
Case Report
Austin J Psychiatry Behav Sci. 2022; 8(1): 1085.
A Rare Case of Factitious Bleeding from Multiple Sites: Munchausen’s Syndrome
Gomes RR*
Associate Professor, Department of Medicine, Ad-din Women’s Medical College Hospital, Dhaka, Bangladesh
*Corresponding author: Richmond Ronald Gomes, Associate Professor, Department of Medicine, Ad-din Women’s Medical College Hospital, Dhaka, Bangladesh
Received: March 14, 2022; Accepted: April 05, 2022; Published: April 12, 2022
Abstract
Munchausen’s syndrome is a psychiatric disorder in which patients inflict on themselves an illness or injury for the primary purpose of assuming the sick role. These patients can present with many different complaints and clinical symptoms including self-inflicted bleeding. This report describes a case of lately diagnosed Munchausen’s syndrome who presented with bleeding per nose, mouth, hemolacria, hemoptysis and hematochezia. Physicians should always consider this rare disorder in cases presented with bleeding symptoms of unknown origin. This interesting and rare case is presented to create awareness amongst all specially to medical population about Munchausen syndrome so that they can be diagnosed easily and treated with efficiency as well as misdiagnosis and unnecessary use of medical resources can be avoided. We recommend collateral history taking, exclusion of all possible etiologies and detailed briefing of family members as it plays a vital role to reduce the mental and financial suffering of the patient.
Keywords: Munchausen’s syndrome; Hemolacria; Hematochezia; Hemoptysis
Introduction
Munchausen’s syndrome is classified as a factitious disorder in the latest version of Diagnostic and Statistical Manual of Mental Disorders (DSM-5) [1]. The term “Munchausen syndrome” was first coined by Richard Asher [2] in 1951 after a German military man, Baron von Munchausen who traveled from place to place telling fantastic tales about his imaginary exploits. He used this term to describe a syndrome in which patients intentionally made symptoms to gain hospital admission repeatedly. The other names of this disorder are hospital addiction, poly-surgical and professional patient syndrome. Patients of munchausen syndrome intentionally produce physical or psychiatric symptoms to gain medical attention and assume a sick role [2]. Munchausen syndrome is a kind of factitious disorder where physical signs and symptoms are predominant and more striking features rather than psychological symptom. Patients with Munchausen syndrome simulate, induce, or aggravate illness to receive medical attention. To achieve this, they may inflict painful, deforming even life-threatening injury on themselves, their children or other dependents. The primary motivation is not avoidance of duties or financial gain rather to receive medical care. Though the exact prevalence of this condition in Bangladesh is not known, limited studies indicate that patients with factitious disorder may comprise approximately 0.8 to 1.0 percent of psychiatry consultation patients [2]. We documented this interesting case of a 18 years female from Dhaka, who was repeatedly reported and admitted in emergency, ENT, EYE, gastroenterology and hematology department with history of bleeding through nose, ears, eyes, anus and mouth and has been a diagnostic dilemma for a long time, till she was successfully diagnosed and treated as a case of munchausen syndrome.
Case Presentation
An 18-year-old unmarried young Bangladeshi female came through the emergency department (ER) with a history of hemoptysis for last twenty-four hours. The patient reported that this was the fourth episode of hemoptysis in one day. She was managed in ER with fluid support and tranexamic acid injections. Her blood pressure was 90/60mm Hg and pulse was 110 per minute. After stabilization, she was transferred to the inpatient ward for further investigation and management. On examination, the patient was in acute distress due to her recurrent bleeding episode. Rest of the physical examination is unremarkable. Her weight was 43kg and height was 152.5cm.
On query, she repeatedly reported in emergency and admitted in ENT, EYE ward with history of bleeding per nose, ears, eyes, mouth and rectum. Earlier she was sent for hematological assessment to ascertain any bleeding or coagulation factor defect. Neither any abnormalities were not found by ENT/EYE specialist nor were any hematological abnormalities detected in laboratory investigations. Her first hospital admission was in 2017 and second time in 2018. On third hospitalization, in 2020 she was sent for psychiatric evaluation. History revealed that the bleeding was intermittent in nature and initially it occurred 10-12 times per day when she was at her residence. But after admission in hospital incidence was decreasing day by day. Lastly it decreased up to 1-2 times per day while staying in hospital.
