutive patients with ESRD in France [12]. Forty-five (3.2%) had ESRD attributed primarily or exclusively to kidney stones, with a significant proportion associated with struvite stones (42%). Tosetto et al. identified a history of kidney stones in only 3.2% of 1901 patients who had ESRD and were on hemodialysis, two thirds of whom (2.1%) had ESRD attributed to the kidney stones [19]. The US Renal Data System (USRDS) reports only 0.2% of all incident patients with ESRD from 2004 through 2008 had kidney stones as the primary cause [18]. Specifically about the pediatric population (age 0–19), in 2007–2011, the overall incident rate of ESRD for pediatric patients was 15.2 per million population, according to USRDS. The reported incidence of ESRD in pediatric patients by primary diagnosis in 2002–2011 showed only 12 cases out of 13,374 attributed to nephrolithiasis, 29 to primary hyperoxaluria and 118 to cystinosis [18].
The cause of kidney failure in patients with nephrolithiasis is multifactorial and includes renal obstruction, recurrent urinary tract infection, frequent surgical interventions and coexisting medical illnesses [11,12,15].
Infection stones, especially when bilateral and developing in staghorn calculus are considered the most common causes of ESRD associated with urolithiasis [20]. Besides that the urological procedures themselves, especially surgery, can damage the renal parenchyma, especially if interventions are repeated and applied in a remnant or solitary kidney [11,21]. In addition to the known mechanisms of infection and obstruction, deposition of crystals in the tubules and interstitium of the kidneys is another mechanism for renal injury mainly observed in patients with genetically transmitted metabolic disorders [11].
The risk for CKD in nephrolithiasis may increase depending on the association of certain conditions, and the risk for renal failure may be quantified as minor, intermediate and major increasing risk factors. The minor increasing risk variable is being female; the intermediate increasing risk are the pediatric population, favorable conditions for urinary tract infection (such as use of urinary indwelling catheter, neurogenic bladder, vesicoureteral reflux, prostatic hypertrophy), anatomic anomalies of the urinary system and other concomitant renal pathological states or injuring renal conditions; and major increasing risk factors are struvite lithiasis, no success in rendering the renal system stone free in the case of struvite stones, rare forms of nephrolithiasis (hereditary forms, secondary hyperoxalurias), single anatomic functional kidney and transplanted kidney [11].
Regarding the type of stone, infection stones made of struvite are the most frequent cause of renal failure. Calcium stones appear to be an infrequent cause of ESRD, such an outcome is mainly due to late diagnosis in patients with primary hyperparathyroidism and, especially, severe forms of idiopathic hypercalciuria and medullary sponge kidney, resulting in multiple stone episodes, with the aggravating influence of recurrent urinary tract infection in several patients [12]. Genetic forms (such as Cystinuria, primary hyperoxalurias) often lead to ESRD, but are rare enough to account for only a few cases of ESRD secondary to lithiasis [11]. Patients with cystine stones have a very high risk of developing CKD (as many as 70%), however ESRD occurs in less than 5% of cystinuric subjects, unlike patients with hyperoxaluria, which develop CKD in the first two decades of life, and 80% progress to ESRD before 40 years of age [11]. Other infrequent metabolic diseases may potentially lead to ESRD, such as Dent’s disease or X-linked hypercalciuric nephrolithiasis with renal failure, familial hypomagnesemia with hypercalciuria and nephrocalcinosis, and oculocerebrorenal Lowe syndrome [12].
In our case, due to the age of onset and the need for early RRT, the most likely cause may be hereditary, especially primary hyperoxaluria. However, the following factors may have contributed to the outcome, as recurrent urinary infections, staghorn calculus with hydronephrosis, bilateral stones, surgical procedures and solitary kidney after nephrectomy. All of these variables contributed to the loss of renal function.
With this report we tried to highlight that nephrolithiasis remains a possible preventable cause of CKD, sometimes requiring RRT. The dissemination of knowledge of the complications associated with nephrolithiasis even in pediatric population should enable early diagnosis and appropriate treatment.
