
Research Article
Phys Med Rehabil Int. 2015; 2(9): 1070.
Neurorehabilitation in Developing Countries: Challenges and the Way Forward
Khan F1,2,3,4,5*, Amatya B1,5, Mannan H³ and Rathore FA5,6
¹Department of Rehabilitation Medicine, Royal Melbourne Hospital, Parkville, Victoria, Australia
²Department of Medicine, Dentistry and Health Sciences, University of Melbourne, Parkville, Victoria, Australia
³Nossal Institute for Global Health, University of Melbourne, Parkville, Victoria, Australia
4School of Public Health and Preventive Medicine, Monash University, Victoria, Australia
5Committee for Rehabilitation Disaster Relief (CRDR), International Society of Physical and Rehabilitation Medicine (ISPRM), Geneva, Switzerland
6Department of Rehabilitation Medicine, CMH Lahore Medical College, University of Health Sciences, Lahore, Pakistan
*Corresponding author: Fary Khan, Department of Rehabilitation Medicine, Royal Melbourne Hospital, 34- 54 Poplar Road Parkville, Melbourne VIC 3052, Australia
Received: November 03, 2015; Accepted: November 25, 2015; Published: November 27, 2015
Abstract
Neurological disorders affect one billion people worldwide and have significant disability-burden with longer-term functional and psychosocial issues that need comprehensive management, including rehabilitation. The prevalence of disability due to neurological conditions is escalating worldwide. These add to the economic burden for healthcare systems (particularly in lowresourced countries), where despite improved acute health care systems, health policies have not extended to include rehabilitation. Neurorehabilitation is interdisciplinary and cross-sectorial, requiring collaborative coordinated effort of diverse sectors, professions, patients and community. This article provides a narrative overview of literature on neurorehabilitation in developing countries and highlights some of the challenges in implementation of the World Health Organization’s Global Disability Action Plan (DAP), focusing on rehabilitation (Objective 2) within the context of neurological conditions. Several issues related to neurorehabilitation are discussed for a systematic approach to build horizontal health care systems that are sustainable and responsive; involvement of bilateral agencies using multi-sectorial approach, new partnerships, strategic collaboration; provision of technical assistance, research and development; and capacity-building for a strong interdisciplinary workforce. Other factors that need to be addressed include governance for strengthening health care systems through logistics, surveillance and service delivery; and adequate scaling. The DAP provides comprehensive summary actions to tackle global disability, including neurological disorder-related disability, and offers governments, policy-makers and other relevant stakeholders a blueprint for implementing recommendations of the World Disability Report and the Convention on the Rights of Persons with Disabilities, and facilitate social inclusion of persons with neurological conditions, in countries at all stages of development.
Keywords: Disability, rehabilitation; Neurological disorder; Developing country; World Health Organisation
Abbreviations
CBR: Community-Based Rehabilitation; COAG: Council of Australian Governments; CP: Cerebral palsy; CRPD: Convention on the Rights of Persons with Disabilities; CT: Computer Tomography; CVD: Cardio-Vascular Disease; DALY: Disability Adjusted Life Years; DAP: Disability Action Plan; HDI: Human Development Index; GDP: Gross Domestic Product; GNI: Gross National Income; ICF: International Classification of Functioning, Disability and Health; LTNCs: Long-Term Neurological Conditions; MRI: Medical Resonance Imaging; NCDs: Non-Communicable Diseases; NDA: National Disability Agreement; NGO: Non-Governmental Organisation; OECD: Organisation for Economic Co-operation and Development; OT: Occupational Therapists; PM&R: Physical Medicine and Rehabilitation; P&O: Prosthetics and Orthotics; PT: Physiotherapists; PwD: Person with Disability; RCI: Rehabilitation Council of India; SCI: Spinal Cord Injury; SLTs: Speech and Language Therapists; TBI: Traumatic Brian Injury; UN: United Nations; WHO: World Health Organization; US: United States; WFN: World Federation of Neurology.
Background
The World Report on Disability estimates over one billion people with disabilities globally, which equates to15% of world population or 1 in 7 people (based on 2010 global population estimates) [1]. Of these 110-190 million have significant difficulties, such as inability to walk, perform self-care, or communicate, or to participate in education or employment [1]. The prevalence of disability is significantly higher in low-income than in high-income countries, with an estimated 80% persons with disability (PwD) living in low-income countries [2]. Disability prevalence rates are also associated with poverty and personal wealth, with 20.7% of PwD in the lowest-wealth compared with 11.0% in the highest-wealth quintile [1,3].
The world-wide prevalence of disability is escalating, potentially due to global trends in population ageing, rise in chronic conditions (including Non-Communicable Diseases, NCDs such as cardio vascular diseases, diabetes etc.) and upsurge in natural/man-made disasters [1,2]. Persons aged 60 years and above are projected to increase from 675 million in 2005 to 1.9 billion by 2050 globally [4]. Over next 30 years, the estimated increase in number of older people with profound disability by 70% [5]. The estimation-based data is sparse, particularly for developing countries, making it difficult to gauge trends and causes over time. Further, national estimates vary considerably amongst countries and are generally difficult to compare [1]. Economic and social costs of disability are difficult to quantify and to date; there is no inclusive estimate data for overall cost [1]. The reasons for this includes: variation in definitions of disability, different data collection and reporting methods, variation in type/content of disability services/programs; limited data on the cost components of disability; lack of standardized methods for costestimation; lack of routine data collection and national registries for disability and others. However, available data suggests that economic and social costs of disability to individuals, families, communities and nations (direct and indirect costs) are significant [1]. The estimated cost of disability is around 10% of public social expenditure across Organisation for Economic Co-operation and Development (OECD) (up to 25% in some countries) [1,6].
The majority of PwD is economically deprived and experience difficulties in accessing basic health services (including rehabilitation) [2]. Only 3% of individuals who need rehabilitation globally receive the service [7], and this is significantly higher for PwD in low-income compared with high-income countries [1]. It is estimated that people needing prostheses or orthotic-related services represent 0.5% of the population in developing countries, and 30 million people alone in Africa, Asia, and Latin America require over 180,000 rehabilitation professionals [8,9]. A global survey of government action (n = 114 countries) in 2006, on the implementation of the United Nations (UN) Standard Rules on the Equalization of Opportunities for PwD reported significant gap in service provision [10]. Rehabilitation policies were not adopted in 48 UN member states (42%); legislation on rehabilitation for PwD not passed in half (50%); and rehabilitation programs not established in 46 countries (40%) [10]. Further, in 2005, one-third of countries globally did not allocate any specific budget for rehabilitation services [1].
Though musculoskeletal conditions (such as arthritis trauma) are prevalent and major cause of disability, neurological insults are more complex, and have a greater disability burden (due to concurrent physical, speech, cognitive and behavioral issues) over longer period of time [11]. Neurological disorders affect up to 1 billion people worldwide and constitute 6.3% of the global burden of disease [12]. Nervous system disorders have significant diseaseburden worldwide with an estimated 92 million disability-adjusted life-years (DALYs) in 2005, which is projected to increase by 12% to 103 million in 2030 [12]. The estimated DALYs for neurological disorders were highest for lower-middle and low-income countries [12]. Of these, cerebrovascular diseases (CVD) such as stroke, infarcts/hemorrhages, contribute more than half of the burden in DALYs, followed by Alzheimer and dementia (12% each) [12]. Further, neurological disorders constitute 12% of total deaths globally, with CVD contributing almost 85% of deaths [12], which is significantly higher in lower-middle income countries compared with high-income countries (16.8% vs. 13.2%) [11]. DALYs per 100,000 population and deaths attributable to 10 most common neurological disorders in 2005 in low-income and low-middle income countries according to the World Bank is tabulated in Table 1.