Inquisitive history digs out that bleeding never started in front of others, when wiped out never bleed further. No abrasions, bruises, lacerations or injury marks were observed in and around bleeding sites and there is no history of per vaginal bleeding. . She had menarche at an age of thirteen years and she had regular menstruation and reported the use of one pad per day for four days every month. Complete work up for bleeding disorders (complete blood count, bleeding time, prothrombin time, activated partial thromboplastin time, serum von Willebrand factor activity with ristocetin cofactor test, quantitative analysis of platelets) and serology (autoimmune disorders) ordered came back normal. Other base line labs were ordered including basic metabolic panel (BMP), liver function test (LFT) chest X-ray (CXR), stool detailed report and urine detailed report was ordered. All her tests came back normal. Upon request of her parents endoscopy of upper GIT and colonoscopy were also performed with normal results. In addition, a viral panel (Hepatitis B and Hepatitis C) and a CT scan of the abdomen and the chest were non-suggestive of any pathology.
The patient was given pantoprazole oral tablets twice a day and was managed symptomatically. Next day she had blood in tears also with sputum as shown in Figure 1 and 2 which was an alarming symptom and raised the concern of hemolacria secondary to ophthalmological disorder. Ophthalmology consult was made and after ruling out every serious possibility like trauma, tumors, etc., she was put under close surveillance for hemolacria episode. There was no mark of any fresh or dried blood on a body orifice and her breast examination was also satisfactory.
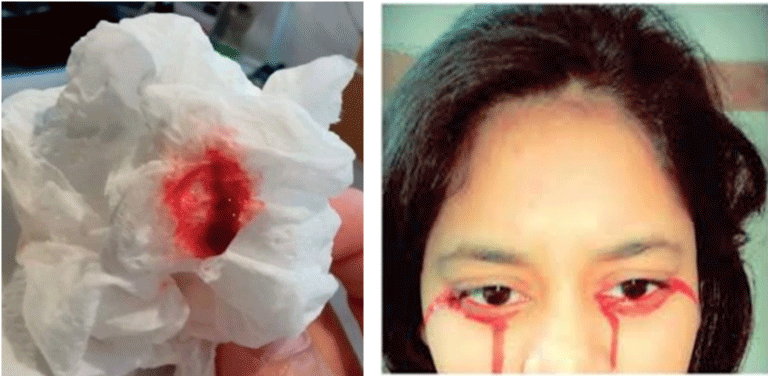
Figure 1: Showing hemoptysis and hemolacria.
On her fifth day of admission, the patient complained of continuous chest pain and she said she had it for three to four times per week since last three years. She added that she forgot to address it on the day of admission. Chest pain was sharp in quality and diffuses in nature. ECG had no acute changes. When asked about any previous episodes of chest pain, she told that she had an episode before and that always relieved by getting some fresh air. According to her, she used to take bath five times in a day. But on examination, she had not changed her clothes since admission. On observation, she was in acute distress and in severe need of any kind of management. Patient demanded medical or surgical treatment to relieve her different symptoms. She was from the low socioeconomic group and family was concerned about her illness and prompt treatment. They had incurred a huge financial loss for last eight months in seeking medical opinions about her various conditions. She was given different treatments but none of them ever helped.
Such plausible and fabricated medical history raised our concern for a psychiatric consult. She was closely observed in psychiatry ward in front of others for hours and no bleeding occurred. Then she was kept alone and within few minutes she had bleeding after having a long session individually with the patient alone and then with her relatives revealed the fact that she was the only female in her family and therefore; the center of attention and care. They counseled family members about her symptoms in detail and advised to keep her occupied in different activities with paying less attention to her complaints. A conclusive diagnosis of Munchausen syndrome was made after a detailed assessment. We discharged her after one week and followed-up with serial cognitive behavioral therapy (CBT) sessions.
Discussion
Factitious disorder has been divided into two groups depending on the types of signs or symptoms feigned. There is one disorder marked by psychological symptoms and another marked by physical symptoms. Both may occur together. In factitious disorder with predominantly psychological signs and symptoms some patients show psychiatric symptoms judged to be feigned. This determination can be difficult and is often made only after a prolonged investigation. The feigned symptoms frequently include depression, hallucinations, dissociative and conversion symptoms, and bizarre behavior. Because the patient’s condition does not improve after routine therapeutic measures are administered, he or she may receive large doses of psychoactive drugs and may undergo electroconvulsive therapy.
