
Review Article
Austin J Nutr Metab. 2016; 3(1): 1038.
Vitamin D and Bone Health in Children
Pitukcheewanont P¹*, Riestra J¹, Nasomyont N² and Punyasavatsut N³
¹Department of Pediatrics, Children’s Hospital Los Angeles, USA
²Department of Pediatrics, University of South Alabama, USA
³Scottish Rite Pediatric Adolescent Consultants, Children’s Healthcare of Atlanta, USA
*Corresponding author: Pisit Pitukcheewanont, Department of Pediatrics, Children’s Hospital Los Angeles, 4650 Sunset Blvd, Mailstop #61 Los Angeles, CA 90027, USA
Received: July 21, 2016; Accepted: August 31, 2016; Published: September 02, 2016
Abstract
Vitamin D insufficiency is a major public health concern worldwide. Vitamin D plays a vital role in bone health through the regulation of calcium and phosphate absorption. In this article, we will discuss various aspects of vitamin D’ association with bone health and the detrimental effects of vitamin D deficiency. Prevention, early identification, and treatment of vitamin D deficiency may have a profoundly positive effect on the quality of life throughout the life span. Lastly, we provide recommendations on vitamin D intake to optimize bone health in children and adolescents.
Keywords: Vitamin D; Vitamin D deficiency; Hypovitaminosis D; Bone health; Children; Adolescents; Bone mineral density
Abbreviations
25OHD: 25-hydroxyvitamin D; 1,25(OH)2D: 1,25-dihydroxyvitamin D; BMD: Bone Mineral Density
Introduction
Osteoporosis is characterized by low bone mineral density (BMD) [1]. Decreased BMD is associated with increased fracture risk. In adults, normal BMD results from the balance between accrual of peak bone mass (PBM) at the end of adolescence and subsequent bone loss with age. It affects approximately 10 million individuals in the United States, causing significant morbidity and mortality. Physical inactivity, immobilization, calcium deficiency, and vitamin D deficiency are examples of important risk factors for osteoporosis.
Vitamin D
Vitamin D is a fat-soluble vitamin and essential nutrient for calcium uptake which comes from two main sources, sun exposure and vitamin D-containing foods [1]. The major source of vitamin D for all age groups is exposure to natural sunlight [1].The main source of vitamin D in the United States is fortified foods. There are two major physiological forms of vitamin D, vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol) (Figure 1). Vitamin D3 is more potent and effective than vitamin D2 for maintaining adequate levels of vitamin D in the body.
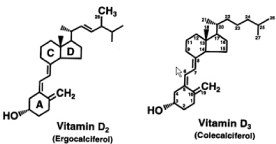
Figure 1: Structures of Vitamin D.
Over the past decade, the view on vitamin D has changed from a strict ‘vitamin’ to a ‘hormone’. The vitamin D receptor is not only expressed in tissues responsible for calcium homeostasis, but also other tissue types involved in the regulation of cellular proliferation, differentiation, apoptosis, and angiogenesis [1]. The extra skeletal effects of vitamin D have been implicated in a number of pathological processes including diabetes, cancer, multiple sclerosis, psoriasis and the inflammatory response [2,3].
Source of vitamin D
Sun exposure: Sunlight exposure is the major source of vitamin D in humans and animals via conversion in the skin. When humans are exposed to sunlight, solar ultraviolet B (UVB) photons are absorbed by the skin, leading to a chemical reaction resulting in the formation of vitamin D3 (cholecalciferol). This is converted by the liver into 25-hydroxyvitaminD3 (calcidiol, 25OHD) and is subsequently converted by the kidney into 1,25-dihydroxyvitamin D3 (calcitriol1,25(OH)2D), the active form of vitamin D.
Although sunscreen and avoidance of direct sun exposure protects against sunburns, premature aging, and cancer of the skin [4], it does interfere with the cutaneous production of vitamin D and can contribute to vitamin D deficiency.