Neurological conditions
DALYs
Death
World
Low income
Low middle income
World
Low income
Low middle income
Cerebrovascular disease
788.4
662.5
1061.2
9.9
6.41
15.81
Alzheimer’s and other Dementias
172
90.7
150.7
0.73
0.41
0.34
Migraine
118.9
114
106.8
0.00
0.00
0.00
Epilepsy
113.4
158.3
80
0.22
0.28
0.17
Tetanus
99.7
228.6
10.8
0.33
0.64
0.04
Meningitis
82.9
143.2
51.2
0.26
0.39
0.18
Parkinson’s disease
25.1
15.1
19.7
0.18
0.06
0.18
Multiple sclerosis
23.4
20.1
23.3
0.03
0.01
0.02
Japanese encephalitis
8.7
13.0
9.0
0.02
0.03
0.01
Poliomyelitis
1.8
2.6
1.6
0.00
0.00
0.00
Total
1434.3
1448.1
1514.3
11.67
8.23
16.77
(Adapted from WHO Neurological disorders: public health challenges 2006 [12])
*Income categories are based on World Bank estimates of gross national income (GNI) per capita in 2001: low income ≤ GNI US$ 745; lower middle income = GNI US$ 746–2975.
Table 1: Disability-adjusted life year (DALYs) per 100,000 population and deaths attributable to neurological disorders globally and for ‘Low’ and ‘Low middle’ income countries (World Bank category)* in 2005.
Neurological Rehabilitation
Neurorehabilitation is the delivery of a coordinated interdisciplinary care program comprising ‘a set of measures that assist individuals who experience (or are likely to experience) disability to achieve and maintain optimal function in interaction with their environment’ [1], for maximum independence and social reintegration [13,14]. The treating team includes neurologists, rehabilitation physicians, nurses and allied health professionals. These programs are individualized and goal-oriented to meet the specific needs of the PwD [15] and encompass the International Classification of Functioning, Disability and Health (ICF) framework, where activity limitation (e.g. mobility, continence, self-care) and participation restriction (e.g. work, driving, community activities) interact with contextual factors (environmental and personal) that influence performance and participatory outcomes [1,4,16].
Long-term neurological conditions (LTNCs) [17] (Box 1) can cause complex disabilities, are costly to treat and have socioeconomic implications due to increased demand for health care, social and vocational services, and caregiver burden [18]. Despite improved medical care and survivorship, people with LTNCs have significant medium to longer-term functional and psychosocial issues that limit daily activity and participation [18]. These require integrated interdisciplinary collaborative care in hospital and community to enable these people to live independently in the community (Figure 1).
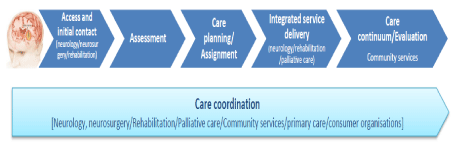
Figure 1: Integrated neurorehabilitation model of care.
Box 1: Classification of LTNCs [17]:
- Sudden onset conditions, e.g. acquired brain injury or spinal cord injury.
- Intermittent and unpredictable conditions, e.g. epilepsy, certain types of headache or early multiple sclerosis (MS), where relapses and remissions lead to marked variation in the care needed.
- Progressive conditions, e.g. motor neurone disease, Parkinson’s disease or later stages of MS where progressive deterioration in neurological function leads to increasing dependence on help and care from others.
- Stable neurological conditions, but with changing needs due to development or ageing, e.g. Post- polio syndrome or cerebral palsy (CP) in adults.
Key Global Initiatives
The UN Millennium Development Goals focus on reducing extreme poverty, improving health, education and environmental sustainability to improve lives of the world’s poorest populations by the year 2015 [4]. All eight goals aim for advancement of rights of PwD, their economic and social empowerment, and active participation [4]. It advocates tailored interventions for local (socioeconomic) conditions, improved levels of human development and health in the developing nations. In 2006, the UN General Assembly adopted Convention on the Rights of Persons with Disabilities (CRPD), together with the World Program of Action and the Standard Rules on Equalization of Opportunities for Persons with Disabilities, which provide strengthened international standards and normative framework for disability [1,19]. The CRPD and ICF highlight various factors and/or barriers, that restrict participation for PwD such as [1]: policies and standards; negative attitudes; lack of provision of services, service delivery (poor coordination among services, inadequate staffing, staff competencies, and training); inadequate funding; and lack of accessibility, consultation and involvement of PwD (in decision-making), data and evidence generation. The CRPD (Article 26) emphasizes access to rehabilitation as vital for PwD to be independent through supporting their physical, mental, social and vocational ability, and for inclusion and participation [1]. Further, the WHO ‘World Disability Report’ (2011) supports implementation of the CRPD and provides comprehensive information on disability with special emphasis on rehabilitation [1].
The WHO launched a number of global public health projects, including Global Initiatives on Neurology and Public Health [12] in response to the ‘Global Burden of Disease’ study, which highlighted neurological disorders as one of the greatest threats to world public health. The WHO in collaboration with the World Federation of Neurology (WFN) conducted an international Survey of Country Resources for Neurological Disorders (109 countries, covering over 90% of world population) and in 2004 published the first comprehensive report on country resources for neurological disorders, to increase professional and public awareness of the global burden and to emphasize the need for provision of neurological care in first-level and referral health facilities [20]. This report highlighted the inadequacy in resources and inequalities in access to care for patients with neurological disorders, especially in those living in the developing world [21]. In 2006, the WHO published: ‘Neurological disorders: public health challenges’ [12], to inform and help governments, public health institutions, NGOs and others to formulate public health policies directed at specific neurological disorders; and technical guidelines and policy papers for improved access for PwD (e.g., community-based rehabilitation; manual wheelchairs, training packages etc.).
In April 2014, the WHO global ‘Disability Action Plan’ (DAP) 2014–2021, provided a comprehensive list of specific actions to achieve the objectives: human- rights based approach (empowerment of PwD); life-course approach (continuum of care); universal health coverage; culturally-appropriate person-centered approach; multisectoral, community-based rehabilitation; and universal design [22]. The main goals of the DAP are to:
- Remove barriers and improve access to health services and programs,
- Strengthen and extend rehabilitation, assistive technology and support services,
- Community-based rehabilitation, and
- Strengthen disability data collection for international comparability, and to support research.
Methods
This article presents an overview of neurorehabilitation status in developing countries and highlights some of the challenges in implementation of the DAP. A comprehensive approach was employed to review the existing literature for neurorehabilitationrelated material. A search of peer-review literature was conducted for the previous 15 years using medical and health science electronic databases: Medline, PubMed, EMBASE, CINHAL, PsycINFO, and Cochrane Library; manual search of relevant journals and bibliographies of identified articles (for additional references). A search of grey literature was conducted using relevant internet search engines and websites including: the Centre for International Rehabilitation Information and Exchange Database of International Rehabilitation Research, the System for Information on Grey Literature in Europe, the New York Academy of Medicine Grey Literature Collection, WHO Libraries, and Google Scholar. Webportals of various healthcare institutions and governmental and non-governmental organisations (NGOs) associated with neurorehabilitation were reviewed for relevant studies. Authors and known experts in the field were also contacted. A narrative overview of key concepts identified in these studies is presented below.
Challenges and potential barriers for implementation of the disability action plan
With progress of society and economy, and improvements in health care systems, health status of populations in developing countries has greatly improved in past half-century. Concomitantly, these countries are confronted with greater scale of disability with multiple and complex causes, including neurological conditions [1,12]. In most developing countries, the emphasis of health care is still directed primarily to curative and preventive aspects of disease, and rehabilitation gets less priority [23]. The DAP provides a major boost for rehabilitation services for the WHO member States, national and international partners and consumer organizations to enhance the quality of life of PwD, worldwide. This resolution calls for the implementation and adaptation of the proposed standardized actions as a national priority [22]. The objectives of the DAP area global standard for applicability across countries, professions, cultures, and sectors worldwide.