Munchausen’s Syndrome is a rare psychiatric disorder and a diagnosis of exclusion was first described by Richard Asher in 1951 [2]. This disorder was named for Baron Karl Friedrich von Munchausen who was born in Germany, joined the Russian military, and was known to tell unreal and fantastic tales about the battles he participated in against the Ottoman Turks [2]. In broad term, Munchausen syndrome is a type of factitious disorder with predominantly physical sign and symptoms to seek hospitalization. Such patients are easily consenting to invasive or non-invasive means of treatment. Many patients even demand an invasive intervention. It is always necessary to rule out malingering or any kind of secondary gain other than the hospitalization [3,4].
Another variant described in the literature is Munchausen by proxy in which a caregiver is fabricating symptoms to instigate medical treatment. One should give special attention to this form where falsification and feigning of symptoms might lead to potential harm to the child. This is a form of child abuse and it should be reported to higher officials or child protecting services if mandatory [5,6].
Asher proposed three types of Munchausen presentation; acute abdomen, acute bleeding episode, neurological emergency. However, it may have a variable presentation. Additionally, people employed in the healthcare industry such as nurses, lab technicians, paramedics and their relatives might have an easy access to medications or other materials which may help them to produce symptoms [7,8]. On the other side, genuine illness may coexist in the same patient or new illness may occur in a patient previously diagnosed with Munchausen. Hence, detailed history and physical examination including prompt laboratory evaluation may be mandatory each time because the management would be different [9,10]. Patients undergo various medical and surgical treatments and incur financial loss especially in places where health care is not covered for individuals.
Factitious disorder with predominantly physical signs and symptoms is the best-known type of Munchausen syndrome. Clinical presentations are myriad and include hematoma, hemoptysis, abdominal pain, fever, hypoglycemia, lupus-like syndromes, nausea, vomiting, dizziness, and seizures. Urine is contaminated with blood or feces; anticoagulants are taken to simulate bleeding disorders; insulin is used to produce hypoglycemia; and so on. Such patients often insist on surgery and claim adhesions from previous surgical procedures. These features are dramatic and more alarming than other types of factitious disorders that distinguish Munchausen syndrome. Among factitious disorder Munchausen Syndromes are alarming and with worse prognosis. Bleeding is one of the main presenting features of Munchausen syndrome. As it is an alarming and more dramatic symptom, extensive investigations and numerous hospitalizations are carried out for diagnosis [11].
There are no reliable statistics regarding the prevalence of this disorder, but it is considered to be rare. Although any age group may be affected, most patients are female and between 20 and 40 years of age [12]. The exact cause of this syndrome is a subject of debate. Some theories suggest that a history of abuse or neglect as a child, or a history of frequent illnesses that required hospitalization might be factors in the development of the syndrome. Researchers are also studying a possible link to personality disorders, which are common in people with Munchausen’s syndrome [13]. This patient was also a young female and possibly to have a histrionic personality disorder.
In Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) no distinction is made between the two and the disorder is divided into that “imposed on self” and that “imposed on another” (factitious disorder by proxy). According toDSM-5, following criteria must be fulfilled to diagnose a case of factitious disorder imposed on self [1]:
• Falsification of physical or psychological signs or symptoms, or induction of injury or disease, associated with identified deception.
• The individual presents himself or herself to others as ill, impaired, or injured.
• The deceptive behavior is evident even in the absence of obvious external rewards.
• The behavior is not better explained by another mental disorder, such as a delusional disorder or another psychotic disorder
Presence of symptoms only when the patient is alone or not being observed, appearance of new or additional symptoms following negative test results, being more comfortable in the hospital than you might think, and history of seeking treatment at different hospitals are the main characteristics of this disorder [14]. This case was fulfilling these indicators which oriented us to a possible diagnosis of a factitious disorder.
Treatment for Munchausen’s syndrome usually involves psychiatric counseling to change the thoughts and behaviors that are causing the condition [1]. Cognitive-behavioral therapy, family therapy and group therapy are the possible treatment modalities of this disorder. Although there are no medicines to treat factitious disorders, they may be used to treat any related condition such as depression, anxiety, or a personality disorder [14]. However, it can be difficult because most people refuse to admit they have a problem and will not cooperate with suggested treatment plans, as seen in this case.
