
Special Article - Stroke Rehabilitation
Phys Med Rehabil Int. 2015;2(6): 1054.
Which is the Best Way to Assess and Follow-Up Fitness to Drive after Stroke?
Björkdahl A1,2,3*, Nilsson L¹ and Jönsson U¹
1Sahlgrenska University hospital, Sweden
2Gothenburg University, Sahlgrenska Academy, Neuroscience and Physiology, Rehabilitation medicine, Sweden
3Ersta Sköndal University College, Campus Bräcke, Sweden
*Corresponding author: Ann Björkdahl, Ersta Sköndal University College, Campus Bräcke, Box 21062, 41804 Gothenburg, Swedan
Received: June 15, 2015; Accepted: July 23, 2015; Published: July 27, 2015
Abstract
Aim: To explore the feasibility to make on-road assessments routinely at 3 months follow-up for all patients with a 3 months verbal prohibition of driving after stroke, to support the physicians decision of fitness to drive.
Methods: From September 2007 to December 2009 there were 151 stroke patients from the stroke units at the hospital eligible for inclusion in the study. Fifty agreed to be assessed by the Nordic Stroke Driver Screening Assessment (NorSDSA) and on-road assessment. As base for discussion about the consequences on resource use relative to accuracy, calculations were made to explore and compare an expected yearly cost for two different assessment conditions, the NorSDSA followed by on-road assessment in uncertain cases and on-road assessment for all cases.
Findings: The yearly need for driving assessments was estimated to 500 patients. With less accuracy than only on-road assessments the NorSDSA with the stipulated cut-off produced a cost benefit of 1,700 €. The NorSDSA resulted in 32% uncertain cases and the certain cases were in 17% in disagreement with the on-road assessment, the gold standard.
Conclusion: It is conceivable and could be recommended to make on-road assessments for all patients with stroke at 3 months follow-up as accuracy is of importance both for patients and society and may save resources in the long run.
Keywords: Driving; Cognitive impairment; Screening; Cost effective; NorSDSA; On-road
Introduction
Many of the persons who survive a stroke are drivers [1]. Since a stroke can affect fitness to drive, physicians are obliged, by Swedish law to determine whether the patient can be allowed to drive after the injury. All patients not fit to drive should be reported to the Swedish Transport Agency that confiscate their driving license. However, as recovery may occur after stroke the Swedish National Guidelines for stroke recommend that the physician discuss driving with all patients before discharge from hospital and make a verbal agreement, with the patients that wish to resume driving, to refrain from driving during a period of 3-6 months. In too many cases there is a lack of compliance with the guidelines and no discussion and decision regarding driving is made. Similar problems seem to be present in many countries according to the report from Fisk et al. [2] indicating that nearly 90% of the stroke drivers do not receive any type of driving evaluation. A reason for the lack of decisions regarding driving after stroke may be that many physicians feel that they are poorly informed and trained in terms of assessing driving fitness [3-5]. In Sweden in some cases the patient gets a verbal prohibition of driving for 3 months at discharge from hospital but follow-up of the agreement with a new decision failure. With this background there is a need for practical and explicit routines on how to handle the issue of driving after stroke in order to facilitate the obligatory duty of the physician as well as make information and procedures clear and equal for all patients.
Driving is a complex activity that requires sufficient attention, perception, and information processing. All of these functions can be affected by a brain injury [1, 6]. To handle complex situations in traffic, driving requires rapid judgments, automatic reactions, and flexibility. It can be difficult for a physician to assess these abilities during a short clinical examination. In many countries there are special driving assessment centers. Sweden does not have that organisation and there are only few official centers for traffic medicine. Since there is a need for evaluations made by professionals with knowledge in traffic medicine, every region, hospital or care centre tries to organise their own routines for how to decide on fitness to drive.
After a stroke the physician, following the National guidelines, should make an agreement with all patients that are drivers to refrain from driving during 3 months, which is clear and easy. At time to decide if there should be a permanent prohibition or the patient should be allowed to resume driving after 3 months it is more problematic. Due to the complex situations that can be encountered during driving and the interacting abilities that are needed to deal with these situations, there is currently no universal, standardised way to assess fitness to drive [7, 8]. The available instruments seldom comprise items for the entire range of situations encountered during driving, which can range from simple to complex [9]. Different assessments also have different levels of ecological validity. In this case, the term ecological validity means the extent to which the assessment reflects a person’s true fitness to drive. There is evidence in the literature that suggests that assessments in real traffic with skilled evaluators have better ecological validity than neuropsychological assessments in a clinic [7, 10]. At present, the on-road assessment is the most accepted method for determining fitness to drive, although the methods have not been standardised [10, 11]. Consequently, the on-road assessment is often used as the gold standard.