Global standards do not always fulfill expectation of enhanced communication at multiple levels in society [24]. There appear to be contrasts and imbalances within operational healthcare systems in many countries in terms of policies, funding structure/infrastructure, capacity, human and physical resources, technology etc. Usually, PwD, including those with neurological conditions, are more vulnerable in society and are affected by constraints in the provision of health-care systems [12]. In terms of neurorehabilitation services, the global picture is still vague. There is lack of routinely collected data for disability, limited information about the needs and unmet needs of PwD, variability in definitions used for disability and various types of disability (e.g., physical, mental, behavioral, intellectual) and variation in settings [1,22]. Further, there is diversity in models of care, interventions and modalities, outcome measurement, type and quality within neurorehabilitation services [1, 22]. Healthcare systems and practices vary amongst countries, however, many challenges in neurorehabilitation are similar to generic rehabilitation services in terms of implementation of the DAP. An additional challenge for neurorehabilitation and the DAP in the context of developing countries is these conditions are often complex, with significant disability-burden worldwide. These people have concurrent physical, speech, cognitive and behavioural issues which can cause cumulative deficits over longer-term requiring specialized services for comprehensive management. These add to the economic burden for the individual (their families) and healthcare systems. Many challenges across healthcare settings for neurorehabilitation occur at both macro (international, governmental, policy) and micro (community, social, individual) level, and are common to most low-resource countries, where despite improved acute health care systems, the health policies have not fully extended to include rehabilitation. Some potential challenges for implementation of the DAP, particularly for neurorehabilitation service provision (2nd DAP objective), are summarised below.
Macro level
Policy and planning: Healthcare organisations and neurorehabilitation services have immense task of developing correct policies, laws, and delivery systems with coordination strategy adapted to local needs. These services may be confronted with expectations stemming from their institutional environment (e.g., government agencies, administrations, patient organizations) concerning improvement of quality of care and clinical outcomes. Policies also need to specifically promote the human rights of PwD [25]. Despite the burden attributed to neurological disorders, many low-middle income countries in the developing world have health policies that do not cover neurological disorders at the same level as other medical conditions [12]. Importantly, these conditions are largely absent from the national health agendas [12]. Legislation or policies for overall management of PwD, have been adapted in many developing countries such as India, Afghanistan, Bangladesh, Sri Lanka [26], Ghana [27], Pakistan [28], Mauritius [29] and others, however, disability culture in many remains in a nascent stage [28]. The existing policies are underfunded and often there is a lack of coordination and collaboration amongst different sectors and ministries involved [30]. Despite availability of policies on rehabilitation in some countries, there is lag in implementation of these policies and/or overall delivery of the rehabilitation service [1]. Further, there is no consensus on who is responsible for enforcing and/or funding new legislations such as CRPD, the other WHO recommendations etc. [30].
Infrastructure: Many persons with neurological conditions require highly specialized skills for appropriate diagnosis and management. Most developing nations lack or have limited number of adequate and efficient health services, particularly in rural areas [31]. In these countries sub-specialized services (such as stroke units) are restricted to urban areas [20]. The availability of rehabilitation services across regions varies, and many developing countries still have limited or no organized rehabilitation services [1]. In many, these services exist through NGO initiatives and charitable organisations; these are often dependent on external funding, independent of national public health systems [26]. The persons with neurological disabilities usually depend on family members for help with daily activities, which perpetuates the cycle of poverty [32]. There is minimal data collection, reporting and informationgathering system, which impedes evaluation and monitoring of the situation over-time to alert the health system to emerging trends, and to facilitate planning [32].
Resources: Lack of funding and human resources can hinder proficient implementation and management of the DAP. Currently, available resources for disability in most countries are inadequate and inequitably distributed [1,20]. In majority of low-income countries there are limited budgets for services for neurological conditions. The WHO survey showed only 10.4% of the responding countries (mainly high-income countries) have a separate budget for neurological illnesses within their health budgets, and two-thirds of the low income countries have no disability benefits available [20]. Out-ofpocket payment by patients is the major source of financing in most low-income countries, which is likely to result in financial hardship and inequity in utilization of healthcare services [20].
Health information systems: In the developing world, healthcare systems are limited by resources, capability and lack of information technology (IT) systems. Data on neurorehabilitation is incomplete and fragmented, and often not disaggregated from other health-care services information [33]. Despite availability of the ICF for over a decade, there is no indicator or common framework for describing and measuring rehabilitation in many countries; and rehabilitation measures are often excluded from existing classification systems [1]. Inadequate health information systems and communication strategies across health care sectors and between providers (notably between primary and secondary care), is still prominent worldwide, even in developed countries like Australia [34]. Other barriers to provision of neurorehabilitation services, include, inconsistent and insufficient data collection processes, multiple clinical information systems and incompatible technologies [1,34].
Referral systems: Many developing countries have no systems of appropriate referral mechanism for neurological illnesses at provincial or national level. Therefore, many people miss appropriate services and/or care continuum in the community, after discharged from an acute facility. An effective referral system is required to ensure a close relationship/coordination between all levels of the health system to ensure those with neurological disorders, receive the best possible care and regular follow-up [12,35]. This will build capacity and enhance access to better quality care and provide costeffective use of hospital, community and primary health care services.
Developing leadership, workforce and capacity: The lack of neurorehabilitation specialists and allied health personnel is a challenge in most developing countries [3]. For example, the median number of neurologists in low-income countries is 0.03 per 100,000 populations, which is considerably lower compared with highincome countries (2.96 per 100,000) [20]. This shortage is particularly evident in regions of Africa, South-East Asia, Eastern Mediterranean and the Western Pacific [20]. According to the WHO survey in sub-Saharan Africa, there are overall 6 rehabilitation physicians for more than 780 million people [1] and this number is much lower for neurorehabilitation specialists [29]. Paucity and inappropriate distribution of healthcare professionals between rural and urban regions contributes to limited rehabilitation service delivery [20]. In many developing countries, there is limited leadership guidance from governmental and other relevant authorities for training and empowerment programs for healthcare workers and PwD [36]. There is need for neurorehabilitation capacity building at national health authority level and other relevant institutions for development of a skilled workforce. Further, lack of training facilities and programs compound the problem of capacity building, specialist training and knowledge transfer for existing professionals.
Micro Level
At this level, the challenge is to assess how the DAP can be used to enhance the effectiveness of care delivery for persons requiring neurorehabilitation, and if so how this can be measured and evaluated using a standardised technique.
Poverty and cost of services: The cost of access to neurorehabilitation services is a barrier for PwD particularly in lowincome countries, where most services are available only as an out-ofpocket payment [37]. Disability can be both a cause and consequence of poverty, which impedes PwD attaining required services [38]. Many PwD, including those with neurological disorders (and family) in low-income countries are either unemployed or have lower incomes, compromising adequate care [38].
Stigma and discrimination: Despite evidence of growing public acceptance of PwD, widespread stigma and discrimination still persists, often because of non-biologic concepts and cultural perception of disabilities [1]. These entrenched concepts and social stigma in public lead to active exclusion of these people from societal participation and opportunities to liaise with the able-bodied in public [27]. Further, there is evidence of wide gender inequalities in accessing rehabilitation services in many low-income countries [39]. This has resulted in unsuccessful implementation of the World Report on Disability’s explicit recommendations for social inclusion such as community-based rehabilitation in African countries [27,40].
Awareness and education: Majority of PwD, are poorly educated and unaware of specialised specialities like rehabilitation; and information about benefits of rehabilitation are not easily available or understandable [1]. Lack of mistrust among PwD for medical practitioners in some cultures is still prevalent, particularly in rural areas, where first preference is to seek help from religious healers and traditional herbal medicine [1,41].
Access to services and assistive technologies: Disability and neurorehabilitation services are limited or often do not exist in rural areas, not only in developing countries but also in some parts of the developed world [1]. As most available services are usually based in urban areas, access to such facilities is often costly, time-consuming and difficult due to lack of transportation [42]. Assistive devices such as canes, crutches, prostheses, wheelchairs etc., are integral part of health care for persons with neurological conditions and widely prescribed to maintain, or improve functional capabilities and participation. In many high-income countries these are provided by national health care systems, through rehabilitation services, insurance companies, charities and NGOs. However, in many lowincome countries there is still large gap in service provision of these essential disability services [1,39].
