
Research Article
Austin J Obes & Metab Synd. 2021; 5(1): 1024.
Influence of the Basal Metabolic Profile on the Evolution of the Pediatric Patient with Obesity
Fernández Fernandez B, Sarasua Miranda, Lorente Blazquez I and Diez López ID*
Department of Pediatric Endocrinology, Araba University Hospital-Txagorritxu, Spain
*Corresponding author: Diez López ID, Department of Pediatric Endocrinology, Araba University Hospital- Txagorritxu, Bioaraba Health Research Institute, 01009 Vitoria-Gasteiz, Spain
Received: April 22, 2021; Accepted: May 19, 2021; Published: May 26, 2021
Abstract
Purpose: To study how basal metabolism influences the somatometric evolution of the child and adolescent population with obesity in a pediatric endocrinology clinic.
Material and Methods: Study of the entire population diagnosed with childhood obesity in a tertiary hospital by means of a multichannel impedanceometry study, TANITA BF 430.
Results: 100 patients were selected by chance and studied from a database with 1400 records. Most of the patients who attend to these consultations for obesity are girls, between 8 and 11 years old. All the patients studied had a basal metabolism lower than the calculated theoretical ideal. The group of boys at the beginning of their follow-up showed a higher basal metabolism and more similar than the group of girls. Girls had a higher amount of fat mass compared to boys at the beginning of their follow up. After their first year of follow-up, both groups achieved a decrease in the percentage of fat mass, double in the case of boys compared to girls. After three years of the study, it was observed that 54% of the boys achieved a reduction in their FM compared to 36% of the girls.
In overall terms, weight reduction is not achieved in this pediatric population. However it is observed a decrease in fat content in the medium term (1-3 years). The reduction of this fat mass could be a protection factor against cardiovascular diseases in adults. Given the same adherence to nutritional programs, it is believed that physical exercise rates influence this reduction. It was also observed that the most relevant data in the evolution of obesity in these patients is the basal metabolism that they present at the beginning of their follow-up.
Discussion: Childhood obesity is a problem of increasing importance in our society. Understanding its characteristics would allow different strategies to be taken for a better treatment and diagnosis of these cases. Boys, in general, achieve a greater reduction in fat mass in the same follow-up time. Due to sexual dimorphism, or a higher rate of physical activity.
Bioelectrical impedanceometry measurement is a simple, cheap and easy to use method in clinical practice to evaluate the energy consumption and the body composition of the patient. In “healthy child” health programs and even in schools, an impedanceometry machine could be purchased to focus physical activity efforts on those boys and girls with a lower basal metabolism, adding a greater consumption factor such as physical exercise. Thus, it would be possible to increase the requirements and the basal metabolism of the patient would increase, favoring the loss of fat mass.
Regarding the use of conventional scales, in this type of patients, if we only look at the weight variable, a bias could be created since it would not be noticed that there has been a decrease in fat content at the cost of an increase in muscle mass.
Conclusion: We consider that it should be recommendable to supply with a multichannel impedanceometry every pediatric endocrine consultation room as it is a non-invasive, and easy-to-use test that can provide a great amount of information about the evolution of these patients, since we believe that focusing efforts on those boys and girls who have a worse basal metabolism could contribute to improving the efficiency and effectiveness of the scarce health resources that we have.
Keywords: Body mass index; TBW
Introduction
Obesity, in adults and in childhood, is one of the most serious public health problems of the 21st century. The World Health Organization (WHO) describes it as an epidemic since it generally affects all countries.
In 2016, more than 41 million children under the age of five were overweight or obese [1]. That same year, according to UNICEF, the prevalence in children and adolescents between the ages of 5 and 19 was approximately 124 million with obesity and 216 million with overweight [2]. In pediatric age, obesity is already the chronic non-communicable disease and the most frequent nutritional and metabolic disorder [3].
The importance resides in the association of obesity with important health problems and the development of serious noncommunicable diseases, such as cardiovascular diseases, high blood pressure, type 2 diabetes mellitus and some types of cancer, which increases social and health costs considerably.
