
Review Article
Austin J Nutr Metab. 2016; 3(1): 1034.
The Health Implications of Vitamin D Insufficiency and Low Energy Availability in Athletes
Arlinghaus K, Ruckstuhl K and Cialdella-Kam L*
Department of Nutrition, Case Western Reserve University, USA
*Corresponding author: Lynn Cialdella-Kam, Department of Nutrition, Case Western Reserve University, School of Medicine-WG 48, 10900 Euclid Avenue, Cleveland, OH 44106, USA
Received: May 28, 2016; Accepted: July 27, 2016; Published: July 29, 2016
Abstract
Vitamin D and its extraskeletal effects has been the subject of recent research in the general population, but in the athletic community, research is scarce. In athletes, vitamin D may help to reduce infections and illnesses and improve muscle health. In this review article, we examined vitamin D insufficiency in the context of athletes with low energy availability (EA), defined as dietary energy intake (EI; kcal/day) less exercise energy expenditure (EEE; kcal/day). In female athletes, EA is considered optimal at >45 kcal/kg of fat free mass (FFM)/ day and associated with menstrual disturbances at ~30 kcal/kg of FFM/day. Adverse health outcomes in female athletes have been associated with low EA including hormonal alterations, abnormal menses, and compromised immune function and musculoskeletal health. Research is limited in male athletes with low EA, but similar health concerns have been reported. To treat low EA in athletes, current guidelines include increasing EI (e.g., inclusion of energy dense foods) or decreasing EEE (e.g., including a day off from training) and ensuring adequate intake of the bone building nutrients, calcium and vitamin D (i.e., meet the recommended dietary allowance (RDA) of 1,000 mg/day and 600 IU/day, respectively). Given vitamin D’s role as an immunomodulator and potential ergogenic aid for skeletal muscle, higher intakes of vitamin D (i.e., >RDA) may be justified as a preventive measure against injuries and illnesses typically associated with low EA; however, further research is warranted.
Keywords: Cytokines; Inflammation; Immune function; Muscle health; Sports performance
Abbreviations
25(OH)D: 25-hydroxyvitamin D; AMP: Antimicrobial Protein Secretion; BMD: Bone Mineral Density; BSAP: Bone Specific Alkaline Phosphatase; EA: Energy Availability; EEE: Exercise Energy Expenditure; EI: Energy Intake; EAR: Estimated Average Requirement; IFN-γ: Interferon-γ; IL: Interleukin; IgM: Immunoglobulin M; IGF- 1: Insulin-like Growth Factor-1; NTx: N-telopeptide; SIgA: Secretory Immunoglobulin A; Th: T helper; TNF-α: Tumor Necrosis Factor-α; RDA: Recommended Dietary Allowance; RED-S: Relative Energy Deficiency in Sport; URTI: Upper Respiratory Tract Infections; UV: Ultraviolet; VDBP: Vitamin D-binding Protein; WBC: White Blood Cell
Introduction
Vitamin D, a key bone nutrient, has been implicated in a variety of domains important to athletic performance including immune function, inflammatory responses, and skeletal muscle function [1,2]. However, only ~44% of athletes have been reported to meet their vitamin D needs based on serum 25-hydroxyvitamin D (25(OH) D) levels [3]. Vitamin D levels are considered to be deficient in athletes if serum 25(OH)D levels are <50 nmol/L (20 ng/mL) and insufficient if levels are between 50 and 75 nmol/L (20-30 ng/mL) [4]. As with the general population, athletes should strive to meet the recommended dietary allowance (RDA) for vitamin D of 600 IU/ day [4,5]. Sun exposure is the primary form of obtaining vitamin D given that dietary sources are limited [6]. Ultraviolet (UV) B rays penetrate the skin, and provitamin D3 (7-dehydrocholesterol) is converted into previtamin D3 as a result [6]. The body’s heat then causes isomerization of this compound into cholecalciferol (vitamin D3), which is further converted into 25(OH)D in the liver and finally into the active form, 1,25(OH) vitamin D, in the kidney [6]. However, regular sun exposure may be limited for a variety of reasons including living in high latitude, adhering to skin cancer prevention guidelines, training primarily indoors, and wearing clothing that covers skin for religious reasons [2,7]. In general, athletes who participate in outdoor sports (e.g., tennis, soccer, cross country, track and field, football, and cycling) have been shown to have higher 25(OH)D levels when compared to those who train indoors (e.g., swimming, basketball, dancing, gymnastics, volleyball, and wrestling) [3,8- 12]. Therefore, vitamin D must be obtained from fortified foods and dietary supplements. Dietary sources and supplements provide vitamin D either as ergocalciferol (vitamin D2) or cholecalciferol (vitamin D3) [13], which is absorbed from the intestine into the bloodstream via chylomicrons [6]. In circulation, vitamin D binds to vitamin D-binding protein (VDBP) and is transported to the liver where it is converted to 25(OH)D and then to 1,25(OH)D in the kidney [6]. In both synthesis pathways, the active form, 1,25(OH)D, is responsible for the associated roles of vitamin D such as immune and musculoskeletal health [13].