Professional, caregiver and consumer groups: Though there is an increasing trend in the number of professional, caregiver groups and NGOs, for PwD worldwide, there is limited number of such organisations for disabled population in low-income countries. According to WHO, there are no NGOs or other professional groups for neurological disorders in 35% of low-income countries [20].
Overview of neurorehabilitation in developing countries
Table 2 provides an overview of rehabilitation status in different developing countries, which potentially comprise barriers that challenge equitable access to rehabilitation services and quality of such services. In most developing countries, much effort has gone to improve the acute care sector, which has seen enormous progress. However, the post-acute care system, including long-term rehabilitation and social reintegration, is immature at many levels [29]. The need for rehabilitation services in developing countries is not well defined in terms of type, settings, and intensity/duration due to lack of disability-disaggregated data within general statistics of the health and social sectors [26]. In most countries (Table 2), these services are still integrated with other health services in public hospitals where basic rehabilitation services are provided but not focused on specific disabilities (such as neurological). Although the WHO promotes the “bottom-up” approach through communitybased rehabilitation for community decision-making, in most cases the process itself is often a “top-down” approach, with rehabilitation professionals still being the decision-makers for need assessment and management, while participation of PwD is limited [43].
Country
Geographical data
Epidemiology: overall disability
Epidemiology: neurological conditions
Policies & Legislation
Funding mechanisms
Human resources
Service delivery
Other issues
Asia
Area: 652,000 km2
Population: 29,825,000
HDI rank: 169
GNI per capita*: $1,560
4.8% of total population, 2.7% with severe disability;
Proportion of PwD to total population: 2.7%; Unemployment: >70%; No access to education: 73%
Total death: NCDs= 37%; cerebrovascular diseases: male 2.6%, (age standard Death Rate: 121.5/100,000 population)
CRPD ratified: 2012; Comprehensive national disability policy 2003; National Disability Action Plan (2008–2011); National Priority Program ‘Health for All
Afghans’ from 2012
Total expenditure on health per capita (2012): $47; Total expenditure on health as % of GDP (2012): 8.7%;
National coordination/funding: Ministry of Labour, Social Affairs, Martyrs; Majority of rehab services funded by NGOs & external
donors
Physicians: 2.3/10,000 people;
No specific specialisation
in PM&R
No data on other health care & allied health personnel
Availability of health centres: 51%
Hospital access: 32.4%
Majority of rehabilitation services funded by NGOs & charities
PT services: 44/364 districts; CBR and
out-reach programs
implemented: 80/364 districts; orthopaedic centres (tertiary level only): 13/34 provinces
No action plan for management of neurological disorders or rehabilitation.
Research in the medical rehabilitation minimal, limited (descriptive epidemiological data only).
War & terrorism, lack of education & training main barriers.
Bangladesh
Area: 147,570 km2
Population: 155 mil
HDI rank: 142
GNI per capita*: $2,030;
43%living below national poverty line of US$1.25/day
10.8% of total population; Proportion of PwD to total population 5.6%
Unemployment: no data; access to education for children: <4%; 0.5% (approx.. 750,000 persons) of the population in needof P&O services
Total death: NCDs= 59%; Cerebrovascular diseases: male 5.9%, female 6.3% (2004)
SCI: 93–174
Persons/million populations, with 14- 22,000 persons needing continuous rehabilitation services;
CP: estimated prevalence is between 2.12–
2.45/1000 live births
CRPD ratified: 2007-8; Disability Welfare Act (2001); National Policy on Disability (2004); Five-year National
Action Plan on Disability (2006); Disability Rights
and Protection Act (2013); signatory to the Asian and
Pacific Decade of Persons with Disabilities (2002–2012) and (2013–2022)
Total health expenditure per capita (2012): $68; Total expenditure on health as % of GDP (2012): 3.6;
National coordination/funding: Ministry of Health and Family Welfare and Ministry of Social Welfare
Physicians: 3.6/10,000 people;
Currently active: PM&R physicians: 200. PT: 1300; PT assistants: 600; SLTs: 33; P&O technicians: very few as no accredited training; over 900 persons completed CBR training courses.
Approx. 4 beds/10,000 population; World Bank funded project currently piloting 68 Integrated Disability Service Centres in 64 districts, in which there are 323 PTs, 83 OTs, 37 P&O &19 speech therapists IDSCs plan to start 32 mobile clinics using adapted buses, equipped with therapeutic equipment.
Majority of rehabilitation services funded and run by NGOs & charities
No official definition, policy or strategy of PM&R in National Health Policy2011 and in the Health, Population and NutritionSector Development Program 2011–2016.
Research in rehabilitation field limited to acute care outcomes.
India [53, 54, 55]
Area: 3,287,590km2
Population: 1.2 billion
HDI rank: 135
GNI per capita*: $3,910
Proportion of PwD to total population 1.8-2.1%
Unemployment: 26-34%; access to education for children: 47.5% (rural area)-44.4% (urban area)
75% live in rural areas; illiterate: 49%
Total death: NCDs = 60%; cerebrovascular diseases: male 6.7%, female 7.5% (age standard Death Rate: 108.05/100,000 population)
Stroke: crude prevalence rates 90-222/100,000 persons; mortality rate 73/100,000 persons
CRPD ratified: 2007; PwD Equal Opportunities, Protection
of Rights & Full Participation Act (1995); Mental Health
Act (1987); National Policy for Persons with Disabilities (2006)
National Handicapped and Finance Development Cooperation provides loans on concessional terms for self-employment; 3% reservation in employment for PwD in governmental jobs; provision of tax relief for families & PwD
National coordination/funding: Central Coordination Committee and Central Executive disability Committee, under the Ministry of Social Justice & Empowerment
Physicians: 7/10,000 people;
several national institutions and 250 private institutions conduct training courses for rehabilitation specialists
5 composite, 4 regional and 120 district rehabilitation centres, institutions at village, intermediary and district level exits throughout for welfare of PwD
Large rural population, poverty, limited access, financial issues for PwD & cultural taboos about disability.
Currently an upward trend in research in the medical rehabilitation.
.
Sri Lanka
Area: 65,610 km2
Population: 21.1 mil
HDI rank: 73
GNI per capita* : $6,030
1.6% of total population 2001 census (underestimated), according to WHO estimated 3 mil PwD; 14.4% of households
have a member with a disability or with chronic illness (2009/10); Approx. 105,000 persons require P&O services
Total death: NCDs= 75%; cerebrovascular diseases: 6.3%, (stroke 3rd most cause of total death)
SCI: 3000-4000 persons needing continuous rehabilitation services, annual incidence: 250-300 persons;
CP: estimated prevalence is between 2–2.5/1000 live births
CRPD ratified: 2007; Protection of the Rights of Persons with Disabilities Act
(1996); RanaviruSeva Act (1999a); Visually Handicapped
Trust Fund Act (1992); Sri Lanka Federation of the Visually
Handicapped (Incorporation) Act (2007); National Policy on Disability for Sri Lanka (2003)
Total expenditure on health per capita (2012): $189; Total expenditure on health as % of GDP (2012): 3.2;
National coordination/funding: Ministry of Social Services, and National Council for Persons with Disabilities
Ministry of Social Services provides various welfare support for PwD and their families including financial support, assistive devices
Physicians: 6.8/10,000 people; currently employed in government hospitals: 363 PTs; 107 OTs and 35 S<s;8,000 of the 14,000 CBR volunteers;
No trained rehabilitation medicine physicians
Ministry of Health runs 5 rehabilitation hospitals in 5 provinces and has short-term plans to have at least one rehabilitation hospital per province
50 Base Hospitals and District Hospitals also have smaller PT units and 8 physical rehabilitation centres in 6 districts produce P&O devices.
Political stability and social taboos barriers to accessing rehabilitation.
Research in rehabilitation limited mostly to acute care outcomes.
