
Case Report
Phys Med Rehabil Int. 2016; 3(4): 1093.
Prosthetic Rehabilitation of a Patient with an Ocular Defect with Custom-made Ocular Prosthesis: A Case Report
Bhochhibhoya A¹*, Mathema S² and Maskey B²
¹Department of Prosthodontics and Maxillofacial Prosthetics, Nepal Medical College, Nepal
²Department of Prosthodontics and Maxillofacial Prosthetics, People’s Dental College and Hospital, Nepal
*Corresponding author: Bhochhibhoya A, Department of Prosthodontics and Maxillofacial Prosthetics, Nepal Medical College, Attarkhel, Kathmandu, Nepal
Received: July 05, 2016; Accepted: July 19, 2016; Published: July 22, 2016
Abstract
The disfigurement resulting from an ocular defect causes significant impact on the self-image and personality of an individual. Patients with such maxillofacial deficiencies often face crippling problems associated with functional disability and social reactions. Thus, rehabilitation of ocular defects is essential for physical and psychological wellbeing of the patient and to improve their social acceptance. The objective of prosthetic rehabilitation is to mimic natural esthetics so as to provide a cosmetically acceptable prosthesis. A custom ocular prosthesis is a noble alternative in situations where surgical reconstruction or the use of implants is precluded. This article outlines a simplistic procedure for construction of custom-made ocular prostheses in a patient with ocular defect following traumatic injury.
Keywords: Ocular; Custom-made; Maxillofacial; Prosthetic rehabilitation
Introduction
The unfortunate loss of an eye is generally associated with a congenital defect, trauma, tumor, sympathetic ophthalmia or the need for histological investigations [1]. Ocular trauma often results in phthisis bulbi; a small, shrunken, non-functional eye [2]. Surgical procedure for these conditions may necessitate an orbital evisceration, enucleation or exenteration. Evisceration involves removal of contents of the globe, leaving the sclera intact. Enucleation is a more aggressive procedure in which the entire eyeball is severed from the muscles and optic nerve. Exenteration, the most radical, involves removal of the contents of the orbit [3].
The mutilation caused by loss of an eye has a crippling effect on the person’s personality which causes significant physical and emotional problems [2-5]. Most patients experience significant stress, primarily due to the functional disability and to public reactions to the disfigurement [6]. Prosthetic rehabilitation of such ocular defect with a cosmetically acceptable prosthesis that reproduces the color, form and orientation of iris is required to endorse psychological comfort to the patient and to make them socially acceptable [7]. Various methods of rehabilitating such ocular defects include either ready-made or custom-made ocular prosthesis [8-11]. Plethora of fabrication techniques forcustom made ocular prosthesisexistswhich permits variations during its construction.
The art of making artificial eyes has been known tomankind from the days of the early Egyptianswell before 3000 BC. Ambroise Parre is considered the pioneer of modern artificial eye. He made use of both glass and porcelain eye. Not until World War II, andthe development of refined plastics has there beenthe option for a satisfactory aesthetic ocular prosthesis [6,12,13].
Ready-made stock eye prosthesis comes in standard sizes, shapes, and colors and they require no special skills or materials for fabrication. They are relatively inexpensive and less time consuming. However, custom made ocular prosthesis have several advantages including improved adaptation to underlying tissues, better mobility of the prosthesis, even distribution of pressure due to equal movement thereby reducing the incidence of ulceration, improved fit, comfort and enhanced esthetics. However, a custom made prosthesis is more expensive than a stock prosthesis, and multiple steps are required for its fabrication [6,14-16].
Case Presentation
A thirty-five year old male was referred to the Department of Prosthodontics and Maxillofacial Prosthetics, People’s Dental College and Hospital for prosthetic rehabilitation of an ocular defect. The patient gave the history of trauma of right eye three year back and consequently the eye had shrunken.
Clinical examination revealed enophthalmic and phthisical globe with corneal opacity (Figure 1). The intraocular tissue bed was healthy and the depth between the upper and lower fornices was adequate. The posterior wall of the defect showed synchronous movements. The conjunctival lining and palpebral fissure did not exhibit any abnormality. Fabrication of custom-made ocular prosthesis was planned for the patient since it gives better result than ready-made stock eye prosthesis.
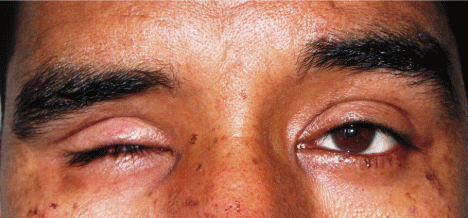
Figure 1: Clinical presentation.
Impression of the ocular defect was made using molded shell or stock ocular tray technique by injecting light body polyvinyl siloxane impression material (Reprosil, DentsplyInt) into the eye socket using an stock ocular tray assembled to a 5 ml modified disposable syringe (Figure 2) [14]. The patient was seated erect, requested to stare at a distant spot holding his gaze in a straight forward direction while the impression was being made. Petroleum jelly was applied to eyelashes and eyebrow to prevent sticking of impression material. The impression was retrieved from the socket and evaluated for any defects and voids (Figure 3).
