
Research Article
Phys Med Rehabil Int. 2018; 5(1): 1137.
Stress Fracture and Pubalgia: Spatiotemporal Trends, Revisit Rates and Causes
Pedrinelli A*, Hernandes AJ, Ejnisman L, Fagotti L, de Almeida AM and Lazaretti T
Grupo de Medicina d Esporte, Instituto de Ortopedia e Traumatologia do Hospital das Clinicas (HCFMUSP), Faculdade de Medicina, Universidade de S&aTilde;o Paulo, SP, Brazil
*Corresponding author: Pedrinelli A, Grupo de Medicina d Esporte, Instituto de Ortopedia e Traumatologia do Hospital das Clinicas (HCFMUSP), Faculdade de Medicina, Universidade de S&aTilde;o Paulo, SP, Brazil
Received: December 18, 2017; Accepted: January 31, 2018; Published: February 08, 2018
Abstract
Background: Pubalgia and pelvic stress fractures are common among athletes, with different therapeutic options having achieved varying rates of pain reduction and early return to sport activities.
Aims: We aimed to evaluate the rate of 90-day hospital revisits and its determinants after a surgical procedure for pubalgia and a diagnosis pelvic stress fracture, and to assess the trend of pelvic stress fracture prevalence over time.
Methods: This was a longitudinal secondary data analysis of patients undergoing surgical procedures for pubalgia and stress fracture of the pelvis in Florida, Kentucky and Maryland, derived from three HCUP state-specific databases.
Results: Of 2,112 subjects with pubalgia, the average age was 44.2 (± 23), 53.8% were female, 61% white and 15.9% were readmitted, the mean revisit time being 6.35 (± 18) days. Risk factors for revisits included age > 42 [OR: 2.41 (1.89, 3.09)], female gender, and a Charlson comorbidity score > 0 [OR: 2.3 (1.74, 3.01)]. The 678 participants with stress fractures presented a mean age of 65 years (± 19.1), 77% were female, 87% White, with a revisit rate of 24.9% with an average time of 8.65 (± 20.3). Increased 90-day revisit rates were associated with a Charlson co-morbidity score > 0 [OR: 3.11 (2.16, 4.52)] and Van Walraven score > 0 [OR: 2.53 (1.78, 3.64)], whereas private insurance payment decreased the risk of revisits.
Conclusion: Comorbidities and age significantly increased the risk of revisits for both conditions, while being female was an independent risk factor for pubalgia patients.
Keywords: Pubalgia; Stress fracture; Revisit; Spatiotemporal trend
Abbreviations
NSAIDs: Nonsteroidal Anti-Inflammatory Drugs; FAI: Femoroacetabular Impingement; MRI: Magnetic Resonance Imaging; SID: State Inpatient Database; SASD: State Ambulatory Surgery Database; SEDD: State Emergency Department Database; STROBE: STrengthening the Reporting of OBservational Studies in Epidemiology; HCUP: Healthcare Cost and Utilization Project; AHRQ: Agency for Healthcare Research and Quality; AHA: American Hospital Association.
Introduction
Pubalgia (groin pain) is a common cause of early retirement in many sports disciplines [1] and is frequently observed among athletes who perform sudden cutting, pivoting and kicking movements [1,2]. Pubalgia remains a diagnostic and therapeutic challenge [3–6]. The repetitive use of the pubis symphysis with the resulting progressive lesions on rectus abdominus, adductor muscles (rectaladductor syndrome) and the symphysis itself (osteitis pubis and joint injury) account for 40% of Pubalgia cases. “Sports hernia” or anteroinferior abdominal wall insufficiency is responsible for another 40% of pubalgia cases while diseases of the neighboring structures including the hip, iliopsoas, hamstring, sacroiliac, nerves as well as urogenital diseases account for 20% [7]. Athletic pubalgia, intraarticular hip pathologies (labral/femoroacetabular impingement), traumatic myotendinous ruptures (hip adductors, rectus abdominis), and diseases of the abdominal wall (inguinal hernias) are considered as differential diagnoses [1]. Recent consensus suggests a diagnostic classification based on five clinical entities; adductor, hip joint, pubic bone stress injury, iliopsoas-, and abdominal wall-related pathology [3]. Initial therapy for pubalgia is usually conservative consisting of massage, heat or ice, and NSAIDs, followed by rehabilitation. However, available evidence suggests that nonsurgical approach is unsuccessful. Surgical treatment options include open and laparoscopic repair of the abdominal wall and pelvic floor muscles as well as arthroscopy for femoroacetabular impingement (FAI) when the latter is comorbidity. Laparoscopic repair allows earlier return to sporting activities [8]. In one series, 32% of patients required arthroscopy for FAI after muscle repair surgery for pubalgia [2]. Another series reported 89% of patients returning to sports after both pubalgia surgery and arthroscopy for FAI were performed [9,10] as opposed to 25% following pubalgia surgery alone, and 50% with arthroscopy for FAI alone [2]. Optimum outcomes and unrestricted return to sports have been reported especially with concurrent, staged management of pubalgia surgery and arthroscopy [11].
Different treatment modalities for pubalgia and pelvic stress fractures have shown varying degrees of success at reducing pain and permitting the return to normal activities. However, no study to the best of our knowledge has described the trends on readmissions and revisits geographically over time.
Stress fractures which include fatigue and insufficiency fractures are frequently seen among sportsmen and women [12], as a result of repetitive stress on bone [13,14]. Rarely, they may result from radiotherapy [15]. Fatigue fractures result from the constant application of abnormal stresses on a normal bone while insufficiency fractures are due to normal cyclical loading on abnormal bone [14]. Stress fractures are more common in females [16] than males. Stress fractures of the pelvis are relatively rare making up just about 1-2% of all stress injuries [13,14,17] but can be particularly devastating since they require a longer rehabilitation period of approximately 6-12 months compared with 4-8 weeks for stress fractures at other sites [17]. They are more common among track and field athletes and those involved in other running sports disciplines [12]. The sites of the fractures typically vary with sports disciplines [12] and with the age of the subject. Fibular and tibial stress fractures occur mostly in the younger athletes while femoral and tarsal stress fractures are more frequent in the older [17]. In the adult, most of the repetitive injuries occur concurrently in the sacrum, pubic rami, and symphysis [14,15]. Pubic rami fractures which are more common in women, result in pain in the adductor, inguinal or perineal region [13]. Plain radiographs and MRI are the major diagnostic procedures for stress fractures [13,15,18]. Initial management is conservative, comprising analgesia, bed rest [18–20] with cessation of the precipitating activity [16] followed by an ‘active’ therapy where the athlete continues physical exercises depending on the fracture site [16]. In insufficiency fractures, this initial phase precedes anabolic or antiresorptive medications (calcium and vitamin D supplements, bisphosphonates, and teriparatide) meant to reduce the risk of further fractures [18– 20]. Electrical stimulation and extracorporeal shock wave therapy as adjunctive therapies have been reported to hasten recovery and return to sporting activities [19,20]. Surgery is required when the fracture site is unstable or in the setting of neurological deficits or disruption in the alignment of the sacrum. Osteosynthesis with screws or hinge fixation is the procedure of choice [19]. Reinforcement with methylmethacrylate cement [18,19], bone graft or bone graft substitutes have also been used to enhance fracture healing [18].