Pacific region
Papua New Guinea [56, 57]
Area: 462,840 km2
Population: 7.2 mil
HDI rank: 157
GNI per capita*: $2,740
PwD: 975,000 people 2% or about 19,500 people receive services;
Disability prevalence range:0.9% to11.1%
Total death: NCDs= 42%; cerebrovascular diseases: 4.1%, (age standard Death Rate: 103.3/100,000 population)
CRPD ratified: 2007-8; Disability Welfare Act (2001); National Policy on Disability (2004); Five-year NationalAction Plan on Disability (2006); National Health Plan 2011-2020 (2011)
Total expenditure on health per capita (2012): $151; Total expenditure on health as % of GDP (2012): 5.2; 20% of health sector expenditure in PNG from donors, with Australia contributing the single largest share.
National coordination/funding: National Department of Health
Physicians: 0.5/10,000 people; 326 medical officers; 2032 allied health workers, 1622 nurses/midwives; 1093 community health workers (2012)
1 national referral hospital, 1 specialist, 4 regional and 16 provincial public
Hospitals;
Free of charge public health and primary health care services; lack of data on rehabilitation
Service delivery fragmented between National Department of Health and provincial governments.
Social taboos about disability and other cultural issues.
Limited rehabilitation research.
Africa
Madagascar
Area: 587,041 km2
Population: 22.2 mil
HDI rank: 155
GNI per capita*: $930
Based on WHO Report on Disability, estimated person with disability 2.8 mil
Total death: NCDs= 39%; cerebrovascular diseases: female 6.4% (age standard Death Rate: 134.9/100,000 population)
CRPD ratified: 2007; National Decade of Disabled Persons (2003), The Madagascar Action Plan 2007–2012
Total expenditure on health per capita (2012): $40; Total expenditure on health as % of GDP (2012): 4.1
Government health spending (2008): 14.6%; 70% of total spending on health; 30% contributed international donors and other private sources
National coordination/funding: Ministry of Health
Physicians: 1.6/10,000 people;
(in 2010) and a total of 3,150 doctors, 5,661 nurses, 385 community health workers
Approx. 3 hospital beds per 10,000 people
No data on any welfare support for PwD & their families.
Limited hospital capacity and education training opportunities.
Research in the medical rehabilitation is limited.
Mauritius [29, 44]
Area: 2,040 km2
Population: 1.2 mil
HDI rank: 63
GNI per capita*: $15,060
Proportion of PwD to total population 5.6%
Unemployment: no data; access to education for children: <4%
Total death: NCDs = 85%; cerebrovascular diseases: male 15.4%, female 18.2% (age standard Death Rate: 142.3/100,000 population);
Incidence per million (2005-9): stroke- 428.3–910, TBI-141.6–299.1, SCI-12.5–23.3
CRPD ratified: 2011; Standard Rules on the Equalization of Opportunities
for Persons with Disabilities (2011)
Total expenditure on health per capita (2012): $784; Total expenditure on health as % of GDP (2012): 4.8
National coordination/funding: Ministry of Health and Quality of Life
Ministry provides various welfare support for PwD and their families
Physicians: <0.5/10,000 people;
(in 2010) P&RM specialists; 4, PT: 17; OT: 29; Dietician: 16; S<: 5; clinical psychologists: 4
Apprx.150 medical institutions providing tertiary, primary, district, and regional health care; 7 major hospitals (bed capacity 2500); 19 private Clinics (807 beds)
The welfare system has not given enough weight to specific disability needs.
Research in the medical rehabilitation is limited.
Ghana
Area: 238,535 km2
Population: 25.2 mil
HDI rank: 138
GNI per capita*: $1,910
Prevalence of disability: 7-12% (women=10.6%; men=6.2%; 64% of adults with disabilities are women; 3 most common types of disability: visual, auditory & physical
Impairments; total years of education=2.41 years; primary education percentage
completion rate:
54%
Total death: NCDs= 42%; Cerebrovascular disease: female 6.1% (age standard Death Rate:81.3/100,000 population)
CRPD ratified: 2007-8; Persons with Disability Act (2006),
Total expenditure on health per capita (2012): $106; Total expenditure on health as % of GDP (2012): 5.2
National coordination/funding: Ministry of Health
Physicians: 1/10,000 people;
Ghana Health Service, responsible for service delivery; Ghana Federation of the Disabled
(1987), encompassing
Ghana Society of the Physically Disabled (1980), Association of the Blind (1963), National Association
of the Deaf (1968), Parents Association of Children with Intellectual Disability (2001), Association
of Persons Living with Albinism (2003), andShare Care Ghana (2006)
Attitudinal challenges to full socioeconomic inclusion of PwD.
Built physical environment lacks key accessibility tools that enable social inclusion.
Institutional challenges for PwD cuts across medical, financial, publichealth, social science, and religious arenas.
(Main source: WHO Country Profile; WHO Health Statistics 2011, WHO Global Info base, UN Human Development Report 2014, Handicap International report 2014 [26]).
*Purchasing power parity (PPP) in US$.
CBR: Community based rehabilitation; CP: Cerebral palsy; CRPD: Convention on the Rights of Persons with Disabilities; HDI: Human development index; GDP: Gross Domestic Product; GNI: Gross National Income; OT: Occupational therapists; NCDs = non-communicable diseases; P&O: Prosthetics and orthotics; PM&R: Physical Medicine and Rehabilitation; PT: Physiotherapists; PwD: persons with disability; SCI: Spinal cord injury; SLTs: Speech and Language Therapists; TBI: Traumatic brain injury; WHO: World Health organisation.
Table 2: Summary of current health status, systems and resources for disability in some developing countries.
Despite presence of comprehensive policies, their implementation remains limited in terms of geographical coverage, shortage of trained workers and unclear referral mechanisms between public health services and neurorehabilitation services. Huge challenges exist in many countries in terms of accessibility and lack or poorly developed healthcare infrastructure. Further, medical rehabilitation is yet to be recognised by PwD and their families [44]. In African countries, term ‘rehabilitation’ still has very misleading connotations of patient passivity and dependency [45], while in other countries like Pakistan the term rehabilitation is perceived as just physiotherapy or exercise alone [28,46] (Case study 1). As majority of rehabilitation services are being provided and funded by international donors and organisations, the security situation in some regions (such as Afghanistan, Pakistan) have restricted these organisations to expand their services to rural areas and sustainability of the few existing services is at risk [26]. In countries like Australia where, various major policies, projects and initiatives have been developed to address health issues, including health for PwD, there is still a wide gap between the health status of Indigenous people and that of other Australians (Case study 2). In Mauritius, there has been significant improvement in its health care system, especially in acute care sector (such as frontline services and procedures e.g. cardiac surgery) and controlling communicable diseases, however, post-acute care, including neurorehabilitation is still problematic at many levels (Case study 3) [29,44]. While in Madagascar, the concept of rehabilitation is still in early stages with many limitations (Case study 4).
Case study 1: Neuro-rehabilitation in Pakistan
Pakistan is a low-middle income country (area of 803,940 km2 and population of 180 million) with relatively under-developed and varied health care system between the rural and the urban areas. It is ranked 146th in Human development Index, with Gross National Income per capita of US $ 2,880. In recent years there is increased awareness about NCDs and physical disabilities. There are currently over 188,000 doctors (8.3 physicians/10,000 people) registered with the Pakistan Medical and Dental Council , and 170 trained neurologist -majority based in urban areas.
Rehabilitation is in infancy in Pakistan and confused with ‘physiotherapy and exercises’ alone by many health care professionals and general public. In 1997 College of Physicians and Surgeon of Pakistan (CPSP) recognized Physical Medicine and Rehabilitation (PM&R) as a specialty and started the 4-year Fellowship training program. To date 48 physicians have successfully qualified the PM&R Fellowship, and majority (30) are working in the military facilities; while only 15 PM&R physicians in the private and public health sector for majority of the PwD in Pakistan. Many medical schools and hospitals do not have specialised rehabilitation departments; and there is limited undergraduate teaching of rehabilitation medicine. Currently, there are estimated 1700 Physiotherapists in Pakistan and 1300 expected to graduate within one year. There are less than 200 trained occupational therapists, 250 speech and language therapists and no formally trained nurses in neuro-rehabilitation.