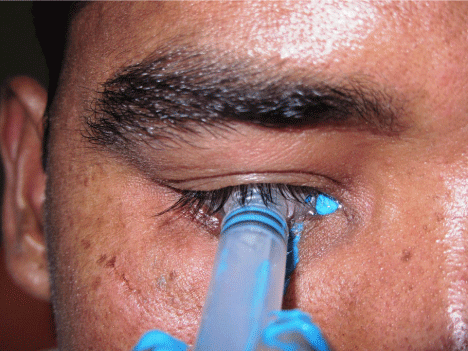
Figure 2: Stock tray ocular impression.
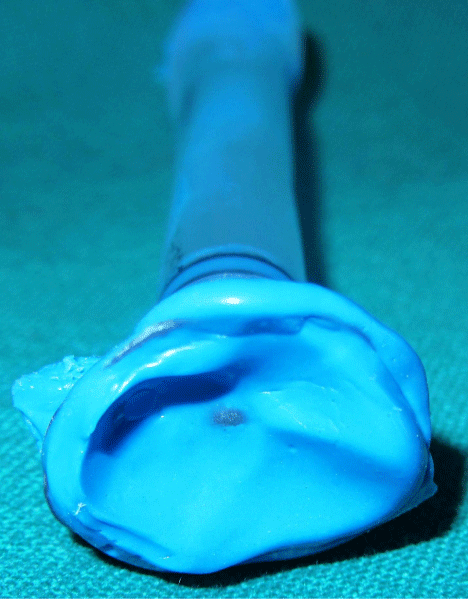
Figure 3: Evaluation of ocular impression.
Clinical and Laboratory Steps
The impression was invested in alginate (Zelgan, DentsplyInt) and the alginate mould was partially split after setting, and impression of the socket retrieved (Figure 4). Baseplate wax (Modelling wax, DPI) was melted and poured in the mold to fabricate a scleral wax pattern (Figure 5). Wax pattern was polished and checked for the accuracy of fit and adjusted until satisfactory contours of the eyelids were achieved. The position of the iris of the natural eye was used as a guide to mark the iris position on the wax pattern. An iris disk approximately 0.5mm smaller than the actual measurement was selected, allowing for magnification of the iris by the clear acrylic which produces three dimensional effects. The iris disk was positioned in the marked area after scooping out wax from that area. After the placement of iris disk, the wax pattern was polished and tried in for evaluating its position and gaze (Figure 6). The wax pattern was dewaxed and processed in the two piece flask using heat polymerizing acrylic resin (DPIHeat cure, DPI), the shade of which was initially matched with the scleral portion of the natural eye. The scleral blank was tried in. The supraorbital folds, margins of eyelids and iris plane were evaluated to match with the natural eye (Figure 7).
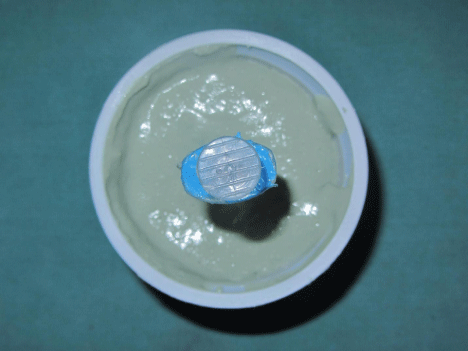
Figure 4: Preparation of alginate mold.

Figure 5: Scleral wax pattern.
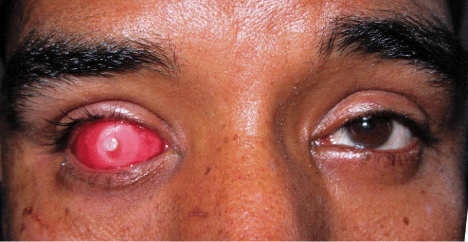
Figure 6: Evaluation of wax pattern and positioning of iris disc.
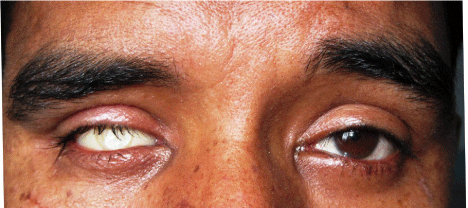
Figure 7: Acrylic scleral blank try in.
The scleral blank was painted with acrylic colors (W&N Artists’ Acrylic) to match the coloration of natural eye. Iris portion of scleral blank was colored in a layering fashion to mimic the colored striations in the patient’s iris. A dark black spot was painted in the center of iris to represent the pupil. Next, the limbus or fuzzy demarcation between the iris and sclera was painted. Characterization was done by adding red rayon fibers in the sclera part to simulate vasculature. The entire scleral portion is then coated with monomer polymer syrup and allowed to dry (Figure 8). Finally, the scleral blank was replaced into the flask and clear acrylic resin packed into the mold space. The flask was closed and the resin heat cured. This laminate of clear acrylic gives a life like appearance and depth for the characterization. It was finished and polished to a high shine, disinfected and stored in water for 24 hours before insertion.