However, other factors such as resource utilisation may also shape the choice of assessment method and on-road assessment is relatively time consuming and need collaboration with a driving school. Therefore, the ideal situation would be to have screening methods that allow the identification of cases that need a more thorough examination [12]. The Nordic Stroke Driving Screening Assessment (NorSDSA) is widely used in Sweden and specifically designed for assessing driving. It has been found to be one of the available tests that best reflect fitness to drive [13]. In spite of this, these kinds of tests are limited, and a study by Selander et al.[14] conclude that the NorSDSA should not be used as a stand-alone test to determine the fitness to drive of individuals, which is the most common way in Sweden [15].
From the perspective of the stroke driver, evaluations and information about driving after stroke is unclear and with unexpected results according to their self-appraisal and a decision to cease driving disrupt ability to participate in meaningful activities [16].
Given the above aspects of problems with routines, evaluations and information it is important to explore possible solutions to improve routines for the physicians, accuracy in evaluations and understanding of the patient for the decisions that are made. As onroad assessment has been found to be the most ecologically valid way to examine fitness to drive and yet not is the standard evaluation, it would be of interest to explore if it would be feasible and appropriate to use the on-road assessment routinely. Probably the main reason for not using the on-road assessments is that it is considered to be time-consuming and costly. The aim of the study was to explore the feasibility to make on-road assessments routinely at 3 months followup for all patients with a 3 months verbal prohibition of driving after stroke, to support the physicians’ decision of fitness to drive.
Research questions
1. Is it feasible and appropriate to make on-road assessments at a 3 months follow-up for all patients with stroke?
2. Is there an acceptable difference in accuracy between NorSDSA and on-road assessment as gold standard in order to choose NorSDSA instead of on-road assessment?
Methods
All patients admitted to a primary stroke unit at a university hospital between September 2007 and June 2009 was considered for inclusion in the study. Patients were excluded if they did not have a driving license or driving experience, or would be dependent on extensive care in the future. Patients with direct medical obstacles to driving, such as epilepsy, neglect or hemianopsia, were also excluded. Patients in need of an adapted vehicle were referred to a driving centre as this kind of resources was not available in the present structure. Adaptations would not be made before no further improvements would be expected, which is too early to determine at 3-months follow-up. The occupational therapists at the unit searched the medical records to determine if there were reasons for exclusion from the study according to the exclusion criteria’s.
Due to reorganisation of the stroke units at the hospital in June 2009, patients thereafter until the end of December 2009 were recruited from other hospitals belonging to the university hospital. From these hospitals patients in needed of a more thorough investigation were referred to the study by a physician.
Procedure
The routine on the units was that all patients diagnosed with a stroke were prohibited from driving by verbal agreement until they had seen the physician for a new decision during a return visit 3 months after discharge. At discharge, the patients who were eligible for a driving assessment received a letter informing them that they would be contacted shortly before their return visit to the hospital. Just before the return visit, the patients were contacted by telephone and asked to participate in a driving fitness examination. Just before the return visit, the patients were contacted by telephone and asked to participate in a driving fitness examination. They were informed that the study was a possibility to have a more thorough assessment of fitness to drive and would supply the physician with material for rapid and correct decisions of driving.
If the patient consented to participate, the examination was performed in two sessions at the driving school. The first session, NorSDSA was administered. At the second session, an on-road assessment was performed assessed by a different OT. This assessment took place in a car with dual controls and the patient was accompanied by a traffic instructor responsible for safety and provision of instructions for the drive on a predetermined route that included a range of different traffic situations. Before finishing, the patient was asked to give his or her opinion of his/her performance and was also given feedback by the OT of her perception of the performance. The discussion after the driving produced information about the patient’s awareness of problems, which was also documented.
