
Special Article : Stroke Rehabilitation
Phys Med Rehabil Int. 2015;2(1): 5.
A Liaison Critical Pathway for Stroke Rehabilitation: Current Status and Features of Western District of Saitama in Japan
Shinichiro Maeshima1*, Aiko Osawa1 and Norio Tanahashi2
1Department of Rehabilitation Medicine, Saitama Medical University International Medical Center, Japan
2Department of Neurology, Saitama Medical University International Medical Center, Japan
*Corresponding author: Shinichiro Maeshima, Department of Rehabilitation Medicine II, School of Medicine, Fujita Health University, Japan
Received: December 03, 2014; Accepted: December 26,2014; Published: January 05, 2014
Abstract
In Japan, division of functions among medical institutions has been promoted as a national policy and a liaison critical pathway (LCP) communitybased has been promoted for stroke treatment. We examined our 3-year experience with operation of such a LCP and its effects from the perspectives of an acute care hospital. We examined the contents of 819 LCP forms returned from the cooperation hospitals during the 3-year period and we investigated changes in activities of daily living, duration of hospital stay, outcomes and compared differences in functional outcomes among the cooperation hospitals. Based on comparison by year, no difference was observed in duration of hospital stay, functional independence measure (FIM) scores on admission and at discharge, FIM gain, the rate of discharge to home during the 3-year period, or FIM efficiency improved in the third year. Based on comparison among the hospitals, there were differences in length of stay, FIM scores on admission and at discharge, FIM gain, FIM efficiency and rate of discharge to home among the cooperation hospitals. The LCP is a valuable tool that promotes closer cooperation among medical institutions and allows them to obtain patient information easily. Reducing incomplete entries and providing feedback on variations in functional assessment results to each cooperation hospital should allow qualitative improvement of rehabilitation services to be attempted.
Keywords: Stroke care; Rehabilitation; Critical pathway; Activities of daily living
Abbreviations
LCP: Liaison Critical Pathway; FIM: Functional Independence Measure; ADL: Activities of Daily Living; mRS: modified Rankin Scale
Introduction
Medical care for stroke has been greatly transformed by improvements in emergency medical systems [1], advancements in treatments, such as thrombolytic therapy [2,3] and neuro endovascular therapy [4], team-based medicine at the stroke unit [5], guidelines for stroke treatment [6] and so on. Meanwhile, the Japanese medical system has changed remarkably since the beginning of this century [7]. In an effort to promote "division of functions among medical institutions," the Diagnosis Procedure Combination (prospective payment system) was introduced [8]. As a result, acute and chronic care hospitals were clearly distinguished by indices, such as mean duration of hospital stay and referral rate. The nursing care insurance system and the convalescence rehabilitation ward were also introduced. Furthermore, the basic framework of the medical programs was recently included in the Medical Service Law and policies to achieve functional division and cooperation among medical institutions, seamless continuation of medical care and early return to life at home were developed [9,10]. With such a social background, the "community-based liaison critical pathway (LCP)" is drawing attention as a path from an acute care hospital through a convalescence rehabilitation ward/hospital to home. Although the critical pathway [11] has been introduced on a hospital-by-hospital basis in the past, functional division and cooperation among medical institutions in each region are necessary for efficient medical care. The LCP began to be integrated into the Japanese medical system a few years ago. However, little is known about efficacy and problem on that medical system using the LCP generally. From the perspective of an acute care hospital engaging in rehabilitation, we would like to discuss our experience with 3-year operation of the LCP and its effects, as well as the position and role of the acute care hospital in this system.
Materials and Methods
Community medical program and LCP for stroke
In Saitama Prefecture, with a population of 7 million people, there are 18 healthcare management hospitals (acute care hospitals) registered as medical institutions engaging in the medical service system for stroke and 28 community cooperation participating hospitals (cooperation hospitals) with convalescence rehabilitation wards. At the acute care hospital, a treatment plan form (LCP for stroke) is prepared [12] by attending physician and nurses according to the LCP within 7 days after a patient is hospitalized. The treatment plan is explained, and provided to the patient and family members in written form. Then, the acute care hospital becomes eligible to receive medical treatment fees. At the cooperation hospital, the information on the LCP form brought by the patient is checked. After the form has been filled out with the provided rehabilitation services and patient status at discharge, it is returned to the acute care hospital. However, if the patient is still hospitalized after the hospital stay limit (180 days), medical treatment fee for the LCP will not be reimbursed. Meetings are regularly held for information exchange approximately 3 times a year. The necessary agenda is to share clinical information and to confirm whether assessment and revision of the cooperation path are appropriately performed. Furthermore, our hospital holds conferences and lectures annually with the staff of the hospitals in our neighboring regions. By presenting data using the LCP on stroke treatment and the rehabilitation services provided to patients, we are also providing educational opportunities.
