
Research Article
Phys Med Rehabil Int. 2014;1(5): 6.
The Role of Interlaminar and Transforaminal Epidural Steroid Injections for Discogenic Low Back Pain without Radiation
Priyesh Mehta, Dev Sinha, Clark Smith, Jaspal R Singh*
Department of Rehabilitation Medicine, Weill Cornell Spine Center, USA
*Corresponding author: Jaspal R Singh MD, Department of Rehabilitation Medicine, Weill Cornell Spine Center, USA
Received: December 01, 2014; Accepted: December 19,2014; Published: December 23, 2014
Abstract
Background: Transforaminal and Interlaminar Epidural injection of local anesthetics with or without steroids is one of the most commonly used interventions in managing chronic low back and lower extremity pain. However, there has been a lack of well-designed randomized, controlled studies to determine the effectiveness of epidural injections in the treatment of lumbar discogenic back pain.
Study Design: A systematic review of interlaminar and transformainal epidural injections with or without steroids in managing chronic low back pain of dicogenic origin.
Objective: To evaluate the effect of transforaminal and interlaminar epidural injection epidural injections with or without steroids in discogenic back pain.
Methods: A literature review was performed using PubMed, EMBASE from 1966 - December 2012, Cochrane database, Clinical Trial Registry, previous systematic reviews and cross references published in the English language. The level of evidence was classified as Level I, II, or III based on the quality of evidence developed by the U.S. Preventive Services Task Force (USPSTF).
Outcome Measures: The primary outcome measure was pain relief (shortterm relief = up to 6 months and long-term > or = 6 months). Secondary outcome measures of improvement in functional status, psychological status, return to work, and reduction in opioid intake were utilized.
Results: The evidence level II-2 for interlaminar epidural steroid injection for short term pain relief for lumbar discogenic back pain and level II-3 for transforaminal epidural steroid injection for short term pain relief for lumbar discogenic back pain.
Limitations: The limitations of this study include the paucity of literature and lack of randomized controlled trials.
Conclusion: The results of this systematic evaluation for the treatment of discogenic pain of indicated evidence levels of level II-2 for interlaminar injections and level IIIfor transforaminal injections.
Keywords: Epidural Steroid Injections; Discogenic pain; Interlaminar; Transforaminal
Introduction
The high incidence of chronic low back pain with or without lower extremity pain impacts the lives of many Americans, and incurs substantial health care and other societal costs. The lifetime incidence of low back pain is reported to be as high as 84% and the prevalence of chronic low back pain is about 23%, with 11-12% of the population being disabled by low back pain [1]. Back pain results in about 40% of absences from work and is second to only the common cold as the most frequent cause for sick leave. The cost of back pain in the United States ranged from $50 billion to $ 100 billion yearly and continues to rise [2]. An analysis of data from the National Health Interview Survey (NHIS) estimated that in a given 1-year period, there are about 22.4 million cases of back pain that last a week or more, and these cases were estimated to result in a total of about 149 million lost workdays [3]. The pathophysiology of both low back pain and radicular pain has been the subject of ongoing research, with discogenic pain comprising a major cause of non-specific low back pain. While the umbrella term "discogenic pain" may refer to radicular pain caused by disc pathology, for the purposes of this manuscript, discogenic pain is defined as pain resulting from internal derangements of the intervertebral disc without associated herniation or impingement of nerve roots. A proposed mechanism of discogenic back pain is an inflammatory change of the intervertebral disk, and multiple studies indicate that nerve endings penetrate into the nucleus pulposus (NP) [5]. It has been reported that substance P and calcitonin generelated peptide are also contained in the NP and with the presence of penetrating nerves could be involved with transmitting nociceptive information from the disc [12]. With the availability of diagnostic blocks and interventional techniques including discography, facet joint blocks and sacroiliac joint blocks, axial/discogenic pain can be more reliably attributed to specific pain generators [7, 8, 16-19].