The OT documented the result in the medical record. In total, three OTs experienced in working with stroke patients and trained in traffic medicine, were involved in the assessments. As there was no available standardised observation method for the on-road assessment at the time, an observation template and guidelines were made to secure as equal assessments as possible. To assure acceptable inter-reliability, the OTs also simultaneously observed and independently assessed, the on-road driving of two different patients. These assessments were then compared and discussed. There were an agreement on the pass or fail result and good agreement regarding their notes on the observation template. The OT and the traffic instructor compared their experiences from the drive before the feed-back to the patient and a good agreement was found on the general question of pass or fail, 96% agreement on the 50 assessments in the study. However, the decision was to be made by the OT.
Assessments
Nor SDSA: The Stroke Driver Screening Assessment (SDSA) is a cognitive instrument that was developed in Great Britain by Nouri and Lincoln to assess driving after stroke [17]. The SDSA has been translated and validated for Nordic traffic conditions, where it is known as NorSDSA [13, 18]. The adaptations made in the Nordic version included changing the illustrations of traffic situations so that the driver was on the right-hand side of the car. The traffic signs were also adapted to reflect Swedish conditions. The instrument has been shown to be valid and reliable [13, 17]. The instrument comprises four tasks: dot cancellation, directions, compass directions, and recognition of traffic signs. The time is recorded and the result is given in points. Dot cancellation examines precision and visual selective attention by a task to mark all groups of four dots on a sheet with several lines. In the Direction task, the patient is given a number of cards with a lorry and a car going in different directions and he/ she must find the right square in which to place the card according to the arrows in a co-ordinate system. Compass directions demands good visuospatial orientation, the ability to reason and understand the relationship between the different directions, the ability to divide attention, and good working memory, when placing cards with two vehicles leaving a traffic circulation in different directions in a coordinate system. Recognition of traffic signs examines the ability to use different traffic signs in different traffic situations, mental processing speed, and working memory.
The result of the test is divided into:
- Failure to pass (≤ -0.5)
- Uncertain or slightly negative (-0.5-0)
- Uncertain or slightly positive (0-0.5)
- Pass (≥ 0.5)
There is no clear instruction on how to handle the uncertain results. In this study we have chosen to see these results as uncertain and therefore in need of additional assessments.
On-road assessment: The assessment was based on the literature on how to perform a valid and reliable road test [10, 19]. The following traffic situations were included: traffic lights, circulation, crossroads, left turn, crossing bicycle path, prohibition to turn left, country road, highway, residential area, speed limits of 50, 70, and 90 km/h, and following traffic signs. The route was the same for all assessments and took about an hour to complete. The distance was 25Km.
During the drive, an OT observed and documented the patient’s performance, driving style, behavior and problems on an observation template according to the domains of assessment described by Patomella et al. [20, 21]. The instrument was under development and could therefore not yet be fully used. The domains that were assessed were maneuvering, orientation, conforming to traffic regulations, maintaining control, reaction, attention, and problem solving. After the drive, the observations were compiled and collated into a decision of pass or fail.
For a decision to fail the patient, the drive had to contain several insecure situations or "a risk" of serious accident or actions and situations that required the intervention of the traffic instructor for reasons of safety. The on-road assessment was documented in the medical records: the results in each observation template area were recorded along with a clear recommendation regarding pass or fail.
Administration: The median time for preparation before the assessment, performance, summation and documentation was 1,5 hours for the NorSDSA respectively 2,5 hours for the on-road assessment. As the study was exploring the need for assessments, it was convenient to use a driving school providing the resources just when needed. With this organisation there was a fee for the use of the car, and the instructor which the patient had to bear (1,000 SEK ≈ 106 €).
Analyses
To examine the proportion in need of further examination with an on-road assessment after the NorSDSA, due to a not certain result of pass or fail, the four NorSDSA categories were calculated and the two middle categories representing uncertain cases were merged into one category. Second, the total time consumption and cost were computed and compared to the costs of a scenario where only onroad assessments were given in all cases.
As the accuracy of the results are of great importance further examinations were performed in order to explore if there were discrepancies in decisions between NorSDSA pass or fail and the gold standard, on-road assessment. For this purpose analysis of the agreement between NorSDSA and on-road assessments was performed with a Kappa analysis. This analysis yielded an agreement value and its significance. According to Peat [22], Kappa values of 0.5, >0.7, and >0.8 represent moderate, good, and very good agreement, respectively. Positive and negative predicted values were also calculated to determine the probability that Nor SDSA screening accurately detects the patients who are unfit and fit to drive.