Vitamin D is a particularly important micronutrient for female athletes with low energy availability (EA) [14]. EA refers to the calories remaining after exercise (i.e., dietary energy intake (EI; kcal/day) less exercise energy expenditure (EEE; kcal/day)) for daily living activities and metabolic processes [14]. Females with an EA of <45 kcal/kg of fat free mass (FFM) per day are considered to have suboptimal EA and are at an increased risk for stress fractures, musculoskeletal injuries, and immunosuppression [14]. Furthermore, low EA has been associated with menstrual dysfunction at levels of ~30 kcal/ kg of FFM per day based on energy restriction studies conducted in sedentary women [15,16]. However, EA assessment requires accurate measurements of both EI and EEE [17]. In addition, adverse health consequences such as menstrual dysfunction occur in some women with EA >30 kcal/kg of FFM per day [18]. Females have primarily been the focus of low EA, particularly with regard to the female athlete triad, which describes the interrelationship among EA, bone health, and menstrual function [14]. Relative Energy Deficiency in Sport (RED-S) was recently introduced with the goal of including both female and male athletes and recognizes a diverse array of health and performance effects associated with low EA [19]. Such effects extend beyond the previously recognized components of the female athlete triad and include disruptions in metabolic rate, immunity, protein synthesis and cardiovascular health [19]. The purpose of this review article is to describe the health and sports performance implications of vitamin D insufficiency in the context of athletes with low EA.
Low energy availability and vitamin D
Athletes in sports in which low body fat confers a competitive advantage such as running, cycling, and gymnastics are at increased risk for low EA [4]. In female athletes, low EA has been linked to poor bone health, menstrual dysfunction, hormonal disruptions (i.e., low thyroid, insulin-like growth factor-1 (IGF-1), and leptin levels, and high cortisol levels), compromised immune function, and increased risk of musculoskeletal injuries [14,19]. Key nutrition interventions include improving EA by increasing EI (e.g., energy dense snacks) or decreasing EEE (e.g., incorporating a day off from training) and by ensuring that athletes meet the RDA for the key bone nutrients, calcium and vitamin D [18-21]. To our knowledge, no studies have examined whether athletes with low EA have a higher prevalence of vitamin D insufficiency compared to normal controls, but a few studies have reported dietary intake and circulating 25(OH)D levels in athletes with low EA or EI [18,22,23]. Viner, et al. (2015) assessed dietary intake via 3-day food logs male and female cyclists (n=10), 70% of whom were classified as having low EA (defined as < 30 kcal/ kg FFM/day) across the season. All cyclists were reported to have inadequate food intake of vitamin D (i.e., < RDA). Although, 90% of the cyclists reported taking calcium (500-1,000 mg/day) and vitamin D supplements (400-5,000 IU/day) due to insufficiencies [23]. In a 6-month carbohydrate-protein intervention in endurance-trained female athletes (8 with exercise-induced menstrual dysfunction and 9 eumenorrheic controls), Cialdella-Kam, et al. (2014) reported that slightly over half had dietary vitamin D intakes less than the Estimated Average Requirement (EAR) of 400 IU/day as determined by analysis of 7-day weighed food records. Only 3 individuals with menstrual dysfunction had low EA (<30 kcal/kg FFM/day) and mean EA was similar in eumenorrheic and oligo/amenorrheic athletes (~37-38 kcal/ kg FFM/day) [18]. All participants, including the three individuals with low EA and menstrual dysfunction, had adequate blood levels of 25(OH)D (average levels=~105 nmol/L) with 40% reporting using a vitamin/mineral supplement [18]. In adolescent female cross country runners (n=39), Barrack, et al. (2010) examined the relationship among energy deficiency (defined as <2000 kcal/day), elevated bone turnover, and vitamin D levels. Runners with elevated bone turnover exhibited a profile of energy deficiency and had lower serum 25(OH)D levels (n=13; mean=80.6 nmol/L) compared to those with normal bone turnover (n=26, mean=91.6 nmol/L) [22]. Prevalence of inadequate dietary vitamin D intake (<RDA) was similar for both groups (39% and 46% for normal and elevated bone turnover groups, respectively) [22]. Based on these few studies, vitamin D insufficiency does not appear to be more prevalent in those with low EA vs. normal controls, but further research in this area is warranted. Moreover, low EA has been associated with decreased bone mineral density (BMD) and increased risk of stress fractures [14]. Athletes are classified as vitamin D deficienct at serum 25 (OH)D levels between 50-70 nmol/L; however, higher serum 25(OH)D levels (i.e., up to 125 nmol/L) have been proposed to prevent stress fractures and to optimize adaptations from training [4,24,25]. In addition, intensive exercise training and/ or low EA can lead to chronic stress, inflammation, and impaired immunity and musculoskeletal health (Figure 1) [26-28]. As discussed below, vitamin D is involved in immunomodulation and possibly helps to maintain skeletal muscle health [1,2,29]. Thus, higher levels of vitamin D (>RDA) may be warranted in athletes with low energy availability to protect against injuries and illnesses and to optimize sports performance [4,24,25,29].