Epidural steroid injections (ESI) are one of the most common interventional techniques for managing chronic low back pain with or without lower extremity radiation [6, 7, 11]. Some patients with axial back pain improve with conservative treatment however in a recent literature review for non-operative management for discogenic pain; Young et al concluded that there are few high-quality studies evaluating non-operative treatments for reducing discogenic low back pain. Out of those studies physical therapy modalities including traction therapy reported no significant improvements in VAS scores [4]. Various types of interventional procedures are can be utilized for patients with chronic axial pain without radicular components. Friedly et al reported that as many as 36% of patients with persistent axial low back pain receive epidural injections and this percentage may be continuing to rise, especially in the Medicare population [6]. Fluoroscopy improves the efficacy of these injections by ensuring proper needle positioning and targeted delivery of the therapeutic agent as well as preventing complications [6, 7]. Epidural injections are administered by accessing the lumbar epidural space by various techniques including interlaminar (ILESI), caudal and transforaminal (TFESI) approaches. There are significant differences between these three approaches. While caudal epidural steroid injections are considered to be the safest, they often require high volumes to reach the site of pathology [8]. ILESI refer to injections into the space between the laminae of adjacent vertebrae. With this approach the injectate disperses over a greater area as compared to the transforaminal approach and thus this type of injection is commonly used for bilateral or multilevel symptoms [14]. TFESI target the foramen between the vertebrae through which the nerve roots exit. This injection preferentially delivers injectate to the ventral epidural space at the suspected pathologic site [13].
The effectiveness, indications and medical necessity of ESI's for internal derangements of the intervertebral disc without associated herniation or impingement of nerve roots is controversial. This may be attributed to the high variability in evidence and the lack of sufficient randomized controlled trials. Many clinicians extrapolate from studies on the treatment of radiculopathy when considering the benefits of ESI for axial discogenic pain. While the long-term benefit of epidural steroids is debated for radiculopathy, the short-term pain benefit from weeks to months for sub-acute pain is recognized [9-11].
In contrast to the evidence for treatment of radicular pain, little evidence exists regarding ESI in treatment of intrinsic axial discogenic pain despite this being a more common cause of low back pain. The paucity of evidence may be partially due to the difficulty in clinically diagnosing discogenic pain with validated diagnostic tools. Discography remains to be controversial for diagnosing discogenic back pain with multiple studies indicating concerns for the high false positive rate, the lack of concordance, potential confounding factors, and safety of the procedure [15, 16, 17]. Due to the ongoing debate this review looks to evaluate the evidence for transforaminal and interlaminar ESI in treatment for axial/discogenic lower back pain. To our knowledge this is one of the first reviews evaluating the effectiveness of transforaminal and interlaminar epidural steroid injections for the management of lumbar discogenic pain without radicular symptoms.
Methods and Materials
Literature search
A comprehensive literature search of databases was conducted including PubMed, EMBASE from 1966 - December 2012, Cochrane database, Clinical Trial Registry, previous systematic reviews and cross references published in the English language. The search was performed looking specifically for discogenic low back pain with focus on transforaminal and interlaminar epidural injections. Search terminology included "discogenic pain", "axial pain", "disc related pain", "selective nerve root block", "low back pain", "lumbar transforaminal epidural injections" and "lumbar interlaminar epidural injections".
Selection criteria
The review focused on randomized controlled trials and nonrandomized observational studies. The populations of interest were patients suffering from chronic discogenic low back pain without radicular symptoms. In addition participants must have failed previous pharmacotherapy and a physical therapy program prior to pursuing interventional pain treatment options. Studies in which subjects had radicular component of pain or there was involvement of the facet and/or sacroiliac joints were excluded. Further if the caudal approach was used to administer the epidural injection, these studies were excluded as well.
Outcome parameters
The primary outcome parameters were of documented pain relief in terms of numerical pain rating scale and/or visual analog scale at various points in time. These time points included 2-3 months, 4-6 months and 12 months following intervention. Successful outcome was defined as >50% reduction in pain from baseline. If individual studies did not report this value, it was extrapolated from the data. In addition functional improvement (measured by Oswestry Disability Index), change in psychological status, return to work, reduction of opioid use or non-narcotic analgesics and other interventions and complications were evaluated.
Analysis of evidence
Quality analysis was conducted using 5 levels of evidence developed by the U.S. Preventative Services Task Force (USPSTF), ranging from Level I to III with 3 subcategories in Level II, as illustrated in Table 1.