Additionally the results of the two assessments were plotted together (see Figure 3) to explore if there were areas with total agreement. As base for discussion about the consequences on resource use relative to accuracy, calculations were made to explore how changed cut-offs on Nor SDSA would influence the costs.
Ethical aspects
The study was considered to be required for developing routines and an application for ethical approval was not acquired, but was approved by the director of department. However, ethical considerations were taken into account to ensure that the patients were not at risk. Written information was provided and the participants were asked for their consent to participate in the study.
Findings
Since there was a reorganisation in June 2009, only data collected before that was included in the analyses exploring the proportion of patients in need of a driving assessment after the stroke onset. In total, 441 patients had a stroke and were admitted to the stroke unit of the hospital during study period, September 2007 to June 2009. Of these, 110 (25% of the whole cohort) were eligible and included in the analyses of the number of patients that yearly would require decisions on driving. Every year, approximately 2000 patients are admitted to the stroke units of the university hospital. Extrapolation of the eligible rate of our patients to this number means that about 500 cases would have to be assessed for driving fitness by the physicians every year.
Thirty patients (27% of the eligible patients) agreed to be assessed for their fitness to drive and could be included in the comparisons between the two assessment methods (Figure 1). There were different reasons for the drop-out of the 80 eligible patients not included, such as they would stop driving, disagreed with making the assessment or had already got a clearance for driving from a physician not aware of the study. However, the sample was representative for patients were it may be questionable if the patient should drive or not three months after stroke. From the 41 patients referred from the other stroke units in the hospital complex after the reorganisation 20 agreed to participate in the assessments.
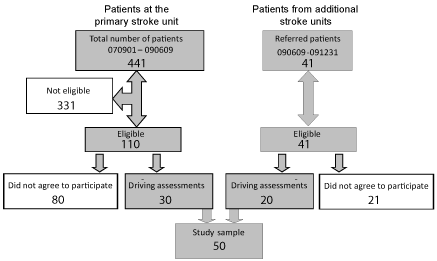
Figure 1: Disposition of the 482 consecutive stroke patients during the study.
In total, 151 patients were eligible for a driving assessment. Of these, 102
declined to take a driving test. The remaining 50 patients were assessed and
formed the sample.
When using NorSDSA, 32% of the patients received an uncertain result soliciting further evaluation with an on-road assessment, (Figure 2). Thus, of the 500 patients who would be screened every year at the hospital, 160 would have to undergo a subsequent on-road test. The NorSDSA and on-road assessments took on average 1.5 and 2.5 hours, respectively. Thus, it would take 1150 hours per year to screen the 500 patients with NorSDSA and perform subsequent on-road testing of those who had an uncertain result. By contrast, it would take 1250 hours to give all 500 patients an on-road assessment immediately. Thus, the NorSDSA screening would provide a benefit of 100 hours. The cost of an occupational therapy assessor is in median 17 €/hour. Thus, the NorSDSA-based procedure would cost 19,550 € every year, while on-road testing of all patients would cost 21,250 €. Thus, the screening process is associated with a cost benefit of 1,700 €.
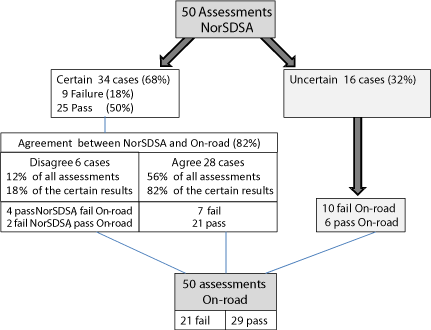
Figure 2: Schematic depiction of the numbers and percentages of the sample
patients (n=50) who obtained certain and uncertain NorSDSA results during
screening. The 16 patients who had an uncertain result (32%) had to have
an on-road assessment. The bottom of the figure shows the results of the
on-road assessments. The agreement between the NorSDSA and on-road
assessment methods in terms of the patients who had certain NorSDSA
results is shown in the middle box.