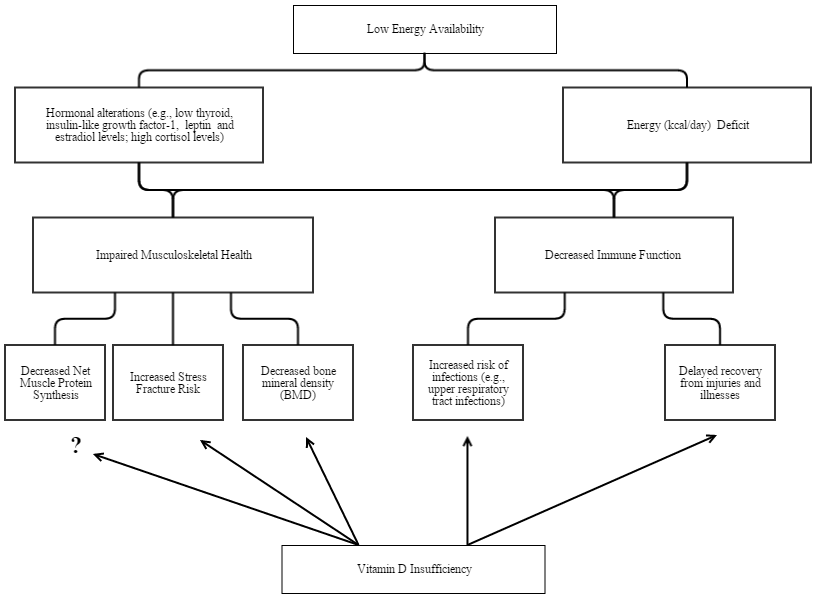
Figure 1: Theoretical Implications of Vitamin D Insufficiency in the Context of Low Energy Availability. Energy Availability (EA) is a term used in athletes to quantify
how much energy (kcal/day) is available for metabolic processes and daily living activities and is calculated by subtracting exercise energy expenditure (kcal/day)
from energy intake (kcal/day). In female athletes, EA is considered to be reduced at <45 kcal/kg of fat free mass (FFM) per day and low at <30 kcal/kg of FFM
per day [9]. Low EA has been associated with hormonal disruptions, impaired musculoskeletal health, and immunity as depicted in the figure and other health
consequences such as menstrual dysfunction and endothelial dysfunction [9]. The implications of vitamin D insufficiency (defined as <50 nmol/L) [4] in athletes with
low EA has not been well-documented. However, the theoretical implications are as follows: 1) increased bone resorption resulting in further decreases in bone
mineral density (BMD) and increased risk of stress fractures, 2) increased inflammation and suppression of immune function leading to increased risk of upper
respiratory tract infections (URTI) and delayed recovery from injuries and illnesses, and 3) potentially altered muscle metabolism. The net result is suboptimal
sports performance and general health. Further research is needed to elicit the implication of vitamin D insufficiency in athletes with low EA.