I
Evidence obtained from a least one properly randomized controlled trial
II-1:
Evidence obtained from well-designed controlled trials without randomization
II-2:
Evidence obtained from well-designed cohort or case-control analytic studies, preferably from more than one center or research group
II-3:
Evidence obtained from multiple times series with or without the intervention. Dramatic results in uncontrolled experiments could also be regarded as this type of evidence
III:
Opinions of respected authorities, based on clinical experience descriptive studies and case reports or reports of expert committees
Adapted from the U.S. Preventive Services Task Force (USPSTF) (29).
Table 1: Quality of evidence development by USPSTF.
Methodological quality assessment
Only studies meeting the inclusion criteria were reviewed. Each study was evaluated by 2 physicians (CS and JRS) for stated criteria and any disagreements were resolved by a third physician (PM).
Results
A literature search was carried out for lumbar interlaminar and transforaminal epidural steroid injections for chronic low back pain or discogenic pain without radicular symptoms as shown in Figure 1. Our review yielded 3 studies addressing effectiveness of ILESI and 1 study using TFESI for treatment of axial discogenic pain.
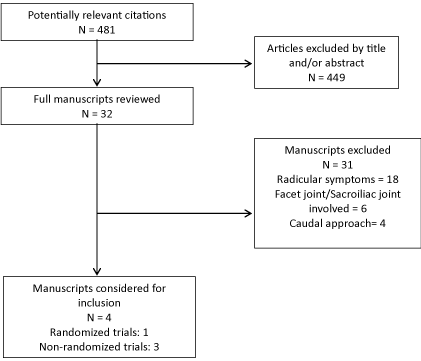
Figure 1: Flow diagram illustrating selection process of included articles.
Study characteristics
Interlaminar Epidural Steroid Injection: Table 2 illustrates the details of studies looking at the effectiveness of lumbar interlaminar epidural injections for discogenic pain.
Study/Methods
Participants
Intervention(s)
Outcome(s)
Result(s)
Conclusion(s)
Manchikanti et al (2012)
(18)
Active control, double-blind, Randomized controlled trial
120 patients with lumbar axial or discogenic pain of at least 6 months duration into two groups. 6 mL 0.5% lidocaine alone = 60, and 5 mL 0.5% lidocaine with 1 mL 6% betamethasone. = 60. No patients with facet joint or sacroiliac joint diagnosed by anesthetic blocks were include. None of patients had undergone surgery
Lidocaine alone or Lidocaine mixed with betamethasone
Timing: 3 mos, 6 mos, 12 mos
Primary outcome measures:
NRS (0-10), ODI scale (0-50). Secondary outcome- employment status, opioid intake. Significant improvement was defined as at least 50% decrease in pain and disability
Significant improvement in pain relief was seen in 83% and 73% for Group I and Group II respectively, 72% and 75% at 6 months, and 77% and 67% at 12 months.
Positive short term <6months, and positive long term >6 months relief with anesthetic with or without steroid for the treatment of chronic lumbar axial pain
Lee et al (2010)
(20)
Non-Randomized controlled trial
81 patients with low back pain without radicular symptoms and no improvement with conservative therapy.
Axial back pain was diagnosed with a non-validated compression maneuver.
1 mL of 40mg triamcinolone mixed with 1 mL of 0.5% bupivacaine and 1mL normal saline
Timing: <1mos, 1-3 mos, 3-6 mos, >6 mos
Outcome measures:
Reduction of >50% of pain score after injection
78% showed improvement in pain <3 months and 77.5% >3 months, median symptom free interval 154 days
Positive short term benefit
Table 2: Details of trials studying the effectiveness of lumbar interlaminar ESI on discogenic pain.
Manchikanti et. al performed a randomized- double blinded control trial to compare the effectiveness of lumbar ILESI for managing chronic low back pain of discogenic origin. Patients with at least 6 months duration of low back pain with failure to improve with conservative treatment including but not limited to physical therapy, exercises, medications or chiropractic manipulation were included in this study. Two groups of patients were studied, with 60 patients in each group receiving either local anesthetic only or local anesthetic with non-particulate betamethasone. Outcome measures were the numeric pain rating scale and Oswestry Disability Index. Secondary outcome measures included employment status and opioid intake. Significant improvement (defined as >50% reduction in VAS and ODI) was seen in 77% of patients in the group with anesthetic only and 67% in the group with anesthetic and betamethasone. In addition there were significant differences in opioid intake within the groups over time. The largest methodological flaw in this study was that the majority of patients had both back and leg pain. While this study was aimed at assessing the efficacy of ILESI on chronic lumbar axial pain, 65% of the patients had some form of leg pain. The authors concluded that for those with chronic function-limited low back pain refractory to conservative treatment, lumbar ILESI with or without steroids are effective for managing discogenic low back pain. There is some short term benefit <6 months as well as long term benefit >6 months with ILESI based on pain relief and functional assessment. The findings also concluded average total relief per year of 40.0 ± 15.6 weeks in Group I and 39.6 ± 12.4 in Group II.
