
Special Article – Physical Rehabilitation
Phys Med Rehabil Int. 2016; 3(2): 1082.
Physical Therapy in Wilson’s Disease: Case Report
Maiarú M*, Garcete A, Drault ME, Mendelevich A, Módica M and Peralta F
Instituto de Rehabilitación Psicofísica, Buenos Aires, Argentina
*Corresponding author: Maiarú M, Instituto de Rehabilitación Psicofísica, San José 819, Floor 2, Department 5, Ciudad Autónoma de Buenos Aires, Argentina
Received: April 03, 2016; Accepted: May 10, 2016; Published: May 13, 2016
Abstract
Case Presentation: A 32 years old male patient, diagnosed 16 years ago. He walks by himself with notorious unsteadiness. The evaluation was directed to gait and balance disorders. The treatment was based on three aspects: static balance, dynamic balance and functional capacity exercises. Results from all evaluations showed post-treatment improvement. After the treatment, the difference achieved between the usual gait speed and the maximum gives the possibility to the patient to vary greatly in speed, which is proposed as a marker of potential for adaptation to different environments and task demand. Improvement in Timed Up and Go was enough to overcome the cut-off point that predicts risk of falls in people with PD (11.50 seconds). This report is, to our knowledge, the first to describe an approach to physical therapy for movement disorders present in Wilson’s disease.
Keywords: Wilson’s disease; Rehabilitation; Movement disorders; Physical therapy
Case Presentation
A 32 years old male patient diagnosed with neurological symptomatic Wilson’s Desease (WD). Regarding family history, he has a sister with a pre-symptomatic diagnosis of the same disease.
In 1996, at the age of 14, the patient is admitted for presenting a clinical picture of bradykinesia, rigidity and gait disturbance for which required assistance. Through a nuclear magnetic resonance brain study which showed hyper intense lesions in basal ganglia, together with the presence of the Kayser-Fleischer ring, in 1998 the patient was diagnosed with WD, for which drug treatment begins.
In 2014, generalized dystonia is evident with lower limbs prevalence which hindered the gait, causing recurrent falls according to the patient’s report. In September of the same year the patient’s medical team decided to work in consultation with Instituto de Rehabilitación Psicofísíca (I.Re.P.) to begin rehabilitation. The patient was under medication with strict control of his neurologist, the medication did not change in the year before start or during the physical therapy treatment.
The patient presents walking independently without walking aid or assistance of another person to the initial kinesic evaluation. He reported having recurrent falls, near-falls per day in the last week, so the Timed Up and Go (TUG) was evaluated [1]. Gait speed was measured using the 10 meter walk test (10MWT), the static balance using the Clinical Test for the Sensory Interaction on Balance (mCTSIB) [2], the dynamic balance using the Functional Gait Assessment (FGA) and confidence in balance using Activities-specific Balance and Confidence Scale (ABC Scale). Results from all tests and scales evaluated pre and post intervention are grouped in Table 1.
The patient gave written informed consent for the presentation of this case report.
Kinesic Treatment
Treatment goals were to reduce the risk of falls and the difficulty to overcome architectural barriers. The treatment was based on static and dynamic balance exercises and on functional capacity training.
Treatment frequency was 2 times a week for 2 months and 20 days, along with a plan of home exercises to be held 3 times a week.
Exercises aimed at improving static balance
The training began with standing exercises, on a stable surface, with feet together, semi-tandem and tandem, trying to improve them up to the one-foot standing position [3]. In these positions the patient was trained with his eyes closed trying to modify sensory weighting in favour of somatosensory information [4]. These exercises were performed in 4 series of 1 minute duration with 3 minutes breaks.
Exercises aimed at improving dynamic balance
This training was done on a treadmill under kinesiologist supervision. Initially the patient could not keep up the gait without the help of his upper limbs, so the first goal was to get stability to achieve release. Once this was achieved, the gait was performed with horizontal and vertical head turns [4]. In the later stages of treatment, the patient performed gait on treadmill with eyes closed. A cognitive task was added to these exercises as a variant of difficulty [5]. The dosage was delivered according to the patient’s tolerance, allowing him to perform cycles of approximately 3 minutes with breaks of 5 minutes this type of training lasted approximately 1 hour per session.
Exercises aimed at functional capacity training
This training stage was aimed at patient’s daily activities in which he found some difficulties, for instance, walking up and down stairs or ramps, picking up objects from the floor and unstable surface gait [4,5]. The patient was dosed according to his tolerance, with rest periods between 3 and 5 minutes, with a total time of 30 minutes.
The session ended with stretching of the muscles of the lower limbs for 15 minutes.
The treatment presented no problems or associated injuries in its development. On the other hand, the patient reported being satisfied with it.
In the final evaluation, the patient showed a genuine self-reported improvement in balance confidence with ABC scale and near-falls per day during the last week, and it was objectified by the TUG, 10MWT, FGA, CTSIB-M tests (Table 1).