Liaison clinical pathway and flow of patients
At the acute care hospital, the following items are given in the LCP form in addition to basic information, such as date of onset and disease name: neurological symptoms, details of drug treatment, the presence or absence of behavioral problems, explanation of prognosis, date of discharge, daily living functional assessment at discharge, activities of daily living (ADL) assessed with the functional independence measure (FIM) [13], modified Rankin Scale (mRS) [14] and eating conditions. In the procedure to transfer a patient from the acute care hospital, a medical social worker who receives a request from the doctor in charge of the patient informs several convalescence rehabilitation hospitals near the residential area of the patient. The patient's family members directly visit those hospitals and decide which hospital the patient will be transferred to. Then, the patient is transferred from the acute care hospital to the cooperation hospital with the referral and LCP forms.
At the cooperation hospital, the LCP form, brought by the patient, is filled out with the following items: ADL or eating conditions on admission and at discharge, mRS at discharge, daily living functional assessment, independence degree of daily living for the disabled and demented elderly, date of discharge and outcome after discharge. After the patient is discharged, the form is sent to the acute care hospital by mail.
In this study, we reviewed all patients who underwent rehabilitation at our hospital and were then transferred to cooperation hospitals with LCP forms.
Patients
During 3 years of operating the LCP (July 2008 to June 2011), there were 2, 241 stroke patients for whom rehabilitation was requested. This study involved 819 of these patients (36.5%) who were transferred to cooperation hospitals with convalescence rehabilitation wards along the LCP of Saitama Prefecture. The ages ranged from 11 to 98 (69.9 ± 12.4) years. There were 516 men and 303 women. The primary diseases included cerebral infarction in 378 patients, intracranial hemorrhage in 353, sub arachnoid hemorrhage in 78 and other cerebrovascular disorders in 10. The time from onset to the start of rehabilitation was 3.0 ± 4.6 days and the mean duration of hospital stay was 33.8 ± 16.1 days.
Procedure
When the LCP forms were not returned by 6 months after patients had been transferred from the acute care hospitals, the staff of the regional liaison office contacted the cooperation hospitals by telephone or facsimile to urge them to return the forms and to ascertain the reasons for not returning them. Then, we examined the contents of returned forms in ADL, duration of hospital stay, outcomes, etc., at the cooperation hospital during the 3-year period. Differences in functional outcomes were also compared among 6 cooperation hospitals returning 10 or more LCP forms.
Statistical analysis
Data were statistically analyzed using Kruskal-Wallis tests and chi-square tests. Significance was set at the p<0.05 level. Statistical analyses were performed using the JMP version 8.02 for Macintosh software (SAS Institute Inc., Cary, NC, USA).
Results
Status of collection and entries of the LCP forms
The ultimate collection rate of the LCP forms prepared during the 3-year period was 78.6% (644 patients). The reasons for the LCP forms of the remaining 175 patients not being collected from the cooperation hospitals were as follows: 64 patients (36.6%) were "not admitted to the convalescence rehabilitation ward but rather to another ward (sanatorium) on admission"; 13 patients (7.4%) were "transferred to another hospital due to acute deterioration in their conditions"; 9 patients (5.1%) were "transferred from the convalescence rehabilitation ward to another ward (medical care type)"; "the duration of stay at the convalescence rehabilitation ward exceeded the computation period (6 months)" in 9 patients (5.1%); 6 patients (3.4%) "died"; 14 patients (9.7%) did "not bring their LCP forms" and the reason was "unknown or no reply" in 60 patients (34.3%).
Functional improvement and outcomes at convalescence rehabilitation wards
The time from admission to our hospital to transfer to the convalescence rehabilitation hospitals (duration of stay at the acute care hospital) was 33.8± 16.1 (median: 31, range: 3-158) days. The FIM scores on admission to the cooperation hospitals were 66.1± 33.6 (median: 67, range: 18-126). The FIM scores at discharge from the cooperation hospitals were 95.9± 29.8 (median: 107, range: 18-126). The FIM gain (FIM score at discharge - FIM score on admission) was 29.6± 23.3 (median: 25, range: -24 to 109). The mean duration of hospital stay was 97.1± 59.3 days (median: 90, range: 3-317). The FIM efficiency (FIM gain/duration of hospital stay) was 0.41 ± 0.42 (median: 0.31, range:-0.44-3.55).