A prospective, randomized study of athletes with sports hernia reported that the surgical repair (laparoscopic mesh repair) was more efficient than conservative therapy, with 90% of patients who received surgical mesh returning to sporting activities within three months and being pain-free at the one-year follow-up [21]. Hip arthroscopy performed concomitantly for comorbid FAI has also been shown to enable a return to sporting activities [11]. However, few studies have reported the use of validated outcome measures. The Doha agreement identifies a significant association with methodologically weaker studies reporting higher rates of positive treatment outcomes [22]. The rates of readmissions, revisits, and their distribution over time and geographical regions are yet to be described.
According to the Hospital Readmissions Reduction Program created by the Patient Protection and Affordable Care Act, establishing surgical readmission rates is crucial, since they engender quality care and cost-containment [23]. Rates of readmission following surgery vary extensively, from 9% to 50%, across US hospitals [24–27]. In one series, 51.5% of those who had been discharged after surgery were either rehospitalized or died within the first year following discharge [27]. Postoperative complications are the most important risk factors for post-surgery readmissions [26,28]. Other risk factors reported among orthopedic patients include the length of hospitalization or admission to the intensive care unit, race, marital status and Medicaid insurance status. The latter three factors may indicate the state of a patient’s social and economic resources [29]. Other risk factors include index surgical admission complications, non-home discharge, patient comorbidities, teaching hospital status, and higher surgical volume. Surgical site infection is reported to be the most common reason for surgical readmissions [28]. Although some of these risk factors and reasons for surgical readmissions can apply to pubalgia and pelvic stress fracture patients who undergo surgical management, they are not specific to these patients. Indeed, risk factors and reasons for revisits and readmissions of pubalgia and pelvic stress fracture patients managed surgically, and the geographical pattern in which they occur over time is unknown.
In light of this gap in the literature, the objectives of our study are to (1) Evaluate the rate of 90-day hospital revisits and its risk factors following a surgical procedure for pubalgia and a diagnosis of stress pelvic fractures using three State HCUP databases. (2) Evaluate the trend of prevalence of stress fractures of the pelvis over time using spatial time series.
Materials and Methods
Study design
This study is a secondary data analysis of a longitudinal followup of patients undergoing surgical procedures for pubalgia and a diagnosis of stress fracture of the pelvis in Florida, Kentucky and Maryland as derived from three HCUP state-specific databases: The State Inpatient Database (SID), the State Ambulatory Surgery Database (SASD) and the State Emergency Department Database (SEDD). This study evaluates (1) The rate of 90-day hospital revisits following surgical procedures for pubalgia and a diagnosis of stress pelvic fractures as well as the corresponding risk factors and (2) the spatiotemporal trend in the prevalence of pelvic stress fractures This study is described per the STROBE (STrengthening the Reporting of OBservational studies in Epidemiology) guidelines [30].
Ethics
The Institutional Review Board of the University of Sao Paulo, Brazil approved our study.
Setting
The Healthcare Cost and Utilization Project (HCUP) is a system of databases composed of patient data reported by state and private data organizations, hospital associations and the federal government. It is sponsored by the Agency for Healthcare Research and Quality (AHRQ). We obtained data from three HCUP databases: The State Inpatient Database (SID) [31], the State Ambulatory Surgery Database (SASD) [32] and the State Emergency Department Database (SEDD) [33] in Florida, Kentucky, and Maryland for three years. The databases include de-identified discharge records for individual patients from all sources of coverage - Medicare, Medicaid, private insurance, and self-pay/uninsured. The SID consists of discharge records of all inpatient hospital visits including those admitted via the emergency department, the SASD covers ambulatory survey visits and release, and the SEDD reports records from emergency department visits that do not result in an admission. Individual patient records across all three databases were linked and tracked using an encrypted patientlevel identifier. Our study focused on patients who underwent surgical procedures for pubalgia, and stress fracture of the pelvis in Florida, Kentucky, and Maryland between the years 2010 and 2013.
The HCUP databases contain links to the AHA Annual Survey data elements containing additional hospital-specific indicators calculated from the American Hospital Association (AHA) data. The HCUP American Hospital Association (AHA) Linkage Files were used to link all the HCUP states databases with hospital-level longitude and latitude.
Participants
We identified patients who underwent a surgical procedure for pubalgia (ICD9 diagnostic code 848.8; CPT codes: 27299, 49659, 49999; ICD9 procedure code: 8045) or had a diagnosis of stress fracture of the pelvis (ICD9 diagnostic code: 73398; 73396) from 2010 to 2013 in Florida, Kentucky and Maryland. We excluded patients with previous abductor-tendon lesions, and inguinal hernia operations.
We defined the index surgical procedure as the first surgery for each pubalgia patient or the first index visit for patients with stress fractures from 2010 to 2013. The encrypted patient identifier connecting patients to subsequent procedures was used to calculate 90-day hospital revisit rates.
Outcomes measures
The 90-day hospital revisit rates and risk factors associated with revisits were analyzed using visit linkage variables across patient encounters. The time between the index procedure and hospital revisit in each of the three databases was used to calculate readmission rates. We defined a 90-day hospital readmission as a readmission to an ambulatory surgery center or inpatient hospital admission within 90 days from the index procedure. The other outcome variable was the spatial location of the visit between 2010 and 2013 as determined by the longitude and latitude of the hospital where care was provided.
Demographic data were defined at the time of the index procedure including age, race, patient residence (large metropolitan =1 million residents, small metropolitan ›1 million residents, micropolitan between 10,000 and 50,000 residents, or neither metropolitan nor micropolitan), primary expected payer (Medicaid, Medicare, private insurance, self-pay, or other). Co-morbidities categorized using the International Classification of Diseases (ICD-9). Mainly, Deyo- Charlson Comorbidity Index [34] and the Elixhauser-van Walraven Comorbidity Index [35] were also considered to determine their possible effect on surgical complication and revisit. Both indices are validated for their ability to predict mortality [36,37]. The Charlson Comorbidity Index is a weighted score derived from the sum of the scores for each of the comorbidities [34,35]. The Elixhauser-van Walraven Comorbidity Index includes a set of 30 acute and chronic comorbidity indicators, and the index score is based on the total number of comorbidity categories required to predict in-hospital mortality [35,38]. The cutoffs of ›5 for Charlson score and ›23 for Van Walraven score were chosen to represent the median so that we would have a similar number of subjects in each group, following a convention in a similar range from other publications [39,40].
Statistical methods
Our exploratory analysis started by evaluating the distributions, frequencies, and percentages for each of the numeric and categorical variables and then assessing categorical variables for near-zero variation or categorical variables with a low frequency of observations [41].