Data regarding disability and burden of neurological diseases is sparse and mostly comes from hospital- based studies conducted in tertiary care medical institutes/hospitals located in major cities. There is no national registry for stroke, neurological disorders or physical disabilities. The last national census was conducted in 1998 and disability was vaguely documented. There is a huge burden of neurological disorders, including stroke, with about 1,000 people diagnosed every day, out of which 400 die. The age standard total death rate from cerebrovascular disease is estimated to be 117.9/100,000 population. There are no comprehensive stroke units and only two centers in the country offer thrombolysis and six hospitals offer coordinated stroke services. Majority of stroke cases are managed in general medical wards, which often lack follow up, plan or referral for stroke rehabilitation. There are also some centers for spinal cord injuries run by NGOs such as International Red Crescent. The neurorehabilitation services for others e.g., multiple sclerosis, brain disorders (including traumatic brain injury (TBI), brain tumours), neuro-degenerative disorders are yet to be established.
There are only two institutes of PM&R in the country: Armed Forces Institute of Rehabilitation Medicine primarily catering for the military and another in private sector. There are no uniform protocols or guidelines for management of different neurological disabilities and rehabilitation is mostly neglected in official guidelines. For example, the clinical practice guidelines of the Pakistan Society of Neurology, reference the word “rehabilitation” only at 4 occasions, without any detail. There are many NGOs working in Pakistan in the field of disability but their focus is mainly on the social aspects and philanthropic support rather than comprehensive medical rehabilitation. There is no central body for the oversight and coordination, resulting in frequent duplication of effort. There is lack of funding not only for comprehensive management of neurological conditions, but for overall disability management and minimal awareness regarding neurorehabilitation amongst the public and health care professionals, who still practice traditional medical model rather than rehabilitation model for functional restoration and improvement in quality of life. Other barriers include lack of awareness and the perception of neurological disability as an end -oflife situation.
Source: Pakistan Medical and Dental Council, Rathore FA et al 2011, Rathore FA et al 2007 [28,46,47].
Case study 2: Indigenous health in Australia
The Australian Bureau of Statistics (2013) estimate suggests 700,000 indigenous Australians, these compared with their nonindigenous counterparts suffer ill-health, such as:
- Infant mortality rate 3 times higher than the national average.
- Age-standardised death rate 1.9 times higher and life expectancy around 10-11 years less.
- Age-standardised separation rate due to hospitalisation 2.5 times higher.
- Cardio-vascular disease (CVD) 1.2 times more common, with age-adjusted death rate from CVD 1.7 times higher.
- Diabetes 3.3 times more common.
- 2.7 times more likely to feel high or very high levels of psychological distress.
- Hospitalisation rate for injury 2.0 times higher.
- 42% of aged 15 years or older were employed and 17% were unemployed.
- Mean equalised gross household income 41% less.
Disability is a major issue in indigenous population, with 50% aged 15 years and over reporting some form of disability or a longterm health condition, in 2008. Further, 7.9% of all Indigenous people require assistance with core activities (i.e. had a profound/ core activity restriction), which is 2.2 times higher compared to other Australians. One third (36%) of indigenous people with a disability or long-term health condition had problems accessing health care services and one in three (32%) adults experienced discrimination in the previous 12 months.
In response to the Social Justice Report 2005, highlighting the vast gap between the health of Indigenous and other Australiansthe Australian government through the Council of Australian Governments (COAG) initiated ‘Closing the Gap’ commitment to achieve Indigenous health equality within 25 years. The National Disability Agreement (NDA) was further developed by the COAG to improve the outcomes for Indigenous people with disability. As a part of NDA, the National Indigenous Access Framework was initiated to ensure that the needs of Indigenous people with disability are addressed through accessible and appropriate service delivery, which includes accommodation, support, community support, community access, respite and employment services. The NDA support services were used by 41% population aged 0-64 years. In 2008, an advisory body for the government on the achievement of equitable and sustainable health outcomes in indigenous population, the National Indigenous Health Equality Council was established.
Despite various initiatives and policies, there remains a wide gap between the health status of Indigenous people and that of other Australians, particularly in disability. Rehabilitation services are limited in remote areas where majority of Indigenous Australians reside. Most services are either institutional-based and/or run by outreach services and many Aboriginal communities get limited access to institutional services, due to geographical distance, costs, culture and language. Other barriers in service provision are similar to those of developing countries, including: workforce shortages and staff-turnover, lack of awareness, inadequate communication across care sectors, geographical landscape, socioeconomic and other issues in rural and remote Australia.
Source: Australian Bureau of Statistics, Australian Indigenous Health Info Net [48,49].
Case study 3: Neurological rehabilitation in Mauritius
Mauritius has had an upsurge of NCDs, including neurological conditions. The period incidence-rate and period-prevalence rate for stroke (2005-09) ranged from 300.6 to 622.9 and 352.1 to 882.6 per 100,000 population, respectively. Stroke represented 26.5% of all deaths recorded from cerebrovascular diseases. The incidence rate and prevalence rate for TBI was slightly lower, ranging from 95.3 to 216.8 and 98.8 to 233.7 per 100,000 populations, respectively. While the incidence rate for spinal cord injury (SCI) ranged from 8.8-16.8 per 100,000 populations.
There are few trained rehabilitation specialists in the country. As of 2009, there were 1,500 doctors in the public and private sectors, 4 PM&R specialists (no neurorehabilitation specialists), only 17 physiotherapists and 33 assistants employed by the government, with one PT seeing almost 200 patients per day and thus delegating care to assistants. There are limited training programs for rehabilitation specialists in the academic institutions to date. Although, acute facilities for diagnostics (Computer Tomography Scan, Medical Resonance Imaging) and treatment (neurosurgery, cardiology, cardiac surgery and thrombolysis for stroke), have made significant progress in Mauritius; adequate long-term care for neurologically disabled, including rehabilitation is yet to be developed.
The Ministry of Health oversees the Community-Based Rehabilitation (CBR) programs, which do not focus exclusively on patients who need neurorehabilitation. However, regular home visit initiatives for the elderly under the CBR, provides some indirect benefit for neurologically disabled individuals. The government provides various welfare benefits for PwD (and their families) including financial support, assistive devices, advocacy, counseling, concessions for adults and refund transportation costs for disabled children (accompanying parents) attending schools, customs duty exemption on specially adapted cars. However, this system has not given enough weight to specific disability needs and PwD (and their relatives) are not aware and often fail to claim such benefits. Further, limited available resources could be utilized more appropriately.
The barriers in service provision for neurorehabilitation include: minimal access to healthcare services, weak coordination amongst the healthcare professionals and facilities, lack of adequate management in the community (such as home care; specialised equipment), inadequate human resources, lack of provision of infrastructure accessible for PwD and cultural stigma.
Source: MRC report 2012, Soopramanien A 2012 [29,44].
Case study 4: Rehabilitation services in Madagascar
Madagascar is the fourth largest island in the world situated in the Indian Ocean, with over 22.2 million inhabitants. There is no epidemiological data on disability in Madagascar. However, according to WHO’s World Report on Disability prevalence figures equates to 2.8 million PwD in Madagascar. Madagascar ratified National Decade of Disabled Persons 2003-2013 in 2002 in accordance with the continental plan of action of the African Decade and the UN CRPD in 2007.
The health system is struggling, due to unstable political situation, poverty, high illiteracy, and decrease in international aid. Access to medical care is limited for the general population, and especially for PwD and those living in rural areas accessibility and affordability are the main barriers. Further, disability is still perceived as a curse and/ or contagious disease in many parts of the country and PwD are often isolated and marginalized.