Nutrition: Very few natural foods contain vitamin D. Flesh of fatty fish, fish liver, fish oil and fish liver oil are among the best natural nutritional sources of vitamin D. Other natural sources such as cheese, beef liver and eggs have a small amount of Vitamin D. Nowadays fortified cow milk is the main source of vitamin D in the United States. Other fortified products include, juices, cereal, bread, yogurt and margarine.
Vitamin D status
The World Health Organization defines the ‘International Unit’ (IU) of vitamin D3 as the activity of 0.025 g of the international standard preparation of crystalline vitamin D3. One IU of vitamin D3 equals 0.025 g, or 65 pmol. The unit definition of the active metabolite, calcitriol was set to be equivalent in molar terms to that of the parent vitamin D3. Thus, 1 unit is 65 pmol of calcitriol; as such the unit of calcitriol is much more active than the unit of vitamin D itself. The vitamin D requirements for children or adults have not been precisely defined. Historically, it was defined on the basis of the vitamin D content in a teaspoon of fish oil, a quantity shown to be sufficient to prevent rickets.
The serum concentration of 25OHD is the best indicator for vitamin D status due to its abundance in the circulation and the long half-life. Committee of the Pediatric Endocrine Society has recommended that a serum 25OHD level of >50 nmol/L (>20 ng/mL) is indicative of vitamin D sufficiency, a level of 37.5–50.0 nmol/L (15– 20 ng/mL) as vitamin D insufficiency, a level of <37.5 nmol/L (<15 ng/mL) as vitamin D deficiency, and a level of ≤12.5 nmol/L (≤5 ng/ mL) as severe deficiency for children [5]. Serum alkaline phosphatase is noted to elevate when serum 25OHD is less than 50.0 nmol/L (20 ng/mL) [6].
Vitamin D insufficiency /deficiency
Vitamin D insufficiency: Although there is no consensus on the optimal 25OHD concentration for skeletal health, a US expert panel considered a 25OHD concentration of >27.5 nmol/L (11 ng/mL) as an indicator of adequate vitamin D status from birth through 18 years and a concentration of >30 nmol/L (12 ng/mL) for adults aged 19–50 years [7,8]. The panel based these values on their associations with linear growth and bone mass in infants, the absence of signs and symptoms of vitamin D deficiency in children, and the relation of 25OHD with PTH concentrations and calcium balance in adults. A UK expert panel considered a plasma on concentration of >25 nmol/L (10 ng/mL) as an index of suboptimal vitamin D status [1]. Some suggest that a minimum level of 30 ng/mL (75 nmol/L) is necessary in older adults for overall health and disease prevention but insufficient data are available to support them [1-3,8,9]. This value is higher than the lower end of the reference range, suggesting that the lower end of current reference range is too low.
The report from the Drug and Therapeutics Committee of the Lawson Wilkins Pediatric Endocrine Society has recommended that a serum 25OHD level of >50 nmol/L (20 ng/mL) is considered as indicative of vitamin D sufficiency and level of 37.5–50.0 nmol/L (15–20 ng/mL) as vitamin D Insufficiency for children [5].
Vitamin D deficiency: Similar to vitamin D insufficiency, there is no consistent definition of vitamin D deficiency. The values range from <5 ng/mL to <20 ng/mL [6,10]. The report from the Drug and Therapeutics Committee of the Lawson Wilkins Pediatric Endocrine Society has recommended that a serum 25OHD level of <37.5 nmol/L (15 ng/mL) is considered indicative of deficiency and <12.5 nmol/L (5 ng/mL) as severe deficiency for children [5].
Severe vitamin D deficiency generally presents as rickets and osteomalacia in children and osteomalacia in adults. However, plasma 25OHD concentration in rickets and osteomalacia ranges from the undetectable to around 8 ng/mL (20 nmol/l) [11].
Vitamin D and Bone health
Vitamin D is essential for calcium uptake and bone development and remodeling [12]. A meta-analysis has shown a clear association between circulating vitamin D levels and BMD, although the association between circulating vitamin D levels and fracture risk was not as well supported [13].