Our modeling strategy to evaluate risk factors employed a series of logistic regression models for the odds ratio and 95% confidence intervals of revisit within 90 days from the surgical procedure for pubalgia and a diagnosis of a stress fracture of the pelvis. Survival curves were calculated using Kaplan-Meier plots. To evaluate the geographical spread of surgical procedures and diagnoses for each of the pubalgia and stress fracture conditions over time, we used the longitude and latitude of each hospital facility (available from the American Hospital Association Database) where patients received care, stratified by year. We displayed years in consecutive maps. All analyses were performed using the R language [42].
Results
Descriptive data
Regarding pelvic stress fracture, our sample comprised 678 individuals with a mean age of 65 years old (± 19.1), 77% were female, and 87% were White. Medicare was the most common payment mechanism covering 62.7% of the population. The vast majority of our sample (95.3%) lived in metropolitan areas. The mean Charlson comorbidity index was 1.01 (± 1.57) while the mean Van Walraven score was 2.94 (± 5.92). Revisit rate was 24.9% and average time to those who had a revisit was 8.65 (± 20.3) days after the medical encounter. Across the study period, only the proportion of subjects with a lower socioeconomic status increased from 2009 to 2013 (Table 1).
Variable [Missing]
Total (678)
2009 (97)
2010 (127)
2011 (116)
2012 (112)
2013 (119)
2014 (107)
p
Age (y) [0]
65 (± 19.1)
66.2 (± 17.2)
64.3 (± 19.9)
65.2 (± 19.6)
66.7 (± 19.1)
64 (± 17.9)
64.2 (± 20.7)
0.835
Female [0]
522 (77%)
70 (72.2%)
95 (74.8%)
95 (81.9%)
88 (78.6%)
90 (75.6%)
84 (78.5%)
0.606
Race [8]
- White
583 (87%)
90 (92.8%)
104 (83.2%)
104 (89.7%)
95 (88%)
103 (86.6%)
87 (82.9%)
- Black
34 (5.1%)
1 (1%)
3 (2.4%)
7 (6%)
8 (7.4%)
6 (5%)
9 (8.6%)
- Hispanic
42 (6.3%)
5 (5.2%)
14 (11.2%)
3 (2.6%)
4 (3.7%)
10 (8.4%)
6 (5.7%)
- Asian or Pacific Islander
4 (0.6%)
0 (0%)
0 (0%)
1 (0.9%)
0 (0%)
0 (0%)
3 (2.9%)
- Native American
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
- Other
7 (1%)
1 (1%)
4 (3.2%)
1 (0.9%)
1 (0.9%)
0 (0%)
0 (0%)
Payment source [0]
0.328
- Medicare
425 (62.7%)
57 (58.8%)
84 (66.1%)
75 (64.7%)
68 (60.7%)
70 (58.8%)
71 (66.4%)
- Medicaid
26 (3.8%)
2 (2.1%)
2 (1.6%)
5 (4.3%)
8 (7.1%)
5 (4.2%)
4 (3.7%)
- Private insurance
193 (28.5%)
37 (38.1%)
35 (27.6%)
30 (25.9%)
31 (27.7%)
32 (26.9%)
28 (26.2%)
- Self-pay
13 (1.9%)
0 (0%)
3 (2.4%)
3 (2.6%)
0 (0%)
5 (4.2%)
2 (1.9%)
- No charge
1 (0.1%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
1 (0.8%)
0 (0%)
- Other
20 (2.9%)
1 (1%)
3 (2.4%)
3 (2.6%)
5 (4.5%)
6 (5%)
2 (1.9%)
Location [3]
0.466
- Non-CBSA
20 (3%)
3 (3.2%)
4 (3.2%)
4 (3.4%)
2 (1.8%)
1 (0.8%)
6 (5.6%)
- Micropolitan Statistical Area
12 (1.8%)
2 (2.1%)
3 (2.4%)
4 (3.4%)
1 (0.9%)
2 (1.7%)
0 (0%)
- Metropolitan Statistical Area
643 (95.3%)
90 (94.7%)
119 (94.4%)
108 (93.1%)
109 (97.3%)
116 (97.5%)
101 (94.4%)
Median household income (percentile) [11]
0.002
- 0 to 25th
186 (27.9%)
17 (18.1%)
25 (20.7%)
30 (25.9%)
34 (30.6%)
38 (32.2%)
42 (39.3%)
- 26th to 50th
209 (31.3%)
34 (36.2%)
33 (27.3%)
35 (30.2%)
26 (23.4%)
41 (34.7%)
40 (37.4%)
- 51st to 75th
185 (27.7%)
29 (30.9%)
47 (38.8%)
31 (26.7%)
35 (31.5%)
25 (21.2%)
18 (16.8%)
- 76th to 100th
87 (13%)
14 (14.9%)
16 (13.2%)
20 (17.2%)
16 (14.4%)
14 (11.9%)
7 (6.5%)
Charlson comorbidity score [0]
1.01 (± 1.57)
1.22 (± 1.72)
1.09 (± 1.57)
0.78 (± 1.25)
0.95 (± 1.37)
1.04 (± 1.75)
0.99 (± 1.7)
0.357
Van Walraven comorbidity score [0]
2.94 (± 5.92)
3.56 (± 6.03)
3.12 (± 5.8)
2.39 (± 5.65)
2.72 (± 4.98)
3.08 (± 6.53)
2.84 (± 6.45)
0.776
Revisit [0]
169 (24.9%)
26 (26.8%)
34 (26.8%)
24 (20.7%)
32 (28.6%)
24 (20.2%)
29 (27.1%)
0.545
Table 1: Patient sample characteristics for stress fracture of the pelvis or of the femoral neck categorized by year.
Factors associated with an increased 90-day revisit after a stress pelvic fracture of the pelvis were Charlson co-morbidity score > 0 [OR: 3.11 (2.16, 4.52)], and Van Walraven score > 0 [OR: 2.53 (1.78, 3.64)]. Patients with private insurance payment had lower risk of revisits [OR: 0.49 (0.32, 0.75)] (Table 2).
Revisit
Age (y) = 68
1 [Reference]
Age (y) > 68
1.42 (1, 2.01)
Female FALSE
1 [Reference]
Female TRUE
0.84 (0.56, 1.26)
Race White
1 [Reference]
Race Black
1.46 (0.67, 3)
Race Hispanic
1.08 (0.51, 2.15)
Race Asian or Pacific Islander
1.02 (0.0501, 8.01)
Race Native American
Race Other
0.51 (0.0268, 3.01)
Payment source Medicare
1 [Reference]
Payment source Medicaid
1.07 (0.43, 2.44)
Payment source Private insurance
0.49 (0.32, 0.75)
Payment source Self-pay
0.44 (0.0669, 1.66)
Payment source No charge
0 (, 7.550194e+41)
Payment source Other
0.13 (0.007, 0.62)
Median household income (percentile) 0 to 25th
1 [Reference]
Median household income (percentile) 26th to 50th
0.75 (0.47, 1.18)
Median household income (percentile) 51st to 75th
0.81 (0.51, 1.28)
Median household income (percentile) 76th to 100th
0.75 (0.41, 1.34)
Charlson comorbidity score = 0
1 [Reference]
Charlson comorbidity score > 0
3.11 (2.16, 4.52)
Van Walraven comorbidity score = 0
1 [Reference]
Van Walraven comorbidity score > 0
2.53 (1.78, 3.64)
Table 2: 90-Day revisit odds ratio for stress fracture of the pelvis or of the femoral neck.