There are estimated 1.6 physicians, less than 1 physiotherapist and an average of 3 hospital beds per 10,000 populations. Majority of hospitals and medical facilities are concentrated in urban areas (mainly the capital). Despite these barriers to access, health services have shown a trend toward improvement over the past 2 decades. In the last 5 years, some development has occurred in rehabilitation. It is one of few sub-Saharan African countries with established rehabilitation network. The Malagasy Department of Health in conjunction with a UK based Charity commenced post-graduation training in rehabilitation, (including neurorehabilitation) at the University of Antananarivo. To date there are 10 rehabilitation specialists in the country, including 8 recently completed the post-graduate course. Other progress includes the newly formed National Association of Rehabilitation Medicine, which hosted its first national congress in practice for cerebral palsy. Spinal cord rehabilitation is planned for commencement in tertiary hospitals in 2015. The communication and collaboration between rehabilitation and acute care sector health care professionals is minimal. There are some grassroots associations for PwD mainly funded and provided by the NGOs and charitable organisations, such as the National Collective of Organizations Working for Disabled Persons, Handicap International, and Christian Blind Mission etc.
Source: Disability World [50]; World Health Statistics 2011 [51] and Author’s personal experience and communication with experts in Madagascar
On a positive note, there are countries that have made significant leaps in developing rehabilitation programs for PwD, such as India. India was one of the first countries to sign and ratify the UN Convention, and established the Rehabilitation Council of India (RCI) in 1986 [52]. In 1993, the Indian Parliament enacted the RCI Act and set it up as Statutory Body. The RCI currently regulates and monitors services given to PwD, develops education curriculum and maintains a Central Rehabilitation Register of all qualified professionals and personnel working in the field of Rehabilitation and Special Education. The trend of year-wise status of registration of rehabilitation professionals and personnel in the Central Rehabilitation Register has quadrupled from 2001-2 (20,118 registration) to 2012-13 (78,514 registrations) [52]. India has a long tradition of implementing CBR programs, involving the families and caregivers with good effect using local traditions. Use of technology such as mobile phone apps have also been developed to facilitate communication and education programs for PwD. Stroke and Spinal cord rehabilitation are well developed in urban areas, however, issues such as infrastructure, trained personnel etc. for rural populations are similar to those in other developing countries.
Discussion
Neurological conditions are complex and require specialized services for comprehensive management. The global increase in prevalence of neurological conditions has affected disability and added
to the economic burden for national healthcare systems, particularly in low-resourced countries. Despite significant improvements in the acute health care systems in many developing countries, health policies have not extended to include rehabilitation services. For survivors of neurological insults (such as SCI, TBI, or stroke), structured long-term neurorehabilitation and NGOs for specific neurological disability are limited or do not exist. In many countries (including developed countries like Australia) most neurorehabilitation programs exists in ‘silos’. Neurorehabilitation has evolved beyond conventional medical views to include consideration of needs of PwD, their function and social reintegration. It is an expensive resource; and the evidence to support specific neurorehabilitation interventions has long been neglected. The emerging advances in information and communication technology provide opportunities for alternative efficient and cost-effective method to deliver therapy using web-based devices (computer, mobile phones etc.) in a settings convenient for patients, such as telerehabilitation in-home, by minimising the barriers of distance, time, cost and healthcare system load [58]. The benefit and applicability of telerehabilitation/ telehealth for persons with neurological conditions have been well documented in literature [58]. Further, there is a trend in progress towards ‘Universal Health Coverage’ in many countries worldwide, such as increasing enrolment in government health insurance, a movement towards expanded benefits packages, decreased out-ofpocket spending and increased government spending on health [59]. There is imperative for greater awareness of the gaps in resources for neuro rehabilitative care, to assist health planners and policy-makers to identify areas for urgent attention and planning.
The DAP provides comprehensive summary actions to tackle global disability and offers governments, policy makers, and other relevant stakeholders a blueprint for implementing the recommendations of the World Disability Report and CRPD, and facilitate social inclusion of persons with neurological conditions. Some recommendations to facilitate the process of implementation and change in practice include: the DAP actions should not be taken as a conceptual framework or academic information only, but used in practice at all levels of society; all involved partners and stakeholders should follow a rigorous process with effective and regular communication, in the implementation process. Further, although implementation is voluntary, the UN Member States, and partners should not interpret the DAP as lenient regulation, but adapt as legislation. Potential challenges/barriers ahead for global diffusion and implementation of the DAP, depends upon the country’s health system to perform four vital functions: service provision, resource generation, funding and stewardship [12].
Summary
The significant longer-term health consequences of neurological conditions in low-resource countries can overwhelm the person (caregivers), society and the health system. The DAP sets up an agenda for all sectors of society for collaborative effort for successful implementation. Some of the recommendations to facilitate implementation of the DAP in neurorehabilitation in low-resource countries include:
- A systematic approach to building health care systems and processes for integrated neurorehabilitation services from acute care through to community; and inclusion of primary health care.
- Set up a Global Health Fund using forums like the G20 to mobilize funding role in emerging countries, as these are especially relevant to neurological conditions with complex longer-term disability.
- Bilateral assistance for persons with neurological disability: health security/macroeconomics, financial - Universal health coverage (such as ‘Medicare’ in Australia), job creation, resources tailored to country characteristics (governance, policy, mindset etc.).
- To keep foreign multilateral and private agencies focusing on neurorehabilitation as instruments of aid, grants, concessions, aid-in-kind etc. under contractual laws.
- Time-based outcomes using the DAP with bilateral agencies working with other agencies, using multisectorial approach, new partnerships, strategic collaboration, provision of technical assistance, research and development.
- Investment in education and skill-development of neurorehabilitation professionals.
- Capacity building for a strong interdisciplinary workforce for neurorehabilitation.
- Post-2015 Millennium development goals should focus on sustainable neurorehabilitation programs, a governmental approach and resource scarcity.
- Infrastructure and IT support for sustainable health care for neurorehabilitation to drive economic growth and support health security.
- Governance support for strengthening neurorehabilitation health care systems through logistics, surveillance and service delivery.
Acknowledgment
This review was supported from internal resources of the Rehabilitation Department, Royal Melbourne Hospital, Royal Park Campus, and Melbourne, Australia.
Authors’ Contribution
FA and BA were involved in all aspects of the review. FA and BA coordination and prepared the final draft of the manuscript. HM provided valuable input into design and critically reviewed the manuscript. FR provided valuable assistance with the case studies and discussion. All authors read and approved the final manuscript.
References
- World Health Organization. World Report on Disability. Geneva: WHO; 2011.
- World Health Organization. Promoting access to healthcare services for persons with disabilities, in Disability and rehabilitation. Geneva: WHO; 2006.
- Bethge M, von Groote P, Giustini A, Gutenbrunner C. The World Report on Disability: a challenge for rehabilitation medicine. Am J Phys Med Rehabil. 2014; 93: S4-11.
- United Nations General Assembly. Keeping the promise: realizing the Millennium Development Goals for persons with disabilities towards 2015 and beyond: Report of the Secretary-General, New York: UN; 26 July 2010.
- Giles LC, Cameron ID, Crotty M. Disability in older Australians: projections for 2006-2031. Med J Aust. 2003; 179: 130-133.
- Organisation for Economic Co-Operation and Development. Sickness, disability and work: keeping on track in the economic downturn (Background paper). Paris: OECD; 2009.
- South-North Centre for Dialogue and Development. Global survey of government actions on the implementation of the standard rules of the equalisation of opportunities for persons with disabilities. Amman: Office of the UN Special Rapporteur on Disabilities; 2006.
- Lindstrom A. Appropriate technologies for assistive devices in low-income countries. In: Hsu JD, Michael JW, Fisk JR, editors. AAOS Atlas of orthoses and assistive devices. Philadelphia: Mosby/Eslevier; 2008.
- Wooding S, Raphael B. Psychological impact of disasters and terrorism on children and adolescents: experiences from Australia. Prehosp Disaster Med. 2004; 19: 10-20.
- South-North Centre for Dialogue and Development. Global survey of government actions on the implementation of the standard rules of the equalisation of opportunities for persons with disabilities. Amman: Office of the UN Special Rapporteur on Disabilities; 2006.
- Khan F, Turner-Stokes L, Ng L, Kilpatrick T. Multidisciplinary rehabilitation for adults with multiple sclerosis. Cochrane Database Syst Rev. 2007; : CD006036.
- World Health Organization. Neurological disorders: public health challenges. Geneva: WHO; 2006.
- Department of Health. National Services Framework (NSF) for Long-term Conditions. Leeds: DH; March 2005.