Risk factors for vitamin D deficiency
Lack of dietary vitamin D: It may occur in people on a vegetarian diet who do not drink milk products, in people who are lactoseintolerant, or in those unable to absorb fat-soluble vitamins. Eating oily fish, such as salmon and mackerel, three or four times weekly, is usually adequate to meet the vitamin D requirement in children [14].
Lack of sun exposure: Sunlight is the primary source of vitamin D via conversion in the skin. This source of vitamin D is reduced in environmental conditions where sunlight exposure is limited.
Although chronic excessive exposure to UVB sunlight increases the risk of actinic keratosis and squamous cell carcinoma of the skin, the avoidance of direct sun exposure increases the risk of vitamin D deficiency. UVB exposure can be influenced by several factors. Lack of vitamin D production by the skin may also occur during indoor confinement because of chronic illness [15] or prolonged indoor work during daylight hours. One-third of students at Boston University who stayed indoors for long periods and always wore sun protection were vitamin D-insufficient by the end of winter [16].
Dark clothing: Individuals wearing black clothing exclude 100% of UVB light [17], while the use of sunscreen factor 8 or more excludes 95% of UVB light [2]. It has been suggested that the use of sunscreens to prevent skin cancer may actually put individuals at risk of vitamin D deficiency [18], potentially leading to osteoporotic fractures. However, there are discordant results from other studies of chronic sunscreen users that report no difference in vitamin D levels [19,20].
Pollution: Vitamin D production may be reduced in areas with severe air pollution, a common problem in many big cities. Children living in an area of Delhi, India with high levels of atmospheric pollution have significantly lower 25-hydroxyvitamin D levels than a comparable group of children living in a less polluted area of Delhi [21].
Skin pigmentation: Increased skin pigmentation also reduces the capacity of the skin to produce vitamin D. Darker-skinned people and lighter-skinned people have similar capacities to synthesize vitamin D, but, at average levels of sun exposure, vitamin D synthesis is less efficient among darker-skinned people because of their increase in skin melanin [22]. This increase in melanin requires that the skin be exposed to longer periods of sunlight in order to make the same amount of vitamin D compared with lighter-skinned individuals. Multiple studies have shown an increase in vitamin D deficiency among darker-skinned infants and children [23-28].
Living in high altitude: Higher latitude contributes to decreases in UVB. The oblique angle at which sunlight reaches the atmosphere at higher latitudes leads to a longer path through the atmosphere and ozone layer, ultimately causing increased scatter and decreased UVB [29].
Lack of prenatal care and breast feeding: Neonates born to mothers with low 25-hydroxyvitamin D levels have decreased vitamin D level at birth and are at increased risk of developing hypocalcemic seizures and rickets [30].
Human breast milk contains only small amounts of vitamin D. Thus, children who are exclusively breast-fed and do not receive vitamin D supplementation or adequate exposure to sunlight are at high risk of developing vitamin D deficiency and/or manifestations of rickets [31].
Skeletal effects of vitamin D
Vitamin D is essential for bone development and remodeling. It promotes intestinal calcium and phosphorus absorption, allowing for proper function of parathyroid hormone and inducing osteoclast differentiation [13]. A meta-analysis has also shown a clear association between circulating vitamin D levels and BMD [32].
Calcium is both actively and passively absorbed in the small intestine, and low vitamin D levels are associated with impairment of the active absorption of calcium. In individuals with vitamin D deficiency, only 10-15% of dietary calcium is absorbed [33].
Skeletal effects of vitamin D deficiency include osteomalacia due to failure of calcification of osteoid in adults with mature bone and rickets due to impaired longitudinal bone growth and epiphyseal dysplasia in children with growing bone.