It is suspected that the presence of common causal factors could explain the global nature of this problem. Among other theories arises that of the Thrifty Genotype [4,5], whose hypothesis maintains that, due to the way of life of primitive man, the human genome developed a tendency to create energy reserve tissues for periods of famine based on fats since they provide more calories in less volume. This type of genes in a current way of life, characterized by food in abundance, cheap and with high fat contents, and the tendency to sedentary lifestyle of the population, would be responsible for the aforementioned global epidemic of the 21st century: obesity [6-8]. In developing countries, the prevalence of obesity and overweight in preschool children exceeds 30%, which represents a significant risk for them to become adults with metabolic syndrome and obesity [1].
Obesity is defined as an excess of body fat, the result of a positive energy balance persisting over a long period of time [9]. This situation in childhood develops different types of complications [10]. At first, problems such as flat feet, insulin resistance, increase in androgens, increase in cholesterol, LDL (Low-Density Lipoproteins) and triglycerides, as well as pulmonary, menstrual, type 2 diabetes and psychological disorders, such as deteriorated self-image.
After the first two or four years of the onset of obesity, obese children increase the risk of high blood pressure, hypercholesterolemia, increase in LDL, and decrease in HDL (High-Density Lipoprotein). If this situation persists, the presence of an increase in coronary diseases, vascular hypertension, vascular kidney disease, atherosclerosis, arthritis and certain neoplasias is added in adulthood, which are those that increase morbidity and explain mortality in adult life. Furthermore, obesity in pediatric age is related to other comorbidities such as: sleep apnea, nonalcoholic steatohepatitis, cholelithiasis, pseudotumor cerebri, gastrointestinal reflux and polycystic ovary syndrome [10].
A simple tool to assess this problem is the Body Mass Index (BMI), which represents both fat mass and fat-free mass, so it is an indicator of weight and not of adiposity as such. It is independent of height, allowing the comparison of the body weights of individuals of different heights [10].
Body composition is made up of two major components: Body Fat Mass (BFM) and Lean Body Mass (LBM). Fat mass refers to the fat tissue, lipids that the human body has, while lean mass in turn is divided into three main components: Total Body Water (TBW), mineral content, mainly bones, and protein content like muscles.
In the first year of life there is a significant increase in body fat content, followed by a period of decline that ends between the 4 to 6 years of age, increasing later until the end of adolescence, known as adipose rebound. The earlier the rebound begins, the greater the risk of later obesity [11]. Childhood overweight is established above the 85th percentile of BMI, and obesity above the 95th percentile of BMI [12]. Due to the physiological differences between boys and girls, graphics and percentiles are created for each sex [10,13,14].
In Spain, the ALADINO study has evaluated the prevalence of childhood overweight and obesity every 4 years since 2011. In 2019, a downward trend is observed since 2011 and stable compared to 2015 [15]. Currently in Spain overweight in the child population is 23.3% and obesity 17.3% [15]. Poor eating habits, low physical activity and low socioeconomic status of the family influence these results. A significant percentage of parents mistakenly perceive their children’s overweight or obesity as normal.
The child population with overweight oro bese has, in general, greater weight at birth than thin or normal weight children. By sex, overweight is more prevalent in girls and obesity in boys. In children, the frequency of overweight is higher in those of 9 years and regarding obesity in those of 7, 8 and 9, compared to younger age groups. In girls, there are no age differences in overweight, while obesity increases from 6 to 8 years old [15].
Being thin does not necessarily mean having a lower percentage of body fat than people who are thinner, since the latter can be more muscular. A high percentage of fat tissue increases the risk of developing cardiovascular diseases, diabetes, hypertension and certain types of cancer [16,17]. Accurately assessing the weight of a person is to know the body composition, that is, the amount of lean body mass and fat body mass in their organism. There are different measurement methods, each of them with advantages and disadvantages: [16]
• Octopolar multi-frequency impedance measurement: An electrical current of very low intensity runs through the body, interacts with body water, which has a constant proportion of muscle mass. This data, together with the sex, age and height of the patient, calculates the body muscle mass. Fat mass does not conduct electricity, so it is not directly measured.