- Australian Rehabilitation Alliance. The need for a National Rehabilitation Strategy: working towards a clear and united rehabilitation strategy for Australia (Position Statement). Canberra: ARA; 10 August 2011.
- Khan F, Amatya b, NgL, Drummond K, Olver J. Multidisciplinary rehabilitation after primary brain tumour treatment. Cochrane Database Syst Rev. 2013; 1: CD009509.
- World Health Organisation. The International Classification of Functioning, Disability and Health. Geneva: WHO; 2001.
- Royal College of Physicians, National Council for Palliative Care, and British Society of Rehabilitation Medicine. Long-term neurological conditions: management at the interface between neurology, rehabilitation and palliative care. Concise Guidance to Good Practice series, No 10. London: RCP; 2008.
- Turner-Stokes L, Sykes N, Silber E, et al. From diagnosis to death: exploring the interface between neurology, rehabilitation and palliative care in managing people with long-term neurological conditions. Clin Med. 2007; 7: 129-136.
- United Nations. Convention on the Rights of Persons with Disabilities. 2006.
- World Health Organization and World Federation of Neurology. Atlas: country resources for neurological disorders. Geneva: WHO; 2004.
- Janca A, Prilipko L, Costa e Silva JA. The World Health Organization's work on public health aspects of neurology. J Neurol Neurosurg Psychiatry. 1997; 63 Suppl 1: S6-7.
- World Health Organization. WHO global disability action plan 2014–2021: Better health for all people with disability. In: Sixty-seventh world health assembly- A67/16. Provisional agenda item 13.3. Geneva: WHO; 2014.
- Bhatia M, Joseph B. Rehabilitation of cerebral palsy in a developing country: the need for comprehensive assessment. Pediatr Rehabil. 2000; 4: 83-86.
- Walgenbach P. The production of distrust by means of producing trust. Organisation Stud. 2001; 22: 693-714.
- Mannan H, Eltayeb S, Maclachlan M, Amin M, McVeigh J, Munthali A, et al. Core concepts of human rights and inclusion of vulnerable groups in the mental health policies of Malawi, Namibia, and Sudan. Int J Ment Health Syst. 2013; 7: 7.
- Axelsson C. Mapping report of physical rehabilitation services in Afghanistan, Bangladesh, Odisha (India) & Sri Lanka., Handicap International, 2014.
- Tuakli-Wosornu YA, Haig AJ. Implementing the World Report on Disability in West Africa: challenges and opportunities for Ghana. Am J Phys Med Rehabil. 2014; 93: S50-57.
- Rathore FA, New PW, Iftikhar A. A report on disability and rehabilitation medicine in Pakistan: past, present, and future directions. Arch Phys Med Rehabil. 2011; 92: 161-166.
- Soopramanien A. Mauritius calling: medical care and neurorehabilitation needs in an oceanic idyll. Arch Phys Med Rehabil. 2012; 93: 2377-2381.
- World Health Organization. Disability and rehabilitation status review of disability issues and rehabilitation services in 29 African Countries. Geneva: WHO; 2004.
- World Health Organization, Swedish Organizations of Disabled Persons International Aid Association. Part 1. Community-Based Rehabilitation as we experienced it - voices of persons with disabilities. Geneva: WHO; 2002.
- Parnes P, Cameron D, Christie N, Cockburn L, Hashemi G, Yoshida K. Disability in low-income countries: issues and implications. Disabil Rehabil. 2009; 31: 1170-1180.
- Worrall LE, Howe T, O'Callaghan A, Hill AJ, Rose M, Wallace SJ, et al. The World Report on Disability as a blueprint for international, national, and local aphasia services. Int J Speech Lang Pathol. 2013; 15: 106-112.
- Digiacomo M, Davidson PM, Taylor KP, Smith JS, Dimer L, Ali M, et al. Health information system linkage and coordination are critical for increasing access to secondary prevention in Aboriginal health: a qualitative study. Qual Prim Care. 2010; 18: 17-26.
- Turner-Stokes L, Sykes N, Silber E; Guideline Development Group. Long-term neurological conditions: management at the interface between neurology, rehabilitation and palliative care. Clin Med. 2008; 8: 186-191.
- Kusumastuti P, Pradanasari R, Ratnawati A. The problems of people with disability in Indonesia and what is being learned from the World Report on Disability. Am J Phys Med Rehabil. 2014; 93: S63-67.
- Mitra S, Findley PA, Sambamoorthi U. Health care expenditures of living with a disability: total expenditures, out-of-pocket expenses, and burden, 1996 to 2004. Arch Phys Med Rehabil. 2009; 90: 1532-1540.
- Mitra S, Sambamoorthi U. Disability prevalence among adults: estimates for 54 countries and progress toward a global estimate. Disabil Rehabil. 2014; 36: 940-947.
- Eide AH, Øderud T. Assistive technology in low income countries. In: Maclachlan M, Swartz L, editors. Disability and international development. Dordrecht, Netherlands: Springer; 2009.
- Kuyini AB, Alhassan AR, Mahama FK. The Ghana community-based rehabilitation program for people with disabilities: what happened at the end of donor support? J Soc Work Disabil Rehabil. 2011; 10: 247-267.
- McAllister L, Wylie K, Davidson B, Marshall J. The World Report on Disability: an impetus to reconceptualize services for people with communication disability. Int J Speech Lang Pathol. 2013; 15: 118-126.
- Elrod CS, DeJong G. Determinants of utilization of physical rehabilitation services for persons with chronic and disabling conditions: an exploratory study. Arch Phys Med Rehabil. 2008; 89: 114-120.
- Lang R. Empowerment and CBR? Issues raised by the South Indian experience (Chapter 9). In: Stone E, editor. Disability and Development: Learning from action and research on disability in the majority world. Leeds: The Disability Press; 1999; p. 130-148.
- Mauritius Research Council. Needs assessment on neurological rehabilitation services in Mauritius. Mauritius: MRC; 2012.
- Kurawa SS. The impact of disability on self and society: an agenda for research on rehabilitation of disabled in Nigeria. Procedia Soc Behav Sci. 2010; 5: 1804-1810.
- Rathore MF, Rashid P, Butt AW, Malik AA, Gill ZA, Haig AJ. Epidemiology of spinal cord injuries in the 2005 Pakistan earthquake. Spinal Cord. 2007; 45: 658-663.
- Pakistan Medical and Dental Council. Statistics.
- Australian Bureau of Statistics. 4727.0.55.003 - Australian Aboriginal and Torres Strait Islander Health Survey: Biomedical Results. 2012-13.
- Australian Indigenous Health Info Net. Overview of Australian Indigenous health status, 2013. 2014.
- Razafinjato F. Madagascar: the official launch of the Decade of Disabled Persons.
- World Health Organization. World health statistics 2011. Geneva: WHO; 2011.
- Rehabilitation Council of India. 26th Annual Report 2012-13. New Delhi: RCI; 2013.
- Bhaumik S. Study stokes debate over patterns of non-communicable disease in India. BMJ. 2013; 347: f4695.
- Dalal PM, Bhattacharjee M. Stroke epidemic in India: hypertension-stroke control programme is urgently needed. J Assoc Physicians India. 2007; 55: 689-691.
- Dalal P, Bhattacharjee M, Vairale J, Bhat P. UN millennium development goals: can we halt the stroke epidemic in India? Ann Indian Acad Neurol. 2007; 10: 130-136.
- WHO and the National Department of Health. Health Service Delivery Profile: Papua New Guinea. Geneva: WHO; 2012.
- Shaw A. Rehabilitation services in Papua New Guinea. P N G Med J. 2004; 47: 215-227.
- Khan F, Amatya B, Kesselring J, Galea M. Telerehabilitation for persons with multiple sclerosis. Cochrane Database Syst Rev. 2015; 4: CD010508.
- Lagomarsino G, Garabrant A, Adyas A, Muga R, Otoo N. Moving towards universal health coverage: health insurance reforms in nine developing countries in Africa and Asia. Lancet. 2012; 380: 933-943.