We compared 6 cooperation hospitals returning 10 or more LCP forms. A difference was observed in duration of hospital stay among the acute care hospitals, and there were differences in duration of hospital stay, FIM scores on admission and at discharge, FIM gain, FIM efficiency and rate of discharge to home among the cooperation hospitals (Table 1).
Hospital A
N=129
Hospital B
N=206
Hospital C
N=22
Hospital D
N=95
Hospital E
N=277
Hospital F
N=68
df
P value
Duration at acute hospital (days)
34 (6-96)
34 (8-135)
30.5 (13-50)
35 (14-81)
25 (3-158)
31 (10-78)
5
<0.0001
FIM scores on admission
57
(8-121)
63
(15-120)
62.5
(25-116)
60
(17-124)
80
(18-126)
57
(18-116)
5
0.0036
FIM scores at discharge
107.5
(18-126)
107
(18-126)
102
(53-123)
103
(21-126)
112
(18-126)
96
(19-126)
5
0.0368
FIM gain
32
(-97-109)
26
(-79-97)
27.5
(-55-55)
24
(-41-84)
20
(-18-105)
19.5
(-83-85)
5
0.0169
LOS in cooperation hospitals (days)
146
(10-317)
106
(12-247)
92
(17-157)
152
(28-280)
45
(7-177)
103
(19-172)
5
<0.0001
FIM efficiency
0.28
(-0.01-3.52)
0.26
(-2.72-2.19)
0.31
(-0.06-0.829
0.22
(-0.11-0.75)
0.43
(-0.44-3.55)
0.3
(0-1.06)
5
<0.0001
Rate of discharge to home (%)*
79.0
61.4
95.2
72.8
84.7
70.6
5
<0.0001
FIM, functional independence measure; LOS, length of stay Median (range).
Kruskal-Wallis test for no difference in correspondence between groups. *Chi-square test was also used to compare among the rate of discharge to home. (Chi-square=31.35, df=5, p<0.0001).
Table 1: Comparison of LOS, FIM scores, and rates of discharge to home among hospitals.
Comparison of the 3-year period
According to comparisons among years comprising the 3-year period, the collection rate of the LCP forms decreased in the second year but improved in the third year (Figure 1). Duration of hospital stay gradually increased in the acute care hospitals. In the cooperation hospitals, no difference was observed in duration of hospital stay, FIM scores on admission and at discharge, FIM gain, or the rate of discharge to home during the 3 years or FIM efficiency improved in the third year (Table 2).
July 2008-June 2009
N=243
July 2009-June 2010
N=266
July 2010-June 2011
N=310
df
P value
Duration at acute hospital (days)
28 (3-76)
32 (7-122)
33 (7-158)
2
0.0004
FIM scores on admission
66 (17-126)
67.5 (18-126)
66.5 (8-124)
2
0.3677
FIM scores at discharge
105 (12-126)
108 (18-126)
107 (18-126)
2
0.2197
FIM gain
24 (-97-97)
28.5 (12-91)
24 (-55-109)
2
0.3784
LOS in cooperation hospitals (days)
101 (3-317)
86 (7-248)
87 (8-280)
2
0.1930
FIM efficiency
0.24 (-2.72-2.5)
0.33 (-0.44-2.4)
0.33 (-0.17-3.5)
2
0.0454
Rate of discharge to home (%)*
71.9
74.9
79.8
2
0.1389
FIM, functional independence measure; LOS, length of stay Median (range).
Kruskal-Wallis test for no difference in correspondence between groups. *Chi-square test was also used to compare among the rate of discharge to home.
Table 2: Comparison of LOS, FIM scores and rates of discharge to home during 3 years.
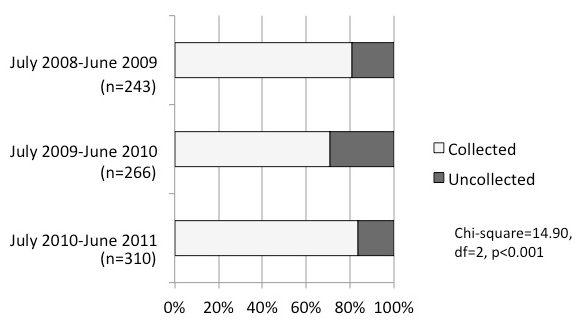
Figure 1: Collection rate of the LCP during 3 years.