When performing the survival analysis for the 90-day revisit after stress fractures of the pelvis, hazard ratios were higher for subjects above 68 years of age [1.39 (1.03, 1.89)], or for subjects who presented Charlson co-morbidity indexes > 0 [2.69 (1.95, 3.72)]. However, hazard ratios were lower for those subjects having their procedures covered under private insurance [0.53 (0.36, 0.77)] (Table 3).
Revisit
Age (y) = 68
1 [Reference]
Age (y) > 68
1.39 (1.03, 1.89)
Female FALSE
1 [Reference]
Female TRUE
0.84 (0.59, 1.19)
Race White
1 [Reference]
Race Black
1.34 (0.73, 2.47)
Race Hispanic
1.07 (0.58, 1.98)
Race Asian or Pacific Islander
1.15 (0.16, 8.2)
Race Native American
(,)
Race Other
0.56 (0.0788, 4.03)
Payment source Medicare
1 [Reference]
Payment source Medicaid
1.04 (0.51, 2.13)
Payment source Private insurance
0.53 (0.36, 0.77)
Payment source Self-pay
0.46 (0.11, 1.85)
Payment source No charge
0 (0, Inf)
Payment source Other
0.15 (0.0208, 1.07)
Median household income (percentile) 0 to 25th
1 [Reference]
Median household income (percentile) 26th to 50th
0.78 (0.52, 1.15)
Median household income (percentile) 51st to 75th
0.85 (0.57, 1.26)
Median household income (percentile) 76th to 100th
0.78 (0.47, 1.3)
Charlson comorbidity score = 0
1 [Reference]
Charlson comorbidity score > 0
2.69 (1.95, 3.72)
Van Walraven comorbidity score = 0
1 [Reference]
Van Walraven comorbidity score > 0
2.26 (1.66, 3.08)
Table 3: Survival analysis: 90-Day readmission hazard ratio for stress fracture of the pelvis or of the femoral neck.
Our sample of individuals with pubalgia comprised of 2112 subjects of average age 44.2 (± 23), 53.8% of them female, 61% white, and 24% of them paying using Medicare. Most of the subjects resided in metropolitan areas (93.4%). The mean Charlson comorbidity index was of 0.28 (± 0.78) while the average Van Walraven score was of 0.86 (± 3.61). The percentage of individuals readmitted was 15.9%, the mean revisit time being 6.35 (± 18) days after the procedure (Table 4).
Variable [Missing]
Total (2,112)
2009 (272)
2010 (342)
2011 (385)
2012 (352)
2013 (392)
2014 (369)
P
Age (y) [0]
44.2 (± 23)
41.6 (± 23.1)
43 (± 24.3)
43.6 (± 22.6)
45.7 (± 22.9)
45 (± 21.8)
45.4 (± 23.4)
0.185
Female [0]
1,136 (53.8%)
133 (48.9%)
181 (52.9%)
218 (56.6%)
199 (56.5%)
213 (54.3%)
192 (52%)
0.354
Race [16]
- White
1,278 (61%)
182 (67.4%)
210 (63.1%)
226 (59.2%)
217 (61.6%)
223 (56.9%)
220 (59.9%)
- Black
388 (18.5%)
49 (18.1%)
70 (21%)
66 (17.3%)
54 (15.3%)
77 (19.6%)
72 (19.6%)
- Hispanic
365 (17.4%)
28 (10.4%)
47 (14.1%)
73 (19.1%)
70 (19.9%)
79 (20.2%)
68 (18.5%)
- Asian or Pacific Islander
5 (0.2%)
1 (0.4%)
3 (0.9%)
0 (0%)
0 (0%)
1 (0.3%)
0 (0%)
- Native American
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
0 (0%)
- Other
60 (2.9%)
10 (3.7%)
3 (0.9%)
17 (4.5%)
11 (3.1%)
12 (3.1%)
7 (1.9%)
Payment source [0]
< 0.001
- Medicare
507 (24%)
61 (22.4%)
90 (26.3%)
81 (21%)
85 (24.1%)
91 (23.2%)
99 (26.8%)
- Medicaid
345 (16.3%)
51 (18.8%)
68 (19.9%)
54 (14%)
52 (14.8%)
54 (13.8%)
66 (17.9%)
- Private insurance
796 (37.7%)
82 (30.1%)
92 (26.9%)
179 (46.5%)
148 (42%)
162 (41.3%)
133 (36%)
- Self-pay
302 (14.3%)
51 (18.8%)
67 (19.6%)
40 (10.4%)
39 (11.1%)
55 (14%)
50 (13.6%)
- No charge
27 (1.3%)
4 (1.5%)
7 (2%)
1 (0.3%)
3 (0.9%)
9 (2.3%)
3 (0.8%)
- Other
135 (6.4%)
23 (8.5%)
18 (5.3%)
30 (7.8%)
25 (7.1%)
21 (5.4%)
18 (4.9%)
Location [16]
< 0.001
- Non-CBSA
66 (3.1%)
5 (1.9%)
14 (4.1%)
9 (2.3%)
10 (2.9%)
17 (4.4%)
11 (3%)
- Micropolitan Statistical Area
72 (3.4%)
14 (5.2%)
18 (5.3%)
23 (6%)
8 (2.3%)
5 (1.3%)
4 (1.1%)
- Metropolitan Statistical Area
1,958 (93.4%)
250 (92.9%)
307 (90.6%)
352 (91.7%)
331 (94.8%)
365 (94.3%)
353 (95.9%)
Median household income (percentile) [34]
< 0.001
- 0 to 25th
661 (31.8%)
73 (27.3%)
109 (32.8%)
119 (31.1%)
108 (31.2%)
131 (34.2%)
121 (33%)
- 26th to 50th
642 (30.9%)
89 (33.3%)
111 (33.4%)
103 (26.9%)
83 (24%)
138 (36%)
118 (32.2%)
- 51st to 75th
522 (25.1%)
71 (26.6%)
71 (21.4%)
101 (26.4%)
114 (32.9%)
84 (21.9%)
81 (22.1%)
- 76th to 100th
253 (12.2%)
34 (12.7%)
41 (12.3%)
60 (15.7%)
41 (11.8%)
30 (7.8%)
47 (12.8%)
Charlson comorbidity score [0]
0.28 (± 0.78)
0.36 (± 1.03)
0.24 (± 0.66)
0.26 (± 0.73)
0.27 (± 0.8)
0.29 (± 0.83)
0.26 (± 0.66)
0.684
Van Walraven comorbidity score [0]
0.86 (± 3.61)
1.07 (± 4.54)
0.83 (± 3.28)
0.72 (± 3.48)
0.91 (± 3.88)
0.74 (± 3.34)
0.96 (± 3.24)
0.833
Revisit [0]
336 (15.9%)
58 (21.3%)
62 (18.1%)
51 (13.2%)
57 (16.2%)
62 (15.8%)
46 (12.5%)
0.028
Table 4: Sample characteristics of subjects with pubalgia categorized by year.
