
Research Article
Phys Med Rehabil Int. 2016; 3(7): 1106.
Self-reported Physical Activity after Stroke and its Determinants?
Van de Port IGL¹*, Van der Werf H², Schepers VPM³ and Kwakkel G4
¹Revant Rehabilitation, Breda, The Netherlands
²Merem Rehabilitation Center ‘De Trappenberg, Huizen, The Netherlands
³Brain Center Rudolf Magnus and Center of Excellence for Rehabilitation Medicine, University Medical Center Utrecht and De Hoogstraat Rehabilitation, Utrecht, The Netherlands
4Department of Rehabilitation Medicine, VU University Medical Centre, Amsterdam, The Netherlands
*Corresponding author: Van de Port IGL, Revant Rehabilitation, 4817 JW Breda, The Netherlands
Received: November 06, 2016; Accepted: November 29, 2016; Published: December 01, 2016
Abstract
Studies show that the physical activity level of individuals after stroke is low. Since this population is at risk for secondary complaints physical activity is an important outcome. Self reported questionnaires give insight in the amount and intensity of physical activity. In addition, identifying related factors can help to guide interventions to increase physical activity.
Objectives: To examine physical activity as measured by the Physical Activity Scale for Individuals with Physical Disability (PASIPD) in people in the chronic phase after stroke and investigate factors that predict physical activity measured with PASIPD.
Methods: In this longitudinal study, stroke survivors completed the Dutch version of the PASIPD, a 7-day recall self-report questionnaire including 12 items capturing physical activity in recreation, household and occupational domain. Total physical activity is expressed in metabolic equivalent (MET) hours per day. Possible determinants, i.e. patient and stroke characteristics and clinical outcomes, were measured at the end of inpatient rehabilitation. The PASIPD was collected at least one year after finishing the studied outpatient rehabilitation period.
Results: Mean PASIPD score of the 116 participants was 17.1 (SD 12.4) MET h day-1. Multivariate analysis showed that a higher education level, a positive score on the letter cancellation task and a higher score on the fatigue severity scale were significantly (p<.05) related to a lower score on the PASIPD, explaining 13% of the variance.
Conclusion: Physical activity is low after stroke. Level of education, visuospatial neglect and fatigue should be taken into account in clinical care and designing future interventions.
Keywords: Stroke; Physical activity; Self-report questionnaire; Prognosis
Introduction
Stroke survivors often suffer from functional limitations which lead to a reduction in physical activity (PA), deconditioning and predisposition to a sedentary lifestyle [1-4]. Different studies show that physical activity levels of patients after stroke are far below agematched normative values [5]. Since it is known that an inactive lifestyle may contribute to a heightened risk for recurrent stroke and secondary complications like heart diseases, monitoring physical activity is important in people after stroke [2,6]. Especially in the chronic phase after stroke, a decrease in physical activity has been identified. Despite an often very intensive and effective rehabilitation period. Being able to identify the determinants that are related to physical inactivity is valuable to further improve the care and behavior changing interventions to stimulate physical activity in this population.
Physical activity is a multidimensional construct that includes intensity, frequency, duration and variety [7]. A recent review of English et al. [5] highlighted a lack of knowledge about the amount and intensity of physical activity amongst post stroke people. However, previous studies suggested that a certain intensity of the exercise is needed to lead to a cardio protective effect, which underlines the importance of also getting insight in the intensity of the physical activity.
The Physical Activity Scale for Individuals with Physical Disability (PASIPD) is a self-reported questionnaire relating physical activities including leisure, household, and work-related activities to metabolic equivalents (METS) [8]. Using this outcome measure will give insight in the amount, variety and intensity of the physical activity. In the PASIPD, patients are asked to report the frequency of each activity in the previous week. Each activity is weighted with a metabolic equivalent that reflects the intensity of that specific activity. With that, not only the type and amount of physical activity is measured, but also an estimate is given of the intensity of the conducted activities.