To explore the agreement between the NorSDSA and the onroad gold standard in the 50 cases, the cases classified as certain passes or fails by NorSDSA (N=34) were subjected to Kappa analysis. The agreement was 0.58, which is considered to indicate moderate agreement. The positive predictive value for the same group, which indicates the probability of NorSDSA correctly detecting patients who are not fit to drive, was 78%. Thus, more than one of five patients who are not fit to drive will not be detected by NorSDSA. The negative predictive value, which indicates the probability of NorSDSA correctly detecting the patients who are fit to drive, was 84%. However, these percentages were calculated when 32% of the NorSDSA-assessed sample was already removed due to uncertain results. This fairly high percentage should also be taken into account when determining how serious the incorrect decisions are? Table 1 lists the reasons for failure on the on-road assessment for the four cases in the study with divergent results of pass on NorSDSA and failure on the on-road assessment.
Person
Age
NorSDSA
Result
Domain
Problems during the on-road test
1
76
4
Maneuvering
Reversed and braked at crossroads
Orientation
Went in the wrong direction, did not maintain the correct distance from other cars, came close to colliding had problems planning and changing lanes
Problem solving
Hesitant, asked for help in conjunction with having difficulties
Awareness
Lacked awareness of fellow road users and the environment
2
78
4
Orientation
The distances from the preceding cars were too short the driver came too close during overtaking.
Conforming with traffic regulations
Did not follow the speed limits and stop signs.
Problem solving
Hectic, indecisive
Awareness
Lacked awareness at bicycle paths, crossings and when passing a bus.
3
74
4
Orientation
Difficulty following road signs, drove too close to the left and on one occasion drove in the oncoming lane, which required intervention
Conforming with traffic regulations
Drove too fast, drove on the wrong side of a traffic sign with a specified direction
Problem solving
Did not notice any problems that needed solving, too slow
Awareness
Lack of awareness of memory and attention problems
4
84
4
Orientation
Stopped in the middle of the road and asked for advice about what to do on three occasions
Reaction
Slow
Attention
Lacked attention to the environment and fellow road users
Problem solving
Did not adjust to demands from the environment, lacked judgment
Awareness
Did not acknowledge that they did not look to the right or that this was necessary
Table 1: The table shows the reasons why four patients who passed the NorSDSA failed on the on-road assessment.
To further explore the performance of NorSDSA and the agreement between the two assessment methods, the raw NorSDSA scores and the pass/fail results of the on-road assessment were plotted together (Figure 3). Visual inspection revealed three areas in the plot: the area at the bottom where the two tests agreed that the patient was not fit to drive (four cases whose NorSDSA scores ranged between -1.4098 and -2.1035), the area in the middle where the two tests disagreed about whether the patient was fit to drive (29 cases), and the area at the top where the two tests agreed that the patient was fit to drive (17 cases whose NorSDSA scores ranged between 1.4659 and 3.4209). Thus, for a total pass-fail agreement cutoffs of need to be -1.5 and 1.5 (Figure 3). Applying these cut-offs to the data would mean that there would then be 29 unsure cases (58%) that needed further examination. Extrapolation of these data to the annual hospital patients means that the screening process would cost the hospital 1475 hours/year (500 cases x 1.5 h + 290 cases x 2.5h) compared to 1250 hours/year when all patients immediately undergo an on-road assessment. Thus, the screening process would cost 225 hours more for a similar result if changing the cut-offs for more confident results.
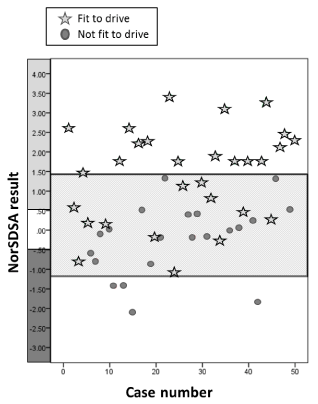
Figure 3: Plot of the result of NorSDSA (y-axis) and on-road assessment
indicated by stars (pass) and dots (fail) of the sample (x-axis, N=50). On
the Y-axis the white area indicate uncertain results, dark grey certain fail and
light grey certain pass. Above the line at 1,5 all cases have received a pass
on both assessments and below the line at -1,5 there is an agreement of fail
on the assessments. From this result alternative cut-offs could be made that
indicates uncertain results on NorSDSA between -1,5 and 1,5.
In some studies NorSDSA has been dichotomized into pass and fail according to a cut-off at zero. In this condition there was a disagreement between the NorSDSA and the on-road assessment as the gold standard in 13 cases (26 %) which is a high number of wrong decisions.