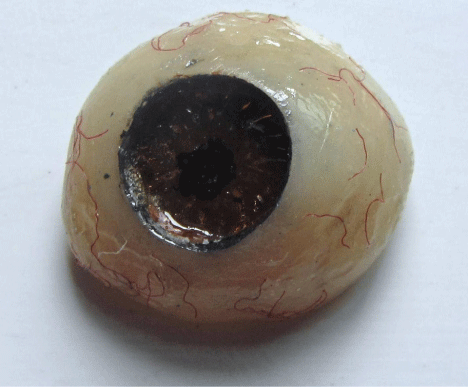
Figure 8: Scleral blank painting.
The patient was instructed on insertion, removal and hygiene of the prosthesis (Figure 9). Periodic recall visits were planned after 1 day, 1 week and 6 months for evaluation and necessary adjustments.
Discussion

Figure 9: Insertion of ocular prosthesis.
The disfigurement caused by loss of an eye has a crippling effect on the person’s personality which poses significant physical and emotional problems. Rehabilitating such patients with ocular defect is a challenging and time consuming task. The importance of meticulous treatment planning and steps in fabricating an ocular prosthesis has been explained. Numerous techniques exist for the fabrication of custom ocular prosthesis including empirical fitting a stock eye, modifying astock eye and the custom eye technique. The method of choice depends on type of defect, operator skills and availability of material and equipment.
A custom ocular prosthesis is a good option when reconstruction by plastic surgery or the use of osseointegrated implants is not possible or not desired [17]. Although the prosthesis cannot restore the vision but it reduces the psychological trauma and allows the patient to return to an accustomed life-style [2-4]. The close adaptation of the custom made prosthesis reduces potential stagnation spaces at the prosthetic tissue interface which helps in uniform pressure distribution and reduces the incidence of conjunctival abrasion or ulceration. Fluid collection in the space could cause tissue irritation and increase bacterial growth [13-15].
Conclusion
Prosthetic rehabilitation of a patient with ocular defect helps in boosting confidence and makes them socially acceptable. The procedure described here is simple, cost effective, and can be carried out in regular dental set-up. This method has provided good results in terms of esthetics, patient’s acceptance and satisfaction.
References
- Perman KI, Baylis HI. Evisceration, enucleation, and exenteration. Otolaryngol Clin North Am. 1988; 21: 171-182.
- Lubkin V, Sloan S. Enucleation and psychic trauma. Adv Ophth Plast Reconstr Surg. 1990; 8: 259-262.
- Guttal SS. A Simple Method of Positioning the Iris Disk on a Custom-Made Ocular Prosthesis. J Prosthodont. 2008; 17: 223-227.
- AdarshN, Pradeep, Suresh BS, Yogesh RB, Rachana KB. Ocular Prosthesis Made Easy: A Case Report. Intl J Dent Clin. 2011; 3: 105-106.
- Marunick MT, Harrison R, Beumer J. Prosthodontic rehabilitation of midfacial defects. J Prosthet Dent. 1985; 54: 553-560.
- Artopoulou I, Montgomery P, Wesley P, Lemon J. Digital imaging in the fabrication of ocular prostheses. J Prosthet Dent. 2006; 95: 327-330.
- Jain S, Makkar S, Gupta S, Bhargava A. Prosthetic Rehabilitation of Ocular Defect Using Digital Photography: A Case Report. J Indian Prosthodont Soc. 2010; 10: 190–193.
- Erpf S. Comparative features of plastic and/or glass in artificial eye construction. Arch Ophthalmol. 1953; 50: 737-738.
- M El-Dakkak. Problem solving technique in ocular prosthetic reconstruction. Saudi Dental Journal. 1990; 2: 7–10.
- E Kale, AMes, Izgi AD. A technique for fabrication of an interim ocular prosthesis. J Prosthodont. 2008; 17: 654–661.
- Smith RM. Relining an ocular prosthesis: a case report. J Prosthodont. 1995; 3: 160–163.
- Fernandes AU, Goiato MC, Batista MA, Santos DM. Color alteration of the paint used for iris painting in ocular prostheses. Braz Oral Res. 2009; 23: 386-392.
- Sandeep C, Gopinadh A, Kavya R, Phani PB, Sampath K, Krishna CA. A time saving method to fabricate a custom ocular prosthesis. J Orofac Res. 2013; 3: 42-45.
- Mathew FM, Smith MR, Suttion JA. The ocular impression: a review of the literature and presentation of an alternate technique. J Prosthodont. 2000; 9: 210–216.
- J Beumer and I Zlotolow. Restoration of facial defects. J Beumer. In Maxillofacial Rehabilitation: Prosthodontic and Surgical Considerations. Mosby, St. Louis, Mo. 1996; 350–364.
- Ow RK, S Amrith. Ocular prosthetics: use of a tissue conditioner material to modify a stock ocular prosthesis. J Prosthet Dent. 1997; 2: 218–222.
- Jurel SK, Singh RD, Siddhartha R, Gupta DS. Fabrication of custom ocular prosthesis using a graph grid: a case report. Int J Clin Dent Sci. 2011; 2: 68-71.