Inflammation and immunity
Immunomodulating properties of vitamin D have been well documented in animal and cellular studies [30] with only a few, however, examining the relationship between vitamin D status and inflammatory and immune markers in athletes [31-34]. In elite male (n=51) and female (n=19) athletes, Cox, et al. (2008) examined the relationship among upper respiratory tract infections (URTI), white blood cell (WBC) counts, immunomarkers, and circulating 25(OH) D levels. In this study, athletes with upper respiratory symptoms were classified as “infectious” (n=21) if they had a bacterial or viral infection, “suggestive” (n=19) based on differential WBC counts, and “unknown” if they had symptoms of unknown origins [32]. WBC and neutrophil counts were lowest in the unknown group and serum 25(OH)D concentrations were approximately twofold higher (mean=168.1 nmol/L) when compared to the infectious (mean=79.2 nmol/L) and suggestive (mean=76.9 nmol/L) groups [32]. In agreement with Cox, et al. (2008), He, et al. (2013) reported that male and female endurance-trained athletes (average training load=10h/ week) with low circulating 25(OH)D levels (n=18, <30 nmol/L) experienced more URTI symptoms over the course of 16 weeks of winter training than those with optimal levels (n=11, >120 nmol/L). In addition, plasma concentrations of the antimicrobial peptide cathelicidin was positively correlated with plasma 25(OH)D levels in a subset of athletes examined (n=80), and Secretory Immunoglobulin A (SIgA) secretion rate was higher in the optimal group vs. other groups [31]. SIgA is a critical antibody in protecting oral cavities, lungs, and guts from invading pathogens, and suppressed levels have been associated with URTI independent of vitamin D status in endurancetrained athletes [35]. Further evidence for the relationship among immune function, cytokine concentrations, and vitamin D status is provided by He, et al. (2014). Blood samples from a subset (n=43) of the previously defined study population [31] were analyzed for circulating cytokine concentrations. The anti-inflammatory cytokine, IL-10 and the pro-inflammatory cytokine, IFN-γ, were reported to be elevated in the high vitamin D group (>80 nmol/L) compared to the low vitamin D group (<40 nmol/L) [33]. Both of these cytokines play a role in viral defense, and thus higher circulating 25(OH)D levels may be protective against viral infections [33].
Contrary to the previous studies [31-33], Willis, et al. (2012) reported no relationship between serum 25(OH)D levels and the immunomodulating cytokines, IFN-γ and IL-4, nor with the antiinflammatory cytokine IL-10, in male (n=9) and female (n=10) endurance-trained runners (mean miles/week=30.8 to 34.7). However, cytokines can be affected by a variety of factors including diet, time of day, and exercise [36]; in the study by Willis, et al. (2012), no direct markers of immunity were assessed [34]. Tumor Necrosis Factor- α (TNF-α), which at high levels can negatively impact musculoskeletal health, was found to be inversely correlated with serum 25(OH)D levels, suggesting that vitamin D deficiency may increase the risk for injuries in runners [36]. In male and female collegiate athletes of various indoor and outdoor sports (n=41), Halliday, et al. (2011) reported mixed findings on the association between vitamin D status and documented illnesses (i.e., common cold, flu or other URTI), noting a correlation between status and illness in the spring season only. However, cytokines and immune markers were not assessed [11]. Of the athletes who participated, ~88% had sufficient vitamin D levels (>80 nmol/L) in the fall, ~36% in winter, and 80% in spring [11]. Taken together, conflicting evidence exists regarding the impact of vitamin D status on the incidence of illness in athletes [11,31-34], but vitamin D may modulate cytokine expression and immune cell function [31-33]. Additional research in athletes is necessary in order to determine optimal levels of vitamin D for immune function [1] and possibly for the prevention of URTI. The combination of vitamin D insufficiency, suppressed immune function, and low EA may have negative implications on athletes’ recovery, especially in sports with multiple training sessions per day or among those with high volume competition schedules. Thus, in athletes with low EA, vitamin D should be assessed, and supplementation should be considered for those with vitamin D insufficiency.
With regard to vitamin D supplementation in athletes, research is lacking related to immune function. In a randomized, double-blind, placebo-controlled study, Lewis, et al. (2013) examined the effects of season-long vitamin D supplementation in male and female collegiate swimmers and divers (n=32). The athletes were assigned to either 4,000 IU vitamin D per day (n=19) or placebo (n=13) for 6-months [37]. All athletes had sufficient 25(OH)D (>32 ng/mL) levels at baseline; however, the vitamin D group had lower baseline levels (mean=~130 nmol/L) compared to the placebo group (mean=160 nmol/L) [37]. At 6-months, four individuals in the placebo group and one in the vitamin D group had levels <80 nmol/L [37]. Over the course of the intervention, only one athlete reported an illness (i.e., URTI, influenza, gastroenteritis, or common cold), and 13 athletes experienced at least one injury (i.e., bone, connective, or muscle) [37]. Serum 25(OH)D levels were not associated with markers of bone turnover (i.e., bone specific alkaline phosphatase (BSAP) and N-telopeptide (NTx)), inflammatory cytokines (TNF-α, IL-6 and IL1-β), or injuries and illnesses [37]. Nevertheless, 77% of injuries were associated with a decline in 25(OH)D levels (range: 27-117 nmol/L) [37]. Given that all athletes had sufficient 25(OH)D levels at baseline, high vitamin D reserves at the beginning of the season may help to protect athletes from experiencing connective tissue and muscle injuries during the season. While no injuries to bone were reported, this may be due to the nature of the sports assessed (i.e., swimming and diving). Future research in this area should include more intervention-based studies with larger sample sizes of diverse populations in order to more clearly define optimal 25(OH)D concentrations necessary for health and sports performance preservation.