Rickets
Rickets is a constitutional disease that only happens during childhood, characterized by impaired longitudinal bone growth, with cup-shaped metaphysis, widened and disorganized bone structure. Bone responds with compensatory proliferation of peripheral growth cartilage cells thus creating epiphyseal dysplasia, commonly known as rickets [34].The incidence of rickets has been increasing worldwide, possibly due to an increase in use of sunscreen and less time being spent outdoors [35]. In the United States, rickets due to vitamin D deficiency occur almost exclusively to breastfed infants who receive no vitamin D supplementation or pediatric patients with malabsorption or end-stage renal disease. Breast milk contains very low vitamin D (approximately 20-60 IU/liter) [1,3,10].
Vitamin D deficiency rickets becomes apparent during infancy and childhood. Infants may present with restlessness, slow growth, and delayed gross motor development. Gradual changes of bone due to abnormal mineralization can be visible over time especially at the end of long bones, resulting in enlargement of the wrists and ribs (rachitic rosary). The bone then becomes distorted as evidenced by bowlegs. Radiologic findings in affected longs bones may include widening of the growth plates and flaring and fraying of the metaphysis. Skull changes such as craniotabes, bossing and delay in closure of the skull bones may be noticed in infants with rickets. Late appearance of the teeth and early teeth fall out or decay can also be observed [36]. In severe cases that go untreated, bone may become fragile and fracture prone.
Treatment of vitamin D deficiency
Vitamin D: We recommend a similar regimen of1000 IU/day of vitamin D for infants <1 month old, 1,000 – 5,000 IU/day for infants 1-12 months old, and 5,000-15,000 IU/day for children older than 12 months for both nutritional deficiency and vitamin D deficiency rickets [37]. For a short term treatment, vitamin D2 2,000 IU/day, vitamin D2 50,000 IU/week, or vitamin D3 2,000 IU/day yield equivalent outcomes in the treatment of vitamin D deficiency among young children [4]. Vitamin D dosing should be reduced to 400 IU/ day after radiological evidence of healing is observed in 2 to 4 weeks of therapy.
Calcium: Calcium supplements should be considered in the presence of concurrent hypocalcemia. Calcitriol may be necessary in doses of 0.02-0.08 mcg/kg per day in two to three divided doses until calcium levels normalize. Calcium supplementation may be necessary to avoid subsequent hypocalcemia from “hungry-bone” syndrome in hypocalcemic and non-hypocalcemic children, especially those being treated with high doses of vitamin D supplementation [3].
Vitamin D supplementation
Nutritional vitamin D becomes essential when sun exposure is insufficient. Supplementation with vitamin D should be recommended for known risk groups of rickets development. Children with some liver and kidney diseases may need active vitamin D supplementation.
In 2008, the American Academy of Pediatrics (AAP) recommended vitamin D supplementation of 400 IU/day for all full-term breast-fed infants regardless of the level of formula supplementation, and 400 to 800 IU/day for preterm infants [38]. The Canadian Pediatric Society endorsed 800 IU/day of vitamin D for breast-fed infants during the winter months. The Endocrine Society suggested that infants and children aged 0-1 year require 400-1000 IU/day of vitamin D [10].
Based on the 2008 guidelines of the AAP, children who do not ingest at least 1 L of vitamin D-fortified milk per day, should receive 400 IU vitamin D per day as a supplement [38]. However, consuming 1L of milk may not be practical in some children. Due to the increased risk of iron deficiency, children aged 1-5 years should consume no more than 600 mL (20 Oz) of milk per day. The Endocrine Society suggests that children aged 1-18 years (both male and female) require 600-1000 IU /day of vitamin D [10].
Current Dietary Reference Intakes (DRIs) were developed by the Food and Nutrition Board (FNB) at the Institute of Medicine of the National Academies (formerly National Academy of Sciences) for vitamin (Table 1).
Age
AI
RDA
Male
Female
Pregnancy
Lactation
0 – 6 months
400 IU
6 - 12 months
400 IU
1 - 3 years
600 IU
600 IU
4 - 8 years
600 IU
600 IU
9 - 13 years
600 IU
600 IU
14 - 18 years
600 IU
600 IU
600 IU
600 IU
19 - 50 years
600 IU
600 IU
600 IU
600 IU
51 - 70 years
600 IU
600 IU
>70 years
800 IU
800 IU
*Adequate Intake (AI) is the experimentally determined estimate of nutrient intake by a defined group of healthy people.