• Dual X-ray Absorption (DXA): “Gold standard”. It determines the corresponding weights and percentages of fat, bone and muscle tissue. It allows assessing the specific location of an excess of fat or muscle tissue. It evaluates the distribution of android and gynoid fat and these two data are two of the best predictors of health risks.
• Anthropometry: It consists of measuring skin folds using a “caliper”, different perimeters and diameters. It needs to be measured by an expert. Applying a series of formulas subsequently, the body composition and the somatotype are determined. It reports the magnitude and distribution of subcutaneous fat. However, it only provides regional body fat data, not the deep fat. Also, it is not useful for measuring folds in obese people.
• Image morphological study: it observes subtle changes in body silhouette, volumes and postural habits.
Metabolism represents energy expenditure at a baseline situation without stress. And it is primarily determined by age, sex, size, and body composition. The most used technique for its determination is indirect open-circuit calorimetry; its value can also be estimated using predictive equations. The most used in the pediatric population are those of Schofield and those of the WHO [18].
In 2017, a study led by the Imperial College London and the WHO concluded that the number of children and adolescents (between the ages of 5 and 19) with obesity has multiplied by 10 in the world in the last four decades. It is also indicated that in 2022 there will be more children and adolescents with obesity than children with low weight.
Two articles on body composition in the adolescent [19] and adult [20] population have been found in the literature, but not in the child population. Both highlight the fact that the female population has a higher percentage of body fat mass; and that in overall; the obese population has a lower basal metabolism than estimated, higher in men than in women. In general, in terms of intake, this population falls within the normal limits of the FAO/WHO recommendations; at the same time that they present insufficient total energy expenditure.
Detecting excess weight early and preventing it during childhood is essential to achieve a greater impact on health.
With the aim of finding another explanation for excess weight in childhood, apart from those already mentioned, this work will focus on finding a causal relationship between basal metabolism and excess weight in the child population.
Hypothesis
Given the importance of the knowledge and management of obesity due to its relationship with certain comorbidities in the child population, it seems necessary to know if children who attend hospital consultation for childhood obesity referred from primary care have a basal metabolism or caloric intake below what is expected for their age and sex. Assuming that this fact is an associated risk factor for obesity or, on the other hand, its usual treatment is more difficult than usual.
Aim
To study how basal metabolism influences the somatometric evolution of the child and adolescent population with obesity in a pediatric endocrinology consultation.
Material and Methods
An anonymized and coded database of a pediatric endocrine clinic in a tertiary hospital was used, which records the body composition of patients by means of impedance measurement at different consultations, up to 3 years of follow-up.
Finally, a sample of 100 people was selected from the database that had 1,400 patients.
Inclusion criteria
• Patients referred from primary care, less than 14 years of age at the time of referral, who present a lack of weight control.
• Minimum age 6 years, due to impedance measurement limitation.
• Minimum longitudinal follow-up 12 months (at least 2 visits).
Deferral criteria
• Patients with syndromic or similar diseases that could justify their overweight or obesity.
Results
The type of patient who mainly attends these consultations is 11-years-old girls (Figure 1 and 2).
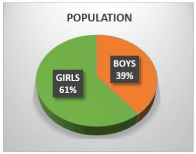
Figure 1: Pediatric population attending consultation for weight control in OSI
Araba, by sex.
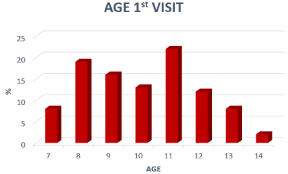
Figure 2: Age distribution of the pediatric population that attends consultation
for weight control at OSI Araba.
In girls, it is observed that most of them start the follow-up at two different ages or at 8 years of age or, mostly, at 11 years.
On the other hand, men make up less than half of the sample and generally begin their follow-up at 9 years, following a homogeneous trend between 8 and 11 years (Figure 3).