The mechanism by which vitamin D exerts its effects on immunity is still under investigation. Briefly, both the inactive form (25(OH) D) and the active form (1,25(OH)D) have been found to impact the immune system via intracrine, paracrine and endocrine functions (see He, et al. 2016) [1]. In innate immunity, the actions of include stimulating antimicrobial protein secretion (AMPs) and regulating epithelial cells and lymphocytes (i.e., natural killer cells, T cells, and B cells), thereby promoting increased cytokine production, T helper (Th) cell regulation, and a stronger epithelial barrier [1]. The role of vitamin D in adaptive immunity is less researched, but vitamin D may possibly regulate cytokine production [31,33]. In sum, adequate vitamin D levels are needed to support immune function. Thus, vitamin D assessment and monitoring over the course of the season is recommended, particularly in athletes at risk for low EA and/or among those who experience frequent injuries and illnesses.
Muscle strength and performance
Vitamin D deficiency has long been associated with muscle weakness, particularly in aging populations in which ~50% worldwide are estimated to be deficient [38]. However, only a few studies have examined the relationship between vitamin D and muscle strength and athletic performance [39-46] (Table 1). Only Close, et al. (2013b) reported any performance improvements related to vitamin D supplementation [40] with most studies finding no effect [39,41,42]. All of the studies presented in Table 1 included athletes from intermittent team sports; thus, findings may not be applicable to endurance-based sports such as running, cycling, and swimming and other sporting events. A few studies have been conducted in weight-sensitive sports [43,44], specifically classical ballet and judoka. In a randomized, placebo-controlled, double-blind trial, Wyon, et al. (2015) reported that a single bolus dose (i.e., 150,000 IU) of vitamin D3 in national level judoka athletes (n=22) was associated with a 13% increase in quadriceps and hamstring strength, whereas no improvements were observed in the placebo group. In ballet dancers, Wyon, et al. (2014) reported an improvement in vertical jump and isometric quadriceps strength with vitamin D3 supplementation (2,000 IU/day for 4-months). However, the link with vitamin D status was not well delineated in this study. Finally, in Nascar pit crew members (n=28) and high school athletes (n=33), the effect of vitamin D2 supplementation on muscle function and exercise-induced muscle damage was examined with no association found [45,46]. Future research should investigate the relationship between vitamin D supplementation and muscle health and strength in endurance-based sports and in athletes at risk for low EA. Different treatment approaches may be warranted in those with acute vs. chronic deficiency and may vary by sport and season of year.
Study
Athletes Examined
Intervention Groups
Vitamin D Status
Performance Outcomes
[40]
Male club-level athletes including soccer and rugby players
40,000 IU/day (n=10)
20,000 IU/day (n=10)
Placebo (n=10)
57% of participants had baseline 25(OH)D levels <50 nmol/L.
At 12-wk, plasma levels were higher in 20,000 IU/day and 40,000 IU/day vs. placebo group.
No improvements realized for 1-RM bench press, 1-RM leg press, vertical jump, and 20m sprints.
[40]
Male soccer players
5,000 IU/day (n=5)
Placebo (n=5)
70% of participants had baseline 25(OH)D levels <50 nmol/L.
Plasma levels were higher at 8-wk in the supplement group but not in the placebo group.
Improvements realized for vertical jump (~3 cm mean increase) and 10m sprint (~0.03 sec mean decrease) in supplement group with no improvement in placebo group.
No improvements realized for 1-RM bench press, 1-RM back squat, 30m sprint, and Illinois agility test.
[41]
Male soccer players who underwent high intensity interval training (HIIT) for 8 wk
5000 IU/day (n=20)
Placebo (n=16)
61% had baseline 25(OH)D levels <50 nmol/L.
At 8-wk, plasma levels were higher in supplement vs. placebo group.
No improvements realized for 30-s wingate test, sprints at 5m, 10m, 20m, and 30m, squat jump, and countermovement jump.