References
- Smith J, Stapleton FB. Epidemiology of and risk factors for nephrolithiasis in children. In: UpToDate, Post TW, editor. UpToDate, Waltham MA. 2015
- Johnson CM, Wilson DM, O’Fallon WM, Malek RS, Kurland LT. Renal stone epidemiology: a 25-year study in Rochester, Minnesota. Kidney Int. 1979; 16: 624-31.
- Miyake O, Yoshimura K, Tsujihata M, Yoshioka T, koide T, Takahara S, et al. Possible causes for the low prevalence of pediatric urolithiasis. Urology. 1999; 53: 1229-1234.
- Miyake O, Yoshimura K, Yoshioka T, Koide T, Okuyama A. High urinary excretion level of citrate and magnesium in children: potential etiology for the reduced incidence of pediatric urolithiasis. Urol Res. 1998; 26: 209-213.
- Sas DJ, Hulsey TC, Shatat IF, Orak JK. Increasing incidence of kidney stones in children evaluated in the emergency department. J Pediatr. 2010; 157: 132-137.
- Bergsland KJ, Coe FL, White MD, Erhard MJ, DeFoor WR, Mahan JD, et al. Urine risk factors in children with calcium kidney stones and their siblings. Kidney Int. 2012; 81: 1140-1148.
- Dwyer ME, Krambeck AE, Bergstralh EJ, Milliner DS, Lieske JC, Rule AD. Temporal Trends in Incidence of Kidney Stones among Children: A 25-Year Population Based Study. J Urol. 2012; 188: 247-252.
- Milliner DS, Murphy ME. Urolithiasis in pediatric patients. Mayo Clin Proc. 1993; 68: 241-248.
- Schwarz RD, Dwyer NT. Pediatric kidney stones: long-term outcomes. Urology. 2006; 67: 812-816.
- Pietrow PK, Pope JC 4th, Adams MC, Shyr Y, Brock JW 3rd. Clinical outcome of pediatric stone disease. J Urol. 2002; 167: 670-673.
- Gambaro G, Favaro S, D’Angelo A. Risk for Renal Failure in Nephrolithiasis. Am J Kidney Dis. 2001; 37: 233-243.
- Jungers P, Joly D, Barbey F, Choukroun G, Daudon M. ESRD Caused by Nephrolithiasis: Prevalence, Mechanisms, and Prevention. Am J Kidney Dis. 2004; 44: 799-805.
- Gillen DL, Worcester EM, Coe FL. Decreased renal function among adults with a history of nephrolithiasis: A study of NHANES III. Kidney Int. 2005; 67: 685-690.
- Vupputuri S, Soucie JM, McClellan W, Sandler DP. History of kidney stones as a possible risk factor for chronic kidney disease. Ann Epidemiol. 2004; 14: 222-228.
- Kartha G, Calle JC, Marchini GS, Monga M. Impact of stone disease: chronic kidney disease and quality of life. Urol Clin North Am. 2013; 40: 135-147.
- KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney Int Suppl. 2013; 3: 1-150.
- El-Zoghby ZM, Lieske JC, Foley RN, Bergstralh EJ, Li X, Melton LJ 3rd, et al. Urolithiasis and the Risk of ESRD. Clin J Am Soc Nephrol. 2012; 7: 1409- 1415.
- U.S. Renal Data System, USRDS 2013 Annual Data Report: Atlas of Chronic Kidney Disease and End-Stage Renal Disease in the United States, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda MD. 2013.
- Tosetto E, Graziotto R, Artifoni L, Nachtigal J, Casone C, Conz P, et al. Dent’s disease and prevalence of renal stones in dialysis patients in Northeastern Italy. J Hum Genet. 2006; 51: 25-30.
- Collins AJ, Foley RN, Herzog C, Chavers B, Gilbertson D, Ishani A, et al. US renal data system 2010 annual data report. Am J Kidney Dis. 2011; 57:521- 526.
- Worcester E, Parks JH, Josephson MA, Thisted RA, Coe FL. Causes and consequences of kidney loss in patients with nephrolithiasis. Kidney Int. 2003; 64: 2204-2213.