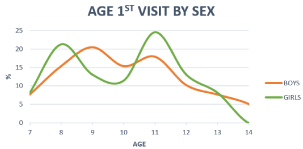
Figure 3: Distribution of age at first visit by sex of the pediatric population that
attends consultation for weight control at OSI Araba.
The entire sample studied presented a basal metabolism lower than that corresponding to their age and sex, on average the difference was -209 kcal in both boys and girls.
In the light of this analysis, it is obtained that the mean basal metabolic rate at the first visit in boys was 1664±262.54kcal, and 1408±125.54kcal in girls. While, according to their calculated theoretical water needs with the TBW predictive equations [18], the ideal basal metabolism of boys would be 1740 kcal and that of girls would be an average of 1700 kcal (Figure 4).
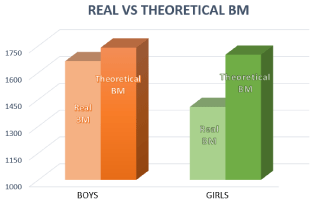
Figure 4: Real and theoretical basal metabolism calculated by sex of the
pediatric population that attends consultation for weight control in OSI Araba.
All patients who come for obesity control are instructed in standardized child nutrition educational programs.
After the first 12 months of follow-up, basal metabolism in both sexes increased. Boys reached 1738±276.84 kcal and girls reached 1449±123.20 kcal.
The calculated theoretical basal metabolism increases steadily with age. This trend, although with values lower than those desired, is maintained in the analyzed sample in all age ranges except 9 years; at this age the basal metabolism has more similar values to the calculated theoretical metabolism with a difference of -85 kcal (Table 1).
AGE at the start of follow-up
BM medium
BM theoretical medium
Mean difference BM
EvoBFM
1 YearEvoBFM
3 Years7
1.315
1.422
-107
-0,5
1,6
8
1.409
1.517
-108
-1,7
-1,5
9
1.534
1.619
-85
-0,4
0,3
10
1.481
1.691
-210
-1,7
-4,5
11
1.505
1.817
-311
-1,9
-2,2
12
1.56
1.878
-318
-0,7
-1,0
13
1.717
2.077
-360
-2,3
-2,7
14
2.077
2.237
-161
-16,2
-11,5
Table 1: Evolution of basal metabolism and body fat mass by age groups of the pediatric population attending the consultation for weight control at OSI Araba.
After one year of follow-up, all age groups achieved a decrease in body fat mass content. The higher success rate was at 11 years, achieving a reduction of almost 2% in fat mass.
At 9 years of age, despite a basal metabolism more similar to the theoretical one, the lowest rate of reduction in fat content is achieved per year, that is -0.4%
After three years, there continues to be an overall decrease in the percentage of fat mass. The 7 and 9-year-old groups, after three years of follow-up, show a slight increase in their fat content (+ 1.6% and + 0.9%, respectively), corresponding to the start of adolescence.
Whereas the 10-year-old group, after three years achieved a reduction of 4.5%.
A greater difference is observed in the 14-year-old group, but due to such extreme data and the low prevalence of the sample at this age, they are considered non-representative values.
Regarding the study of body composition by sex:
At the beginning of the control, the boys had an average of 36.4 ± 6% of fat mass and the girls an average of 37.1±3% of fat mass.
After the first year, there is a decrease in fat content in both sexes. Boys had around 34.2±6% of fat mass (-2.2%) and girls 35.9±4% (-1.2%) (Figure 5).
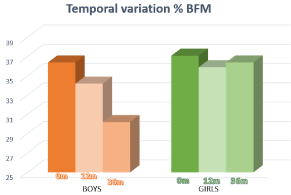
Figure 5: Temporal variation of the percentage of body fat mass by sex of the
pediatric population that attends consultation for weight control at OSI Araba.
After one year, the boys in the study show an increase of 2.2% (65.8 vs. 63.6%) in lean body mass content. Of this, 72% of this increase corresponds to mineral-protein components. So these boys have increased height and their muscle development.
The girls in the study, after the first check-up per year, increased their lean body mass content by 1.2% (62.9 vs. 64.1%), of which 75% corresponds to mineral-protein component and the remaining 25% to body water (Table 2).