The aims of the present study are 1) to examine the level of physical activity as measured by the PASIPD in people in the chronic phase after stroke and 2) to investigate factors that are predictive for amount of physical activity according to the PASIPD. Based on the current literature in the healthy and stroke population [9-11] we include demographic and stroke characteristics such as age, gender and stroke severity, physical outcome measures, mood and fatigue as possible determinants related to physical activity.
Methods
Participants and design
Stroke survivors who participated from 2009 until 2011 in the FIT-stroke trial were approached. The FIT-stroke trial is a prospective single blinded randomized controlled trial conducted by specially trained staff in nine rehabilitation centers in the Netherlands [12]. All subjects completed an inpatient rehabilitation program in one of the nine rehabilitation centres. The following inclusion criteria were used: verified stroke according to the World Health Organization (WHO) definition (19), ability to walk a minimum of 10m without physical assistance from a therapist (Functional Ambulation Categories =3), discharged home from a rehabilitation centre, need to continue physiotherapy during outpatient care to improve walking competency and/or physical condition, giving informed consent and being motivated to participate in 24 fitness training sessions over a 12-week period, or in usual care. Patients were excluded if they had severe cognitive deficits as evaluated by the Mini-Mental State Examination (<24 points), were unable to communicate (i.e. <4 points on the Utrechts Communicatie Onderzoek; UCO) or lived more than 30km from the rehabilitation centre. After inclusion, the participants received an outpatient rehabilitation program of either 12 week task oriented circuit class training or regular face-to-face physiotherapy after discharge from their inpatient rehabilitation period. Primary outcome measure was the Stroke Impact Scale [12,13]. The present study concerns a sub analysis of the FIT-stroke population including an extra follow up measurement at least one year after finishing the FIT-Stroke outpatient rehabilitation period. Data of both the control and intervention group was included.
Procedure
The participants were addressed by mail and requested to complete and return a questionnaire about physical activity. Three weeks after the questionnaire was sent non-responders were contacted once by telephone and were requested to return de questionnaire. Informed consent was obtained from all the participants during the FIT-stroke trial. The study was approved by the Medical Ethics Committee of the University Medical Centre of Utrecht, the Netherlands and registered in the Dutch Trial Register (trial number NTR1534).
Measures
Physical activity level is measured by the Physical Activity Scale for Individuals with Physical Disabilities (PASIPD). The PASIPD is 7-day recall self-report questionnaire capturing physical activity in three domains (recreation, household and occupational activities). It consists of 13 questions [14]. We used the Dutch version: a 12 item questionnaire in which question 10 on lawn work and question 11 on outdoor gardening are merged, because this better represents the Dutch situation. Domain scores can be calculated for Leisure Activities (item 2-6), Household activities (item 7-11) and Work/ volunteer (item 12). The total physical activity is expressed in metabolic equivalent hours per day (MET h day-1) and is calculated by the sum of the average hours of physical activity daily multiplied with a metabolic equivalent value associated with the intensity of the activity for each item. The maximum score of the Dutch version is 182.3 MET h day-1 compared to 199.5 MET h day-1 in the original PASIPD. The Dutch PASIPD has been found to have a test-retest reliability of r = 0.77 (p< 0,05) [8].