Discussion
Although use of the LCP by medical professionals does not improve the conditions of patients, this path allows them to receive continuous treatment from the acute care hospital through the convalescence rehabilitation hospital and finally to their homes. By using the path, the acute care hospitals can easily obtain information on functional and other outcomes of patients transferred to cooperation hospitals and the cooperation hospitals can obtain detailed information on conditions of patients during stays at their previous hospitals [15].
Meanwhile, because treatment plans and overall procedures which have been determined at the discretion of individual doctors on a hospital-by-hospital basis are standardized, the LCP requires standardization of documentation and assessment methods. The LCP with fixed entry items may serve as a valuable tool for resolving problems after stroke. The entry items of the LCP developed in our region are simplified so that even personnel who are not familiar with rehabilitation can readily understand them. The path does not require any description of difficult technical terms or therapies. Thus, its merit is the ease of completing the LCP form. However, because there are no items pertaining to the progress of rehabilitation, patient background, or life before disease onset, we will struggle for reform the LCP which can provide enough information to allow appropriate rehabilitation services to be offered at cooperation hospitals in near future. Meanwhile, there were patients who had to be admitted to a sanatorium because their conditions did not allow aggressive rehabilitation although the patients were transferred with the expectation of being admitted to a convalescence rehabilitation ward, those who could not be discharged to home but were transferred to nursing facilities and those who acutely deteriorated or died a few days after transfer. These patients who should probably not have been transferred to convalescence rehabilitation hospitals under normal circumstances accounted for at least 10%. We advocate that the conditions and indications for transfer be reviewed.
Regarding incomplete entries of the LCP forms by the cooperation hospitals, the commonly missing items were prognosis and outcomes. Our study also revealed the following present conditions: there are only a few cooperation hospitals with certified specialists in not only stroke treatment but also rehabilitation; management of stroke patients is insufficient; and regular functional assessment is not performed. Promotion of the LCP is often considered to reduce the duration of stay at the acute hospital [16]. However, introduction of the LCP into our institutions did not affect the duration of stay at the acute hospitals. Instead, the duration was prolonged at 3 years. This may be attributable to the following factors. Because there are few specialists in either rehabilitation or stroke treatment at the cooperation hospitals in our region, it is difficult to handle patients with especially severe disorders or those requiring continuation of stroke treatment. In addition, because costs for drugs, blood test and X-rays exams during admission to the convalescence rehabilitation ward are included in the fee for the hospital visit, the cooperation hospitals also strive to reduce these costs as much as possible. Thus, dialysis patients and that receiving mechanical ventilator support are not admitted to the convalescence rehabilitation ward. We also considered the possibility that there may be influences of the following conditions: patients with complications, such as pneumonia, urinary tract infection and hemorrhagic infarction, cannot be transferred until their systemic conditions are stabilized and treatments such as anticoagulant, anti arrhythmic and antihypertensive drugs are difficult to administer and maintain at many cooperation hospitals without specialists.
As a feature facilitating rehabilitation, introduction of the LCP allowed the acute care hospitals to obtain information on patients transferred to the convalescence rehabilitation ward regarding functional outcomes and places to which the patients were moved after discharge from the ward.
Although there was no difference in FIM scores on admission and mean duration of hospital stay between data in our region and the annual report of the Japan Convalescence Rehabilitation Liaison Council [16], FIM scores at discharge and FIM gain in our region were higher than those in the annual report. FIM efficiency in our region greatly exceeded that in the annual report. This may be attributable to some cooperation hospitals having provided excellent rehabilitation services. In addition, risk management and early treatment were prioritized at the acute care hospitals and many patients were transferred to the convalescence rehabilitation hospitals without receiving adequate rehabilitation. Thus, marked improvement in daily living functional assessment and so on, might have been prompted when patient conditions stabilized after transfer. Furthermore, qualitative differences among the convalescence rehabilitation hospitals were revealed in terms of duration of hospital stay and FIM efficiency. Due to regional characteristics and individuality based on association with other institutions and so on, differences among the convalescence rehabilitation hospitals are likely to occur in hospitalized patient populations and among therapeutic strategies.