Lee et. al evaluated ILESI for managing discogenic low back pain without radicular symptoms. This study implemented a nonvalidated compression maneuver to diagnosis axial back pain. This compression maneuver was performed by placing the patient in prone position and drawing an imaginary line between the tops of the iliac crest. The examiner presses on various spots near this target and positive sign is a definite sharp pain on 1 side and not the other. Therefore it is unclear that these patients suffered from "discogenic" pain or back pain from another etiology. Eighty one patients with axial low back pain without radiation and minimal improvement with medication and physical therapy for 2 weeks were included in the study. Lumbar ILESI were performed at levels L3-L4, L4-L5, L5- S1. The injectate consisting of 40mg triamcinolone, 0.5 mL normal saline and 1.0 mL bupivacaine hydrochloride 0.5% was injected into the posterior epidural space through the interlaminar approach for all patients. Pain relief using a percentage reduction in pain scores were assessed at multiple time point intervals (1mo, 2mo, 6mo, >1yr). The authors concluded that interlaminar ESI for axial LBP was effective in 77.8% of patients. Majority of the patients reported pain relief at initial short term follow up with 37% having >6 months of symptom relief. The study also indicated that two-thirds of patients through telephone survey indicated positive satisfaction and were willing to repeat the procedure. In addition there is possible inclusion bias where only short term follow up patients were included in this study.
Effectiveness: As shown in Table 2, of the three studies included in the evidence synthesis all three showed short term benefit (< 6 months) with the one randomized-double blinded controlled study indicating a long term benefit (>6 months).
Transforaminal Epidural Steroid Injection: Table 3 illustrated the details of studies looking at the effectiveness of lumbar transforaminal epidural injections for discogenic pain. While no study met all the inclusion criteria, this study contained patients with mixed pathologies of radiculopathic low back pain.
Study/Methods
Participants
Intervention(s)
Outcome(s)
Result(s)
Conclusion(s)
Rosenberg et al (2002)
(21)
Non-Randomized controlled trial
34 patients with "radiculopathic" low back pain
60-80mg Methylprednisolone mixed with lidocaine with epinephrine and bupivacaine.
Timing: 2mos, 6mos, 12mos
Outcome measures: telephone questionnaire
68% showed pain relief at 2 months, 56% at 6 months, 59% at 12 months
Positive short and long term benefits however limited by mixed pathology of patients.� Not truly axial discogenic pain patients.
Table 3: Details of trials studying the effectiveness of lumbar transforaminal ESI on discogenic pain.
Rosenberg et al. investigated the effectiveness of transforaminal epidural steroid injections (TFESI) for "radiculopathic" low back pain in a nonrandomized controlled study. The study evaluated 34 patients with discogenic low back pain treated with TFESI containing 60-80 mg methylprednisolone acetate (DepoMedrol), 1 ml 1.5% lidocaine (with epinephrine 1:200,000) and 1 ml of 0.25% bupivacaine Patients were followed up with pain scores at 2 months, 6 months and 1 year. The authors observed the most significant reduction in pain score was seen in the discogenic back pain group when compared to other groups including patients with spinal stenosis and previous back surgery patients. However, the authors' definition of "discogenic" comprises both axial and radicular pain components and this is the greatest limitation of this study. They concluded that transforaminal pain ESI can offer significant pain reduction in the short term and long term for discogenic pain; however study was limited due to small sample size. In addition the study failed to include functional measures as one of their outcome measures, an important indicator of therapeutic success.
Effectiveness: This was the only study looking at TFESI for discogenic back pain however patients with both leg and back pain were included. Given this, the results showed short term benefits but conclusions regarding the utility of TFESI in the management of axial pain based on this study cannot be confirmed.