[42]
Collegiate male and female soccer players
3000 IU/day delivered by oral spray solution (n=22)
Placebo (n=20)
72% had baseline 25(OH)D levels <50 nmol/L.
At 12-wk, plasma levels were higher in supplement vs. placebo group.
No improvements realized for handgrip strength, vertical jump, and maximal aerobic capacity (VO2 max).
Table 1: Studies on Vitamin D Supplementation and Strength and Performance Outcomes in Athletes.
To our knowledge, Cialdella-Kam, et al. (2014) is the only study that has examined the impact of low EA and skeletal muscle strength and power. In this study, no difference in muscle strength and power was observed during a 6-month intervention aimed at improving EA and restoring menses [18]. The relationship between vitamin D status and muscle strength and power was not evaluated in this study; however, all individuals had sufficient plasma 25(OH)D levels [18]. Insufficient vitamin D and low EA cause bone and muscle to be susceptible to injury and degradation. If an injury is experienced, recovery may be impaired as a result of significant endocrine crosstalk among muscle and bone [47,48]. The role of vitamin D in this context requires further research, but it is reasonable to suspect that vitamin D is necessary for optimal biochemical communications between muscle and bone.
Conclusions
Vitamin D plays a vital role in general health, particularly for bone health and immune function. It also may be important for optimal sports performance by reducing the incidence and severity of URTI, preventing musculoskeletal injuries such as stress fractures, and aiding in recovery from exercise training and injuries. In athletes with low EA, vitamin D insufficiency may further increase the risk of low BMD, stress fractures, and compromised immune function. However, research in athletes is needed to better understand vitamin D’s roles in these realms and to determine appropriate supplement strategies for athletes who are vitamin D deficient. In addition, the optimal plasma level of 25(OH)D has not yet been ascertained with regard to optimizing immune and musculoskeletal health in athletes. For example, the Endocrine Society recommends that plasma 25(OH)D levels >75 nmol/L are needed for optimal bone health (52), whereas current recommendations for athletes are >50 nmol/L [4]. He, et al. (2016) suggest >75 nmol/L may be optimal for immune function. Additional research is needed to determine optimal levels, which may vary by sport (e.g., indoor vs. outdoor, endurance vs. intermittent sports) and season. Intense exercise training may require higher levels of vitamin D intake to prevent injuries and optimize training adaptations; however, further research on the relationship between exercise training and serum 25(OH)D is warranted. In sum, while sensible sun exposure and dietary sources such as fatty fish and fortified foods (e.g., fluid milk, ready-to-eat breakfast cereals) are acceptable methods for increasing serum 25(OH) D levels, current evidence suggests that athletes may require increased amounts, thereby potentially warranting personalized supplementation regimens.
References
- He CS, Aw Yong XH, Walsh NP, Gleeson M. Is there an optimal vitamin D status for immunity in athletes and military personnel? Exerc Immunol Rev. 2016; 22: 42-64.
- Todd JJ, Pourshahidi LK, McSorley EM, Madigan SM, Magee PJ. Vitamin D: Recent Advances and Implications for Athletes. Sports Med. 2015; 45: 213-229.
- Farrokhyar F, Tabasinejad R, Dao D, Peterson D, Ayeni OR, Hadioonzadeh R, et al. Prevalence of vitamin D inadequacy in athletes: A systematic-review and meta-analysis. Sports Med. 2015; 45: 365-378.
- Thomas DT, Erdman KA, Burke LM. Position of the Academy of Nutrition and Dietetics, Dietitians of Canada, and the American College of Sports Medicine: Nutrition and Athletic Performance. Journal of the Academy of Nutrition and Dietetics. 2016; 116: 501-528.
- Ross AC, Taylor CL, Yaktine AL, Del Valle HB. Dietary reference intakes for calcium and vitamin D. Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium. The National Academies Collection: Reports funded by National Institutes of Health. 2011.
- Holick MF. Sunlight, ultraviolet radiation, vitamin D and skin cancer: how much sunlight do we need? Advances in experimental medicine and biology. 2014; 810: 1-16.
- Baggerly CA, Cuomo RE, French CB, Garland CF, Gorham ED, Grant WB, et al. Sunlight and Vitamin D: Necessary for Public Health. J Am Coll Nutr. 2015; 34: 359-365.
- Flueck JL, Hartmann K, Strupler M, Perret C. Vitamin D deficiency in Swiss elite wheelchair athletes. Spinal Cord. 2016.
- Peeling P, Fulton SK, Binnie M, Goodman C. Training environment and Vitamin D status in athletes. Int J Sports Med. 2013; 34: 248-252.
