
Special Article – Cerebral Palsy
Phys Med Rehabil Int. 2016; 3(3): 1086.
Cerebral Palsy in the 21st Century: Cerebellar Injury in the Survivors of Extreme Prematurity
Bodensteiner JB*
Department of Neurology and Pediatrics, Mayo Clinic, 200 First Street SW, Rochester, MN, USA
*Corresponding author: John B. Bodensteiner, Department of Neurology and Pediatrics, Mayo Clinic, 200 First Street SW, Rochester, MN, USA
Received: April 12, 2016; Accepted: June 21, 2016; Published: June 23, 2016
Abstract
The face of cerebral palsy is changing in the 21st century. Infants who are born extremely prematurely (Less than 1Kg and Less than 28 weeks of gestation) are surviving in increasing numbers, both with and without brain injury. The incidence of cerebral palsy is between 10 and 15% in these patients. As a result they account for an increasing proportion of patients with cerebral palsy. In this paper I review the classical forms of CP as defined by neurological criteria and then discuss some of the more or less unique features of cerebral palsy in the survivors of extreme premature birth.
Keywords: Cerebral Palsy; Extreme prematurity; Cerebellar injury; Pseudobulbar affect
Introduction
Cerebral palsy has been around as long as Homo sapiens. The definition of the condition we call Cerebral Palsy (CP) varies widely among health care providers depending on the orientation of the individual provider involved. For some, the presence of a nonprogressive dysfunction of the central nervous system that affects the motor function of the individual is sufficient for the diagnosis. I believe, however, that a more discriminating definition is useful if the physician is to draw conclusions about the etiology, management and prognosis of the patient and his/her motor disability. To state it differently, from the standpoint of the neurologist, the term CP should be used when the injury which results in motor disability is stable and non-progressive, occurs at or near the time of birth, involves a previously normal and obviously immature nervous system, and affects the motor system (at least). In this definition the etiology and the timing of the brain injury is important. This definition also excludes malformations of the brain from the diagnosis of CP which may at first seem inappropriate but if a diagnosis is to allow one to understand something about the etiology, infer something about the clinical features to be expected, and to some extent, the prognosis and management going forward, then a more exacting definition of the condition is necessary. In the practice of medicine these days, a diagnosis has become just a tool for billing purposes but the true meaning of a medical diagnosis is more than that.
Once the patient has been determined to have CP there are as many different classifications of the disability as there are different health care providers involved in their care. One classification would describe the nature of the motor disability such as spastic, dystonic or ataxic. Another would describe the distribution of the disability such as diplegia, quadriplegia, hemiplegia, bilateral hemiplegia, appendicular or truncal or gait ataxia. Functional classifications can be useful also to indicate the severity of the disability. Most use a combination of various classifications such as Mild spastic hemiplegia or moderate spastic diplegia etc.
Classical Forms of Cerebral Palsy
The most common types of CP are fairly clearly delineated and can usually be correlated with the nature of the insult and the timing of the insult. I will describe the typical clinical types, their neuropathological correlates and the timing and nature of the brain insult which gives rise to the type of CP.
Spastic CP
It is useful to further divide spastic CP into descriptions of the distribution of the motor involvement, for example: Spastic diplegia, spastic tetraplegia (spastic quadriplegia), spastic hemiplegia and spastic double hemiplegia. Each subtype typically has its own clinical history with respect to the timing and nature of the insult, and its own prognosis. Each of the subtypes of spastic CP will also have distinct implications for management and outcome of the patients.
Spastic Tetraplegia
Spastic tetraplegia (spastic quadriplegia) involves all four limbs more or less equally. The typical story is that this is the result of a catastrophic event near the end of the pregnancy (Close to term) where there is loss of blood flow and global asphyxia. The infant is comatose for several days and requires ventilation and blood pressure support for several days as well. The most common causal events would include placental abruption or uterine rupture or maternal shock. The clinical result is a microcephalic child with global disabilities including microcephaly and intellectual disabilities. The neuropathological spasticity and correlate of this type of CP is called multicystic encephalomalacia (Figure 1) and the imaging may also show hydrocephalus ex vacuo (Figure 2).
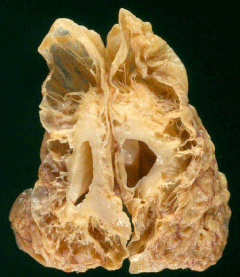
Figure 1: Multicystic Encephalomalacia. The end result of severe HIE in a
near term infant. (Courtesy of Dr. S.S. Schochet, MD).