Risk factors for revisit after pubalgia were age > 42 [OR: 2.41 (1.89, 3.09)], female gender [OR: 1.34 (1.06, 1.7)], and Charlson comorbidity score > 0 [OR: 2.3 (1.74, 3.01)] (Table 5).
Revisit
Age (y) = 42
1 [Reference]
Age (y) > 42
2.41 (1.89, 3.09)
Female FALSE
1 [Reference]
Female TRUE
1.34 (1.06, 1.7)
Race White
1 [Reference]
Race Black
0.64 (0.46, 0.89)
Race Hispanic
0.72 (0.51, 1)
Race Asian or Pacific Islander
0 (, 1.385595e+12)
Race Native American
Race Other
0.51 (0.19, 1.1)
Payment source Medicare
1 [Reference]
Payment source Medicaid
0.55 (0.39, 0.77)
Payment source Private insurance
0.32 (0.24, 0.43)
Payment source Self-pay
0.16 (0.0909, 0.26)
Payment source No charge
0.31 (0.0727, 0.9)
Payment source Other
0.31 (0.17, 0.53)
Median household income (percentile) 0 to 25th
1 [Reference]
Median household income (percentile) 26th to 50th
0.89 (0.66, 1.2)
Median household income (percentile) 51st to 75th
0.91 (0.66, 1.24)
Median household income (percentile) 76th to 100th
0.93 (0.62, 1.37)
Charlson comorbidity score = 0
1 [Reference]
Charlson comorbidity score > 0
2.3 (1.74, 3.01)
Table 5: 90-day revisit odds ratio for pubalgia.
Survival analysis for revisits in subjects experiencing pubalgia demonstrated that age > 42 years old [HR: 2.24 (1.79, 2.82)], female sex [HR: 1.3 (1.04, 1.61)] and Charlson co-morbidity index > 0 [HR: 2.12 (1.67, 2.69)] are risk factor for revisits after the first encounter. On the other side, being reimbursed with a mechanism other than Medicare and a Black/African-America race was associated with decrease risk of a revisit [HR: 0.66 (0.49, 0.91)] (Table 6).
Revisit
Age (y) = 42
1 [Reference]
Age (y) > 42
2.24 (1.79, 2.82)
Female FALSE
1 [Reference]
Female TRUE
1.3 (1.04, 1.61)
Race White
1 [Reference]
Race Black
0.66 (0.49, 0.91)
Race Hispanic
0.74 (0.54, 1)
Race Asian or Pacific Islander
0 (0, Inf)
Race Native American
(,)
Race Other
0.54 (0.24, 1.21)
Payment source Medicare
1 [Reference]
Payment source Medicaid
0.59 (0.44, 0.79)
Payment source Private insurance
0.36 (0.27, 0.46)
Payment source Self-pay
0.18 (0.11, 0.3)
Payment source No charge
0.36 (0.11, 1.12)
Payment source Other
0.35 (0.2, 0.59)
Median household income (percentile) 0 to 25th
1 [Reference]
Median household income (percentile) 26th to 50th
0.9 (0.69, 1.19)
Median household income (percentile) 51st to 75th
0.92 (0.69, 1.23)
Median household income (percentile) 76th to 100th
0.93 (0.65, 1.34)
Charlson comorbidity score = 0
1 [Reference]
Charlson comorbidity score > 0
2.12 (1.67, 2.69)
Table 6: Survival analysis for subjects with pubalgia: 90-day revisit hazard ratio.
Mapping spatial trends over time
Florida: We observed a north-to-south trend in the prevalence of stress fractures of the pelvis in the state of Florida. This pattern was maintained over the studied period. The Western regions of the state presented the lowest prevalence, with the northeastern and southeastern regions of the state having the highest concentration of cases in 2010 and 2011 (Figure 1).
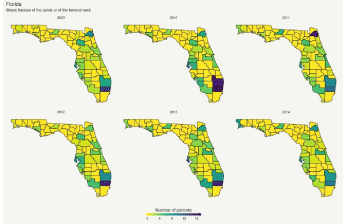
Figure 1: Geospatial trends in the prevalence of stress fractures of the pelvis or of the femoral neck in Florida.
Kentucky: The prevalence of stress fractures of the pelvis was higher in the northern regions of the state of Kentucky than in other areas, reaching a peak in 2011, and increased in the western regions during the studied period. Moreover, the eastern region of the state experienced a peak of these fractures in 2012 (Figure 2).
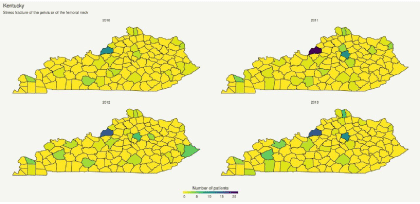
Figure 2: Geospatial trends of the prevalence of fractures of the pelvis or of the femoral neck in Kentucky.
Maryland: Although the prevalence of stress fractures was widespread around the state, Baltimore and its surrounding areas remained the regions with the largest concentration of events. There were no major temporal trends observed in this region regarding stress fractures. Contrarily, the Northwestern parts of the state experienced a decrease in the prevalence of stress fractures (Figure 3).
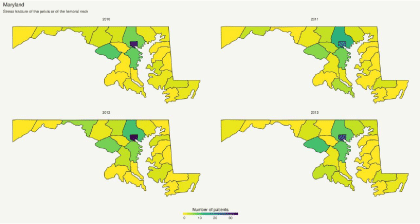
Figure 3: Geospatial trends of the prevalence of fractures of the pelvis or of the femoral neck in Maryland.
Discussion
To the best of our knowledge, this was the first study evaluating (1) the rate of 90-day hospital revisits and its risk factors following a surgical procedure for pubalgia or a diagnosis of stress pelvic fractures using three HCUP State databases and (2) the spatiotemporal trend in the prevalence of pelvic stress fractures. Approximately, 24.9% of all stress pelvic fracture patients and 15.9% of pubalgia patients presented a revisit within 90 days of their index procedure. The risk of a revisit was significantly greater coupled with co-morbidities and among elderly patients with both conditions, while female sex was an independent risk factor for pubalgia patients. Other factors associated with a lower risk of revisit included payment through a private insurance for stress pelvic fractures, Black or African-American race, and having the procedure reimbursed through anything other than Medicare among pubalgia patients. When evaluating the prevalence of stress fractures over time in three states, we observed the largest concentration of cases in 2010 and 2011 in the state of Florida, with the Northern and Eastern regions of Kentucky state experiencing a peak of these fractures in 2011 and 2012. In Maryland, the largest concentration of events was observed in Baltimore and its surrounding areas, contrary to the Northwestern parts of this state, which experienced a decrease in the prevalence of stress fractures.