The possible predictors of physical activity, i.e. the independent factors were determined at completion of the outpatient rehabilitation program of 12 weeks in the FIT-stroke trial. Patient characteristics were age, gender, living situation, level of education, employment before stroke, sport participation before stroke and participation in circuit class training in outpatient rehabilitation. Level of education was dichotomized, being scored “high” for patients with intermediate vocational education or higher. Sport participation before stroke was dichotomized, being scored “yes” when the patient weekly participated in sports or walked or cycled more than two hours weekly. Stroke characteristics were time since stroke and type of stroke. In addition different clinical outcomes were determined. Visuo-spatial neglect was measured by the Letter Cancellation Task (LCT). This measure was dichotomized being scored “positive” when patients scored three omissions or more on the hemiplegic side, compared to the other side. The Six Minute Walking Test (6 MWT) was used to measure basic functional mobility and endurance. The patient is asked to walk six minutes at a comfortable speed, the distance walked is measured. The Time Up and Go test (TUG) is a test of basic functional mobility. The patient is asked to rise from a chair and walk 3 meters as fast as possible, cross a line, turn and walk back and sit down again. This test has been shown to identify patients at risk for falling. The fear of falling was measured by the Falls Efficacy Scale (FES), a 13 item questionnaire which determines perceived selfefficacy at avoiding falls during essential, non-hazardous activities of daily living. The Fatigue Severity Scale (FSS) was used to determine fatigue. It consists of 9 items, and scores for each item range from 1 to 7. In a reliability study with two independent observers and 18 stroke patients, FSS showed an intra-observer correlation coefficient (ICC) of 0.82. The Hospital Anxiety and Depression Scale (HADS) was used to determine anxiety and depression. It is a simple measure to determine mood, emotional distress, anxiety depression and emotional disorder. The questionnaire consists of 14 items (7 anxiety, 7 depression), each with a 4-point rating scale (0-3) and has proved to be responsive to change. More detailed description and references of the used measures can be found in the study protocol of FIT-stroke trial [13].
Statistical analysis
Baseline characteristics were analyzed using descriptive statistics at the end of the 12 weeks intervention period. Baseline characteristics where compared between included patients, who returned a valid questionnaire and non-included patients, who did not return a (valid) questionnaire by the independent-samples T test for normally distributed data, Mann-Whitney-U test for not normally distributed data and Chi-square test for nominal data. Data were considered normally distributed when skewness values were between -1 and 1. The relations between the PASIPD score and the independent variables (i.e. patient characteristics, stroke characteristics, and clinical outcomes) was first analyzed using bivariate regression analysis. Variables with a level of significance lower than 0.2 were included in the multiple regression analysis. Multicollinearity diagnostics was applied between candidate determinants for the outcome of PASIPD score. In case of multicollinearity (r >0.8) only the variable with the highest correlation to the PASIPD score was included in the multivariate regression analysis. The remaining variables were used in a backward regression analysis two tailed using p<0.05 as the level of significance. Data were analyzed with statistical package SPSS (version 22.0).
Results
After completion of the FIT stroke trial 190 of the 242 participants agreed to be approached for further research. These participants were addressed by mail at least one year after completion of the 12 weeks outpatient intervention (Figure 1). In total 111 participants returned the questionnaire (58%). Of the non-responders (N=79), 56 were contacted by phone. Twenty-eight of the phoned non-responders returned the questionnaire, resulting in a response rate of 73% (139 of 190). Of the 139 returned questionnaires 19 were incomplete, one was invalid because the participant had an abdominal surgery in the recent history which interfered with physical activity, and three questionnaires were misinterpreted by the responder, leaving data of 116 participants available for analysis.
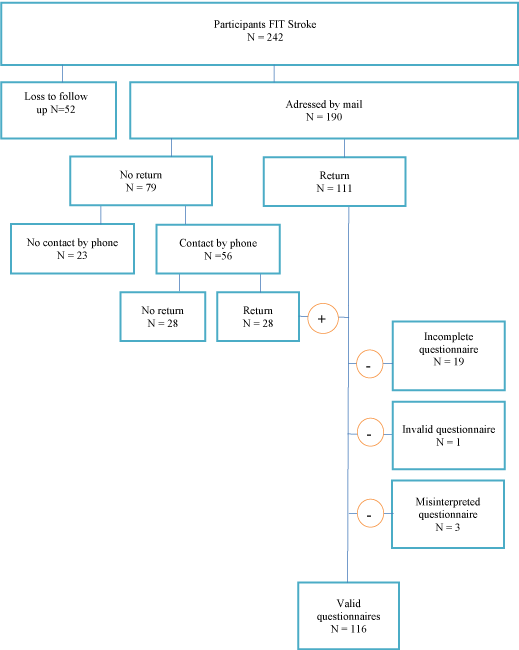
Figure 1: Flow chart included participants.