- Valtuena J, Dominguez D, Til L, Gonzalez-Gross M, Drobnic F. High prevalence of vitamin D insufficiency among elite Spanish athletes the importance of outdoor training adaptation. Nutr Hosp. 2014; 30: 124-131.
- Halliday TM, Peterson NJ, Thomas JJ, Kleppinger K, Hollis BW, Larson- Meyer DE. Vitamin D status relative to diet, lifestyle, injury, and illness in college athletes. Medicine and science in sports and exercise. 2011; 43: 335- 343.
- Maruyama-Nagao A, Sakuraba K, Suzuki Y. Seasonal variations in vitamin D status in indoor and outdoor female athletes. Biome Rep. 2016; 5:113-117.
- Wacker M, Holick MF. Vitamin D- effects on skeletal and extra skeletal health and the need for supplementation. Nutrients. 2013; 5: 111-148.
- Nattiv A, Loucks AB, Manore MM, Sanborn CF, Sundgot-Borgen J, Warren MP. American College of Sports Medicine position stand. The female athlete triad. Medicine and science in sports and exercise. 2007; 39: 1867-1882.
- Loucks AB, Callister R. Induction and prevention of low-T3 syndrome in exercising women. Am J Physiol. 1993; 264: R924-R930.
- Loucks AB, Verdun M, Heath EM. Low energy availability, not stress of exercise, alters LH pulsatility in exercising women. J Appl Physiol. 1998; 84: 37-46.
- Guebels CP, Kam LC, Maddalozzo GF, Manore MM. Active women before/ after an intervention designed to restore menstrual function: resting metabolic rate and comparison of four methods to quantify energy expenditure and energy availability. Int J Sport Nutr Exer Metab. 2014; 24: 37-46.
- Cialdella-Kam L, Guebels CP, Maddalozzo GF, Manore MM. Dietary intervention restored menses in female athletes with exercise-associated menstrual dysfunction with limited impact on bone and muscle health. Nutrients. 2014; 6: 3018-3039.
- Mountjoy M, Sundgot-Borgen J, Burke L, Carter S, Constantini N, Lebrun C, et al. The IOC consensus statement: beyond the Female Athlete Triad- -Relative Energy Deficiency in Sport (RED-S). British journal of sports medicine. 2014; 48: 491-497.
- Arends JC, Cheung MY, Barrack MT, Nattiv A. Restoration of menses with nonpharmacologic therapy in college athletes with menstrual disturbances: a 5-year retrospective study. International Journal of Sport Nutrition and Exercise Metabolism. 2012; 22: 98-108.
- Sundgot-Borgen J, Meyer NL, Lohman TG, Ackland TR, Maughan RJ, Stewart AD, et al. How to minimise the health risks to athletes who compete in weight-sensitive sports review and position statement on behalf of the Ad Hoc Research Working Group on Body Composition, Health and Performance, under the auspices of the IOC Medical Commission. British Journal of Sports Medicine. 2013; 47: 1012-1022.
- Barrack MT, Van Loan MD, Rauh MJ, Nichols JF. Physiologic and behavioral indicators of energy deficiency in female adolescent runners with elevated bone turnover. Am J Clin Nutr. 2010; 92: 652-659.
- Viner RT, Harris M, Berning JR, Meyer NL. Energy Availability and Dietary Patterns of Adult Male and Female Competitive Cyclists with Lower Than Expected Bone Mineral Density. I J Sport Nutr Exer Metab. 2015; 25: 594- 602.
- Lappe J, Cullen D, Haynatzki G, Recker R, Ahlf R, Thompson K. Calcium and vitamin D supplementation decreases incidence of stress fractures in female navy recruits. J Bone Miner Res. 2008; 23: 741-749.
- Ruohola JP, Laaksi I, Ylikomi T, Haataja R, Mattila VM, Sahi T, et al. Association between serum 25(OH)D concentrations and bone stress fractures in Finnish young men. J Bone Miner Res. 2006; 21:1483-1488.
- Gleeson M. Immunological aspects of sport nutrition. Immunology and cell biology. 2016; 94:117-123.
- Grosset-Janin A, Nicolas X, Saraux A. Sport and infectious risk: a systematic review of the literature over 20 years. Med Mal Infect. 2012; 42: 533-544.
- Simpson RJ, Kunz H, Agha N, Graff R. Exercise and the Regulation of Immune Functions. Prog Mol Biol Transl Sci. 2015; 135: 355-380.
- Dahlquist DT, Dieter BP, Koehle MS. Plausible ergogenic effects of vitamin D on athletic performance and recovery. J Inter Soc Sports Nutr. 2015; 12: 1.