Modified from National Academy of Sciences Dietary Reference Intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride.
Table 1: Recommended Adequate Intake (AI)* and Recommended Dietary Allowance (RDA) for vitamin D by Age Group (IU/day).
Conclusion
Vitamin D plays an important role in bone health in children and adolescents. Establishment of good PBM during childhood and puberty will ensure good bone health later in life. Supplementation with vitamin D should be recommended for known risks for development of rickets to ensure that children and adolescents will maintain adequate BMD through adulthood and therefore minimize risk of osteoporosis and fracture in adulthood.
References
- Holick MF. Vitamin D deficiency. N Engl J Med. 2007; 357: 266-281.
- Matsuoka LY, Ide L, Wortsman J, MacLaughlin JA, Holick MF. Sunscreens suppress cutaneous vitamin D3 synthesis. J Clin Endocrinol Metab. 1987; 64: 1165-1168.
- Pitukcheewanont P, Lin SF, Punyasavatsut N. Vitamin D deficiency in children and adolescents. In Lerner V,Chanoch M. Vitamin D Deficiency. 2011: Nova Science Hauppauge, New York.
- Pitukcheewanont P, Punyasavatsut N, Feuille M. Physical activity and bone health in children and adolescents. Pediatr Endocrinol Rev. 2010; 7: 275-282.
- Institute of Medicine of the National Academies. Dietary intakes for calcium and vitamin D. National Academies of sciences: 2010.
- Jones G, Blizzard C, Riley MD, Parameswaran V, Greenaway TM, Dwyer T. Vitamin D levels in prepubertal children in Southern Tasmania: prevalence and determinants. Eur J Clin Nutr. 1999; 53: 824-829.
- Favus MJ. American Society for Bone and Mineral Research. Primer on the metabolic bone diseases and disorders of mineral metabolism. 4th ed. (Kelseyville, Calif.): American Society for Bone and Mineral Research: 1999.
- Lloyd T, Chinchilli VM, Johnson-Rollings N, Kieselhorst K, Eggli DF, Marcus R. Adult female hip bone density reflects teenage sports-exercise patterns but not teenage calcium intake. Pediatrics. 2000; 106: 40-44.
- Autier P, Gandini S. Vitamin D supplementation and total mortality: a meta-analysis of randomized controlled trials. Arch Intern Med. 2007; 167: 1730-1737.
- Misra M, Pacaud D, Petryk A, Collett-Solberg PF, Kappy M. Drug and Therapeutics Committee of the Lawson Wilkins Pediatric Endocrine Society. Vitamin D deficiency in children and its management: review of current knowledge and recommendations. Pediatrics. 2008; 122: 398-417.
- Looker AC, Johnson CL, Lacher DA, Pfeiffer CM, Schleicher RL, Sempos CT. Vitamin D status: United States, 2001-2006. NCHS Data Brief. 2011; 1-8.
- Holick MF. Vitamin D and bone health. J Nutr. 1996; 126: 1159S-64S.
- Cranney A, Horsley T, O'Donnell S, Weiler H, Puil L, Ooi D, et al. Effectiveness and safety of vitamin D in relation to bone health. Evid Rep Technol Assess (Full Rep). 2007; 1-235.
- Holick MF. Calcium and vitamin D in human health. ANNALES NESTLE. 2002; 60: 83-93.
- Del Arco C, Riancho JA, Luzuriaga C, González-Macías J, Flórez J. Vitamin D status in children with Down's syndrome. J Intellect Disabil Res. 1992; 36: 251-257.
- Tangpricha V, Pearce EN, Chen TC, Holick MF. Vitamin D insufficiency among free-living healthy young adults. Am J Med. 2002; 112: 659-662.
- Matsuoka LY, Wortsman J, Dannenberg MJ, Hollis BW, Lu Z, Holick MF. Clothing prevents ultraviolet-B radiation-dependent photosynthesis of vitamin D3. J Clin Endocrinol Metab. 1992; 75: 1099-1103.