Of the responders two persons (2%) reported a recurrent stroke. There were no significant differences in patient and stroke characteristics between included and non- included patients except for sport participation before stroke. Included patients were more sportive before stroke than non-included patients. The mean age of participants at completion of outpatient rehabilitation was 58.7 ± 7.7 years and the majority was living together. There were more male than female participants (31% female), this is proportional to the participants of FIT stroke trial. More than half of the participants were employed before stroke. Time since stroke at completion of outpatient rehabilitation was 5.9 ± 1.7 months and infarctions were more frequent than hemorrhages. Focusing on the clinical outcomes, it became clear that included participants had a better mobility than non-included participants, represented in the scores of the TUG test and 6MWT (Table 1). Only a small part of the participants had a positive LCT.
Included (N= 116)
Non-included (N = 126)
Patient characteristics
Mean age� in years ± SD
58.7 ± 9.9
56.2 ± 10.6
Female gender (%)
36 (31)
48 (38)
Living alone (%)
16 (14)
27 (21)
Higher education (%)
64 (55)
61 (48)$
Employed before stroke(%)
71 (61)$
78 (62)$
Sport participation before stroke (%)
91 (78)$*
81 (64)$$
Participation circuit class training (%)
65 (56)
60 (48)
Stroke characteristics
Months since stroke ± SD
5.9 ± 1.7
6.0 ± 1.5
Ischemic stroke (%)
90 (77)
108 (86)
Clinical outcomes
Positive LCT (%)
7 (6)
10 (8)
TUG score in seconds ± SD
15.0 ± 15.4*
11.0 ± 6.1
6 MWT in metres ± SD
409.6 ± 117.8*
360.3 ± 143.6$
FES mean score ± SD
101.9 ± 20.5
103.0 ± 21.7
FSS mean score ± SD
4.4 ± 1.6
4.1 ± 1.7
HADS mean score ± SD
7.7 ± 5.7
9.4 ± 6.6
SD: Standard Deviation. *Significant difference included-non-included (p<0.05). $1 missing. $$4 missing. LCT: Letter Cancellation Task; TUG: Time get Up and Go test; 6 MWT: Six Minute Walking Test; FES: Fall Efficacy Scale; FSS: Fatigue Severity Scale; HADS: Hospital Anxiety and Depression Scale.
Table 1: Patient and stroke characteristics and clinical outcomes of the included and non-included patients at completion of outpatient rehabilitation program (12 weeks).
The mean PASIPD score was 17.1 (SD 12.4) MET h day-1. Scores ranged between 0.17 and 57.3 MET h day-1. The following scores were calculated for the different categories; Leisure: 10.6 (SD 9.7), Household activities 4.7 (SD 4.5) and Work 1.8 (SD 4.0) MET h day-1. At the time of filling out the questionnaire the mean time since stroke was 2.23 years (SD 0.57).
Bivariate and multivariate analyses
Table 2 represents the relation between the independent variables measured at completion of outpatient rehabilitation and the PASIPD score in the chronic phase after stroke. In the univariate analysis, level of education, time since stroke, type of stroke, LCT, 6MWT and FSS were significantly related to PASIPD score (p<0.2). Multicollinearity of the independent variables was not present; therefore all variables were included in the multivariate analysis. A higher education level, a positive score on the LCT and a higher score on the FSS were significantly (p<0.05) related to a lower score on the PASIPD (Table 2). After including these variables, the multivariate model explained 13% of the total variance.
Bivariate analysis
Multivariate analysis
Determinants
Standardized Beta
p
Standardized Beta
p
Mean age� in years
-0.004
0.966
Gender
-0.09
0.361
Living situation
-0.07
0.450
Education level
-0.26
0.005
-0.27
0.003
Employed before stroke
0.10
0.305
Sport participation before stroke
0.09
0.332
Participation circuit class training
0.06
0.555
Time since stroke
-0.16
0.082
ns
Type of stroke
-0.12
0.196
ns
Hemiplegic side
0.05
0.625
LCT
-0.19
0.044
-0.18
0.042
TUG
-0.02
0.861
6 MWT
0.12
0.191
ns
FES
0.09
0.362
FSS
-0.17
0.077*
-0.18
0.041
HADS total
-0.12
0.210
LCT: Letter Cancellation Task; TUG: Time get Up and Go test; 6 MWT: Six Minute Walking Test; FES: Fall Efficacy Scale; FSS: Fatigue Severity Scale; HADS: Hospital Anxiety and Depression Scale. *p<0.2.