The patients’ perception of performing the NorSDSA and the on-road assessment: The patients’ experience of performing the NorSDSA could be of value to understand the discrepancies between the assessments as well as why the on-road assessment could be more useful to accomplish awareness. The interview after the NorSDSA indicated that several patients questioned the test and its relevance: they felt that it was childish, images were difficult to see and understand and the time limitations were stressful and not relevant. Some patients thought, however, that performing the test was useful and it did not cause them any problems. All patients found the onroad assessment relevant although not all agreed with the decision if they were unfit to drive. Some patients complained about being in an unfamiliar car which made it more difficult to drive.
The observations of the OTs: The OTs observed different behaviors when the patients performed the NorSDSA. In half of the sample the test was performed in a concentrated, rational, calm and organised manner, and in half of the sample the patients had difficulties remembering and understanding instructions, had a slow tempo or stressed or forced behaviour or showed lack of involvement and uncertainty about what to do. At the on-road assessment several patients appeared nervous in the beginning but most patients became more relaxed after a few minutes. Some patients tried to make a conversation which sometimes distracted.
Awareness of problems: Many of the patients did not admit to any problems with their driving performance. However, when the OT described situations where problems occurred, some of the patients agreed after a discussion that they had made some mistakes.
Discussion
The present study showed that around a quarter of the patients admitted to the stroke unit were eligible for an assessment of driving fitness. Moreover, given that two of the four categories of NorSDSA results represent uncertain results, 32% of NorSDSA-assessed patients would need further assessment, preferably with an on-road assessment. Since the screening with NorSDSA is also quite timeconsuming, it provided only a small gain in time or cost compared to on-road assessment.
Since driving is a complex activity, it is not easy to develop a rapid and correct method for screening. For security reasons it is important to find those patients not fit to drive but it is also important from a health perspective to allow driving for patients fit to drive. NorSDSA does not clearly classify patients into pass or fail categories, which mean that it will only detect relatively few patients who do not need further examination. Based on the numbers in the present study, it was calculated that 160 patients in the hospital would have to have an additional driving assessment after the NorSDSA screening every year. On this basis, compared to the immediate use of the on-road test, the screening process would only save the hospital about 100 hours, or 1,700 €, a year. That is only 8% less than the costs for onroad assessments of all patients.
A screening test is mostly used to select cases that have the sought-after feature, after which those cases will proceed with a more thorough examination. In the case of the NorSDSA-based screening process, this process aims to distinguish the cases with a clear decision from those whose results are uncertain and require further examination. Since screening instruments are often limited in terms of sensitivity and specificity, it was important to explore the agreement between the NorSDSA-based screening process and the gold standard as well as to determine the probability that the screening method correctly detected the "right" patients and did not miss the patients whose driving skills place him/her and the public at risk. These analyses showed that the screening process agreed only moderately with the gold standard and that as many as one in five patients who were actually not fit to drive would pass the NorSDSA examination and be free to continue driving. In addition, 16% of the patients who are assessed will be prohibited to drive despite being fit to drive. In our hypothetical hospital scenario, this means that every year, the activities of 80 people will be curtailed because they are not allowed to drive despite being fit to drive, while 110 patients will be placing themselves and other road users at risk because they have been incorrectly assessed as being fit to drive. These numbers are far too high to be satisfying and are consistent with the findings of Selander et al. [14], who concluded that NorSDSA should not be used alone to assess the driving fitness of stroke patients. In addition, the present study suggests that using NorSDSA to select patients for additional assessment is also of doubtful utility.
The plot of the NorSDSA and on-road test results was analysed visually in an attempt to adjust the cut-off for passes and failures so that the patients who did not need further examination could be more accurately detected by NorSDSA. However, because the area of disagreement was so large, the adjusted cut-offs actually increased the costs of the screening procedure compared to immediate on-road testing. Thus, there does not seem to be an easy way to improve the screening accuracy of NorSDSA.