The most important prognostic factors of these patients are early suspicion and identification of disease, prompt psychiatric referral and the presence of mood disorder or personality disorder6. The three major goals in the treatment and management of factitious disorders are (1) to reduce the risk of morbidity and mortality, (2) to address the underlying emotional needs or psychiatric diagnosis underlying factitious illness behavior, and (3) to be mindful of legal and ethical issues. Perhaps the single most important factor in successful management is a physician’s early recognition of the disorder. In this way, physicians can forestall a multitude of painful and potentially dangerous diagnostic procedures for these patients. Good liaison between psychiatrists and the medical or surgical staff is strongly advised. Although a few cases of individual psychotherapy have been reported in the literature, no consensus exists about the best approach. In general, working in concert with the patient’s primary care physician is more effective than working with the patient in isolation. Physicians require a great deal of tolerance to strengthen patient-therapist alliance. This will help to develop conscious selfcontrol of the patient so that he or she can minimize the feigned illness symptoms [15]. Patient should be steered towards psychiatric treatment in an empathic, non confrontational, face saving manner. Psychiatrists should treat the underlying psychiatric condition, such as Axis I or Axis II disorder. In psychotherapy, addressing coping strategies and emotional conflict is beneficial. After the diagnosis of our patient, management of her underlying stress, regular counseling and psychotherapy sessions resulted in an excellent prognosis of our patient. We also recommended follow up visit which could not be ensured due to lack of mental health awareness of parents.
We suggest that physicians should report more cases of Munchausen syndrome. As this disease is not researched extensively more research should be done to understand the disease and its cultural, social and psychological aspects. More research can find out the best treatment strategy for such patients and develop a culturally sensitive treatment approach.
Conclusion
Patients who might belong to solitary lifestyle or who face sudden cessation of attention from people might feign their symptoms and assume a sick role to get the medical attention. The primary and only intention in such cases is to get the desired level of attention as before. A diagnosis of Munchausen does not exclude coexistence of a genuine illness and hence detailed physical and prompt evaluation is cardinal before definite diagnosis. Munchausen and other conditions in the spectrum of factitious disorders remain heavily underdiagnosed by psychiatrists as well as general physicians. This case report will contribute towards enhancement of knowledge among the physicians and increase the awareness of general population about Munchausen syndrome. In conclusion, factitious causes should always be considered in unclarified origin of bleeding, especially in cases presented with dramatic but inconsistent medical history, and an unusual personal behavior.
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Publishing. 2013.
- Asher R. Munchausen’s syndrome. Lancet. 1951; 1: 339-341.
- Yates GP, Feldman MD. Factitious disorder: A systematic review of 455 cases in the professional literature. Gen Hosp Psychiatry. 2016; 41: 20-28.
- Padhye KP, David KS, Dholakia SY, et al. Munchausen syndrome: A forgotten diagnosis in the spine. Eur Spine J. 2016; 25: 152-156.
- Braham MY, Jedidi M, Chkirbene Y, et al. Caregiver-fabricated illness in a child: A case report of three siblings. J Forensic Nurs. 2017; 13: 39-42.
- Doughty K, Rood C, Patel A, et al. Neurological manifestations of medical child abuse. Pediatr Neurol. 2016; 54: 22-28.
- Rabbone I, Galderisi A, Tinti D, et al. Case report: When an induced illness looks like a rare disease. Pediatrics. 2015; 136: 1361-1365.
- Inui K, Hanafusa T, Namiki T, et al. Intractable postoperative wounds caused by self-inflicted trauma in a patient with cutaneous Munchausen syndrome presenting as a pyoderma gangrenosum-like lesion. Case Rep Dermatol. 2016; 8: 97-101.
- Bass C, Glaser D. Early recognition and management of fabricated or induced illness in children. Lancet. 2014; 383: 1412-1421.
- Brown AN, Gonzalez GR, Wiester RT, et al. Care taker blogs in caregiver fabricated illness in a child: a window on the caretaker’s thinking? Child Abuse Negl. 2014; 38: 488-497.
- Koufagued K, Chafry B, Benyass Y, et al. Munchausen syndrome revealed by subcutaneous limb emphysema: A case report. J Med Case Rep. 2015; 9: 172.
- Jaghab K, Skodnek KB, Padder TA. Munchausen’s Syndrome and Other Factitious Disorders in Children: Case Series and Literature Review. Psychiatry (Edgmont). 2006; 3: 46-55.
- Alinejad NA, Oettel DJ. Factitious disorder as repeated diabetic ketoacidosis: a case report. Innov Clin Neurosci. 2011; 8: 41-47.
- Cleveland Clinic. Diseases and Conditions. Munchausen Syndrome.
- Almeida J, da Silva JA, Xavier M, et al. Munchausen syndrome mimicking psychiatric disease with concomitant genuine physical illness. BMJ Case Rep. 2010; 2010: 0720103142.