Our study reported an overall 90-day revisit rate of 24.9% and 15.9% after stress pelvic fractures and pubalgia surgical procedures, respectively. This percentage is comparable to previous studies evaluating other hip conditions, where 19% of all hip fracture patients were readmitted within three months [43]. A prospective observational study reported high 90-day revisits rates of 41% after hospitalization for hip fractures [44]. In contrast, a retrospective study on patients who underwent total hip arthroplasty or total knee arthroplasty reported an overall 90-day readmission rate of 7.8% [45]. Heterogeneity is often observed in readmission rates across different studies, ranging from 34% [46] at four weeks to 16.7% [47] over six months. Reasons for the wide heterogeneity in readmission rates have been debated, with some of the literature focusing on factors such as comorbidities [48,49], age [50], gender [50,51], race [52,53] and payer group [54].
Higher co-morbidity indices were one of the factors consistently associated with a high revisit rate for both conditions in our study. Our results agree with previous literature where the primary causes for revisits were associated with medical comorbidities rather than with hospital-acquired or surgical complications [48,49]. Patients with common co-morbidities such as infections, diabetes, pulmonary disease, renal failure, delirium, cardiac arrhythmias, and congestive heart failure have been reported to be associated with an increased risk of readmission [43,48,49,55,56], as have those presenting high body mass index and high American Society of Anesthesiologist scores [57]. Patients with co-existing medical conditions have an increased risk of revisits due to poor functional status and deteriorating preexisting illnesses [44]. A higher risk of revisits after discharge reflects the patient’s medical condition, reinforcing the hypothesis that minor active clinical problems can lead to revisits if untreated before discharge [43]. Furthermore, malnutrition is one of the determinants of increased hospital revisits [58]. It is therefore essential to identify and manage any medical and rehabilitation issues before discharge to prevent readmissions related to co-morbid conditions.
In our study, socio-demographic characteristics such as older age and female gender were also independent risk factors for higher revisit rates. Older age has been previously associated with an increased risk of hospital readmission both within and beyond 30 days for fragility fractures [50], including hip fractures [45,49]. This supports the view that elderly patients have a lower degree of functional recovery, with poor mobility and inability to functionally cope with the surgical stress after discharge, which in turn may account for higher revisit rates [44,59]. Also, female gender as a risk factor for higher readmission rates has been reported in retrospective studies investigating patients undergoing proximal humerus fracture surgery [51] and septorhinoplasty [52]. Stress fractures are more common in females due to geometric skeletal differences, women presenting a wider pelvis and a longer femur compared to men [60]. Elderly female patients with fractures have an increased risk of having osteoporosis and osteopenia, which are reported as prognostic factors for failure after fracture fixation, these patients also presenting decreased bone marrow density [51,61]. In contrast, previous studies reported male sex as an independent risk factor for higher readmission rates [48– 50,62], potential reasons being the increased mortality risk in men with hip fractures, heavy alcohol and tobacco consumption, and advanced age with poor health status in the presence of chronic conditions [63–65].
Consistent with previous research using the same HCUP databases, the Black or African-American race was one of the factors associated with a decreased risk of a revisit [52]. One potential explanation is that Black and African American patients are less prone to osteoporosis due to higher peak bone mass, lower bone turnover rates, and advantageous femur geometry [66,67], which might explain their lower readmission rates after orthopedic conditions as reported in our study. In contrast to our findings, racial and ethnic disparities have been previously reported to lead Black and African American patients to have higher revisit rates when compared with White patients [68–71]. Notably, Black patients treated at minorityserving hospitals presented higher revisit rates than when treated at non-minority-serving hospitals [53,68]. The leading causes of racial disparities seem to be related to poor-quality of hospital care [72,73], associated patient poverty or low socioeconomic status [53], and issues in access to health care services in outpatient settings that might prevent revisits [74]. Patients with Medicaid, private insurance, and self-pay payer insurance were additional factors associated with decreased revisit rates in our study. This finding is similar to previously-reported results by the North Carolina program’s transitional care intervention. According to their report, a 20% reduction in readmission risk among Medicaid patients was observed among those with complex chronic medical conditions when compared to clinically similar patients receiving usual care [75]. Contrary to our findings, higher revisit rates are reported in patients with Medicaid insurance when compared to patients with other insurance types [51,54,76,77]. It has been suggested that less access to medical care, poor functional status leading to decreased functional outcomes, and different reimbursement rates for payer types might all affect patient care, ultimately resulting in hospital revisits [78].
In relation to the spatiotemporal trends, Florida, Kentucky and Maryland states presented a regional increase in the prevalence of stress fractures, but with different patterns across states. In Florida, a higher prevalence was more noticeable in the southern portions of the state. In Kentucky, the rise in prevalence of stress fractures occurred particularly in the northern and eastern regions, presenting a peak prevalence in 2011 and 2012. In Maryland, this increase was prominent around the Baltimore region. The progressive concentration of cases in metropolitan areas such as Baltimore might be explained by the progressive migration of ill and disabled people to cities for healthcare access [79,80]. Although the distribution of pelvic stress fractures was more widespread in Maryland, we also observed a decline in prevalence in the northwestern parts of the state.
Despite filling an important gap in the literature, our study does have limitations usually associated with an observational design. First, despite our best efforts in controlling for missing rates, some of our variables had high rates. To minimize this limitation, we made use of imputation algorithms followed by sensitivity analyses to ensure that our conclusions were valid under different assumptions. Second, the analysis was limited to the three states of Florida, Kentucky, and Maryland, which may have unique patients and care patterns that may not be representative of the entire USA. Although we cannot claim representativeness, these three states are likely not outliers to these conditions, and therefore our results should be mostly applicable to other areas of the United States and other parts of the world.
Future studies should further investigate which types of complications are bringing patients back to the hospital. Moreover, including other indicators of quality of care besides readmissions should be relevant, including factors such as patient satisfaction, function, and quality of life [81] With better understanding of the causes and risk factors of revisits to optimize patient care, policymakers and hospital administrators can focus on allocating health service resources to improve patient outcomes and reduce the overall burden of healthcare cost.
References
- Oliveira AL de, Andreoli CV, Ejnisman B, Queiroz RD, Pires OGN, Falótico GG. Perfil epidemiológico dos pacientes com diagnóstico de pubalgia do atleta. Rev Bras Ortop. 2016; 51: 692–696.
- Elattar O, Choi H-R, Dills VD, Busconi B. Groin injuries (athletic pubalgia) and return to play. Sports health. 2016; 8: 313–323.
- Rankin AT, Bleakley CM, Cullen M. Hip joint pathology as a leading cause of groin pain in the sporting population: A 6-year review of 894 cases. Am J Sports Med. 2015; 43: 1698–1703.
- Nam A, Brody F. Management and therapy for sports hernia. J Am Coll Surg. 2008; 206: 154–164.
- Puig P, Find P, Savalli L. Pubalgia: From diagnosis to return to the field pubalgia. In: Annals of adaptation and physical mechanics. 2004; 47: 356– 364.
- Kluin J, Hoed PT den, Linschoten R van, IJzerman JC, Steensel CJ van. Endoscopic evaluation and treatment of groin pain in the athlete. Am J Sports Med. 2004; 32: 944–949.
- Balconi G. US in pubalgia. J Ultrasound. 2011; 14: 157–166.