In this study, patient attributes, concomitant diseases, early dysfunction, ADL, social background factors, and so on, were not controlled and the cooperation hospitals had sole discretion regarding the quality of rehabilitation services provided after transfer. Nevertheless, it is not legally problematic that specialists in stroke treatment or rehabilitation are not always present at convalescence rehabilitation wards. As patients are hospitalized longer, hospitals receive more medical treatment fees. This aspect of the healthcare insurance system is speculated to reduce the quality of rehabilitation services. If patients are hospitalized for a long period, they and their families will lose motivation to return to society. In order to help stroke patients return to meaningful and enjoyable lives as early as possible, we consider it necessary to attempt to improve the quality of rehabilitation services by providing feedback on characteristics of each hospital obtained in this study.
Anyway, the collection rate of the LCP forms from the cooperation hospitals was approximately 80% and was highest in the third year. This may be attributable to the regional liaison office urging the cooperation hospitals to participate fully and that cooperation among hospitals was strengthened through study sessions, and so on. We suggest that, to improve the prognosis of stroke after rehabilitation, the continuous effort is important to strengthen the liaison network with LCP.
Conclusion
Reducing incomplete entries and providing feedback on variations in functional assessment results to each cooperation hospital should allow qualitative improvement of rehabilitation services to be attempted. The LCP is a valuable tool that promotes closer cooperation among medical institutions and allows them to obtain patient information easily.
Acknowledgements
We would like to express our deepest gratitude to Mr. Hiroshi Arai, the staff of the regional liaison office who contacted the cooperation hospitals.
References
- Albright KC, Branas CC, Meyer BC, Matherne-Meyer DE, Zivin JA, Lyden PD, et al. ACCESS: acute cerebrovascular care in emergency stroke systems. Arch Neurol. 2010; 67: 1210-1218.
- [No authors listed]. Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. N Engl J Med. 1995; 333: 1581-1587.
- Yamaguchi T, Mori E, Minematsu K, Nakagawara J, Hashi K, Saito I, et al. Japan Alteplase Clinical Trial (J-ACT) Group. Alteplase at 0.6 mg/kg for acute ischemic stroke within 3 hours of onset: Japan Alteplase Clinical Trial (J-ACT). Stroke. 2006; 37: 1810-1915.
- Meyers PM, Schumacher HC, Connolly ES Jr, Heyer EJ, Gray WA, Higashida RT. Current status of endovascular stroke treatment. Circulation. 2011; 123: 2591-2601.
- Tan KM, Austin B, Shaughnessy M, McDonald M, O'Keeffe S, Mulkerrin EC . An audit of the impact of implementation of a stroke care pathway in an acute teaching hospital. Ir J Med Sci. 2007; 176: 75-79.
- Shinohara Y. Japanese guidelines for the management of stroke 2009.J Stroke Cerebrovasc Dis. 2011; 20 (Suppl): S1-S209.
- Hashimoto Y, Watanabe S, Hirata Y, Hirano T. Referral system and liaison critical pathway for stroke. Jpn J Stroke. 2009; 31: 491-496.
- Ministry of Health, Labour and Welfare. Draft Policy on Structural Reform of the Medical System. October 19, 2005.
- Ministry of Health, Labour and Welfare. The Fifth Medical Service Law Amendment. April 1, 2007.
- Miyai I, Sonoda S, Nagai S, Takayama Y, Inoue Y, Kakehi A, et al. Results of new policies for inpatient rehabilitation coverge in Japan. Neurorehabil Neural Repair. 2011; 25: 540-547.
- Cooper D, Jauch E, Flaherty ML. Critical pathways for the management of stroke and intracerebral hemorrhage: a survey of US hospitals. Crit Pathw Cardiol. 2007; 6: 18-23.
- Saitama Medical Association: Liaison critical pathway for stroke in Saitama prefecture. https://saitama-cvd.com/download.html. accessed March 3, 2012.
- Granger CV, Hamilton BB, Linacre JM, Heinemann AW, Wright BD . Performance profiles of the functional independence measure. Am J Phys Med Rehabil. 1993; 72: 84-89.
- van Swieten JC, Koudstaal PJ, Visser MC, Schouten HJ, van Gijn J . Interobserver agreement for the assessment of handicap in stroke patients. Stroke. 1988; 19: 604-607.
- Tokunaga M, Watanabe S, Hirano T, Hirata Y, Hashimoto Y, Yanagida H. A survey of the medical record data fields used for cerebral infarction patients in the course of designing a liaison-critical pathway. Jpn J Rehabil Med. 2006; 43: 834-838.
- Kaifukuki Rehabilitation Ward Associations: 2001-2008 Multi-year Report from the Annual Survey Committee of Kaifukuki Rehabilitation Ward Assosiation. 2009; 48-49.