Group Statistics
Sex
N
Average
Standar desviation.
Typ. of the average
BMI 1st visit
1
39
259,908
321,650
,51505
0
61
259,008
274,005
,35083
BM1st visit
1
39
1664,28
262,548
42,041
0
61
1408,23
125,544
16,074
Percentage FBM 1st visit
1
39
363,923
608,304
,97407
0
61
370,967
394,309
,50486
Percentage MM 1st visit
1
39
636,077
608,304
,97407
0
61
629,033
394,309
,50486
Percentage TBW 1st visit
1
39
465,564
446,641
,71520
0
61
460,328
288,084
,36885
BMI 1st year
1
39
262,321
322,294
,51608
0
61
257,726
292,998
,37515
BM 1st year
1
39
1737,97
276,845
44,331
0
61
1448,66
123,207
15,775
Percentage FBM 1st year
1
39
341,718
660,853
105,821
0
61
358,852
443,132
,56737
Percentage MM 1st year
1
39
658,282
660,853
105,821
0
61
641,148
443,132
,56737
Percentage TBW 1st year
1
39
481,718
485,191
,77693
0
61
469,344
324,401
,41535
BMI 3years
1
27
277,304
380,609
,73248
0
46
272,963
561,547
,82796
BM 3years
1
27
1929,07
301,142
57,955
0
46
1494,46
259,396
38,246
Percentage FBM 3years
1
27
302,000
753,831
145,075
0
46
363,804
703,027
103,656
Percentage MM 3years
1
27
698,000
753,831
145,075
0
46
614,457
1,025,306
151,173
Percentage TBW 3years
1
27
510,815
552,317
106,293
0
46
448,109
759,190
111,937
Table 2: Body composition analysis by group statistics.
68% of the patients, regardless of their age or sex, achieved a reduction in fat content after one year of control, so it can be said that they actually managed to lose weight. After three years, 61% of the sample persists in a decrease in their body fat content, the remaining 7% gain fat, that is, they gain weight (Figure 6).
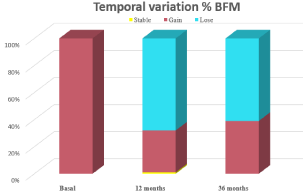
Figure 6: Temporal evolution of the percentage of body fat mass of the
pediatric population that attends consultation for weight control at OSI Araba.
After three years, the fat content in boys was reduced to 30±7.5%. Girls, on the other hand, increased the fat content compared to the previous control, (+ 0.5% GM) although they do not reach initial figures (Figure 5).
Despite finding numerical differences, this result of body composition after three years for BFM, LBM and TBW are not statistically significant, since Levene’s test for equality of variances show a p>0.05.
54% of boys after three years achieved a reduction in fat mass compared to 36% of girls.
Most of the patients who achieved a reduction in fat mass after three years of follow-up are those who started the control at 11 years.
Regarding the relationship between the kg of weight and the weight situation of the pediatric population: (Figure 6- 10).
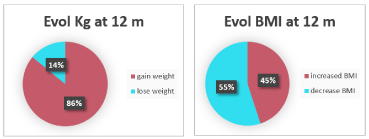
Figure 7 and 8: Evolution at 12 m of the weight in KG and BMI of the pediatric
population that attends the consultation for weight control at OSI Araba.
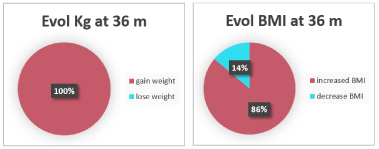
Figure 9 and 10: Evolution at 36 m of the weight in KG and BMI of the
pediatric population that attends consultation for weight control in OSI Araba.
In the first year, 86% of the studied sample increased their initial weight and 45% their BMI value. Whereas, in the same time, only 31% increased their body fat content.
The same occurs after three years, 100% increased their initial weight and 86% increased their BMI, but 61% decreased their fat content.
The lack of relationship between weight and body fat content is observed, which is really harmful to health.