- Swan Jr KG, Wolcott M. The athletic hernia: A systematic review. Clin Orthop Relat Res. 2007; 455: 78-87.
- Munegato D, Bigoni M, Gridavilla G, Olmi S, Cesana G, Zatti G. Sports hernia and femoroacetabular impingement in athletes: A systematic review. World J Clin Cases. 2015; 3: 823.
- Larson CM, Pierce BR, Giveans MR. Treatment of athletes with symptomatic intra-articular hip pathology and athletic pubalgia/sports hernia: A case series. Arthroscopy. 2011; 27: 768–775.
- Larson CM. Sports Hernia/Athletic Pubalgia: Evaluation and Management. Sports Health. 2014; 6: 139.
- Iwamoto J, Takeda T. Stress fractures in athletes: Review of 196 cases. J Orthop Sci. 2003; 8: 273–278.
- Behrens SB, Deren ME, Matson A, Fadale PD, Monchik KO. Stress fractures of the pelvis and legs in athletes: A review. Sports Health. 2013; 5: 165–174.
- Miller C, Major N, Toth A. Pelvic stress injuries in the athlete. Sports Med. 2003; 33: 1003–1012.
- Tins BJ, Garton M, Cassar-Pullicino VN, Tyrrell PN, Lalam R, Singh J. Stress fracture of the pelvis and lower limbs including atypical femoral fractures—a review. Insights Imaging. 2015; 6: 97–110.
- Reeder MT, Dick BH, Atkins JK, Pribis AB, Martinez JM. Stress fractures. Sports Medicine. 1996; 22: 198–212.
- Matheson G, Clement D, McKenzie D, Taunton J, Lloyd-Smith D, MacIntyre J. Stress fractures in athletes: A study of 320 cases. Am J Sports Med. 1987; 15: 46–58.
- Matcuk GR, Mahanty SR, Skalski MR, Patel DB, White EA, Gottsegen CJ. Stress fractures: Pathophysiology, clinical presentation, imaging features, and treatment options. Emerg Radiol. 2016; 23: 365–375.
- Longhino V, Bonora C, Sansone V. The management of sacral stress fractures: Current concepts. Clin Cases Miner Bone Metab. 2011; 8: 19.
- Tsiridis E, Upadhyay N, Giannoudis P. Sacral insufficiency fractures: Current concepts of management. Osteoporos Int. 2006; 17: 1716–1725.
- Paajanen H, Brinck T, Hermunen H, Airo I. Laparoscopic surgery for chronic groin pain in athletes is more effective than nonoperative treatment: A randomized clinical trial with magnetic resonance imaging of 60 patients with sportsman’s hernia (athletic pubalgia). Surgery. 2011; 150: 99–107.
- Weir A, Brukner P, Delahunt E, Ekstrand J, Griffin D, Khan KM, et al. Doha agreement meeting on terminology and definitions in groin pain in athletes. Br J Sports Med. 2015; 49: 768–774.
- Anijar YE. The patient readmission rate penalty in the affordable care act. Health L & Pol’y Brief. 2014; 8: 57.
- Fry DE, Pine M, Pine G. Medicare post-discharge deaths and readmissions following elective surgery. Am J SurgAm J Surg. 2014; 207: 326–330.
- Tsai TC, Joynt KE, Orav EJ, Gawande AA, Jha AK. Variation in surgicalreadmission rates and quality of hospital care. N Engl J Med. 2013; 369: 1134–1142.
- 26. Kassin MT, Owen RM, Perez SD, Leeds I, Cox JC, Schnier K, et al. Risk factors for 30-day hospital readmission among general surgery patients. J Am Coll Surg. 2012; 215: 322–330.
- Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009; 360: 1418–1428
- Merkow RP, Ju MH, Chung JW, Hall BL, Cohen ME, Williams MV, et al. Underlying Reasons Associated With Hospital Readmission Following Surgery in the United States. JAMA. 2015; 313: 483–495.
- Dailey EA, Cizik A, Kasten J, Chapman JR, Lee MJ. Risk factors for readmission of Orthopaedic surgical patients. J Bone Joint Surg Am. 2013; 95: 1012–1019.
- Elm E von, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies. PLoS Med. 2007; 4: e296.
- Healthcare cost and utilization project. Overview of the state inpatient databases (SID).
- Healthcare cost and utilization project. Overview of the state ambulatory surgery and services databases (SASD).
- Healthcare cost and utilization project. Overview of the state emergency department databases (SEDD).
- Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with icd-9-cm administrative databases. J Clin Epidemiol. 1992; 45: 613–619.
- Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J Chronic Dis. 1987; 40: 373–383.
- Chu Y-T, Ng Y-Y, Wu S-C. Comparison of different comorbidity measures for use with administrative data in predicting short-and long-term mortality. BMC Health Serv Res. 2010; 10: 140.
- Quan H, Li B, Couris CM, Fushimi K, Graham P, Hider P, et al. Updating and validating the charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol. 2011; 173: 676–682.
- Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998; 36: 8–27.
- Kim SM, Kim MJ, Jung H, Kim K, Kim SJ, Jang JH, et al. Comparison of the Freiburg and Charlson comorbidity indices in predicting overall survival in elderly patients with newly diagnosed multiple myeloma. Biomed Res Int. 2014; 2014: 437852.
- Ladha KS, Zhao K, Quraishi SA, Kurth T, Eikermann M, Kaafarani HM, et al. The Deyo-Charlson and Elixhauser-van Walraven Comorbidity Indices as predictors of mortality in critically ill patients. BMJ open. 2015; 5: e008990.
- Kuhn M, Johnson K. Applied predictive modeling. 2013. Springer. ISBN-13.
- R Core Team. R: A language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2015.
- Hahnel J, Burdekin H, Anand S. Re-admissions following hip fracture surgery. Ann R Coll Surg Engl. 2009; 91: 591–595.
- Giusti A, Barone A, Razzano M, Pizzonia M, Oliveri M, Pioli G. Predictors of hospital readmission in a cohort of 236 elderly discharged after surgical repair of hip fracture: One-year follow-up. Aging Clin Exp Res. 2008; 20: 253–259.
- Saucedo JM, Marecek GS, Wanke TR, Lee J, Stulberg SD, Puri L. Understanding readmission after primary total hip and knee arthroplasty: Who’s at risk? J Arthroplasty. 2014; 29: 256–260.
- Boockvar KS, Halm EA, Litke A, Silberzweig SB, McLaughlin M, Penrod JD, et al. Hospital readmissions after hospital discharge for hip fracture: Surgical and nonsurgical causes and effect on outcomes. J Am Geriatr Soc. 2003; 51: 399–403.
- Ottenbacher KJ, Smith PM, Illig SB, Peek MK, Fiedler RC, Granger CV. Hospital readmission of persons with hip fracture following medical rehabilitation. Arch Gerontol Geriatr. 2003; 36: 15–22.
- French DD, Bass E, Bradham DD, Campbell RR, others. Rehospitalization after hip fracture: Predictors and prognosis from a national veterans study. J Am Geriatr Soc. 2008; 56: 705–710.