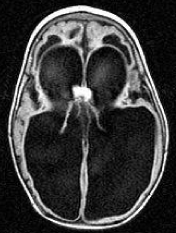
Figure 2: Hydrocephalus Ex-vacuo. MRI findings in a patient with Spastic
Tetraplegia.
Spastic Diplegia
Spastic diplegia is the term used when the lower extremities are the primary site of spasticity in the patient with CP. Although the upper extremities are considered spared in this type of CP this a relative statement in that there usually is some involvement in the arms and some corresponding impairment of function though considerably less than the lowers. Clinically these children may have motor disabilities mostly in ambulation with relative preservation of the other functions and they may or may not have intellectual disabilities. These children may or may not have microcephaly depending on the extent and severity of the insult to the developing brain. This type of CP typically results from an insult in the period between 30 and 34 weeks of gestational age when the germinal matrix is metabolically active and thus vulnerable to injury. The neuropathological correlate of spastic diplegia is periventricular leukomalacia (Figure 3), which may be cystic if the injury is severe enough, and the neuroimaging (Figure 4) shows abnormal signal in the corresponding region of the brain.
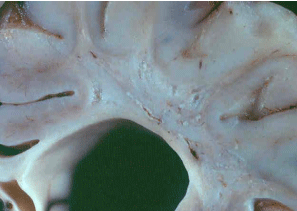
Figure 3: Post mortem section of the brain at the middle of the lateral ventricle
showing gliosis and small cystic changes in the periventricular white matter.
Characteristic of Spastic Diplegic CP. (Courtesy of Dr. S.S. Schochet, MD).
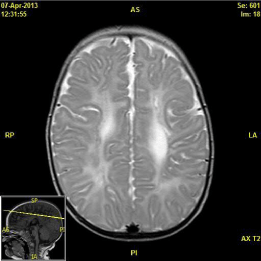
Figure 4: MRI of a child with spastic diplegic CP showing high signal intensity
in the periventricular white matter with small cystic change in the left frontal
region.
Spastic Hemiplegia
This lesion may occur in an infant at any gestational age and represents an infarction of the brain usually in a vascular distribution, i.e. a neonatal or prenatal stroke. The reason for the occlusion of the artery is usually not apparent but it can be anything from a genetic predisposition to vascular thrombosis, physical trauma or inflammatory processes and I think the possibility of embolization of placental syncytium into the fetal circulation is greatly underestimated as a cause of prenatal stroke. The child with a unilateral stroke often has surprisingly good function with relatively minor motor handicaps and relatively well preserved higher cortical functions with typically good language development and overall cognitive function. This relative preservation of function is presumably due to the ability to shift the non-hard wired functions to undamaged portions of the brain and/or to the opposite hemisphere. The neuropathological correlates are those of cerebral vascular disease at any age except that as the infant grows the volume loss due to the damaged hemisphere results in a shift of the normal midline structures and reposition of the falx cerebri (Figure 5).
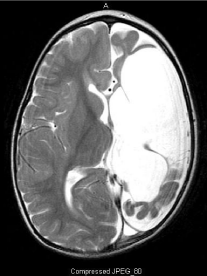
Figure 5: MRI of a child with hemiparetic CP showing a large infarct of the
entire L MCA distribution and subsequent to the volume loss, shift of the
midline falx.
Spastic Double Hemiplegia
Spastic Double Hemiplegia is different than spastic quadriplegia in that there is a bilateral infarction, usually middle cerebral artery distribution which results in the upper extremities being more severely involved than the lowers as is typical in strokes involving the cortical spinal tract in older individuals. In contrast to the hemiparetic CP patients, those with double hemiplegia will usually be microcephalic with significant intellectual disability in addition to their motor handicaps (Figure 6).
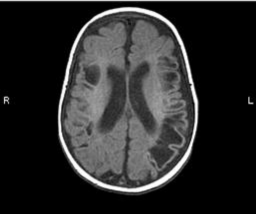
Figure 6: MRI of a patient with spastic double hemiplegia, microcephaly and
intellectual disabilities. There is cystic encephalomalacia in the distribution of
the middle cerebral artery bilaterally.