- Farrerons J, Barnadas M, López-Navidad A, Renau A, Rodríguez J, Yoldi B, et al. Sunscreen and risk of osteoporosis in the elderly: a two-year follow-up. Dermatology. 2001; 202: 27-30.
- Marks R, Foley PA, Jolley D, Knight KR, Harrison J, Thompson SC. The effect of regular sunscreen use on vitamin D levels in an Australian population. Results of a randomized controlled trial. Arch Dermatol. 1995; 131: 415-421.
- Sollitto RB1, Kraemer KH, DiGiovanna JJ. Normal vitamin D levels can be maintained despite rigorous photoprotection: six years' experience with xeroderma pigmentosum. J Am Acad Dermatol. 1997; 37: 942-947.
- Agarwal KS, Mughal MZ, Upadhyay P, Berry JL, Mawer EB, Puliyel JM. The impact of atmospheric pollution on vitamin D status of infants and toddlers in Delhi, India. Arch Dis Child. 2002; 87: 111-113.
- Dawson-Hughes B. Racial/ethnic considerations in making recommendations for vitamin D for adult and elderly men and women. Am J Clin Nutr. 2004; 80: 1763S-1766S.
- Weisberg P, Scanlon KS, Li R, Cogswell ME. Nutritional rickets among children in the United States: review of cases reported between 1986 and 2003. Am J Clin Nutr. 2004; 80: 1697S-1705S.
- Specker BL, Tsang RC, Hollis BW. Effect of race and diet on human-milk vitamin D and 25-hydroxyvitamin D. Am J Dis Child. 1985; 139: 1134-1137.
- Stein EM, Laing EM, Hall DB, Hausman DB, Kimlin MG, Johnson MA, et al. Serum 25-hydroxyvitamin D concentrations in girls aged 4-8 y living in the southeastern United States. Am J Clin Nutr. 2006; 83: 75-81.
- Cosgrove L, Dietrich A. Nutritional rickets in breast-fed infants. J Fam Pract. 1985; 21: 205-209.
- Callaghan AL, Moy RJ, Booth IW, Debelle G, Shaw NJ. Incidence of symptomatic vitamin D deficiency. Arch Dis Child. 2006; 91: 606-607.
- Binet A, Kooh SW. Persistence of Vitamin D-deficiency rickets in Toronto in the 1990s. Can J Public Health. 1996; 87: 227-230.
- Diamond J. Evolutionary biology: geography and skin colour. Nature. 2005; 435: 283-284.
- Markestad T. Effect of season and vitamin D supplementation on plasma concentrations of 25-hydroxyvitamin D in Norwegian infants. Acta Paediatr Scand. 1983; 72: 817-821.
- Kreiter SR, Schwartz RP, Kirkman HN Jr, Charlton PA, Calikoglu AS, Davenport ML. Nutritional rickets in African American breast-fed infants. J Pediatr. 2000; 137: 153-157.
- Peacock M. Calcium absorption efficiency and calcium requirements in children and adolescents. Am J Clin Nutr. 1991; 54: 261S-265S.
- Lowdon J. Rickets: concerns over the worldwide increase. J Fam Health Care. 2011; 21: 25-29.
- Hochberg Z. Rickets--past and present. Introduction. Endocr Dev. 2003; 6: 1-13.
- Daniels ED, Pettifor JM, Moodley GP. Serum osteocalcin has limited usefulness as a diagnostic marker for rickets. Eur J Pediatr. 2000; 159: 730-733.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011; 96: 1911-1930.
- Gordon CM, Williams AL, Feldman HA, May J, Sinclair L, Vasquez A, et al. Treatment of hypovitaminosis D in infants and toddlers. J Clin Endocrinol Metab. 2008; 93: 2716-2721.
- Huang S.A, Lifshitz F. Hypothiroidism. Pediatric endocrinology. 5th ed. New York: Informa Healthcare: 2007.