Transforaminal and Interlaminar Epidural Steroid Injection: Table 4 illustrated the details of studies looking at the effectiveness of lumbar transforaminal or interlaminar epidural injections for discogenic pain. Only one study met the inclusion criteria.
Study/Methods
Participants
Intervention(s)
Outcome(s)
Result(s)
Conclusion(s)
Buttermann (2003)
(19)
Non-Randomized controlled trial
232 patients with low back pain due to DJD for 1 year treated with ESI (interlaminar and transforaminal).
Patients stratified by the presence or lack off endplate changes.
Betamethasone
Total number of injections = 1-2
Timing: 1-3 mos, 4-6mos, 7-12 mos, 1-2 years
Outcome measures: VAS, ODI, Pain Diagram, opinion of success
VAS went from ~6.75 � 4.75 and ODI 47 �35 at 2 year follow up
Positive short term benefit in 25% of patients with inflamtory end -plate changes causing discogenic pain.
Table 4: Details of trials studying the effectiveness of lumbar transforaminal ESI or interlaminar ESI on discogenic pain.
Buttermann et al. aimed to determine the effect of spinal steroid injections for axial low back pain resulting from lumbar degenerative disc disease (DDD). ESI were performed in 232 patients with betamethasone and outcome measures were visual analog score (VAS), Oswestry disability index (ODI) and a pain diagram at 1-3 months, 4-6 months, 7-12 months and 1-2 years. This study simultaneously looked at patients who had undergone epidural steroid injections as well as those who had discograms without or without intradiscal steroids. The data was kept separate amongst the groups and only those undergoing ESI were used in this analysis. The greatest flaw of this study is that the paper does not specifically stratify those patients undergoing TFESI vs ILESI. All ESI were grouped into one category thus making it difficult to include this only as a study for ILESI. The authors concluded improved pain and function at short term follow up however results are not clear. The percentage improvement in VAS or ODI is not mentioned and therefore no conclusions can be made based on the results of this study. In addition this study they had a high dropout rate (51%) as well as an increased number of patient requiring surgical fusions.
Level of Evidence: The evidence based on the USPSTF is level II-2 for ILESI for short term pain relief for lumbar discogenic back pain. The evidence is level III for TFESI for short term pain relief for lumbar discogenic back pain (Table 5) [29].
Interlaminar Studies
Level of Evidence
Manchikanti et al (2012) [23]
I
Buttermann (2003) [19]
II-2
Lee et al (2010) [20]
II-3
Overall
II-2
Transforaminal Studies
Rosenberg et al (2002) [21]
III
Overall
III
Table 5: Individual Studies Level of Evidence and Grading Recommendations.
Discussion
This review evaluating the efficacy of lumbar TFESI and ILESI in patients with lumbar discogenic pain without radiculitis indicated Level II-2 evidence for interlaminar epidural injections and level III for transforaminal epidural injections. In this review, 1 randomized trial and 3 observational studies were included in assessing the effectiveness in discogenic pain. We were able to find only 1 randomized trial that met criteria for inclusion evaluating the role of ILESI or TFESI in managing pain of disc origin.
The current review shows that transforaminal epidural steroid injections in the treatment of discogenic pain can result in 68% pain relief at 2 months, 56% at 6 months and 59% at 12 months [21]. The relative low risk and potential effectiveness of transforaminal epidural steroid injections in the treatment of discogenic pain make this a viable treatment choice for patients [22].
This review reveals common limitations among the reviewed studies of small sample size and inconsistent methodology for diagnosing discogenic back pain. Manchikanti et al. had an adequate study size of 120 patients when compared to the other studies however did not include differences in baseline demographic characteristics with respect to weight and sex [23]. In addition discogenic back pain was diagnosed by symptoms without specific MRI findings, another limitation of the study. However, they were able to exclude patients with facet and sacroiliac joint involvement with diagnostic anesthetic blocks unlike the other studies [18]. Butterman et. al in their non-randomized control trial treated degenerative disc disease in 232 patients with ESI using the interlaminar approach and used discography with or without intradiscal steroids to diagnosis patients with discogenic pain [19]. Lee et all was limited by using a non-validated paraspinal compression maneuver to treat patients with axial low back pain. In addition they failed to identify the pain generator of lower back pain they intended to treat (ie. discogenic, facet joint, and sacroiliac joint) which could have led to inaccurate targeted intervention [20]. They excluded patients with bilateral pain symptoms (often present in patients with discogenic pain) due to the non-specificity in the physical exam maneuver and pain induced by the maneuver itself. In the study performed by Rosenberg et al. discogenic back pain was diagnosed exclusively by MRI findings (disc herniation, bulging discs or degenerative disc disease) [21].