Finally, it was studied which of all the available variables had the most influence on these results, and it was the value of the basal metabolism that the patient presents at the beginning of the followup (Figure 11 and 12).
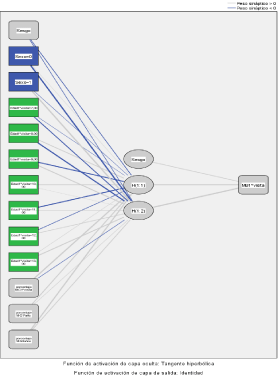
Figure 11: Analysis of the relationship of different variables in the evolution of
the obese pediatric population.
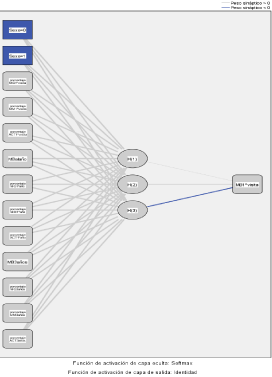
Figure 12: Analysis of the relationship of several variables in the evolution of
the obese pediatric population.
Discussion and Conclusion
Childhood obesity is a problem of increasing importance in our society. Knowing its characteristics would allow different strategies to be taken for a better treatment and diagnosis of these cases.
One of the strategies is to know if those girls and boys who have a worse evolution are those who either move less, consume more food or, on the contrary, their body could have a lower metabolism. The present essay focuses on this possible third cause in which it was called the Thrifty Gene syndrome. Among the main methods of the study of consumption, the bioelectrical impedance measurement was chosen as it is a simple, cheap and easy-to-use method in clinical practice. It has been shown that the basal metabolism of these patients is globally lower than the theoretical one, more noticeable in girls as well as the presence of a higher percentage of fat mass in girls compared to boys, as it has been published in previous studies; In a novel way, it has been concluded that the patients who fare worse over a follow-up time of between 1 and 3 years are girls, who on average had a basal metabolism markedly lower than the theoretical one for their age and sex.
In turn, it is observed that after one year of follow-up and all of them employing standardized educational programs in child nutrition, the boys achieve a greater reduction in the percentage of fat mass. From this it can be deduced that a basal metabolism more similar to the needs intervenes positively when it comes to burning the excess of body fat.
It was observed how 86% of the individuals in the study after one year of follow-up gained weight, while only 31% presented an increase in their fat content. From this it can be deduced that the changes in nutritional habits of these patients, added to their growth, influence weight gain at the expense of increasing other parameters, without the need for an increase in fat content. There is a risk of committing a bias when assessing the total weight by not perceiving that there has been a decrease in fat content at the cost of an increase in muscle mass. In the pediatric population, the gross data of total weight and BMI are not faithful to the seriousness of this disease and its evolution, what makes more interesting to know their body composition. One of the most reliable methods to determine this composition is bioimpedance measurement, such as the one used in this study.
It has previously been shown how after 12 months of follow-up, the boys reduced their LBM by 2.2%, therefore an increase in BFM and that, of this, 72% corresponded to the mineral-protein component. The girls in the same period, reduced the BFM more discreetly, a 1.2%, and the increase of the mineral-protein component was of 75%.
A growth in height and an increase in muscle content can be seen, greater in girls, this can be a result of the fact that they start puberty two years earlier. This growth period would be key to achieving a reduction in fat mass and for overweight or obese patients to be normal weight.
Regarding the fat content by sex, both presented on average very similar percentages, although the girls presented slightly higher numbers. Interestingly, it was observed that the boys after reevaluating them after 12 months achieved a greater reduction, twice that of the girls. It can be deduced that, given the same adherence to nutritional programs, since both achieve a reduction, boys perform on average more physical activity than girls, which influences basal metabolism and a subsequent decrease in fat content.
One of the purposes was to find out which of the variables, of all available, had the most global influence on the results of the population. Characteristically, the value of the basal metabolism of the boy and girl at the time of the start of follow-up, turned out to be the variable that most influences the evolution of these patients, regardless of other variables such as sex, age, BFM at the beginning, etc.