The patients who were approved by the NorSDSA test but failed the on-road assessment encountered several serious problems which affected their ability to make quick and correct decisions. This ability is described as the tactical level in the model developed by Michon [23]. The problems occurred in situations that required a great deal of attention to the environment and fellow road users and that caused traffic hazards. For example, the patients omitted to look back when changing lanes and did not pay attention to bicycle paths, crossroads, and traffic signs. A substantial part of the problem with information processing was due to the reduced tempo of the process and caused safety risks by hesitancy and slowness that affected their performance. The lack of forward planning and lack of attention to the environment resulted in dangerous situations. A study by Lundqvist et al. [24] confirms that stroke patients often have a reduced ability to plan forward and pay attention to traffic signs, traffic lights and bicycle paths (i.e., the environment). The NorSDSA assessment and most other cognitive screening tests do not reveal these problems because the tests does not impose the high demands for executive functioning that are experienced during driving. Indeed, impairments in executive functioning are difficult to elicit in a standardised test situation as the executive system controls and manages several cognitive processes, such as planning, reasoning, task flexibility and problem solving [25].
Most of the patients who were unfit to drive showed a lack of awareness of problems which is common after a stroke [26]. Fitness to drive includes having an understanding of shortcomings as this allows the person to adjust to different demands from the environment. If this understanding is lacking it is even more important that the assessment procedure is sensitive and detects all patients who are not fit to drive. Notably, one of the advantages of the on-road test over NorSDSA is that the assessor can directly refer to the problematic traffic situations experienced during the drive when discussing the result afterwards, which helps to increase the awareness of the patient.
Some patients failed to pass the NorSDSA test but passed the on-road assessment. This could be explained by the reactions to the test that were expressed by some of the patients as well as indications from the OT observation that several patients had difficulties understanding and remembering the instructions of the NorSDSA and were unfamiliar with the kind of tasks. A stroke can also generate difficulties in terms of learning ability. All patients had long experience with driving, which suggests that while driving, they probably perform certain procedures automatically. A brain injury does not necessarily mean that the automatic processess involved in driving, which should be considered in the assessment of driving fitness, are affected [19]. Also, in the present study, five of the eight patients who passed the on-road assessment but failed the NorSDSA drove a car with an automatic gearbox. Thus, this environmental adaptation may help greatly in making the patient fit to drive. NorSDSA cannot take the effect of such an adaptation into account.
A limitation of the present study was that there are no true results that could be used to verify the performance of the NorSDSA. The analyses relied on the on-road assessment, which served as the gold standard, but may also be questioned because it involved subjective evaluations made by the assessors. To minimize differences, standardisation was strived for by templates, consensus discussions and by using the same route and traffic instructor to ensure that the assessments were as reliable as possible. Another limitation was the large drop-out which in some ways was due to the difficulty to implement routines that are followed. We have looked at the dropout and could not find that they differed in characteristics or injury from those in the sample.
Conclusion
Although this study did have some limitations, it can be concluded that using a screening process with NorSDSA added relatively little advantage in terms of time and costs compared to routinely applying the on-road test. Analogously with other studies it was found that NorSDSA was not sufficiently reliable in terms of classifying fit and unfit drivers as accuracy is of great importance since both incorrect decisions of pass and fail may have serious consequenses. The onroad assessment has the advantage in that it directly assesses the response of the patient to real-life complex and distracting situations and that the result may be discussed in relation to actual problems that occured. This may help the patient to gain awareness about their driving limitations an important factor that may be worth the extra costs. In the present study, with a catchment area of 800 000 inhabitants, the yearly admission of stroke to the hospital is around 2000 patients, yielding 500 in need of a driving assessment which is reasonable to handle. To conclude the results support that a feasible routine for decisions of driving, after the first intermission to drive after stroke, could be that all patients in need of more thourough assessment are assessed with an on-road evaluation before the return visit to the physician. From the plot with the two assessments the best agreement was for the patients fit to drive possibly indicating that some patients may be easier to detect and could be excluded from further asessments. For future research it may be useful to explore if there are some tools to select which patients that need an on-road assessment, and which can be returned to driving on the basis of their doctor’s informal clinical judgement.
Acknowledgments
The study was supported with grants from the County of Vastra Gotaland.
References
- Socialstyrelsen. Nationella riktlinjer vid stroke sjukvård. 2009.
- Fisk GD, Owsley C, Pulley LV. Driving after stroke: driving exposure, advice, and evaluations. Arch Phys Med Rehabil. 1997; 78: 1338-1345.
- Marshall S, Demmings EM, Woolnough A, Salim D, Man-Son-Hing M. Determining fitness to drive in older persons: a survey of medical and surgical specialists. Can Geriatr J. 2012; 15: 101-119.