Table 2: Bivariate and multivariate analysis including PASIPD as dependent variable.
Discussion
The aim of this longitudinal study was to examine the level of physical activity of chronic stroke survivors and to explore determinants of physical activity. The mean score of the PASIPD was 17.1 ± 12.4 MET h day-1. This score is comparable to that of other studies in which patients with chronic disabilities were included. The PASIPD scores varied between 11.3 – 21 MET h day-1 in the studies that also used the Dutch 12 item version [8,15-17]. If our score is roughly corrected to compare it to the 13 item version, the total score would be (17.1/11)x12 = 18.7 MET hour day -1. This score is within the range reported in studies using the original 13 item questionnaire, i.e. 7.6 – 36.34 MET hour day -1 [14,18-22]. Giacobbi et al found a relatively high score of 36.34 ± 15.29 MET hour day-1 in 26 patients with different disabilities recruited at a wheelchair user’s basketball tournament [22]. This higher score might be explained by the lower age of the participants and by the fact that they already proved to be physically active by their involvement in a basketball tournament. A study including 26 patients one year post stroke reported lower scores, i.e. 7.8 ± 7.6 MET hour day -1, which might be explained by inclusion of people with more severe disabilities represented by a median Functional Ambulation Category score of 3 [18]. The chronic stroke population in the study of Frost et al. also scored lower with a mean PASIPD score of 10.6 ± 10 MET hour day-1. Again, these participants seemed less physically fit, represented by a mean walking speed 0.8 m/s during the 10 meter walking test. The participants in the present study were included only with a FAC score of 3 and higher. In addition, the included participants showed better outcomes on the 6MWT and TUG compared to the non responders, suggesting a relatively fit group of participants.
In the multivariate analysis, a higher level of education and the presence of neglect and fatigue were significantly related to low physical activity. Especially the negative correlation with education level was surprising, since several studies show a positive relation between level of education and physical activity or healthy life style in healthy older populations [9,11,23-25]. In contrast, it has been suggested that people with lower education report higher physical activity related for example strenuous job or heavy household activities [26]. This might be an explanation for the inverse relationship, although it has to be realized that the majority of the included participant did not work at the time of testing. Visuo-spatial neglect has previously been described as a factor negatively related to physical activity measured objectively by accelerometry [27] and by a self-reported questionnaire [28]. Although different outcome measures were used our study underlines the negative effect of neglect on physical activity. The association between fatigue and physical activity is scarcely researched. No significant association was found between fatigue and physical activity in the study of Michael et al. [10]. Recently, Duncan et al showed a significant moderate correlation between fatigue and physical activity as measured by the Activ PAL at 1, 6 and 12 months after stroke in a larger sample [29]. The current study shows that fatigue as measured in the subacute stage after stroke had a longitudinal significant inverse relation with physical activity in the chronic phase after stroke even after correcting for several other determinants such as depression. However, the explained variance is low and the unique causal relation between fatigue and physical activity requires further investigation. Previous studies suggested that PASIPD scores correlate moderately to the 6MWT (r=0.31) and Berg Balance Scale (r=0.33) [21] and to gait speed (r=0.42) [20] in people after stroke. Reported correlation with Barthel Index and Functional Ambulation Categories is higher [27]. In the present study the 6MWT showed longitudinally a low but significant bivariate association with PASIPD. Sport participation before stroke and participation in the circuit class training was not significantly related to physical activity in the chronic phase after stroke.