It can be observed how basal metabolism can influence a person’s tendency to gain weight. For example, a person with a low basal metabolic rate (who therefore burns fewer calories while resting or sleeping) will tend to gain more pounds of body fat over time than a similarly tall person with an average basal metabolic rate who eats the same amount of food and practices the same amount of physical exercise.
In view of these results and the importance of the situation of obesity in the child population, we propose to carry out a new study that includes variables that were not included in this study to analyze in more detail the child population affected by obesity, such as ethnicity, the type of family to which they belong, the economic resources they have and customs.
On the other hand, it would also be interesting to evaluate body composition, not only by age and sex, but also taking into account pubertal development, that is, the Tanner stage at the time of data collection.
Due to the current mobility restrictions and economic crisis derived from the COVID-19 pandemic worldwide, it would be interesting to study its impact on the weight control and prevalence of this disease in the population, especially in the pediatric population.
We emphasize the importance of the impedance measurement study and to focus efforts on the population with the worst basal metabolism and to contribute to improving the efficiency and effectiveness of the scarce health resources that we have. Achieving an effective action in childhood obesity will improve life expectancy and its quality in adulthood.
References
- OMS | Comisión para poner fin a la obesidad infantil. 2020.
- Español UC. Malnutrición, obesidad infantil y derechos de la infancia en españa. 2020.
- Rivero Urgell M, Aznar Moreno LA, Dalmau Serra J, MorenoVillares JM, Aliaga Pérez A, García Perea A. Libro Blanco de La Nutrición Infantil. 2015.
- Bermudez V, Joanna J, Quintero R, Hospital W. Predisposición humana a la Obesidad, Síndrome Metabólico y Diabetes: El genotipo Ahorrador y la incorporación de los diabetogenes al genoma humano desde la Antropología Biológica. 2011.
- Valenzuela B A. ¿Porqué Comemos Lo Que Comemos? Rev Chil Nutr. 2011; 38: 198-209.
- Tarbal A. La Obesidad Infantil: Una Epidemia Mundial. 2006.
- Cascales Angosto M. Pandemia Del Siglo Xxi. 14-46.
- Controlling the global obesity epidemic. 2021.
- OMS | Obesidad. 2021.
- Kaufer-Horwitz M, Toussaint G. Indicadores antropométricos para evaluar sobrepeso y obesidad en pediatría. Bol méd Hosp Infant Méx. 2008; 65: 502- 518.
- Fundación para la Formación e Investigación Sanitarias de la Región de Murcia (ffis). Rebote Adiposo Precoz. 2014.
- José M, Sopena M. Valoracion Nutricional En La Obesidad Infantil. 2007: 1-32.
- Carrascosa A, Fernández JM, Ferrández Á, et al. Estudios Españoles de Crecimiento. An Pediatría. 2008; 68: 552-569.
- Güemes-Hidalgo M, Muñoz-Calvo MT. Obesidad en la infancia y adolescencia. Pediatr Integr. 2015; 19: 412-427.
- Aladino E. Estudio sobre la Alimentación, Actividad Física, Desarollo Infantil y Obesidad en España 2019. 2019.
- Mesa T. ¿Cómo se mide la composición corporal?. Neolife. Blog. 2016.
- Rodriguez R. Conceptos para adelgazar : ¿ Sabes qué es la masa magra , la masa grasa y la grasa visceral ? Muy saludable. 2017.
- MorÁis López A, Rivero de la Rosa M, Galera Martínez R, et al. Calculo Requerimientos Energetico-Proteicos Para El Soporte Nutricional. Acta Pediatr Esp. 2011; 69: 211-216.
- Marcela Reyes J, Erick Díaz B, Lydia Lera M, Raquel Burrows A. Ingestay metabolismo energético en una muestra de adolescentes chilenos con sobrepeso y obesidad. Rev Med Chil. 2011; 139: 425-431.
- Liang X, Chen X, Li J, Yan M, Yang Y. Study on body composition and its correlation with obesity A Cohort Study in 5121 Chinese Han participants. Med (United States). 2018; 97: e10722.