Further, in this study we have shown studies indicating the benefit of epidural steroid injections for discogenic lumbar back pain for short term pain relief [24]. However, these conclusions need further evaluation with more randomized control trials as only one study showed a long term benefit with an interlaminar approach [18].
The interlaminar approach allows greater dispersion over a greater area as compared to the transforaminal approach [25]. TFESI have also been referred as either diagnostic or therapeutic selective nerve root blocks (SNRBs). SNRBs deliver the medication directly into the space around the involved nerve root and in the case of TFESI it has been speculated that the use high volumes of injectate can make the procedure "non-selective". A study by Furman et al. investigated thirty patients undergoing TFESI with the goal of determining the minimum amount of contrast flow necessary to consider the procedure "selective" for the specified nerve root level. The patients were injected with contrast dye in 0.5mL intervals and using fluoroscopy it was documented when contrast extended either to a superior or inferior spinal segment or crossed the midline spine to the contralateral side. Results of this study showed that 30% of TFESI were no longer "selective" after 0.5mL, this percentage increased to 67% with 1.0mL, 87% with 1.5mL and 90% with 2.5mL [26-28]. Based on this study it can be surmised that TFESI may be as effective for bilateral or multilevel symptoms when compared to ILESI.
The correct diagnosis and treatment of axial LBP are still challenging. Provocation discography was known to be the best diagnostic method for discogenic LBP, but there is a still debate about the role of provocation discography for the diagnosis of discogenic LBP. In addition, to the author's knowledge, this is one of the first reviews evaluating the effectiveness of transforaminal and interlaminar epidural steroid injections for the management of lumbar discogenic pain without radicular symptoms. The results of this review may be applied to interventional pain practices however the differences between transforaminal vs interlaminar epidural steroid injections are not significantly different based on the studies contained in this review.
Conclusion
The results of this review are provided utilizing contemporary review methodology utilizing randomized trials and observational studies, even though most of the evidence was derived from observational studies. Randomized trials utilizing a consistent definition of discogenic pain and clear outcome measures must be examined to further promote research in this area.
References
- Rosenberg SK, Grabinsky A, Kooser C, Boswell MV. Effectiveness of transforaminal epidural steroid injections in low back pain: a one year experience. Pain Physician. 2002; 5: 266-270.
- Cassidy JD, Carroll LJ, Côté P. The Saskatchewan health and back pain survey. The prevalence of low back pain and related disability in Saskatchewan adults. Spine (Phila Pa 1976). 1998; 23: 1860-1866.
- Guo HR, Tanaka S, Halperin WE, Cameron LL . Back pain prevalence in US industry and estimates of lost workdays. Am J Public Health. 1999; 89: 1029-1035.
- Lu Y, Guzman JZ, Purmessur D, Iatridis JC, Hecht AC, Qureshi SA, et al. Nonoperative management of discogenic back pain: a systematic review. Spine (Phila Pa 1976). 2014; 39: 1314-1324.
- Schwarzer AC, Aprill CN, Derby R, Fortin J, Kine G, Bogduk N. The prevalence and clinical features of internal disc disruption in patients with chronic low back pain. Spine (Phila Pa 1976). 1995; 20: 1878-1883.
- Friedly J, Chan L, Deyo R. Increases in lumbosacral injections in the medicare population. Spine (2007). Volume 32, Number 16, pp 1754-1760
- el-Khoury GY, Ehara S, Weinstein JN, Montgomery WJ, Kathol MH. Epidural steroid injection: a procedure ideally performed with fluoroscopic control. Radiology. 1988; 168: 554-557.
- Banaszkiewicz PA, Kader D, Wardlaw D. The role of caudal epidural injections in the management of low back pain. Bull Hosp Jt Dis. 2003; 61: 127-131.
- Buttermann GR. The effect of spinal steroid injections for degenerative disc disease. Spine J. 2004; 4: 495-505.