- Jang RW, Man-Son-Hing M, Molnar FJ, Hogan DB, Marshall SC, Auger J, et al. Family physicians' attitudes and practices regarding assessments of medical fitness to drive in older persons. J Gen Intern Med. 2007; 22: 531-543.
- Moorhouse P, Hamilton L, Fisher T, Rockwood K. Barriers to assessing fitness to drive in dementia in nova scotia: informing strategies for knowledge translation. Can Geriatr J. 2011; 14: 61-65.
- Lundqvist A, Alinder J, Rönnberg J. Factors influencing driving 10 years after brain injury. Brain Inj. 2008; 22: 295-304.
- Korner-Bitensky N, Bitensky J, Sofer S, Man-Son-Hing M, Gelinas I. Driving evaluation practices of clinicians working in the United States and Canada. Am J Occup Ther. 2006; 60: 428-434.
- Devos H, Akinwuntan AE, Gélinas I, George S, Nieuwboer A, Verheyden G. Shifting up a gear: considerations on assessment and rehabilitation of driving in people with neurological conditions. An extended editorial. Physiother Res Int. 2012; 17: 125-131.
- D'apolito AC, Massonneau A, Paillat C, Azouvi P. Impact of brain injury on driving skills. Ann Phys Rehabil Med. 2013; 56: 63-80.
- Fox GK, Bowden SC, Smith DS. On-road assessment of driving competence after brain impairment: review of current practice and recommendations for a standardized examination. Arch Phys Med Rehabil. 1998; 79: 1288-1296.
- Odenheimer GL, Beaudet M, Jette AM, Albert MS, Grande L, Minaker KL. Performance-based driving evaluation of the elderly driver: safety, reliability, and validity. J Gerontol. 1994; 49: M153-159.
- Devos H, Akinwuntan AE, Nieuwboer A, Truijen S, Tant M, De Weerdt W. Screening for fitness to drive after stroke: a systematic review and meta-analysis. Neurology. 2011; 76: 747-756.
- Lundberg C, Caneman G, Samuelsson SM, Hakamies-Blomqvist L, Almkvist O. The assessment of fitness to drive after a stroke: the Nordic Stroke Driver Screening Assessment. Scand J Psychol. 2003; 44: 23-30.
- Selander H, Johansson K, Lundberg C, Falkmer T. The Nordic stroke driver screening assessment as predictor for the outcome of an on-road test. Scand J Occup Ther. 2010; 17: 10-17.
- Larsson H, Lundberg C, Falkmer T, Johansson K. A Swedish survey of occupational therapists' involvement and performance in driving assessments. Scand J Occup Ther. 2007; 14: 215-220.
- Patomella AH, Johansson K, Tham K. Lived experience of driving ability following stroke. Disabil Rehabil. 2009; 31: 726-733.
- Nouri FM, Lincoln NB. Validation of a cognitive assessment: Predicting driving performance after stroke. Clinical Rehabilitation. 1992; 6: 275-276-281.
- Nouri FM, Lincoln NB. Predicting driving performance after stroke. BMJ. 1993; 307: 482-483.
- Lundqvist A, Alinder J, Alm H, Gerdle B, Levander S, Rönnberg J. Neuropsychological aspects of driving after brain lesion: simulator study and on-road driving. Appl Neuropsychol. 1997; 4: 220-230.
- Patomella AH, Tham K, Kottorp A. P-drive: assessment of driving performance after stroke. J Rehabil Med. 2006; 38: 273-279.
- Patomella AH, Tham K, Johansson K, Kottorp A. P-drive on-road: internal scale validity and reliability of an assessment of on-road driving performance in people with neurological disorders. Scand J Occup Ther. 2010; 17: 86-93.
- Peat J. Health science research: A handbook of quantitative methods. Allen & Unwin, Sydney. 2001.
- Michon JA. Critical view of driver behavior models: What do we know, what should we do? 1985; 485-524.
- Lundqvist A, Gerdle B and Rönnberg J. Neuropsychological aspects of driving after a stroke-in the simulator and on the road. Applied Cognitive Psychology. 2000; 14: 135-150.
- Chaytor N, Schmitter-Edgecombe M. The ecological validity of neuropsychological tests: a review of the literature on everyday cognitive skills. Neuropsychol Rev. 2003; 13: 181-197.
- Patomella AH, Kottorp A, Tham K. Awareness of driving disability in people with stroke tested in a simulator. Scand J Occup Ther. 2008; 15: 184-192.