Athetoid/Dystonic Cerebral Palsy
Although the terms athetoid and dystonic cerebral palsy are not the same they are used together here to describe the end result of basal ganglia injury and the resulting clinical picture of abnormal fluctuation of tone which results in athetoid movements under the appropriate circumstances. The prototype of damage to the basal ganglia resulting in athetoid/dystonic cerebral palsy (A/D CP) is kernicterus. The more common clinical situation today, however, is a relatively mild asphyxia event in a term infant who has been predisposed or “set up” for injury by the presence of placental insufficiency prior to the insult. This combination was shown to produce basal ganglia damage and A/D CP and resulted in what is known as the “Two hit hypothesis” of basal ganglia damage [1].
Typically, the story I hear is that there was difficulty with the delivery and the infant required resuscitation as a newborn. The child may have required ventilator support for a few hours but then everything seemed to stabilize. The child is thought to be normal until later in the first year when fluctuations in tone are noted. This progresses to the dystonic CP as the infant grows. Since the injury most prominently involves the basal ganglia and the cortex is relatively spared, the patient may have a great deal of difficulty with motor function, but the possibility exists that cognition is relatively spared. One fairly typical andwell-documented situation is when the motor handicap is so severe that the children with preserved intellect have no ability to express themselves. The typical neuropathological correlate of A/D CP is the disorganization of the basal ganglia, particularly the glubus pallidus us and the putamen called status marmaratus. This abnormality can be easily seen in pathological specimens (Figure 7) but which in many cases is below the resolution of the MRI scans and thus when a patient comes along with CP and a normal MRI the likelihood is that the child has basal ganglia injury which cannot be seen on the MRI.
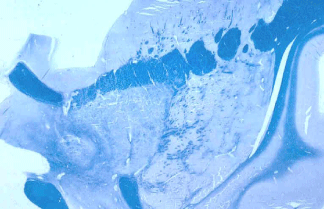
Figure 7: The disorganization of the GP can be seen in this post mortem
section thru the basal ganglia at the level of the internal capsule. (Courtesy
of Dr. S.S. Schochet, MD).
Dystonic CP is frequently mistaken for spastic CP and therapies for spasticity are not very effective for dystonic CP. The distinction between the two is difficult, however, and the fact is that most children with CP have a mixture of spasticity and dystonia. Determination of the relative components of spasticity and dystonia is very difficult as there are no easily applicable clinical measures of functional motor abnormalities that distinguish between the two much less allow the determination of the relative contributions of both to the motor dysfunction of the individual patient.
Ataxic CP
In the past ataxic cerebral palsy was largely a misnomer in the sense that most of the patients so designated had malformations of the brain rather than birth related injury to a previously normal brain [2]. In the last decade or so, however, the increasing numbers of infants surviving extremely premature birth (EPB defined as less than 1000gm birth weight and less than 28 weeks gestation) has resulted in an increasing number of children with cerebellar injury and resulting ataxia [3,4]. The most common difficulty the survivors of extreme premature birth have is behavioral and cognitive with almost half of the children affected to some degree [5-9]. About 10% have cerebral palsy (motor impairment) which typically presents as a mixture of some ataxia, some spasticity and some dystonia with a motor impairment out of proportion to the degree of any one of the components [6-12]. With the description of the cerebellar injury in the children with EPB came the recognition of the vulnerability of the cerebellum in the 24th to 28th week of fetal development [4,5]. Of the children with EPB who have CP almost 2/3 have deficient white matter in the region of the trigone of the lateral ventricle [12]. Most of these have little or no gliosis in the affected white matter which is presumably due to the fact that the oligodendroglia which would ordinarily produce gliosis as the end result of HIE are unable to do so because of the degree of immaturity at the gestational age in question [13]. The second most common brain injury in these children, however, is to the cerebellum [12]. The cerebellar injury is often not apparent in neonatal ultrasound studies but in MRI imaging later it is often clearly visible (Figure 8).
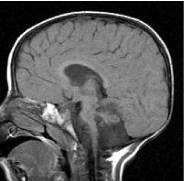
Figure 8: Sagittal MRI of an infant with mixed ataxic, spastic, dystonic CP.
The survivor of a 26-week gestation with a birth weight of 600Gm.
Recently, disruption of the cerebro-ponto cerebellar pathways has been implicated in the development of a particular type of behavioral dysregulation known as pseudo-bulbar affect in adults with a variety of conditions such as MSA (multisystem atrophy), dementia, stroke, traumatic encephalopathy etc [14,15]. A similar pathological crying/ laughter has recently also been described in the children with EPB who have structural cerebellar injury on neuroimaging [16]. Suggesting that the cerebellum plays a more important role in the modulation of behavior than previously recognized and this fact may account for a proportion of the behavior disabilities these children have.