The present study has some limitations that should be taken into account when interpreting the results. First of all physical activity, as determined by frequency and intensity of the activity, and the sort activity, was measured by the self-reported questionnaire PASIPD. The drawback of self-report measures is recall bias and the possibility to provide socially desirable responses. Van den Berg et al suggested that the PASIPD overestimated the duration spent on an activity compared to the registration of an accelerometer [15]. Previous studies show that the correlation coefficient between PASIPD and an accelerometer varied from 0.19 to 0.30 (p < 0.05) in different populations with physical limitations [8,15]. Since it is shown that the correlation between objective and subjective measures of physical activity is low, and may reflects different constructs [18], future research is required that take confounding factors of self-reported physical activity into account. Another fact to take into consideration is that the multivariate prediction model explained 13% of the total variance of self-reported physical activity measured by the PASIPD. This means that other non researched variables will be related to physical activity. Coping and other psychological factors such as self-efficacy and locus of control which might be related to physical activity and need to be included in future research [30]. Also, context related factors like the housing situation, area of living, for example rural versus urban, or the family composition might influence daily physical activity. Future research needs to be longitudinal and with a large enough population like the present study to be able to include several determinants in one analysis. The present study included a large study population and it was therefore possible to study many determinants representing the whole ICF spectrum.
Overall, this study contributes to the current literature by offering new information about the self-reported physical activity in the chronic phase after stroke and possible related factors. Since the PASIPD is expressed in METs per day, we provided not only information about the amount of physical activity, but also about the intensity. Despite the fact that this value is comparable to other patient population, it is worrying that the level of activity is this low. Especially when keeping in mind that the included group was relatively good functioning and that it has been suggested that the PASIPD overestimates the level of physical activity [15]. The presence of fatigue and visuo-spatial neglect and a higher education were negatively associated with physical activity. These determinants need to be addressed in future studies in which it is aimed to improve physical activity after stroke.
References
- Ursin M, Ihle-Hansen H, Fure B, et al. Effects of premorbid physical activity on stroke severity and post-stroke functioning. Journal of Rehabilitation Medicine. 2015; 47: 612-617.
- Gordon N, Gulanick M, Costa F, et al. Physical activity and exercise recommendations for stroke survivors: an American Heart Association scientific statement from the Council on Clinical Cardiology, Subcommittee on Exercise, Cardiac Rehabilitation, and Prevention; the Council on Cardiovascular Nursing; the Council on Nutrition, Physical Activity, and Metabolism; and the Stroke Council. Stroke. 2004; 35: 1230-1240.
- Eng J, Tang P. Gait training strategies to optimize walking ability in people with stroke: a synthesis of the evidence. Expert review of neuro therapeutics. 2007; 7: 1417-1436.
- Gebruers N, Vanroy C, Truijen S, et al. Monitoring of physical activity after stroke: a systematic review of accelerometry-based measures. Archives of physical medicine and rehabilitation. 2010; 91: 288-297.
- English C, Manns PJ, Tucak C, et al. Physical activity and sedentary behaviors in people with stroke living in the community: a systematic review. Phys Ther. 2014; 94: 185-196.
- Lee C, Folsom A, Blair S. Physical activity and stroke risk: a meta-analysis. Stroke. 2003; 34: 2475-2481.
- Cheung Y, Moon Y, Kulick E, et al. Leisure-Time Physical Activity and Cardiovascular Mortality in an Elderly Population in Northern Manhattan: A Prospective Cohort Study. J Gen Intern Med. 2016.
- van der Ploeg HP, Streppel KR, van der Beek AJ, et al. The Physical Activity Scale for Individuals with Physical Disabilities: test-retest reliability and comparison with an accelerometer. J Phys Act Health. 2007; 4: 96-100.
- Hosseinpoor AR, Bergen N, Kostanjsek N, et al. Socio-demographic patterns of disability among older adult populations of low-income and middle-income countries: results from World Health Survey. Int J Public Health. 2015; 61: 337-345.
- Michael K, Macko RF. Ambulatory activity intensity profiles, fitness, and fatigue in chronic stroke. Top Stroke Rehabil. 2007; 14: 5-12.