- Guillot X, Semerano L, Saidenberg-Kermanac’h N, Falgarone G, Boissier MC. Vitamin D and inflammation. Joint Bone Spine. 2010; 77: 552-557.
- He C-S, Handzlik MK, Fraser WD, Muhamad AS, Preston H, Richardson A, et al. Influence of vitamin D status on respiratory infection incidence and immune function during 4 months of winter training in endurance sport athletes. 2013; 19: 86-101.
- Cox AJ, Gleeson M, Pyne DB, Callister R, Hopkins WG, Fricker PA. Clinical and laboratory evaluation of upper respiratory symptoms in elite athletes. Clin J Sport Med. 2008; 18: 438-445.
- He C-S, Fraser WD, Gleeson M. Influence of vitamin D metabolites on plasma cytokine concentrations in endurance sport athletes and on Multiantigen stimulated cytokine production by whole blood and peripheral blood mononuclear cell cultures. ISRN Nutrition. 2014.
- Willis KS, Smith DT, Broughton KS, Larson-Meyer DE. Vitamin D status and biomarkers of inflammation in runners. Open Access Journal of Sports Medicine. 2012; 3: 35-42.
- Gleeson M, Bishop N, Oliveira M, McCauley T, Tauler P, Muhamad AS. Respiratory infection risk in athletes: association with antigen-stimulated IL- 10 production and salivary IgA secretion. Scandinavian journal of medicine & science in sports. 2012; 22: 410-417.
- Zhou X, Fragala MS, McElhaney JE, Kuchel GA. Conceptual and methodological issues relevant to cytokine and inflammatory marker measurements in clinical research. Curr Opin Clin Nutr Metab Care. 2010; 13: 541-547.
- Lewis RM, Redzic M, Thomas DT. The effects of season-long vitamin D supplementation on collegiate swimmers and divers. Int J Sport Nutr Exerc Metab. 2013; 23: 431-440.
- Lauretani F, Maggio M, Valenti G, Dall’Aglio E, Ceda GP. Vitamin D in older population: new roles for this ‘classic actor’? Aging Male. 2010; 13: 215-32.
- Close GL, Leckey J, Patterson M, Bradley W, Owens DJ, Fraser WD, et al. The effects of vitamin D(3) supplementation on serum total 25 OH D concentration and physical performance: a randomised dose-response study. Br J Sport Med. 2013; 47: 692-696.
- Close GL, Russell J, Cobley JN, Owens DJ, Wilson G, Gregson W, et al. Assessment of vitamin D concentration in non-supplemented professional athletes and healthy adults during the winter months in the UK: implications for skeletal muscle function. J Sports Sci. 2013; 31: 344-353.
- Jastrzebska M, Kaczmarczyk M, Jastrzebski Z. The effect of vitamin d supplementation on training adaptation in well trained soccer players. J Strength Cond Res. 2016.
- Todd JJ, McSorley EM, Pourshahidi LK, Madigan SM, Laird E, Healy M, et al. Vitamin D3 supplementation using an oral spray solution resolves deficiency but has no effect on VO2 max in Gaelic footballers: results from a randomised, double-blind, placebo-controlled trial. Eur J Nutr. 2016:1.
- Wyon MA, Wolman R, Nevill AM, Cloak R, Metsios GS, Gould D, et al. Acute Effects of Vitamin D3 Supplementation on Muscle Strength in Judoka Athletes: A Randomized Placebo-Controlled, Double-Blind Trial. Clin J Sport Med. 2015; 26: 279-284.
- Wyon MA, Koutedakis Y, Wolman R, Nevill AM, Allen N. The influence of winter vitamin D supplementation on muscle function and injury occurrence in elite ballet dancers: A controlled study. J Sci Med Sport. 2014; 17: 8-12.
- Nieman DC, Gillitt ND, Shanely RA, Dew D, Meaney MP, Luo B. Vitamin D2 supplementation amplifies eccentric exercise-induced muscle damage in NASCAR pit crew athletes. Nutrients. 2014; 6: 63-75.
- Shanely RA, Nieman DC, Knab AM, Gillitt ND, Meaney MP, Jin F, et al. Influence of vitamin D mushroom powder supplementation on exerciseinduced muscle damage in vitamin D insufficient high school athletes. J Sports Sci. 2014; 32: 670-679.
- Brotto M, Bonewald L. Bone and muscle: Interactions beyond mechanical. Bone. 2015; 80:109-114.
- Brotto M, Johnson ML. Endocrine crosstalk between muscle and bone. Curr Osteoporos Rep. 2014; 12: 135-141.