The increasing number of EPB infants who suffer a high incidence of neurological difficulties has resulted in an increasing number of survivors with and without handicaps. With ten percent of these survivors having the mixed CP with elements of ataxia usually mixed with degrees of spasticity and dystonia, this group represents an increasing proportion of the children with CP currently and certainly will be even more so in the future. Recognition of this situation is of some importance for two reasons, First, the management of the motor disabilities is not as simple as with the more straight forward spastic CP and these children do not respond as well as others, with more typical spastic CP, to efforts to improve their motor function. Second, the behavior dyscontrol and particularly the emotional incontinence called pseudo bulbar affect is relatively common in these patients and if recognized and treated may respond to interventions [17].
References
- Brann AW, Meyers RE. Central nervous system findings in the newborn monkey following severe in utero partial asphyxia. Neurology. 1975; 25: 327-338.
- Schaefer GB, Sheth RD, Bodensteiner JB. Cerebral dysgenesis: An overview. Neurologic Clinics, Pediatric Neurogenetics. GB Schaefer and JB Bodensteiner (Eds), Philadelphia, WB Saunders. 1994; 12; 773-788.
- Johnsen SD, Tarby TJ, Lewis KS, Bird R, Prenger E . Cerebellar infarction: an unrecognized complication of very low birthweight. J Child Neurol. 2002; 17: 320-324.
- Bodensteiner JB, Johnsen SD. Cerebellar injury in the extremely premature infant: A newly recognized but relatively common outcome. J Child Neurol. 2005; 20: 139-142.
- Volpe JJ. Cerebellum of the premature infant: rapidly developing, vulnerable, clinically important. J Child Neurol. 2009; 24: 1085-1104.
- Bayless S, Stevenson J. Executive functions in school-age children born very prematurely. Early Hum Dev. 2007; 83: 247-254.
- Larroque B, Ancel PY, Marret S, et al. Neurodevelopmental disabilities and special care of 5-year old children born before 33 weeks of gestation (the EPIPAGE study): a longitudinal cohort study. Lancet. 2008; 371: 813-820.
- Allin M, Walshe M, Fern A, Nosarti C, Cuddy M, Rifkin L, et al. Cognitive maturation in preterm and term born adolescents. J Neurol Neurosurg Psychiatry. 2008; 79: 381-386.
- McQuillen PS, Ferriero DM. Selective vulnerability in the developing central nervous system. Pediatr Neurol. 2004; 30: 227-235.
- Messerschmidt A, Brugger PC, Boltshauser E, Zoder G, Sterniste W, Birnbacher R, et al. Disruption of cerebellar development: potential complication of extreme prematurity. AJNR Am J Neuroradiol. 2005; 26: 1659-1667.
- Johnsen SD, Bodensteiner JB, Lotze TE. Frequency and nature of cerebellar injury in the extremely premature survivor with cerebral palsy. J Child Neurol. 2005; 20: 60-64.
- Bodensteiner JB, Johnsen SD. Magnetic resonance imaging (MRI) findings in children surviving extremely premature delivery and extremely low birthweight with cerebral palsy. J Child Neurol. 2006; 21: 743-747.
- Volpe JJ, Kinney HC, Jensen FE, Rosenberg PA. The developing oligodendrocyte: key cellular target in brain injury in the premature infant. Int J DevNeurosci. 2011; 29: 423-440.
- Parvizi J, Joseph J, Press DZ, Schmahmann JD. Pathological laughter and crying in patients with multiple system atrophy-cerebellar type. Mov Disord. 2007; 22: 798-803.
- Parvizi J, Anderson SW, Martin CO, Damasio H, Damasio AR. Pathological laughter and crying: a link to the cerebellum. Brain. 2001; 124: 1708-1719.
- Pitts J, Bodensteiner JB. Pseudobulbar Affect in Survivors of Extreme Prematurity With Cerebellar Injury: Support for the Cerebellar Link in Pathological Laughter and Crying. J Child Neurol. 2016; (In Press).
- Parvizi J, Arciniegas DB, Bernardini GL, Hoffmann MW, Mohr JP, Rapoport MJ, et al. Diagnosis and management of pathological laughter and crying. Mayo Clin Proc. 2006; 81: 1482-1486.