- Pratt M, Macera CA, Blanton C. Levels of physical activity and inactivity in children and adults in the United States: current evidence and research issues. Med Sci Sports Exerc. 1999; 31: S526-533.
- van de Port IG, Wevers LE, Lindeman E, et al. Effects of circuit training as alternative to usual physiotherapy after stroke: randomised controlled trial. BMJ. 2012; 344: e2672.
- van de Port IG, Wevers L, Roelse H, et al. Cost-effectiveness of a structured progressive task-oriented circuit class training programme to enhance walking competency after stroke: the protocol of the FIT-Stroke trial. BMC Neurol. 2009; 9: 43.
- Washburn RA, Zhu W, McAuley E, et al. The physical activity scale for individuals with physical disabilities: development and evaluation. Arch Phys Med Rehabil. 2002; 83: 193-200.
- van den Berg-Emons RJ, L'Ortye AA, Buffart LM, et al. Validation of the Physical Activity Scale for individuals with physical disabilities. Arch Phys Med Rehabil. 2011; 92: 923-928.
- de Groot S, van der Woude LH, Niezen A, et al. Evaluation of the physical activity scale for individuals with physical disabilities in people with spinal cord injury. Spinal Cord. 2010; 48: 542-547.
- Eriks-Hoogland IE, de Groot S, Post MW, et al. Correlation of shoulder range of motion limitations at discharge with limitations in activities and participation one year later in persons with spinal cord injury. J Rehabil Med. 2011; 43: 210-215.
- Baert I, Feys H, Daly D, et al. Are patients 1 year post-stroke active enough to improve their physical health?. Disabil Rehabil. 2012; 34: 574-580.
- Ellis R, Kosma M, Cardinal BJ, et al. Physical activity beliefs and behaviour of adults with physical disabilities. Disabil Rehabil. 2007; 29: 1221-1227.
- Frost Y, Weingarden H, Zeilig G, et al. Self-Care Self-Efficacy Correlates with Independence in Basic Activities of Daily Living in Individuals with Chronic Stroke. J Stroke Cerebrovasc Dis. 2015; 24: 1649-1655.
- Rand D, Eng JJ, Tang PF, et al. Daily physical activity and its contribution to the health-related quality of life of ambulatory individuals with chronic stroke. Health Qual Life Outcomes. 2010; 8: 80, 7525-8-80.
- Giacobbi PR, Jr, Stancil M, Hardin B, et al. Physical activity and quality of life experienced by highly active individuals with physical disabilities. Adapt Phys Activ Q. 2008; 25: 189-207.
- Shaw BA, Spokane LS. Examining the association between education level and physical activity changes during early old age. J Aging Health. 2008; 20: 767-787.
- Chad KE, Reeder BA, Harrison EL, et al. Profile of physical activity levels in community-dwelling older adults. Med Sci Sports Exerc. 2005; 37: 1774-1784.
- Kaplan MS, Newsom JT, McFarland BH, et al. Demographic and psychosocial correlates of physical activity in late life. Am J Prev Med. 2001; 21: 306-312.
- He XZ BD. Differences in leisure-time, household, and work-related physical activity by race, ethnicity, and education. Journal of General Internal Medicine. 2005; 20: 259-266.
- Kunkel D, Fitton C, Burnett M, et al. Physical inactivity post-stroke: a 3-year longitudinal study. Disabil Rehabil. 2015; 37: 304-310.
- Pahlman U, Savborg M, Tarkowski E. Cognitive dysfunction and physical activity after stroke: the Gothenburg cognitive stroke study in the elderly. J Stroke Cerebrovasc Dis. 2012; 21: 652-658.
- Duncan F, Lewis SJ, Greig CA, et al. Exploratory longitudinal cohort study of associations of fatigue after stroke. Stroke. 2015; 46: 1052-1058.
- Morris J, Oliver T, Kroll T, et al. The importance of psychological and social factors in influencing the uptake and maintenance of physical activity after stroke: a structured review of the empirical literature. Stroke Res Treat. 2012; 2012: 195249.