- Kates SL, Behrend C, Mendelson DA, Cram P, Friedman SM. Hospital readmission after hip fracture. Arch Orthop Trauma Surg. 2015; 135: 329– 337.
- Mathew SA, Gane E, Heesch KC, McPhail SM. Risk factors for hospital representation among older adults following fragility fractures: A systematic review and meta-analysis. BMC Med. 2016; 14: 136.
- Zhang AL, Schairer WW, Feeley BT. Hospital readmissions after surgical treatment of proximal humerus fractures: Is arthroplasty safer than open reduction internal fixation? Clin Orthop Relat Res. 2014; 472: 2317–2324.
- Spataro E, Piccirillo JF, Kallogjeri D, Branham GH, Desai SC. Revision rates and risk factors of 175 842 patients undergoing septorhinoplasty. JAMA Facial Plast. Surg. 2016; 18: 212–219.
- Tsai TC, Orav EJ, Joynt KE. Disparities in surgical 30-day readmission rates for Medicare beneficiaries by race and site of care. Ann Surg. 2014; 259: 1086.
- Schairer WW, Zhang AL, Feeley BT. Hospital readmissions after primary shoulder arthroplasty. J Shoulder Elbow Surg. 2014; 23: 1349–1355.
- Pollock FH, Bethea A, Samanta D, Modak A, Maurer JP, Chumbe JT. Readmission within 30 days of discharge after hip fracture care. Orthopedics. 2015; 38: e7–e13.
- Martin CT, Gao Y, Pugely AJ. Incidence and risk factors for 30-day readmissions after hip fracture surgery. Iowa Orthop J. 2016; 36: 155.
- Kester BS, Williams J, Bosco JA, Slover JD, Iorio R, Schwarzkopf R. The association between hospital length of stay and 90-day readmission risk for femoral neck fracture patients: Within a total joint arthroplasty bundled payment initiative. J Arthroplasty. 2016; 31: 2741–274
- Lim SL, Ong KCB, Chan YH, Loke WC, Ferguson M, Daniels L. Malnutrition and its impact on cost of hospitalization, length of stay, readmission and 3-year mortality. Clin Nutr. 2012; 31: 345–350.
- Khan M, Hossain F, Dashti Z, Muthukumar N. Causes and predictors of early re-admission after surgery for a fracture of the hip. J Bone Joint Surg Br. 2012; 94: 690–697.
- Beck T, Ruff C, Shaffer R, Betsinger K, Trone D, Brodine S. Stress fracture in military recruits: Gender differences in muscle and bone susceptibility factors. Bone. 2000; 27: 437–444.
- Goldhahn J, Suhm N, Goldhahn S, Blauth M, Hanson B. Influence of osteoporosis on fracture fixation-a systematic literature review. Osteoporos Int. 2008; 19: 761–772.
- Buecking B, Eschbach D, Koutras C, Kratz T, Balzer-Geldsetzer M, Dodel R, et al. Re-admission to level 2 unit after hip-fracture surgery–risk factors, reasons and outcome. Injury. 2013; 44: 1919–1925.
- Trombetti A, Herrmann F, Hoffmeyer P, Schurch M, Bonjour J-P, Rizzoli R. Survival and potential years of life lost after hip fracture in men and agematched women. Osteoporos Int. 2002; 13: 731–737.
- Jiang HX, Majumdar SR, Dick DA, Moreau M, Raso J, Otto DD, et al. Development and initial validation of a risk score for predicting in-hospital and 1-year mortality in patients with hip fractures. J Bone Miner Res. 2005; 20: 494–500.
- Bass E, French DD, Bradham DD, Rubenstein LZ. Risk-adjusted mortality rates of elderly veterans with hip fractures. Ann Epidemiol. 2007; 17: 514– 519.
- Silverman SL, Madison RE. Decreased incidence of hip fracture in Hispanics, Asians, and blacks: California hospital discharge data. Am. J. Public Health. 1988; 78: 1482–1483.
- Aloia JF. African Americans, 25-hydroxyvitamin d, and osteoporosis: A paradox. Am J Clin Nutr. 2008; 88: 545S–550S.
- Jha AK, Fisher ES, Li Z, Orav EJ, Epstein AM. Racial trends in the use of major procedures among the elderly. N Engl J Med. 2005; 353: 683–691.
- Martin J, Wang TY, Loriaux DB, Desai R, Adogwa O, Kuchibhatla M, et al. Race as a predictor of postoperative hospital readmission after spine surgery. Neurosurgery. 2016; 63: 191.
- Girotti ME, Shih T, Dimick JB, others. Racial disparities in readmissions and site of care for major surgery. J Am Coll Surg. 2014; 218: 423–430.
- Gani F, Lucas DJ, Kim Y, Schneider EB, Pawlik TM. Understanding variation in 30-day surgical readmission in the era of accountable care: Effect of the patient, surgeon, and surgical subspecialties. JAMA surgery. 2015; 150: 1042–1049.
- Regenbogen SE, Gawande AA, Lipsitz SR, Greenberg CC, Jha AK. Do differences in hospital and surgeon quality explain racial disparities in lowerextremity vascular amputations? Ann Surg. 2009; 250: 424–431.
- Dimick J, Ruhter J, Sarrazin MV, Birkmeyer JD. Black patients more likely than whites to undergo surgery at low-quality hospitals in segregated regions. Health Aff. 2013; 32: 1046–1053
- Hayanga AJ, Kaiser HE, Sinha R, Berenholtz SM, Makary M, Chang D. Residential segregation and access to surgical care by minority populations in us counties. J Am Coll Surg. 2009; 208: 1017–1022.
- Jackson CT, Trygstad TK, DeWalt DA, DuBard CA. Transitional care cut hospital readmissions for north Carolina Medicaid patients with complex chronic conditions. Health Aff. 2013; 32: 1407–1415.
- Friedman B, Basu J. The rate and cost of hospital readmissions for preventable conditions. Med Care Res Rev. 2004; 61: 225–240.
- Jiang HJ, Wier LM. All-cause hospital readmissions among non-elderly Medicaid patients, 2007: Statistical brief# 89. Agency for Health Care Policy; Research (US), Rockville (MD); 2006.
- Martin CT, Callaghan JJ, Liu SS, Gao Y, Warth LC, Johnston RC. Disparity in total joint arthroplasty patient comorbidities, demographics, and postoperative outcomes based on insurance payer type. J Arthroplasty. 2012; 27: 1761– 1765.
- MELTON III LJ, Brian DD, Williams RL. Urban–Rural differential in breast cancer incidence and mortality in Omisted County, Minnesota, 1935–1974. Int J Epidemiol. 1980; 9: 155–158.
- Melton LJ, Ochi JW, Palumbo PJ, Chu C-P. Sources of disparity in the spectrum of diabetes mellitus at incidence and prevalence. Diabetes Care. 1983; 6: 427–431.
- Chen LM, Jha AK, Guterman S, Ridgway AB, Orav EJ, Epstein AM. Hospital cost of care, quality of care, and readmission rates: Penny wise and pound foolish? Arch Intern Med. 2010; 170: 340–346.