Initial evaluation
Final evaluation
Difference
Cut-off point
TUG
15.6 s
12.1 s
3.5 s
> 11.5 s
10MWT
usual speed
0.87 m/s
1.19 m/s
37%
-
10MWT
maximum speed
1.25 m/s
1.92 m/s
53%
-
Speed
difference0.38 m/s
0.73 m/s
92.1%
-
FGA
12/30 points
19/30 points
7 points
<15/30
Near-falls /day
Last week
1
0
1
-
ABC scale
60%
71.2%
11.2%
69%
mCTSIB
Normal
Normal
Without difference
-
TUG: Timed up and go; TM10m: 10 Meter Walk test; FGA: Functional Gait Assessment; ABC scale: Activity Balance Confidence scale; mCTSIB: modified Clinical Test for the Sensory Interaction on Balance; s: seconds; m/s: metres per second.
Table 1: Test results and scales evaluated pre and post intervention.
Discussion
The kinesic approach to this pathology is still based on empirical principles due to the limited evidence available, as works consulted do not provide information about physical therapy.
After the treatment, the difference achieved between the usual gait speed and the maximum gives the possibility to the patient to vary greatly in speed, which is proposed as a marker of potential for adaptation to different environments and task demand [6].
The changes observed in the FGA, with the cut-off point 15/30 as assessed by Leddy et al. in 2011 in patients with Parkinson’s disease (PD), indicate that the patient stopped having risk of falls (Figure 1) [7]. In the ABC scale the patient exceeded the minimum detectable change of 11.12% suggested for people with PD, and also exceeded the 69% cut-off point suggested by Mak & Pang in 2009 as a fall predictor after one year of follow up for the same people [8]. Improvement in TUG was enough to overcome the cut-off point that predicts risk of falls in people with PD (11.50 seconds) as reported by Nocera et al. in 2013 [9].
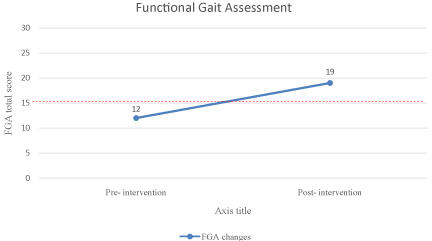
Figure 1: Functional Gait Assessment.
As constraint, we have not found assessment tools validated in this patient population. Due to the patient moved to another city, it was not possible to make a follow up. As the WD is considered Parkinsonism, according to the International Classification Diseases to Neurology, it was decided to use the tests and cut-off points validated in this population [10].
Conclusion
This case report is, to our knowledge, the first to describe an approach to physical therapy on movement disorders present in WD, more specifically on gait and balance disorders. We consider necessary to carry out further research on different interventions that serve to justify and improve the physiotherapy approach in movement disorders.
References
- Maidan I, Freedman T, Tzemah R, Giladi N, Mirelman A, Hausdorff JM. Introducing a new definition of a near fall: intra-rater and inter-rater reliability. Gait Posture. 2014; 39: 645-647.
- Mancini M, Horak FB. The relevance of clinical balance assessment tools to differentiate balance deficits. Eur J Phys Rehabil Med. 2010; 46: 239-248.
- Schoneburg B, Mancini M, Horak F, Nutt JG. Framework for understanding balance dysfunction in Parkinson's disease. Movement disorders: official journal of the Movement Disorder Society. 2013; 28: 1474-1482.
- Herdman SJ. Vestibular Rehabilitation, 3rd ed. Philadelphia: F. A. Davies Company; 2007.
- An HJ, Kim JI, Kim YR, Lee KB, Kim DJ, Yoo KT, et al. The effect of various dual task training methods with gait on the balance and gait of patients with chronic stroke. J Phys Ther Sci. 2014; 26: 1287-1291.
- Steffen TM, Hacker TA, Mollinger L. Age- and gender-related test performance in community-dwelling elderly people: Six-Minute Walk Test, Berg Balance Scale, Timed Up & Go Test, and gait speeds. Phys Ther. 2002; 82: 128-137.
- Leddy AL, Crowner BE, Earhart GM. Functional gait assessment and balance evaluation system test: reliability, validity, sensitivity, and specificity for identifying individuals with Parkinson disease who fall. Phys Ther. 2011; 91: 102-113.
- Mak MK, Pang MY. Fear of falling is independently associated with recurrent falls in patients with Parkinson's disease: a 1-year prospective study. J Neurol. 2009; 256: 1689-1695.
- Nocera JR, Stegemöller EL, Malaty IA, Okun MS, Marsiske M, Hass CJ; National Parkinson Foundation Quality Improvement Initiative Investigators . Using the Timed Up & Go test in a clinical setting to predict falling in Parkinson's disease. Arch Phys Med Rehabil. 2013; 94: 1300-1305.
- World Health Organization. Application of the International Classification of Diseases to Neurology. 2 ed. Geneva, Switzerland: World Health Organization; 1997.