- Gharibo C, Varlotta G, Rhame E, Liu E, Bendo J, Perloff M. Interlaminar verses transforaminal epidural steroids for the treatment of subacute lumbar radicular pain: A randomized, blinded, Prospective Outcome study. Pain Physician (2011); 14: 449-511
- Ackerman WE 3rd, Ahmad M . The efficacy of lumbar epidural steroid injections in patients with lumbar disc herniations. Anesth Analg. 2007; 104: 1217-1222, tables of contents.
- Kuraishi Y, Hirota N, Sato Y, Hino Y, Satoh M, Takagi H . Evidence that substance P and somatostatin transmit separate information related to pain in the spinal dorsal horn. Brain Res. 1985; 325: 294-298.
- Derby R, Kine G, Saal JA, Reynolds J, Goldthwaite N, White AH, et al. Response to steroid and duration of radicular pain as predictors of surgical outcome. Spine (Phila Pa 1976). 1992; 17: S176-183.
- Parr AT, Diwan S, Abdi S . Lumbar interlaminar epidural injections in managing chronic low back and lower extremity pain: a systematic review. Pain Physician. 2009; 12: 163-188.
- Carragee EJ, Tanner CM, Khurana S, Hayward C, Welsh J, Date E, et al. The rates of false-positive lumbar discography in select patients without low back symptoms. Spine 2000; 25:1373-1380; discussion 1381.
- Carragee EJ, Barcohana B, Alamin T, van den Haak E . Prospective controlled study of the development of lower back pain in previously asymptomatic subjects undergoing experimental discography. Spine (Phila Pa 1976). 2004; 29: 1112-1117.
- Wetzel FT, LaRocca SH, Lowery GL, Aprill CN. The treatment of lumbar spinal pain syndromes diagnosed by discography. Lumbar arthrodesis. Spine (Phila Pa 1976). 1994; 19: 792-800.
- Manchikanti L, Cash KA, McManus CD, Pampati V, Benyamin RM. Preliminary results of a randomized, double-blind, controlled trial of fluoroscopic lumbar interlaminar epidural injections in managing chronic lumbar discogenic pain without disc herniation or radiculitis. Pain Physician 2010; 13: E279-E292.
- Buttermann GR. The effect of spinal steroid injections for degenerative disc disease. Spine J. 2004; 4: 495-505.
- Lee JW, Shin HI, Park SY, Lee GY, Kang HS. Therapeutic trial of fluoroscopic interlaminar epidural steroid injection for axial low back pain: effectiveness and outcome predictors. AJNR Am J Neuroradiol. 2010; 31: 1817-1823.
- Rosenberg SK, Grabinsky A, Kooser C, Boswell MV . Effectiveness of transforaminal epidural steroid injections in low back pain: a one year experience. Pain Physician. 2002; 5: 266-270.
- Goodman BS, Posecion LW, Mallempati S, Bayazitoglu M . Complications and pitfalls of lumbar interlaminar and transforaminal epidural injections. Curr Rev Musculoskelet Med. 2008; 1: 212-222.
- Manchikanti L, Malla Y, et al. A Prospective Evaluation of Complications of 100,00 Fluoroscopically Directed Epidural Injections. Pain Physician 2012; 15:131-140.
- Glaser SE, Shah RV . Root cause analysis of paraplegia following transforaminal epidural steroid injections: the 'unsafe' triangle. Pain Physician. 2010; 13: 237-244.
- Candido A, Raghavendra, M, et al. Aprospective evaluation of iodinated contrast flow patterns with fluoroscopically guided lumbar epidural steroid injections: the lateral parasagittal interlaminar epidural approach versus the transforaminal epidural approach. Anesth Analg. 2008 Feb;106: 638-644.
- Furman MB, Lee TS, Mehta A, Simon JI, Cano WG. Contrast flow selectivity during transforaminal lumbosacral epidural steroid injections. Pain Physician. 2008; 11: 855-861.
- ROBECCHI A, CAPRA R. [Hydrocortisone (compound F); first clinical experiments in the field of rheumatology]. Minerva Med. 1952; 43: 1259-1263.
- Manchikanti L . Role of neuraxial steroids in interventional pain management. Pain Physician. 2002; 5: 182-199.
- Berg AO, Allan JD. Introducing the third U.S. Preventive Services Task Force. Am J Prev Med 2001; 20: S3-S4.